Abstract
Background:
Wound infections constitute a significant problem in surgical procedures. In cesarean sections (CS), this is particularly important as a wound infection not only results in increased morbidity but also has far-reaching implications by way of pelvic organ disease, disturbance of the bonding process between mother and baby in the puerperium, and a longer hospital stay with its inherent problems.
Objective:
This study was conducted with the aim to determine the incidence and risk factor associated with surgical site infection (SSI) following cesarean section.
Methodology:
A retrospective cross-sectional study was conducted for 400 women undergoing cesarean section procedures during an 18-month period from January 2013 to June 2014 at Hospital Pulau Pinang, Malaysia. Patients’ socio-demographic, clinical data and incidence of SSI following the CS were noted using a standardized data collection form. SPSS v 21 was used for data analysis.
Results:
In total, 18.8% of the study participants developed SSI. Multivariate logistic regression analysis identified the following: higher body mass index (≥30 kg/m2) (odds ratio [OR]: 0.555; 95% confidence interval [CI] = 0.313-0.985, P = .044), increase in the blood loss during surgery (≥500 mL) (OR: 0.757; 95% CI = 0.423-1.354, P = .034), prolonged hospital stay (≥4 days) (OR: 0.439; 95% CI = 0.260-0.740, P = .002), spinal anesthesia (OR: 1.543; 95% CI = 1.230-1.937, P = .021), breech baby presentation (OR:2.927 95% CI = 1.020-8.400, P = .046), and intrathecal analgesia (OR:1.567; 95% CI = 1.246-1.970, P = .001) had statistically significant association with incidence of SSI.
Conclusions:
Surgical site infections are common among women undergoing CS at Hospital Pulau Pinang. Special attention and enhanced clinical management of patients with identified risk factors for developing SSI may decrease its incidence.
Introduction
Surgical site infection (SSI) is the second most common infectious complication after urinary tract infection following cesarean section (CS) delivery. 1 Surgical site infection after cesarean section is associated with increased maternal morbidity, prolonged hospital stay, and increased medical costs. 2 The beneficial effect of antibiotic prophylaxis in reducing occurrences of infection associated with elective or emergency cesarean section is already well established.3,4 In many institutions, the antibiotic administration is performed after the umbilical cord has been clamped, justified by the neonatal impact of antimicrobial use.4,5 Although antimicrobial prophylaxis reduces the risk of endometritis and incisional SSI when administered correctly, much has been discussed about its real impact due to the small number of studies and their limitations.4,6,7
The rates of SSI after CS reported in the literature ranges from 3% to 15%, depending on the surveillance methods used to identify infections, the patient population, and the use of antibiotic prophylaxis.8,9 The risk factors for SSI in association with cesarean section are many, including those case-mix issues present in the surgical patient population such as age, factors such as type of CS (elective vs emergency), and patient care practices such as antibiotic prophylaxis. Analysis of the combined effects of the intrinsic and extrinsic risk factors predisposing patients to SSI is necessary to detect the common links. The intrinsic factors are patient related, and the extrinsic factors are related to the management and care. Although the intrinsic factors cannot be changed, the risk they present in terms of infection is identifiable and manageable. Surgical site infection is linked to factors associated with surgery, which may influence the risk of infection. Another risk factor which may contribute to SSI is body mass index (BMI). A greater rate of infection associated with obese women undergoing CS surgery has been reported. 10
This study was conducted to determine the SSI rate and to identify risk factors for SSI after cesarean section. A better understanding of predictors might improve infection control by reducing the clinical effects of post-cesarean infections.
Materials and Methods
Study design
The current retrospective chart review of 400 cesarean deliveries was conducted at a Hospital Pulau Pinang in Malaysia from January 2013 to June 2014. This study included all the women who had delivered a baby through cesarean including (emergency and elective cesarean) in Hospital Pulau Pinang from January 2013 to June 2014 with completed data charts.
A standardized data collection form was used to collect the information of patient’s socio-demographics and clinical characteristics. The information collected included the following: medical record number, age, race, BMI, duration of surgery, duration of hospital stay, cesarean type, anesthetic technique, acute pain service, blood loss during surgery, previous CS, indication of CS, and the incidence of SSI.
Sampling and sample size
The sample size was calculated according to the following assumption: the prevalence of cesarean section (28%) was taken from a study setting in Penang (1479 cesarean cases from 5214 deliveries in 2013. This information was taken after a discussion with the head of department at Hospital Pulau Pinang as the latest estimates indicate that the prevalence of CS in Penang was 17.4% in 2006). 11 There was a confidence interval (CI) of 95%, and an allowable margin of error of 5%. Using the Raosoft online equation, the calculated sample size was 306. With 30% uncompleted data, the target number was 400.
Surgical site infection
An SSI is an infection that occurs after surgery in the part of the body where the surgery took place. Surgical site infections can sometimes be superficial infections involving the skin only. Other SSIs are more serious and can involve tissues under the skin, organs, or implanted material.
All women who underwent cesarean in Hospital Pulau Pinang received prophylaxis antibiotic. Preoperation antibiotics are given approximately within 60 minutes before surgery. This include Unasyn IV (ampicillin and sodium/sulbactam sodium) 1.5 and 3 g, respectively, according to the weight of the patients. This is given routinely to prevent postoperative infection. The surgery is performed by the consultant, and the abdomen is prepped for surgery using abdominal gel preparation. The abdomen is carefully washed and disinfected to reduce the amount of bacteria on the skin and the chances of infection following delivery. The mother is placed on an operating table. If she is going to have an epidural or spinal anesthesia for the cesarean, it is usually performed at this time. If she will be receiving general anesthesia (being put to sleep), the anesthesia is usually not administered until just before the surgeon is ready to begin the surgery; this is done to minimize the time the drugs circulate in the mother’s bloodstream with the potential to reach the baby. Although these drugs are not harmful to the baby, they can make the baby somewhat slow to adapt to life and can increase the risk for respiratory distress requiring resuscitation.
The mother’s arms are typically placed on boards extending directly out from her body. This allows easy access to the mother’s veins, to administer medicine. It also prevents the mother from unconsciously reaching down to her belly during the surgery and contaminating the operative field, thus increasing the risk for infection.
Statistics
The collected data were entered into the computer and analyzed using SPSS software (version 21). The results are presented as a mean with 95% confidence limits or standard deviations. A P value of <.05 was accepted as statistically significant. A χ2 test was used to identify factors which had statistical significant association with the incidence of SSI. In addition, logistic regression analysis was employed to quantify the effect of the significant variables and their effects on SSI incidence, to obtain a final model predicting.
Results
The mean age for the women was 30.36 ± 4.8 (range = 17-45) years. The mean weight was 73.35 ± 14.3 (range = 38.00-129.8) kg, and the mean height was 156 ± 0.61 (range = 143-175) cm. The BMI for these women was less than 30 in 63.5% of the patients and more than 30 for the rest. The BMI ranged between 18 and 56 with a mean of 29.89. In addition, 76.5% of these women were Malay, 14.5% Chinese, and 9% were Indian. Regarding indications, the main indications were fetal distress 27.8% and previous CS 26.0%. In addition, 63.25% of the patients had an emergency cesarean, whereas 36.75% had an elective cesarean; 89.75% received spinal anesthesia, whereas 7% received general anesthesia and 3.25% received epidural anesthesia. A summary of the sample characteristics is presented in Table 1.
Demographic characteristics for 400 patients having CS in Hospital Pulau Pinang (HPP) from 2013 to 2014.
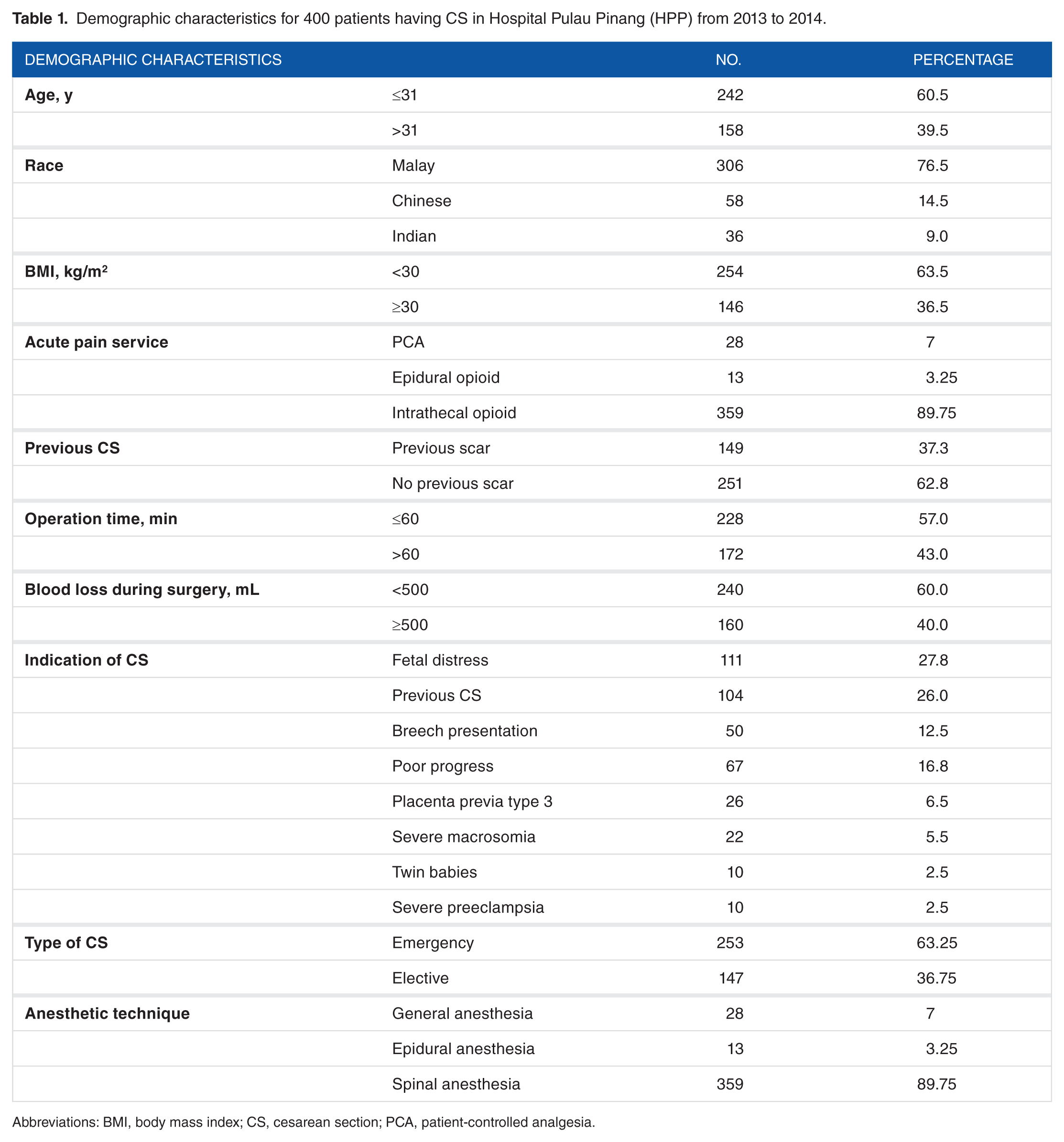
Abbreviations: BMI, body mass index; CS, cesarean section; PCA, patient-controlled analgesia.
Table 2 represents the percentage of antibiotic drugs used by the women who underwent cesarean.
Percentage of antibiotic drugs used by cesarean patients at Hospital Pulau Pinang (HPP).
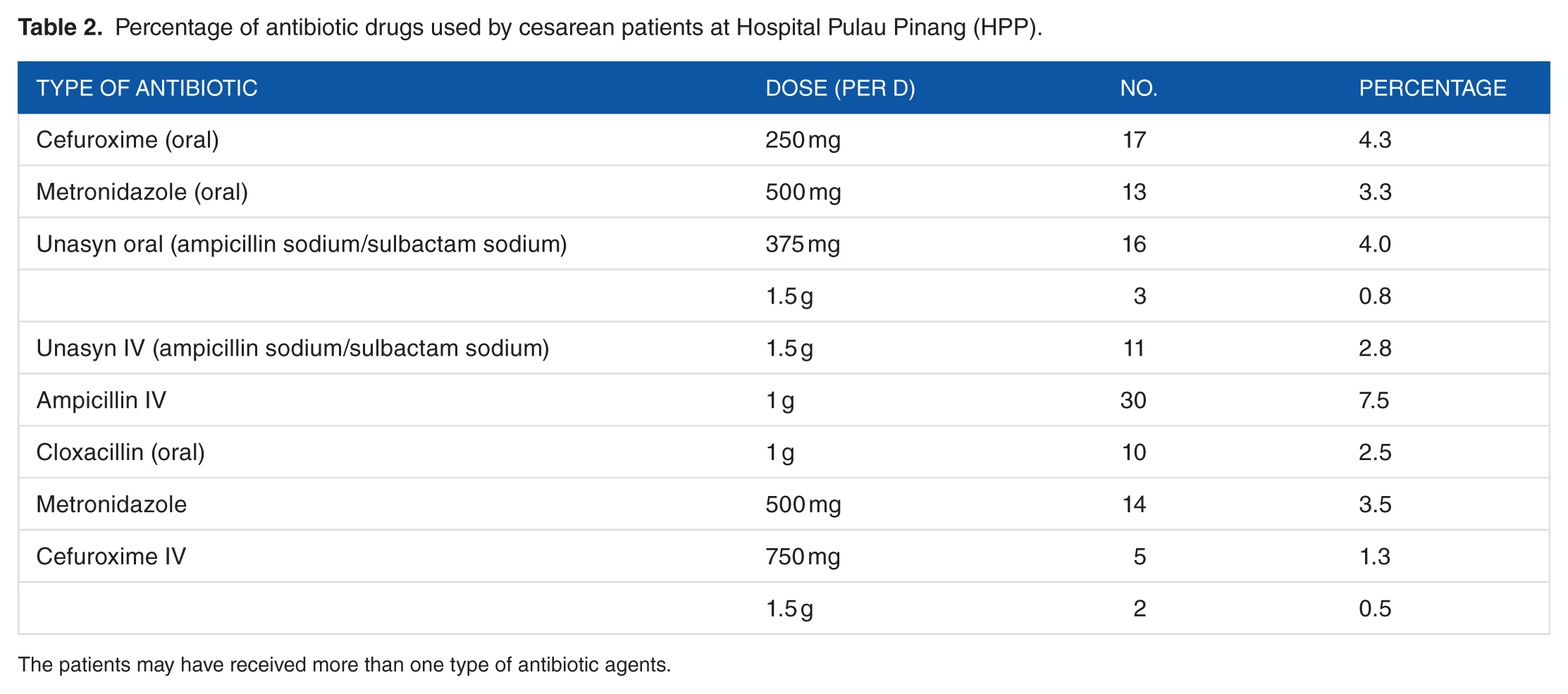
The patients may have received more than one type of antibiotic agents.
To examine the relationship between SSI incidence and patient demographic characteristics, χ2 test was used. The results are presented in Table 3. These results showed that there was a statistically significant association between duration of hospital stay and the incidence of SSI (P = .002). In addition, there was a significant association with acute pain service (P = .001), blood loss during surgery (P = .043), BMI (P = .013), anesthetic techniques (P = .001), and indication of CS (P = .012). However, there was no association between race, operation time, age, previous CS, and CS type with the incidence of SSI.
Factors affecting the incidence of SSI in cesarean patients at Hospital Pulau Pinang (HPP) (n = 400).
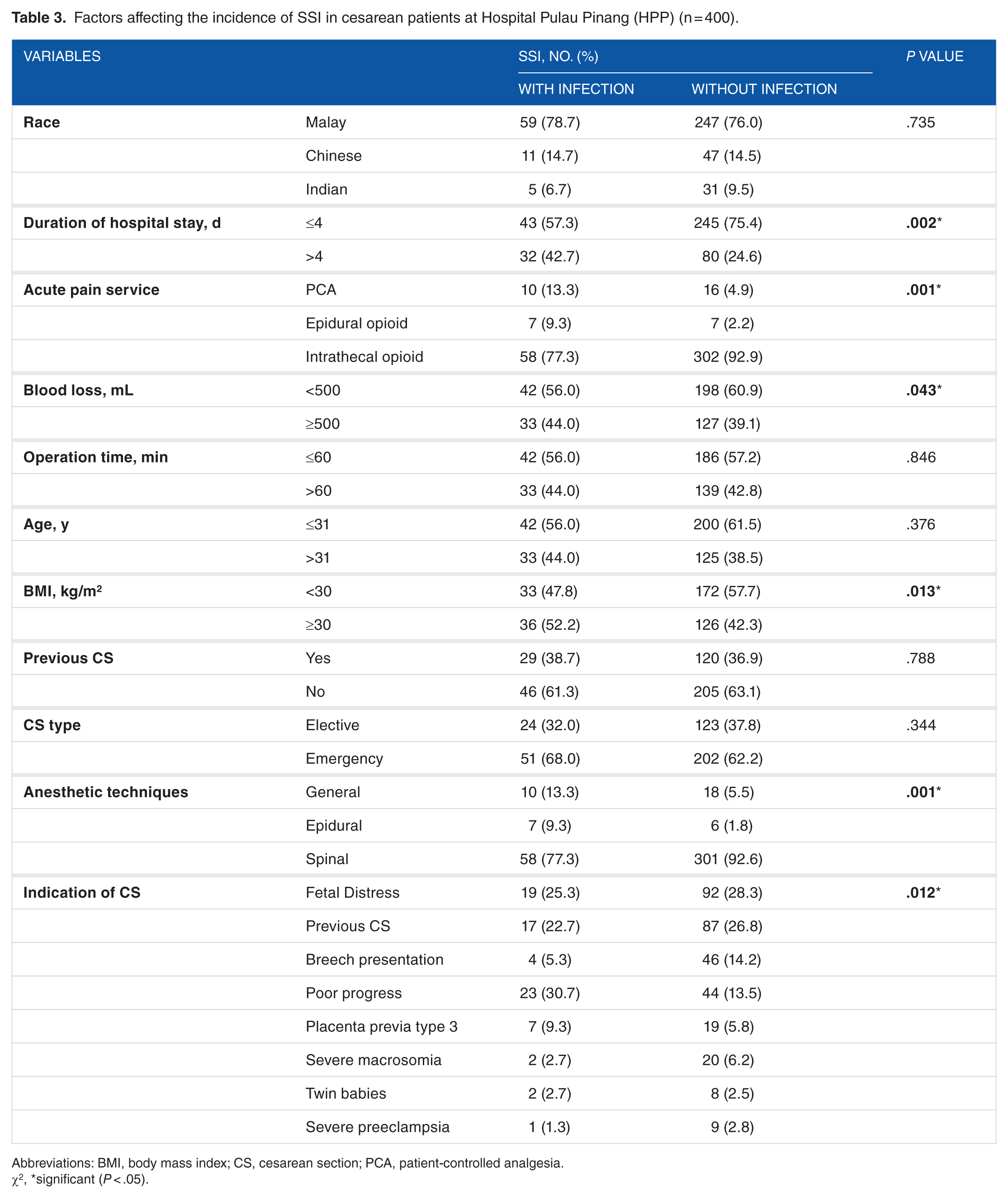
Abbreviations: BMI, body mass index; CS, cesarean section; PCA, patient-controlled analgesia.
χ2, *significant (P < .05).
A multivariate logistic regression was performed to ascertain the effects of BMI, blood loss during surgery, acute pain service, duration of hospital stay, anesthetic techniques, and indication of CS on the likelihood that participants had SSI, as can be seen in Table 4. The results show that a higher BMI as well as an increase in the blood loss during surgery were associated with increase the likelihood of having SSI. Women with a breech presentation baby had more likelihood of having SSI compared with women having other types of CS indication. Turning to anesthetic techniques, patients with spinal anesthesia and intrathecal analgesia had more likelihood of having SSI. These variables were found to be independent predictors for SSI in the women who underwent cesarean.
Contribution factors effect on SSI incidence for cesarean patients at Hospital Pulau Pinang (HPP).
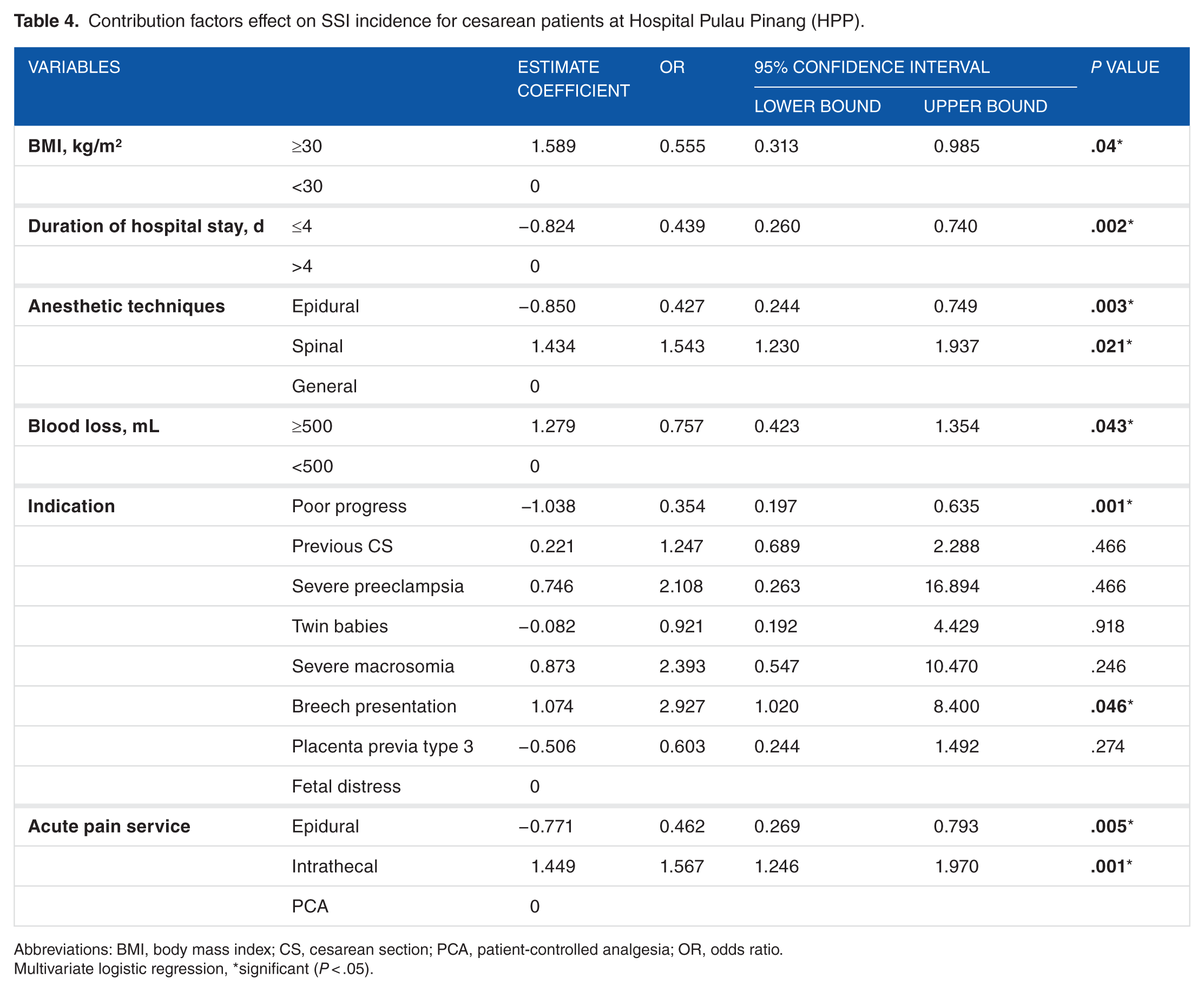
Abbreviations: BMI, body mass index; CS, cesarean section; PCA, patient-controlled analgesia; OR, odds ratio.
Multivariate logistic regression, *significant (P < .05).
Discussion
Incidence of SSI
In this study, the prevalence of SSI following CS was 18.8%; however, the rate was higher than the 11.2% reported by Hughes in a tertiary-care referral center in Malaysia. 12 Ward et al 13 in a multicenter collaborative study of SSI following CS in the United Kingdom reported an overall wound problem of 13.6% and an SSI rate of 8.9%. This, however, ranged between 2.9% and 17.9%. These authors prospectively studied CS wound infection, including the use of postdischarge surveillance. We did not use postdischarge surveillance in our study, but all patients who complained of SSI postoperatively were included. An SSI rate of 18.8% in our patients was more than the range of 2.9% to 17.9% sited above in the United Kingdom. We are unable to explain the discrepancy between the results of that study and ours, although it could be due to ethnic, environmental, or genetic differences between that particular study population and ours.
Risk factors associated with CS SSI
Multiple logistic regressions showed 6 variables independently associated with post-cesarean SSI; these variables are BMI, blood loss during surgery, breech baby presentation, intrathecal analgesia, spinal anesthesia, and duration of hospital stay. These variables were found to be independent predictors for SSI in the women who underwent cesarean.
The findings of this study demonstrated that a significant association between SSI and BMI has been noted, and this was in line with other studies.10,13–15 This may be a result of the standard dosage of prophylactic antibiotics achieving inadequate tissue concentrations in obese women, 16 particularly if there has been no adjustment to the dose in proportion to BMI. In addition, the relatively poor perfusion of adipose tissue may impair wound healing and decrease the local immune response, enabling infection to occur. 17 The incision for obese women may also need to be longer and therefore involve more tissue becoming exposed to contamination. 16 Although suturing of the subcutaneous tissue space is recommended to reduce the risk of wound infection and dehiscence for women with >2 cm of subcutaneous fat, as yet, there is no recommendation regarding the optimal incision type for obese women. 18 However, there may be limited opportunities to tackle obesity by giving dietary advice in early pregnancy or preconception. 18
Likewise, the findings of this study showed that there is a significant correlation between SSI and blood loss during surgery; this was in line with other studies that found risk of postoperative infection has been shown to be proportional to the volume of blood loss during cesarean.19,20 Tran et al found that the risk of SSI increased 30% for every 100-mL increment of blood loss. A high volume of blood loss is usually associated with poor control of bleeding, increased tissue damage from prolonged retraction and manipulation, as well as more sutures. Suture, a foreign body, can promote contamination and reduce local resistance mechanisms. 21
This study provides evidence that intrathecal analgesia and spinal anesthesia are associated with a higher risk of post-cesarean section SSI compared with general anesthesia and epidural anesthesia. However, another study in Taiwan found that general anesthesia is associated with a higher risk of post-cesarean section SSI compared with neuroxial anesthesia. 22 Mechanisms underlying the differential impact of the modes of anesthesia on post-CS SSI are largely unknown.
The findings of this study show that babies with a breech presentation are at a greater risk of post-cesarean SSI. This factor is a unique contribution to research and was not tested before. Further research in this area is encouraged.
Prolonged hospital stay has been shown to be a risk factor for post-cesarean SSI. Barbut et al 23 found that infected patients were hospitalized for longer (median: 6 days) than noninfected patients. Prolonged hospital stay has been identified as being a risk factor for SSI and nosocomial infections. Alternatively, prolonged hospital stay may be a result of SSI.
The findings from this study did not show a correlation between SSI and other variables such as age, race, previous CS, and CS type. However, type (emergency or elective) of CS was not a significant determinant of SSI in this study. Generally, patients undergoing emergency CS are at higher risk of infections24,25 because of inadequate preparation time owing to maternal or fetal threat, and similar results have been recorded by other researchers. 26
Conclusions
This study showed that the rate of SSI following cesarean section is approximately 18.8% in Pinang, considering the large number of women undergoing cesarean section in Malaysia. These infections are likely to incur substantial additional health care costs. Significant independent risk factors for SSI were as follows: higher BMI, increase in the amount of blood loss during surgery, breech baby presentation, intrathecal analgesia, spinal anesthesia, and the duration of hospital stay. The risk factors identified in this study are important in terms of the potential review of practice and subsequent reduction in SSI. Post-cesarean SSI commonly complicates CS in our unit. Strategies for the prevention of this morbidity in CS patients must aim to control mother’s weight during pregnancy and reduce intraoperative blood loss. Patients should be made aware of the risk of SSI, particularly where there is a high risk due to the type of anesthesia and analgesia or known patient risk factors. This will allow patients to make better informed decisions about whether to proceed with surgery in maternal request cesarean. More studies regarding effect of anesthesia and analgesia type as possible contributing factors to the development of SSI after cesarean section are required to be conducted. In addition, effort should be made to reduce length of hospital stay after cesarean section. Overall strategies that reduce CS rate will lower this morbidity and its sequelae.
Limitations
A retrospective chart review may result in collecting inaccurately charted information from the medical record. Some charts had more thorough charting than others. Misinterpretation of meaning in the written documentation is also a possible source of error. Extraneous variables such as environmental conditions and socioeconomic status cannot be controlled, may not even be identified, and may affect the results. Despite these limitations, this study provides valuable information regarding the post-cesarean SSI as well as risk factors affecting SSI.
Footnotes
Acknowledgements
The authors would like to acknowledge Dr Hadeer Akram AbdulRazzaq for his scholarly guidance and support throughout this study.
Peer review:
Five peer reviewers contributed to the peer review report. Reviewers’ reports totaled 512 words, excluding any confidential comments to the academic editor.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
HHJ conceived and designed the experiments and wrote the first draft of the manuscript. SASS jointly developed the structure and arguments for the paper. AHK made critical revisions and approved final version. OTD analyzed the data. AHA contributed to the writing of the manuscript. RU agree with manuscript results and conclusions. All authors reviewed and approved the final manuscript.
Disclosures and Ethics
The ethical approval of this study was granted by the National Institutes of Health (NIH), Ministry of Health, Malaysia, with research number NMRR-14-559-19654.
