Abstract
Globally, surgical site infections are one of the common infections which lead to a large amount of mortality and morbidity in postsurgical care. The risk for surgical site infection is multidimensional which includes mainly; patient, surgery, and hospital-related factors. This study is aimed to determine the burden of SSIs along with contributed risk factors. A prospective observational cross-sectional study was conducted in one of the largest public-sector hospitals in Pakistan. A total of 412 patients were recruited in the study with full consent and monitored for 30 days after surgery with direct and indirect surveillance. Overall, in seven different surgical procedures the incidence (29.8%) rate of SSI was observed; in appendectomy (
Introduction
Globally, surgical infections contributed to a large burden of disease. LMICs (lower-middle-income countries) have many challenges in managing. 1 Likely, one of the great challenges is the increasing rate of antimicrobial resistance (AMR), probably linked to the misuse of antibiotics adds to challenge. Expansion of surveillance, prevention of infection, and antimicrobial stewardship programs are preliminary steps forward and have a role in the prevention of surgical infections. 1 Surgical site infections (SSIs) are common infections developed after surgery. Centers for Disease Control and Prevention (CDC) defined Surgical Site Infections (SSIs) as “infections that occur after surgery at the site of incision, organ, or space.” 2 The ECDC (European Centre for Disease Prevention and Control) postulates the same that SSI must happen within thirty days after surgery without implant. 3 Current findings by the WHO (World Health Organization) reported that SSI remains the second most common type of HAIs (Hospital-Acquired Infections) in the United States and Europe that is linked with increased length of stay at hospitals. 4 Additionally, in the US alone during the period from 2006 to 2009, nearly 1.9% of surgical operations were affected by SSIs. 5
The rate of SSI is higher in the developing world than that in developed countries. The post-discharge surveillance of SSI in elective clean and clean-contaminated surgical procedures was carried out during 2019 and 15% incidence was reported in LMICs. 6 The prevalence of HAIs was lower in 2015 than in 2011 after continuation to make improvements in the prevention of such infections, as per strategies increased by CDC. 5 HAIs may affect approximately 5% to 20% of patients during hospitalization. It is estimated that in Europe, about 7.5 million patients (acute hospitals 3.5, 4.2 million in the tertiary care facilities) develop HAIs every year. Nearly 147,000 patients in European hospitals die annually from HAIs, directly or indirectly, with SSIs at the forefront. 7 A 2002 Canadian study reported a 4.25% incidence rate of wound infection after cardiac surgery approximately 29,000 patients.8,9 The incidence of SSIs is four times higher in LMIC. 10 The SSIs accounted for approximately 31% of all HAIs and up to 20% of post-surgical readmissions. 10
Recently, a study reported from Pakistan showed that in older patients, 4 out of 9 developed SSIs, and those who underwent emergency surgeries were the most affected. 11 Pakistan is the seventh most populated country in the world with a population of 212.2 million. Pakistan established its first National Infection Guidelines in 2006. 12 WHO has developed evidence-based guidelines and recommendations for the prevention of SSI.13,14 Implementation of these guidelines and further modification is a challenge in Pakistan. 15 Most of the health care setups have no institutional guidelines or SOPs to follow. 16 No detailed data is available on SSIs from Pakistan and few pilot studies are documented which are totally against WHO criteria in a region. Inappropriate choice, the timing of administration, and the combination of SAP observed in Pakistan. 17
Factors associated with an increased risk of SSI include; emergency procedures and longer duration of surgery. 18 Numerous risk factors are involved in SSI with a complex relationship as; surgery, patients, microbial, and environment-related factors. 18 The incidence rate of SSIs mainly depends upon the health care facility, surgical procedure, and level of care. Patients of SSIs are closely linked with increased length of stay, delayed wound healing, pain, discomfort, long-lasting disability, and even death. 19 Single-incision Laparoscopic Surgery (SILS) is technically feasible and safe for patients undergoing colorectal surgery with no unusual complications. 20
Clinicians should limit the use of quinolones and remain aware of the possibility of resistance developing by colistin. 21 Surgeons’ perspective has shown that the associated risk factors and treatment outcomes of surgical patients may have a direct association with the incidence of SSIs. 22 Antibiotic prophylaxis is one of the major domains to prevent and reduce the rate of surgical site infections. Mainly antimicrobial stewardship (AMS) programs are also focused on an audit of surgical prophylaxis. 23 The current study is aimed to examine the incidence rate of surgical site infection along with risk factors responsible.
Methods
Study design and setting
A cross-sectional study was carried out in the general surgical wards. The current study was conducted in 92-bed general surgery wards of PIMS (Pakistan Institute of Medical Sciences), a 592-bed tertiary care teaching hospital associated with Shaheed Zulfiqar Ali Bhutto Medical University (SZABMU). PIMS hospital is one of the largest hospitals in the country, located in the capital, Islamabad.
The United States CDC (Center for disease control and Prevention) surveillance methods were used. 24 Trained assistants (two nurses and two pharmacists) collected indirect surveillance data from patient medical records through validated data collection forms. Research study assistants also investigated all surgical sites during wound dressing and changing 24 to 48 h after the surgical procedure (direct surveillance). Swabs of suspected SSIs were taken and sent for analysis by assistants, along with post-discharge surveillance. For the post-discharge surveillance, patients were asked to come back for follow up after 30 days. If this did not happen consented patients were contacted through mobile phone numbers and if SSIs were suspected, patients were then asked to visit the same hospital to possibly confirm the diagnosis. The National Health Safety Network CDC criteria were used for the SSI diagnosis. 24 Patient’s medical records, antibiotics prescriptions were collected and presented in the shape of drug utilization.
Sample size, study participants, and patients characteristics
The sample size was determined through Ra-osoftTM calculator with the confidence interval 95%, a margin of error 5%, and the assumption of 80% an adherence rate. This created a sample size requirement of 385. Attrition rate assumed at about 20% and the existence of outliers, a sample of 412 respondents was needed to be included in the present study.
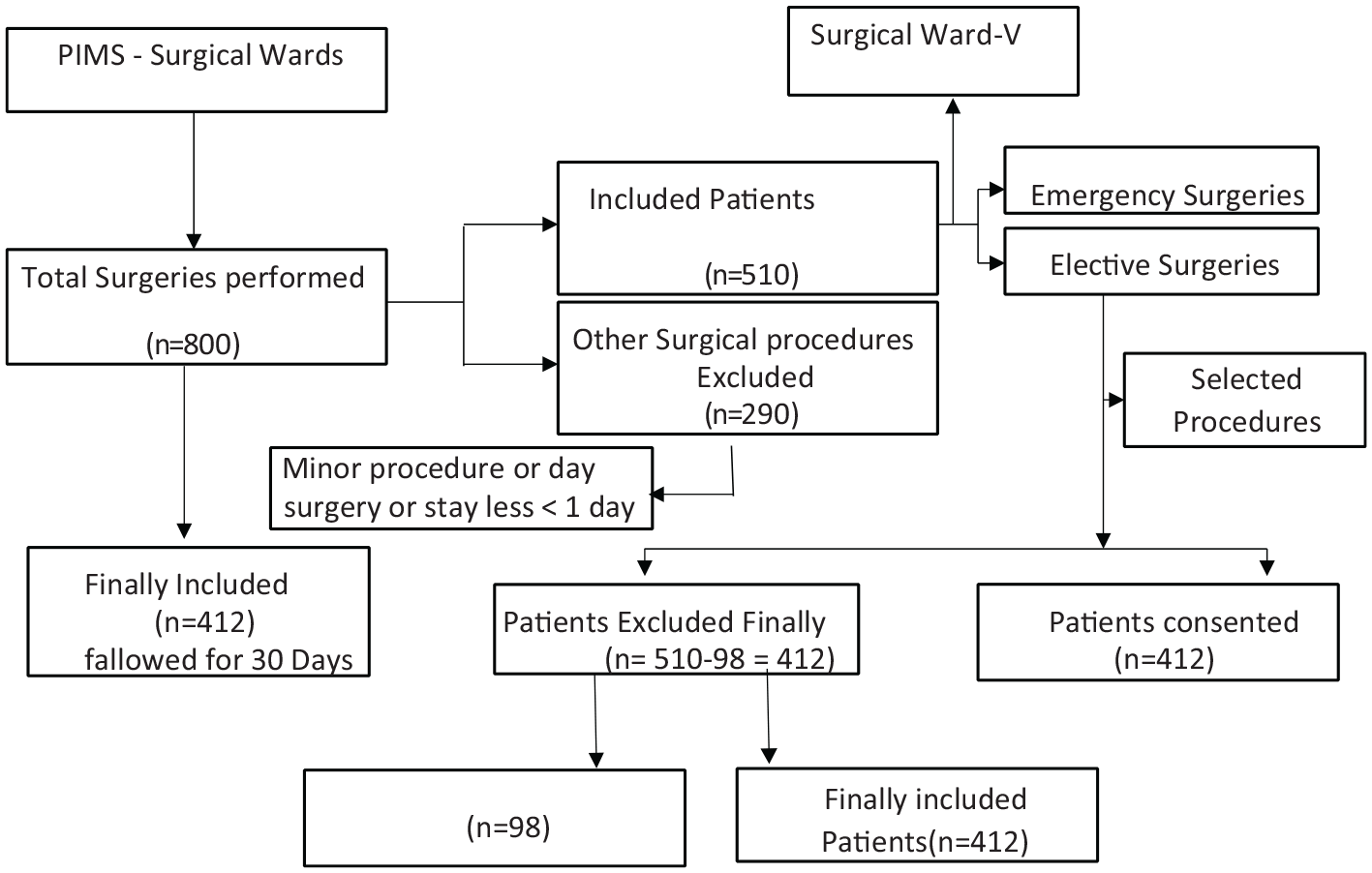
All patients admitted between November 2016 and August 2017 were prospectively included in the survey. All non-surgical patients were excluded from the study. A total of 800 patients were admitted to the given surgical wards. Among (
Sampling techniques and laboratory method
Collected swabs samples were plated on the medium of blood and MacConkey agar. For the identification of pathogenic bacteria, standard and conventional methods were used.
25
Antibiotics susceptibility testing was done through the Kirby-Bauer disc-diffusion method on Mueller-Hinton agar plates. The Disc strength was according to the recommendation of CLSI (Clinical Laboratory Standard Institute). CLSI interpretation criteria were used for the susceptibility and resistance. Gram-negative bacteria intermediate susceptible isolates were considered resistant in the calculations.
Data collection
A literature survey was done with (MeSH) keywords before the questionnaire development and different questionnaires were reviewed concerning incidence, factors responsible for the SSIs, along with antibiotics rationality. Finally, a comprehensive data collection form was developed that included (a) general identification and patient information, (b) demographics and socio-demographics (gender, age, education, financial status, residence, occupation, and marital status) (c) patient diagnosis-related, (d) surgery-related, (e) pre and post-operative antibiotics, (f) hospital facilities related factors, (g) KUNIN and MUST criteria. The data collection form was first validated from the research committee of the pharmacy department and two experts from the other academic institutes validated the data collection forms through the face and content validity (Supplemental File S1). The hospital review research committee alongside the ethical review board also approved the final validity of the data collection forms and approve the data collection commencement (Schematic/Flow Chart 1).
Ethical approval
Ethical approval was obtained from the Quaid-i-Azam University Bio-Ethical Committee with assigned protocol number BEC-FBS-QAU-103, the PIMS Hospital Ethical Review Board reference number 1-1/2105/ERB/ SZABMU also ap-proved the study.
Statistical analysis
The Data were analyzed through IBM SPSS Statistics version 22 (IBM, Armonk, NY, USA). Percentages and frequencies were determined for categorical and binary variables. Descriptive analysis and SSI cumulative incidence rates were calculated through different statistical techniques. The associations between variables were explored through the Pearson ϰ
2
test. A regression model was used for the association of SSIs with other factors. Simple linear regression was used to recognize the factors affecting and leading to the incidence of SSI. Multiple linear regression analysis was conducted to variables have the statistical significance of the univariate analysis to separate the factors (independent). For each predictor related to patients, surgery, and guidelines beta (standard error and
Results
Patients demographics
A total of 800 patients were registered for different surgical procedures, out of a total of 510 patients went through general surgeries, and finally, 412 patients were recruited on a purely informed consent basis (Schematic/Flow Chart 1). Overall,
Demographics of the participants and association with the incidence of SSI.
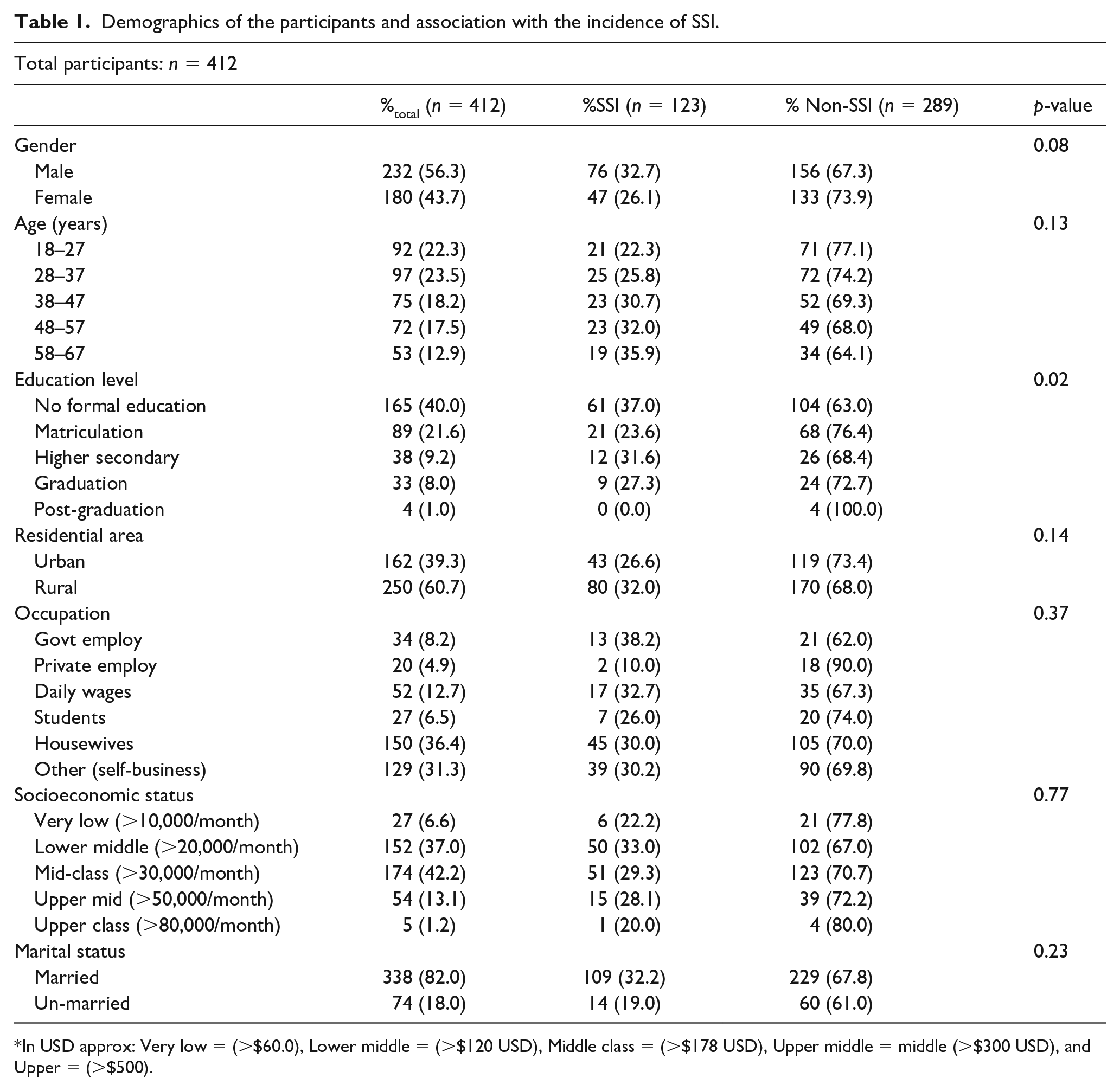
In USD approx: Very low = (>$60.0), Lower middle = (>$120 USD), Middle class = (>$178 USD), Upper middle = middle (>$300 USD), and Upper = (>$500).
Burden: Incidence of SSIs
Overall, out of 412 patients, 123 (29.85%) have developed SSIs and observed in seven different surgical procedures include; appendectomy (
Incidence of surgical site infections.

Associated risk factors
Patients related factors
Various patients related factors associated with SSIs were identified and are shown in Table 3. Elevated ranges of blood pressure and albumin level were significantly (95% CI:
Patients related factors association with surgical site infections.
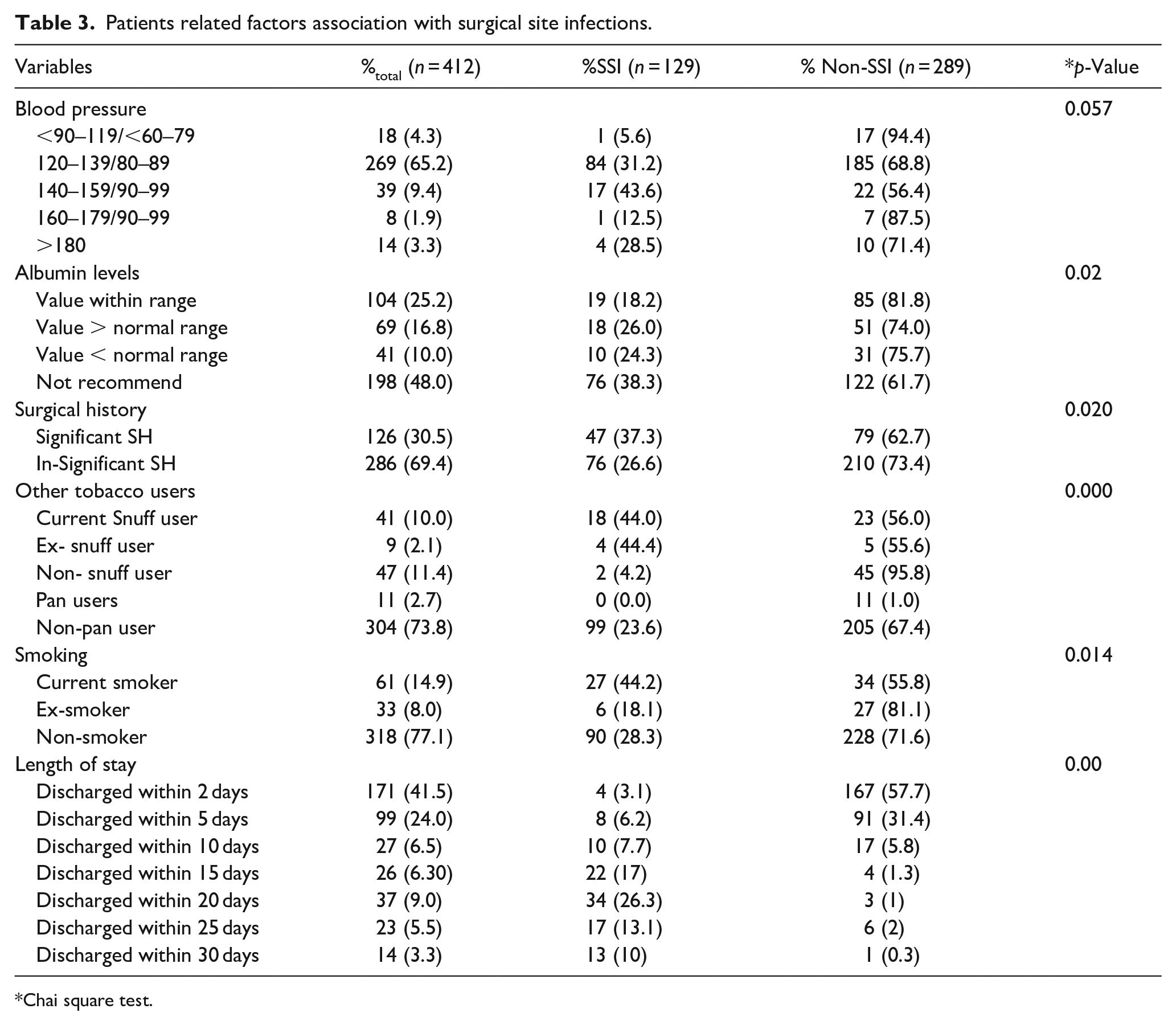
Chai square test.
Surgery-related factors
Surgical procedures were linked with the incidence of SSIs (
Association of surgery related factors with surgical site infections.

UB: urinary bladder related surgeries; PT: prostate related surgeries.
Hospital related factors
Length of stay at hospital (LOS)
Prolonged hospitalization is directly associated (
Hospital facilities for the individual patient
The hospital facilities provided to every single patient was observed in terms of poor, fair, good, and very good category. Various hospital facilities related factors found a significant association with the incidence of SSI. Ventilation, hygienic condition, bed dressing, diet plan, availability of waste bins, and biosafety signs (
Guidelines used and incidence of SSIs
Different guidelines were used which are still ignored at surgical wards and hospitals. The CDC guidelines were used for the classification of surgical wounds and observed significant results (
After adjusting contributory factors of SSI incidence, the univariate analysis consists; patient-related factors (BP, albumin level, surgical history, and length of stay), surgery-related factors (nature of the surgery, surgical procedures, length of surgical procedures), and related guidelines (KUNIN, MUST, CDC). Antibiotics prophylaxis included pre- and post-operative along with the total duration of antibiotics. The model fit statistics summary (
Model summary.

Model summary:
Antibiotics prescribed
Antibiotics were prescribed to the patients before (pre-operative), intra-operative (before 60 min of operation) and post-operative (after the completion of surgical procedures). Pre-operative antibiotics prescribed included cefoperazone and amikacin (
Overall, more than 83% did not receive antibiotics prophylaxis before the surgical procedure. Cefoperazone and sulbactam were the most prescribed antibiotics pre and post-operatively. The combination of cefoperazone and sulbactam along with amikacin was also used in pre and post-surgical patients. Prescribed antibiotics before and after the surgical procedures have differences (Table 6). No specific rational guidelines were in practice and the prescribed antibiotics were measured with the KUNIN criteria. Most patients received irrational and inappropriate therapy before and after surgery.
Antibiotics prescribed for surgical patients.

Causative agents
The culture sensitivity test was performed in only 79 infected patients (65 positive and 14 with negatives results) out of 123. Various causative agents were reported in positive cases and that was responsible for the development of SSIs. The most common pathogens involved in SSI were
Causative agents.

Discussion
The present study is the first of its kind to report the SSI rate in seven different surgical (emergency and elective) procedures in the largest tertiary care hospital in the capital of Pakistan. Multifactorial risk factors were associated with the incidence of SSI. Different strategies need to curb the incidence of SSI in Pakistani hospitals. The present results may relate to other LMICs. The overall incidence rate was found 29.85% in seven different general surgical (elective and emergency) procedures. The average rate of SSI (
Associated risk factors have the potential to increase the chance of SSI. Current research shows the risk factors have potential toward the incidence of SSI. Patients, surgery, and hospitals related factors were checked against the incidence of SSI and found significant results (
The Lancet Commission on Global Surgery projected that about 5 billion people lack access to safe and reasonable surgical care. 37 Worldwide burden of SSIs, the several gaps in evidence-based guidelines, and essential for a global approach, for the prevention of SSIs WHO decided to prioritize the development of evidence-based commendations. 13 Total 13 recommendations on preoperative preventive measures were presented and these guidelines take into account the benefits and harm balance, the evidence quality, patient values and preferences, cost, and resource use implications.13,14 Later on WHO presented 16 recommendations for SSIs prevention. 14 Appropriate surgical antibiotics prophylaxis (SAP) may reduce the risk of SSI but proper guidelines are needed to follow for the individual procedure. Recently, Khan et al., study reported the poor adherence to the pre-operative antibiotics guidelines and in another study by Khan et al., stated that the most common antibiotics cefuroxime and ceftriaxone were used inappropriately. 38 Our study also reported that no adherence to SAP was found during pre- and post-surgical prophylaxis. We also recommend educational interventions along with the implementation of AMS programs.39,40 The above authors also reported that approximately 89% of the patients who underwent surgical operations received antibiotics. 41 The same results were found in our study as only six patients didn’t receive antibiotics after surgery. The selection of a therapeutic agent, the timing, and the use of broad-spectrum antimicrobial were the common problems in the given setting.23,38,41
Besides the strength the given study has many limitations; firstly, the study has been taken in one tertiary care hospital so the findings may not generalizable to the whole country. The total period of the study and the sample size is not that much larger. The given study was conducted in general surgical wards only.
Global strategies and solutions are required as surgical infections constitute a worldwide problem. This consists of improving tools and techniques for source control, surveillance programs, and as well as antibiotic-stewardship, infection control, and practices of prevention to control AMR. 37 The combined efforts will lead to a decrease in the incidence of SSI.
Conclusion
To the best of the author’s knowledge, the current surveillance study is the first of its kind in Pakistan. The current research tried to show the reasons behind the occurrence of SSI events and gave an overall scenario of the SSIs. Associated risk factors and treatment outcomes have a direct association with the incidence of SSI. This is an alarming situation in Pakistan and still, no proper SSI reporting system with central databases exists. Evidence-based guidelines implementation at the hospital is the need of an hour. The hospital-based antimicrobial stewardship programs are need of the hour to curb SSIs. Moreover, further studies at the national level are required.
Supplemental Material
S1-Data_collection_form.miR – Supplemental material for Occurrence, associated risk factors, and treatment of surgical site infections in Pakistan
Supplemental material, S1-Data_collection_form.miR for Occurrence, associated risk factors, and treatment of surgical site infections in Pakistan by Faiz Ullah Khan, Yu Fang, Zakir Khan, Farman Ullah Khan, Zafar Iqbal Malik, Naveed Ahmed, Amir Hayat Khan and Asim.ur. Rehman in European Journal of Inflammation
Supplemental Material
S2-Patient-Related_Factors_MR – Supplemental material for Occurrence, associated risk factors, and treatment of surgical site infections in Pakistan
Supplemental material, S2-Patient-Related_Factors_MR for Occurrence, associated risk factors, and treatment of surgical site infections in Pakistan by Faiz Ullah Khan, Yu Fang, Zakir Khan, Farman Ullah Khan, Zafar Iqbal Malik, Naveed Ahmed, Amir Hayat Khan and Asim.ur. Rehman in European Journal of Inflammation
Supplemental Material
S3-Surgery-Related_Factors_miR – Supplemental material for Occurrence, associated risk factors, and treatment of surgical site infections in Pakistan
Supplemental material, S3-Surgery-Related_Factors_miR for Occurrence, associated risk factors, and treatment of surgical site infections in Pakistan by Faiz Ullah Khan, Yu Fang, Zakir Khan, Farman Ullah Khan, Zafar Iqbal Malik, Naveed Ahmed, Amir Hayat Khan and Asim.ur. Rehman in European Journal of Inflammation
Supplemental Material
S4-Related_Guidelines_miR – Supplemental material for Occurrence, associated risk factors, and treatment of surgical site infections in Pakistan
Supplemental material, S4-Related_Guidelines_miR for Occurrence, associated risk factors, and treatment of surgical site infections in Pakistan by Faiz Ullah Khan, Yu Fang, Zakir Khan, Farman Ullah Khan, Zafar Iqbal Malik, Naveed Ahmed, Amir Hayat Khan and Asim.ur. Rehman in European Journal of Inflammation
Footnotes
Acknowledgements
We (authors) highly appreciate the support of the given hospital, university, and all who helped us for the present research.
Authors contribution
Conceptualization, A.R. Data curation, F.U.K. Formal analysis, Z.K., F.U.K. Methodology, N.A., A.R. Project administration Z.I.M., A.R. Supervision, A.R. Writing validation, A.H.K. Review and editing, Y.F. The final manuscript read and approved by all authors.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Ethical approval for this study was obtained from the; Quaid-i-Azam University Bio-Ethical Committee has provided the ethical approval before the execution of the study and have assigned protocol number BEC-FBS-QAU-103, and PIMS (Pakistan Institute of Medical Sciences) Hospital Ethical Review Board granted ethical approval with reference number 1-1/2105/ERB/ SZABMU.
Informed consent
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
