Abstract
Objectives:
Type 2 diabetes mellitus (T2DM) is a persistent metabolic illness causing elevated glucose levels due to insulin resistance. Social media has been found to positively impact diabetes management by boosting motivation, adherence, emotional support, and sharing evidence-based information, thereby enhancing patients’ glycemic control efforts and achieving HbA1c targets. Primarily to examine the influence of social media within a random sample Iraqi population of T2DM patients on the control of diabetes, as measured by HbA1c levels.
Methods:
A multicentric cross-sectional study involves patients diagnosed with T2DM recruited between December 30, 2019 and November 8, 2023. Patients diagnosed with T2DM, who visited the outpatient clinic at least twice during the study period, were included. The sample size comprised 2921 patients. Various social media platforms available including, Facebook, WhatsApp, Instagram, Telegram, X (formerly known as Twitter), and Viber, were reported.
Results:
The study involves 2921 participants with a mean age of 53.3 years, 56% of them successfully reached their HbA1c target within a mean of 18.17 months. A significant correlation was found between achieving the target and using social media (P = .0001), with a shorter average duration among social media users compared to non-users. A family history of diabetes also significantly correlated with achieving the desired outcome, suggesting a probable positive correlation (P = .019).
Conclusion:
The study reveals a significant association between social media usage and glycemic control, introducing the importance of technology-based interventions in enhancing diabetes self-management, highlighting the relationships between social media engagement and HbA1c target achievement.
Plain Language Summary
This study looked at how using social media might help people with Type 2 Diabetes in Iraq manage their blood sugar levels better. The researchers found that there is a strong connection between using social media and better blood sugar control. This means that people who engage more with social media tend to manage their diabetes more effectively. The study suggests that social media and other technology-based tools could be important for helping people with diabetes take better care of their health. This is especially important for patients and those who support them, as it highlights a new way to improve diabetes management.
Background
Diabetes mellitus (DM) is a persistent illness of metabolism that is defined by an extended period of elevated glucose levels. Based on the findings of the 10th edition of the International Diabetes Federation (IDF) Diabetes Atlas, the global prevalence of diabetes has been consistently rising. Diabetes continues to pose a substantial challenge to the overall health and well-being of individuals worldwide. 1 According to the IDF Diabetes Atlas 10th edition, the number of individuals (aged 20-79) with diabetes in 2021 was expected to be 537 million. It is projected that this number would increase to 643 million by 2030 and 783 million by 2045.1 -3
Considering the worldwide prevalence of diabetes, it is important to note that this condition can lead to significant harm to many organs such as the heart, blood vessels, eyes, and kidneys. Consequently, diabetes continues to be a significant contributing factor to heart attacks, stroke, blindness, dementia, renal failure and even increased risk of multiple sclerosis.1,2,4 -6
Type 2 diabetes mellitus (T2DM) is characterized insulin resistance within body tissues and impaired production of insulin, which affects a large number of people globally. The primary objective in managing T2DM is to attain glycemic control, which is assessed by measuring the levels of glycosylated hemoglobin (HbA1c). 2 Although traditional healthcare interventions are important for managing diabetes, the emergence of social media has provided additional opportunities for patient involvement and assistance. 7
Realistically, social media plays a vital role in healthcare communication by enabling the exchange of information, providing peer support, and improving patient education for those diagnosed with (T2DM). These platforms, such as Facebook, Twitter, Instagram, and patient-specific forums, provide a digital space for immediate connection, overcoming geographical limitations and promoting a feeling of community among patients. Research has indicated that social media has a beneficial effect on the management of diabetes, as patients have reported heightened motivation, emotional assistance, and a sense of strength in their efforts to achieve glycemic control. Social media’s interactive nature facilitates the immediate spread of evidence-based information, equipping patients with the most recent developments in diabetes management. Furthermore, social media platforms offer a means for ongoing surveillance and input, enabling patients to monitor their blood glucose levels, physical activity, and dietary habits. This facilitates customized therapies and fosters cooperation between patients and healthcare providers.8 -10
Social media offers potential advantages in diabetes management, but it also poses challenges like privacy concerns, misinformation, and internet hostility. It’s essential to establish clear rules and verify information reliability to mitigate potential negative consequences. 11
Despite the growing body of literature on the use of social media for managing T2DM, limited research has focused on specific populations in developing regions. This study aims to fill this gap by exploring the impact of social media on attaining HbA1c targets among individuals with T2DM in Iraq. By focusing on this unique cultural and regional context, we contribute to the global understanding of the potential benefits and challenges of utilizing social media in diabetes management.
The study aims primarily to examine the influence of social media communication with doctors in random sample of T2DM patients within outpatient clinics from multiple centers on the control of diabetes mellitus, as measured by HbA1c levels. Further, the study explored whether the duration of contact with physicians through social media affected control status and the achievement of HbA1c targets.
Patients and Methods
Study design
A multicentric cross-sectional study included 2921 participants was carried out upon a randomly selected sample from the population of Iraqi population from multiple cities. The primary objective of this study was to examine whether using social media to communicate with doctors could affect the management of diabetes mellitus, with HbA1c levels being used as an indicator of control status. Two endocrinologists and two medical informatics professionals with a background in social network research had pilot-tested the questionnaire among 5% of total population before administration of the final version (Supplemental Figure 1). The study participants were recruited from multiple outpatient clinics between December 30, 2019 and November 8, 2023.
To facilitate participant engagement with healthcare providers, we employed a multi-faceted approach. Participants were encouraged to communicate with their healthcare providers through scheduled virtual consultations, asynchronous messaging via social media platforms, and periodic check-ins through dedicated diabetes management apps. These methods were designed to provide timely support while addressing the feasibility concerns of real-time direct access to physicians. Detailed instructions and schedules were provided to participants to optimize their engagement and ensure consistent follow-up.
Inclusion and exclusion criteria
The inclusion criteria were that any patient who had been diagnosed with type 2 diabetes mellitus and had made at least 2 visits to the clinic during the designated study period would be considered eligible for inclusion. Patients who did not meet these criteria were excluded.
Settings and data collection
A comprehensive approach was adopted to establish communication with the patients, utilizing various social media platforms prevalent in Iraqi society, including Facebook, Telegram, Instagram, WhatsApp, X (formerly known as Twitter), and Viber. Additionally, all patients were provided with their physician’s private phone number, facilitating easy and straightforward contact. The purpose of these communication channels was to provide patients with guidance on insulin use, dosage adjustments, injection methods, dietary control, and addressing any queries or consultations related to their condition.
Each patient underwent laboratory testing for HbA1c blood levels using the Bio-Rad HbA1c testing system. The cutoff for the target HbA1c level was set at 7.5% or less, in accordance with the recommendations of the American Diabetes Association (ADA). 12 Data collected for analysis included age, gender, HbA1c levels at each clinic visit, the status of contact through various communication methods, and the achievement of target HbA1c levels.
Statistical analysis
The statistical analyses were conducted using SPSS version 26.00. The Chi-square test was utilized to assess the attainment of HbA1c targets between those who utilized social media and those who did not. The examination of survival rate, represented by a Kaplan-Meier curve, was used to evaluate the duration needed to achieve the desired HbA1c levels. Descriptive statistics were used to summarize the attributes of the patients.
Ethical consideration
This observational study solely gathers clinical data through in clinic interviews. Prior to requesting a written informed consents from all the participants, participants were provided with a comprehensive description of the study’s objectives, methodologies, and significance. The names and identifying numbers of human subjects will be stored in a dedicated spreadsheet that will be secured with a password and available exclusively to investigators. Identification numbers will replace names and personal information in the data analysis process.
Results
Demographic characteristics
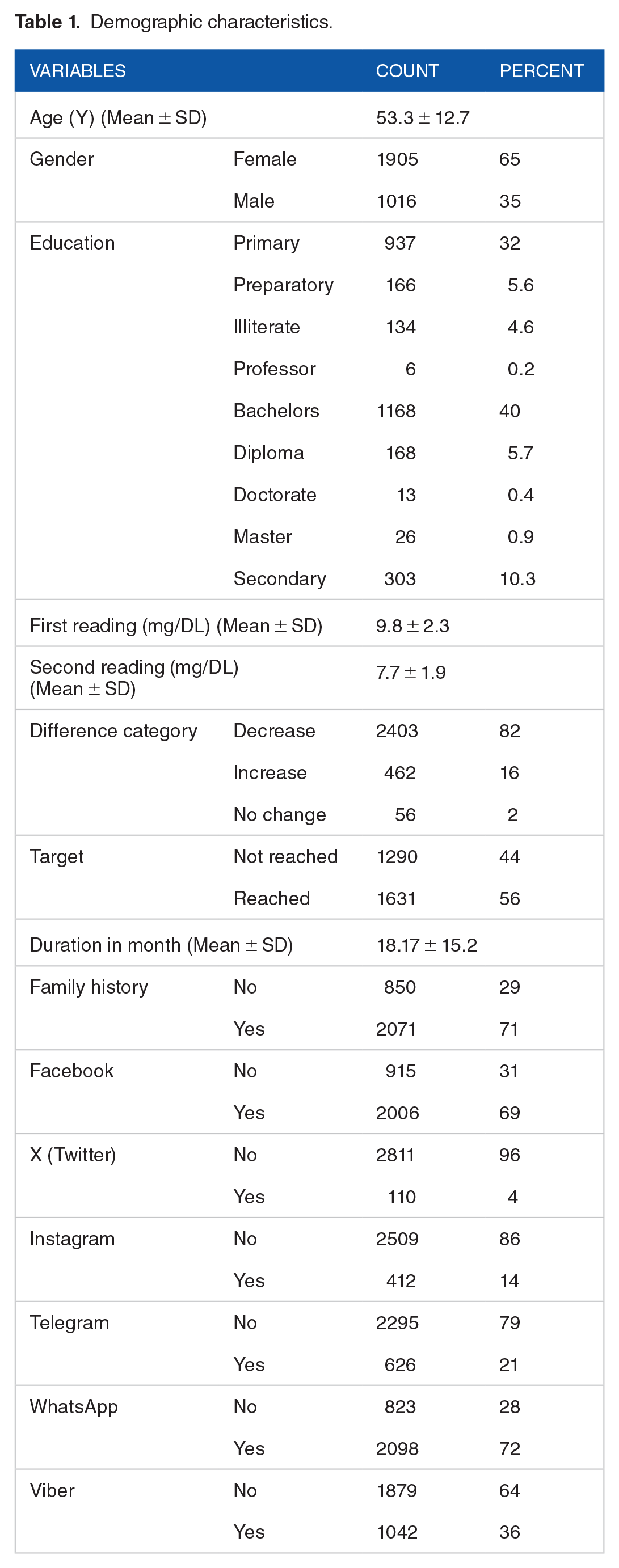
The majority of participants were females (65%) with a mean age of 53.3 years (SD = 12.7). Education levels were variable, with a significant portion holding bachelor’s degree (40%), followed by primary school degree (32%) while only a few subjects holding higher degrees. Blood glucose readings show a mean decrease from the first reading (9.8 mg/DL) to the second reading (7.7 mg/DL). A notable proportion of patients achieved their blood glucose target (56%), within an average duration of 18.17 (SD = 15.2) months. Moreover, WhatsApp was the most popular social media website among participants (72%), followed by Facebook (69%). Most of the patients (75%) spent about 3 hours on social media to follow their DM status.
The table outlines participants’ demographics, social media usage, family history, and the prevalence of reaching blood glucose targets (Table 1).
Demographic characteristics.
Association between achieving target HbA1c and social media
Among participants who don’t use social media, 761 individuals did not reach the target HbA1c, while 747 did. In contrast, regarding social media users, 529 only did not reach the target, and 884 did. Overall, the association between social media usage and target achievement is statistically significant (P = .0001) (Table 2).
Association between HbA1c target achievement and social media.

Social media users versus non-users: target HbA1c achievement duration
Individuals who failed to achieve the target HbA1c did not show a significant variation in the mean duration between those who use social media (17.29 months) and those who do not (18.42 months), as indicated by a non-significant P-value of .44. However, individuals who successfully reached the goal HbA1c had a noticeably shorter average duration (18.18 months) for social media users compared to those who did not use social media (18.56 months), with a P-value of .001. This suggests a probable connection between shorter duration for target attainment HbA1c for social media users (Table 3 and Figure 1).
Duration difference among the two study groups.

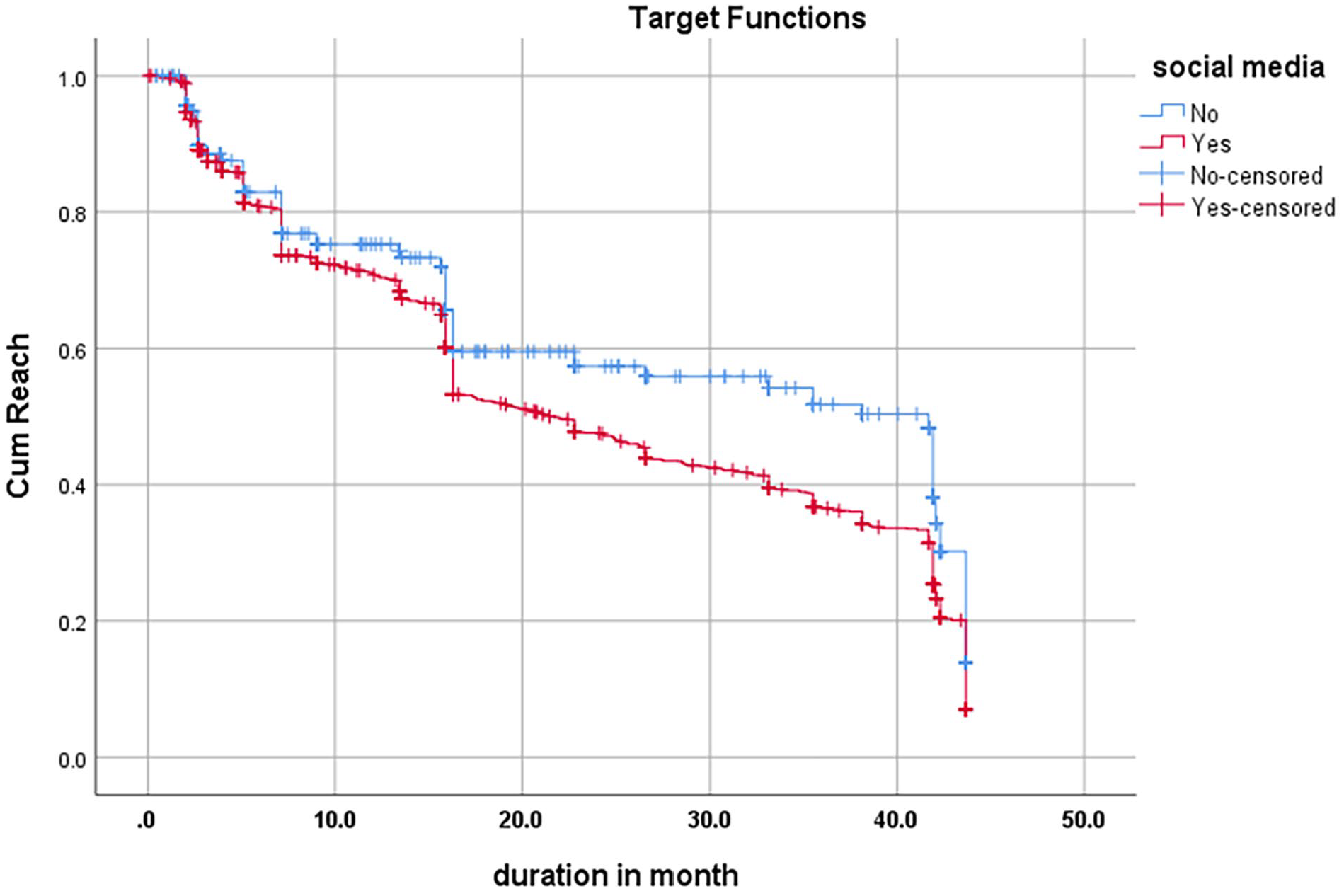
Kaplan Meir chart of duration needed to achieve HbA1c target.
Family History of DM as a predictor of Hb1Ac target achievement
Out of the individuals without any DM family history, 404 participants failed to reach the target, while 446 successfully reached target Hb1Ac. However, among the individuals with a positive family history, 886 individuals were unable to reach the target, while 1185 individuals were able to reach it. This suggests a strong correlation between having a family history and the probability of achieving target Hb1Ac. A P-value of .019 indicates a significant association (Table 4).
Relation between target achievement and DM family history.

We collected data on the frequency and nature of patient-provider communications. Participants who engaged in high-frequency communications (at least once per week) with their providers showed significantly greater reductions in HbA1c levels compared to those with less frequent interactions (P < .05). The types of communication included virtual consultations (45%), asynchronous messaging (35%), and periodic check-ins (20%). These findings underscore the importance of sustained and frequent engagement in achieving better diabetes management outcomes.
Comparison of social media users and non-users
Our analysis revealed that while social media users demonstrated significant reductions in HbA1c levels, a notable proportion of non-social media users also met their target HbA1c levels. Specifically, 55% of social media users achieved their HbA1c targets compared to 50% of non-social media users. This suggests that while social media usage contributes positively, other factors such as regular medical follow-ups, lifestyle modifications, and robust support systems are also critical in managing T2DM effectively. These findings highlight the multifaceted nature of diabetes management and the need for integrated approaches.
Discussion
This multicentric cross-sectional study found that the investigated a population of T2DM patients of Iraqi population which was mostly comprised of females (65%) with a mean age of 53.3 years. Additionally, a significant proportion of the population had variable educational levels, while only 4.6% being illiterate. The blood glucose readings were analyzed twice and showed a decrease in the mean value from the first to the second measurement. Moreover, 56% of the group successfully reached their Hb1Ac target within an average time period of 18.17 months. A significant correlation was found between achieving the HbA1c target and using social media, with a statistically significant P-value of .0001. Furthermore, social media users who achieved HbA1c had a shorter average duration compared to those who did not use social media, revealing a significant correlation between a shorter average duration and target attainment, but exclusively among social media users (P = .001). While a family history of diabetes significantly correlated with achieving the desired outcome, indicating a probable link between familial propensity and the likelihood of reaching the state of control (P = .019).
The role of social media as a tool in diabetes management is considered a new trend in the middle east region and especially within Arabic countries. Despite the widespread use of social media among population in these regions, there is a lack of research on its use among individuals with diabetes, apart from few studies13,14 Thus, there is a significant gap in understanding the effectiveness of these platforms.
According to our findings, WhatsApp, Facebook, and viber are the top social networks for the diabetic population in Iraq. The primary factors driving patients’ preference toward WhatsApp and Facebook in our population, include widespread access to these platforms among Iraqis, convenient access to healthcare information, enhanced comprehension facilitated by audio and video features. Notably, 2 previous studies conducted by Sap et al 15 and Kamel Boulos et al 16 revealed that the majority of patients used Instagram and WhatsApp to receive health guidance regarding their DM illnesses. Further, online diabetes education, intervention, and support are commonly sought by young people using major social network platforms such as Facebook, Twitter, WhatsApp, Instagram, and Skype as Petrovski and Zivkovic 17 reported in their research.
The main outcome of our study goes in parallel with Chen et al 18 meta-analysis, which included 25 randomized clinical trials (RCTs) containing 2838 Chinese patients. This meta-analysis indicates that patient education provided through social media groups, either alone or in combination with face-to-face sessions, led to substantial improvements in DM management. This was shown through enhanced control of fasting blood sugar levels (FBS), postprandial blood glucose levels after 2 hours (2h-PBG), and levels of HbA1c. Additionally, our findings are similar to those presented in a 2014 meta-analysis by Toma et al 19 that involving individuals with T2DM. This could be explained b the facts that social media platforms facilitated educational experiences through improving participants’ understanding of diabetic self-management regimens and motivation to follow self-care guidelines by providing frequent prompts on educational material and medication adherence, compared to traditional in-person experiences. Further, social media users also had the opportunity to openly inquire with their physicians regarding any daily updates of the disease.
Considering HbA1c as the major predictor of diabetes control, improvements in HbA1c levels were found among T2DM patients receiving health education through private groups on Facebook and special diabetic networks compared with non-social media patients in the control group.17,20
Another systemic review and meta-analysis by Kong and Cho 21 shed the light on the importance of continuous blood glucose monitoring (CGM) and frequent follow-up including 17 RCTs, which revealed that CGM led to a reduction in HbA1c levels within various centers when during a period of more than 24 weeks.
In the other hand, a meta-analysis conducted by Mita et al 22 specifically studying patients with noncommunicable illnesses found no obvious benefits associated with the usage of social media. However, there are numerous other studies that have identified some positive impacts among those affected by chronic diseases.23 -25
The significant association between family history and HbA1c target achievement reinforces the role of genetic factors in diabetes outcomes. 26 While our findings align with existing literature, the unexpected prevalence of target achievement among individuals with no family history challenges conventional expectations. 27 This prompts a reevaluation of the complex interplay between genetic and environmental factors and underscores the need for comprehensive assessments in clinical practice. In developing countries where telemedicine is either underdeveloped or unavailable, social media serves as an effective alternative for maintaining patient follow-up and engagement with healthcare providers.
While our study demonstrates the positive impact of social media on diabetes management, the feasibility of direct, real-time access to physicians is limited by practical constraints such as time and patient load. To address these concerns, we propose alternative models, including the utilization of diabetes educators and trained healthcare professionals who can provide timely responses and support. This approach not only alleviates the burden on physicians but also ensures sustained patient engagement.
Recommendations and Limitations
We suggest acknowledging social media as an emerging helpful tool to improve patient compliance and adherence to follow-up appointments and medical directions. Additionally, it is recommended to promote patients to continue extended communication and updates with their physicians via social media platforms. While, in order to improve the research quality about diabetes management and social media platforms, we recommend increasing the sample size and establishing a defined study duration in order to collect more thorough and accurate data. Future research should also explore tailored social media interventions that consider individual patient needs and preferences. Additionally, longitudinal studies are necessary to assess the long-term sustainability and impact of these interventions. Clinically, the incorporation of social media tools should be complemented by robust follow-up systems and lifestyle modification programs to optimize diabetes management. One of the limitations of this study is we did not calculate Mean HBA1c level, duration of Diabetes and prevalence of complications in study population as these may possible confounding factors that affect in achieving target HBA1c. Also, we did not calculate the percentage of patients who may have provided false or incorrect information on social media to manage their T2DM, as they will not answer it properly. The power analysis for sample size calculation was not done because we do not have a population frame to depend on and it is one of our limitations as well. Although, the questionnaire was pilot tested for validity among 5% of population before administration.
Conclusion
Our study provides valuable insights into important aspects of diabetes care, revealing complex interactions between social media use and glycemic control. The strong correlation between the use of social media and the accomplishment of HbA1c targets presents a new opportunity for intervention techniques, highlighting the effectiveness of technology-based methods in improving diabetes self-care. Nevertheless, the subtle connections revealed, particularly in relation to the length of time spent on social media, require thoughtful deliberation in order to create tailored solutions. The surprising frequency of target attainment in people without a familial background challenges traditional assumption and necessitates a more comprehensive comprehension of the interaction between hereditary and environmental influences. These consequences highlight the ever-changing nature of diabetes research and underline the significance of tailored, evidence-based therapies to maximize glycemic control in various groups.
Supplemental Material
sj-jpeg-1-end-10.1177_11795514241293346 – Supplemental material for Exploring the Impact of Social Media on Attaining HbA1c Targets in Individuals with Type 2 Diabetes Mellitus in Iraq: A Cross-Sectional Study
Supplemental material, sj-jpeg-1-end-10.1177_11795514241293346 for Exploring the Impact of Social Media on Attaining HbA1c Targets in Individuals with Type 2 Diabetes Mellitus in Iraq: A Cross-Sectional Study by Jabbar J. Atia, Ahmed Dheyaa Al-Obaidi, Ahmed Sermed Al Sakini, Yousif Ali Al-Saady, Assalah Othman, Hashim Talib Hashim, Mustafa Najah Al-Obaidi, Hasan Al-Obaidi and Nooraldin Merza in Clinical Medicine Insights: Endocrinology and Diabetes
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
