Abstract
Introduction:
Human papillomavirus (HPV)-positive and HPV-negative oropharyngeal squamous cell carcinomas (OPSCCs) are 2 distinct cancers, with HPV-positivity conferring a better prognosis. Smoking status is a complicating factor for both patient populations. There have been scattered literature that have reported on incomplete information regarding the profiles of their patient population. Details including age and sex distributions, TNM staging, histology grading, recurrence time and types, death rates, and the direct causes of deaths have been reported incompletely in the literature. Here, based on the experience at our university medical centers, we explored all the details of the important clinical profiles of HPV-negative OPSCC, HPV-positive OPSCC in smokers and nonsmokers.
Objective:
In this article, we compare detailed clinical profiles of HPV-negative OPSCC and HPV-positive OPSCC in both smokers and nonsmokers. The clinical profiles we elucidated here include patients’ age and sex distribution, general health conditions, histology grading, TNM staging, perineural invasion (PNI), and lymphovascular invasion (LVI), extracapsular extension (ECE), recurrence rate and types, death rate, and direct causes. Specifically, we divided HPV-positive OPSCC into smokers and nonsmokers and compared the different clinical profiles between these groups to give a better idea of the complicating role of smoking in the development of HPV-positive OPSCC.
Method:
All patients with OPSCC at a tertiary care publicly funded county hospital and a tertiary care university hospital from June 2009-July 2015 were retrospectively reviewed. The attending physicians were the same at both hospitals. The primary outcome measure was posttreatment 2-year follow-up status (locoregional recurrence, distant recurrence, death rate). Other measures included HPV status based on p16 staining, smoking history, age, sex, comorbidities, tumor size, nodal and distant metastasis information, LVI, PNI, ECE, and tumor histology grade.
Results:
A total of 202 patients with OPSCC were identified. They were categorized into 3 groups: HPV-negative OPSCC group (HPV−), HPV-positive smoker group (HPV+SMK+), and HPV-positive nonsmoker group (HPV+SMK−). Patients of HPV− group are older (61.1 ± 11.6 years) than the other groups on average. The HPV− group has the highest percentage of women (22.7%). The HPV− patients with OPSCC have more comorbidities than the HPV+SMK+ group and the HPV+SMK− group, although there is no statistical difference. Grade 2 tumor is the most common histology grade for HPV− patients with OPSCC, whereas grade 3 is the most common grade for HPV+SMK+ and HPV+SMK− groups. Both PNI and LVI are positive at around 40% for all groups without any significant difference, but ECE is very common for HPV− OPSCC, at 86.7%, which is significantly higher than that of the HPV+SMK+ and HPV+SMK− groups. There was no difference of bilateral neck metastases noticed among different groups. For T staging and N staging, although HPV+SMK− and HPV+SMK+ patients have relatively lower T stages and higher N stages, there is no significant difference. HPV+SMK− group has highest TNM stages. All death rates and recurrence rates increase with time, but the death rate of HPV− group is about 4 times higher than that of the HPV+SMK+ group and 6 times higher than that of the HPV+SMK+ group. The major recurrence type of HPV− OPSCC and HPV+SMK+ is locoregional, and the major recurrence type of HPV+SMK+ is distant metastasis.
Conclusions:
Our data confirmed that HPV+ OPSCC normally presents with more advanced stage, however, it has better prognosis. In comparison, HPV− OPSCC presents at an earlier stage, but the prognosis is worse. Based on their clinical profiles, we noted that HPV-positive OPSCC cells are more “mobile”; they metastasize sooner and further. However, HPV-negative OPSCC cells are more locally infiltrative, leading to more locoregional recurrence. The HPV-positive patients usually are younger and healthier at diagnosis. Although HPV-positive OPSCC tend to be histologically higher grades, there was no statistical difference noticed. Metastatic and recurrent patterns are very different between HPV-positive and HPV-negative patients, but the death rate of HPV-negative patients is way higher, and it is mainly due to locoregional recurrences, which is the major recurrence type for HPV-negative patients. Of our note, smoking is a complicating factor for HPV-positive OPSCC, and it makes the death rate, recurrence rate, histology grade, and TNM staging shift toward HPV-negative OPSCC. How smoking makes HPV-positive OPSCC behave more like OPSCC-negative OPSCC deserves more translational research for further elucidation.
Keywords
Introduction
Over the past few decades, a significant amount of research has confirmed that human papillomavirus (HPV)-positive (HPV+) and HPV-negative (HPV−) oropharyngeal squamous cell carcinoma (OPSCC) are 2 distinct clinical entities.1,2 In addition, literature has shown a rising incidence of HPV+ OPSCC.3,4 Patients with either type of OPSCC can be stratified into smokers and nonsmokers, which further complicates prognosis and treatment algorithms. HPV+ disease is more susceptible to radiation therapy and, in general, portends a more favorable outcome. 5 However, HPV+ patients with OPSCC who smoke have less favorable outcomes than HPV+ nonsmokers. 6 Abstention from smoking in patients with HPV+ OPSCC is associated with lower mortality, better functional outcomes, and higher response to initial chemoradiation. 7
HPV+ OPSCC is identified by testing the tumor specimen for the p16 protein tumor marker. 8 The neoplastic processes leading to these tumors include the dysregulation of the cell cycle by the HPV viral E6 and E7 proteins and impairment of DNA repair mechanisms by viral proteins E2 and E3. 9 Viral proteins E6 and E7 are implicated in the disruption of p53 and retinoblastoma (RB) tumor suppressor gene pathways. 10 As HPV+ tumors have profound proliferative effects from direct modification of Rb and p53, these tumors often do not require other mutations for oncogenesis. This is in comparison with HPV− tumors, which often have many oncogenic mutations working in concert, including TP53, NOTCH, PIK3CA, cyclin D1, and CDKN2A.11,12
In addition to pathologic differences, HPV+ and HPV− tumors differ in terms of natural history and treatment response. Compared with HPV− tumors, HPV+ disease tends to have better overall survival rate, longer progression-free survival, better disease control with primary surgery only, lower rates of metastasis on presentation, and higher response rates to radiation therapy.11,13,14 This extensive body of literature has resulted in HPV+ OPSCC being treated as a distinct clinical entity, including different options for treatment algorithms.
A current area of new research in HPV+ OPSCC is the exploration and employment of de-escalating treatment algorithms.15,16 Several avenues are being pursued to this end.17,18 An important fact to come out of many of these studies is that there is a distinct population of nonresponders, sometimes up to 20% of the study population. Identifying these populations of nonresponders will be essential for the creation of safe, highly efficacious de-escalation algorithms. One of the complicating factors is smoking, which is present in some HPV+ patients with OPSCC. There has been scattered evidence reporting incomplete information regarding the profiles of patient populations, especially HPV+ smoking patients. Details including age, sex, TNM staging, histology grading, recurrence time and types, death rates and the direct causes of deaths have been reported incompletely in the literature. Here, based on our experience at the University of Southern California, which includes a large public hospital and a large private hospital, we explored all the details regarding the important clinicopathological profiles of HPV− OPSCC and HPV+ OPSCC in smokers and nonsmokers. The aim of this study is to better understand and provide more details regarding the clinical profile of smoking HPV+ patients with OPSCC, who comprise most of the HPV+ patient population. This information will be used to develop pathways toward further management of OPSCC and individualized patient care.
Methods
The patients with OPSCC diagnosed and treated at the University of Southern California hospitals between June 2009 and July 2015 were identified with CPT (Current Procedural Terminology) codes from our electronic medical record system. Their clinicopathological information was retrospectively analyzed. The primary clinical parameters evaluated were smoking history, HPV status, pathologic characteristics of the primary tumors, locoregional recurrence, distant recurrence, and survival rate as evaluated at the 2-year posttreatment visit. Tumor grade was determined on surgical pathology reports per the guidelines of the American College of Pathologists. The HPV status was based on p16 staining rather than presence of HPV DNA, as it is the standard practice at our institution. Charlson Comorbidity Index (CCI) scores were used to ascertain the overall health of patients. Secondary information identified included patient age, sex, race, and comorbidities. These data were collected mainly by reviewing the electronic medical records, but phone calls to patients were used to obtain any supplementary information. Recurrence and survival rates were calculated by following up on patients either through electronic records or direct phone calls for a total of 24 months. All patients were observed clinically for recurrence with supplementary imaging as needed.
For statistic studies, all numerical data such as patient ages and CCI were analyzed using t test. Categorical data such as lymphovascular invasion (LVI), perineural invasion (PNI), extracapsular extension (ECE), TNM staging, and sex distribution were analyzed with χ2 test or Fisher exact test, depending on the number of patients in each category. All the tests were 2-sided and results were considered significant for P values less than .05. SAS 9.1 was used for major statistical calculations (SAS Institute Inc., Cary, NC, USA).
Results
Patient population
A total of 202 patients with OPSCC were identified through retrospective chart review. Based on their p16 staining status, 45 patients were HPV-negative and the rest were HPV-positive. Among HPV-positive patients, 91 were identified as either current or previous smokers and 61 patients denied any smoking history. All patients’ treatment plans were discussed at a multidisciplinary tumor board and developed in accordance with National Comprehensive Cancer Network guidelines. The age, ethnicity, HPV status, and smoking history of patients are summarized in Table 1. Based on their HPV status and smoking history, patients were divided into 3 groups including HPV-negative OPSCC (HPV−), HPV-positive smokers (HPV+SMK+), and HPV-positive nonsmokers (HPV+SMK−).
Demographic summary of patient population.

Abbreviation: CCI, Charlson Comorbidity Index.
Data include average age, sex distribution, CCI, and ethnicity. Smoking distribution is the proportion of current to former tobacco use among patients designated as “smokers.”
Age distribution
The average age was 61.1 ± 11.6 years for the HPV− group, 56.2 ± 7.7 years for the HPV+SMK− group, and 56.6 ± 7.9 years for the HPV+SMK+ group. There is a statistical difference in age between the HPV− group and the HPV+ group (including both HPV+SMK− and HPV+SMK+), as indicated in Figure 1 (P < .05). However, there was no difference in age between the HPV+SMK+ and the HPV+SMK− groups, as indicated in Table 1 (P > .05).
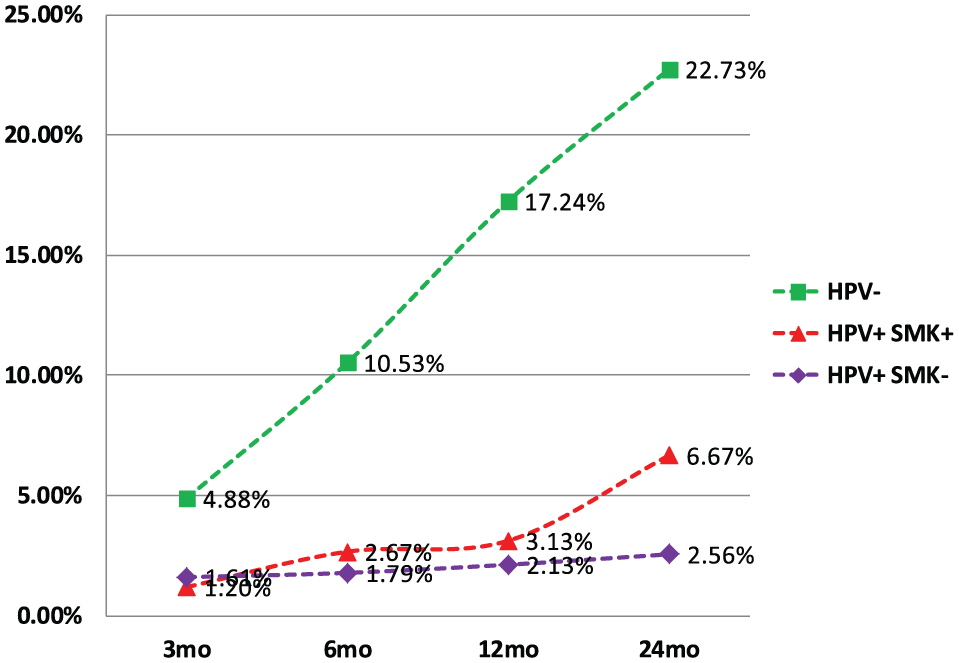
Trends of death rates of different groups with time (in months, mo). The horizontal axis shows the sampling intervals after initial diagnosis. HPV+SMK+ group had slow increase initially but it had a sudden and steep uptrend after 1 year, which is concerning, especially considering the uptrend is parallel to the curve of the HPV− group.
Sex distribution
Among the HPV− group, female patients accounted for 22.7% of the group population. However, female patients merely comprised 6.6% of the HPV+SMK+ group and 16.7% of the HPV+SMK− group. The only statistical difference in sex distribution was identified between the HPV− group and the HPV+SMK+ group, as shown in Table 1 (P < .05), indicating that the HPV− group may have a higher percentage of female patients.
Charlson Comorbidity Index
The CCI was calculated based on the comorbidities of each patient. The CCI is a quantified index for a patient’s general health. From our analysis, the HPV− patients had the highest average CCI (2.24 ± 1.43), whereas the HPV+SMK− group had the lowest average CCI (1.47 ± 1.23). The CCI score of the HPV+SMK+ fell in between at 2 ± 1.74. The results are shown in Table 1 (P > .05).
Tumor histology grade
The HPV− group had moderately differentiated tumor (grade 2) as their most common type (51.1%), followed by poorly differentiated squamous cell carcinoma (grade 3, 42.2%). Both HPV+SMK+ and HPV+SMK− groups had grade 3 as their most common histology grade (54.3% and 52.5%). Grade 2 tumor was the second most common grade for both at 43.2% and 45.9%, respectively. The results are shown in Table 2 (P > .05).
Summary of tumor characteristics and histopathology for HPV−, HPV+SMK+, and HPV+SMK− groups.
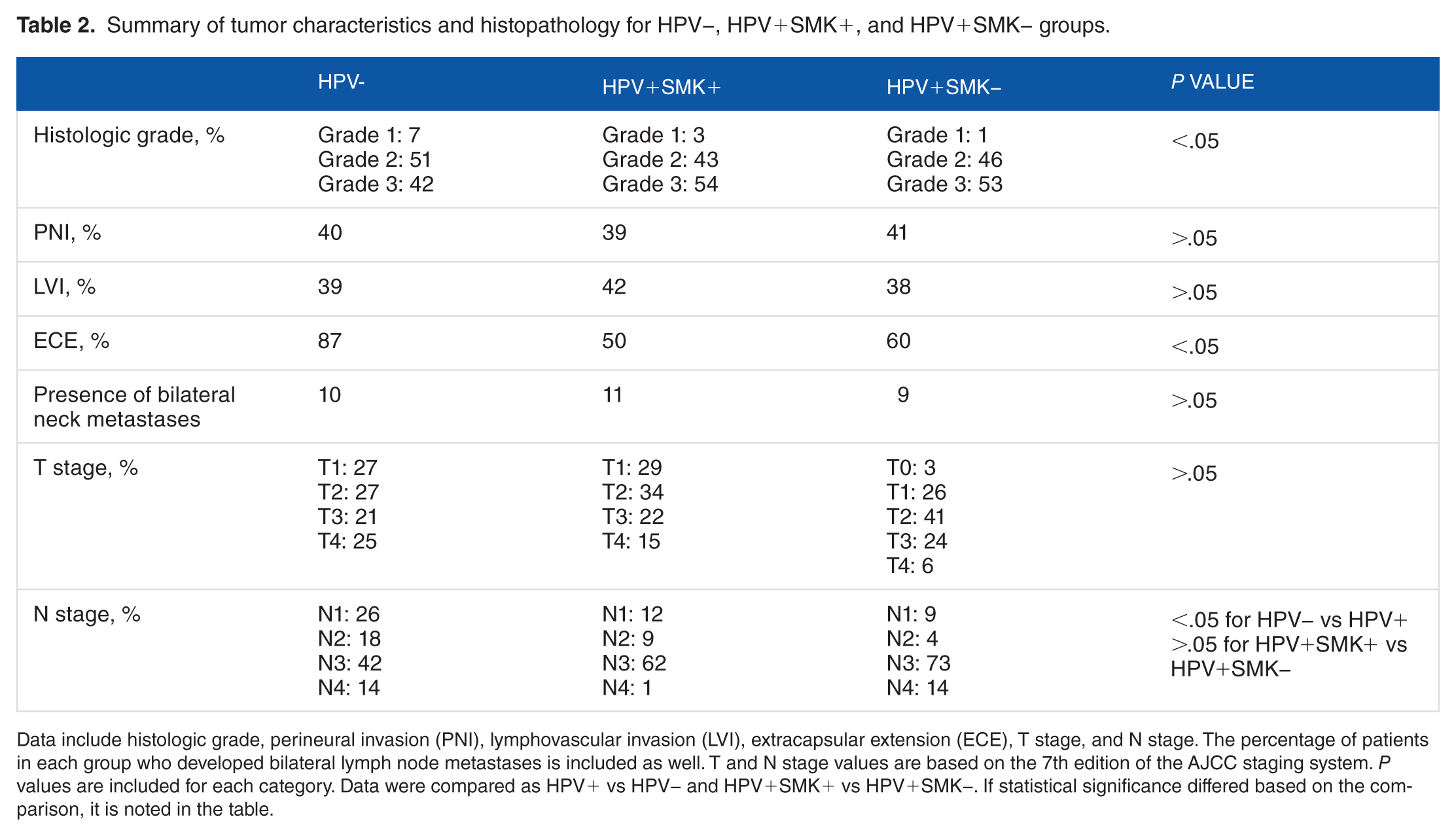
Data include histologic grade, perineural invasion (PNI), lymphovascular invasion (LVI), extracapsular extension (ECE), T stage, and N stage. The percentage of patients in each group who developed bilateral lymph node metastases is included as well. T and N stage values are based on the 7th edition of the AJCC staging system. P values are included for each category. Data were compared as HPV+ vs HPV− and HPV+SMK+ vs HPV+SMK−. If statistical significance differed based on the comparison, it is noted in the table.
PNI and lymphovascular invasion
About 40% of HPV− cancers had positive PNI on histology. The HPV+SMK+ group had 38.9% positive PNI, whereas the HPV+SMK− group had 40.9%, as shown in Table 2. Statistical analysis did not indicate any significant difference among these groups (all P > .05) regarding PNI. For LVI, 39.1% of the HPV− cancers were positive on histology. The HPV+SMK+ group had LVI at a rate of 41.8%, compared with 39.3% for the HPV+SMK− group. Similarly, there was no statistical difference among them (P > .05) as shown in Table 2.
Extracapsular extension
Extracapsular extension was found to be positive in 86.7% of the HPV− patients, 50% of the HPV+SMK+ group, and 60% of the HPV+SMK− patients. There was statistical difference between the HPV− and the HPV+SMK+ groups (P < .05) and between the HPV− and HPV+SMK− groups (P < .05). There was no statistical difference between the HPV+SMK+ group and the HPV+SMK− group (P > .05). The results are shown in Table 2.
Bilateral neck metastases
Based on radiologic and pathologic evidence, bilateral neck metastases were found in 10.3% HPV− patients, 10.99% of HPV+SMK+ patients, and 9.38% of HPV+SMK− patients. There was no statistical difference among them (P > .05). The results are shown in Table 2.
TNM staging (based on the AJCC 7th edition, 2010)
Based on the primary tumor size, T2 was the most common T staging for all groups. It was most common in the HPV+SMK− group (41.0%), and least common in the HPV− group (27.3%), as shown in Table 2. Of note, HPV− patients had the highest percentage of T4 tumors (25.0%), whereas HPV+SMK− tumors had the lowest rate of T4 staging (6.10%). There was no statistical difference when they were compared (P > .05).
Regarding N staging, N2 was the most common N stage for all groups. N stages were divided into early (N0-N1) and late (N2-N3). The late N stages were more common in HPV+ patients, regardless of their smoking status. Early N stages were more common in the HPV− group, and there is statistical difference between HPV− and HPV+ groups (both P < .05). However, there is no difference between the HPV+SMK+ and the HPV+SMK− groups (P > .05). The results are shown in Table 2.
Death rate
All groups had slowly increasing death rates with time. However, the increase was most pronounced in the HPV− group, doubling the baseline rate of 4.88% approximately every 6 months, reaching 22.73% at 24 months after diagnosis. The uptrending death rates of the HPV+ patients were not significant with HPV+SMK+ patients having higher death rates than that of the HPV+SMK−, as shown in Figure 1.
Recurrence rate and recurrence type
The recurrence rate, including both locoregional and distant recurrences, steadily increased during 2 years of follow-up for all groups. The recurrence rate of the HPV− patients was highest at 51.85% at 24 months after diagnosis. The rates of the HPV+ groups tracked somewhat lower rate of 37.04% and 21.43% for the HPV+SMK+ and HPV+SMK− groups, respectively. The results are shown in Figure 2.
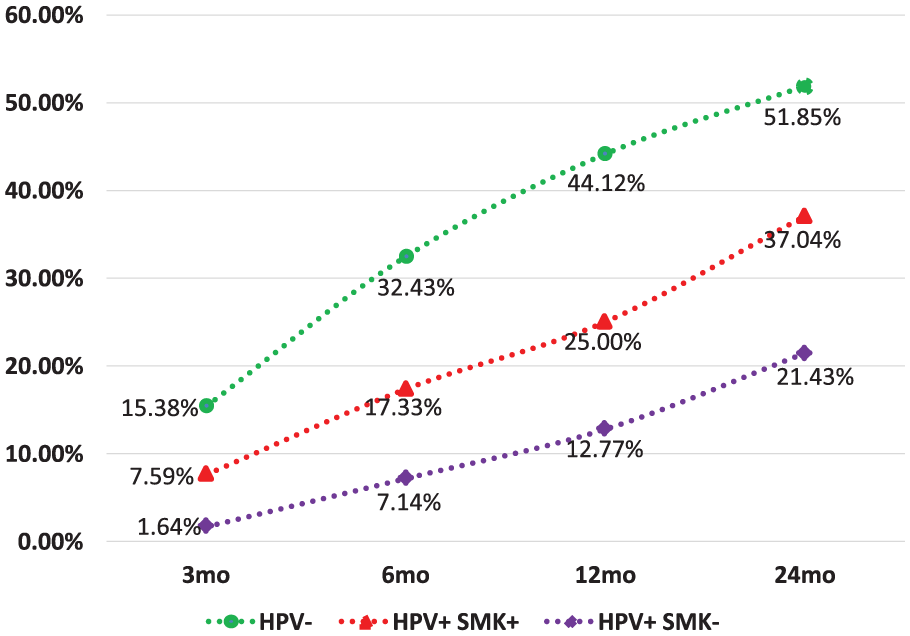
Trends of recurrence rate, including both locoregional and distant recurrences, of different groups with time (in months, mo). The horizontal axis shows the sampling intervals after the initial diagnosis.
Of note, the major type of recurrence observed in HPV− patients was locoregional (79%), which was also the leading cause of death for this group. However, the main type of recurrence seen in the HPV+SMK− group was distant metastasis (78%). The recurrence profile of HPV+SMK+ was similar to that of the HPV− group, with 70% of the recurrences being locoregional, as shown in Figure 3.
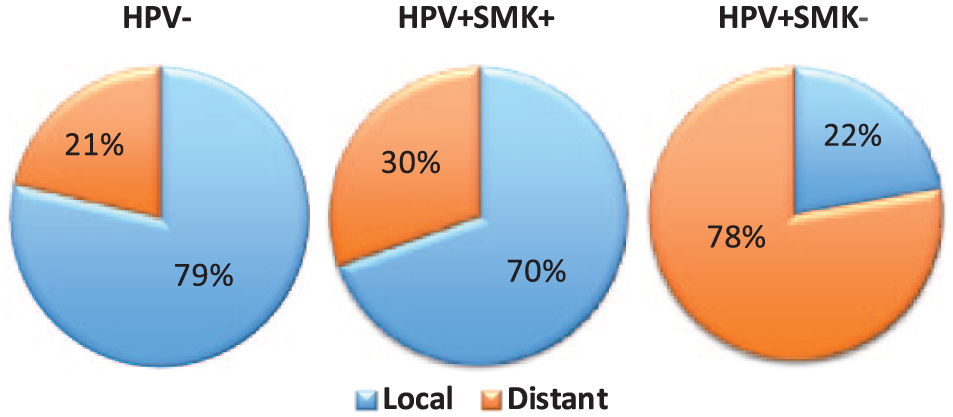
The recurrence types (locoregional recurrence, in blue; distant metastasis, in orange) of oropharyngeal squamous cell carcinoma in different groups. The pie graphs show only the relative portions of each recurrence type in each patient group, it does not represent the total recurrence rate for each group. Our data showed that HPV− had the highest recurrence rate. Of note, HPV+SMK+ group has similar recurrent pattern as the HPV− group.
Discussion
The HPV status has been shown to be a significant variable in the natural history of OPSCC. Differentiating between HPV-positive and HPV-negative OPSCCs would aid in the development of more accurate prognostic models as well as de-escalation strategies for these 2 distinct patient populations. De-escalation can be implanted in various ways, including the employment of alternative chemotherapeutic agents or the use of less aggressive chemoradiation protocols. We have analyzed our experience treating OPSCC at the University of Southern California, and to our surprise, most of the HPV+ patients were current or former smokers, which made further management more complicated. It is a challenge to stage and plan the therapy for HPV+ smokers with OPSCC as the clinicopathological characteristics of their tumors are shifted toward HPV− cancers, as shown by our data.
Multiple large database studies have shown that patients with HPV+ OPSCC tend to present at younger ages compared with HPV− patients.19,20 In our patient population, HPV+ patients also presented at younger ages with fewer comorbidities; however, the age difference was not as significant as reported. Our data show that HPV+ OPSCC occurs less frequently to female patients, especially female nonsmokers, which is consistent with a recent report. 3 Given the current trend of therapy de-escalation for HPV+ OPSCC and the younger age of patients, smoking history should be considered before implementation of treatment as there is a risk of therapeutic inadequacy for smokers with HPV+ OPSCC, which will potentially result in increased rates of treatment resistance and residual disease. This initial concern was the major purpose of this research report.
In addition, our data show that HPV+ patients presented with higher grade tumors, less T4 tumors, higher N staging, and more advanced TNM stages than the HPV− patients. Such data are consistent with prior reports. 21 Although HPV+ OPSCC normally presents at advanced stages, the death rate is significantly lower, as shown in our data. Our results indicate that smoking history shifted the death rate of HPV+ patients toward that of the HPV− patients, although overall rates remained lower in the HPV+ smoker group. Smoking also increased the rate of ECE for HPV+ tumors but it had very limited effect on the prevalence of PNI and LVI. Our staging system used here was based on the 7th edition of AJCC staging guidelines. The 8th edition staging system expends the criteria for HPV+ OPSCC, which basically downstages most HPV+ OPSCC. Our data show that, according to the 7th edition, the prevalence of PNI, LVI, and ECE for HPV+ OPSCC was not significantly lower than that of HPV− OPSCC, which is concerning when we follow the 8th edition AJCC staging system, especially for HPV+ smoking patients.
The most significant effect of smoking on the clinicopathological characteristics of HPV+ OPSCC was the significant increase in death and locoregional recurrence rates among HPV+ smokers. The effect of smoking on PNI and LVI was not obvious. The presence of smoking reduces the difference between histologic grade and TNM staging of HPV+ and HPV− OPSCC. This study is not without limitations. Given the inherent variability in age and sex among HPV+ and HPV− patients, it is difficult to equalize baseline features in the groups prior to comparison of tumor characteristics and clinical outcomes. Therefore, it is possible that baseline features may have served to confound results. Retrospective analysis is also limited in that it cannot determine causality. The specific mechanism by which smoking makes HPV-positive OPSCC behave more like HPV-negative OPSCC deserves more translational research for further elucidation.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
CL: Study design, data collection, data analysis, manuscript drafting; GT: Data analysis, manuscript drafting; GML: Manuscript drafting; TVW: Data collection and analysis; DSM: Data collection and analysis; UKS: Study design, data analysis and interpretation; NCK: Study design, data analysis and interpretation, principal investigator.
