Abstract
Aim and objective:
This systematic review and meta-analysis was conducted to assess the prevalence, burden and epidemiology of methicillin-resistant
Methodology:
Electronic databases such as PubMed and databases of the National Institute of Science Communication and Information Resources and Indian Council of Medical Research Embase were searched for relevant literature published from 2005/01/01 to 2020/05/13 in English language, according to the predefined inclusion and exclusion criteria. A manual search was also conducted using the key term “MRSA ‘or’ Methicillin Resistant
Result:
A total of 34 studies involving 16 237 patients were included in the final meta-analysis. The pooled proportion of patients with MRSA infection was 26.8% (95% CI: 23.2%-30.7%). The MRSA infection was more prevalent among male patients (60.4%; 95% CI: 53.9%-66.5%) as compared to female patients (39.6%; 95% CI: 33.5%-46.1%), while the prevalence of MRSA was higher among adults (18 years and above; 32%; 95% CI: 5%-80%) in comparison to pediatric patients (0-18 years; 68%; 95% CI: 20%-94.8%). The degree of heterogeneity was found to be significant.
Conclusion:
The prevalence of MRSA in India was relatively high at 27% with a higher proportion observed among men aged >18 years. The high prevalence of MRSA infections in India necessitates the implementation of surveillance and preventive measures to combat the spread of MRSA in both hospital and community settings.
Keywords
Introduction
Antimicrobial resistance is a serious global health concern that limits the prevention and treatment of infections, especially in a hospital setting. Antimicrobial resistance develops by the inactivation of the antibiotic, altered drug access to the target, modification of target, and decreased uptake. 1
As early as 1942, penicillin-resistant
The antimicrobial resistance patterns differ geographically, and the Asia-Pacific region accounts for one-third of the world’s population reporting a steadily increasing incidence of MRSA in healthcare settings since the 1980s.
7
Methicillin-resistant
The increasing trend of good clinical practices in hospitals has brought down the incidence of hospital-acquired MRSA infections; however, there is a steady increase in community-acquired MRSA infections, which poses challenges, particularly in densely populated countries like India. Further, the economic burden associated with the cost of treatment, long-term hospitalization, and the psychological stress considerably impact the healthcare systems across all regions. 10
Over the past few years, several studies have reported the prevalence of MRSA in different clinical settings within the Indian subcontinent, but the results are inconsistent with limited sample sizes.8,11
-13 Furthermore, few studies from the country suggest an impact of age and gender on MRSA carriage.14,15 It is imperative to understand the prevalence of risk factors, such as age and gender, on MRSA colonization at the country level to facilitate the implementation of appropriate infection control measures. This systematic review and meta-analysis was conducted to assess the prevalence, burden and epidemiology of methicillin-resistant
Methodology
This systematic review and meta-analysis was conducted in accordance with the Preferred Recording Items for Systematic Reviews and Meta-Analysis (PRISMA).
Eligibility criteria for studies
All human studies, published from 2005/01/01 to 2020/05/13 in English language that evaluated Indian patients of all age groups with a confirmed diagnosis of MRSA, were eligible for inclusion. We have also considered studies focusing on the Indian subcontinent, in particular or as one of the study sites.
Exclusion criteria for studies
All studies on MRSA patients that were conducted outside India or/and not conducted in the Indian population were excluded from the analysis. In addition, case studies, review articles, or studies for which full text was not available were excluded.
Measurements
The primary outcome of this study was the proportion of patients with MRSA in India. The secondary outcome was to determine the proportion of patients with MRSA across different age groups and gender from an Indian perspective.
Search strategy
We performed a systematic search on PubMed, using the key terms “(((Methicillin-Resistant
Data extraction
Data was collected from all the primary studies using a structured sheet in Microsoft Excel. Any discrepancies arising while entering the data were sorted out by discussion among all the contributors. The study characteristics extracted included authors details, year of publication, title of study, place of study, and type of study. Patient parameters included the number of study participants and their mean age. Two reviewers were involved in data extraction. Any disagreements among reviewers were resolved by discussion.
Statistical analysis
To determine the proportion of MRSA, a meta-analysis was performed of 95% confidence interval (CI). Besides, a meta-analysis using a random-effects method (DerSimonian and Laird method), the degree of heterogeneity
Results
A total of 229 studies were retrieved via PubMed and Google Scholar search, while 17 studies were obtained by handsearching. No additional studies were retrieved via ICMR, IDSA, WHO, and NICE database search. Around 40 relevant studies (Figure 1) were identified. The exclusion criteria were: were duplicates (70), case reports (54), does not include relevant data (30), does not match region and geography (06), does not include human participants (1), and reviews (25). All of the 40 studies were considered for qualitative as well as the quantitative synthesis of etiological agents. Ultimately, only 34 of 40 studies were included in the MRSA meta-analysis,8,9,15
-46 as the remaining 6 studies did not include data relevant to MRSA (4 efficacy studies, 1 study that described heteroresistance to vancomycin among methicillin-resistant
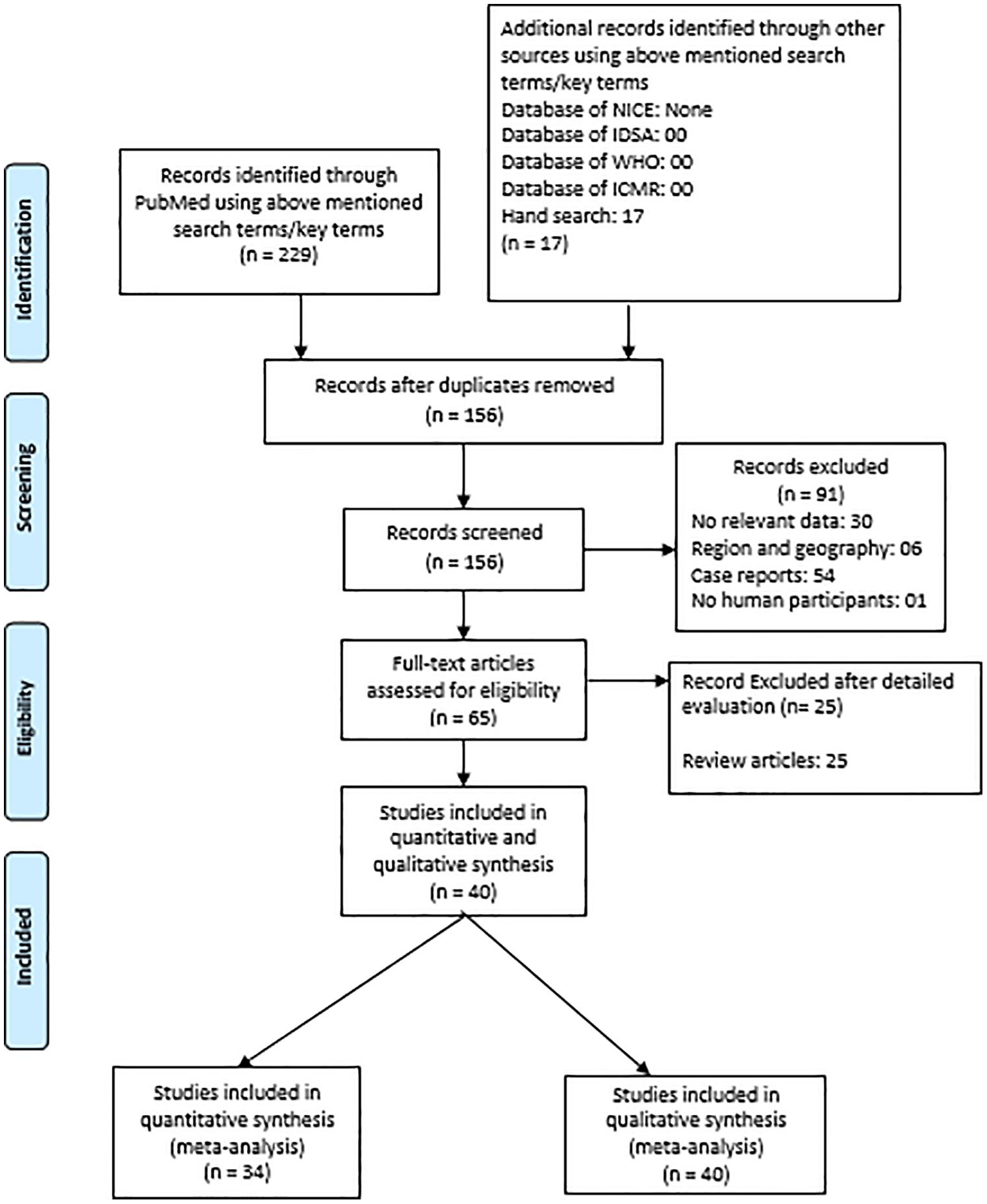
PRISMA flow diagram.
Study characteristics.
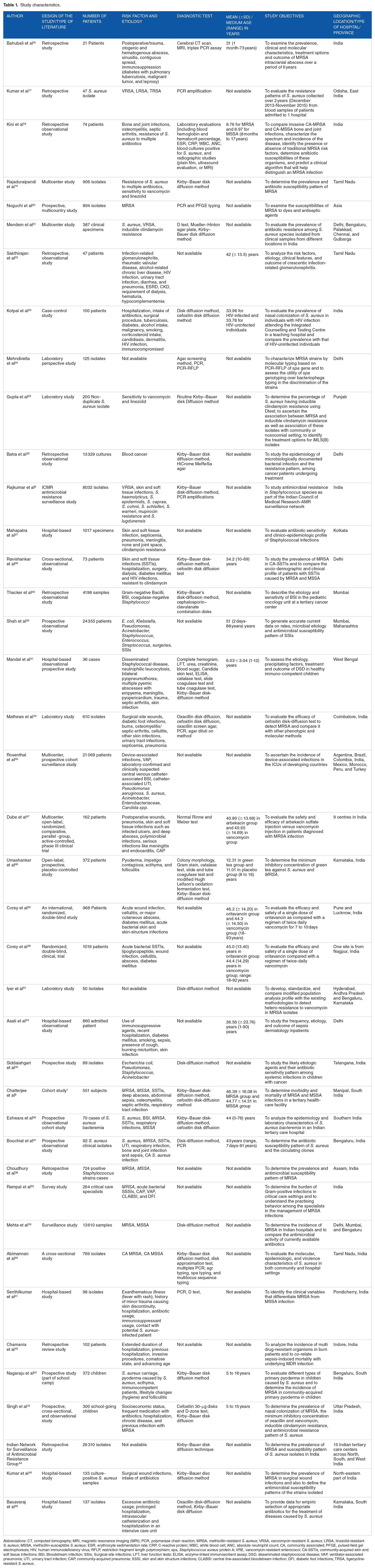
Abbreviations: CT, computed tomography; MRI, magnetic resonance imaging (MRI); PCR, polymerase chain reaction; MRSA, methicillin-resistant
Primary outcome
The meta-analysis included 16 237 patients aged between 1 month to 93 years. Clinical diagnosis was made by polymerase chain reaction assay, pulsed-field gel electrophoresis typing, radiologic evaluations (computed tomography and magnetic resonance imaging), laboratory evaluations, D test, Mueller–Hinton agar plate, antimicrobial discs methods like Kirby–Bauer disc diffusion method, Candida skin test, enzyme-linked immunosorbent assay, catalase test, slide coagulase test, tube coagulase test, Normal Rinne and Weber test, colony morphology, and Gram’s stain. Majority of studies used antimicrobial disc methods such as Kirby–Bauer disc diffusion method for clinical diagnosis of MRSA (Table 1).
The pooled proportion of patients with MRSA infection was 26.8% (95% CI: 23.2%-30.7%;
Proportion of MRSA infection in Indian patients.
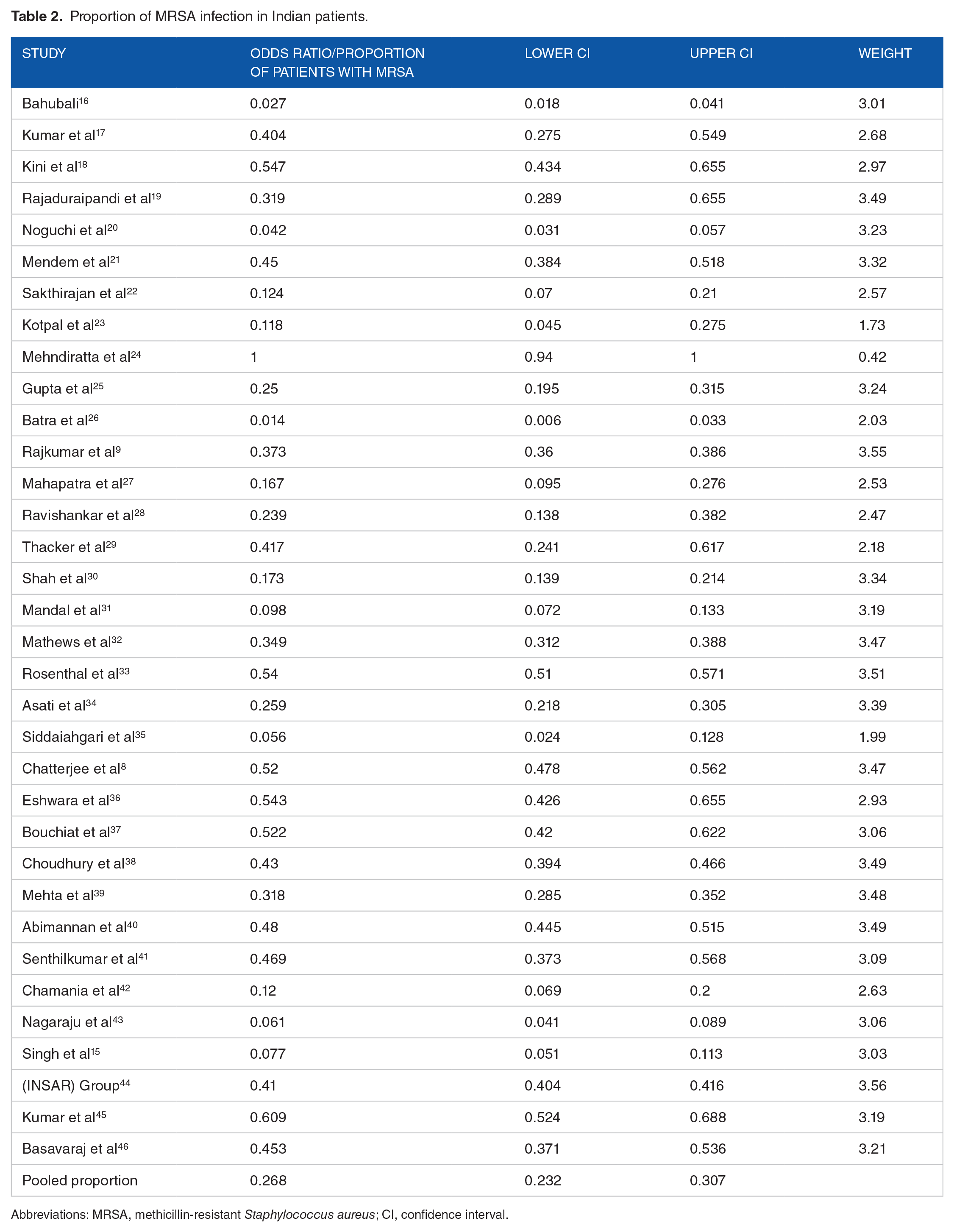
Abbreviations: MRSA, methicillin-resistant
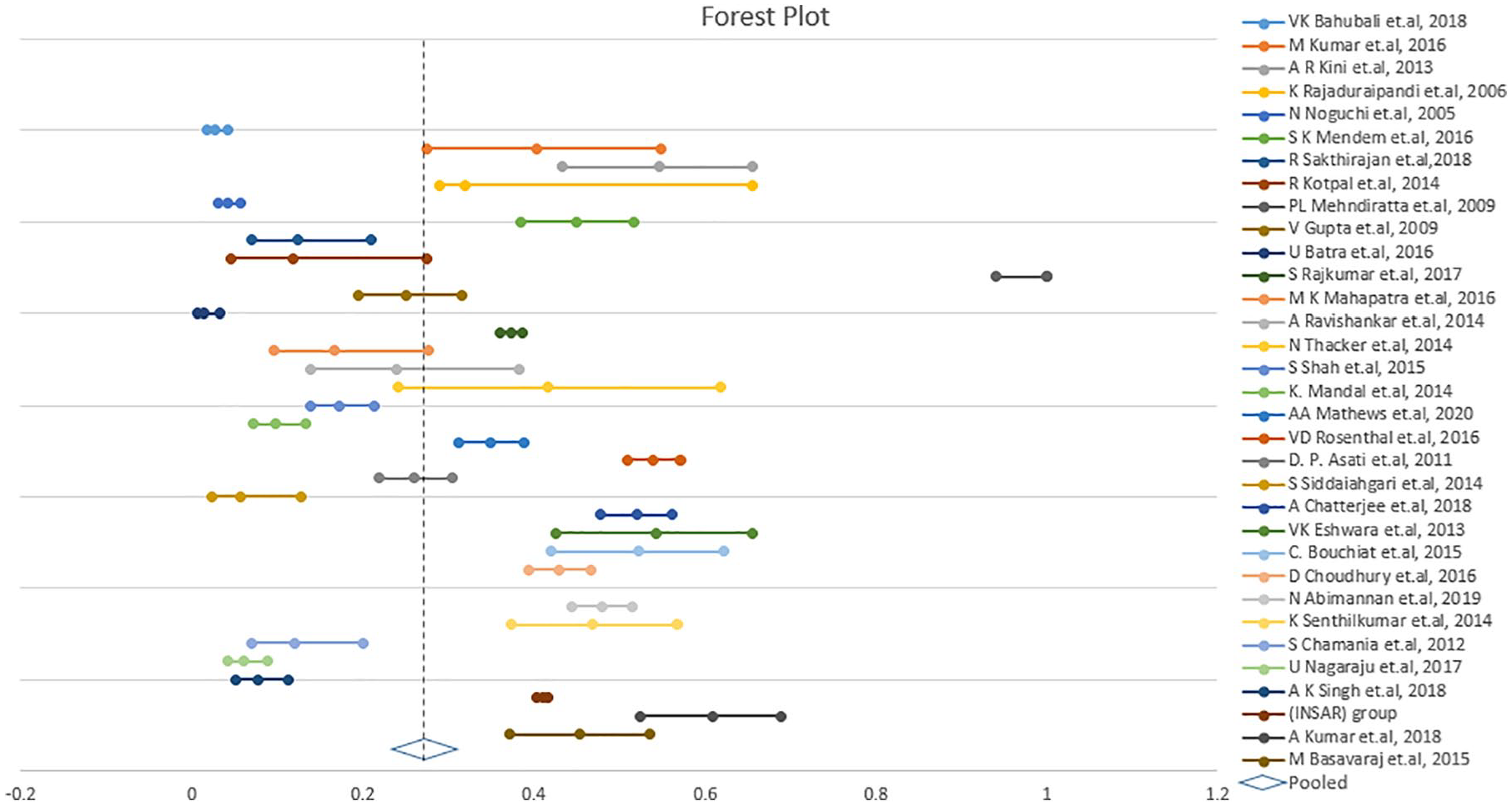
Forest plot displaying meta-analysis of proportion of prevalence in MRSA. Binary random effects model was applied to get pooled proportion and 95% confidence interval (0.268; 95% CI 0.232-0.307;
Secondary outcome
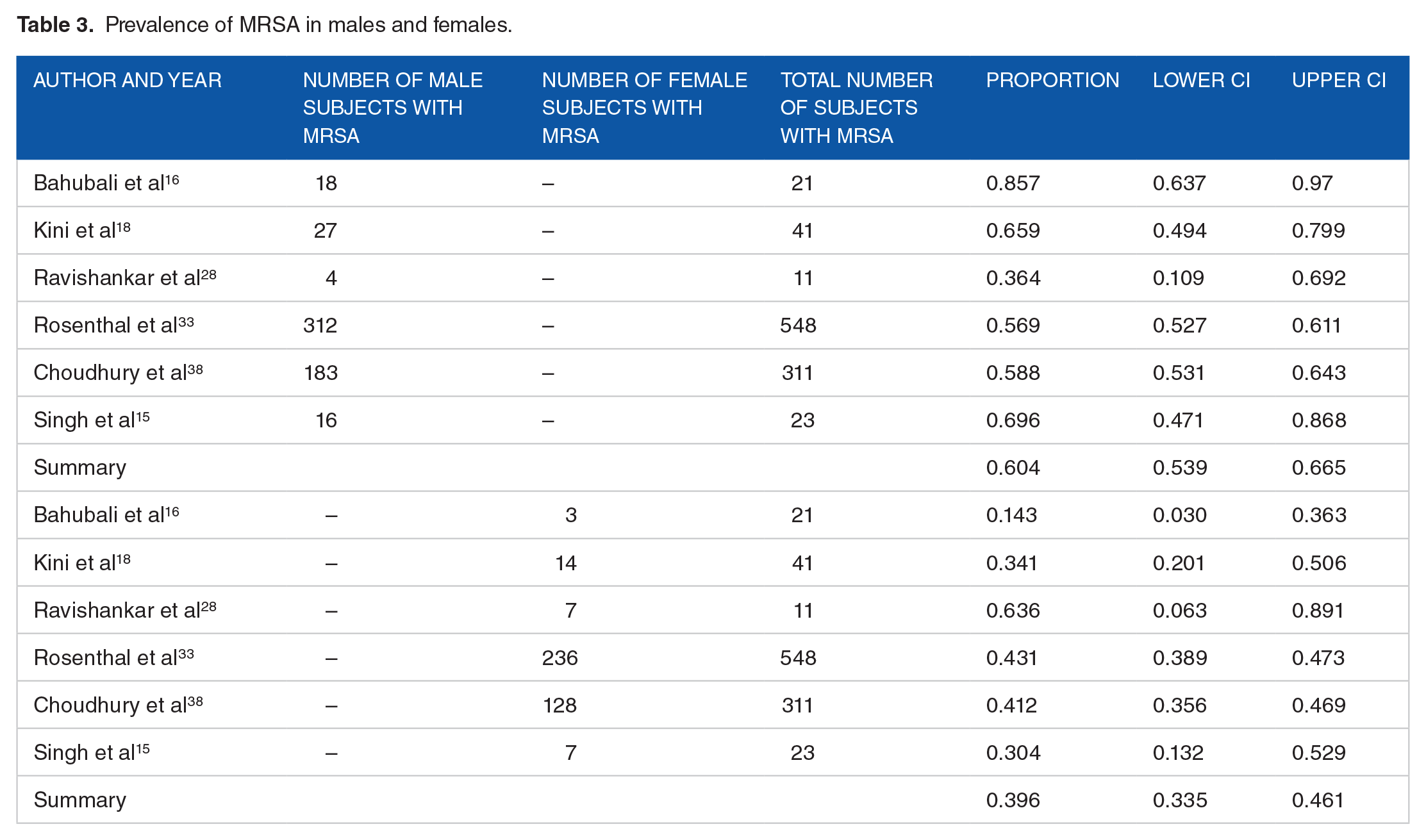
According to the subgroup analysis, the prevalence of MRSA infection was more in males [60.4%; 95% CI 53.9%-66.5%] than in female [39.6%; 95% CI 33.5%-46.1%] (Table 3) while prevalence was more in adult (18 years and above; 68%; 95% CI 20%-94.8%) in comparison with pediatric patients (0-18 years; 32%; 95% CI 5%-80%) (Table 4).
Prevalence of MRSA in males and females.
Prevalence of MRSA in adult and pediatric patients.
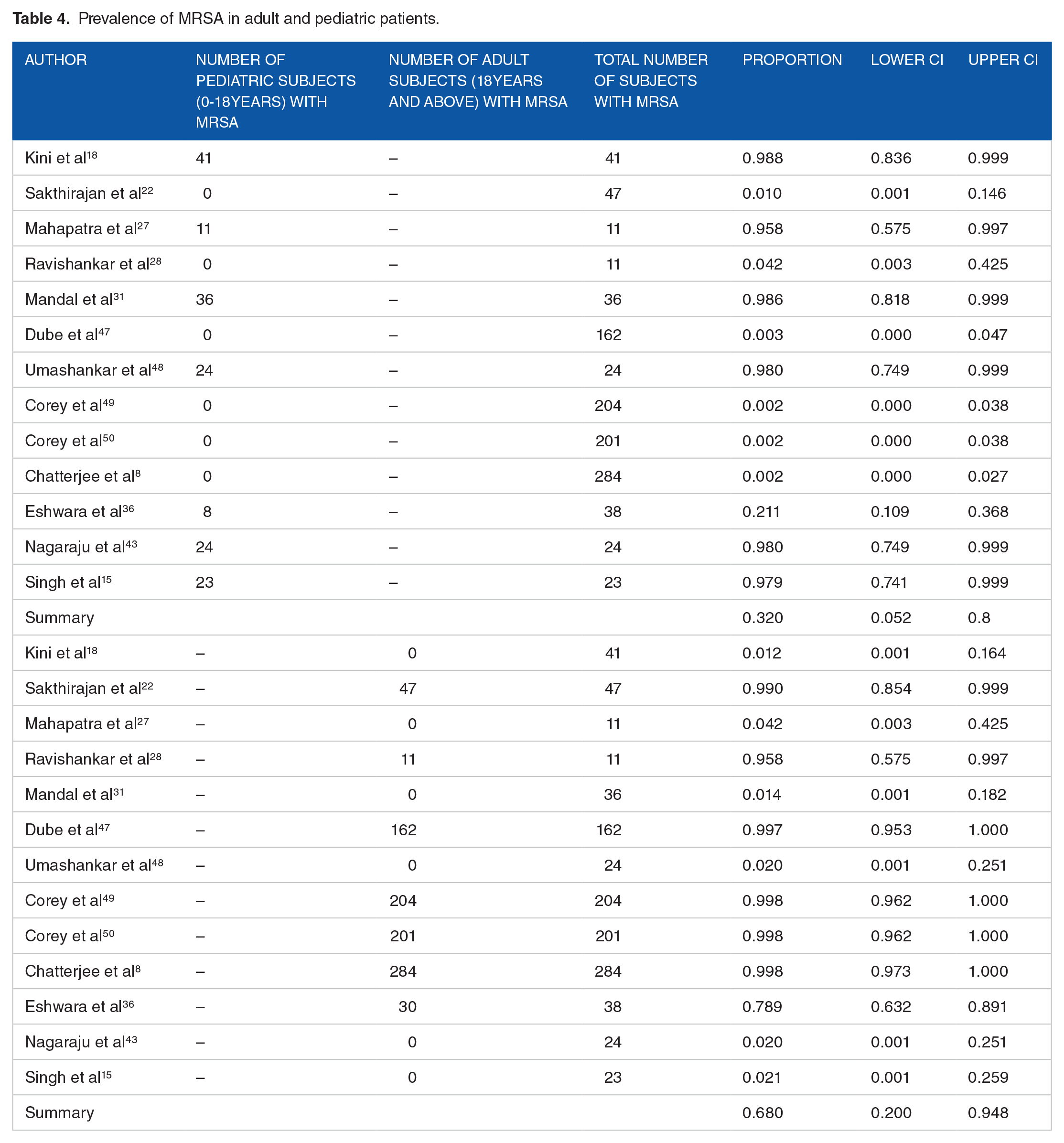
A total of 10 studies8,16,18,23,28,31,36,38,41,46 identified risk factors and co-morbidities, including diabetes, tuberculosis, malignancy, leprosy, extremes of age, group-house inhabitants, high mean body temperature (101.80°F), history of preceding illness/upper respiratory tract infections/trauma, abnormal laboratory values (hemoglobin [<9.5 g%], erythrocyte sedimentation rate [>35 mm/h], c-reactive protein [>32 mg/dL], leucocytes (>14 000 cells/109 L), absolute neutrophil count [(>65%]), immuno-compromised status, hospitalization in the last 3 months, present intake/history of antibiotics, history of surgical procedures, history of alcohol intake and smoking, history of intravenous drugs, history of corticosteroid intake, history of mucocutaneous candidiasis, history of dermatitis, history of sexually transmitted infections, socio-economic status, chronic kidney disease, heart disease, chronic obstructive pulmonary disease, rheumatoid arthritis, MRSA carriage (nasal or axillary or perineal or hand carriage in patients), prolonged duration of hospital stay, and irrational use/over prescription of antibiotics.
Four studies conducted in India focusing on the treatment of MRSA infections were identified; Arbekacin sulfate (200 mg) has shown 79% cure rate 47 and vancomycin hydrochloride (1000 mg BD) has shown a curate rate of 100% cure rate, 47 78.90%, 49 and 82.9% 50 in 3 studies, respectively. Besides, 2 studies suggested oritavancin as one of the treatment options for MRSA infections, with a cure rate of 82.30% 49 and 80.1%, respectively. 50
The survey conducted by Rampal et al, indicated an increasing trend in the prevalence and associated mortality in Gram-positive bacterial infections in critical care settings in India. 52 The limitations of the existing anti-MRSA agents necessitate the development of a newer agent with a broad spectrum anti-bacterial activity along with an improved safety profile.
Discussion
In order to reduce the burden of MRSA infections, continuous efforts should be made to prevent the spread and emergence of resistance by early detection of the resistant strains and using proper infection control measures in the hospital setting.
17
As most
In recent years, increasing prevalence of hospital-acquired and community-acquired MRSA infections have been reported in Indian population.40,43 This meta-analysis is the first to report the recent prevalence estimates and burden of MRSA among the Indian population. We also identified the high-risk groups in terms of age and gender so as to improve the disease surveillance and interventions of MRSA.
The pooled prevalence of MRSA in our study was 26.8%. These findings are almost similar to the estimates from other regions. The meta-analysis study by Wong et al has reported an MRSA prevalence of 0% to 23% in community settings and 0.7% to 10.4% in hospital settings in the Asia-Pacific region. Further, the study also reported a higher prevalence of community-acquired MRSA in India (16.5%-23.5%), followed by Vietnam (7.9%) and Taiwan (3.5%-3.8%). 54 A meta-analysis conducted by Wu and colleagues had reported an MRSA prevalence rate of 21.2% (95% CI, 18.5%-23.9%) in the healthy Chinese population. 2 Further, the reported prevalence of MRSA in Ethiopia, was 30.90% [95% CI, 21.81%-39.99%], while in Europe and the United States the prevalence rate was only 1.8% (95% CI, 1.34%-2.50%).55,56
The subgroup analysis reported a higher prevalence of MRSA among males compared to females in the Indian population (60.4% vs 39.6%), thereby indicating male gender to be a risk factor for MRSA infections. Similar to our findings, multivariate analysis by Harbath and colleagues reported male gender as 1 of the 9 independent risk factors of MRSA with an odds ratio of 1.9 (1.3-2.7). 57 In addition, a long-term study, spanning 7 years, conducted by Kupfer et al suggested male gender as a significant risk factor for MRSA acquisition. 58 Behavioral and physiological factors contribute to the high occurrence of MRSA in male population. Behavioral practices that may potentially influence MRSA colonization and infection rates in males include personal hygiene issues (including hand hygiene and nose picking and nail-biting habit), profession (those working with livestock industry), and playing contact sports. The physiological and immunological factors increasing the MRSA prevalence in males include an aggressive inflammatory immune response and higher levels of circulating inflammatory cytokine tumor necrosis factor-α. 14 Limited data on the association of higher gender differences and MRSA necessitate further research on the association between gender dimorphism and higher MRSA carriage in males.
Findings from our analysis indicate a higher prevalence of MRSA among adults (>18 years) compared to the pediatric population including adolescents (68% vs 32%). 59 An increased prevalence of MRSA in the adult population is associated with age-related changes including malnutrition and anatomic and physiologic modifications along with immune system dysfunction. Another meta-analysis by Lim et al studying the prevalence of MRSA in the Asia-Pacific region has reported a higher MRSA carriage prevalence among adults compared to children below 18 years of age. Similarly, a study by Wu et al had reported younger age as an influencing factor for MRSA colonization in healthy Chinese population. 2 The existing literature on the differences in MRSA carriage among different age groups is inconsistent because of the differences in the population included in such studies. Further studies are needed to assess the prevalence of MRSA across different age groups within similar cohorts.
The differences in prevalence across different geographic regions may be attributed to the methodologic variations of isolation and detection of MRSA, study population included for analysis, availability of health-care services, and the economic level of the assessed regions.
In our analysis, we also identified the treatment options for MRSA. Findings from the 4 studies included in our analysis suggest arbekacin sulfate of 200 mg, vancomycin hydrochloride of 100 mg, and oritavancin as the treatment options for MRSA infections in India.47,49,50 Various clinical studies and systematic reviews have reported beneficial clinical outcomes with these antibiotics in the treatment of MRSA infections.60 -62
The strengths of our meta-analysis is inclusion of a larger number of studies having a sufficiently large sample size. Further, as MRSA infections are a serious public health concern, this meta-analysis, the first to be conducted in the Indian population, may provide epidemiologic data on MRSA and the associated risk factors.
Our study has a few limitations in terms of inclusion of studies that had heterogeneity in the prevalence of MRSA and wide variation in patient cohorts. Further prospective studies are required to verify these results in order to facilitate preventive measures for mitigating MRSA in the Indian subcontinent.
Conclusion
This meta-analysis documents the prevalence of MRSA in India, which is considerably higher than that reported in other Asian countries. Further, the increased prevalence of MRSA in male patients of age >18 years highlights the need for further examination in these high-risk cohorts. Appropriate surveillance and preventive measures for reducing the risk of development and transmission of MRSA in the Indian subcontinent are indispensable.
Footnotes
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This metaanalysis was funded by Pfizer Limited, India.
Author Contributions
CJG was involved in the design of meta-analysis, did the data analyses, and wrote the first draft of this manuscript with input from SW who assisted with the tables and figures and GR who also advised on the statistical analyses. All authors contributed to refining their approved submitted manuscript.
