Abstract
Background:
Healthcare providers are in high occupational risk of Hepatitis B virus infection than that of the general population because of the high risk of occupational exposure to patients’ body fluids and accidental sharp injuries. There are no large facility-based studies conducted on the prevalence of HBV infection and its associated factors among health care providers in eastern Ethiopia.
Objective:
This study aimed at investigating the seroprevalence of Hepatitis B Virus and its associated factors among the healthcare providers in public health facilities in eastern Ethiopia.
Methods:
A facility-based cross-sectional study was conducted among 438 randomly selected healthcare providers in eastern Ethiopia from March to June 2018. Pretested structured questionnaire was used to collect data on socio-demographic characteristics and other risk factors. In addition, a 2.5 ml blood was collected and the serum was analyzed for Hepatitis B surface antigen using the Instant Hepatitis B surface antigen kit. Data were entered using Epidata version 3.1 and analyzed using SPSS statistical packages version 22. Descriptive summary measures were used. Bivariate and multivariable logistic regression was conducted at 95% CI. An association at P-value <.05 was considered statistically significant.
Results:
A total of 438 (92.02% response rate) health care providers have participated in this study. The prevalence of hepatitis B virus infection was 9.6%. There were no significant differences in the HBV infection rates among healthcare providers with respect to socio-demographic characteristics (P-value >.05). After adjusting for some variables, the following variables remained statistically significantly associated with HBsAg positive result in the multivariable analysis: exposure to body fluids (AOR = 3.0; 95% CI [1.25, 7.05]), history of needle stick injury (AOR = 4.70; 95% CI [2.10, 10.55]), history of operation/surgery (AOR = 4.88, 95% CI [1.43, 16.62]), history of multiple sexual partner (AOR = 7.48; 95% CI [2.08, 26.96]), and being unvaccinated (AOR = 6.09; 95% CI [2.75, 13.51]).
Conclusion:
This study showed a high prevalence of HBV infection among health care providers in eastern Ethiopia. This is significant because health professionals may be at increased risk of chronic complications and may also be source of infection for their clients and general population during their healthcare practice. Management commitment that should focus on occupational safety and health promotions is necessary.
Introduction
Viral hepatitis is one of the most common infectious diseases worldwide. Hepatitis B virus (HBV) is the most serious type of viral hepatitis that causes inflammation of the liver and in many cases can lead to chronic liver disease and put people at high risk of death from cirrhosis of the liver and liver cancer.1,2 Hepatitis B virus infection caused 1.34 million death worldwide in 2015 which was comparable to deaths caused by tuberculosis and higher than those caused by Human immunodeficiency virus (HIV). 3 A study in Ethiopia indicates 5% of healthcare workers are infected with HBV. 4 It is thought to be 50 to 100 times more infectious than HIV. 5 Chronic or lifelong illness from HBV results in the development of cirrhosis of the liver and liver cancer.1,6 People with chronic hepatitis B have a 15% to 25% risk of dying earlier from HBV related complications. 7
Hepatitis B virus is spread by contact with infected blood or body fluids, from mother to child, transfusion of blood, or blood products and unprotected sexual intercourse.2,8,9 Healthcare providers are in high occupational risk of HBV infection because they usually come in contact with patients’ blood and other body fluids in a healthcare set up. Literature indicate that healthcare personnel are 4 times more likely to be infected by HBV than that of the general adult population. 10 The most common routes of transmission from patients to workers are needle stick and other sharps injuries, followed by mucocutaneous exposure. 11
Studies estimated that the incidence of injuries to healthcare workers caused by sharp objects ranges from 1.4 to 9.5 per 100 healthcare workers per year, resulting in 0.42 HBV infections per 100 sharp-object injuries per year. 12
The risks for occupational infection with blood-borne pathogens have been a source of concern among health professionals because of their frequent and often substantial exposures to patient blood and body fluids. Occupational exposure to HBV among health professionals did not receive great attention in the Ethiopian setting. There are a limited number of wider facility-based studies conducted on seroprevalence of HBV among health care professionals working in health facilities particularly in eastern Ethiopia. This study, therefore, aimed to investigate the seroprevalence of HBV and its associated factors among healthcare providers in eastern Ethiopia which is expected to fill this information gap. The finding of this study will probably provide concrete evidence for policy makers and program implementers so that evidence-based strategic and operational decisions can be made on HBV vaccine access and occupational safety and health promotions.
Methods and Materials
Study design and setting
A facility-based quantitative cross-sectional study was conducted in public health facilities of Harari Region, Dire Dawa city administration, and east and west Hararghe zones of Oromia Regional State in eastern Ethiopia from March to June 2018. Data obtained from the Respective health offices indicate there were around 211 public health facilities (9 general hospitals, 1 primary hospital, and 1 specialized university hospital and 200 health centers) in the study area where 115 health centers and 5 hospitals are found in East Hararghe, 65 health centers and 2 hospitals in west Hararghe, 12 health centers and 2 hospitals in Dire Dawa, and 8 health centers and 2 hospitals in Harar. The Eastern part of Ethiopia is known for its high population density (Diredawa being the second largest city and Harar the ninth), preceded by southern nation and nationalities and Amhara region, and it’s the route for the national import and export through Djibouti and Somali land ports.
Participants and sampling procedures
Multistage sampling technique was used for each region (Harari region, Diredawa, and 2 zones of Oromia region) and facilities were then stratified into hospitals and health centers (Figure 1). Accordingly, all 11 hospitals and 30 health centers, from 200 health centers found in study area, were selected by Lottery method. The health centers selection was based on their overall percentage representation out of 200 HC found in this part of Ethiopia. Randomly selected healthcare providers who were working at the selected health facilities and healthy enough to provide information were included. There was no exclusion of study participants’ because this was managed with addition of 10% non-response.
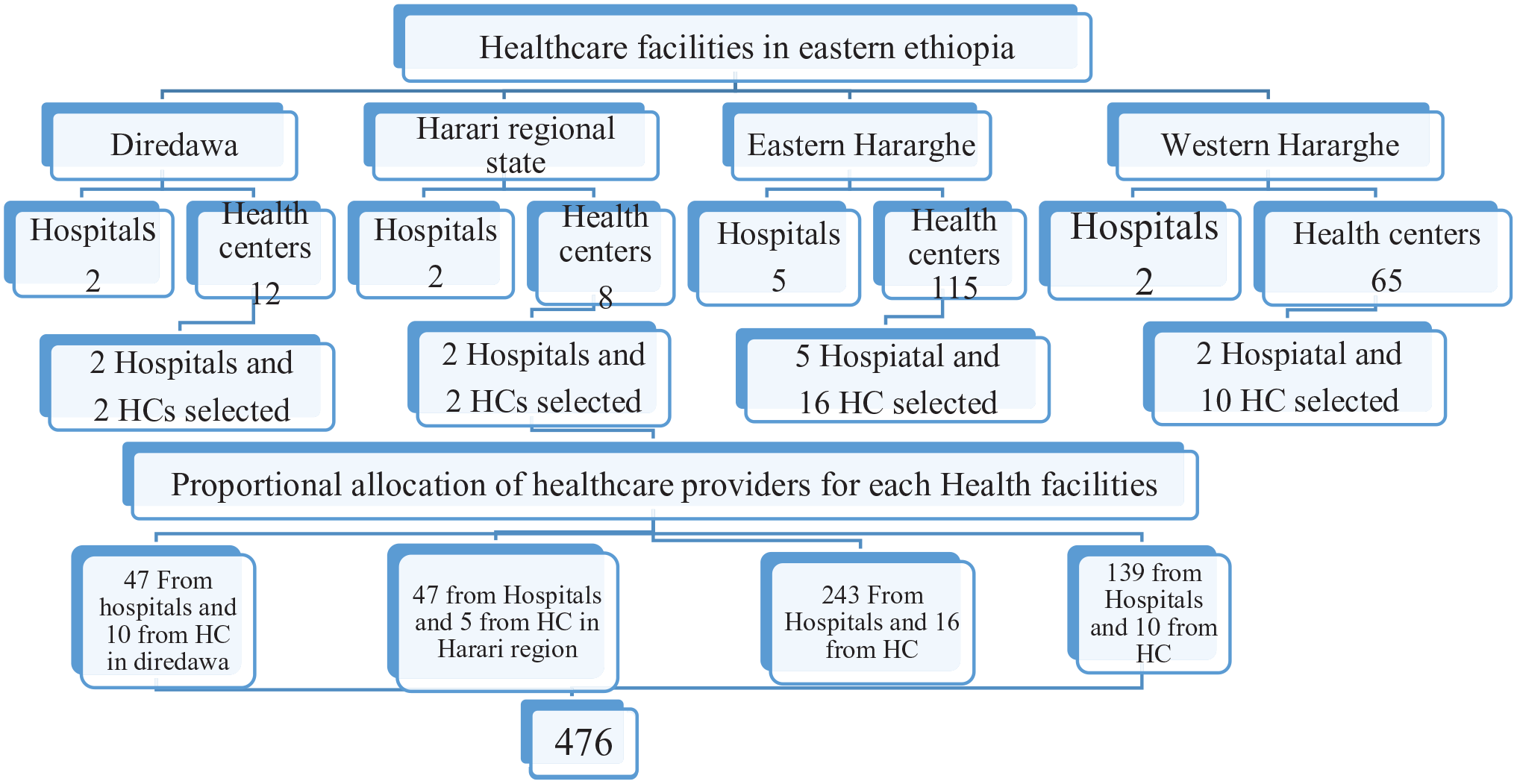
Flow diagram of health facility and participant selection for HBV infection study among healthcare providers in Eastern Ethiopia, 2018 (NB: HC; Health center).
The sample size was determined using a single population proportion formula for both objective with an assumption of 80% power, 0.05% margin of error, and a design effect of 1.5. The larger sample size was obtained with the first objective (prevalence of HBV from the previous study by Geberemicheal et al 13 which was 7.3%). Accordingly, 476 samples were needed with a 10% non-response rate. The study participants were then proportionally allocated for respective selected health institutions based on the number of study population working at each selected health institution. Samples of health professionals were drawn within each health institution by a simple random sampling method by using the lottery method (Figure 1). Registered institutional identification number (ID) of study participants were used as a sampling frame.
Variable measurements: The primary outcome of this study was the prevalence of HBV infection among health care providers
➢ Hepatitis B surface antigen positive (+HBsAg): Presence of Hepatitis B surface antigen in an individual’s serum.
➢ Knowledge on universal precaution guideline: was measured using a 10 question item and categorized as yes or no.
➢ The following independent variables were included in the data collection:
Socio demographic characteristics, ever diagnosed for HBV, exposure to blood and blood product of other patient, previous immunization with hepatitis B vaccines, history of jaundice, blood transfusions, and previous operations, presence of sign and symptom of liver disease, history of liver diseases, sexual exposure, family history of liver disease, year of study/service, ward of attachment.
Data collection and data quality control: A structured questionnaire was used for data collection from health care providers. Five nurses and 5 public health professionals were recruited for data collection. The questionnaire was developed after reviewing different literature13-17 and pretested on 5% of sample size working at hospitals that were not included in the study. The questionnaire was translated into the local language (Afan Oromo and Amharic). During data collection, the data was checked for its completeness each day by supervisors and investigators after it was collected. For blood sample collection, all materials we used were checked for their production date and functionality before purchase. A blood sample was collected with standard precaution and was stored in the recommended temperature.
Blood sample: Five laboratory professionals were recruited to collect the blood samples. About 2.5 ml of venous blood samples were collected into tubes aseptically after written consent was obtained from study subjects. Serum was separated by centrifugation at 3000 r/minutes for 5 minutes after the blood was clotted. The blood samples were labeled with unique identification numbers. The serum was separated by centrifugation and was placed into Eppendorf tubes.
The serological tests were performed using hepatitis B surface antigen rapid test kits which work in the principle of immunochromatography. The serum was tested for HBsAg by Wondfo 1 step HBsAg test strip according to the manufacturer’s manual (Guangzhou Wondfo Biotech Co., Ltd [Wondfo]). This test strip has sensitivity and specificity of 96.2% and 99.3% respectively. Precautions were taken during sample testing such retesting sample and keeping equipment from cross contamination. Single quality-assured serological in vitro diagnostic test (rapid diagnostic test [RDT]) to detect HBsAg antibody was used.
Data processing and analysis
Collected data were entered into Epidata version 3.1 and exported to SPSS version 22 statistical packages for analysis. Descriptive summary measures were conducted for presenting the findings. Binary logistic regression analysis was done to measure association between dependent and independent variables. Variables with P-value ⩽0.2 in bivariate analysis were entered into multivariable logistic regression analysis at a 95% confidence interval to determine the presence of an association between explanatory variables and the sero-positivity of HBV among healthcare providers. P-value <.05 at 95% CI was taken as a cut-off point for statistical significance. Model fitness was checked using Hosmer Lemeshow goodness of fit.
Ethical considerations
Ethical approval was obtained from the Institutional Health Research Ethics Review Committee (IHRERC) of Haramaya University, college of health and medical science (CHMS) (Ref. No IHRERC/093/2017). Informed, written, and signed consent was obtained from each participant. Data was collected anonymously for confidentiality of participants. Results were communicated to study subjects based on their request and counseling was given for treatment for hepatitis B virus infection.
Results
Sociodemographic characteristics of the study subjects
A total of 92.02% (438/476) health professionals from 11 hospitals and 30 health centers have participated in this study (Table 1). About 63.5% (278/438) of these participants were males. The median age of the study participant was 28 years old (IQR = 7). About two-thirds of the respondents were nurses (65.5%). The majority of the study participants (51.8%) were married whereas the median years of service was 4 years (IQR = 3). Out of the 438 study participants, 47% (206/438) were Muslim and 48.1% (211/438) were Oromo ethnic groups (Table 1).
Socio-demographic characteristics of the study participants, eastern Ethiopia, 2018.
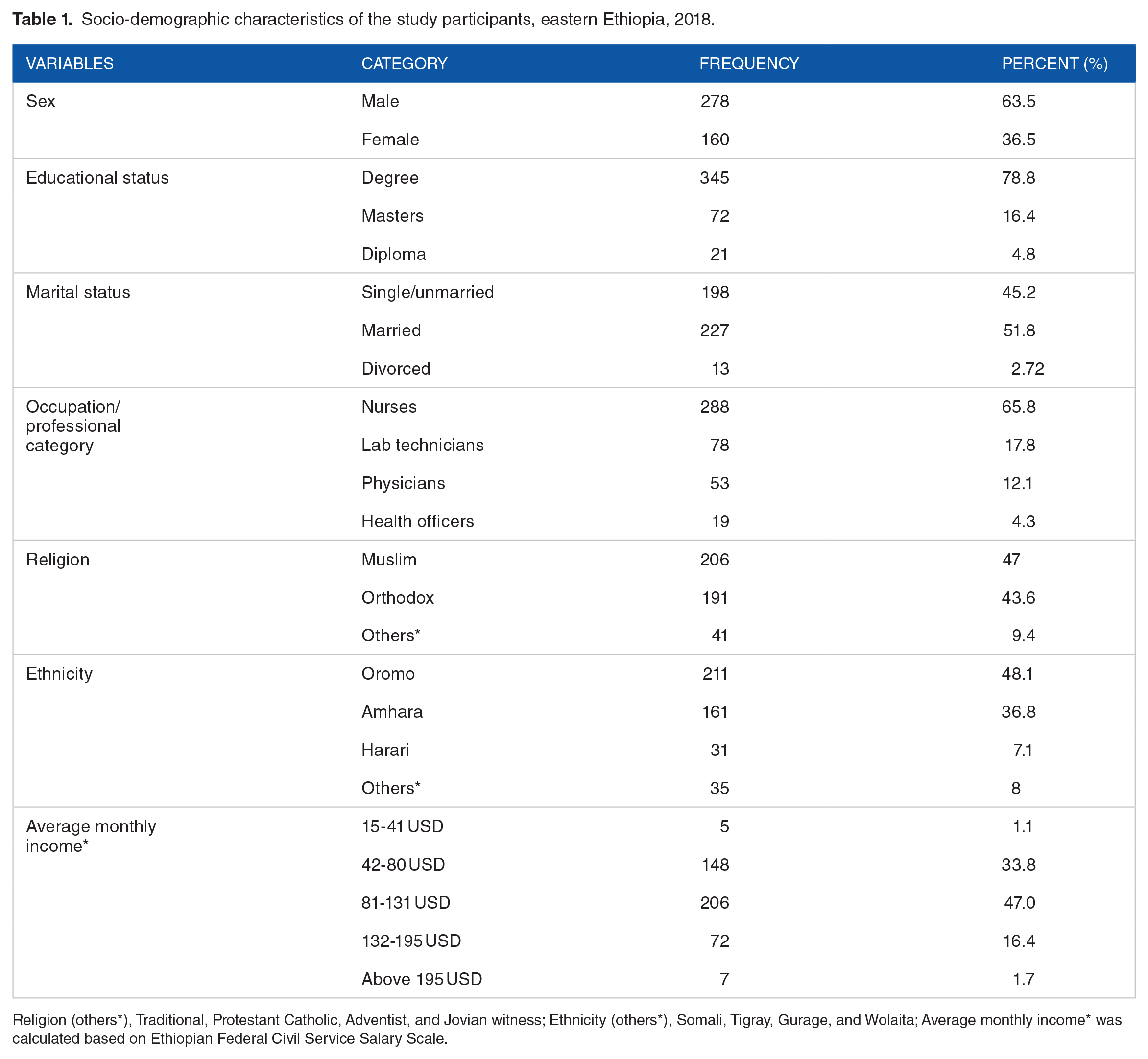
Religion (others*), Traditional, Protestant Catholic, Adventist, and Jovian witness; Ethnicity (others*), Somali, Tigray, Gurage, and Wolaita; Average monthly income* was calculated based on Ethiopian Federal Civil Service Salary Scale.
Healthcare providers’ occupational and other risks for HBV
According to this study, 87.7% (384/438) of the study participants have knowledge of universal precaution guideline and 58.4% (256/438) have participated in any training program about infection prevention or universal precaution. More than 3-quarters (78.1%) of the study participants have participated in the collection of patients’ bloods and 90% of respondents said that they cleaned their hands after touching or collection of blood or other body fluids. Of these, 3 quarters (75.57%) used plain water and soap whereas 25.43% of them used alcohol-based hand rubbing. From all participants, 9.6% said that they did not wear personal protective equipment (PPE) frequently. Twenty-nine (29/42) of those who do not frequently use PPE said they did not wear it because it is not always necessarily followed by uncomfortable to wear always (8/42) and supply out of stock (5/42). About 317 (72.4%) of the study participants said they used glove consistently for personal protection during work. On the other hand, about half (54.3%) of the study participants have a history of exposure to any type of body fluids (such as blood, peritoneal, pericardial, pleural, synovial, cerebro-spinal fluid [CSF] amniotic fluids, and others). Among those who were exposed to body fluids, 33.64% (73) of them had exposure to body fluids at least twice (Figure 2).
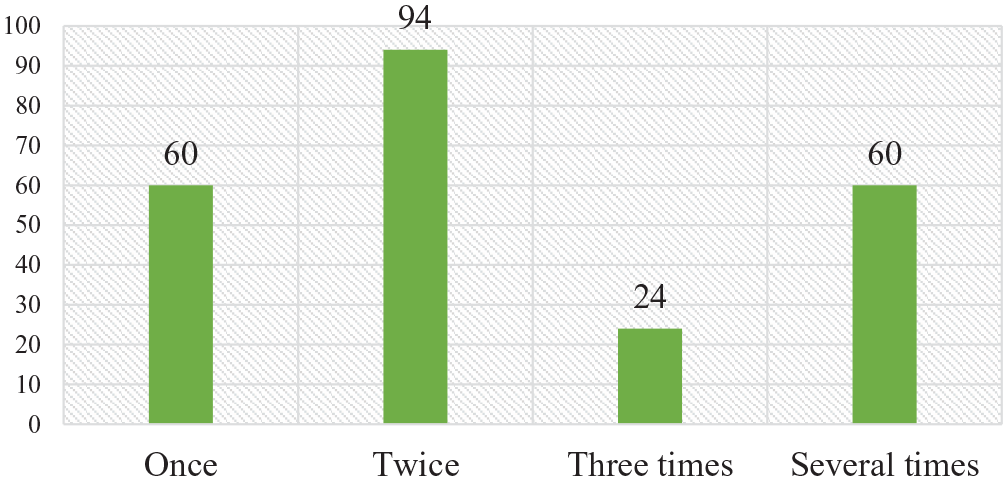
Frequency of exposure to body fluids among health care providers in public health facilities in eastern Ethiopia, 2018.
On the other hand, 41.8% (183/438) had a history of needle stick injury. Among those with a history of needle stick injury, 19.12% had needle stick injury several times (Figure 3).
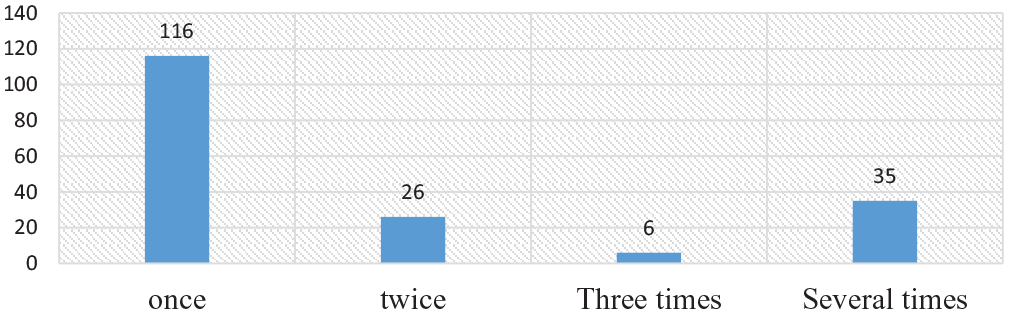
Frequency of needle sticks injury among health care providers in public health facilities in eastern Ethiopia, 2018.
The majority of the respondents (61.6%) said they ever cared for hepatitis virus positive patients. In addition, 7.1% of the respondents said they underwent surgical operations. Approximately 10% of the study participants had received blood from donors and 6.8% and 19.25% had a history of tattooing and tooth extraction respectively. Furthermore, 2.5% of the study participants said they have been diagnosed with jaundice and/or liver diseases. From the total study subjects, 5.3% said that they had a history of multiple sexual partners out of which 3.4% had multiple sexual partners in the last 1 year. Thirteen study subjects (3.0%) had a history of sexual intercourse with commercial sex workers. Thirty-seven study subjects (8.4%) said that they had a family history of chronic liver diseases. Among the total study subjects, 82.2% said that they have been fully vaccinated for HBV.
Prevalence of hepatitis B infection among study subjects
Forty-two, (9.6%; 95% CI [6.8, 21.3]) of the respondents are found positive for HBsAg. More than half (59.52%, 22/42) of those positive cases were among Nurses. But there was no significant difference in infection among professional category (P-value: >.05) (Table 2).
Prevalence of HBV infection among different professional category in the study area, eastern Ethiopia, 2018.
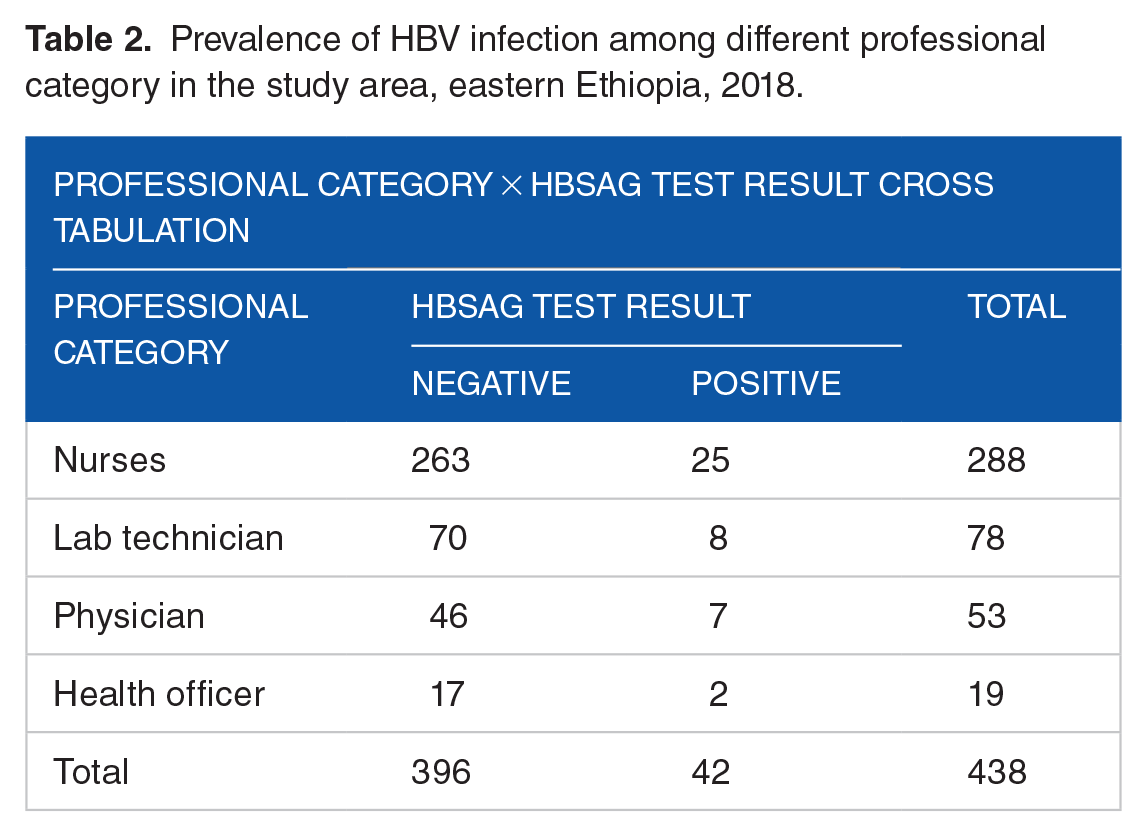
Significant difference in infection rate was observed between those exposed to body fluids and those who did not (P-value = .002), between those with history of needle stick injury and not (73.81%, 31/42, P-value = .0001; but not between those with history of other sharp injury [P-value = .63]), between those with history of surgical operation and not (P-value = .001), between those with history of multiple sexual partners and not (P-value = .001), and being fully vaccinated or not (P-value = .001). But there was no statistically significant difference in HBV infection status by sex and other socio-demographic variables, knowledge, and training on universal precaution guidelines, patient blood collection, wearing personal protective equipment, or care for patients with hepatitis, history of blood transfusion, history of diagnosis for jaundice, or family history of liver disease, history of tattooing, and history of tooth extraction (P-value ⩾.05).
Factors associated with HBV infection among the study population
In the bivariate logistic regression analysis, variables with a P-value of <0.2 were selected for multivariable analysis by adjusting for other variables.
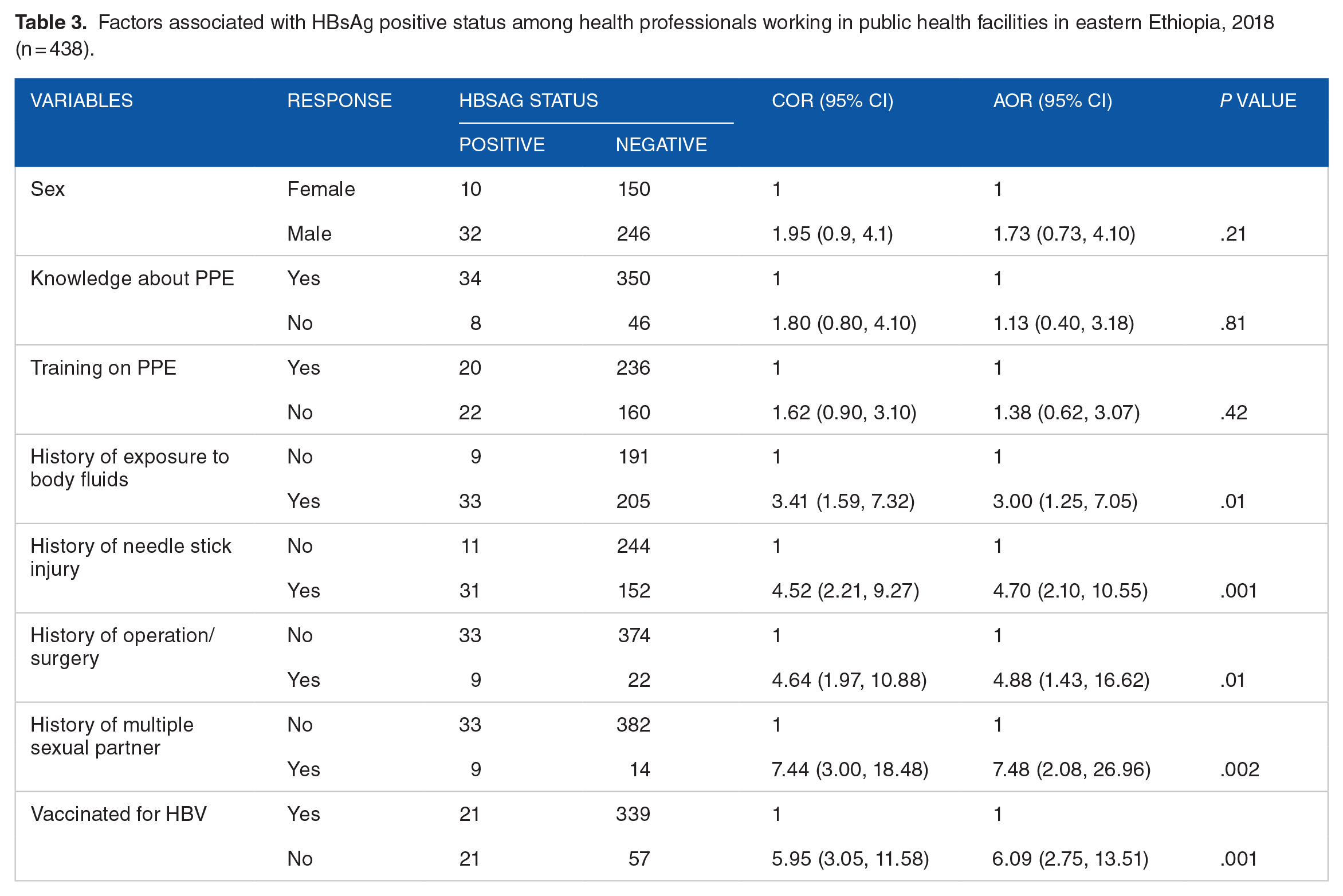
Health professionals who were exposed to body fluids were 3 times (AOR = 3.0; 95% CI [1.25, 7.05]) more likely to be positive for HBsAg compared with those who have no history of exposure to body fluids (Table 3). Health professionals who have a history of needle stick injury were 4.7 times (AOR = 4.70; 95% CI [2.10, 10.55]) more likely to be positive for HBsAg than those who have no a history of needle stick injury. Study participants who have a history of operation/surgery were 5 times (AOR = 4.88, 95% CI [1.43, 16.62]) more likely to be positive for HBsAg than their counterparts (Table 3). The odds of being positive for HBV infection is almost 7.5 times higher in those who had multiple sexual partners (AOR = 7.48; 95% CI [2.08, 26.96]) than their counterpart. Moreover, health professionals who have never been vaccinated for HBV were 6 times (AOR = 6.09; 95% CI [2.75, 13.51]) more likely to be positive for HBsAg compared to those who have received a vaccine for HBV (Table 3).
Factors associated with HBsAg positive status among health professionals working in public health facilities in eastern Ethiopia, 2018 (n = 438).
Discussions
According to this study, the seroprevalence of hepatitis B among health care provider is high among health care providers in eastern Ethiopia (nearly 1 out of 10 healthcare providers are infected with HBV). This finding is higher than other studies from Peshawar Pakistan, 18 Nigeria, 19 Thailand, 20 northwest, southwestern, and central Ethiopia.21-23 The finding of this study goes in line with the report of articles in which high prevalence (⩾8%) hepatitis B infection occurs in countries like North America, South America, Sub-Saharan Africa, and most Asian countries which Ethiopian is one of them.24-26 This high prevalence could be explained by high level of occupation exposure to body fluids and sharp injuries among our study subjects. In addition, the number of facilities involved in our study may account for this high prevalence. The finding of our study is relatively consistent with studies done among healthcare professionals in Uganda, 14 Tanzania, 27 and southern Ethiopia. 13
On the other hand, more than two third of healthcare providers in our study had received full dose of HBV vaccine. It is similar to a study conducted in Kenya, 28 but higher than study conducted in southwestern Niger, 19 Northern Tanzania, 29 Cameroon, 30 Pakistan, 18 and Addis Ababa Ethiopia. 31 This high vaccination status is mainly due to a free HBV vaccine being provided to healthcare workers by Ethiopian government in the past 5 years.
The odds of HBV infection were 3 times more likely among health professionals’ who were exposed to body fluids compared with those who have no history of exposure to body fluids. It is a fact that HBV is transmissible when blood or another bodily fluid from a person with the virus enters the body of an individual as well as from mother to a newborn child during delivery.8,32,33 A study by Davis 9 showed that the virus can survive outside the body for at least 7 days in which it can still cause infection if it enters the body of a person who has not received vaccination against it. This finding indicates the need for improved health promotion and management interventions to prevent exposure to body fluids. Adequate personal protective equipment supplement and training on precaution guideline is necessary.
This study showed almost 5-fold higher risk for HCWs to acquire HBV infection if they ever had needle stick injury than their counterpart. This finding is supported by a study in northeast Ethiopia. 34 Similarly, numerous studies have shown that occupational exposure puts health personnel at risk of hepatitis B infection with higher rates following needle stick injuries.35-37 History of operation/surgery significantly increased the odds of HBV infection by about 5 times than those with no history of surgery in the current study. Previous studies have also identified similar finding where HBV transmissions resulted from non-compliance with aseptic techniques like due to cross-contamination of medical equipment and devices including inadequately sterilized needles and medical instruments, the reuse of disposable needles and syringes, and contamination of multiple-dose medication vials during surgical procedures.9,38,39
Sexual routes are also highly efficient modes of transmission for HBV.8,24 According to this study, those who had multiple sexual partners in the last year were almost 7.5 times more like to be infected by HBV than their counterparts. This finding is similar to studies conducted in Tigray Ethiopia, 40 Slovakia, 41 and Iran. 42 This is scientifically well-established facts where sexual route plays an important role in the transmission of HBV.43-45
Moreover, this study revealed that the odds of being positive for HBV are higher (6 times) if health professionals were not vaccinated for HBV. This finding is similar to studies conducted in Thailand 20 and northern Tanzania. 29 Studies indicated that HBV vaccines constituted a landmark of great importance for medical practice which lowers HBV transmission rates. 29
Unlike a study in Uganda, 14 service year and training on PPE were not significantly associated with HBV infection status in this study. Blood transfusion was also not significantly associated with HBV infection mainly due to blood screening before donation. This is supported by a study conducted by Alter where transmission of HBV via transfusion or transplant has been virtually eliminated in countries that test donors for HBsAg and virally inactivate plasma-derived products. 8
Strength and limitation of the study
The representativeness of the finding of this study can be appreciated as it included a large-scale health facilities and geographic areas. However, we recognized certain limitations including insufficient immunoassay logistics supply which restricted this study to provide data on other HBV serological markers as HBeAg, IgM, and IgG anti-HBc. In addition, the use of rapid tests in the absence of confirmatory conventional immunoassays may also a limitation. This limited the study classifying whether infections are acute or chronic and whether the degree of infectivity correlates with a high level of HBV replication or not.
Conclusions
The prevalence of hepatitis B virus infection among healthcare workers in this study was high compared to other findings. The majority of HCWs were exposed to potential risks of infection mainly body fluids like blood. More than two-thirds of them were vaccinated against HBV which is higher than previous studies. But these findings highlight the need for continuous improvement of the working environment of health care providers on the provision of sterile surgical procedures and personal protection from needle stick injury. The vaccination program to HCWs should continue to be implemented despite good vaccination coverage. Appropriate intervention should be focused on occupational safety and health promotions. Moreover, this finding indicates the need for improved health promotion and management interventions to prevent exposure to body fluids.
Footnotes
Acknowledgements
We thank all of the staff at Harari region, Dire Dawa city Administration, west Hararghe, and east Hararghe zone administrations and health facilities for providing organizational support. We would like to extent our appreciation for all of our data collectors and supervisors. Lastly, we would like to acknowledge Haramaya University for funding this study.
Author Contributions
DA and TT conceived the study and drafted the proposal. DA, TT, BH, and AG had substantial contributions to the study design and development of the data collection checklist. AT drafted the manuscript. DA, BH, AT, and TT wrote and corrected the manuscript. All authors read the manuscript and approved it.
Availability of Data and Materials
Most of the data generated or analyzed during this study are included in this published article. The full datasets used and/or analyzed during the current study is available from the corresponding author on reasonable request.
Ethics Approval
The study protocol was approved by Institutional Health Research Ethics Review Committee (IHRERC) of Haramaya University, College of Health and Medical Sciences (CHMS) (Ref. No IHRERC/093/2017). All methods were carried out in accordance with relevant guidelines and regulations of Haramaya University. Thus, informed, written, and signed consent was obtained from each participant.
Consent to Participate
Consent to participate from study subjects were written and signed individually on hard copy. Thus, it is not possible to submit all consents form.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was funded by Research Affairs Office of Haramaya University.
