Abstract
Introduction:
Patients with malignancies frequently develop infections as a result of surgical procedures and fungating wounds leading to pus formation. This cross-sectional study was conducted to explore the bacteriological spectra of infections of various cancer sites and their antibiotic sensitivity patterns among the patients visiting minor operation theatre (OT) of B.P. Koirala Memorial Cancer Hospital (BPKMCH), Chitwan, Nepal.
Methods:
Over a period of 3 months from September to November 2018, a total of 183 wound exudates and pus samples were collected and analyzed by standard microbiological procedures. Isolates were identified based on the colony characters, Gram staining and an array of biochemical tests. Antibiotic susceptibility testing was performed by Kirby-Bauer disc diffusion technique according to criteria set by CLSI, 2016. Methicillin resistance in Staphylococcus aureus was tested with the help of cefoxitin using disc diffusion method.
Results:
Out of the 183 samples, 149 (81.4%) were culture positive. Among 13 different isolates identified, S. aureus (43.0%) was predominant followed by E. coli (14.0%). Higher incidence of bacteria was seen among the males (52.3%), in the age group 51 to 60 years (26.8%) and among the patients undergoing surgical intervention to deal with cancer (34.2%). The prevalence of wound infection was significantly affected by gender, age, and treatment regimen (P < .01). Out of the total 68 S. aureus isolates, 38 (44.1%) were deemed as Methicillin-resistant Staphylococcus aureus (MRSA). Among the 158 isolates, 85 (53.8%) were multi-drug resistant (MDR). Cefepime was the most effective antibiotic for Gram positive isolates whereas both imipenem and meropenem were found to be equally more effective for Gram negative isolates.
Conclusion:
This study suggests that patients with malignancies harbor pathogenic bacteria; therefore, prudent use of antibiotics is essential to prevent the emergence of MDR pathogens.
Introduction
Cancer, an expansive term used to describe a plethora of diseases, is an abnormal condition in which the cells of the body divide and spread at an alarming rate. With an estimated 8 million deaths and 32 million cases diagnosed in between 2011 and 2015 and 14 million infected individuals worldwide in 2012 alone cancer is the leading cause of mortality and morbidity and warrants serious investigation and intervention in a global scale.1-3
Over a hundred types of cancer are recognized by the National Cancer Institute. 4 Just like the disease, treatment of cancer is also highly unique and is provided based on the needs of the patients, the tumor size, location of the tumor, and also the stage of the disease progression. Patients’ general health and wellbeing are also taken into consideration and their preferences for the options are available. 5 Some treatment measures, especially chemotherapy and radiation therapy, prevent the bone marrow from making blood cells that are essential for fighting microbes increasing the chance of developing an infection.6,7
In medicine, a wound is a form of physical trauma caused either due to puncture of the skin or due to blunt force. 8 An infection, however, is the successful invasion and proliferation of healthy tissue of the body resulting in the formation of pus. The wound can be colonized by a wide array of organisms and is influenced by factors such as a type, depth, location, and level of tissue perfusion and also the antimicrobial efficacy of the host immune response. 9 In cancer, infection is mostly associated with surgery, seen in 2.0% to 20.0% of the cases, and fungating tumors, characterized by leaking ulcerative lesions with an unpleasant smell, bleeding, and itching.10,11 Infection is the most important cause of complications in cancer and infection caused by antibiotic resistant microbes results in prolonged hospital stays and more expensive treatment.12,13
Among cancer patients, the wide prescription of the broad-spectrum antibiotics as prophylaxis has altered the composition of normal flora and resulted the emergence of arrays of multi-drug resistant (MDR) pathogens including methicillin-resistant Staphylococcus aureus (MRSA), vancomycin-resistant Enterococci (VRE).14,15 Many unusual pathogens infect patients with underlying immunodeficiencies, especially patients with hematological malignancies with some of them assuming increasing importance in cancer. 16 Knowledge of infectious etiology and appropriate antimicrobial agent can significantly improve the treatment but this information is not easily available in Nepal. Hence this study aimed to investigate the drug resistance patterns of microbes infecting wounds in patients with underlying malignancy and determine any significant association between various possible risk factors.
Materials and methods
MDR organisms were differentiated based on their ability to resist 3 or more classes of antimicrobial agents among the 6 major classes used in the study. 20 Methicillin resistance in S. aureus was tested with the help of cefoxitin using disc diffusion method and classification was done based on CLSI guidelines. 18 These drugs were selected based on the prescription frequencies and availability in the study area. In order to monitor quality (potency) of disks, a standard strain of S. aureus (ATCC-25923) and E. coli (ATCC-25922) were tested at regular interval and whenever new batches of antimicrobial discs were used.
Results
Distribution of bacterial isolates
Out of the total 81.4% (149/183) growth positive samples, mono bacterial growth was noted in 94.0% (140/149) samples, while the remaining 6.0% (9/149) samples showed poly bacterial growth, bringing the total number of isolates to 158. Among the total 158 bacterial isolates, Gram positive bacteria were predominant with 101 (63.9%) isolates, while Gram negative isolates made up 36.1% of total isolates. In total, 13 different types of bacterial isolates were identified among which S. aureus (43.0%) was predominant, followed by E. coli (13.9%) (Figure 1).
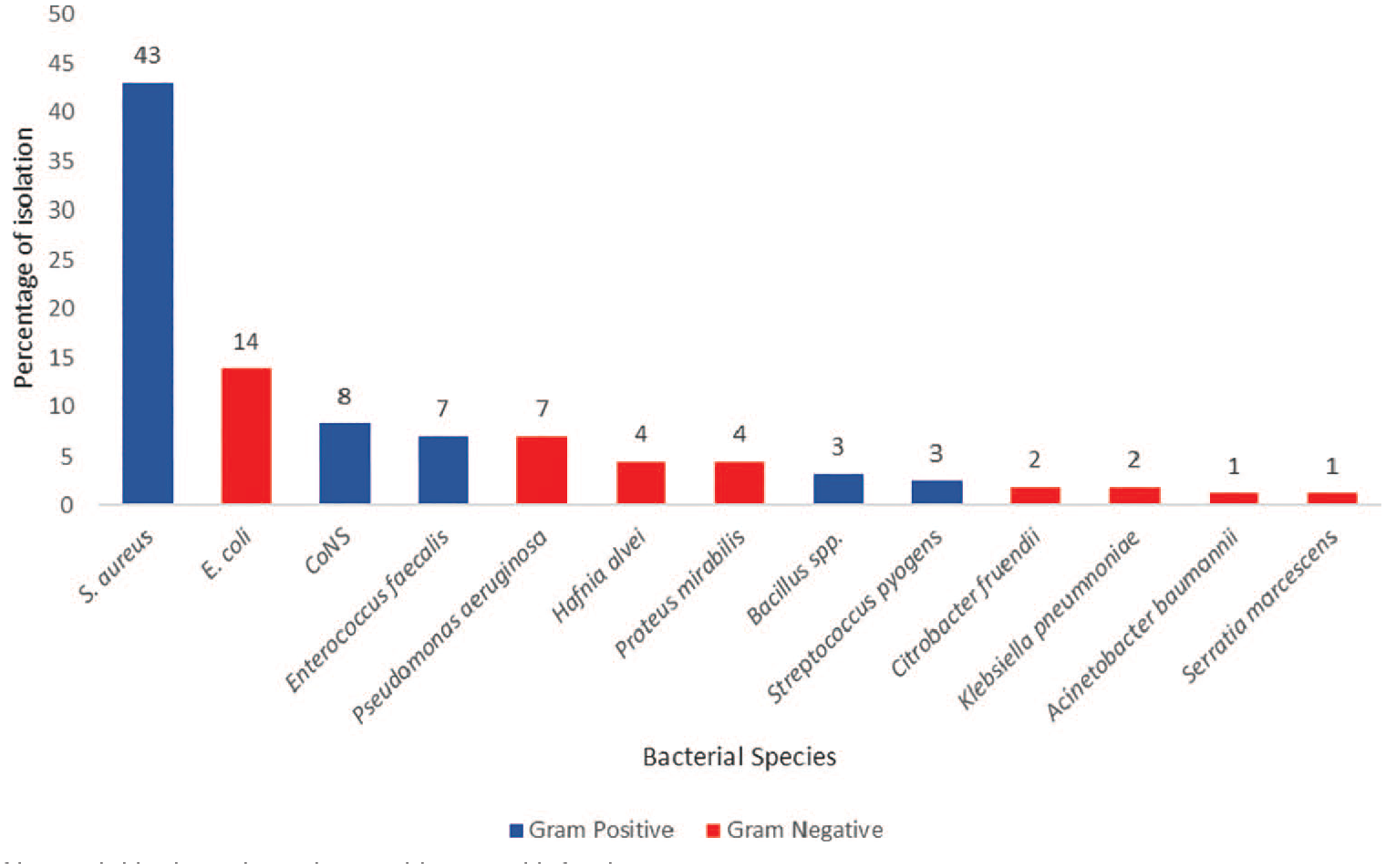
Frequency of bacterial isolates in patients with wound infection.
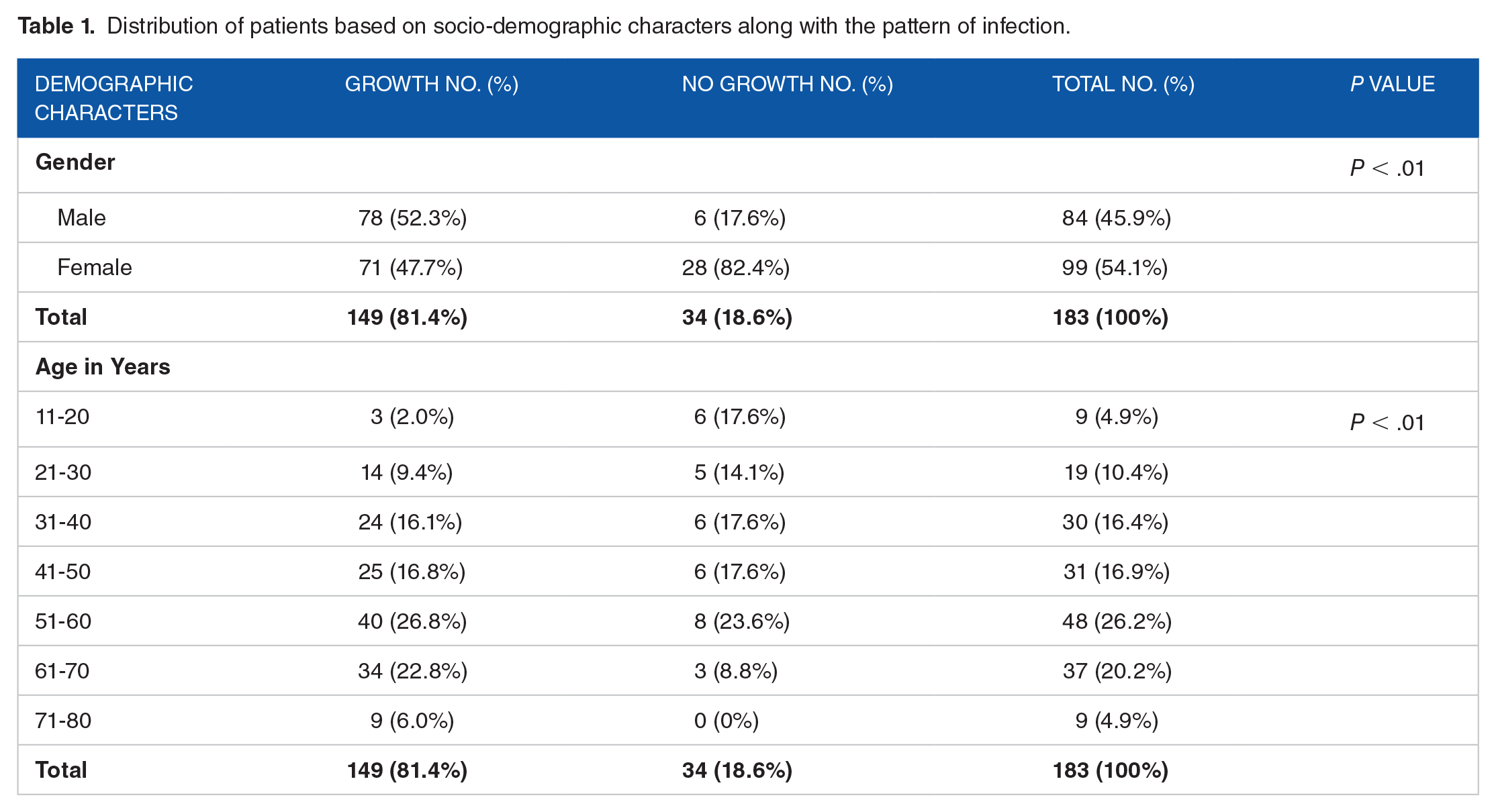
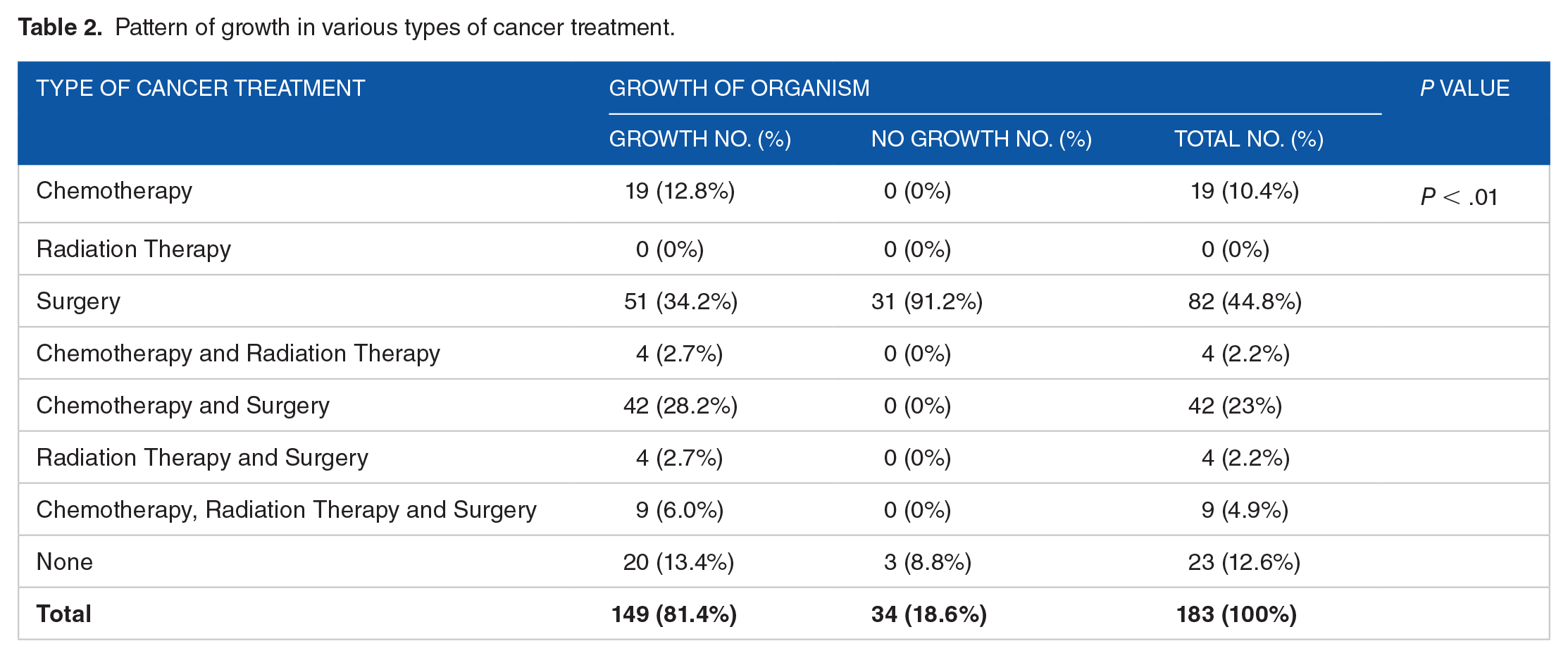
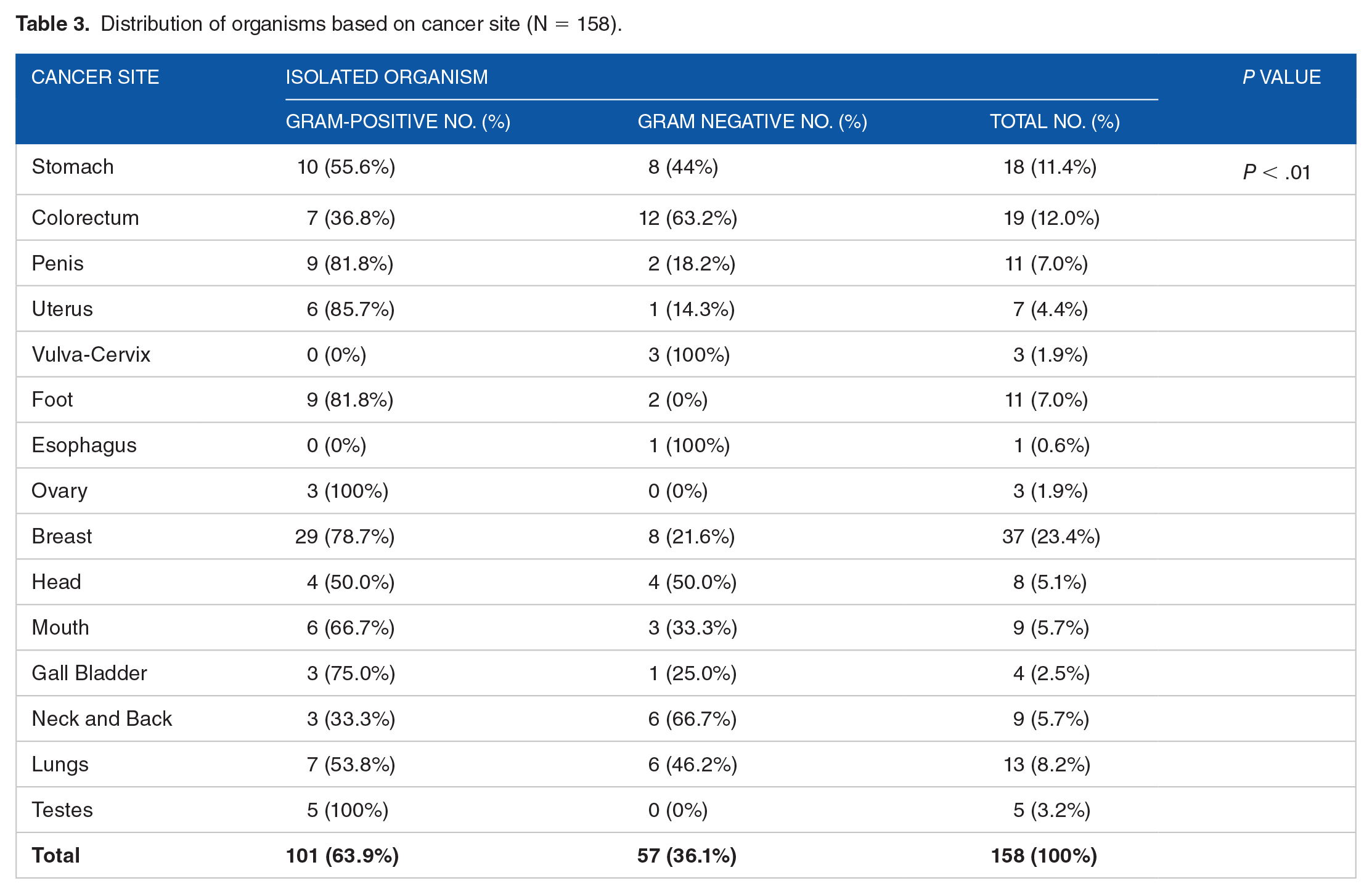
In terms of gender-wise distribution, it was noted that although the sample distribution ratio of male to female was 0.84:1, the growth positive ratio of male and female was 1.09:1 (Table 1). In this study pus sample and wound exudates were collected from patients ranging in age from 10 to 80 years old. The highest growth was seen in group 51 to 60 followed closely by 61 to 70 and then 41 to 50 (Table 1). A high proportion of growth was seen among patients undergoing cancer treatment. Out of 149 growth positive samples, the highest proportion (34.2%) of the sample was collected from patients who opted for surgical intervention. The second highest number of positive specimens belonged to the patients who received combination treatment for chemotherapy and surgery. Out of the growth negative samples, 91.2% were collected from patients who received surgical treatment (Table 2). Among the 158 total isolates, the largest proportion of the organisms was isolated from the breast (23.4%) among which 29 (78.4%) were Gram positive and 8 (21.6%) were Gram negative. A significant correlation was noted between the incidence of bacterial isolation with the site of cancer (P < .01) (Table 3).
Distribution of patients based on socio-demographic characters along with the pattern of infection.
Pattern of growth in various types of cancer treatment.
Distribution of organisms based on cancer site (N = 158).
Antibiotic susceptibility testing
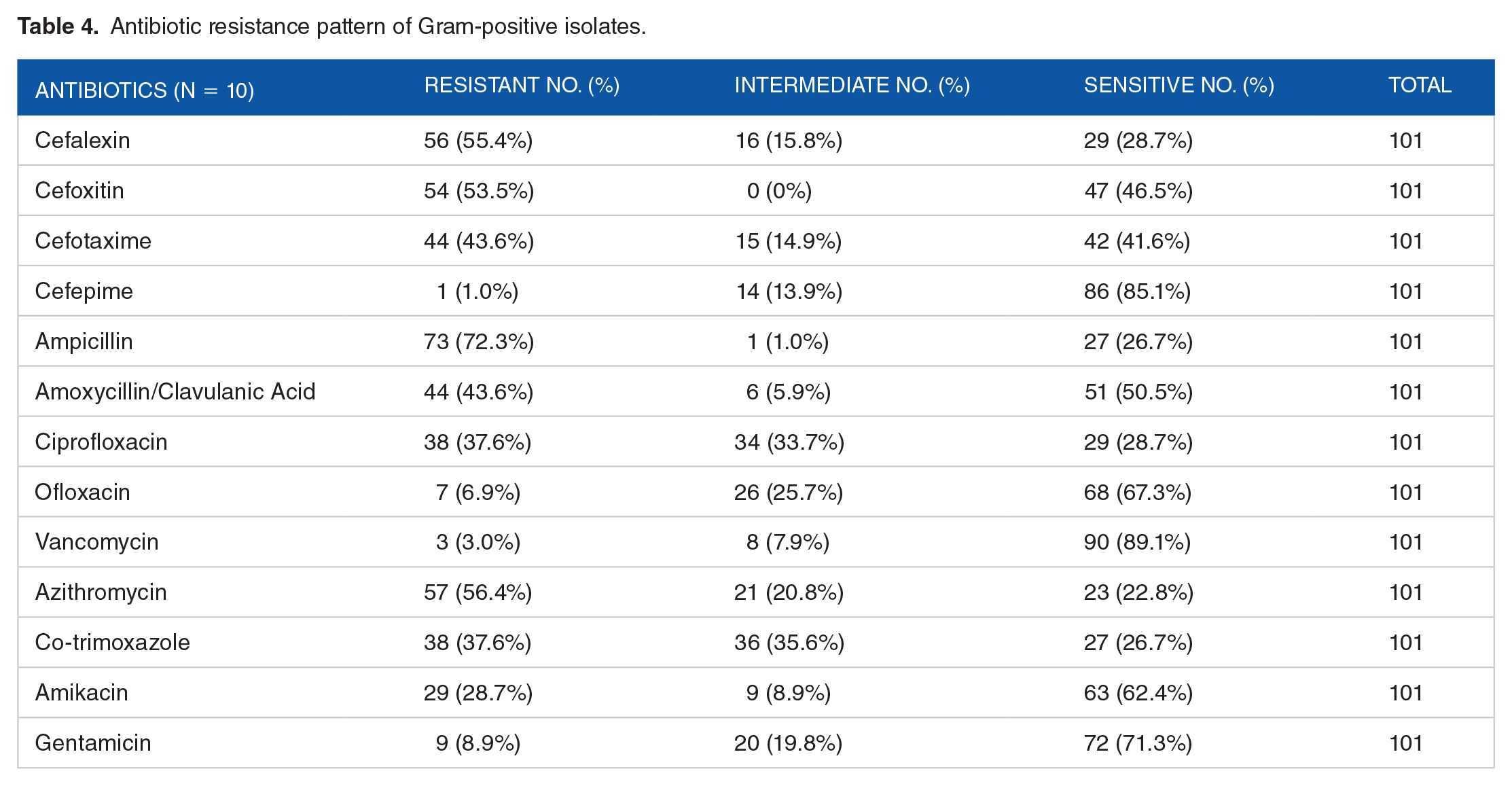
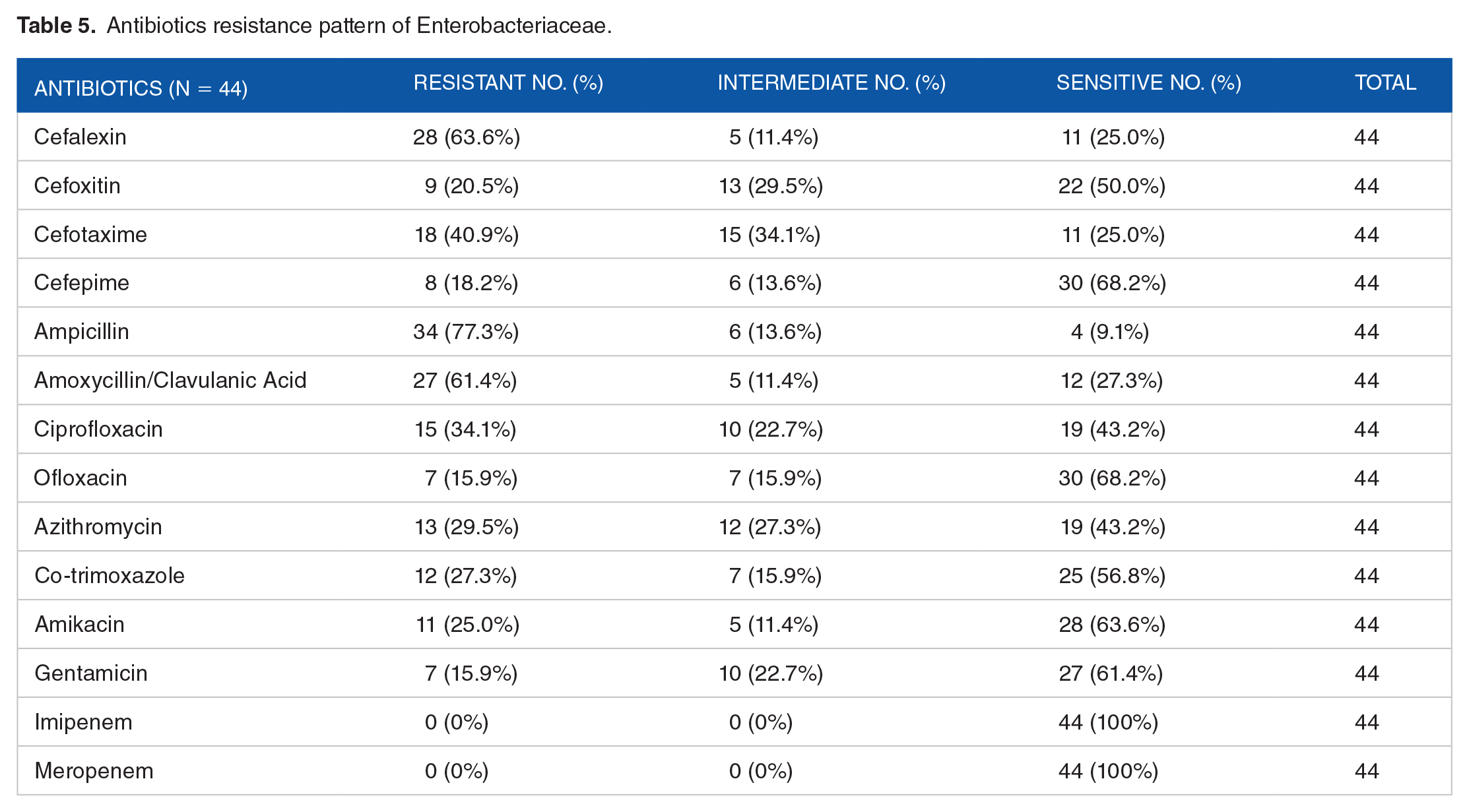
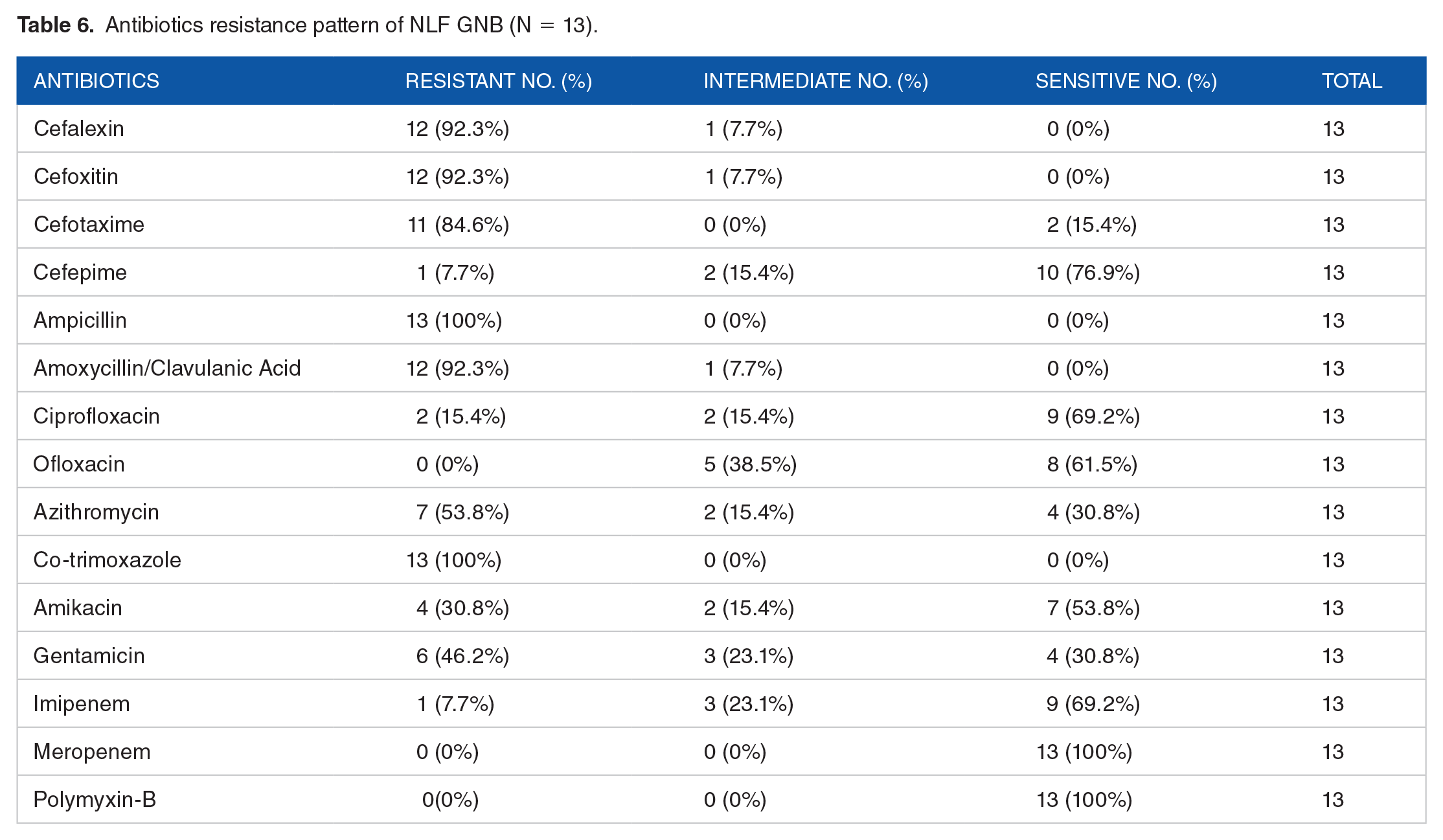
Among the 101 Gram positive isolates subjected to antibiotic sensitivity testing, the highest proportion of organisms showed resistance against ampicillin, with 73 (72.3%) isolates resisting the drug. Gram positive isolates showed the least resistivity toward cefepime (1.0%) (Table 4). Among total 68 S. aureus isolates, 55.9% (38) isolates resisted cefoxitin and were deemed as MRSA, while the rest 44.1% (30) were methicillin sensitive Staphylococcus aureus (MSSA) (Table 4). Out of 14 common antibiotics used against Enterobacteriaceae isolates, a high proportion of them resisted ampicillin (77.3%) followed by cefalexin (63.6%). Very low resistance was seen against ofloxacin 15.9% followed by cefepime 18.2%. None of the isolates resisted imipenem and meropenem (Table 5). Among various cephalosporins used against non-lactose fermenting Gram negative bacilli (NLF GNB), high degree of resistance was seen against cefalexin (92.3%), cefoxitin (92.3%), and cefotaxime (84.6%) while cefepime was found to be the most effective drug with only 1 (7.7%) isolate resisting it. Ofloxacin, meropenem, and polymyxin-B were found to be highly effective with none of the NLF GNB isolates resisting them (Table 6).
Antibiotic resistance pattern of Gram-positive isolates.
Antibiotics resistance pattern of Enterobacteriaceae.
Antibiotics resistance pattern of NLF GNB (N = 13).
Discussion
Out of the total 183 samples examined, growth was seen in 81.4% (149) samples and the remaining 18.6% (34) samples did not show any growth. Although the number of samples collected from the female was higher (54.9%), most of these samples did not show any growth and the final distribution of total culture positive samples (149) among males and females was fairly similar (52.3% and 47.7% respectively). The frequency with which infection occurred was higher among the males, which was statistically significant (P < .01). There is a high degree of variation between this and other studies both in terms of positivity rate. The result of this sample distribution rate is consistent with the result of the study by Masaadeh and Jaran, with 52.2% male and 47.8% females among the total 115 growth positive samples. 21 A different picture was seen in a study by Rolston and his associates, with females accounting for 61.0% of the total cases while males accounted for just 39.0%. 22
The variation in positivity rate may be due to the difference in cultural techniques, sampling procedure and some underlying conditions such as diabetes and the stage of cancer. Use of self-prescribed prophylactic antibiotics might have further contributed to this. The disparity between the sample collection ratio and growth positivity ratio of male and female may be due to the fact that men are involved in certain occupations that increase the risk of trauma and infection. This coupled with the fact that many of the females in this study were being treated for breast cancer which is dealt with surgery along with antibiotic therapy can explain the gap.
Although samples were collected from a diverse age group stretching from 10 to 80, most of the participants in the study were aged 40+. Furthermore, infection was most commonly seen in the age group 51 to 60. This result was statistically significant at 1% level of significance. In a study carried out by Raza et al in non-cancer patients, infection was most common in the age group 21 to 40. 23 However, Mukhtar et al reported an average age of 51 in their research among cancer patients with infection. 24 Since the sample for this study was collected exclusively from patients with underlying malignancies, a shift was seen in the age group that highlighted the older generation. This is in par with a work of Vilar-Compte et al who showed the age ⩾58 greatly increases the risk of infection in cancer patients who have undergone surgery. 25
Out of 149 growth positive samples, only 6.0% (9) were poly-bacterial while a majority, 94.0% (140), were monomicrobial. S. aureus was the predominant organism of the poly-bacterial infection, while P. aeruginosa and E. coli shared the second position. There lies a high degree of variation between the results of this study and other similar studies. In a study by Rolston et al, polymicrobial infections accounted for 31.0% of the cases in surgical site infection (SSI) associated with breast cancer, 22 whereas another study on pus sample of non-cancer patients also recorded multiple growths in 31.5% of cases. 26 This gap in isolation and identification of polymicrobial infection can be accounted to the fact that most of the patients attending the minor OT have had some form of antibiotic therapy. This coupled with the fact that only aerobic organisms were cultured, leaving out the anaerobes which make up a large portion of the isolates found in infection, may explain the reason for the low polymicrobial count. 27
In this study, the infection was seen mostly in the cases with combined cancer therapy, signifying that this form of combined treatment makes an individual more susceptible to various infections. Lower positivity rates of culture among patients who had only surgical interventions may be explained by the fact that these patients were under antibiotic therapy and had no other intervention in place that could reduce their immune response.
In the present study, a total of 158 isolates were observed among which 101 (63.9%) were Gram positive, whereas the remaining 57 (36.1%) were Gram negative. As a whole, the most prevalent organism was S. aureus which was isolated 68 (43.0%) times and E. coli was the second most isolated at 13.9%. A similar pattern of bacterial isolation was seen in different studies throughout the world. In an Egyptian study conducted by Eldomany and Abdelaziz, regarding the characterization and antibiotic susceptibility of Gram negative isolates, it was found that E. coli was the most common isolate (30.0%) followed by P. aeruginosa (24.0%) and Acinetobacter baumannii (18.7%). 28 In another study, Mukhtar et al 24 found organisms like E. coli, P. aeruginosa, Serratia marcescens, A. baumannii, Proteus sp. Enterobacter, Citrobacter sp. etc. but the most commonly isolated organism was S. aureus (30). Separate studies by Rolston et al, Bhat et al, and Uzuka et al also confirmed these findings.22,29,30
High prevalence of S. aureus may be due to its distribution in the human body. Other normal flora like E. coli, K. pneumoniae, Citrobacter sp. were also commonly found in various cases of infection. These GNB are commonly found in the GI tract of the humans and prevent overgrowth of common organisms. Particularly in neutropenic patients, frequent use of antibiotics disrupts this delicate balance and can lead to overgrowth of such organisms. Organisms like P. aeruginosa and A. baumannii were also isolated commonly due to their innate ability to resist a plethora of antimicrobial agents, providing it an opportunity to grow, where it would normally have out-competed.
Out of the 158 organisms isolated, 37 (23.4%) were from the patients with breast cancer. Majority of the organisms isolated from this site were Gram-positive (78.4%). Other sites with high infection load were stomach and colorectal cancer at 18 (11.4%) and 19 (12.0%) respectively. Compared to other sites these sites had a higher number of Gram negative isolates at 8 (44.4%) and 12 (63.2%) respectively. A significant relation was observed between the site of cancer and isolation of organism (P < .01).
In another study that looked at the prevalence of organism based on the site of cancer similar result was seen. 22 Higher prevalence of Gram negative isolates in cases of colorectal cancer and stomach cancer isn’t surprising as the gastrointestinal region of the human digestive tract is colonized primarily by Gram negative isolates. In case of breast cancer, colonization of surgical or fungating wound by the normal flora of the skin, most commonly Gram positive isolates like S. aureus, may have led to increased isolation of these organisms.
The most effective antibiotic for Gram positive organism in this study was vancomycin (89.1%) followed by cefepime (85.1%), gentamicin (71.3%), ofloxacin (67.3%) and amikacin (62.3%), whereas azithromycin (22.8%), ampicillin and co-trimoxazole (26.7%), ciprofloxacin and cefoxitin (28.7%) had the lowest efficacy. None of the S. aureus isolates were resistant to vancomycin which is consistent with previous works, as most of the studies have shown that drugs like vancomycin and gentamicin have high efficacy but azithromycin, ampicillin, and co-trimoxazole have lower efficacy.31-33
A total of 55.9% of the S. aureus isolates resisted cefoxitin and were Oxacillin-resistant and hence termed as MRSA. Distribution of MRSA in the present study was slightly higher than other studies, as studies by Rolston et al and Bhat et al both recorded a MRSA isolation rate of 40.0%.22,29 The Gram-negative isolates exhibited a high degree of sensitivity toward imipenem (93.0%) and cefepime (70.0%). Ampicillin was the least effective drug for treating Gram-negative infection as 82.5% of isolates resisted it. A high degree of resistance was seen against the first 3 generations of cephalosporins.
Polymyxin-B and meropenem were the most effective antimicrobials for NLF GNB. A high degree of sensitivity was also seen toward imipenem, cefepime, and ciprofloxacin. Ampicillin and co-trimoxazole were ineffective for NLF GNB infections. The efficacy of the first 3 generations of cephalosporins was also minimal. These results are consistent with a study carried throughout the world by Eldomany and Abdelaziz which showed that these pathogens were most sensitive to ciprofloxacin, meropenem, and imipenem while they showed the lowest sensitivity toward ampicillin, cefotaxime, and cefoxitin. 28
Isolates resistant to at least 3 classes of potentially effective anti-microbials were considered MDR in the study. 20 In this study out of 158 bacterial isolates, 87 (55.1%) organisms were found to be MDR. Among the MDR organisms, Gram-positive isolates accounted for 60.0% while Gram-negative isolates accounted for the remaining 40.0%. All of the NLF GNB organisms (P. aeruginosa and A. baumannii) were MDR. A similar pattern of MDR was seen among other studies conducted in Nepal and in other countries. In an Ethiopian study by Hailu et al, MDR was observed in 54.3% of total cases. A similar prevalence of MDR was observed among S. aureus (48.0%) and E. coli (63.6%) in the study. 34 In a study by Mahat et al in Nepal, MDR was seen in 62.3% of the cases, while 96.0% of A. baumannii and 68.0% of P. aeruginosa were MDR. 35
As compared to other studies, a higher degree of resistance was shown by the isolates in the present study. Patients with the underlying condition of malignancies are constantly subjected to antibiotic prophylaxis and treatment that can lead to the different patterns of sensitivity among the isolates observed.
Conclusion
The main culprit of wound infection was S. aureus followed by E. coli, CONS, and E. faecalis. MDR was shown by 53.8% isolates and 56.0% of the S. aureus isolates were MRSA. Infection was most commonly seen in patients undergoing treatment especially among those who opted for surgery. Therefore, regular monitoring of MDR and MRSA pathogens should be done among the clinical isolates not only for therapy but to monitor the spread of resistant organisms throughout the hospital and community. Cancer and its treatment predispose an individual to infection; hence proper prophylactic measures should be designed based on studies like this. Anaerobic culture and molecular characterization of the isolates are further recommended.
Footnotes
Acknowledgements
The authors are grateful to the Department of Microbiology, B.P. Koirala Memorial Cancer Hospital (BPKMCH), Chitwan, Nepal for providing laboratory facilities and guidance to complete the study. We are thankful to the patients and their parents to support in the study.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
SA planned and designed the study. KD performed the laboratory experiments. KD, SK, SS and PS wrote the manuscript and SA revised it. All authors read and approved the final manuscript.
Availability of Data and Materials
All the data obtained during this study are available within the article.
Ethics approval and consent to participate
This study was conducted after obtaining ethical consent from National Health Research Council. Permission to carry out the work was obtained from the research management committee of BPKMCH. Written informed consent was also pursued from patients or guardians of children and any information was kept confidential. All laboratory tests were done free of charge and their results were communicated to the patient’s respective physicians or nurses for beneficiary measures.
