Abstract
Objective:
The aim of this study was to assess physician assistant students’ knowledge about the screening, transmission, management, and prevention of Zika virus infection.
Background:
It is important for health care providers in the United States to recognize the symptoms of Zika so that they can screen, diagnose, and or treat persons exposed to or infected by the virus. Physician assistant students, on completion of their educational program and passing their board examinations, provide care for patients in primary care or specialty settings where they may treat patients who either have the virus or post-virus exposure.
Methods:
A convenience sample of 37 students enrolled in a physician assistant studies program in the Midwestern United States completed an in-person self-administered paper-and-pencil questionnaire that tested their knowledge about Zika virus infection.
Results:
All the respondents knew that the disease is of viral origin; however, only 89% knew that mosquitoes were the natural host. Primary modes of transmission were identified as sexual contact and blood transfusion (47% and 44% of respondents respectively); 47% incorrectly identified amniotic fluid as a transmission mode. More than half (61%) knew that health care providers should ask pregnant women about any possible virus exposure before and during pregnancy at each prenatal visit. Most respondents knew that muscle/joint pain (67%) was one of the symptoms of Zika infection, but only 39%, 25%, and 19% also identified low-grade fever, maculopapular rash, and conjunctivitis respectively as other symptoms. Some participants incorrectly identified antivirals (44%) and nonsteroidal anti-inflammatory medications (36%) rather than the recommended treatments of pain relief (30%) and fever relief (42%) medications for clinical management of the disease.
Introduction
Since the 2015 Zika virus outbreak, approximately 10% of babies born to women with confirmed infection during pregnancy had Zika-associated birth defects.
1
Unlike other infectious diseases such as Ebola and Dengue fever, which have similar symptoms, exposure to Zika in pregnant women or women of childbearing age can lead to microcephaly in their newborns.
1
Mosquitoes primarily the
Early recognition of symptoms of the virus by health care providers is important to ensure that appropriate diagnostic tests are done, resulting in prompt diagnosis and effective treatment for persons who are infected. DeSmet et al 4 recognized that the challenge for clinicians is to identify patients while they are still in the acute phase of the infection. Providing appropriate education to sexually active persons and their partners about the transmission and prevention of Zika also plays a key role in stopping the spread of this infection.
Health care providers such as physician assistants provide care to patients in a variety of settings including primary care clinics or offices, hospitals, nursing homes, and others. Physician assistants diagnose and treat patients for an array of diseases and frequently encounter patients who have flu-like symptoms common to many infectious illnesses such as Zika.
There is limited research on health care providers’ knowledge about Zika infection. In a rapid assessment of the Zika virus, Yung et al 5 found that Singapore physicians’ knowledge of sexual transmission recommendations and the management of congenitally infected infants is very limited. Another study specific to nurse practitioners done using a paper-and-pencil format to survey a convenience sample of 559 nurse practitioners reported significant knowledge gaps in identifying and diagnosing a Zika infection. 6 Furthermore, Moore 6 showed no statistically significant differences between those who were practicing in high-risk areas and those who were not in relation to their knowledge about the virus. Due to rapid scientific changes and recommendation updates, it is important to continue to assess health care providers’ knowledge about Zika virus.
As part of their education, physician assistant students learn to diagnose and treat illnesses and diseases, such as the Zika. This pilot study was done to assess physician assistant students’ knowledge about Zika, as it is important for this group of providers to determine if a patient with flu-like symptoms may have Zika or another condition.
Methods
This pilot study used a cross-sectional research design that examined a convenience sample of individuals enrolled in a Physician Assistant program at a university located in the Midwestern part of the United States. The questionnaire was a modification of the survey instrument used in the Yung et al’s 5 research that examined Singapore clinical specialists’ knowledge on Zika virus. Permission was obtained from the survey’s author(s) before modification of the instrument. The modifications made were to help assess and capture specific information about the US physician assistant students’ knowledge on the screening, diagnosis, and treatment of Zika virus. The Institutional Review Board of the institution gave approval prior to the start of the study.
The survey instrument consisted of 23 questions, which included five multiple-choice responses with one correct answer, along with 18 questions with a “select all that apply” response format, which meant that more than one answer was required. Fifteen demographic items were included in the questionnaire. The questionnaire was not designed to be an exhaustive query about Zika virus, but to capture physician assistant students’ knowledge about the virus in four domains: (1) virus transmission and prevention, (2) clinical knowledge of diagnosis and management, (3) clinical treatment of persons possibly infected with the virus, and (4) CDC recommendations for screening for Zika virus infection.
Face validity was established for the original instrument through a comprehensive literature review of previous studies that examined health care providers’ knowledge of Zika virus. Moore 6 described only face validity in the survey of nurse practitioners. Content validity was re-established by having six content experts review the questionnaire and provide feedback on the instrument items. 7 Face and content validity were re-established for the modified instrument prior to using it in this study. Revisions were made to the questionnaire based on feedback from the content experts.
The questionnaire was administered to the participants in person, by providing each individual with a paper copy of the survey and a pencil. Descriptive statistics (frequencies and percentages) and nonparametric Kruskal-Wallis
Results
Sample characteristics
The questionnaire was administered to a cohort of 37 first-year physician assistant studies students during one class session. Of the cohort, 36 students completed the questionnaire, which resulted in a response rate of 97%. Most of the respondents were non-Hispanic (74%, n = 26) whites (63%, n = 22), females (58%, n = 21), younger than 30 years old (78%, n = 28), and who had earned a bachelor’s degree (83%, n = 30), as outlined in Table 1. The respondents were mostly Ohio residents (68%, n = 25), currently employed in an urban health care setting (56%, n = 15), and in acute care (46%, n = 12). Approximately, 72% (n = 26) indicated that they had previously provided direct care to patients in the United States, with 1 to 5 years (33%, n = 12) being the most common response for the number of years participants had provided direct care to patients in the United States. In addition, one respondent indicated having 21 to 30 years’ experience providing care to patients, which reflected that students had prior exposure and experience in other health care fields before enrolling in the physician assistant studies program. Furthermore, 9% (n = 3) of the respondents had cared for an adult patient with symptoms and/or exposure to Zika, and 6% (n = 2) had cared for an infant and a child with symptoms and/or exposure to this virus. When asked where they received most of their information about Zika, the majority identified television (44%, n = 10), then social media (39%, n = 9) as their sources of information as shown in Figure 1.
Demographics and characteristics of the respondents and Kruskal-Wallis
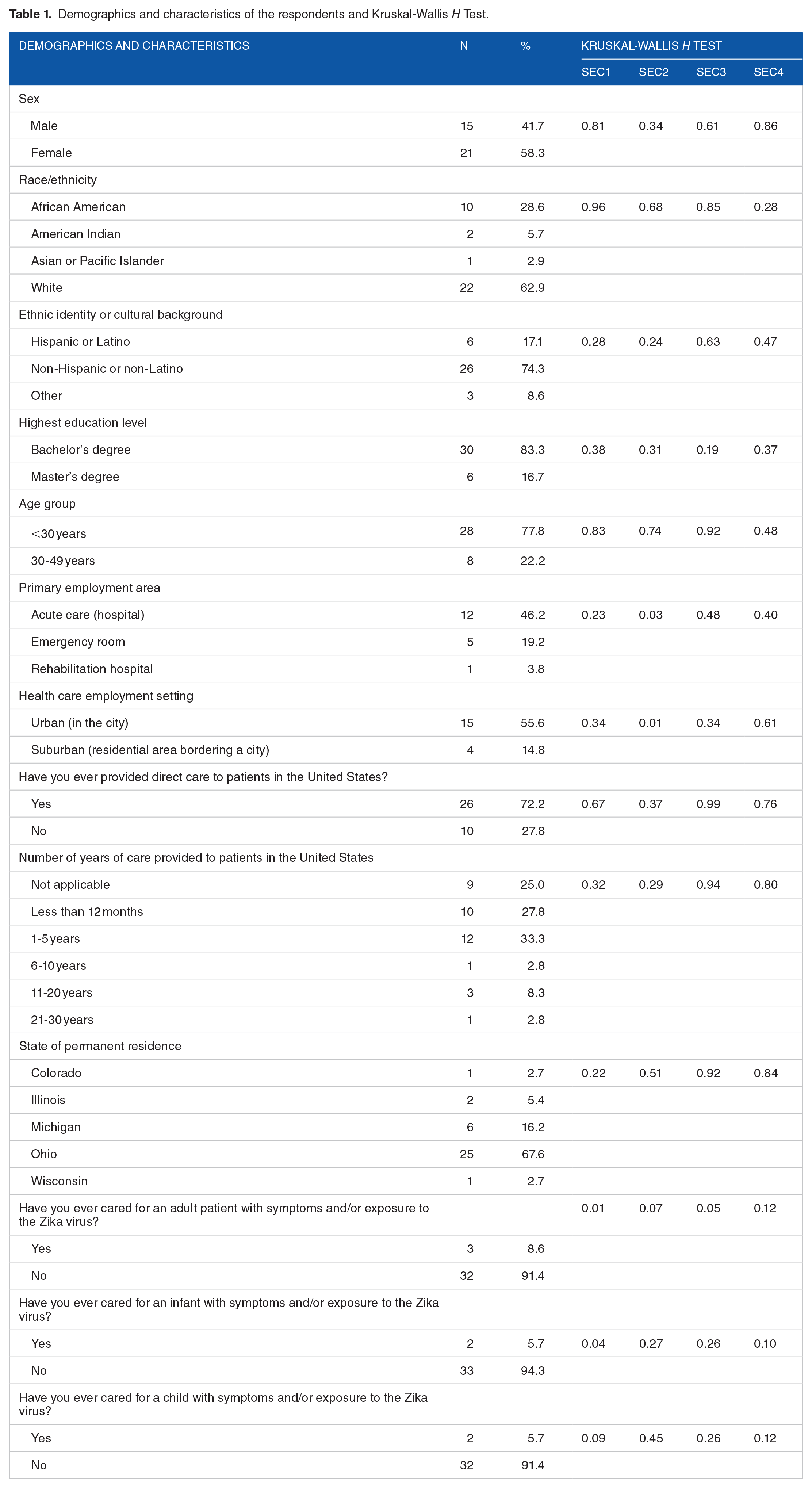
N = 36. Percentages may not equal 100% due to rounding and/or non-reported answers. SEC1: Knowledge on the Epidemiology, Transmission, and Symptoms of the Zika Virus; SEC2: Knowledge on the Risks, and Screening Recommendations and Testing of the Zika Virus; SEC3: Knowledge on the Clinical Management of the Zika Virus; SEC4: Knowledge on the Risks and Guidelines for Pregnant Women to the Zika Virus.
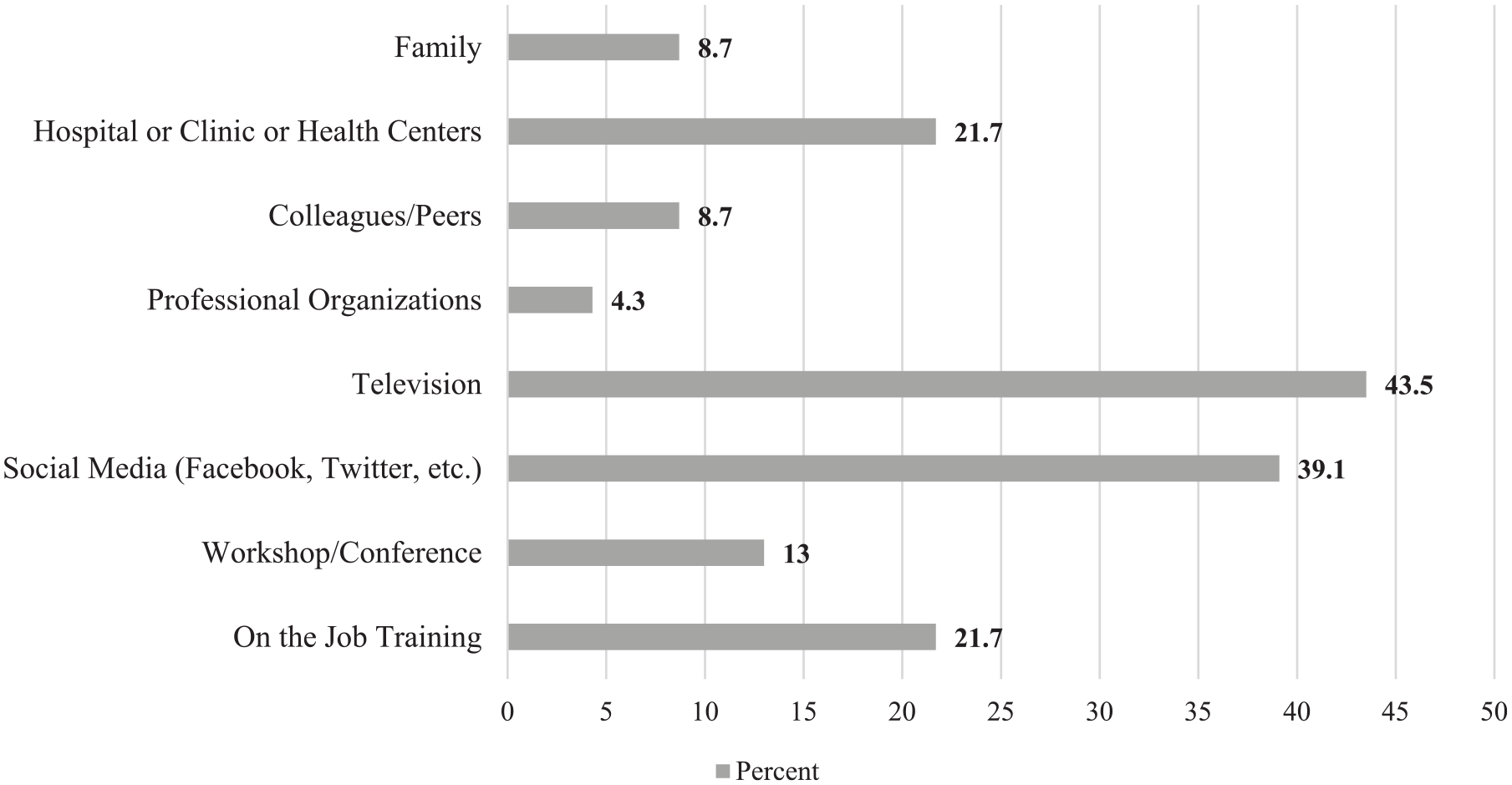
Physician assistant students’ response to where they receive information about the Zika virus.
Descriptive analysis
Identifying physician assistant students’ knowledge of the epidemiology, symptoms, and transmission of Zika virus was the focus of the first several questions in the survey as referenced in Table 2. Most respondents (56%, n = 20) did not know that
Response to survey questions on physician assistant students’ knowledge on the epidemiology, transmission, and symptoms of the Zika virus.
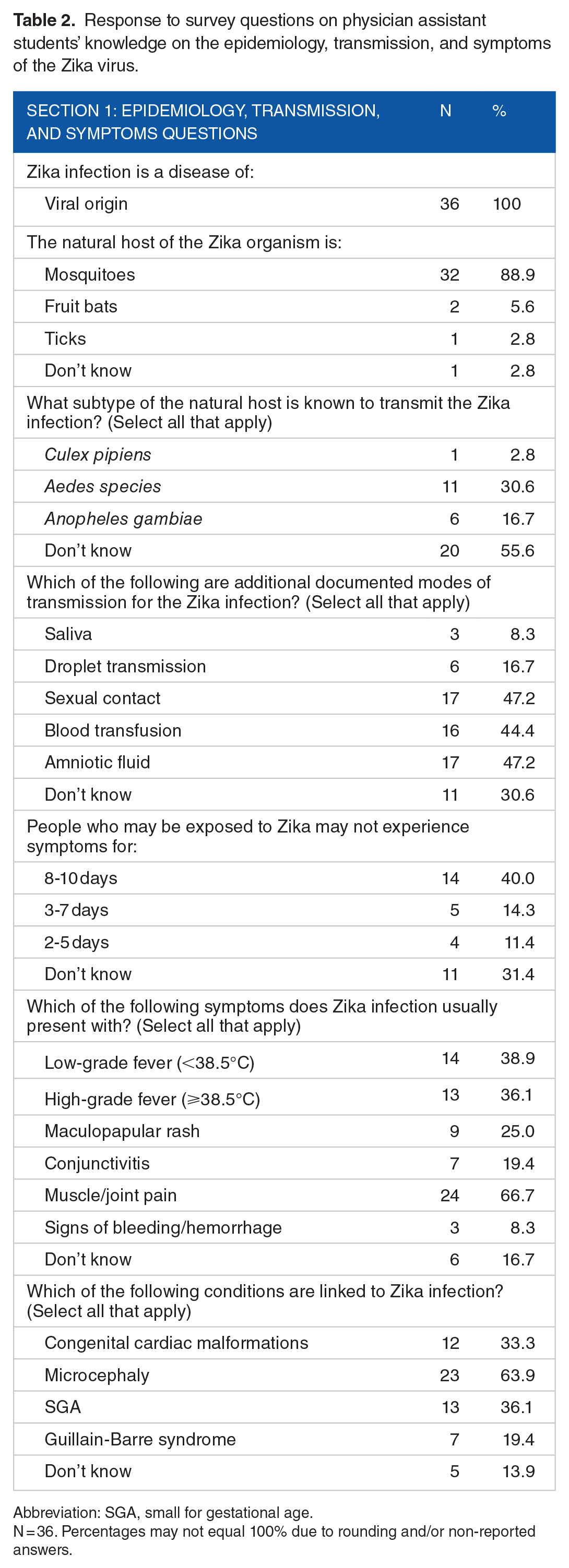
Abbreviation: SGA, small for gestational age.
N = 36. Percentages may not equal 100% due to rounding and/or non-reported answers.
Responses outlined in Table 3 focused on identifying participant’s knowledge related to the risks, and screening recommendations and testing for the Zika. Pregnant women (83%, n = 30), women of childbearing age (42%, n = 15), and children between the ages of 0 and 14 years (33%, n = 12) were identified as being at the most risk of harm from infection. Respondents recognized that symptomatic pregnant women with possible exposure to the virus (67%, n = 24) and those with no symptoms but with ongoing exposure (53%, n = 19) should be tested for the virus. In addition, respondents recognized that pregnant women with no symptoms but who were recently exposed (61%, n = 22) and those possibly exposed who have a fetus that has prenatal ultrasound findings consistent with congenital Zika virus syndrome (47%, n = 17) should consider being tested for the virus.
Response to survey questions on physician assistant students’ knowledge on the risks, screening recommendations and testing of the Zika virus.
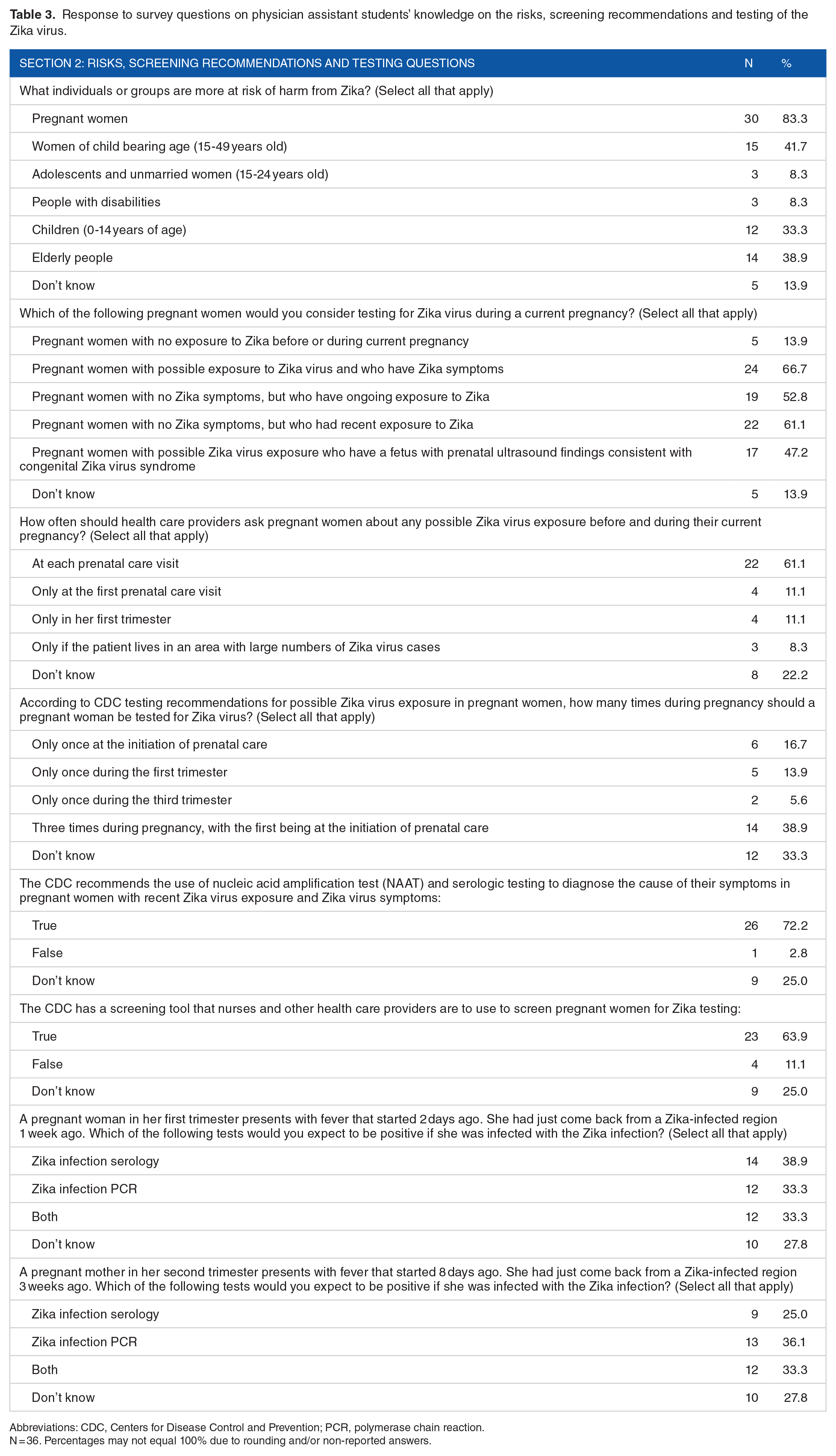
Abbreviations: CDC, Centers for Disease Control and Prevention; PCR, polymerase chain reaction.
N = 36. Percentages may not equal 100% due to rounding and/or non-reported answers.
More than half (61%, n = 22) of respondents answered that health care providers should ask pregnant women at each prenatal care visit about any possible Zika exposure that may have occurred before and during pregnancy. Thirty-nine percent (n = 14) of respondents were aware that the CDC recommends that asymptomatic pregnant women should be tested for possible Zika virus exposure 3 times during their pregnancy, but 33% (n = 12) of the participants did not know this. Seventy-two percent (72%, n = 26) of participants were aware that the CDC recommends the use of nucleic acid amplification test (NAAT) and serologic testing to diagnose recent Zika virus infection in pregnant women. Furthermore, 64% (n = 23) of respondents knew that the CDC has a screening tool that nurses and other health care providers should use to screen pregnant women for Zika virus exposure. Both Zika virus serology and Zika virus infection PCR (polymerase chain reaction) (33%, n = 12) were identified as tests that will give a positive result if a pregnant woman in her first trimester presents with a fever after visiting a region with Zika.
Table 4 summarizes participants’ knowledge about the clinical management of Zika. Pain relief and fever relief medications (excluding nonsteroidal anti-inflammatory medications) and fluid rehydration were correctly identified by 31% (n = 11), 42% (n = 15), and 50% (n = 18) respectively of participants as options for the clinical management of Zika. Some participants incorrectly identified antivirals (44%, n = 16) and nonsteroidal anti-inflammatory drugs (36%, n = 13) as options for the clinical management of the infection. Approximately 26% (n = 9), 29% (n = 10), and 34% (n = 12) of the students correctly recognized saliva, cerebrospinal fluid (CSF), and amniotic fluid respectively as samples they would use to test for the virus. Fifty percent (n = 18) and 33% (n = 12) of respondents recognized that testing an infant or the umbilical cord serum for the infection and collecting infected CSF respectively are diagnostic tests for infants with microcephaly or intracranial calcifications who were born to women who traveled to or resided in an area with Zika infection while pregnant. Fifty-four percent (n = 19) of respondents did not know the clinical evaluation and laboratory tests that should be considered for infants with possible congenital Zika infection, while 29% (n = 10) correctly selected cranial ultrasound as one of their options.
Response to survey questions on physician assistant students’ knowledge on the clinical management of the Zika virus.
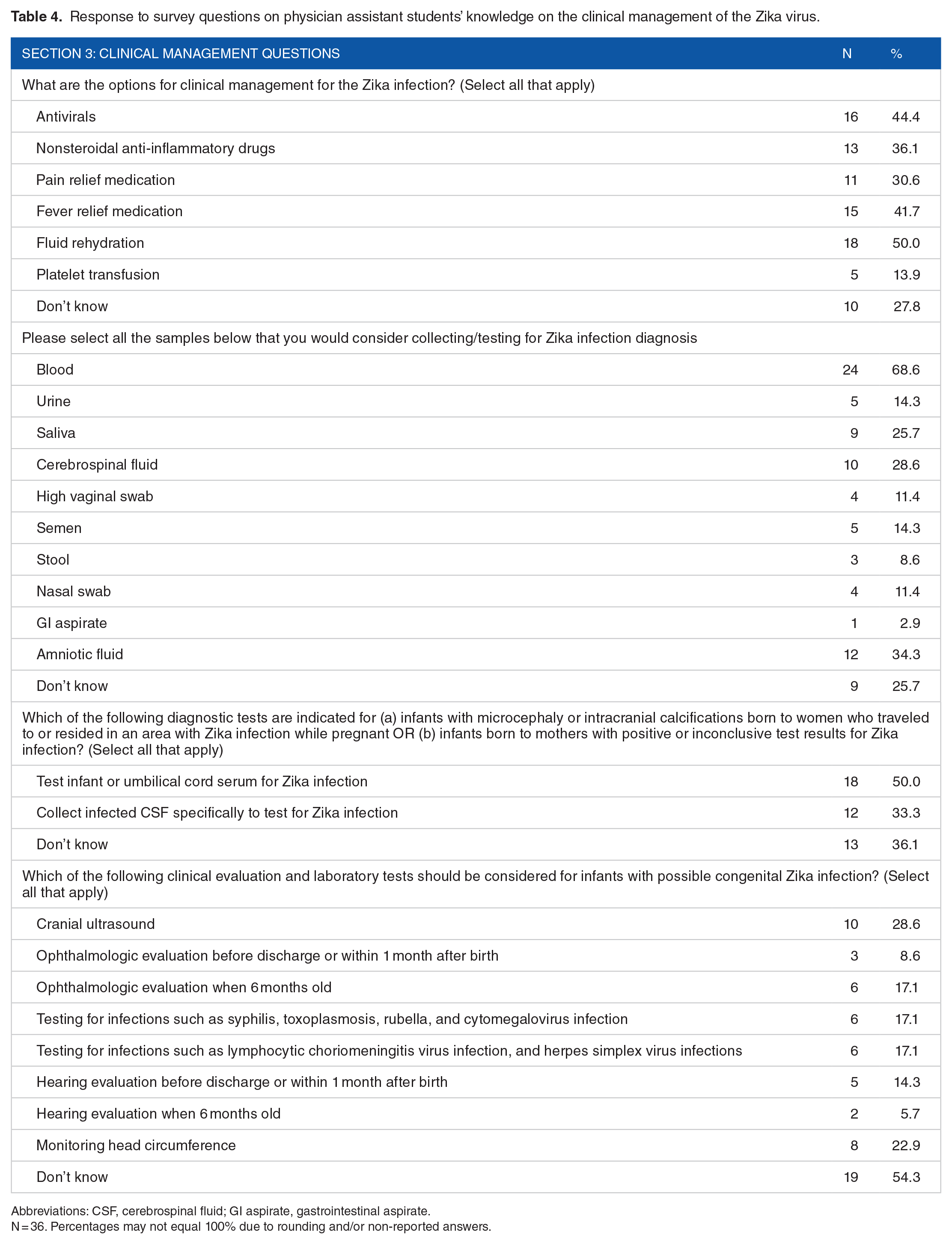
Abbreviations: CSF, cerebrospinal fluid; GI aspirate, gastrointestinal aspirate.
N = 36. Percentages may not equal 100% due to rounding and/or non-reported answers.
Miscarriage (60%, n = 21), abortion (29%, n = 10), medical complications (43%, n = 15), and being sick (40%, n = 14) were identified as risks to pregnant women who are exposed to Zika virus, as shown in Table 5. The risk of not growing or developing normally in the womb (26%, n = 9), miscarriage (43%, n = 15), being stillborn (26%, n = 9), being born with microcephaly (51%, n = 18), and being born with a disability (40%, n = 14) were identified as risks to the fetus or baby if a woman contracts Zika virus infection while pregnant. The use of insect repellent (60%, n = 21), wearing long-sleeved clothing and trousers (54%, n = 19), and staying in an air-conditional or screened-in room (37%, n = 13) were identified as CDC guidelines for pregnant women traveling to Zika-affected countries to lower the risk of transmission of the disease. Twelve percent (n = 4) of participants correctly identified that abstaining from sexual intercourse or using condoms appropriately throughout pregnancy is the CDC’s advice about sexual intercourse for pregnant women and their partners returning from a Zika virus–affected area. However, 70% (n = 23) of the respondents did not know these recommendations.
Response to survey questions on physician assistant students’ knowledge on the risks and guidelines for pregnant women exposed to the Zika virus.
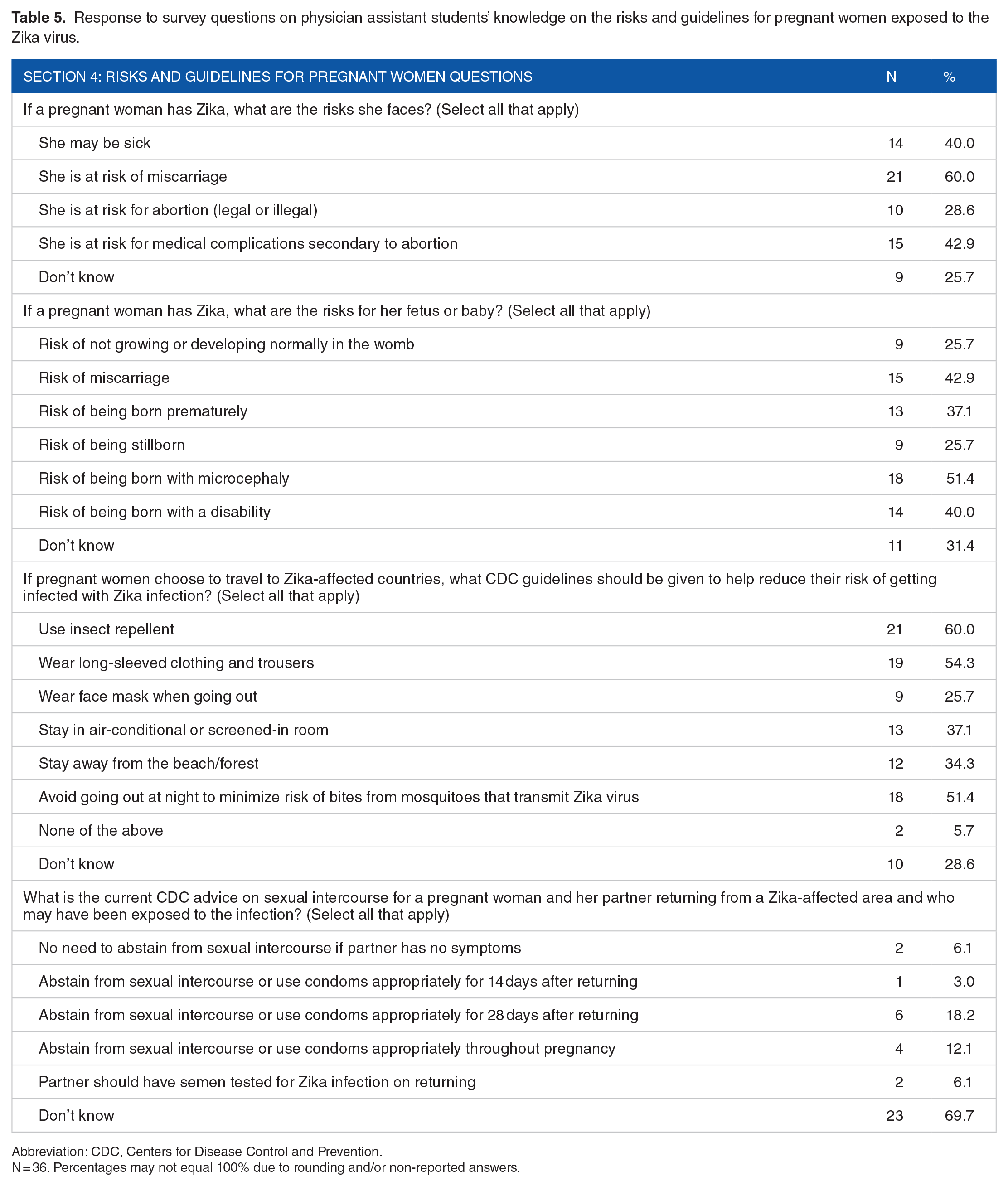

Abbreviation: CDC, Centers for Disease Control and Prevention.
N = 36. Percentages may not equal 100% due to rounding and/or non-reported answers.
Bivariate analysis
The bivariate analysis for each of the demographic characteristics and each group of knowledge questions is documented in Table 1. The Kruskal-Wallis
Physician assistant students’ knowledge of the epidemiology, and transmission and symptoms of the virus was also statistically significant based on whether or not participants had provided care for an adult with symptoms and/or exposure to the virus (
Discussion
This study explored physician assistant students’ knowledge of Zika virus, focusing on critical areas that health care providers and students should be aware of if they encounter patients with symptoms and/or exposure to the virus. Based on the results from this pilot study, students had limited knowledge of the epidemiology, transmission, risks, and screening recommendations and clinical management of the Zika virus. The demographic data of these students included residents from five states: Colorado, Illinois, Michigan, Ohio, and Wisconsin, with the majority being non-Hispanic whites from Ohio, employed in the acute care setting in urban settings.
This study revealed (see Table 2) that more than half of the participants were not knowledgeable of the specific species of mosquitoes that were vectors of the Zika virus (
Most participants knew that pregnant women were most at risk of harm; however, less than one third identified children between the ages of 0 and 14 years old as also being at increased risk of harm from Zika virus infection (Table 3). About two thirds of participants knew that pregnant women with possible exposure to Zika virus should consider testing for the virus. Less than half of the participants had knowledge of the CDC’s recommendations for asymptomatic pregnant women with ongoing risk of exposure to the virus to be tested at least 3 times during pregnancy for the Zika virus. Most participants knew that the CDC recommended using nucleic acid amplification test (NAAT) and serologic test for recent Zika exposure and or symptom onset for the diagnosis in pregnant women.
Half of the participants knew that fluid hydration is recommended for management of the infection. Less than half knew that pain relief and fever relief medications (excluding nonsteroidal anti-inflammatory medications) were other treatments. Almost half of the participants surveyed did not know that nonsteroidal anti-inflammatory medications are not options for clinical management of the Zika virus. The results in this study pertaining to the use of fluid hydration were different from those in Yung et al’s 5 study where 90% of respondents identified fluid hydration for the clinical management of symptoms. Respondents in Yung et al’s 5 study correctly identified fever relief (90%) and pain relief (82.7%) medications as other treatment options. The differences in the knowledge in these two groups may be attributable to many factors, with possibly the most important being that the participants in Yung et al’s 5 study were practicing physicians while respondents in this study are first-year students.
Participants’ responses to questions on the risks, and CDC’s recommendations for screening and testing for the Zika virus were statistically significant based on their primary area of employment and employment location. Those employed in a suburban setting had more knowledge in these areas. Participants’ knowledge of the epidemiology, transmission, and symptoms of Zika virus infection was also statistically significant based on whether or not they had provided care to an adult or infant with symptoms of Zika virus infection or exposure to the virus.
Students in this study lacked knowledge about CDC recommendations for screenings, as well as diagnostic tools for Zika virus. The natural host of the virus, identification of at-risk populations, and the symptoms of infection are also areas in which participants had limited knowledge. Most participants selected the television as their source of information about the virus, with social media being the second most frequently identified source of information. Professional organizations and journals were the least frequently selected source of information, which may highlight the importance of social media and television as sources of information.
Participants who had cared for adults or infants who either were exposed to the virus or had symptoms of the virus were more knowledgeable about the epidemiology, transmission, and symptoms of the virus than those without these experiences were. In addition, students who identified their primary place of employment as a suburban setting were more knowledgeable about the risks, and recommendations for virus screening and testing.
Limitations
The major limitation of this study is that the sample size is small, consisting of a convenience group of physician assistant students at a university in the Midwestern United States. Therefore, the findings from this study are not generalizable to other physician assistant studies students, but only to first-year physician assistant studies students of this institution. Another limitation relates to the lack of reliability data for the research instrument. Pilot testing the instrument before using it in a larger study is recommended. Another recommendation is to replicate this study with a national random sample of physician assistant studies students after the survey instrument has been pilot tested. Retesting this group of students as they get to the end of their program of studies to compare what they know or retain about Zika virus, as they get closer to caring for patients independently, should also be done.
Conclusions
This was the first study that examined a group of future health care professionals’ knowledge about Zika virus. This pilot study contributed baseline information about physician assistant students in one physician assistant studies program about their knowledge of Zika virus. Although the study did not present any new knowledge about the screening or management of the virus, it is valuable in that it was able to identify what one cohort of students who are future health care professionals know about various aspects of this virus.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
CW contributed to study design, identified study population, facilitated access to study population, assisted with writing and edits to manuscript. CT assisted with study and survey design, data collection, writing/editing of manuscript. LL assisted with study and survey design, performed all data analysis, contributed to writing and editing of manuscript. MW assisted with study/survey design, contributed to writing/editing of manuscript. MAB assisted with study/survey design, literature review, writing of manuscript. SL assisted with study design and data collection.
