Abstract
There has been tremendous breakthrough in the development of technologies and protocols for counselling, testing, and surveillance of resistant human immunodeficiency virus strains for efficient prognosis and clinical management aimed at improving the quality of life of infected persons. However, we have not arrived at a point where services rendered using these technologies can be made affordable and accessible to resource-limited settings. There are several technologies for monitoring antiretroviral resistance, each with unique merits and demerits. In this study, we review the strengths and limitations of prospective and affordable technologies with emphasis on those that could be used in resource-limited settings.
Introduction
In 2015, about 2.1 million new cases of human immunodeficiency virus (HIV) infections were recorded. Global surveillance reports indicate that 36.7 million people are living with HIV, and in June 2016, it was reported that 17 million people living with HIV were recipients of antiretroviral (ARV) therapy (ART). 1 An estimated 1.1 million people died from AIDS-related illnesses in 2015. 1 Sub-Saharan Africa bears the largest burden of HIV/AIDS cases, with about 65% of all new HIV infections occurring in that region. 1 With no cure for HIV infection, years of laborious scientific research led to the discovery of 26 Food and Drug Administration–approved ARV drugs with different pharmacologic/pharmokinetic activities. 2
To combat resistance to these ARV drugs, highly active ART consisting of combined drug regimens is administered to persons living with HIV. Most of the combination therapies include 2 nucleoside reverse transcriptase (RT) inhibitors and a single non-nucleoside RT inhibitor (NNRTI) or protease inhibitor (PI). 3 Alternative treatments include combinations of integrase or entry inhibitors with RT inhibitors and PIs are used. Despite the ARTs and treatment plans combined by clinical pharmacologists to keep the viral load (VL) to the barest minimum and enable patients live long with healthy lives, ARV drug resistance may occur, thus defeating the therapeutic efficacy of ARV regimens. 3
Antiretroviral therapy should be initiated in all children, adolescents, pregnant and breastfeeding women, and adults living with HIV, regardless of World Health Organization (WHO) clinical stage and at any CD4 cell count. 4 Antiretroviral therapy monitoring is vital to improve the quality of life of people living with HIV/AIDS (PLWHA) through the reduction in HIV transmission and the prevention of large-scale resistance of the HIV to ART. Consequently, recommendations on routine ART monitoring and investigation of treatment outcome have been considered in the 2016 WHO consolidated guidelines on the use of ART for the treatment and prevention of HIV infection. Based on these, HIV VL testing is recommended as the preferred monitoring approach to diagnose and confirm ART failure. 4 Because of the unavailability of routine HIV VL testing facility in all health care centres in Africa, CD4 count and clinical monitoring are used to diagnose treatment failure, with targeted VL testing to confirm viral failure where possible. 4 Periodic VL tests are the most accurate way of determining whether ART is working to suppress replication of the virus. Achieving viral suppression protects the body’s immune system, helps PLWHA stay healthy, and prevents transmission to other previously uninfected people. An elevated VL suggests that treatment provision needs attention, including offering adherence support and HIV resistance testing. 4
To maintain prolonged care and treatment for more than 10 million HIV-infected persons living in low-income and middle-income countries (LMICs) such as those in sub-Saharan Africa, effective policies and funding are crucial in achieving viral suppression through the availability of affordable technologies to monitor the effectiveness and durability of available ARV drugs. In LMICs, challenges associated with achieving these goals have been observed; these include inadequate laboratory logistics, ARV drug availability, and insufficient clinical care and management experts. Due to high cost of diagnostic tests and limited laboratory capacity, the use of genotypic resistance test (GRT) to arrive at best possible clinical decisions in the selection of ARV drugs for better management of patients with HIV is hardly a reality in LMICs. 5
The achievement of effective ART monitoring can reduce the transmission of HIV and avoid large-scale resistance of the HIV to ARV drugs. 6 The technologies used in ART resistance monitoring make up for existing efforts in enhancing clinical decision making for affected individuals with treatment failure and fast-tracking population-based surveillance of viral resistance to ART. The HIV drug-resistant testing technologies include sequence-based investigations (in-house Sanger-based GRT and next-generation sequencing [NGS]), point mutation assays (PMAs), and genotype-free data-based prediction systems.5,6
The technologies used to detect HIV drug resistance can be rated based on several parameters by which performance of each can be assessed. These parameters vary from one technology to the other and involve sensitivity or percentage of the target bases that represent one or several sequence reads, specificity or percentage of sequences that map to desired target regions, uniformity or variability in the sequence coverage over target areas, precision (reproducibility) or how close measured results from replicate experiments correlate with each other, cost, level of bioinformatics expertise needed for operation, and DNA amount needed for assay or per mega base of the target. Technologies with high specificity and uniformity require less sequencing and low cost to determine appropriate coverage of sequence data for downstream investigation. 5 In this review, we provide detailed protocols for each technology to enable end users to easily compromise between specificity, sensitivity, and uniformity for any project of concern. In addition, we compared the merits and demerits of each technique with the aim of providing available options of these testing technologies for people living in LMICs.
Clinical indications for HIV drug resistance testing
Investigating drug resistance is routinely prescribed by the physician as part of the primary care received by newly enrolled persons for clinical care of HIV infection. 7 Resistance testing should be done irrespective of the patient’s choice to either commence therapy with ARVs immediately or delay treatment. 8 If the choice is to delay treatment, resistance testing may be repeated consequently when consumption of ARVs is resumed. The results of primary HIV resistance testing can comparatively detect whether initial infection was with a drug-resistant strain of HIV or not. Drug resistance testing results are used to decide which ARVs to include in a person’s first treatment regimen. 8 After treatment is resumed, secondary drug resistance testing is required if HIV VL results are indicative that the HIV regimen is poorly controlling viral proliferation and informs the physicians choice to prescribe second-line ARV drugs. Drug resistance testing is also recommended for all pregnant women living with HIV prior to commencing therapy on and also in some pregnant women already on HIV medications. 8
Resistance testing is requested in cases of virologic failure when a treatment change is being considered. Laboratory investigations for such cases should be characterized by (1) a confirmed detectable VL from 2 independent consecutive samples collected after an undetectable measurement, (2) a steady or increasing VL after the initiation of medications (HIV RNA levels >1000 copies/mL), and (3) detectable VL 6 months after treatment initiation. In persons with HIV RNA levels >500 copies/mL, but <1000 copies/mL, drug resistance testing is usually unnecessary because of low success rates recorded but should still be considered. 9 In such cases of treatment failure, resistance testing is requested on the premise that the patient is consistently taking his medication at the time of the sampling. If the sample is collected without the presence of selective pressure, the chances are high that wild-type strain of the virus will be detected instead of the mutant. 9
Separate studies conducted in Canada and Italy developed a study design aimed at examining the reliability and clinical utility of standard GRTs in cases of low-level viraemia – a VL between 50 and 999 copies/mL.10,11 The retrospective study involving 4915 samples collected from 2492 people who received care in British Columbia between 1996 and 2012 reported an 88% occurrence of drug resistance in tests conducted when VL was below 1000 copies/mL. 10 Successful results were obtained from three-quarters of samples with VLs below 250 copies/mL and from 90% of samples where VL was above 250 copies/mL. 10
The study also examined the use of HIV resistance tests in a subset of 196 people taking their first ARV combination that had experienced low-level viraemia and had no record of a baseline resistance. At the time of resistance testing, the patients had a median CD4 count of 415 cells/mm3, with a median VL of 374 copies/mL. Approximately a fifth (19%) of the patients under study developed resistance during their time with low-level viraemia. Only 5% of patients with a VL between 50 and 250 copies/mL developed resistance, compared with 30% of individuals with VLs between 750 and 999 copies/mL. 10
Utility and efficiency of dried blood spots as an alternative method of specimen collection for HIV genotyping
Dried blood spots (DBSs) are increasingly becoming appealing as alternative specimen collection format for HIV genotyping especially in areas where low-cost diagnostic techniques are desired. They are easy to obtain, less stressful on the patient, easy to process and transport, and require simplified storage conditions.12,13 Plasma HIV genotyping detects the RNA contained within the cell-free circulating virus. However, template material present in DBSs consists of RNA from circulating virus and DNA from the cell-associated, integrated provirus. 14
Studies have shown that genotyping results from DBS are highly informative and efficiently equivalent to the results obtained when using plasma for conventional sequencing methods. 14 Recent studies have demonstrated good correlation of results obtained from DBS and plasma samples in resource-limited settings such as Malawi, Kenya, Nigeria, and Senegal. 15 In contrast, some studies have demonstrated that concordance of genotyping results in plasma and DBS is not absolute and variation may be accorded to certain factors such as the VL, the duration an individual has been infected with HIV, and ART status. It has been noted in a previous study that the plasma/DBS concordance is the highest when VL is ≥5000 copies/mL and/or the patient has not been treated with ARTs and/or the person got infected with HIV within ≤2 years. 14
Causes of HIV Drug Resistance
Genetic mutations in the genome of HIV
DNA viruses unlike RNA viruses exhibit proofreading mechanisms which enable them retain their original genetic composition during replication. However, an RNA virus such as HIV, due to the lack of a proofreading exonuclease, will have each new copied genome differing from the parent virus, by at least a single nucleotide. 16 This repair inability of HIV RT confers a high mutational rate to the virus (approximately 5-10 nucleotide mis-incorporations per genome per viral cycle). 17 For some ARV drugs, such as lamivudine and certain NNRTIs (eg, nevirapine), a single mutation can confer high-level resistance. When these drugs are given in combinations to partially suppress viral replication, drug-resistant mutants predominate within weeks. 18
HIV unchecked by ARV drugs in an infected person
Due to its large progeny, HIV can replicate up to a billion copies of new viral particles per day. 19 When combined, both factors (genetic mutations in the genome of HIV and HIV unchecked by ARV drugs in an infected person) promote increased viral plasticity, leading to the presence of viral quasi-species within patients, frequent escape from the host’s immune system, and the emergence of resistant viral strains under drug selective pressure. 20
Some other factors that may hinder the efficacy of ARTs in patients include individual differences in pharmacokinetics, several adverse drug reactions, limited drug absorption and penetration into reservoirs of viral multiplication, and coinfections with other pathogens. In a study, multidrug-resistant HIV-1 highlighted a 3-fold increased risk of death following the diagnosis of multidrug resistance, compared with the risk observed overall in HIV-infected individuals. 21
Increased provision of ART has led to the emergence of therapeutic failure and acquired drug-resistant HIV in patients who will require more expensive advanced lines of ART to control the disease. Along with increased and quicker access to laboratory-based VL monitoring, feasible and cost-effective technologies to detect drug-resistant HIV could help maximize the duration of use of available drug regimens. Current existing affordable technologies include in-house Sanger and NGS in centralized laboratories, as well as PMAs and genotype-free systems that predict response to ART at point of care. 6
In sub-Saharan Africa, which is home to some of the world’s poorest countries, a substantial number of adults and children receiving first-line ART are likely to develop treatment failure within the first 5 years on the drug regimen. 22 Among those patients on first-line drugs, an estimated 70% to 90% acquire drug-resistant HIV. 23 In sub-Saharan Africa, a fewer than 1 million people are on second-line ART regimens but numbers are estimated to increase to about 4 to 6 million people by 2030. 24 In future, there will be a demand for third-line and other advanced therapies. Low-income and middle-income countries are currently facing challenges managing the growing numbers of patients requiring second, third, and more advanced lines of therapy, driven by the limited availability of ARV drugs, diagnostic technologies, and clinical expertise. In contrast, high-income countries adopt efficient guidelines which ensure the availability of GRTs which promote profound response of adequate ART regimen in patients with failure to ARV drugs. 25
Policies for the Regulation of ART Monitoring in Resource-Limited Setting
To effectively monitor HIV disease progression and the durability of ART options in resource-limited settings, WHO guidelines have been developed and these guideline recommend the use of VL monitoring in addition to CD4 cell count which, unlike VL assay, lacks the ability to determine the proportion of HIV-infected patients who require alteration in their regimen following ART failure. 24
Despite the guidelines provided by the WHO to ensure that countries formulate favourable policies to assess and prevent HIV drug resistance, LMICs are challenged with issues of lack of funding, budgetary allocation, and the complex nature of survey protocols. In terms of the use of drug-resistant technologies, several factors including high capital cost and cost of investigation, limited molecular laboratory facility, lack of skilled manpower, and requirement for cold-chain sample logistics have hampered the vast applicability of these technologies. 26
Essence of HIV Drug Resistance Investigation
Drug resistance investigation serves as an essential tool to aid physicians in the selection of potent ARV drug regimens that will improve the chances of favourable treatment responses. 27 The use of HIV drug-resistant assays in the management of infected patients is beneficial in several ways. Drug-resistant tests avoid the cost and toxicity of medications not likely to function and identify drugs most likely to work effectively. 28 These tests can be used to prevent patients without clinically vital resistant mutations from irrational switch to regimens which are of benefit to those that need such medications. Furthermore, these tests serve as a guide for the selection of effective drug combinations. 6
Laboratory Technologies for Testing HIV Resistance
Genotypic resistance tests are assays that investigate mutations of the viral genome associated with drug resistance following nucleotide sequencing of the target genes. These investigations include sequence-based assays (Sanger-based GRT and next-generation setting [NGS]), PMAs, and Web-based genotype-free prediction systems. 6
Sanger sequencing
This technique, also known as dideoxy sequencing or chain termination, is based on the use of dideoxynucleotides (ddNTPs) which act as DNA chain terminators in addition to the usual nucleotides (NTPs) found in DNA. Dideoxynucleotides share similar features with NTPs; except that instead of having a hydroxyl group (OH), they possess a hydrogen group on the 3′ carbon. These modified NTPs, when integrated into a sequence, avoid the addition of further NTPs. This occurs because a phosphodiester bond cannot form between the ddNTP and the next incoming nucleotide, and thus the DNA chain is terminated. 29
This approach has been modified using automated sequencing to accommodate the sequencing of more DNA within a shorter period. This advancement enables all 4 ddNTPs to react in a tube with different colour dyes. Consequently, the DNA is allowed to separate only on 1 lane. Because the 4 dyes fluoresce at different wavelengths, a laser is used to read the gel to determine the identity of each band based on its unique wavelength. Data are displayed in the form of a chromatogram which indicates coloured peaks that correspond to the nucleotide in that sequence location. 30
This modification has paved way for generation of long individual reads. These assays have been widely validated as some have been developed as kit-based for the detection of HIV subtypes. This technology is commonly available in several African countries where kits are used with the DBS. Unfortunately, this technology is limited in throughput and requires complex and expensive equipment which is sparsely available. Furthermore, this technique is not suited for parallel investigation, lacks the ability to detect minor variants (<20%), requires high capital cost for operation, and is impractical for massive sequencing projects. 6
The high cost can be reduced using open-source reagents, decreasing the number of primers, 1-step amplification,31,32 negotiations with suppliers of the technology, collaboration with non-profit manufacturers, sequencing just reverse transcriptase for failed treatment with first-line ART drugs, and sample pooling. 33
Next-generation sequencing
Due to the high demand for affordable sequencing, the NGS technology was developed with higher high throughput and the ability to parallelize the sequencing process of millions of DNA fragments in a run, which can be used in assaying for resistant strains of HIV to ART. High-throughput sequencing technologies were intended to drastically reduce sequencing costs per genome. Companies involved in the production of NGS include Pacific Biosciences, Oxford Nanopore Technologies, Illumina, Helicos Biosciences, Danaher Motion Cooperation, Applied Biosystems, and 454 Life Sciences. 29
Although equipment costs are still high (>US $100 000), prices are estimated to fall as technological simplifications occur. Despite the high cost per run, the cost of each test is affordable. Higher levels of automation can be achieved through multiplex sequencing, where several primer-barcoded samples are pooled using 24-multiplex (Illumina MiSeq 50; Illumina, San Diego, CA, USA) or 48-multiplex (Roche 454, Penzberg, Germany) systems. Moreover, the potential for full-genome sequencing with minimal additional cost could make NGS a preferred option for evaluation of resistance in patients on PI-based therapy because polymorphisms in group-specific antigen (gag) protein and envelope (env) gene regions could induce PI resistance. 34
Full-genome sequencing also minimizes the need for separate assays for the integrase gene region as the use of integrase inhibitors is anticipated to increase. Further advantages of NGS include the opportunities for simultaneous detection of other pathogens and use with DBSs and broad subtype primers. 35
Unlike Sanger sequencing, multiplex sequencing which is adopted by Illumina MiSeq and Roche 454 systems is more affordable and can generate high throughput. 36 These systems enable full-genome sequencing to be achieved with minimal cost for the assessment of patients failing PI-based ART. 37 Besides HIV, other pathogens can be detected in DBSs using broad subtype primers in NGS. A previous study which compared Illumina and Roche 454 in patients failing raltegravir-based ART observed that Illumina demonstrated larger depth of coverage and increased sensitivity for HIV minority variants as well as lesser false-positive variant calls. 35
The demerits of NGS include high level of expertise and high cost of bioinformatics support needed for data analysis. Ion torrent sequencing technology has been observed to be prone to insertion-deletion errors at homopolymer regions, whereas Illumina sequencing technology is prone to substitution errors and sequence coverage that is not equal. 38
Point mutation assays
These assays provide a means for the investigation of the genetic composition of human as it combines laboratory medicine with molecular genetics for the development of DNA/RNA-based techniques for assessing pathologic conditions. Several methods have been used in the detection of mutation and these could be classified into methods for known, unknown mutations, and both known and unknown mutations. 39
To successfully select a suitable method for the assessment of the point mutation, certain criteria are considered which include the type of nucleic acid, sample type, number of mutations, and the reliability of the method. 39 Methods used for detecting known mutation include restriction fragment length polymorphism, amplification refractory mutation system polymerase chain reaction (PCR), multiplex PCR, nested PCR, real-time PCR, allele-specific amplification, allele-specific oligonucleotide, and single-nucleotide primer extension. Methods for detecting unknown mutation include denaturing gradient gel electrophoresis as well as temperature gradient gel electrophoresis, single-strand conformational polymorphism, hetero-duplex analysis, protein truncation test, and DNA chips. Methods for detecting both known and unknown mutations include reverse transcription-polymerase chain reaction, multiplex ligation-dependent probe amplification, chemical cleavage of mismatch, and oligonucleotide ligation assay. 39
A PMA that can successfully detect 6 resistance mutations in RT successfully detected resistance in 98.8% of patients failing first-line and 61.2% of previously untreated patients. 40 The main problem with the PMA technique is the substantial HIV-1 sequence variability at and surrounding each drug resistance mutation target, which means that multiple experiments are needed per target site. The requirement for multiple tests per site increases the costs of PMAs, especially without affordable multiplexing assays. Therefore, development and validation of low-cost multiplex PMAs might lag behind current clinical practice. 40
Web-based genotype-free prediction systems
This technology uses computational models to generate predictions for response of viruses to ART regimen based on archived databases of ART-managed patients. The processes of this approach involve the ranking of a set of suitable drugs and selection of the most suitable combination of these drugs for a particular patient. These predications are based on inputted clinical and demographical data which include most recent VL, CD4 cell count, and history of previous treatment. 41 This technology has the potential to improve clinical decision making by health care providers who are not required to attain high level of professional expertise. 6
The HIV Treatment Response Prediction System (HIV-TRePS) had an overall accuracy of 78% (Table 1) in prediction of virologic response in independent testing 42 compared with 57% to 60% achieved by GRT with rules-based interpretation for the same cases. The HIV-TRePS, available as a free online service, has the potential to enhance clinical decision making of ART providers with relatively little training. 41
Performance of human immunodeficiency virus resistance testing technologies.
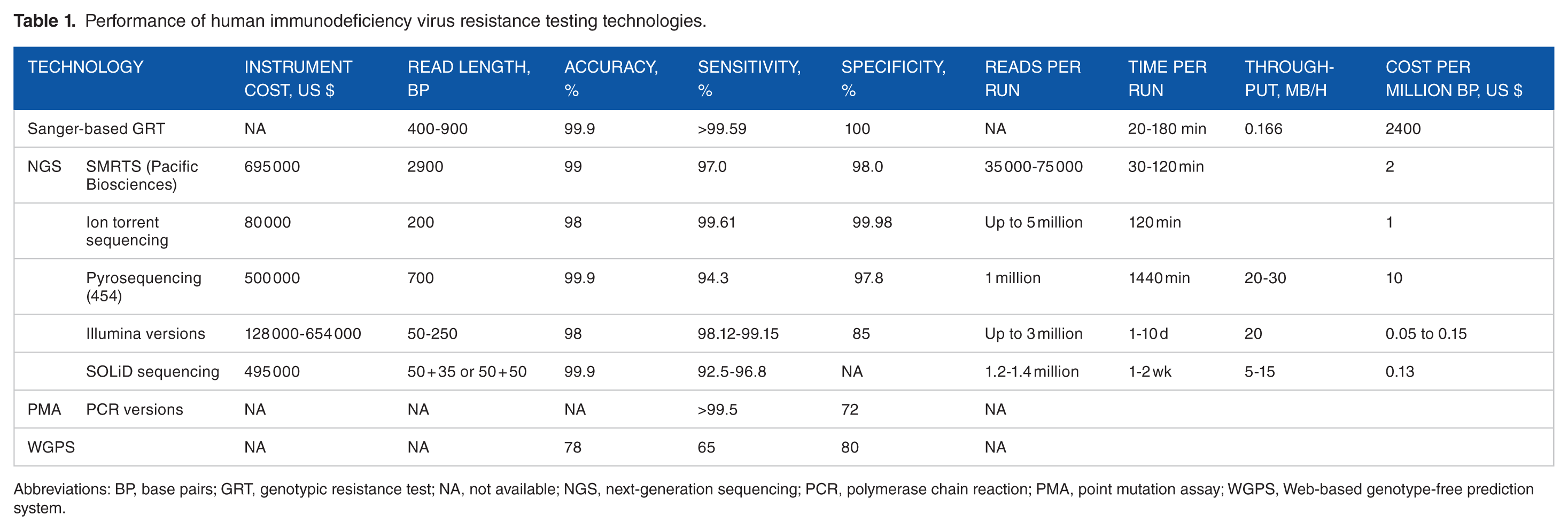
Abbreviations: BP, base pairs; GRT, genotypic resistance test; NA, not available; NGS, next-generation sequencing; PCR, polymerase chain reaction; PMA, point mutation assay; WGPS, Web-based genotype-free prediction system.
Network of Reference Laboratories in Africa Designated for HIV Resistance Testing
The HIV resistance testing centres across the continent comprise a focus of leading national public health laboratories. These laboratories play a key role in strengthening laboratory services in HIV care and management with the aim of improving health outcomes in Africa. This could only be achieved by being at the forefront of implementing several important health initiatives and influencing health policies. At the moment, there exist 6 centres of excellence with national and international repute in laboratory medicine, research, training, policy guidance, technology assessment, and implementation. They include the Ethiopian Public Health Institute (EPHI); the Kenyan Medical Research Institute; the Institute of Human Virology in Nigeria; the West African Network of Excellence for Tuberculosis, AIDS and Malaria (WANETAM) in Senegal; Central African Network on Tuberculosis, HIV/AIDS and Malaria (CANTAM) in Congo; the National Health Laboratory Service (NHLS) in South Africa; National Health Laboratory Quality Assurance and Training Centre (NHLQATC) in Tanzania; and Centre for Human Virology & Genomics (CHVG) in Nigeria. Most of these facilities are in collaboration with the African Society for Laboratory Medicine. 42
The EPHI, previously known as the Ethiopian Health and Nutrition Research Institute (EHNRI), is a national centre of excellence in providing a range of services which include the production of vaccines, trainings, laboratory support service for the national polio, and HIV surveillance programme and other specialized services including polio and HIV molecular drug resistance as well as malaria rapid diagnostic tests lot testing. This centre is accredited by the WHO. 43
The Kenya Medical Research Institute (KEMRI) is a state corporation and research laboratory established to provide support services which comprise performing genotypic HIV drug resistance sequencing among other specialized services. The KEMRI is accredited by the South African National Accreditation Scheme (SANAS) and ISO 15189. 44
The Institute of Human Virology, Nigeria (IHVN) supports the development of systems for the treatment, prevention, and support of both the infected and the affected persons by a host of diseases which includes HIV/AIDS, cancer, tuberculosis, malaria, and other diseases in Nigeria. The roles of this centre involve the implementation of the United States President’s Emergency Plan for AIDS Relief (PEPFAR) programme, research, mentoring to promote quality evidence-based health systems strengthening, advanced laboratory training, and specialized services, such as HIV viral sequencing for drug resistance. 45
The WANETAM is a sub-regional conglomeration of Networks of Excellence. It involves research institutions from Burkina Faso, The Gambia, Ghana, Guinea-Bissau, Mali, Nigeria, and Senegal. The roles of WANETAM involve capacity building, technological transfer, and creation of a regional network for scientific collaborations including HIV resistance testing. 46
The CANTAM, similar to WANETAM, is a sub-regional conglomeration of Networks of Excellence. It brings together 7 high-profile research institutions from Cameroon, Congo, and Gabon. The objectives of CANTAM include mentoring of laboratory facilities in preparation for international accreditation and creation of a regional network for scientific collaborations such as HIV resistance testing. 47
The NHLS located in South Africa is the largest diagnostic pathology service responsible for providing support for the national and provincial health departments in the delivery of top-notch HIV laboratory testing services. Its objectives involve the provision of diagnostic laboratory services, research, teaching and training, and production of serum samples for anti-snake venom, reagents, and media. 48
The NHLQATC supports public health laboratory, quality assurance systems, and training exercises. Its main objectives are to mentor laboratory facilities in the implementation of laboratory quality management systems, provide technical aid, and equip laboratory scientists with updates in laboratory diagnosis especially in the area of HIV drug resistance testing and other molecular diagnostic procedures. 49
The Centre for Human Virology and Genomics (CHVG), previously known as the Human Virology Laboratory, is a research laboratory in the Medical Microbiology Department of the Nigerian Institute of Medical Research (NIMR). This centre provides diagnostic support services which includes ART programme for HIV/AIDS patients, viral hepatitis programme, mentoring of laboratories in the implementation of Quality Management System in preparation for international accreditation to ISO 15189:2012, and other specialized services including HIV-1 drug resistance testing. Similar to KEMRI, the research laboratory at CHVG is the first medical laboratory in Nigeria to be recognized as a South African National Accreditation System (SANAS)-Accredited Medical Testing Laboratory for HIV resistance monitoring in Nigeria. 50
Most of these laboratories get greater part of financial, technical, and logistics funds to run HIV resistance testing from many non-governmental and donor organizations from United States, United Kingdom, and Europe and partly from their host government, thereby subsidizing the cost per test for patients who needed HIV resistance testing. These specialized laboratories make use of all available laboratory technologies in investigating HIV resistance. As Ion Torrent and Illumina sequencing technology are relative cheaper, have the ability to run large number of samples at a time, coupled with high sensitivity and specificity, they appear to be easily applicable in the LMIC for HIV resistance testing (Table 1). Despite the WHO recommends periodic surveillance of drug resistance HIV strains in areas where ART has been in use for >3 years, few studies on HIV resistance test results have been done in LMIC. 51
Limitations of HIV resistance testing
The correlation between the development of drug resistance and the occurrence of clinical failure is a complex one. This is because the development drug resistance is not the sole cause of treatment failure. 52 Other factors have been identified as leading causes are clinical and virologic, notable among them are non-adherence to treatment regimens, the use of insufficiently potent treatment regimens, pharmacokinetic factors that decrease the efficacy levels of one or more drugs in a treatment regimen, and several others. Conversely, a drug may have some benefits even in the setting of resistance because of some, although limited, residual effects of some drugs and because many drug-resistant variants have a reduced replication capacity compared with drug-susceptible variants. 53
Another important limitation of HIV resistance testing is the unreliability of the tests to detect minor genotypic HIV-1 variants. 54 This limitation can complicate the interpretation of resistance tests particularly in patients with complicated treatment histories. Therefore, treatment and resistance history always have to be taken into account. HIV-1 exists in each infected individual as a complex of quasi-species in which many different subpopulations of drug-resistant variants co-exist. 55 Also subpopulations that are no longer actively replicating will remain archived in latently infected cells. The complexity of these quasi-species may influence the success of therapy in ways that cannot be predicted by any single drug resistance test. 55
Conclusions
Access to ART in LMICs has become easier, faster, and cheaper. However, the menace of transfection of drug-resistant strains of HIV is a growing concern for clinical virologists and clinicians. In the long run, the demand for further advanced drug regimens in the event that first-line, second-line, and third-line therapies results in virologic failure and poses a risk of emergence of limited access to ARTs due to the high cost incurred in production and research into advanced lines of treatment.
With the development of in-house reagents for use in NGS and PMAs, resistance testing may well become more accessible especially as promises of cheaper technologies are emerging. A paradigm shift away from blood-based technologies seems feasible with genotype-free prediction systems, although the success rates are not as high as that of NGS and PMAs. In retrospect, the need for centralized laboratories cannot be overemphasized. Funding for such laboratories can be sought from by collective bargaining with technology and reagent providers. Sourcing for grants and donor funds from governments and well-meaning individuals would go a long way in providing for the technological needs as well as clinical expertise required for such laboratories to stay afloat.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
IAN, AUE, and IO collected the information from published literature. IAN and AUE categorized the draft manuscript into different sub-headings and prepared the manuscript. IAN and HAA edited the manuscript and corrected/modified the grammatical content. All authors read and approved the final manuscript.
