Abstract
HIV testing among HIV-exposed infants (HEI) in Malawi is below global targets and, affected by low utilisation of health services after birth. We conducted a mixed methods evaluation of the implementation of services for early infant diagnosis (EID) of HIV against national guidelines in Blantyre, Malawi, to inform the development of strategies to improve EID services uptake. We estimated coverage of HEI enrolment in HIV care and HIV testing at 6 weeks through a retrospective data review. We qualitatively explored implementation gaps in EID services through process mapping of 8 mother-infant pairs (MIP); and investigated healthcare workers’ (HCW) perspectives on the implementation gaps through group interviews with 16 HCWs. We analysed the quantitative data descriptively and conducted a thematic content analysis of qualitative data. Of 163 HEIs born at the study sites, 39 (24%) were enrolled in an HIV care clinic before post-natal discharge, and 85 (52%) received HIV testing by 6 weeks. The median time for MIP to receive EID services was 4 (1-8) hours. The implementation gaps observed during process mapping included: failure to identify and enrol HEI in HIV care clinic; lack of immunisation, counselling for HEI testing, HIV testing, drug refilling, and family planning; and different appointment dates for mother and infant. HCWs reported delays and gaps influencing optimal service provision including: lack of screening to identify MIP, limited supervision for student HCWs when providing services, inadequate capacity of point of care machines, challenges with integrating services, and role confusion. Use of unique identifiers for MIP and establishing a booking system to schedule appointments to suit point of care machine capacity were primary service improvement recommendations. This study identified suboptimal EID services in Malawi due to process, capacity, and system factors. Context-appropriate interventions accommodating systems thinking are needed to enhance service provision.
Background
Progress towards the joint United Nations Programme on HIV (UNAIDS) 95:95:95 goals for HIV testing, treatment, and viral load suppression among children (0-14 years old) in Eastern and Southern Africa is substantially below target at 66:56:44, respectively. 1 Mother-to-child transmission (MTCT) causes 90% of all paediatric HIV infections,2,3 necessitating HIV testing of infants born from HIV-positive women, known as HIV-Exposed Infants (HEIs).4,5 In 2010, the World Health Organization (WHO) recommended testing HEIs at 6 weeks using an HIV virological assay (DNA PCR), followed by a serological HIV assay at 12 months and a repeat HIV serological assay at 18 months. 6 This is known as early infant diagnosis (EID). 5 However, in 2021, the WHO updated the recommendations to diagnose HIV in children below 18 months of age with point-of-care nucleic acid testing, and these were not in use during our study. 7
However, despite WHO’s recommendation, only 71% of HEIs in Eastern and Southern Africa are tested at 6 weeks. 1 In 2019, a systematic review of studies in African countries 8 showed a 39% rate of loss to follow-up of HEI in HIV care clinics (HCC) before 18 months. Several studies in Africa,8-14 have highlighted health system and community factors contributing to the general loss to follow-up in both post-natal care utilisation and HCC.12,15-18 Nkhonjera et al identified lack of privacy and unsynchronised hospital visits for the mother and HEI compromised mother-infant pairing (MIP) as factors leading to HEI loss to follow up among mothers still in HIV care. 19 Whilst initiatives have emerged to strengthen EID systems,20-27 interventions have been reported to be effective in one setting and not the other,20,26 suggesting the need for context-driven understanding of implementation gaps to inform better implementation. Therefore, we conducted a mixed methods study to investigate implementation of EID services in rural and urban primary health facilities against national guidance for Clinical Management of HIV in Children and Adults in Malawi, one of the 10 highest HIV prevalence countries in Africa. 1 The 3 main objectives were to (1) estimate the coverage of HEI enrolment and HIV testing at 6 weeks; (2) explore implementation gaps in EID services for the MIP; and (3) assess health care workers’ (HCW) perceptions of the identified processes of care and their recommendations on implementation gaps.
Methods
Setting
Malawi is one of the countries worst affected by HIV. Despite an overall increase in testing coverage from 29.3% to 79% between 2016 and 2021,1,28,29 HIV testing among HEI is still below the target of 85%, which was set in 2015.1,28 Loss to follow-up is also high among HEI. Van Lettow et al reported 26.2% of HEIs were lost to follow-up over 24 months. 30 Malawi pioneered Option B+ in 2011 to commence all HIV-positive and breastfeeding women on antiretroviral therapy regardless of CD4 cell count and clinical staging. 4 The Malawi Ministry of Health guidelines for Clinical Management of HIV in Children and Adults (2018) and standard operating procedures (SOP) for early infant diagnosis of HIV (2017) guide the implementation of EID services from birth to 24 months old31,32 (See Supplemental File 1). EID implementation was assessed against these documents, which were in effect at the time of the study covering HIV and general post-natal care.
We started with quantitative data collection followed by qualitative data collection 33 in one urban and one rural primary health facility in Blantyre District in Southern Malawi. Blantyre district has the highest HIV prevalence amongst the general population in Malawi at 14.2%. 34 The urban facility, with a 2018 catchment population of 141 123, was purposively selected due to its size 35 and the availability of a point-of-care (POC) testing machine. It is a primary health facility that hosts clinical students for practical experience, including nurses, clinicians, pharmacists and lab technicians. In contrast, the rural facility had a 2018 catchment population of 9001 and no point-of-care machine. Both facilities offered family planning services, outpatient services, child growth monitoring, antenatal immunisation, delivery, and HIV services for adults and infants. Seriously sick patients were referred to the central hospital, a tertiary level that provides specialised services 36 which is 4 and 27 km from the urban and rural facilities, respectively. Health centres are staffed by midlevel practitioners comprising nurses, medical officers, and clinical officers with curative roles. 36 In contrast, health promotion and preventive functions are for health surveillance assistants (HSA) who receive 12-week basic training in primary healthcare approach. Depending on further donor support, others receive additional programme training, for example, nutrition and HIV, expanding their roles and responsibilities. 37 However, due to human resource gaps, curative services are shifting to HSA without formal training and supervision. 36 Malawi has developed several guidelines to instruct task shifting; however, there is limited dissemination and implementation. 37 Some non-governmental organisations with HIV projects in primary health facilities in Malawi, for example, EGPAF, hires HIV diagnostic assistants (HDA) who are trained to provide HIV testing and counselling services and expert clients(EC) who are people HIV infected and open about their status who are trained to support other people living with HIV. 38
Study design
This study had 3 components, as shown in Supplemental File 2. First, we retrospectively 36 extracted routinely available data on all HEIs from January to December 2018 in the facilities to estimate the coverage of HEI enrolment in HCC and HIV testing at 6 weeks. Secondly, to understand service provision from the patient perspective,33,39-42 we conducted a prospective process mapping using direct observation of the care that mother-infant pairs (MIP) received, including general post-natal and HIV care at birth and 6 weeks from November 2019 to March 2020. Finally, we conducted semi-structured group interviews with healthcare workers (HCWs) to explore perceptions of the care processes from observations of MIP and their recommendations to strengthen EID services at the primary health facility.
Data collection
Retrospective data extraction for HEI born at the facility
Two researchers, a female public health specialist (LCSK) (Masters of Public Health) and a male (CM) PMTCT data clerk, reviewed registers and extracted data for all women who were HIV positive and had given birth at the study sites from the Malawi Ministry of Health Maternity register. Both researchers had prior training in the national PMTCT guidelines, the study protocol, data collection tools and good clinical practice (GCP). The enrolment data of HEI in HCC, HIV testing and programme outcomes at 6 weeks’ age were extracted from the HCC register, DNA-PCR sample log book and the Exposed Child Under 24 Months Card, respectively, using a pre-designed data extraction form (Supplemental File 4) The data collectors reviewed each other’s data extraction forms at the end of each day to verify the collected data. They checked with data clerks at the study site for missing and inconsistent information.
MIP process mapping of the patient care journey
A purposive sample of 8 MIP was selected to allow variations in characteristics, including HEI’s age and stage of service access and mothers’ ART duration. The MIP was ineligible if they had had a maternal complication or sick HEI and were under 16 years old. Two female public health specialist (LCSK and SS) (Masters of Public Health) researchers, with training in GCP, study protocol and data collection tools and experience with qualitative studies within the Malawi health care setting, attended morning handovers at the maternity unit and noted the reported HIV-infected women with HEIs who were stable and due for post-natal review. One of the researchers (LCSK) had prior training in the national PMTCT guidelines, and the other (SS) familiarised herself with the guidelines. After handovers, researchers confirmed with nurses on duty to verify the women’s health passport books and maternity registers kept in the nurses’ offices. Women with HEI at 6 weeks were identified with the help of HCW either at immunisation or post-natal clinic when getting their infants weighed before accessing care through health passport review. Researchers verified that the identified women met the study criteria and obtained written informed consent. At the beginning of the study, 2 researchers (LCSK and SS) jointly followed one participant on observations (process mapping) without special considerations apart from meeting the study’s criteria to triangulate different observation perspectives and to ensure cross-observer reliability. Subsequently, they made independent observations using the process mapping guide (Supplemental File 5). Upon completing each mapping daily, researchers used basic flow chart symbols to identify specific activities. They summarised the observed data from the start to the end through diagrams (maps) showing each client’s journey, with an example (Supplemental File 6).
Group semi-structured interviews with healthcare workers
We conducted 4 semi-structured group interviews with 4 HCW in each group. We had 2 HCW group interviews at each site who had worked in the labour ward, post-natal clinic or HCC for more than 6 weeks. The researchers sought individual informed consent from HCW who met the study’s criteria of role variations. We scheduled the group interviews at a time convenient for all members of each group to ensure the participation of all. 43 Researchers used a group interview guide informed by findings from the process mapping, and one researcher moderated the group interviews. Sessions lasted an average of 119 minutes and were digitally recorded with participant consent. We ensured the credibility of findings through member checking. To avoid information loss and ascertain its adequacy, audio recordings in Chichewa were transcribed verbatim, translated to English by a trained transcriber (CK) fluent in both Chichewa and English and then LCSK verified the transcripts. We labelled the interviews with unique identifiers and used password protection accessible only to authorised researchers.
Data analysis
Extracted routine data
Extracted data were analysed using Microsoft Excel and Stata 14 (Stata Corp LP, College Station, TX, USA) to assess the frequency of infants born to HIV-infected women, the proportion of infants enrolled in HCC, enrolment time, the number of infants tested, results of their tests, and the programme outcomes at 6 weeks. Pearson Chi-square tests assessed the association of HEIs’ enrolment in HCC before post-natal discharge between ART clinic provision within and outside the delivery facility. When the cross-tabulation had all cell counts equal to or greater than 5, we used the Pearson Chi-square test, and when the cross-tabulation had any cell count less than 5, we used Fisher’s exact test. The test statistics were 2-sided, with a P-value of <.05 considered significant.
Process mapping data
One researcher (LCSK) developed an initial understanding of the processes, documenting narratives and summarising in a Microsoft Excel spreadsheet the participants’ demographics and themes that emerged in the observation process, guided by the observation guide and noting any emergent issues. Then LCSK discussed all process maps, narratives, and the spreadsheet with 3 other researchers (ALNM, PM and ND). The 4 researchers examined the emerging themes. Then we used the emerging themes to refine the semi-structured interview guide to understand the perspectives of HCW on the processes we observed and further analysis of the process maps followed during the group interviews, noting any contextual aspects such as physical environment and how that influenced EID services in the 2 different facilities.
Semi-structured interviews data
We managed data from the group interviews using Nvivo Pro 12 and analysed them following a thematic approach.44,45 Our initial step was transcribing and translating the audio from Chichewa into English and then reading the transcripts multiple times to familiarise ourselves with the data. Two researchers (LCSK and MP) coded one transcript, discussed it and developed a coding framework. We used the coding framework to code the remaining transcripts whilst paying attention to new codes. Researchers inductively developed codes from the group interview data. While other codes were deductively developed, reflecting the standard guidelines in implementing EID services from birth to 24 months old.31,32 Two researchers sorted the codes, and similar codes were grouped into categories to develop overarching themes. We reviewed the themes refined and labelled them.
Ethics approval
This study was approved by the University of Malawi’s College of Medicine Research Ethics Committee (COMREC P. 7/19/2728) on 10th October 2019. The retrospective data review did not require informed consent, and we did not collect identifying information. All participants provided written informed consent before recruitment.
Results
Characteristics of HIV-positive women who had live births
In 2018, 163 women gave birth to live HEIs in the selected study sites, with a median age at delivery of 28 years, interquartile range (IQR) (17-48 years). Characteristics of women attending the 2 facilities whose data was available are presented in Table 1.
Characteristics of HIV-positive women with live HIV Exposed Infants from January to December 2018 at Urban and Rural Health Centre (N = 163).

Estimated coverage of HIV-exposed infants’ enrolled in HIV care and tested at 6 weeks
We identified 163 infants during the review period, all of whom were singleton:123 in the urban and 40 in the rural facility. Only 85 (52%) tested for HIV at the 6-week milestone, and only 39 (24%) of 163 HEIs born at the study sites were enrolled in HCC at the delivery facility before post-natal discharge. The urban facility used a POC machine to test 57 infants with DNA-PCR, while the rural facility used dry blood spot samples sent to another facility for processing at 6 weeks of age to test 28 infants.
HIV testing and HCC enrolment are presented in Table 2. Among the 123 women who had documented ART status, 37 (30%) had their infants enrolled in HCC before discharge at both facilities. Out of the 93 women who accessed ART at the delivery facility, 30 (32%) were enrolled in HCC at birth. Compared to 30 women who did not access their ARV at the facility, only 7 (23%) were enrolled in care at birth. However, Fisher’s exact test shows no significant association between enrolment and mothers’ ART delivery facility at a P-value of 0.2.
HEIs enrolment in HCC and HIV ascertainment at 6 ‘weeks’ data in the selected health facilities from January to December 2018.

Proportion of infants tested in relation to all HIV-exposed infants born at the facility are determined by: HIV testing divided by all HEIs born at the facility and were not transferred out.
Proportion of HEIs diagnosed positive is determined by: HIV positive divided by HIV tested.
Proportion of HEIs diagnosed HIV negative is determined by: HIV negative divided by HIV tested.
Proportion of HEI without known status is determined by: HEIs without results divided by HIV tested.
Process mapping observations of MIP at birth and 6 weeks in both urban and rural facilities
We conducted process mapping observations of 8 MIP, 3 at birth and 5 at 6 weeks. (Exemplar map presented as Supplemental File 6). Three women were from the rural facility, and 5 were from the urban facility. Mothers’ median age was 31 (16-34) years, and the median ART duration was 9 (6-36) months. The median number of HEI for these women was 2 (1-4). Of the eight, one was a widow, and the rest were married. Seven of the women were housewives, and one was a tailor. The median time for MIP to receive post-natal and EID services was 4 (1-8) hours.
Observations at the urban facility
Nurses and student nurses were responsible for providing services when discharging the MIP at birth, including demonstrating the administration of prophylaxis, initiation of integration of MIP and enrolment of HEI in HCC. Notably, the urban facility had a senior nursing officer, nursing officers, and a Medical doctor who are high-level practitioners trained to provide specialised care. The students were often left alone to provide services to the MIP. Hospital and patient attendants cleaned the wards and supported getting resources from the pharmacy. The HSA provided immunisation at birth and 6 weeks and sometimes tested HEI using POC. Immunisations were delivered daily from Monday to Friday. Expert clients primarily assisted in retrieving files for other clients at the ART clinic. Laboratory technicians offered HIV testing to the HEI at the laboratory using the POC. The HDAs were responsible for providing HIV testing to women when they came for delivery and during pregnancy. Overall, the urban facility had inadequate infrastructure to support integration and privacy when offering services. One room with a 12-bed capacity was used to host women when they came to give birth and after giving birth. In addition, women coming for a postnatal check-up at 1 and 6 weeks, an average of 25 a day, were also accommodated in the same room. All infants were weighed in the same room before nurses started providing services. Nurses isolated one bed and a screen barrier and assessed women for birth, 1 week and 6 weeks postnatal check-ups. Because of limited space, other HCW provided postnatal service in the nurses’ office, and 2 additional rooms close to the office were used for scanning and antenatal clinics. The nurses used the delivery room to provide postnatal services if no woman was in labour. Most post-natal women started accessing care at the post-natal clinic at 6 weeks without the organisation of the care pathways within the facility.
Observations at the rural facility
In contrast, the rural facility was different and had no students. Only one nurse on duty provided family planning, HIV and postnatal care services on a day. Besides EC assisting in retrieving files for other clients, they supplied cotrimoxazole prophylaxis to HEI at 6 weeks. They were always available at the clinic and sometimes did not provide the correct dosages. The number of MIP receiving EID services was smaller than the urban facility. Immunisations were provided on Tuesdays and Thursdays only, and women accessing care on other days could not access immunisations. Women had their infants weighed under a mango tree where HSA hung a weighing scale. However, the rural had more infrastructure than the urban facility for their catchment, with available space for immunisation outside the labour ward. Specific HIV care services were provided to MIP on Wednesdays, different from the immunisation days. Women started accessing care at a 6-week visit at the post-natal or ART clinic with no standard flow of services. The HDA collected DBS samples for HIV testing. There was no linkage from the under-five clinic to HIV services; some women left the facility without HIV services for their infants. Figure 1 summarises the gaps we identified from post-natal discharge to 6 weeks of MIP care journey appointments.

Implementation gaps in EID of HIV services at birth and 6 weeks observed during process mapping at the urban and rural facility.
Perspectives of HCW on the observed implementation of EID services
Group interviews with HCW informed the context for implementation gaps identified during process mapping observations and extracted routine data for HIV-infected post-partum women and HEIs. Supplemental File 7 provides demographic information of HCW in our study. Two major themes emerged: implementation gaps and timeliness of services, as shown in the Supplemental File 3. HCW provided perspectives on implementation gaps with capacity, system, and client-related factors as the subthemes. On timeliness of services, process, client, management, resource and capacity aspects emerged as subthemes. We further present the implementation gaps and timeliness of services-related factors with HCW recommendations for improvement relating to the HIV care guidelines in Malawi (see Table 3).
Healthcare workers’ perspectives of implementation gaps in EID services in line with PMTCT recommendations in Malawi.
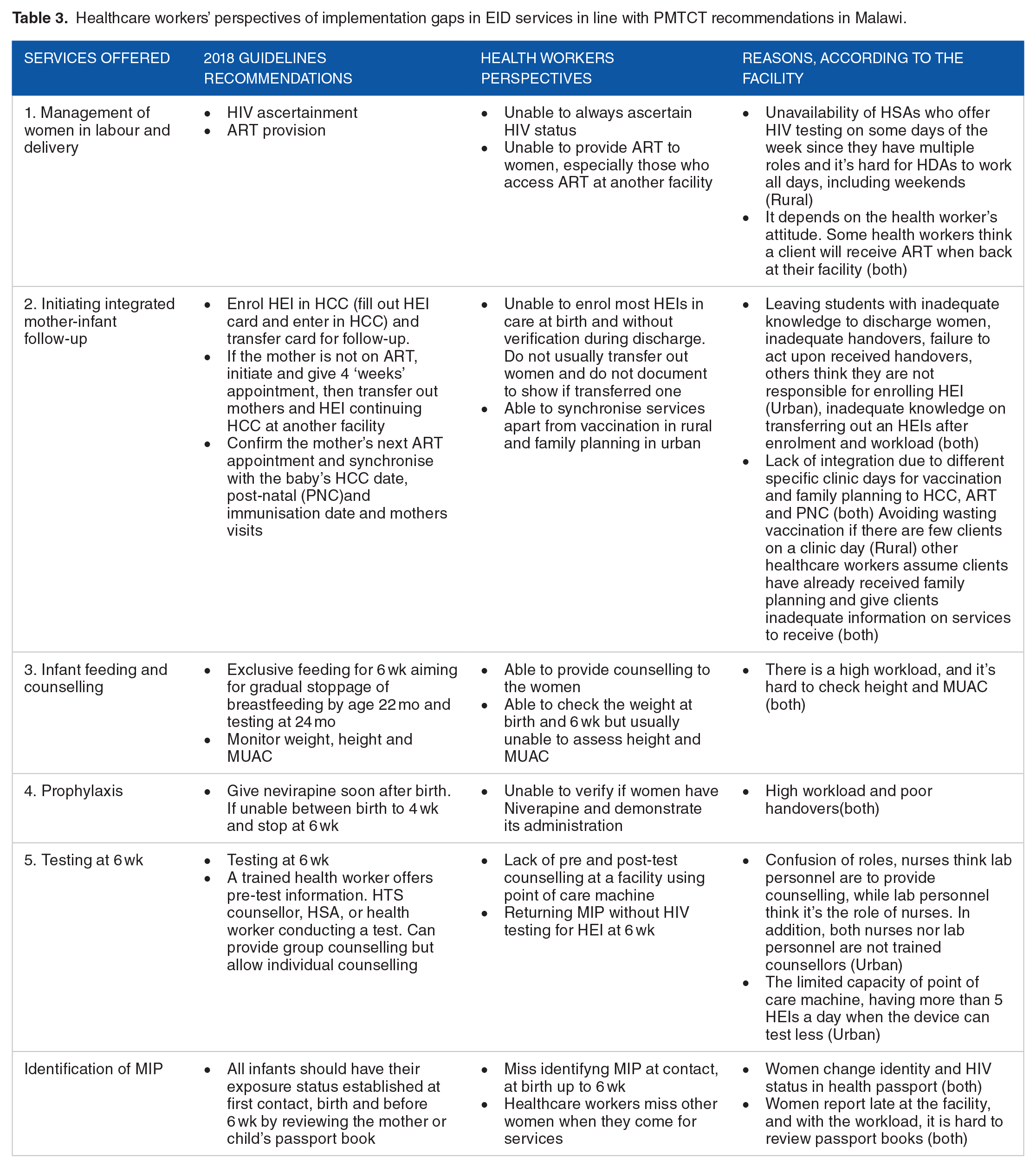
Implementation gaps
This theme discusses different capacity, system and client factors contributing to MIP not receiving all required services at the primary health facilities.
Capacity and system related factor
Shortage of knowledge and skills
Lack of knowledge and skills of HCW affected HIV testing services for HEI and enrolment in HCC. Urban facility HCWs offered HIV testing to HEI but lacked the knowledge and skills to counsel MIP because they were not trained as counsellors. One participant reported: ‘I am a Lab officer trained in all lab work but not a counsellor. As for me, I am not supposed to reveal the results’ (Urban, Lab technician). They provided testing services using the POC machine as one of their roles at the laboratory, thinking that nurses who referred MIP to the lab provided counselling. However, nurses reported not receiving counselling training.
In contrast, the rural facility offered HIV testing and counselling for HEI to MIP through HDA trained in counselling, and HSA who previously conducted the testing focused on other roles. Testing was done through DBS at the rural facility without a POC machine, and it took 4 weeks to receive results from other facilities. Additionally, some urban and rural HCWs had inadequate knowledge of enrolling HEI in HCC and transferring out of HEI. Subsequently, some HEI were not registered in HCC at birth and could wait for HSAs who supported HIV care services to enrol the infant at 6 weeks. One of the efforts to improve knowledge at the urban facility was continuous development meetings, although most nurses did not attend.
Lack of screening to identify MIP among postnatal women
Identifying MIP among different postnatal women to provide appropriate HIV care was challenging. HCW had many postnatal women at the urban facility to serve and did not check each passport book for HIV status. In contrast, the rural facility saw few clients; nevertheless, having one HCW on a shift made it difficult to check HIV status. HCW in the urban provided services in a crowded space and avoided inadvertently disclosing HIV status.
Contrary to rural facilities, HCW did not always check for HIV status. Some HCWs had no interest because previously, they received financial rewards for improving HIV care in a study. As reported, ‘There was money provided in a study in the past, and when the study finished, people are no longer troubled with identifying MIP’ (Rural-HDA). Both facilities rushed through service provision for MIP accessing services midday and did not check HIV status. ‘We should say those who present late, the help rendered to them on that day is cut short, unlike the ones who presented early. Because we follow all the processes, check the file, then screening, then viral load, when one presents late, people are doing this whole thing in haste, so for them to do all the processes, it is very different’. (Rural-data clerk)
Lack of integration of services
Services were provided separately for the mother and infant on different days and places. The rural facility had specific days for services. Immunisation was not offered daily. HSAs had multiple roles and avoided vaccine wastage because few women accessed services daily.
In comparison, the urban facility provided fragmented services due to inadequate infrastructure, and room for service delivery was crowded, contrary to the rural facility; however, there was a distance from one room service point to another. Both facilities were not providing all services in one room. HCW found escorting clients to be a time waste as they had other clients to assist, and this could lead to exposing women’s HIV status. For example, one urban nurse reported, ‘The issue of privacy, other women will be wondering why we are escorting that particular woman’. Integrating services was suggested in both facilities. However, changes could be minimal due to the limited resources that made them provide services on specific days. ‘We need a one-stop shop where one can have a check-up, then a vaccine, off they go, but it is not easy because they fall on different dates’ (Rural-Nurse).
Lack of organisation of service delivery and compliance with national guidelines
Organisation of services, from start to end and coordination of HCW in providing services was a challenge, further contributing to lack of guidelines compliance. The MIP started accessing services at any point, either immunisation or postnatal clinic at rural facility. If a woman accessed immunisation first, HSA did not remind MIP to access HIV services as they thought that was already offered. Contrary, the HCW at the urban facility advised MIP to report for postnatal care before other services. HCWs in both facilities reported following guidelines and conducting quality improvement meetings to improve services. However, did not have guidelines in the rooms for service delivery. ‘We do have it, but it’s not put somewhere that everyone can see and read, but according to my knowledge everyone has the information’ (Rural-Nurse).
Additionally, other HCW at the urban reported knocking off at a time MIP required other services and was unsure if those taking over continued with the services. ‘it depends on the time the baby was born. For example, you are on the night shift, and the baby was delivered at 7 am, and you cannot give nevirapine immediately as you have to wait for 1-hour post-delivery, which will be almost 8 am which you would have knocked off ’ (Urban-nurse). Some HCWs expressed challenges with handovers because of low attendance since HCW reported late for duties. While at the rural facility, HCWs reported working a shift for more days and sometimes gave handovers to other nurses by phone.
Limited capacity of POC only applied to the urban facility. The POC machine had a long processing time. Only 5 HEI could be tested on a day. HCW asked MIP to come on the following day for HEI testing if the capacity for that day was reached. ‘several times, we have sent women because we couldn’t manage to serve many of them in a day, so we had to ask them to come back early the following morning’ (Urban-Lab technician). Other HCWs did not recommend asking clients to come the following day. They suggested scheduling appointments for MIP in line with the POC machine. One participant reported: ‘Assigning specific days for appointments to suit the capacity of the POC, but we need a record book because you might give a particular date already full’ (Urban-Medical doctor).
Lack of supervision for students and HCW
The HCW were unsure of student knowledge levels but relied on them to provide post-partum care to MIP without supervision. For example: ‘There are times when we have a staff shortage. Thereby, you will have to explain to the students what to do, and you will leave them to work on their own on account that if they are in doubt, they should ask you, but you end up learning student has discharged an HEI without enrolment in HCC’ (Urban-nurse). Supervision appeared minimal in both facilities. HCW proposed enhancing leadership and teamwork to improve the implementation gaps. Other HCW found supervision by facility managers challenging because HCW are familiar with and some have attitudes. Other HCW suggested the need for supervisors to have good skills. One nurse reported, ‘You must be a leader and not necessarily a manager to work together. Still, if you are there to spot faults, then people will give you their attitudes. In addition, we also need to recognise when people have done well to motivate them’ (Urban, Nurse).
Client related factors
Change of identity
In both facilities, MIP used multiple health passport books with different names for different services to avoid identifying their HIV status, making it difficult for HCW to know and provide appropriate care. A nurse said, ‘You will only notice when they come at 6 week with a different book not used at antenatal’. Sometimes, MIP do not receive all services despite HCWs referring them.
The HCWs realised gaps in implementation due to capacity, system and client-related factors and expressed need for improvement, acknowledging less commitment and need for strong leadership and how limited resources affected comprehensive service delivery.
Timeliness of services
This theme discusses factors contributing to long hours accessing postnatal and HIV services at birth and 6 weeks in both facilities. Human, material and client-related factors as sub-themes are presented in Table 4. We further explain the process and management-related factors and HCW suggestions for improvement.
Factors contributing to delays in service provision.

Process-related factors
This subtheme indicates processes that contributed to MIP spending long hours to receive services, including multiple services for MIP, documentation and waiting for colleagues to provide services. MIP requires several services at a single visit. However, HCWs identified MIP late to offer multiple services. One nurse reported, ‘They need several services, but there is no clue that this mother is HIV-positive to assist first and send her to the laboratory for HEI testing. They stay on the line until their turn when we know their status and need for other treatment after spending a lot of time on the line’ (Urban-Nurse). HCW in both facilities recommended prioritising postnatal care for MIP among postnatal women to create time for HIV care and suggested using a unique identifier. One participant reported: ‘Putting a yellow tag to know they require your help so fast’ (Rural-nurse).
Health services that HCW provided needed documentation. One participant said, ‘When they arrive for a check-up, they go to HDA where there is a lot of documentation before a blood test. . . if getting nutrition services, there is a lot of documentation. The process of getting nutritional foods also takes time. They have to go on the line for a vaccine with more documentation that makes the mother go home late’ (Rural-nurse). Both facilities, nurses, waited for HSA to administer immunisation before discharging MIP and who administered the vaccines late. ‘will have to wait for our colleagues who give out vaccines to come and give out vaccines right here as we cannot ask the mothers who have just given birth to go out with the babies for vaccination. The waiting sometimes also delays the whole process of discharging the women as we have to wait for our colleagues to come and give out the vaccine’ (Urban-nurse).
Management-related factors
Management of staff schedule shifts, handovers, task allocation, and care organisation were time-contributing factors. The rural facility had one nurse per shift, and some HCWs thought there was a shortage of nurses. Other HCWs clarified that nurses made arrangements to work fewer hours. One participant reported: ‘It is not true to say that we have a shortage of nurses at this health centre; we have 5 nurses, and that arrangement of one nurse on duty is the arrangement they make amongst themselves’ (Rural-Data clerk). While at the urban, challenges with managing staff schedules manifested through training attendance. For example, ‘There are several nurses, but sometimes they attend training for the whole week. Today, about 12 nurses are away, and we are only 10, of which others are on night shifts, others on off duty and the remaining 5 are working in different sections’ (Urban-nurse). Rural facility HCW recommended improving staff scheduling on a shift to have a minimum of 2 nurses.
The rural facility did not provide handovers or develop task allocations since one nurse could work alone for a few days. In contrast, the urban facility delayed preparing task allocation, leading to late work, as handovers were equally finished late. As reported: ‘Sometimes we are delayed during reporting sessions in the morning or due to delays in task allocation’ (Urban-Nurse). The urban facility also had poor care organisation as MIP were sent late for testing using POC. While processing the result took 1 hour, MIP waited to receive other required services until accessing their results after 1 hour. For example: ‘This other day, a woman had to wait for her results until 2 o’clock, and when I gave her the results, she mentioned going for the vaccine. Had we checked her book, we could have advised her to go for the vaccine while waiting for the test result, but we wasted time idling while waiting for the results’ (Urban-HSA).
The HCW in both facilities understands different factors contributing to a longer time to provide services to MIP. The factors are similar in the 2 facilities, although HCWs provided different examples. HCW understand the need for organising care to improve service delivery even without additional resources.
Discussion
We evaluated the implementation of EID services in Blantyre District, Malawi, using a mixed methods approach and estimated coverage of HEI enrolment in HCC and testing at 6 weeks, assessing implementation gaps, including HCW perspectives and their recommendations. Only 24% of infants born at the study facilities were enrolled in HCC before post-natal discharge. This falls far short of the Malawi PMTCT guidelines recommendation of 100%.32,46 Process mapping at both facilities showed that some MIP were discharged at birth without being enrolled in HCC. The low proportion of HEI enrolment in HCC at birth highlights a key missed opportunity to begin monitoring HEI. Overall, 60% of HEI had HCC enrolment documentation regardless of the enrolment time by 2 months, consistent with other studies,47,48 lower than the 80% national 2018 and 2022 report.49,50
From the interviews with HCWs, contributing factors to delay in HEI initiation in HCC include shortages of staff that increased workload, as previously reported.22,24,51 However, our findings showed that poor staff schedules in urban and rural facilities worsen staff shortages. The inadequate handovers for HCW, lack of clinical student supervision, lack of screening to identify MIP and clients changing identity by using different health passport books without documented HIV status have rarely been reported. The lack of screening is not consistent with Malawi PMTCT guidelines.32,46 Some HCWs thought having a unique I.D. for women different from the national identification numbers used when initiating MIP on ART could help identify HIV-infected women who change identity using varying passport books.
Failure to recognise the MIP and providing fragmented services further led to incomplete services and MIP spending long hours at the facility. Screening of women could help identify those needing several services quickly, especially at 6 weeks, when they are recommended to receive multiple services. 46 Other studies have also reported that MIP spends long hours due to factors22,24,51 which impacts retention in HCC.52,53 Our study adds that long processing result time for the POC machine led to long waiting times while acknowledging the benefits of the POC machine.54-56 We recommend facilities with POC machines offer other recommended services whilst MIP are waiting for HIV test results and start offering HIV testing services early to accommodate the machine’s longer processing times.
The factors contributing to low HEI enrolment in HCC also contributed to low HIV ascertainment at 6 weeks, especially failing to identify MIP with minimal difference between urban with POC and rural without. Our estimation data for both facilities indicated low ascertainment at 52%, similar to global and Malawi estimates in 2018. 12 However, the UNAIDS 2022 report has shown good progress in increasing the HIV ascertainment rate for HIV-exposed infants in Malawi to 76%. 1 Notably, HCWs’ interviews revealed that the HIV ascertainment of HEI at 6 weeks remains low due to the restricted capacity of the POC machine. This is because some MIP return without a test, and others do not come back to the hospital. Our finding differs from previous studies that have solely emphasised the advantages of the POC machine.55,56 Participants in our research proposed having a booking system to ensure HCWs schedule an ideal number of clients that the machine would manage to test without returning clients. We recommend using the DBS if POC machine capacity is reached and avoiding returning clients, which could be added to the guidelines.
The lack of counselling for MIP at 6 weeks for the facility that had POC in our study was due to HCW’s role confusion, poor organisation of care and shortage of skills. Another systematic review, 57 reported similar findings for facilities without POC machines. The Malawi standard operation procedures (SOP) in EID services guide the flow of care that includes counselling for facilities using DBS and clarify roles for counselling. 32 However, we recommend an update of the SOP to include the flow of care for facilities with POC machines and mentorship on managing MIP at 6 weeks, including counselling.
The 8% of HEI that had no documentation of their test results was lower than the 25% of infants that had no documentation in Malawi in 2018, 50 similar to other studies. 57 Lack of documentation for test results leads to underreporting HIV rates, especially at a facility with a POC machine where results are available after 1 hour of testing. The HCWs reported feeling overburdened to provide several services requiring independent documentation, similar to other studies. 57 This finding suggests that although HCWs would have a result for an HEI available, they would sometimes not document if they feel they have much information to write. In such circumstances, using electronic medical records would help reduce the burden. Our study showed HCWs understand the importance of providing services simultaneously for the MIP. However, they are compelled to offer them separately due to limited human and material resources, as reported by others.22,24 Mwapasa et al. further wrote that integration of services in Malawi and other low-middle-income settings might seem unrealistic unless there are long-term investments and healthcare worker motivation, among others. 24
Limitations of our study include the use of routinely collected data for only a 1-year period, which additionally had some missing information. However, observation of the implementation and interviews with HCWs in implementing EID services helped to understand the data in detail, considering that HCWs are primary stakeholders who provide the EID services and understand the EID services implementation context. Furthermore, observation through process mapping has been used in several studies,39,41,42 to inform implementation gaps, including in Malawi. 58 The strength of this study was the follow-up of available data for all HEIs born at the study sites regardless of their enrolment status in HCC, which the national report does not account for, learning context practice gaps and policy implications. We recommend developing a context-appropriate intervention to address the implementation gaps to ensure that innovations like POC machines are optimised to improve testing at 6 weeks and develop measures to identify all HEIs from birth to the entire PMTCT cascade to avoid missing opportunities.
In this study, we found HEI enrolment in HCC and HIV testing at 6 weeks was suboptimal. Healthcare workers could not identify and provide timely comprehensive services to mothers and infants because of capacity, including the challenges of the point of care HIV testing for HEIs at 6 weeks, process and system factors necessitating context-appropriate intervention, such as measures to identify HEI within the health facility actively. Our findings align with our study question on evaluating the implementation of services for early infant diagnosis of HIV against national guidelines in Malawi. These findings are essential in planning contextually relevant, pragmatic and feasible research and interventions appropriate in adapting the WHO recommendations on integrating services and use of point-of-care HIV testing for infants at 6 weeks to contribute to ending the HIV pandemic. Our study was conducted in one urban and rural facility, which gives context for both urban and rural, but further scale-up when planning interventions may be required. We recommend future studies to develop and evaluate context-appropriate interventions and engage stakeholders to understand context meaningfully. Our study suggests that a booking system should be considered to manage appointments and provide services accommodating available resources. In conclusion, our study underpins the need to understand the context to address suboptimal HIV services.
Supplemental Material
sj-docx-1-his-10.1177_11786329231224623 – Supplemental material for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi
Supplemental material, sj-docx-1-his-10.1177_11786329231224623 for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi by Leticia Chimwemwe Suwedi-Kapesa, Alinane Linda Nyondo-Mipando, Augustine Choko, Angela Obasi, Peter MacPherson and Nicola Desmond in Health Services Insights
Supplemental Material
sj-docx-2-his-10.1177_11786329231224623 – Supplemental material for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi
Supplemental material, sj-docx-2-his-10.1177_11786329231224623 for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi by Leticia Chimwemwe Suwedi-Kapesa, Alinane Linda Nyondo-Mipando, Augustine Choko, Angela Obasi, Peter MacPherson and Nicola Desmond in Health Services Insights
Supplemental Material
sj-docx-3-his-10.1177_11786329231224623 – Supplemental material for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi
Supplemental material, sj-docx-3-his-10.1177_11786329231224623 for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi by Leticia Chimwemwe Suwedi-Kapesa, Alinane Linda Nyondo-Mipando, Augustine Choko, Angela Obasi, Peter MacPherson and Nicola Desmond in Health Services Insights
Supplemental Material
sj-docx-4-his-10.1177_11786329231224623 – Supplemental material for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi
Supplemental material, sj-docx-4-his-10.1177_11786329231224623 for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi by Leticia Chimwemwe Suwedi-Kapesa, Alinane Linda Nyondo-Mipando, Augustine Choko, Angela Obasi, Peter MacPherson and Nicola Desmond in Health Services Insights
Supplemental Material
sj-docx-5-his-10.1177_11786329231224623 – Supplemental material for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi
Supplemental material, sj-docx-5-his-10.1177_11786329231224623 for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi by Leticia Chimwemwe Suwedi-Kapesa, Alinane Linda Nyondo-Mipando, Augustine Choko, Angela Obasi, Peter MacPherson and Nicola Desmond in Health Services Insights
Supplemental Material
sj-docx-6-his-10.1177_11786329231224623 – Supplemental material for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi
Supplemental material, sj-docx-6-his-10.1177_11786329231224623 for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi by Leticia Chimwemwe Suwedi-Kapesa, Alinane Linda Nyondo-Mipando, Augustine Choko, Angela Obasi, Peter MacPherson and Nicola Desmond in Health Services Insights
Supplemental Material
sj-docx-7-his-10.1177_11786329231224623 – Supplemental material for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi
Supplemental material, sj-docx-7-his-10.1177_11786329231224623 for Process Evaluation of Services for HIV-Infected Post-Partum Women and HIV-Exposed Infants in Primary Health Care Blantyre Malawi by Leticia Chimwemwe Suwedi-Kapesa, Alinane Linda Nyondo-Mipando, Augustine Choko, Angela Obasi, Peter MacPherson and Nicola Desmond in Health Services Insights
Footnotes
Acknowledgements
This manuscript is part of PhD studies at the Liverpool School of tropical Medicine, at the Department of International Public Health. The authors would like to express their gratitude to the research assistants and all their support, all the health workers and post-partum women who participated in the study. We are thankful for the institutional support from the Malawi-Liverpool Wellcome-Trust Clinical Research Programme and College of Medicine for hosting the study and the Blantyre district health office for allowing us to conduct the study in their facilities.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: A pre-PhD internship grant funded by the joint Malawi-Liverpool Wellcome-Trust Clinical Research Programme and College of Medicine.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
LCSK contributed to the conceptualisation, protocol development, and methodology under the supervision of ALNM, PM and ND.
Formal analysis was conducted by LCSK, with discussions and inputs from ALNM, ND, PM, AC, and AO. All authors reviewed and provided feedback on the methodology and analysis and approved the final manuscript.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
