Abstract
Surgical antibiotic prophylaxis (SAP) is considered an important interventional tool for antimicrobial resistance. Guideline compliance was poor across different countries and this results in an inappropriate and overuse of antibiotics. The study was cross-sectional, combining qualitative and quantitative. The Research used the MOH’s Antibiotic Preventive Medicine Guidelines as the standard to verify surgical preventive treatment compliance from patient medical records. Research performed on 373 medical records with surgical indications. The study was conducted from January to June 2019. Data were entered using Epidata software and processed by SPSS software version 19.0. Analysis: calculating OR for related factors. The compliance rate of using prophylactic antibiotics was 83.1%. There is a relationship between the type of incision, the length of time surgery, and compliance with surgical prophylactic use of antibiotics (P < .05). Barriers to adherence to prophylactic antimicrobial therapy include: overcrowding patients, health-care workers “broad-spectrum antibiotic use habits, and health-care workers” views on surgical and muscle environment, the material was not completely sterilized.
Background
According to the WHO Global Guidelines for the Prevention of Septic Infection 2016, wound infection is caused by bacteria entering through the incisions during surgery. They threaten the lives of millions of patients each year and contribute to the spread of antibiotic resistance. In low-income and middle-income countries, 11% of surgical patients become infected in the process. In Africa, up to 20% of women, cesarean sections have wound infections, affecting their health and ability to care for their children. But wound infection is not just a problem in poor countries. In the United States, they contribute to hospital stays of more than 400 000 days at an additional cost of $10 billion a year. 1
In Vietnam, according to the report “Research on evaluation of integrated solutions to reduce the incidence of wound infections at Viet Duc Hospital, Report on the results on the topics of Science and Technology at the Ministry level” by Nguyen et al, 2 each year there is about a 5% to 10% of wound infections occurring. The consequences of surgical infections increase the cost of treatment, prolong hospital stay, and increase the use of antibiotics and possibly increase antibiotic resistance levels.
According to the guidance of the Ministry of Health of Vietnam, principles of using surgical prophylactic antibiotics (SAP) are as follows:
Principle 1. Indications for use of SAP: SAP is indicated in: all surgical interventions under clean surgery—infection. In clean surgery, SAP should apply with some serious surgical interventions that may affect survival and/or function (orthopedic surgery, heart, and blood vessel surgery, neurosurgery, ophthalmic surgery)
Principle 2. Criteria for selection of prophylactic antibiotics: Antibiotics have an effect spectrum consistent with the main strains of bacteria that often cause infection at the surgical site. Antibiotics cause little or no harmful side effects and the less toxic the better. Antibiotics do not interact with anesthetics. Antibiotics are less able to select antibiotic-resistant bacteria. The diffusion capacity of the antibiotic in cells must have a drug concentration higher than the minimum antibiotic concentration to treat infectious bacteria.
Principle 3. Medication route: Intravenous route: Often selected due to rapid drug concentration in blood and tissue.
Principle 4. Time to use the drug: The time to use the SAP should be within 60 minutes before surgery and near the time of skin incision. For patients on antibiotic treatment, on the day of surgery, the timing of antibiotics should be adjusted as close to the operation as possible. In heart surgery lasting more than 4 hours, an additional dose of antibiotics is required.3,4
Although the principles of prophylactic antibiotic use are established and some guidelines have been published, adherence to the guidelines for the use of prophylactic antibiotics in surgery is still faced with a lot of limitations. Some common reasons are the difficulty that health workers have not been updated with knowledge, improper habits on the use of preventive antibiotics, and lack of policies.5-7,12
Musmar et al conducted a retrospective study in 3 Palestinian public hospitals in 2011 published in the journal BMC Surgery (2014) showed the results: Overall compliance for the studied parameters was very low (2%); only 59.8% received their first dose at an inappropriate time, 18.5% had an appropriate antibiotic selection, and 31.8% of patients received antibiotics inappropriate duration. Surgical duration is also directly related to the risk of postoperative surgical site infection.5,8,9
Chi et al conducted a study “Evaluation of compliance with surgical preventive birth regimen at VINMEC TIMES CITY” international hospital in 2018 showed the following results: The compliance rate of general prophylactic antibiotic regimen reached 60.5%, in which compliance with dose, route of administration and repeated dose in surgery was quite high (96%). Compliance with selection and starting point was about 87%. The criterion with the lowest level of compliance was the contingency length with 74.8%. There are 25.2% of the extended antibiotic prophylaxis. 9 Van Thanh et al through research on the use of preventive antibiotics in surgery at the Department of General Surgery of Duc Giang Hospital in 2014, the results: out of 83 surgical cases, all using preventive antibi preventive antibiotics. Among these 83 surgical cases, they fully complied with regulations on using preventive antibiotics of the Ministry of Health. 6 According to the Report on Medical Examination and Treatment of Thu Duc District Hospital 2018, this is a class I hospital, with 1000 beds with the number of surgeries in 2019 is 23 450. With the large number of patients being treated at the surgical treatment departments, the overload of the beds is the most concern of the leaders of the surgical treatment units. To limit hospital infections (due to overloading of beds) and antibiotic resistance; the use of prophylactic antibiotics has been deployed in surgical treatment units—Thu Duc District Hospital. However, to what extent is the compliance with the use of prophylactic antibiotics of Thu Duc District Hospital achieved? And what factors affect compliance with prophylactic antibiotic use? The matter is to have adequate information. To answer those questions, we implement the topic: “Current situation of compliance with the use of prophylactic antibiotics in surgery at the hospital in Thu Duc district, Ho Chi Minh City in 2018.”
Objectives
Describe the current situation of compliance in the use of surgical antibiotic prophylaxis at Thu Duc District Hospital, Ho Chi Minh City in 2018.
Identify the factors related to the compliance rate of use of surgical antibiotic prophylaxis at Thu Duc District Hospital, Ho Chi Minh City in 2018.
Material and Method
Research subjects
Medical records of patients treated with surgery at 6 departments; Team of doctors, pharmacists, and nurses at 6 departments; 6 department leaders.
Time and place
The study had been carried out from January to July 2018 in Thu Duc District Hospital, Ho Chi Minh city, Vietnam.
Research design
Applied cross-sectional design.
Sampling method
Total sampling method was applied, selected all the medical records of patients treated with surgery with clean and clean-contaminated wounds at 6 departments (ENT, Urology-andrology, Obstetrics, Oncology, General Surgery, and Trauma-orthopedic). A total of 724 medical records of 724 patients met the criteria for sampling and selection.
Quantitative data collection
Collecting data from medical records of clinical & para-clinical characteristics, patients’ clinical/research subjects. Use the checklist to assess compliance in the use of prophylactic antibiotics of the medical staff at 6 departments. Investigators: 6 nurses at Thu Duc district hospitals (those nurses do not work at 6 departments selected to gather information).
Results
Characteristics of patients
The study was carried out on 6 departments. A total of 724 subjects were studied, including: ENT 133 (18.40%); Urology-andrology 126 (17.4%), Obstetrics 113 (15.6%); Oncology 86 (11.9%); General surgery 160 (22.1%); Trauma-orthopedic 106 (14.6%).
Characteristics of patients
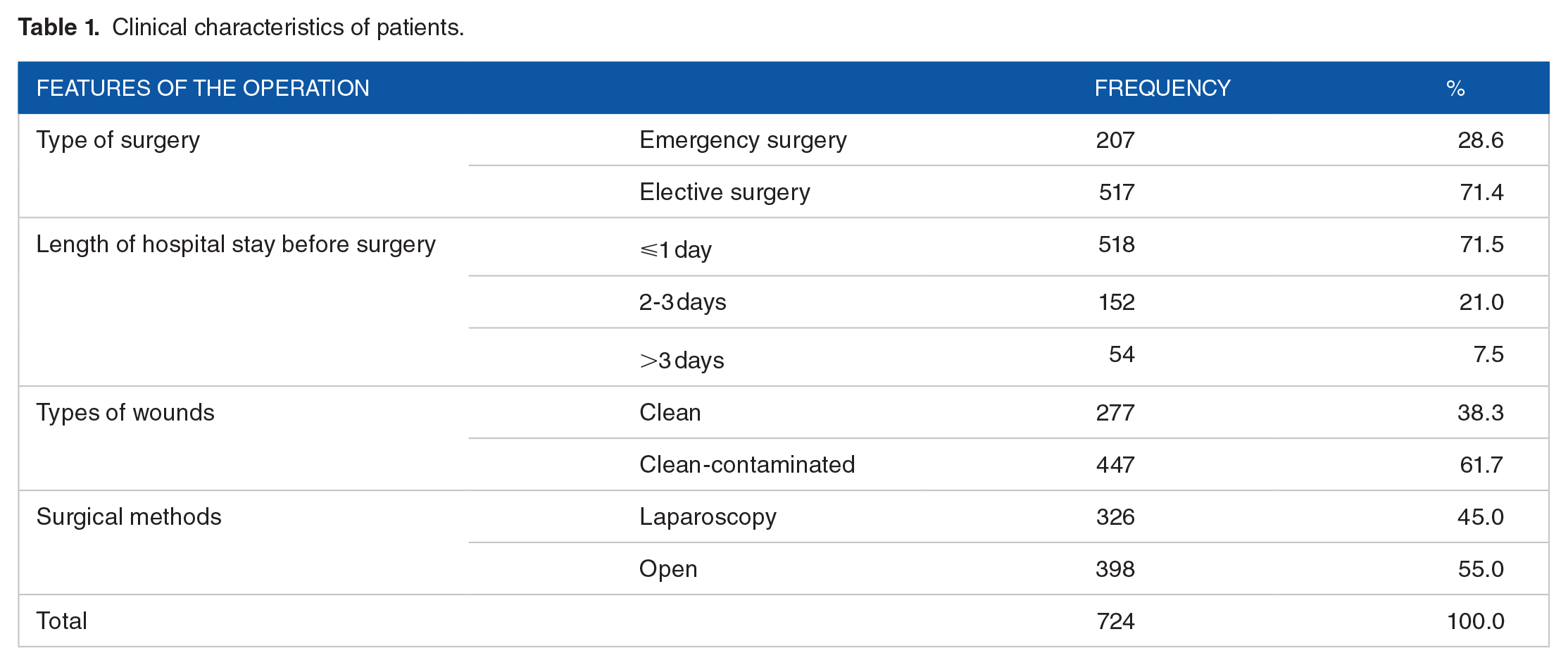
Table 1 indicates that in 724 medical records of patients treated with surgery, 71.4% of medical records are of patients who underwent elective surgery and the remaining 28.6% are of patients who underwent emergency surgery. For cases of emergency surgery, the use of prophylactic antibiotics is often more difficult than an elective surgery. Length of hospital stay before surgery: the rate of patients with a hospital stay of less than 1 day was 71.5%. Type of wound: As a general rule, the use of prophylactic antibiotics applies only to patients who perform a clean wound (type I) or a clean-contaminated wound (type II). Among 724 medical records selected in our study, the rate of patients with a clean-contaminated wound (type II) was (61.7%). Method of operation was 45.0% of cases underwent endoscopy.
Clinical characteristics of patients.
Surgical sites of 724 patients were divided into 10 categories, in which the abdominal surgeries accounted for 28% which was a high rate, and the limb surgery only accounted for 2, 6% (Figure 1).

Surgery site.
Table 2 shows the situation of using antibiotics before admission: 94.6% of patients did not use antibiotics before admission to Thu Duc district hospital.
Use of antibiotics before hospital admission.

Compliance with the regimen in use of prophylactic antibiotics
Use of prophylactic antibiotics
In 724 medical records, we recorded that 48.3% (350/724 medical records) used prophylactic antibiotics. Among 350 patients using prophylactic antibiotics, some groups of antibiotics are widely used such as Cephalosporin, Vancomycin, Moxifloxacin, Aztreonam, and the most used group of antibiotics is Cephalosporin (222/350) 63.4%.
Current use of prophylactic antibiotics
Use of antibiotics at 6 departments
Table 3 show that among 724 medical records of patients selected from the archives of 6 departments (Otorhinolaryngology, Urology-andrology, Obstetrics, Oncology, General Surgery, and Orthopedic), 51.7% (374/724) were of patients undergoing surgical treatment without prophylactic antibiotics. The proportion of medical records of patients treated with antibiotics after surgery is accounted for 4.3%.
The use of antibiotics.

Compliance with prophylactic antibiotics use
Among 350 medical records of patients prescribed with prophylactic antibiotics, 78.0% were treated with the type of prophylactic antibiotics complying with the regimen of Thu Duc district hospital.
According to the protocol of prophylactic antibiotics, the antibiotic is injected into the patient within 30 minutes before the skin incision. Table 4 shows that 73.4% of patients were treated complying with the timing of the use of prophylactic antibiotics.
The use of prophylactic antibiotic treatment in compliance with the department’s regimen.

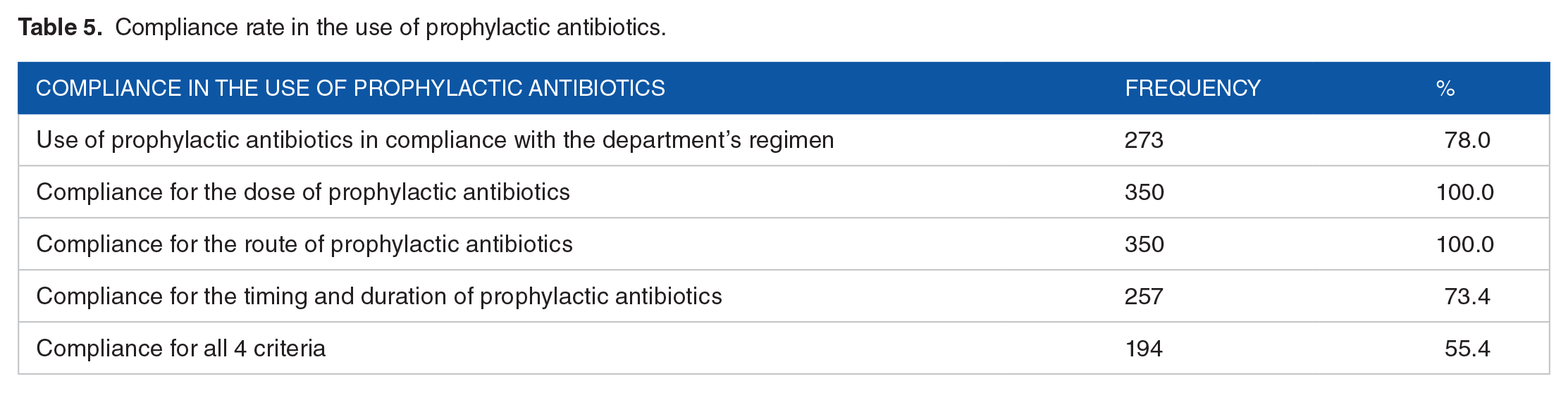
Table 5 indicates that among 350 medical records of patients using prophylactic antibiotics, 100% shows compliance with the dose and route of prophylactic antibiotics. A total of 55.4% of medical records fully comply with 4 criteria for the use of prophylactic antibiotics.
Compliance rate in the use of prophylactic antibiotics.

Some factors related to the prophylactic antibiotics treatment in compliance with the regimen of Thu Duc District hospital in 2018
Factors from the patients
Comments: there was a correlation (P < .05; OR = 1.291) between the group of patients and their disease with the compliance with the regimen on prophylactic antibiotic use. The group of patients without comorbidities complied with the regimen of prophylactic antibiotics 1.291 times higher than the group of patients with comorbidities.
There was a correlation (P < .05, OR = 1.539) between the patient’s wound and compliance with the regimen on prophylactic antibiotic use. The group of patients with clean-contaminated wounds (type II) complied with the regimen of prophylactic antibiotics by 60.3% over patients with clean wounds (type I) at 49.7%. The group of patients with type II wound complied with the regimen of use of prophylactic antibiotics was 1.539 times higher than the group of patients with type I wound.
There is no correlation (P > .05; OR = 1.535) between the group of patients with the use of antibiotics before surgery with compliance with the regimen of prophylactic antibiotic use.
There is a correlation between the duration of hospital stay with the use of prophylactic antibiotics/treatment with antibiotics. Patients with a treatment duration of 5 days used prophylactic antibiotics rate (21.0%) lower than in patients with a treatment duration of 5 days or less (50.9%), differences statistical significance P < .05.
There is a correlation (P < .05; OR = 1.956) between the type of surgery with regimen compliance on prophylactic antibiotic use. Compliance on prophylactic antibiotics for emergency surgery patients (44.9%) was lower than that of patients receiving elective surgery (61.45%).
There was a correlation (P < .05; OR = 1.221) between the surgical method and the compliance with the regimen of prophylactic antibiotics. Patients with laparoscopic surgery comply with the use of prophylactic antibiotics 1.221 times higher than patients undergoing open surgery.
There is a correlation (P < .05; OR = 2.784) between the surgery with the compliance with the regimen of prophylactic antibiotics. Cases of patients with the surgical time of 120 minutes or less comply with a regimen of prophylactic antibiotics 2784 times higher than cases when the surgeries take more than 120 minutes.
There is no correlation (P > .05; O = 1.105) between the number of days in the hospital and the compliance with prophylactic antibiotics prescription.
There is a correlation (P < .05; OR = 2.372) between the supervision and inspection procedures of hospital infection prevention with the compliance with the regimen of prophylactic antibiotic use. Patients at departments with good supervision and inspection of prevention procedures are treated with prophylactic antibiotics 2372 times higher than those at the department with the supervision and inspection of prevention procedures which are not good.
Discussion
Type of surgery
The data in Table 1 show that: Among 724 medical records of patients undergoing surgical treatment in our samples, there are 71.4% of patients undergoing elective surgery, and 28.6% rest are of patients undergoing emergency surgery. For emergency surgery, the use of prophylactic antibiotics is often more difficult than in the case of an elective surgery when the surgeon and the nurse can better prepare the patient. Phan Van Thach’s study showed that 54.2% of patients at Duc Giang Hospital General Surgery had emergency surgery, almost twice as high as our data; Maybe perhaps our research subjects are more diverse with about 6 surgical treatment departments while Phan Van Thanh is only in General Surgery. 9
Type of wound
Table 1 shows that: According to the general principle, prophylactic antibiotics are used only for patients with clean wounds (type I) or clean-contaminated (type II). Among 724 medical records selected in our study, the rate of medical records of patients with clean-contaminated wounds is 61.7%. The rate of type II wounds in surgical patients (with prophylactic antibiotics) in the General Surgery Department of Duc Giang Hospital (in 2014) was 60.3% of patients similar to our study. 6 According to the literature, type I wounds have a risk of wound infection by less than 2%, while type II wounds have a risk of wound infection by 4% to 10%. 6 Thus, the wound condition is often related to the use of prophylactic antibiotics in surgical departments.
Method of operation
The surgeon will decide the method of operation according to the patient’s condition, the type of wound, and the type of disease. Data in Table 1 show that 45.0% of cases are endoscopies. This rate is lower than Phan Van Thanh’s study, which shows that there are 55.0% of patients undergoing endoscopy. 6 The difference is probably due to the difference in patients, because endoscopy is usually applied to laparoscopic surgery and obstetrics while in our research, diseases requiring surgery are very diverse.
Use of antibiotics before hospitalization
Table 2 shows that, the proportion of medical records of patients who have used antibiotics before hospitalization is 5.4% (39/724). Huong 7 stated that 21.6% of patients used antibiotics before being hospitalized for endoscopic cholecystectomy at Hanoi Medical University hospital. In case of the use of antibiotics before surgery, the surgeons often consider before deciding whether or not to use prophylactic antibiotics. In the next section about the analysis of the factor concerning the use of prophylactic antibiotics, we will take a closer look at this question.
Surgical duration
Table 6 show that: Surgical duration is also directly related to the risk of postoperative surgical site infection. According to Hang Cheng et al: The likelihood of SSI increased with increasing time increments; for example, 13%, 17%, and 37% increased likelihood for every 15 minutes, 30 minutes, and 60 minutes of surgery, respectively. The longer the exposure of the surgical site to the environment, the more becomes favorable the wound is to cause surgical site infection. 10 In our study, surgery duration was categorized into 2 groups: 120 minutes or less accounted for 92.0% and over 120 minutes only 8.0%. The average surgery duration was 55.8 ± 68.4 minutes (the shortest was 15 minutes and the longest 690 minutes).
Disease status and treatment associated with compliance with prophylactic antibiotic use.

Length of hospital stay
The number of days hospitalized is also a risk factor for incision infection after surgery, especially for patients whose hospital stay is longer than 30 days. 10 Table 6 show that: Among 724 medical records of the study sample, there were 62/724 cases with the number of days hospitalized for treatment of more than 5 days, accounting for 5.0%; especially, there were 6 cases with more than 30 days of hospital stay. The average number of hospital stay was 5.4 ± 4.5 days (the shortest was 2 days and the longest 57 days), length of hospital stay is also the reason to increase the rate of infection. 10
Current situation of prophylactic antibiotics treatment
Use of prophylactic antibiotics in 6 departments
The data in Table 3 show that the rate of use of prophylactic antibiotics of 724 patients undergoing surgical treatment in 6 departments (Otorhinolaryngology, Urology-andrology, Obstetrics, Oncology, General Surgery, and Orthopedic) of Thu Duc district hospital in the first 5 months of 2018 was 48.3%. According to Huy et al, 11 the percentage of medical records of patients with laparoscopic cholecystectomy at Gia Dinh People’s Hospital using prophylactic antibiotics accounted for 67.4% in 2009 to 2011. The above citations show that the percentage of medical records of patients undergoing surgical treatment using prophylactic antibiotics in our study is lower than in the cited researches. The difference is due to many factors such as the type of disease and the subject of surgery, the method of surgery, the hospital environment.
Use of prophylactic antibiotics complying with the regimen of the Department: Selection of antibiotics for use in prophylactic antibiotics is the first principle. Accordingly, the selected antibiotics must be appropriate for the pathogenic bacteria based on the frequency of common bacteria of each type of surgical treatment and their sensitivity. Antibiotics used should be concentrated enough and remain long enough in the tissue during surgery, and not be harmful to the body (allergies, kidney failure . . .). Finally, it is necessary to choose antibiotics that are not too expensive and do not interact with anesthetics. 13 In our study, the percentage of medical records of the patient treated with prophylactic antibiotics complying with the Department’s regimen was 78.0%; this rate is lower than the 1 reported in the study of Thoa 13 (90.0%). Gouvêa et al 14 reported that according to 10 studies in Europe about compliance with the regimen when using prophylactic antibiotics, the rate of compliance with the regimen in terms of the type of antibiotics varied from 22.0% to 95.0%. Compliance of type of antibiotics for prophylactic antibiotics in different Departments is very complicated.
Prophylactic antibiotics dose adherence: In our study, there were 350 medical records of patients using prophylactic antibiotics and all (100%) of these cases were dose-adherent according to the instructions for use of prophylactic antibiotics in Thu Duc district hospital. The rate of prophylactic antibiotics dose adherence in the study of Thoa 13 was 68.0%.
Factors concerning compliance with prophylactic antibiotics
Table 6 show that: Among 350 medical records using prophylactic antibiotics, there were 189 medical records of patients with type II wounds (clean-contaminated) and the statistics showed a correlation (P < .05; OR = 1539) between the type of patient’s wound and compliance with regulations on the use of prophylactic antibiotic. The medical records of patients with type II wounds (clean-contaminated) treated with prophylactic antibiotics complying with the regimen were 1539 times higher than the medical records of a patient with a clean wound (type 1). According to a research by hospital Vinmec Times City, the compliance rate of use of prophylactic antibiotics in patients with clean wounds and clean-contaminated wounds was similar (96.6% and 95.7%) which is higher than our data (49.7% and 60.3%). 9
Use of antibiotics before surgery versus prophylactic antibiotics: Table 6 show that: no association has been found between antibiotic use before surgery and prophylactic antibiotic use. Medical records of patients who used antibiotics before surgery then treated with prophylactic antibiotics complying with the regimen accounted for 34.5%, lower than the medical records of patients without antibiotic prior to surgery (57.3%), however, this difference is not statistically significant, P > .05.
Factors about the surgery
Table 6 shows that: Type of surgery and the use of prophylactic antibiotics in compliance with the rules: there is a relation (P < .05, OR = 1.956) between the type of surgery with the use of prophylactic antibiotics in compliance with the rules. Medical records of the group of patients undergoing emergency surgery with prophylactic antibiotics accounted for 44.9%, lower than the medical records of the group of patients undergoing elective surgery which is 61.4%. This result shows that for emergency operations, the surgeon needs to pay more attention to prescribing prophylactic antibiotics.
Type of surgery and the use of prophylactic antibiotics complying with the rules: there is a relationship between type of surgery (endoscopy or open surgery) and the use of prophylactic antibiotics in compliance with the rules. Table 6 show that: Patients who underwent endoscopic surgery with prophylactic antibiotics treatment in compliance with the rules were 1.221 times higher than those of patients undergoing open surgery. The factors concerning patients undergoing open surgery are more complicated than those undergoing endoscopy, thus the use of prophylactic antibiotics complying with the rules is more difficult in these cases.
Surgical timing and the use of prophylactic antibiotics complying with the rules: In our study, we found a relation (P < .05; OR = 2.784) between the surgery timing and the use of prophylactic antibiotics complying with the rules. Medical records of the group of patients with surgery duration of 120 minutes or less with prophylactic antibiotics treatment in compliance with the rules were 2.784 times higher than those with surgery duration above 120 minutes. Research by Huong showed that there was no relationship between the surgery duration and the use of prophylactic antibiotics, P > .05; it could be explained by the fact that there is various type of diseases in our research while Huong 7 only studied on 1 disease (laparoscopic cholecystectomy) so this difference is explainable. Hospital stays with prophylactic antibiotics treatment complying with the regimen: patients with stays of less than 5 days with prophylactic antibiotics treatment in compliance with the rules accounted for 55.2%, lower than those with 5 or more days of hospital stays (57.7%). However, this difference was not statistically significant, P > .05.
Hospital infection control: we figured out the relation between the supervision and inspection of prevention procedures and the compliance with regulations on the use of prophylactic antibiotics. Medical records of patients at departments with good supervision and inspection of prevention procedures are treated with prophylactic antibiotics 2.372 times higher than those at the department with the supervision and inspection of prevention procedures which are not good.
Implication
This research showed that the rate of compliance with a regimen of prophylactic antibiotics in surgery in both separate compliance dimensions and full compliance were inadequate. And it also found out some factors which are considered barriers to adherence to prophylactic antimicrobial therapy. Results of this research should be suggestions for hospitals to apply measures to enhance the rate of compliance with prophylactic antibiotic in specific and improve hospital quality in general.
Conclusions
Current status of compliance with a regimen of prophylactic antibiotics in surgery
The rate of using prophylactic antibiotics is different between department: 4.9% at the ENT department and the highest rate was recorded at Surgical Department at 22.6%; Compliance on prophylactic antibiotics accounted for 78.0%; Compliance on the timing of prophylactic antibiotics accounted for 73.4%; Full compliance rate of 4 regulations on the use of antibiotic prophylaxis 55.4%.
Some factors related to compliance with prophylactic antibiotic use in surgery
Group of patients without comorbidity comply with prophylactic antibiotics used 1291 times higher compared to patients in comorbidity; Group of patients with type II wound are treated with prophylactic antibiotics 1.539 times higher than the group of patients with type I wound. Patients with a surgical time of 120 minutes or less are treated with prophylactic antibiotics 2.784 times higher than patients with surgical time over 120 minutes; Patients prescribed with prophylactic antibiotics who underwent treatment duration of 5 days (21.0%), lower than those underwent a treatment duration of 5 days or less (50.9%), the difference was statistically significant with P < .05, OR = 4.275.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
Phan Van Tuong, Chu Huyen Xiem, Nguyen Chi Anh and La Ngoc Quang contributed to the design and implementation of the research, to the analysis of the results and to the writing of the manuscript.
