Abstract
Background:
The use of prophylactic antibiotics in routine knee arthroscopy remains prevalent despite previous evidence suggesting that it may not be necessary, and may indeed carry more risks than benefits. This study aims to determine the incidence of surgical site infections in patients undergoing routine knee arthroscopy without prophylactic antibiotics.
Methods:
This is a retrospective review of 553 consecutive patients who underwent routine knee arthroscopy from 2004 to 2013 by a single fellowship-trained sports surgeon in a single institution. The spectrum of cases included arthroscopic meniscectomy, meniscal repair, microfracture, chondroplasty, removal of loose bodies and lateral retinacular release. No patient received any prophylactic antibiotics. Patient demographics and comorbidities were reviewed and all patients were followed up postoperatively for a minimum of two years. All postoperative complications were recorded.
Results:
There were 349 male and 204 female patients. The mean age was 41.8 years (SD 14.8) and mean operative time was 30.4 minutes (SD 12.3). Two healthy young patients developed postoperative superficial wound infection within one week after surgery, but recovered with outpatient oral antibiotic treatment. The overall infection rate was 0.36%. No cases of deep infection were reported.
Conclusion:
This study showed a very low rate of surgical site infections, comparable with known rates following such operations. This suggests that prophylactic antibiotics are not necessary and avoids the known risks associated with their use.
Introduction
Knee arthroscopy is a common orthopaedic procedure that is routinely used both for diagnostic and therapeutic purposes. This technique was introduced in 1970 and has gained popularity over time because of fewer complications, shorter operative duration, and length of hospitalisation compared to traditional open surgery.1,2 Although routine knee arthroscopic procedures are generally considered clean procedures with low postoperative infection rates,3–9 the use of prophylactic antibiotics remains prevalent because of the widespread belief that they can prevent potential surgical site infections. 10 In 2007, Bert et al. addressed this topic in a study that included 3231 patients and included a control of patients that received antibiotics. The infection rates were comparable, at 0.15% and 0.16%, respectively. 9 Additionally, Wieck and colleagues performed a study similar to this, but the methodology was a prospective, randomised, double-blinded study of 437 patients. Again, there were no cases of deep infection, one case of superficial infection in a patient who did not receive antibiotics, and one minor allergic reaction. 7 The purpose of this study is to determine the incidence of such infections in patients who underwent routine knee arthroscopy without prophylactic antibiotics. The hypothesis is that prophylactic administration of antibiotics prior to routine knee arthroscopies is not necessary in the prevention of surgical site infections.
Methods
This is a retrospective review of 553 patients who underwent routine knee arthroscopies over a 10-year period from January 2004 to December 2013 by a single fellowship-trained sports surgeon in a teaching hospital. The simple knee arthroscopies included in this study were arthroscopic meniscectomies, meniscus repair, microfractures, chondroplasties, removal of loose bodies and lateral retinacular releases. Complex knee arthroscopic procedures such as anterior cruciate ligament (ACL) reconstructions, meniscus transplant, procedures associated with fracture and septic knee were excluded from this study. None of the patients received any prophylactic antibiotics. Patient comorbidities were duly recorded in an electronic documentation sheet.
All of the knee arthroscopies were performed under general anaesthesia. Tourniquets were applied and inflated for all procedures. Patients’ knees were shaved with one-time use disposable surgical clippers, coated with povidone iodine solution, and subsequently given three minutes drying time prior to the incision. The incision was closed with interrupted sutures using Ethilon 4-0 (Ethicon, NJ). All patients either went home the same day or were hospitalised for one day. Patients who stayed overnight usually did so for insurance claimage purposes. They were routinely followed up in the outpatient clinic at two weeks, six months, one and two years post-surgery.
The parameters assessed include age, gender, body mass index, duration of surgery and comorbidities. The demographic data were analysed using SPSS version 21 (SPSS Inc, Chicago, IL, USA).
Results
There were 349 (63.1%) men and 204 (36.9%) women with a mean age of 41.8 years (range, 15–81 years). The average duration of surgery was 30.44 minutes (range, 10–80 minutes). A total of 491 patients (88%) underwent arthroscopic meniscectomies. The rest were microfractures, removal of loose bodies and synovectomy/debridement. The types of patient comorbidities include diabetes mellitus (7.2%), hyperlipidaemia (15%), hypertension (18.3%), chronic renal disease (0.7%) and ischaemic heart disease (2.5%) (Tables 1 and 2).
Demographic Data & Clinical Details Co-morbidities of patients in the study.

Age Distribution of patients in the study.

Two young healthy patients complained of mild pain and erythema around their surgical wounds and were seen within one week in the outpatient clinic. On clinical examination they were noted to have developed superficial wound infections without any knee effusion. Range of motion of the knee was full at 0–130 degrees. No cultures were taken from either patient. Both patients were prescribed outpatient oral antibiotics and recovered well. There were no cases of deep infections, and our overall infection rate was 0.36% (Table 3).
Demographics and Clinical Details of patients with superficial surgical site infections.
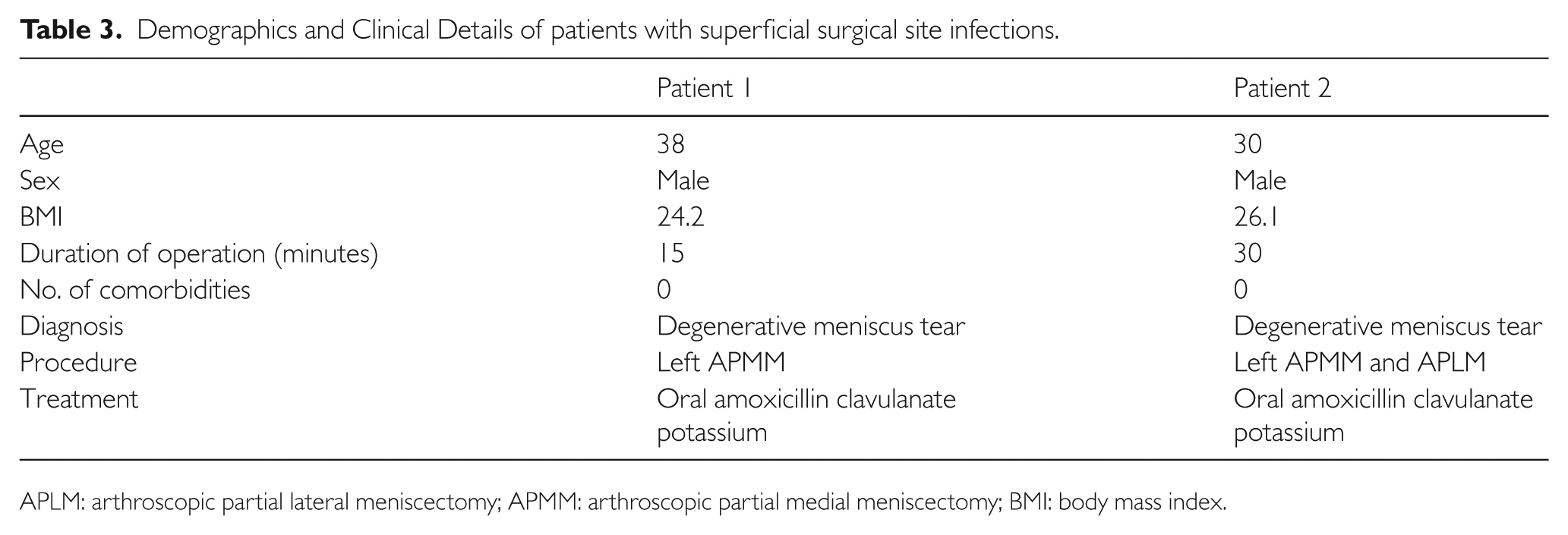
APLM: arthroscopic partial lateral meniscectomy; APMM: arthroscopic partial medial meniscectomy; BMI: body mass index.
Discussion
Wieck et al. conducted a prospective, randomised, double-blind study consisting of 437 individuals that concluded that there was no evidence that antibiotic prophylaxis reduces the rate of infection after arthroscopic surgery. 7 In addition, Bert and colleagues conducted a survey showing that most orthopaedic surgeons still used prophylactic intravenous antibiotics for routine knee arthroscopy, primarily because prophylactic antibiotics are perceived as the standard of care, along with the fear of litigation should surgical site infections occur if prophylactic antibiotics were not used. 9 Based on the low rate of surgical site infections, the senior author of this study does not use prophylactic antibiotics in routine knee arthroscopy. Studies have shown that the overall risk of infection is increased with foreign-body insertion such as ACL implants.10–12 Such patients were excluded from this study because prophylactic antibiotics were given to them.
There are a few factors that may have contributed to the low infection rates in the study. Firstly, the knee arthroscopies were performed electively and are generally considered clean procedures. According to Cruse and Foord, the infection rates of clean procedures are approximately 1% to 2%.13,14 Secondly, short hospital stays also contributed to low infection rates; patients were routinely discharged on the same or first postoperative day and the duration of hospitalisation stay was minimised to reduce the risk of hospital-acquired infections. Thirdly, skin preparation and shaving in all the patients, which are critical steps in preventing surgical site infections, were standardised. The skin is colonised by many different bacteria with half of them being
The reported incidence of post-knee arthroscopy surgical site infections ranges from 0.01% to 0.48%.3–9 However, numerous studies that focused on such infections were subjected to self-reporting bias and lacked uniformity in defining infections. 8 This was until the United States (US) Centers for Disease Control and Prevention introduced the classification of surgical site infections in 1992 into superficial, deep incisional, and organ or space surgical site infections. 19 In our study, superficial and deep wound infections alike were screened retrospectively through the stipulated 10-year archiving of clinical consultation records in the institution. There were only two superficial wound infections reported and no deep wound infections. The infection rate of 0.36% is within the reported range of published literature.
With regards to risk factors for post-arthroscopy infections, Sherman et al. found that patient age (> 50 years) and tourniquet time (> 60 minutes) were statistically significant risk factors for major complications in arthroscopy surgery. 11 These risk factors were not reflected in the study though. Both patients with superficial wound infections were age 30 and 38, respectively, and tourniquet time was 15 and 30 minutes, respectively (Table 2).
Diabetes mellitus has been linked to poorer outcomes in orthopaedic surgeries, with higher rates of surgical site infections reported. 20 In this study, 40 patients (7.2%) had concomitant diabetes mellitus, but none of them developed surgical site infections. In fact, both patients who had superficial infections were healthy individuals with no comorbidities.
Surgical site infections usually present clinically as pain and swelling between the first and second postoperative weeks.
8
The two patients presented with pain and erythema over their surgical sites on the second postoperative week but were clinically non-septic and recovered promptly with oral antibiotics without the need for hospitalisation nor surgical debridement. However, it is important to note that there are reports in the literature that revealed that infections can occur even up to four months post-surgery and a delayed diagnosis of infection with coagulase-negative
To date, there is inconclusive evidence showing that administering prophylactic antibiotics results in lower infection rates in knee arthroscopy. In addition, unnecessary usage of prophylactic antibiotics might lead to drug-related complications, such as allergies, anaphylactic reactions, as well as the promotion of multidrug-resistant bacteria.
22
As in all forms of medical treatment, medical practitioners need to be mindful of the risk-benefit weightage with regards to administering prophylactic antibiotics. For example, side effects of cephalosporin, which include gastrointestinal-related symptoms like nausea or vomiting (30% incidence) and hypersensitivity (up to 5% incidence) when given intravenously 27 far outweigh the risk of post-routine knee arthroscopy surgical site infections (0.01% to 0.48% incidence, 0.36% in the study). We would therefore need to question the wisdom of giving prophylactic antibiotics for routine knee arthroscopy.
Another issue to consider is the cost associated with the use of prophylactic antibiotics. Overutilisation of medical resources can contribute to high healthcare costs. A report by Thomson Reuters in 2010 found that waste in the US healthcare system due to unnecessary healthcare services was $210 billion. 28 A study conducted by Schultz and colleagues on cost impact of redundant antimicrobial therapy in US hospitals found that $163 million could potentially be saved annually. 29 On the other hand, there are two studies that assessed the cost effectiveness of giving prophylactic antibiotics in knee arthroscopy and support its use.6–8 The spectrum of knee procedures in both studies included cruciate ligament reconstruction, meniscal procedures and chondroplasty. Both studies reported superficial and deep knee infections secondary to knee arthroscopy that required hospital admission for repeated surgery and prolonged antibiotics course. D’Angelo and Ogilvie-Harris and Babcock and colleagues stated the cost of care and treatment was approximately US$5000 per single case, and prophylactic antibiotics could have possibly reduced these complications.6–8 However, when looking only at routine knee arthroscopies without reconstructive procedures performed, as in this study, no patients were re-hospitalised as a result of postoperative infections. A prophylactic regimen with cefazolin costs approximately US$6.55 per gram. 30 A national survey from the US showed that 900,000 knee arthroscopic procedures were performed in 2006, and this number represented a 49% increased since 1996. Among those, 100,000 knee arthroscopies were performed for ACL reconstruction. 31 If we exclude the ACL procedures, the estimated cost for the prophylactic antibiotics alone for the 800,000 knee procedures is about $5.2 million. This illustrates the huge spending that could potentially be saved if prophylactic antibiotics were not given routinely for such operations.
As mentioned earlier, the majority of orthopaedic surgeons still employ prophylactic antibiotics in routine knee arthroscopy procedures as shown by Bert et al. 9 This study questions the need to continue such a practice. Large, randomised, multicentre studies may be useful to further validate our finding that prophylactic antibiotics are not necessary for routine knee arthroscopy, which may then lead to standardisation of prophylactic antibiotic protocols across all hospitals.
Limitations of this study include that it is a retrospective study with a limited number of patients, all of whom were treated at the same hospital. There was also no control group to compare outcomes.
Conclusion
This study shows a very low rate of surgical site infections following routine knee arthroscopy. This is comparable to previously published data, with or without the use of prophylactic antibiotics. This suggests that the use of prophylactic antibiotics is not necessary in such operations, with its purported benefit of lowering infections rates far outweighed by its associated risks.
Footnotes
Authors’ contributions
The first author wrote the manuscript and the last author edited and approved the final version of the manuscript. The second author contributed to the analysis and interpretation of the data.
Availability of data and materials
The datasets generated and/or analysed during the current study is held by the corresponding author. Patient data has not been made available publicly to protect patient confidentiality
Conflict of Interest
None declared.
Ethical approval
Ethical approval was not needed.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Informed consent
Informed consent was not sought for the present study because this was an observational study.
