Abstract
Pregnancy-associated breast cancer (PABC) is the most prevalent invasive cancer in pregnant women, notably affecting those aged over 35 years. Postpartum cases exhibit a poorer prognosis than non-PABC women, while the prognosis of PABC is the same as that of non-PABC. Our case report presents a 25-year-old, 20th-week pregnant woman. Abdominal ultrasound revealed hepatic metastases; thus, total body PET/MRI without contrast exhibited two breast masses, bilateral axillary nodules, multiple hepatic metastases and osseous metastases in vertebral column, pelvis, and femoral bones. In conclusion, whole-body MRI (WB/MRI) and PET-MRI are important tools for diagnosing breast cancer in pregnant women and determining the stage of it.
Background
Breast cancer (BC) stands as the predominant malignancy affecting women worldwide. This disease exhibits significant heterogeneity, manifesting diverse molecular profiles categorized into three primary subtypes based on hormone receptor status (estrogen receptor [ER] and progesterone receptor [PR]) and Human Epidermal Growth Factor Receptor 2 (HER2) (Erythroblastic Oncogene B ERBB2) status: luminal ER-positive and PR-positive, further classified into luminal A and B, HER2-positive, and triple-negative breast cancer (TNBC). 1 High-income countries exhibit higher incidence rates of breast cancer. 2 The global age-standardized incidence rate in females is estimated at 48/100 000, ranging from under 30/100 000 in sub-Saharan Africa to over 70/100 000 in Western Europe and North America. 2 Breast cancer is the fifth leading cause of cancer-related deaths globally, accounting for 685 000 fatalities in 2020. 3 Mammography is frequently used as the primary diagnostic method for early detection of breast cancer in Europe and the United States, early detection methods demonstrate efficacy in reducing breast cancer mortality. Recent studies have indicated that breast ultrasound, when used alongside mammography, could enhance the diagnosis of breast cancer and may potentially emerge as a primary method for breast cancer diagnosis, particularly for women with dense breasts. 3
Pregnancy-associated breast cancer (PABC) is the most prevalent invasive cancer in pregnant women, notably affecting those aged over 35 years. The rise in PABC cases is attributed to the trend of women delaying childbearing, representing 1 in 3000 breast cancer patients. 4 When matched for prognostic factors, PABC diagnosed during pregnancy has a prognosis equivalent to non-PABC. However, postpartum period cases exhibit a poorer prognosis than stage-, age-, and diagnosis year-matched non-PABC patients. 5 Magnetic resonance Imaging (MRI), with its superior soft-tissue contrast resolution, multiplanar capability, and lack of ionizing radiation, is optimal for imaging during pregnancy. 6
This case report discusses the importance of whole-body MRI (WB-MRI) and (PET/MRI) in diagnosing breast cancer in pregnant women and its role in accurately determining the stage of the disease.
Case Report
A 25-year-old woman presented to our clinic at the Daffodil 88 Comprehensive Cancer Center in Damascus 4 months ago. At initial presentation (5 months pregnant). She reported experiencing bilateral mammary pain, upper quadrant abdominal pain, and generalized bone pain, particularly in the pelvis, vertebral column, and right femur. A medical examination revealed palpable masses in both breasts with clinical axillary lymphadenopathy. Abdominal examination revealed enlargement consistent with gestational age.
Her medical history indicated a familial predisposition to breast cancer, with both her mother and sister having been affected. She was married at the age of 16 and had given birth to four children. She had no history of hypertension or diabetes and was a non-smoker and non-alcoholic.
Abdominal ultrasonography confirmed a gestational age of 19 weeks with adequate amniotic fluid levels. However, it also revealed multiple hepatic metastases of varying sizes and slight hepatic enlargement, as shown in Figures 1 and 2. Thoracic and lumbar spine evaluations, along with myelogram, were normal (Figure 3).

Demonstrates total body MRI. (A) and (B) Total body MRI showing normal brain and two fetal positioning, (C) total body MRI with PET-like image showing measurements of bilateral breast masses and hepatic metastases, (D) a total body MRI showing bone metastasis in the upper third of the right femur.
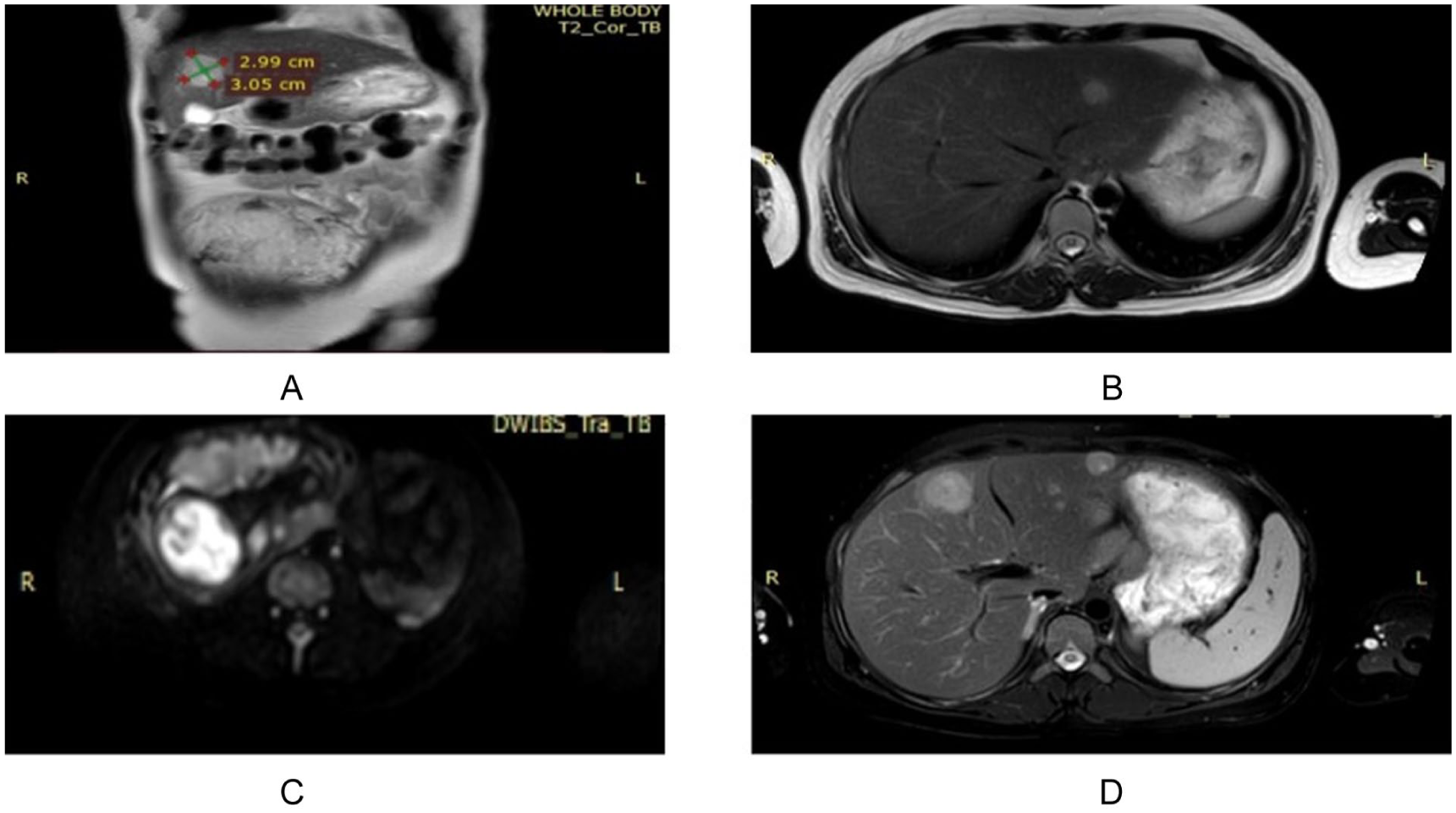
Transverse sections of total body MRI. (A) A measurement of a hepatic metastasis, (B) a left-sided hepatic metastasis, (C) the fetal brain, (D) two hepatic metastases in one section.

Bone material in both long bones and vertebrae. (A) A tiny bone metastasis in the upper third of the right femur, (B) a thoracic and upper lumbar normal myelogram, (C) the thoracic vertebral column, (D) lower thoracic and lumbar columns.
The patient was referred to an interventional radiologist for multiple core biopsies of both breasts. The pathological report confirmed invasive lobular carcinoma in both breasts, characterized by estrogen receptor positivity, progesterone receptor positivity, and HER2 negativity, with a Ki-67 index of 35%.
For comprehensive staging, whole-body MRI was performed without contrast, combined with simultaneous ¹⁸F-FDG PET acquisition (integrated PET/MRI). WB-MRI was combined with simultaneous 18F-FDG PET acquisition. No gadolinium was administered to ensure fetal safety. Imaging extended from head to mid-thigh, providing combined anatomical and functional information for comprehensive metastatic screening. Imaging revealed bilateral breast masses, extensive hepatic metastases, and multiple bone metastases (disseminated, with involvement of the pelvis and femur). The brain and lungs were normal. The 40-minute, contrast-free procedure was well tolerated and provided high-sensitivity anatomical/functional characterization of all imaged organs.
The patient declined to terminate the pregnancy and commenced chemotherapy during the fifth month of gestation and continues to receive treatment.
This report examines the efficacy and safety of total-body PET-MRI during pregnancy and review the literature on similar cases and techniques.
Discussion
PABC is the term to describe breast malignancy detected in women during pregnancy, within the first year of postpartum 7 or at any point of lactation period. 8 0.2% to 2.6% of breast malignancies occur in pregnant women, and for the ages below 45 years, 35% to 55% of breast cancer are diagnosed during 5 to 10 years after childbearing. 9 Our patient is 25 years old and pregnant at the fifth month. Despite the increased risk of occurrence with age, studies show that the aggressiveness and mortality of breast cancer are higher in younger women10,11
Imaging modalities in pregnancy
Determining an accurate imaging modality for both screening and staging is quite significant, in addition to addressing the need for limited ionizing X-ray exposure to the fetus 12 since such kind of radiation is linked to complications like abortion, stillbirth, malformations, growth retardation and carcinogenesis. 13 Abdominal plain films, radionuclide isotope scans, and computerized tomography (CT) scans 14 cannot be performed in pregnant women, however; ultrasound (US) mammography and MRI as relatively safe and reliable imaging techniques.12,15,16 Ultrasonography is the first-line image to pinpoint the tumor and any possible metastasis, with sensitivity reaching 99% and minimal fetal risk 8 ; it is particularly useful for abdominal, breast, and pelvic evaluation. 17 In our case, ultrasound was performed immediately as the patient presented with palpable breast masses, and in some rare cases, US results do not seem to be decisive; hence, mammography may be considered after risk-benefit assessment for the patient and fetus. 12 An ultrasound assessment is generally more precise than mammography regarding to physiological parenchymal changes in gravid and lactating breast. 15
Role of MRI and emerging technologies
The newly designed positioning device allowed for prone PET scans to be acquired and fused with breast MRI scans by combining 18F-FDG PET’s functional tumor information with MRI’s anatomical localization, a diagnostic mechanism for both primary and recurrent breast maternal malignancies can be optimized.
18
Staging and Whole-Body MRI (WB-MRI)
Breast MRI is a promising useful tool for cancer screening, with high sensitivity in detecting breast abnormalities not visible on other imaging methods. However, distinguishing between lactational changes and malignancy on MRI is challenging due to gadolinium uptake and increased breast density during lactation. 24 In breast cancer cases during pregnancy, where many women are diagnosed in advanced stages, comprehensive metastasis assessment is crucial. Common sites for breast cancer metastasis include the lungs, liver, and bones, as demonstrated in our case (imaging revealed bone and hepatic metastases). Safely assessing lung metastases during pregnancy can be achieved through chest radiographs with appropriate abdominal shielding. Liver metastases can be evaluated via ultrasound. Typically, bone metastasis assessment entails a bone scan, but due to potential harm to the developing fetal skeleton from radioactive technetium, non-contrast magnetic resonance imaging is preferred for bone metastasis evaluation during pregnancy.25,26 A comprehensive staging is essential for patients diagnosed with breast cancer during pregnancy, as the disease often presents at an advanced stage in 40% of cases, which is 2.5 times higher than that in non-pregnant patients. 27 Whole-body magnetic resonance imaging (WB-MRI) is a well-established imaging modality utilized in the management of various cancers, with notable applications in multiple myeloma, lymphomas, melanomas, prostate cancer, and breast cancer in particular.28,29 The use of whole-body MRI for cancer staging is justified during the second and third trimesters of pregnancy, as this period allows for the safe administration of anticancer chemotherapy. However, it would be futile to perform WB-MRI during the first 3 months, when the risks associated with chemotherapy are excessive, and a diagnosis would not lead to immediate treatment. 30 In this case, integrated WB-PET/MRI proved to be a safe and effective method for evaluating breast cancer during pregnancy. It facilitates the identification of lesions, localization, and staging with clarity and precision
Conclusions
Our findings suggest integrated PET/MRI is a valuable tool and a sensitive method for evaluating and staging breast cancer during pregnancy. It facilitates precise lesion identification, localization, and staging. By providing simultaneous metabolic (PET) and anatomical (MRI) data, this approach offers superior metastasis detection, complementing the anatomical/detailed structural information provided by the MRI sequences (T1w, STIR, DWI). This combined PET/MRI approach offers a more complete picture for detecting metastases than either modality alone, especially important for lobular carcinoma which can be harder to see on standard imaging.
Regarding safety, multicenter data collection in pregnant cancer patients and long-term newborn monitoring are recommended.
Footnotes
Ethical Considerations
No approval was required.
Consent to Participate
Informed consent was obtained for the use of the anonymized clinical information of this patient in the report.
Consent for Publication
Written informed consent was obtained from the patient for publication of this case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-chief of this journal.
Author Contributions
Maher Salamoon: Conceptualization, Supervision, Writing—review & editing.
Heya Ahmad: Conceptualization, Writing—original draft, Writing—review & editing.
Hanaa Ktyman: Conceptualization, Writing—original draft, Writing—review & editing.
Dana Chaker: Conceptualization, Writing—original draft, Writing—review & editing.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Not applicable.
Provenance and Peer Review
Not commissioned, externally peer-reviewed.
