Abstract
Background:
Though measures are being put in place for the management of Hepatitis B virus (HBV) infection in Nigeria, children remain the most vulnerable to develop chronic hepatitis. Routine screening in children is therefore necessary for effective control. However, the performance of the commonly used immunochromatographic test (ICT) strips has been challenging. Also, identifying the risk factors of transmission in this age group is of importance for the implementation of preventive measures. Hence, the goal of this study was to assess the test performance of the routinely used ICT strip and identify the associated clinical manifestations and risk factors of HBV.
Methods:
A cross sectional study involving 270 children below six years of age was conducted at ESUTH and Favor Child Pediatrics Hospital in Enugu, Nigeria. The subjects were screened for HBV by ICT and ELISA assays and a structured questionnaire was used to obtain participants data including demographic, socioeconomic, signs and symptoms, risk factors and vaccination.
Results:
BBased on ELISA, 31 out of 270 children were positive for HBV with an infection rate of 11.5%. ICT kit showed a low sensitivity of 51.6% in diagnosing HBV but was highly specific (100%) and accurate (94.4%). HBV infection was not associated with sex (χ2: 0.209; p = 0.401). The prevalence of HBV infection was similar in all the age group and HBV infection was not associated (χ2: 2.099; p = 0.914) with age group. All the clinical manifestations were not associated (p > 0.05) with HBV infection. Blood transfusion, shared items, tattoo marks and history of surgery associated significantly (p < 0.05) with HBV infections having odd ratios of 4.247, 4.224, 3.134 and 3.195 respectively. The vaccination rate was 55.2% (159/270) and only 3 (1.1%) out of 159 vaccinated subjected contracted the infection (OR: 0.068, p < 0.0001).
Conclusions:
HBV was prevalent (11.5%) in children below six years old in Enugu metropolis. Moreover, the routinely used ICT test was less reliable than ELISA in diagnosis HBV infection. More so, shared items, blood transfusion, tattooing and history of surgery were potential risk factors while vaccination served as a protective factor against the infection.
Introduction
Hepatitis B virus (HBV) infection constitutes a major public health problem in the world as it is one of the main causes of liver disease and responsible for more than 360 million cases of chronic hepatitis. 1 Annually, about 1 million of these infected people die due to the resultant consequences of the infection such as liver cirrhosis and hepatocellular carcinoma. 2 Hepatitis B virus is responsible for about 47% of hepatocellular carcinoma and 44% of cirrhotic liver disease cases. 3 The burden of this infection is greatest in the sub-Saharan region of Africa with a prevalence of over 8%.4,5 In Nigeria, the prevalence of HBV was estimated to be about 13.6% according to a meta-analysis study and ranged from 0.5% to 46.8% with more than 21 million seropositive individuals. 6
The increasing prevalence of HBV in Nigeria necessitates proper management and the implementation of effective preventive measures. One of the main measures to prevent this infection is through routine vaccination of newborns because children are born without a fully developed natural immune system, but this is not usually the case in certain rural or low-resource health settings. 7 Although the immunization campaign of hepatitis B vaccine by the National Program of Immunization (NPI) is ongoing, the rate of vaccination is still low below expectation. This was confirmed by a study which showed the coverage rate of hepatitis B vaccine in low-resource health settings at about 41%. 8 As such, children are more prone and exposed to the infection and the rate of transmission of the infection is likely to increase. One of the main routes of transmission of HBV to children is by vertical transmission from mothers, whereas sexual intercourse is a principal means of transmission for sexually active partners. More so, other primary sources of infection according to a World Health Organization (WHO) report in 2009 include transfusion of blood from unscreened donors, sharing of household items such as toothbrush, exposure to contaminated or unsterilized surgical equipment for medical and dental procedures, body and ear piercing, tattooing of the body, and the use of unsterilized objects for traditional rituals, circumcision, face marking, etc.9,10 With these multiple routes of transmission, routine screening of blood donors for the presence of hepatitis B surface antigen (HBsAg) is necessary to identify infected individuals and promptly treat them to prevent the development of chronic liver disease and carcinoma which can eventually lead to death.
Routine screening of HBV infection in Nigeria today is commonly done using immunochromatographic test (ICT) strips. This screening technique is very rapid as the results can be obtained in less than 10 minutes and are relatively cheap and affordable. Although the manufacturers claim that these test strips have relatively high sensitivity, specificity, and accuracy, querying performances have been reported as very low level of the anti-HBsAg antibodies may not be detected by the strips. 11 More so, in case of poor diagnosis, presumptive diagnosis can aid clinicians to screen individuals for vital signs of clinical manifestations. Hence, this study was aimed to determine the prevalence of HBV in children by assessing the test performance of the routinely used ICT strips and identify the associated clinical manifestations and risk factors of the infection.
Materials and Methods
Study population and design
This study was a hospital-based cross-sectional study conducted at Enugu State University Teaching Hospital (ESUTH) and Favor Child Pediatrics Hospital in Enugu. Enugu is the capital of Enugu State located in South Eastern Nigeria with latitude and longitude coordinates of 6.459964 and 7.548949. The study design was reviewed and approved by the ethical committee of ESUTH, Enugu, Nigeria, with approval no. ESUTHP/C-MAC/RA/034/165. Written informed consent was obtained from all parents or guardians willing to include their children into the study. The study population consisted of children with minor illnesses and fever who attended the hospitals. Subjects who met the criteria for inclusion which include children less than 71 months old (less than 6 years) and whose parents and guardians provided a written informed consent were recruited into the study. Within the period of February to August 2017, a total of 270 children aged between 0 and 71 months were recruited based on the calculated sample size using the formula: N = Z2pq/d2, where z = normal standard deviation at 1.96 which corresponds to 95% confidence interval (CI); p = prevalence of HBV infection; q = 1 − p; and d = degree of accuracy/precision expected = 0.05. The average prevalence of 23% was obtained from a meta-analysis study in Nigeria by Musa et al. 6 With this prevalence, the calculated sample size was 256 children.
Data collection and serologic screening for HBsAg
After the recruitment, a structured interviewer administered questionnaire on the predisposing factors of HBV infection following a literature review was used to obtain participants data. The data collected included demographic, socioeconomic, background knowledge about HBV, its screening, associated signs and symptoms, risk factors relating to the parent/guardian, as well as vaccination status of the child and preventive measures. After the participants were interviewed, 3 mL of blood was collected through venous puncture, transferred into sterile plain bottles, and allowed to clot. The blood was then centrifuged at 5000 rpm for 5 minutes to obtain the serum. The serum was transported to the National Arbovirus and Vectors Research Centre (NAVRC), Enugu, for enzyme-linked immunosorbent assay (ELISA) analysis using the AntiHBsAg ELISA kit by Dialab Laborinstrumenten Gesellschaft, Austria, and later to the Microbiology laboratory of Godfrey Okoye University, Enugu, for ICT assay using the HBsAg test strip by Heliocare Nantong Diagnos Biotechnology, China, according to manufacturer’s protocol. The mode of action of this ICT strip is based on the principle of antibody-antigen reaction in which antibody present in plasma or serum migrates upward by capillary action and reacts with recombinant antigen present on the chromatographic membrane of the strip thereby generating a color line in the test region.
Data and statistical analysis
The prevalence (%) of HBV infection was calculated as (presence of HBsAg/total population) × 100. The specificity, sensitivity, positive predictive value (PPV), negative predictive value (NPV), and accuracy of ICT test for HBV infection were calculated from true-positive (TP), true-negative (TN), false-negative (FN), and false-positive (FP) results. Sensitivity was calculated as TP/(TP + FN) × 100, specificity as TN/(TN + FP) × 100, NPV as TN/(TN + FN) × 100, PPV as TP/(TP + FP) × 100, and accuracy as ((TP + TN)/sample size) × 100.
Data were analyzed using Statistical Package for Social Science (SPSS) version 16. Results were expressed in frequencies and proportions and presented in tables. Pearson χ2 test was used to determine the association between ICT and ELISA tests in diagnosis of HBV infection. Also, χ2 was used to determine the association of various parameters including sociodemographic characteristics as well as signs and symptoms with HBV infection. Fisher exact test was used to determine the association between 2 categorical variables when the sample size of a group was small (<20). The odds ratio (OR) was generated using binomial logistic regression model to determine the independent contribution of risk factors to HBV infection. All statistical analysis employed a 2-sided test and 95% CI for P value determination. A P value of ⩽.05 was considered statistically significant.
Results
Among the 270 subjects, 31 were tested positive for HBsAg by ELISA giving a prevalence of 11.5%. The ELISA assay was more effective and reliable than the ICT strips in diagnosing HBsAg as it detected 31 HBV-positive subjects as against 16 for ICT strips. As such, ICT test had a low potential in detecting HBV-positive subjects with a sensitivity of 51.6% (16/31). The performances of the 2 tests are summarized in Table 1. As shown in Table 2, the seroprevalence of HBV infection was insignificantly greater (χ2: 0.209; P = .401) in women (7.4%) than in men (4.1%), and thus, the infection was not associated with sex. Also, the prevalence of HBV infection for all the various age groups, 24 to 35 months, 36 to 47 months, 48 to 59 months, and 60 to 71 months, were 7/62 (11.3%), 6/47 (12.7%), 10/80 (12.5%), and 7/54 (13.0%), respectively. As such, HBV infection was not associated (χ2: 2.099; P = .914) with age group of patients. The presence of HBV infection in children was not associated with the parent/guardian level of education (χ2: 3.124; P = .210) or their marital status (χ2: 3. 421; P = .331). Evaluating clinical signs and symptoms of subjects showed all the clinical manifestations: jaundice, dark urine, fever, joint pain, itchy skin, loss of appetite, fatigue, and abdominal pains not to be associated (P > .05) with HBV infection (Table 3). Blood transfusion, sharing of items, tattoo marks, and history of surgery were found to be associated (P < .05) with HBV infections having OR of 4.247, 4.224, 3.134, and 3.195, respectively. Out of the 270 subjects, 159 were vaccinated giving a vaccination rate of 55.2%. Among these 159 vaccinated subjects, only 3 (1.1%) contracted the infection. Thus, vaccination showed a very low OR of 0.068 and was associated (P < .05) with HBV infection as a protective factor (Table 4).
Test performance of ICT and ELISA tests in diagnosing HBV.

Abbreviations: HBV, hepatitis B virus; HBV-ICT, immunochromatographic test for HBV; HBV-ELISA: enzyme-linked immunosorbent assay for HBV.
Association of HBV seroprevalence with demographic characteristic of participants.
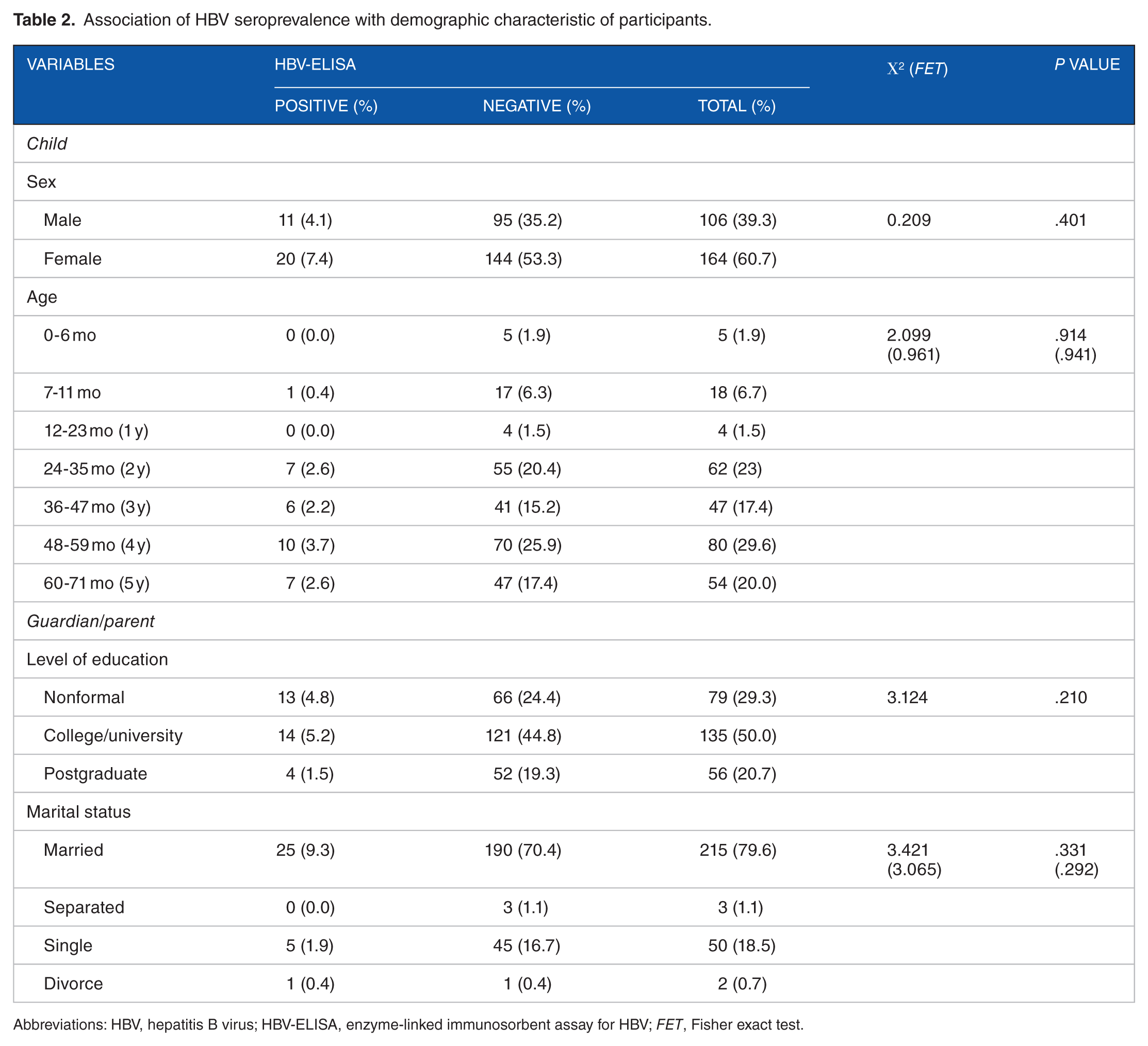
Abbreviations: HBV, hepatitis B virus; HBV-ELISA, enzyme-linked immunosorbent assay for HBV; FET, Fisher exact test.
Association of HBV seroprevalence with signs and symptoms of participants.
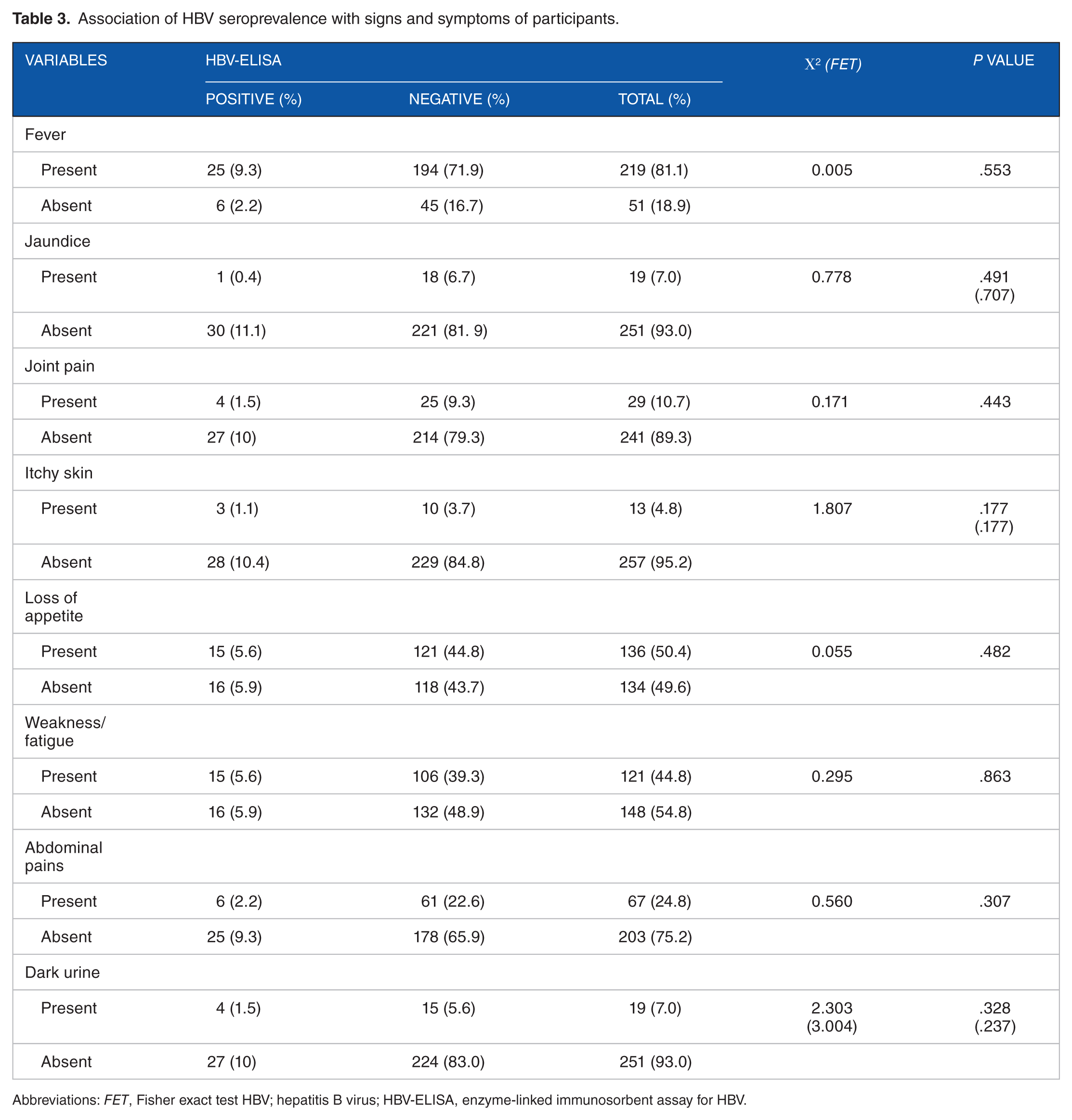
Abbreviations: FET, Fisher exact test HBV; hepatitis B virus; HBV-ELISA, enzyme-linked immunosorbent assay for HBV.
Binomial logistic regression analyses for potential risk factors of HBV infection based on HBV-ELISA diagnosis.
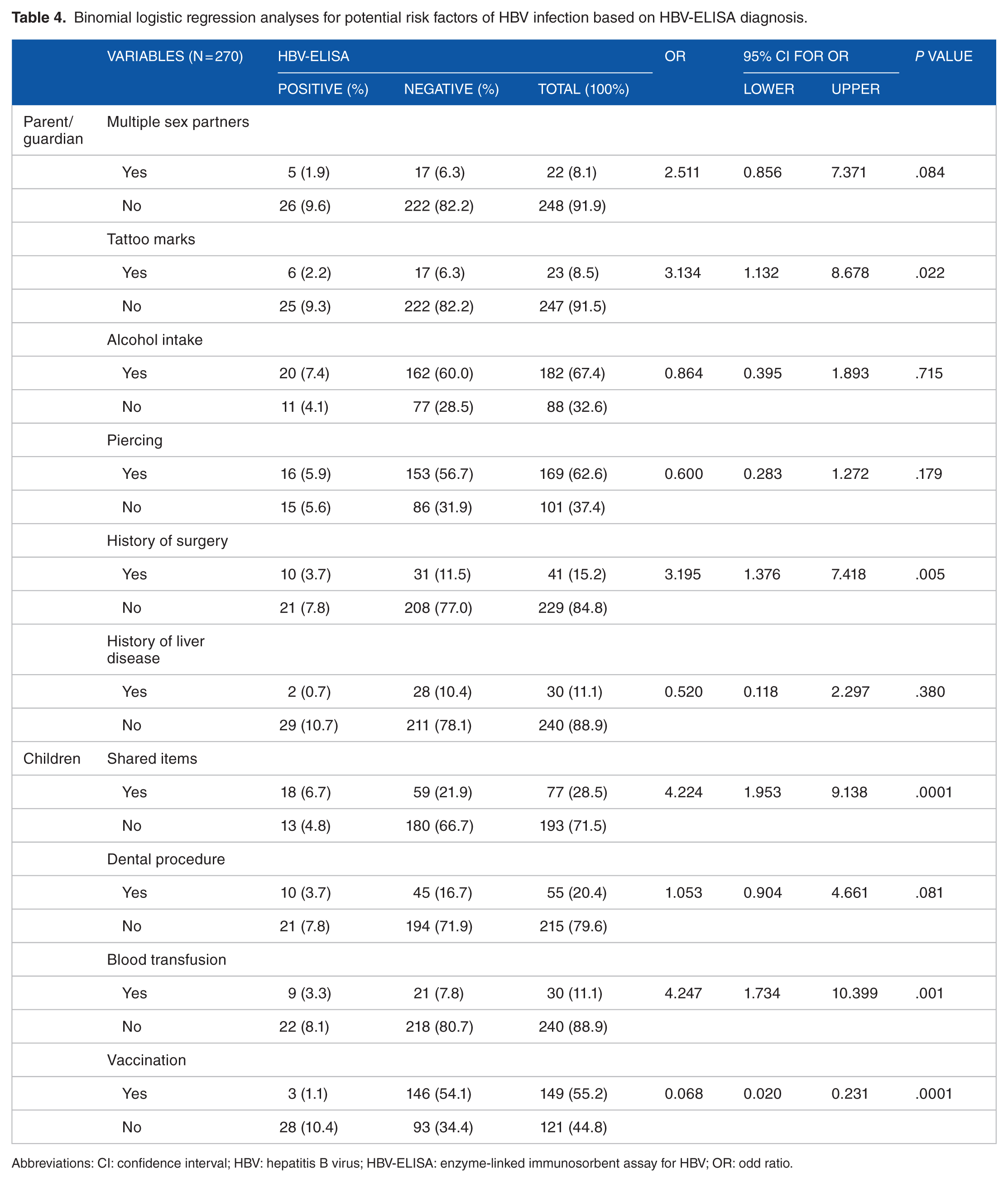
Abbreviations: CI: confidence interval; HBV: hepatitis B virus; HBV-ELISA: enzyme-linked immunosorbent assay for HBV; OR: odd ratio.
Discussion
Although HBV infection remains a serious public health problem in Nigeria, limited data are available on the prevalence among children. Findings from this study showed HBV to have an infection rate of 11.5%. This is in line with a recent meta-analysis study in Nigeria 6 which showed an overall prevalence of 11.5% (CI: 6.0-17.0) in children. This prevalence is lower compared with that of other age groups or populations across Nigeria such as that by Balogun et al 12 who showed HBV to have a prevalence of 28.4% among human immunodeficiency virus (HIV)-positive subjects in LASUTH, Ikeja, Lagos, Nigeria; 13.2% in Ibadan, south-western Nigeria, by Fasola et al 13 ; 20.0% reported by Alao et al 14 among prospective blood donors in Otukpo, Benue State; 14.5% reported by Lawal et al 15 among blood donors in Ibadan; 18.6% by Buseri et al 16 among blood donors in Osogbo, Nigeria; and 17.5% by Okolie et al 17 among patients with HIV in south-eastern Nigeria. The lower prevalence of HBV in children is good news as they are easily exposed to the disease particularly through vertical transmission by their mothers before birth.
Although with low prevalence, effective diagnosis is necessary to accurately screen infected subjects. The ICT strips showed a low sensitivity (51.6%) in detecting HBsAg in this study population when ELISA assay was used as a gold standard. The fact that ICT strips are routinely used for screening HBV infection poses a major challenge as false-negative subjects may harbor the infection for a long time without being detected and may develop to chronic liver disease or hepatocellular carcinoma and possible death.18,19 As such, there is need for constant evaluation of the test performance of the various routinely used ICT strips in Nigeria for screening to eliminate those with low sensitivity and specificity. Although ELISA was reliable in diagnosis of HBV infection, its routine use may not be feasible due to its high cost and longer time of analysis compared with ICT strips. However, in cases of inconclusive results by ICT strips, ELISA should be used as a confirmatory test.
The age of acquiring HBV infection is one of the major determinants of the incidence and prevalence rates, as viral clearance depends on the age of exposure. Reports have shown that more than 90% of exposed neonates and about 30% of children below 5 years of age fail to clear away HBV from the body which later develops to chronic infection, whereas 95% of adult-acquired infections lead to spontaneous clearance.20-22 In this study, the lowest prevalence of HBV was observed in children below 11 months old and highest prevalence was observed in children between 60 and 71 months followed by those between 48 and 59 years of age. However, there was no statistically significant relationship between age and HBV infection (χ2 = 2.185, P = .902).
Although more than half of the individuals with early HBV infection are usually asymptomatic, chronic infection for more than 30 days may tend to manifest symptoms. 23 Our finding showed all the clinical manifestations: jaundice, dark urine, fever, joint pain, itchy skin, depression or weight loss, loss of appetite, fatigue, and abdominal pain not to be associated with HBV infection. This finding is in contrast to that of a previous study which showed dark urine and jaundice to be associated with HBV infection. 24 These clinical manifestations are commonly observed in individuals with chronic liver disease caused by HBV. 24
Several risk factors such as multiple sex partners, practice of homosexuality, presence of tattoo or tribal marks, body piercing, sharing of personal items such as toothbrush, too much alcohol intake, history of any liver disease, blood transfusion, intravenous drug use, dental procedure, and history of surgery have been documented from previous studies to be associated with HBV infection.25,26 Our finding showed history of surgery and tattooing as potential risk factors of HBV infection from parents/guardians to children, whereas shared items and blood transfusion were potential risk factors in children. Among these risk factors, blood transfusion presented the greatest risk. This was supported by a study in Enugu which reported history of blood transfusion as a potent risk factor for both HBV and HCV (hepatitis C virus) infections. 27 This calls for intensive screening of blood using more sensitive immunoassay particularly ELISA to confirm the hepatitis status of blood donors to curb this disease. Other known potential risk factors such as dental procedure, intravenous drug use, and body piercings were found not to be associated with HBV infection in this study population. The reason for this is unknown but may be suggested that some of this practices are uncommon in this region of the country. Furthermore, the possible reason why dental procedure was not associated with HBV infection in children may be due to the fact that such procedures are not commonly done in young children or that these health facilities properly sterilize and disinfect their dental equipment.
Hepatitis B virus is an infection which does not have a treatment and so vaccination is the most effective means of prevention.28,29 Although the National Immunisation Programme (NIP) campaign stipulates the vaccination of all children, the rate is still low especially in low-resource settings. A previous study in Nigeria showed hepatitis B vaccine coverage rate of 41% in low-resource settings. 8 In this study, the vaccination rate was 55.5% suggesting that more children are been vaccinated. More so, very few (<1%) of the vaccinated children contracted HBV infection. Thus, vaccination was found to be a protective factor in preventing HBV infection. This may suggest that early HB vaccine in children less than 1 year of age is effective in protecting them against the infection.
Conclusions
Hepatitis B virus infection had a prevalence of 11.5% in children below 6 years of age. Tattooing and history of surgery of parents/guardians were the most likely risk factors of HBV transmission to children, whereas blood transfusion and sharing of items were the likely risk factors in children. Moreover, vaccination was a protective factor against the infection. The poor performance of ICT strip suggests that a more effective confirmatory test such as ELISA assays be used to diagnose individuals manifesting clinical signs and symptoms with inconclusive ICT diagnosis. Also, early vaccination of children is encouraged to better manage and prevent this infection.
Footnotes
Acknowledgements
The authors are thankful to the medical students of ESUTH, Enugu, for their assistance in data and blood collection. Also, the authors are equally grateful to Mr Emmanuel Ogudu of the National Arbovirus and Vectors Research Center (NARVC), Enugu, for his assistance in ELISA analysis.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author Contributions
MCE, RII, and DCO conceived and designed the study. MCE and GAE conducted the fieldwork, laboratory work, analyzed, and together with RII and DCO interpreted the data. MCE and GAE drafted the manuscript, whereas RII and DNO thoroughly scrutinized the manuscript for quality. All authors read and approved the final manuscript.
