Abstract
The Cytochrome P-4501B1 (CYP1B1) Leu432Val polymorphism has been previously shown to be associated with some types of cancer and affects CYP1B1-mediated metabolism of various infertility drugs. To establish the frequency of CYP1B1 Leu432Val polymorphism among women with a history of infertility drug use, we studied the genotypes of 147 patients with breast cancer with a history of infertility and 150 cancer-free, infertile women (control group) in Northern Iran. A polymerase chain reaction–based restriction fragment length polymorphism assay was used to detect GG (Val/Val), CG (Leu/Val), and CC (Leu/Leu) genotype frequencies, which did not vary significantly between the 2 patient groups (P = .847). We established for the first time that the incidence of CYP1B1 Leu432Val polymorphism is 46.6% among women with infertility history and breast cancer in Northern Iran. Finally, our results do not show any significant association between CYP1B1 Leu432Val polymorphism and breast cancer in infertile women in this region, who have also received infertility treatment.
Introduction
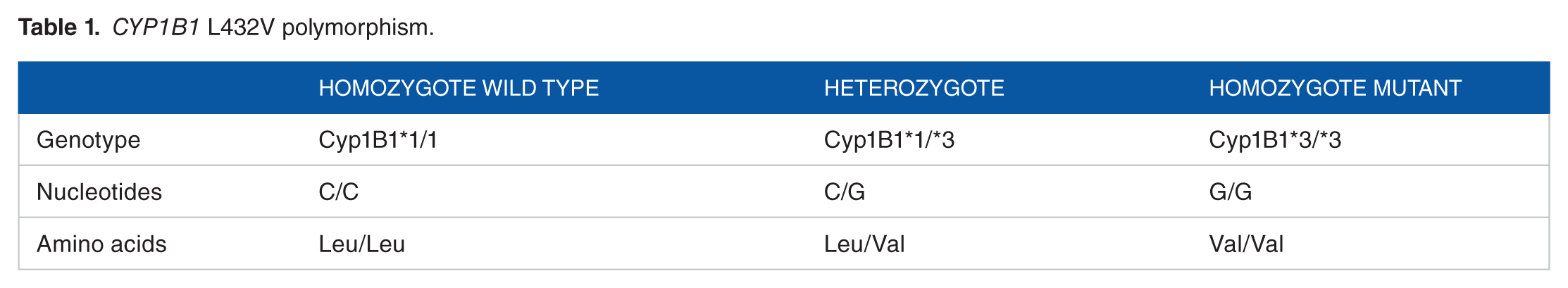
Cytochrome P-4501B1 (CYP1B1) bioactivates environmental procarcinogens and heterocyclic aromatic amines and accelerates the formation of genotoxic 4-hydroxy estradiol (4-OH E2). In many tissues, formation of the 4-OH E2 catechol metabolite, followed by high expression of CYP1B1, has been associated with estrogen-related tumors, such as breast cancer.1,2 The CYP1B1 locus is polymorphic (Table 1), and genetic variations at this locus correlate with increased breast cancer risk in some human populations.3–5 Located at 2p21-22, CYP1B1 contains 3 exons, the third of which encodes a crucial heme-binding domain. One common polymorphism occurring at codon 432 in this third exon causes a Leu → Val conversion (HGVS name: NC_000002.11:g.38298203C > G), predicted to both alter protein bioactivity and contribute to the observed variability in the effects of environmental carcinogenic chemicals between individuals.2,6 Previous studies have shown that the 432Leu allelic variant exhibits a higher level of activity in estrogen hydroxylation than the 432Val variant, resulting in a greater rate of 4-OH E2 production and accumulation, and thus a greater risk of potential carcinogenic (including breast cancer) and estrogenic effects. 7
CYP1B1 L432V polymorphism.
Breast cancer with unclear cause is a major cause of mortality internationally, with an incidence rate of 98/100 000 within white countries. 2 Previous studies indicate that infertile women (ie, those unable to conceive within a 12-month period) have an increased risk of developing breast cancer compared with fertile women, with infertility shown to be both directly and indirectly associated with the disease. 8 This observed higher incidence correlates with increased maternal age at the first birth and to expected nulliparity. Notably, Jensen et al 9 recently reported increased standardized incidence ratio (SIR) for breast cancer after adjustment for parity status.9,10
The association between breast cancer and the use of exogenous reproductive hormones (eg, estrogen treatment) for infertility treatment has been widely studied and is implicated as a likely cause of the increased cancer risk within this group.11–13 Other factors, such as clomiphene use (also for infertility treatment), have been investigated with more controversial results.8,14–20 The CYP1B1 polymorphisms have been shown to affect the metabolism of infertility medications in vitro.21–23 Furthermore, several studies have investigated the association between breast cancer and various CYP1B1 polymorphisms; however, these produced inconsistent and/or contradictory findings.3–5,24–27 Here, we conducted a study on women with infertility history in Northern Iran, with and without breast cancer, to establish and compare the overall frequency of the C → G CYP1B1 polymorphism occurring at codon 432 in exon 3. We found no significant correlation between the CYP1B1 Leu432Val polymorphism and breast cancer among infertile North Iranian women.
Materials and Methods
Study participants
From January 2012 to December 2015, a total of 147 patients with breast cancer and a history of infertility (as verified by a pathologist) and 150 control patients with a history of infertility (matched with the case group according to their age/residence and confirmed to be free of any cancer) were recruited at Babolsar Shahid-Rajaee Oncology hospital or Fatemezahra Infertility and Reproductive Health Research Center. The baseline information, medical history, and usage of infertility drugs (clomiphene or letrozole) and/or the oral contraceptive pills (OCP) of each patient were recorded.
Prior to participation in the study, written informed consent was obtained from all participants, who were also verified as having been residents of Mazandaran Province (in Northern Iran) for a minimum of 10 years. The study was approved by the ethics committee at the Babol University of Medical Sciences.
Sample preparation
Peripheral blood samples (5 mL) were collected from patients and controls in Vacutainer tubes containing ethylenediaminetetraacetic acid (EDTA), and genomic DNA was extracted using a Blood/Cultured Cells Mini kit (Yekta-Tajhiz-Azma Co., Tehran, Iran). All the samples were stored at −20°C until polymerase chain reaction-restriction fragment length polymorphism (PCR-RFLP) analysis.
PCR and RFLP Analysis
A polymerase chain reaction (PCR)–based restriction fragment length polymorphism (RFLP) assay was used to analyze the presence of a C to G transversion mutation at codon 432 of the CYP1B1 gene. Polymerase chain reaction amplification of a 271-bp fragment of the gene, including the region of exon 3 containing the target polymorphism, was achieved using the listed primer sequences (Table 2). Polymerase chain reaction was conducted using a 25-µL PCR mixture containing genomic DNA (3 µL) and YTA Taq DNA polymerase, according to the PCR MasterMix 2× kit (Yekta-Tajhiz-Azma Co.).
The primer sequences for PCR of CYP1B1 gene.

Abbreviation: PCR, polymerase chain reaction.
Polymerase chain reaction cycles performed were as follows: 3 minutes of denaturing at 94°C, followed by 35 cycles of DNA amplification (94°C for 30 seconds, 58°C for 30 seconds, and 72°C for 1 minute) and 10 minutes of DNA extension at 72°C. Following PCR, 5 µL of each PCR product was run on a 3% agarose gel to confirm generation of the expected 271-bp product. Restriction digest was performed with 10 µL of PCR product using 1 unit of Eco57I restriction enzyme (Fermentas, Cheshire, UK) for 4 hours at 37°C. The identity of the resultant digested product was verified on a 3% agarose gel via electrophoresis (with ethidium bromide) at 100 V for 30 minutes. The presence of a G at position 1294 (in CYP1B1 codon 432) generated a unique 271-bp band. Conversely, the presence of a C at position 1294 instead produced both a 166- and 105-bp fragment. Gels were visualized under ultraviolet (UV) light, and the RFLP gel electrophoresis products were read by 2 independent persons unaware of the identities of samples as either cases or controls.
Statistical analysis
We defined whether the frequencies of CYP1B1 genotypes were in Hardy-Weinberg equilibrium using a standard χ2 test. Odds ratios (ORs) and 95% confidence intervals (CIs) were calculated using SPSS Version 16. Odds ratios were applied to measure the strength of the association between breast cancer risk and the occurrence of CYP1B1 genotypes. The χ2 test was applied to compare case and control distributions of CYP1B1 alleles and genotypes. Data are shown as mean ± SD, and differences are considered significant at P ⩽ .05.
Results
The mean age of patients with breast cancer versus that of the control group was not significantly different (P = .071), being 45.4 ± 8.9 years (ranging between 25 and 65 years) and 43.7 ± 7.5 years (ranging between 33 and 63 years), respectively. Furthermore, the residence distribution (urban and rural) between the 2 groups did not show any significant difference (P > .05). Comparison of baseline patient details between the breast cancer and control groups revealed significant differences in menarche age, OCP usage, and duration of oral infertility drug usage between groups (Table 3).
Baseline variables of patients, comparing infertile women with (case) and without (control) breast cancer.

Abbreviations: BMI, body mass index; OCP, oral contraceptive pills.
Only for women with history of pregnancy.
Referring to clomiphene citrate or letrozole.
The PCR-RFLP genotyping results are depicted for representative samples (Figure 1). Based on predicted DNA fragment size following restriction digest, the appearance of only 1 band (271 bp) corresponds to a GG (Figure 1, lane 1), the appearance of 3 separate bands (271, 166, and 105 bp) to a GC (Figure 1, lanes 3 and 4), and the appearance of 2 separate bands (166 and 105 bp) to a CC polymorphic allele at codon 432 of CYP1B1 (Figure 1, lane 5).
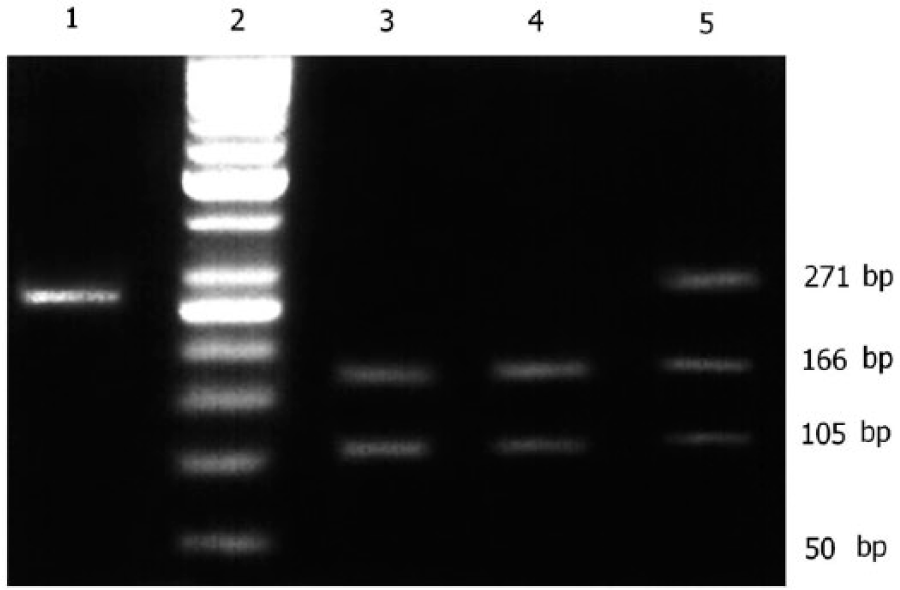
Polymerase chain reaction-restriction fragment length polymorphism to identity CYP1B1 polymorphic genotypes via restriction digest with EcoR57I. Lane 1: mutant homozygous genotype Val/Val (271 bp), lane 2: 50-bp reference ladder, lanes 3 and 4: wild-type homozygous Leu/Leu genotype (166 and 105 bp), and lane 5: heterozygous genotype Leu/Val (271, 166, and 105 bp).
We compared the distribution frequencies of CYP1B1 polymorphisms in breast cancer versus control patients (Table 4 and Figure 2). The frequencies of G and C alleles at codon 432 of CYP1B1 showed no significant differences between the 2 groups (P = .948), with an OR of 0.989 (95% CI: 0.72-1.37). Polymorphism distributions were not in accordance with Hardy-Weinberg equilibrium (P < .05). There was no significant difference in the incidence of GG, GC, and CC genotypes between the 2 patient groups (P = .847) (Table 4).
Association of CYP1B1 Leu432Val genotypes and alleles with breast cancer risk in patients with (case) and without (control) breast cancer.

Abbreviations: CI, confidence interval; OR, odds ratio.

CYP1B1 Lue432Val genotype frequencies in infertile women with (case) and without (control) breast cancer.
Discussion
Polymorphisms within genes that encode enzymes mediating the detoxification or bioactivation of carcinogens can influence the susceptibility of an individual to develop cancer. The CYP1B1 polymorphic alleles investigated in this study affect a crucial enzyme involved in the metabolism of estrogens and xenobiotics and are therefore strong candidates to promote an increased risk of breast cancer.3–5,24–26 For example, women with a Val/Val polymorphic genotype at CYP1B1 codon 432 have a higher percentage of estrogen receptor–positive tumors (P = .03), whereas those with a CYP1B1 Leu432Val polymorphism have modestly higher estradiol levels but similar estrone and estrone sulfate levels. 28
In this preliminary study, we evaluated the incidence of CYP1B1 polymorphisms in women with a history of infertility, who had been settled in the Mazandaran Province of Iran for at least a decade. To the best of our knowledge, this is the first study reporting the frequency of the CYP1B1 Leu432Val polymorphism, with relation to the occurrence of breast cancer, in this group. We estimated the incidence of CYP1B1 Leu432Val polymorphism in the target group to be 0.47 (46.6%), consistent with previous studies on other population samples around the world that report frequency of this allele to range between 0.41 and 0.75.29,30 We did not find any association between the distribution of CYP1B1 polymorphisms at codon 432 and breast cancer (P = .847). The usage of infertility medications (including estrogens), and environmental exposure to other xenobiotics among infertile women, may be a risk factor for breast cancer via the effects of carcinogenic metabolites produced by different CYP1B1 variants.31–36 Supporting this hypothesis, the results of our study indicate that the use of OCP (containing both estrogen and progestin) is associated with an increased risk of developing breast cancer. Furthermore, the duration of infertility drug use, as well as a low menarche age (<12 years), is also significantly correlated with breast cancer (P < .05), consistent with previously published literature.37–39
Previous studies investigating the association between the C → G polymorphism at codon 432 of CYP1B1 and breast cancer in various populations have reported contradictory findings. Although studies of white and Asian populations have demonstrated no significant association between the Leu432Val genotype and breast cancer risk,27,28,40–42 other studies do in fact report a significant correlation.4,27 Incidence of the Leu432Val polymorphism has been reported previously to occur at a frequency of 0.23 in Asian, 0.43 in white, and 0.75 in African American populations.3,43 In our study, the frequency of the polymorphism was estimated to be 0.47, most closely aligning with previously published incidence estimates for white sample populations.
Previously published studies report that notable common polymorphic alleles of CYP1B1 include Arg (80.0%) at codon 48, Ala (80.5%) at codon 119, and Leu (86.6%) at codon 432, with none of these demonstrated to be associated with increased breast cancer risk.28,41,42 Furthermore, the association of increased breast cancer risk with factors related to endogenous estrogen exposure, such as body mass index (BMI) and menstruation years, was not significantly modified by polymorphism of CYP1B1. Notably, it was observed that women with 1 copy of the codon 48 polymorphic variant of CYP1B1 were less likely to have estrogen receptor–positive breast cancer than those who had 2 copies of the corresponding wild-type allele.28,41,42
In contrast to these and to the results of this study, some previous research does report an association between the CYP1B1 Leu432Val polymorphism and breast cancer in whites.44,45 A homozygous Leu/Leu polymorphic genotype was shown to confer a 3.30-fold higher risk of breast cancer (95% CI: 1.76-6.19) and a heterozygous Val/Leu polymorphic genotype was shown to confer a 2.15-fold higher risk (95% CI: 1.31-3.52). 44 Similarly, a study of Asian women reported that a homozygous Leu/Leu or a Val/Leu polymorphic genotype conferred the greatest increased risk of breast cancer.2,26
A history of infertility may be a risk factor for breast cancer, partly through exposure to medications containing estrogen metabolites; however, the results presented here are in accordance with those previous studies that report a lack of correlation between the CYP1B1 Leu432Val polymorphism and breast cancer. Notably, these previous studies consist of higher sample sizes and less confounding variables than others that report a significant association between the Leu432Val polymorphism and breast cancer incidence.
Conclusions
In this preliminary study, we report for the first time that the overall frequency of Leu432Val polymorphism in exon 3 of CYP1B1 is 0.47 in a population of women with infertility history and breast cancer in Northern Iran. The results of our case/control-designed study did not show any significant association between CYP1B1 Leu432Val polymorphism and breast cancer. Further cohort studies, involving larger sample sizes and other ethnic groups, could more robustly rule out association between CYP1B1 polymorphism and breast cancer risk in infertile women.
Footnotes
Acknowledgements
This study was conducted as part of a PhD thesis.
Peer review:
Seven peer reviewers contributed to the peer review report. Reviewers’ reports totaled 970 words, excluding any confidential comments to the academic editor.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project has been funded by the Babol University of Medical Sciences.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
Concepted and designed by MGA, SE, MAD, EZ, DM. Development of methodology was done by MGA, SE, EZ, MAD, MHA. Acquisition of data (provided animals, acquired and managed patients, provided facilities, etc.) was done by MGA, SE, DM, ASM, MG. Analysis and interpretation of data (e.g., statistical analysis, biostatistics, computational analysis) was done by MGA, SE, MAD, MHA, EZ. Writing, review, and/or revision of the manuscript was done by MGA, SE, EZ. Administrative, technical, or material support (i.e., reporting or organizing data, constructing databases) was done by MGA, SE, EZ. Study supervision by MGA, SE, EZ.
