Abstract
Aboriginal and Torres Strait Islander health courses develop the cultural capacity and capability of undergraduate health professionals; however, the expectations of a tertiary education institutions that all First Nations academics can successfully deliver this specialised area of knowledge and develop these capabilities in undergraduates may be ill-conceived. Aboriginal and Torres Strait Islander health courses study the truths of colonisation: the oppression, the massacres and the governmental policies which resulted in The Stolen Generations as well as the ongoing trauma and health concerns resulting from colonisation practices. The very areas being discussed in these health courses are also the history and reality for the First Nations academics tasked with teaching this content. Recognising and understanding some of the issues of having First Nations academics teaching Aboriginal and Torres Strait Islander health courses is an important first step to ensuring no further trauma is inflicted upon these academics.
Introduction
Improving the health outcomes for Aboriginal and Torres Strait Islander peoples requires health professionals to have the cultural capability to provide care which is deemed to be culturally safe. In 2014, the Aboriginal and Torres Strait Islander Health Curriculum Framework (Department of Health, 2014) was introduced to Australian tertiary education institutions to provide guidance on what should be incorporated into their curriculum relating to Aboriginal and Torres Strait Islander peoples. Over time, it became an accreditation requirement for many undergraduate health care programmes to have a standalone course on Aboriginal and Torres Strait Islander health based upon this framework, or in the case of nursing and midwifery, based upon the Nursing and Midwifery Aboriginal and Torres Strait Islander Health Curriculum Framework (Congress of Aboriginal and Torres Strait Islander Nurses and Midwives [CATSINaM], 2017), an adaptation of the original 2014 framework. The inclusion of Aboriginal and Torres Strait Islander health courses in undergraduate health care programmes aims to improve the health outcomes for Aboriginal and Torres Strait Islander peoples through developing five capabilities in future graduates which would support them to provide care that is regarded as culturally safe (Department of Health, 2014). These interconnected cultural capabilities include respect, communication, safety and quality, reflection and advocacy. It is important to have individuals delivering the content who are knowledgeable on Aboriginal and Torres Strait Islander health, history, culture and colonisation, who understand the roles of First Nations health care workers and practitioners and who possess a good understanding on how to provide care that is considered culturally safe. A teaching qualification or extensive teaching experience would also seem to be advantageous.
A search of literature found that there were no research studies specifically investigating the pre-requisites or attributes which tertiary education institutions regarded as important for individuals who are teaching Aboriginal and Torres Strait Islander health courses. It was, however, found that there is some guidance for primary and secondary school education professionals on how to teach Aboriginal and Torres Strait Islander students as well as guidance on how to incorporate Aboriginal and Torres Strait Islander history and culture into primary and secondary school curriculum (Australian Institute for Teaching and School Leadership, 2011; Lloyd et al., 2015).
To provide some insight into the assumptions versus the reality surrounding the teaching of Aboriginal and Torres Strait Islander health courses in tertiary education settings, the authors have evaluated their own experiences as academics and health care professionals in relation to this. The first author, a Murri woman, whose family has been separated from their clan group due to governmental policies, was thrust into coordinating and teaching the Aboriginal and Torres Strait Islander health course at a regional university after the three Aboriginal academics, who had been teaching the course, left in rapid succession. Prior to this, the first author had not taught this course but instead worked for many years in clinical skills and clinical practice courses due to their extensive experience in acute care; however, due to their Indigeneity, the first author was considered the most appropriate person to teach the Aboriginal and Torres Strait Islander health course. The second author, a Gubbi Gubbi and Mandandanji woman, had previously taught an Aboriginal and Torres Strait Islander course through the Indigenous unit at an Australian university. The third author, who is not a First Nations academic, has undertaken Indigenous research and has previously taught First Nations health. The third author, upon commencing at a regional university, was immediately required to coordinate and teach an Aboriginal and Torres Strait Islander health course. Each of the authors has found the assumptions of the tertiary education sector do not always align with the expertise of the academic. To highlight this, the second author has provided insight into their experiences:
As an Aboriginal lecturer I found it easier to teach social work modules than to teach Aboriginal studies modules. I found with the social work modules there was an agreed upon way of teaching social work students and the type of content we were teaching. However, with Indigenous studies, I realised I was ill equipped to teach this, due to the fact I believe I am colonised and only had a Western education in the formative years of my life. I went to university in 1995, and this is where I first started to learn the truth about colonisation, government policies and much of the history from the past 200 years. It was an eye opener for me as I could not believe other human beings could treat a people in the way that they did -and mostly still do. I think I became traumatised in learning all this new information at the Institute of Koori Education (IKE) at Deakin University. In the many years since attending IKE, I have learned so much more about the terrible history of Captain Cook and other settlers who invaded Australia and almost wiped out my people. I am now an advocate for Aboriginal and Torres Strait Islander peoples. (Lingwoodock, 28/1/25)
Background
Colonisation and Aboriginal and Torres Strait Islander health
The arrival of the First Fleet into Australia in 1788 marked the beginning of unprecedented change in the lives of Aboriginal and Torres Strait Islander peoples (Aboriginal Heritage Office, 2025). Australian governments implemented discriminatory and oppressive policies and actions which caused human rights violations as well as institutional racism and discrimination towards Aboriginal and Torres Strait Islander peoples (Eckermann et al., 2011). Colonisation introduced new diseases and triggered massacres and violence, while the governmental policies of protectionism, absorption and assimilation resulted in Traditional Owners being removed from and losing connection to their country, community and culture (Human Rights and Equal Opportunity Commission, 1997; Victorian Public Sector, 2025).
Colonisation has resulted in poorer health outcomes for Aboriginal and Torres Strait Islander peoples. Aboriginal and Torres Strait Islander males born 2020–2022 have a life expectancy of 71.9 years, while females have a life expectancy of 75.6 years. This is 8–9 years less than non-Indigenous peoples with a more pronounced difference (12.4 years) in remote and very remote regions (Australian Bureau of Statistics, 2023). In addition, the burden of disease for Aboriginal and Torres Strait Islander peoples in 2018 was 2.3 times higher than for non-Indigenous Australians. Injuries and chronic health conditions such as cancer, musculoskeletal conditions, cardiovascular and respiratory diseases, and mental and substance use disorders, are the main contributors to the burden (Australian Institute of Health and Welfare, 2024). Behavioural risk factors identified as contributing to these health conditions include dietary risks, alcohol, tobacco and illicit drug use, physical inactivity, child abuse and neglect, unsafe sex, as well as intimate partner violence. Between 2003 and 2018, there has been an overall increase in the burden of disease for Aboriginal and Torres Strait Islander peoples (Australian Institute of Health and Welfare, 2024).
Since the 1960s, Aboriginal and Torres Strait Islander advocates have instigated actions designed to improve the health outcomes for their peoples. Original activities included the development of the first Aboriginal Medical Service in Redfern, New South Wales, in 1971, as well as the commencement of the Close the Gap movement in 2007 (Eckermann et al., 2011). Over time, the Australian Government has also increasingly incorporated strategies and resources into amending the disparity between Aboriginal and Torres Strait Islander health and that of non-Indigenous Australians. Recent endeavours include the National Agreement on Closing the Gap (Australian Government, 2020), the Cultural Respect Framework 2016–2026 for Aboriginal and Torres Strait Islander Health and the National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (Australian Health Ministers’ Advisory Council’s National Aboriginal and Torres Strait Islander health Standing Committee, 2016; Australian Government, 2021).
Critical Whiteness and Eurocentrism
Tertiary education institutions require academics and educators who are well versed and experienced in their fields to teach courses; however, it appears from the experiences of the authors that the main requirement or attribute for teaching an Aboriginal and Torres Strait Islander health course is focused on the academic identifying as First Nations. Although this seems to make sense, there is no consideration of the trauma which may be elicited by having to teach content on the horrendous treatment of your own people or having to manage students whose own worldview is consciously or subconsciously racist or discriminatory.
In addition, the skillsets of the individual, the variations in their personal and professional experiences, the differing impacts which colonisation has had on the individual or their family, or the disconnect they have experienced from community or country are not considered. While both the Aboriginal and Torres Strait Islander Health Curriculum Framework (Department of Health, 2014) and the Nursing and Midwifery Aboriginal and Torres Strait Islander Health Curriculum Framework (CATSINaM, 2017) provide guidance on the inclusions for First Nations health courses, there is an assumption that due to their Indigeneity, every First Nations academic has the requisite knowledge, experiences, capacity and capability to effectively deliver the content.
Understanding the conundrum of what pre-requisites and attributes an individual teaching Aboriginal and Torres Strait Islander health courses should possess requires consideration of the critical Whiteness and Eurocentrism prevalent in Australian universities. Whiteness is not limited to physical features but is the result of shared characteristics and proximity to others. It is developed and sustained through repeated societal interactions with the White dominant culture (Ahmed, 2007; Hafen, 2024). Ahmed (2007) suggests that whiteness trails behind actions, that it goes unnoticed and if people are to disappear into the “sea of whiteness,” they need to approximate whiteness—White identity.
Critical Whiteness Theory spotlights the role race plays in dominant worldviews, human interactions, social differentiation and socio-economic and health disparities. According to Diangelo (2018), Ravulo (2024) and Hafen (2024), critical Whiteness incorporates a number of components, as illustrated in Figure 1: White supremacy—the ideological belief in the superiority of White people; White privilege—being born with unearned privileges and status; White fragility—defensive emotive reactions as a result of discussions on racism; White ignorance—selective constructions of reality which perpetuate racism through ignoring anything which challenges this reality; White innocence—not acknowledging racism and also not wanting to know; and White identity—perceiving oneself as White and interacting as a White person (Diangelo, 2018; Hafen, 2024; Ravulo, 2024). White fragility is influenced by the Western ideologies of individualism, that is, the belief we are all unique and different from others even within a group, and objectivity, the belief we can be free of all biases. Individualism takes the stance that while we belong to varying groups, these are irrelevant to opportunities. This leads to reactions of defensiveness, certitude and argument when discussions of racism occur—White fragility (Diangelo, 2018). Hafen (2024) also discusses the concept of whiteness normativity as a means by which the belief in White supremacy is perpetuated through White ignorance, and that both interpersonal and institutional White ignorance form the foundations for White complicity, that is, strategies used to perpetuate racism through distancing of personal responsibility.
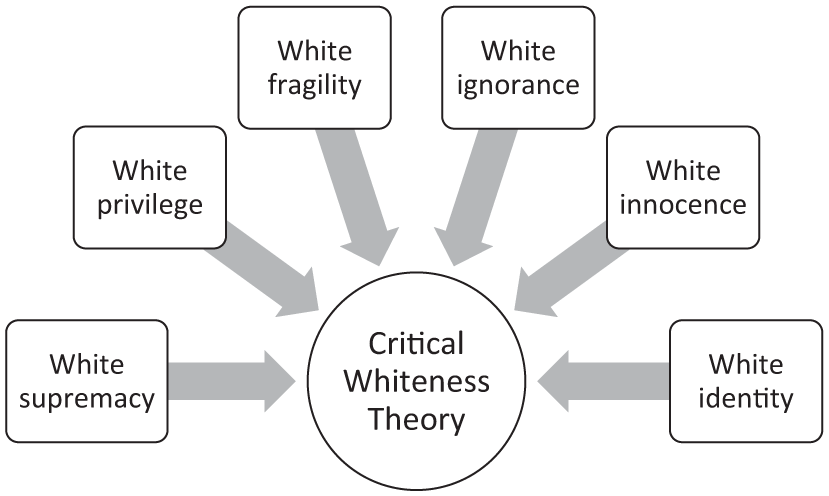
Components of critical Whiteness.
The components of critical Whiteness are implicit in the Eurocentrism prevalent in Australian universities. Ahmed (2007) highlights that being considered “White” propels the institution in an upwards trajectory with a promise of class mobility; that is, through being considered White, the institution demonstrates its superiority to others. The hierarchical structures and systems of knowledge within the Australian tertiary education sector are underpinned by Eurocentrism. Western forms of knowledge and power dominate in higher education through research, the scholarship of learning and teaching and practice frameworks, as well as managerial practices such as academic performance (Workman, 2024). These are important to consider when discussing the assumptions which are made in the Australian tertiary education institutions.
Discussion
Deciding that a First Nations academic should be teaching Aboriginal and Torres Strait Islander health courses demonstrates critical Whiteness: the White supremacy, White ignorance and White innocence of those making the decision. Tertiary education institutions are dominated by non-Indigenous Australians who, in deciding First Nations academics should teach Aboriginal and Torres Strait Islander health courses, are exerting power. As a result, there is a risk of overburdening First Nations scholars with carrying the weight of educating others about Aboriginal and Torres Strait Islander issues (Sivertsen et al., 2023). It further overlooks the need for academic balance and the desire for academics to focus on their specific areas of expertise.
Cultural interface
Since Aboriginal and Torres Strait Islander courses encompass a range of disciplines that examine the social, cultural, political and historical contexts, a collaborative, interdisciplinary approach may ensure that the course content is taught in a holistic and respectful way. First Nations and non-Indigenous academics working together in Aboriginal and Torres Strait Islander courses can create both a position of safety for academics and students alike and a place of discomfort. It provides an opportunity to learn and grow. West et al. (2022) highlight the need for Indigenous-led collaborations for both research and pedagogy in line with First Nations values. It is through working together and sharing that new knowledge and understanding across cultures can be created. Developing two-way understanding across both First Nations and non-Indigenous cultures provides an opportunity for everyone to develop their understanding and capabilities, while also challenging the institutional racism prevalent within tertiary education settings (Rix & Rotumah, 2020; West et al., 2022).
Nakata (2002) uses the term The Cultural Interface to describe the place where Western and Indigenous knowledges and domains intersect. In this interface, the life worlds and ways of knowing and understanding of each domain are interwoven, while at the same time, being in competition and in conflict with each other. Aboriginal and Torres Strait Islander health courses are a place where the Eurocentrism of Australia’s knowledge systems, beliefs and history are contrasted with those of First Nations culture and history as well as the political and social influences on them (Nakata, 2007). Understanding of this cultural interface is well-known to First Nations peoples but can be confronting, confusing and stressful for the non-Indigenous population to navigate. Within Aboriginal and Torres Strait Islander health courses, students as well as academics can be supported through the cultural interface, creating spaces which are culturally safe for everyone.
Assumptions versus reality
There is an assumption that all First Nations academics or health care professionals have been raised on their ancestors’ country and have strong links to this community. This is not the reality for many Aboriginal and Torres Strait Islander peoples. Colonisation continues to impact generation after generation of Aboriginal and Torres Strait Islander peoples including academics. Many Aboriginal and Torres Strait Islander peoples continue to search for their clan group with the desire to link up with the family from whom they have been separated and to find out about their ancestors and the culture of their peoples. Alongside the belief that First Nations academics have strong links to their ancestor’s community is the belief that they also have strong ties to the Aboriginal or Torres Strait Islander community in which they live. Just as a non-Indigenous person takes time to establish themselves in a new area, so too does a First Nations person. If you are not from the area, it can take years to build trusting relationships with the local Aboriginal and/or Torres Strait Islander community (Australians Together, 2025).
The belief that a First Nations academic should teach Aboriginal and Torres Strait Islander health at the tertiary level introduces concerns regarding Aboriginality and what this means. Should academics in this case fulfil their Aboriginality as defined by the government to be permitted to teach the course? Aboriginality as defined by the government requires evidence of being of Aboriginal descent, identifying as an Aboriginal or Torres Strait Islander person and being recognised and accepted by the community in which you live or have previously lived (Australian Institute of Aboriginal and Torres Strait Islander Studies, 2022). Some First Nations academics know through the oral history passed down in their family of their Aboriginal and/or Torres Strait Islander heritage, but due to historical governmental policies, they do not know which clan group or nation they belong to and hence are not able to provide proof of acceptance.
Another general misconception is that Aboriginal and Torres Strait Islander peoples are one homogeneous group, and that one group can speak for and understand the cultural practices of other groups. This is not the reality. There are two diverse nations – the Aboriginal Nation and the Torres Strait Islander Nation. Within Australia there are over 250 Indigenous clan groups, each with their own unique languages, culture, values and practices (Deadly Story, n.d.). While commonalities such as the importance of family, community and country thread through many First Nations groups in Australia, there are also vast differences in cultural practices and beliefs. Many of the cultural practices and beliefs are not appropriate to be shared with outsiders, and so discussions shared in public can only examine those practices and beliefs which are common to most and which are deemed appropriate to share. In addition, Aboriginal and Torres Strait Islander peoples do not always get along. Just as there are conflicts between non-Indigenous peoples, there are also disputes within and between clan groups (Kelly, 2007). In traditional times, there were tribal feuds. This type of competition has carried down the generations, and there is still feuding and opposition even today among Aboriginal and Torres Strait Islander peoples. Like intergenerational trauma, intergenerational feuds have been passed down. Disputes may be over cultural practices and country boundaries, taking of resources, wrong marriages or broken lore, and there is potential for these disagreements to spill over into the tertiary education sector. Differences of opinion and perspectives may result from course content being provided from the perspective of a First Nations academic from one clan group and having students from other clan groups with differing understandings.
An erroneous assumption is that all First Nations academics and health care professionals have worked or continue to work only in primary health care within Aboriginal and/or Torres Strait Islander Community Controlled Health Organisations (ATSICCHOs) and work specifically with Aboriginal and Torres Strait Islander clients. Working within ATSICCHOs allows health care professionals to provide care which is deemed culturally safe, thus increasing the likelihood of attendance by the Aboriginal and Torres Strait Islander clientele (Jongen et al., 2019; Taylor et al., 2020). Some First Nations health care professionals prefer to work within their own community, as they are already known by the people, and they understand the customs, cultural practices and language as well as the historical traumas which have led to a mistrust in the health care system; however, this is not true for all First Nations health care professionals. Although attendance at an ATSICCHO is often preferred by many Aboriginal and Torres Strait Islander people, the reality is that, at times, they must also attend other health care centres, such as hospitals and specialist clinics. First Nations health care professionals, who later become academics, may have worked in a variety of settings, with both Aboriginal and Torres Strait Islander peoples as well as non-Indigenous peoples.
A further assumption is that First Nations health professionals who later became academics have worked with a lot of other Aboriginal and Torres Strait Islander health care professionals. The reality, however, is that Aboriginal and Torres Strait Islander people made up just 3.1% of the health care workforce in the 2021 census (Australian Institute of Health and Welfare, 2025). Unless working in an organisation with a higher percentage of First Nations health care professionals such as an ATSICCHO, then the frequency of a First Nations academic having worked with another Aboriginal or Torres Strait Islander person with any consistency is limited.
There is also a belief that First Nations academics have a good understanding of colonisation as well as Aboriginal and Torres Strait Islander culture and beliefs; however, the reality is that their understanding may be as little as what they were exposed to in school. While there has been a gradual increase in the truths which are being taught in schools, older academics may only have been exposed to the westernised history about colonisation such as “Captain Cook discovered Australia or that Aboriginal people hold corroborees.” It was not until the 2008 National Apology to the Stolen Generations and the ensuing 2010 curriculum reform that the truth of colonisation and the treatment of Aboriginal and Torres Strait Islander peoples were included in Australia’s education curriculum (Keynes, 2024). This means that many academics, including First Nations ones, were not exposed to the truth except through their own research, through family, friends and community. There may be a vast difference between the knowledge a First Nations academic possesses as compared to what is required to effectively lead Aboriginal and Torres Strait Islander health courses.
Advantages, considerations and concerns
The expectations placed upon First Nations academics to be culturally and historically knowledgeable may not always align with the reality of their capabilities and experiences; however, there are advantages as well as considerations when having a First Nations person teaching an Aboriginal and Torres Strait Islander health course. Each of the traits a First Nations academic possesses has effects on the learners within Aboriginal and Torres Strait Islander health courses. These are presented in Figure 2.
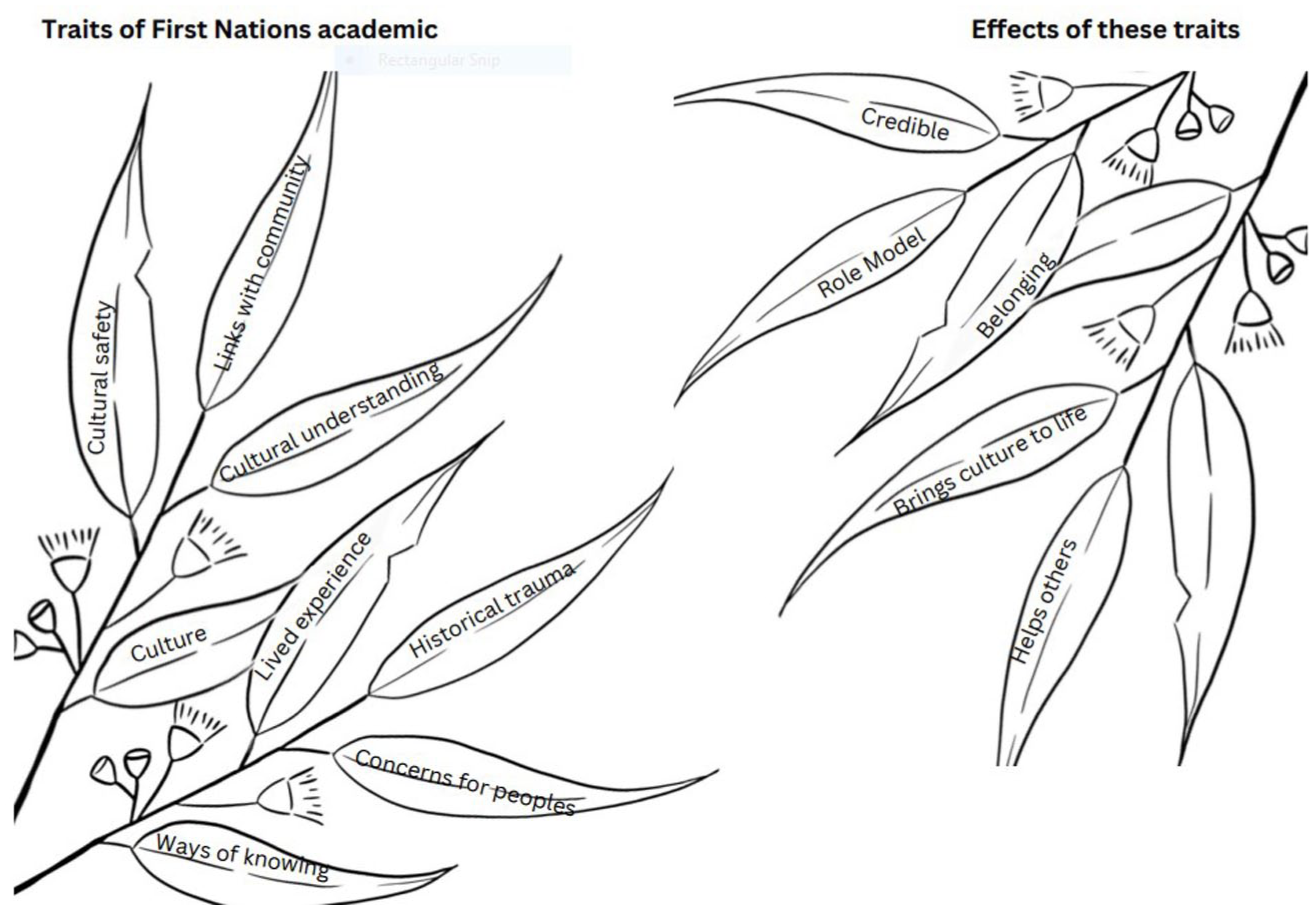
Traits of First Nations academics and the effects of these traits.
The traits of First Nations academics affect the way they present the content and the way the academic is viewed by those they are teaching. As each of the traits is impacted by the experiences, cultural knowledge and understandings of the First Nations academic, these traits may have both positive and negative effects.
Culturally and historically knowledgeable First Nations academics
First Nations academics, who have grown up as part of the community on-country, who understand the customs of their clan group and who have learnt the true history of Australia’s colonisation, may be able to transform the understanding of learners on the history and health of Aboriginal and Torres Strait Islander peoples. These First Nations academics may cultivate a sense of belonging and connection through culture with students who are Aboriginal or Torres Strait Islander. They may be seen as role models of what can be achieved even while navigating the Eurocentrism of Australia and of how knowledge can be used to help others. While these are positive aspects of having a culturally and historically knowledgeable First Nations academic, there needs to be acknowledgement that this understanding is specific to the individual and their clan group. Their life view may not align with those of members of other clan groups, thus limiting their ability to embrace the differential ideas of others or causing conflict.
Storytelling has been used in Indigenous culture to share historical events, culture, values and knowledge for millennia (Geia et al., 2013). The inclusion of storytelling from local Elders as well as discussion of the lived experiences of the culture of First Nations academics can bring Aboriginal and Torres Strait Islander culture to life for non-Indigenous learners enrolled in Aboriginal and Torres Strait Islander health courses. Storytelling allows First Nations academics to emphasise the impacts of the past as well as continued impacts of colonisation. In doing so, they may share personal experiences; however, they are risking exposing themselves to trauma. Having lived experience of culture is an advantage for First Nations academics, but this will have exposed them to the historical and current sufferings of their family and community. Teaching Aboriginal and Torres Strait Islander health courses in which colonisation and its ongoing impact, as well as discrimination and intergenerational trauma, are examined, may cause distress for the academic, which then impacts their social and emotional wellbeing.
As an Aboriginal or Torres Strait Islander person, the First Nations academic may share stories about situations in which they or their family did not receive culturally safe health care. This First Nations academic understands cultural safety and cultural capability through personal experience rather than just from a theoretical point of view. By sharing, they may be seen as more credible by some learners, but others may view them as being biased towards Aboriginal and Torres Strait Islander peoples. The White fragility of non-Indigenous peoples is a challenge which is not easily addressed, and the resultant behaviours can be traumatising for First Nations academics. Rather than being reflective, open to challenging their own understanding, and moving through cultural awareness and cultural sensitivity towards cultural capability in which they can provide care deemed culturally safe, the learners stagnate (Diangelo, 2018; Papps & Ramsden, 1996; Queensland Health, 2010). First Nations academics who give voice to information which is not affiliated with the Eurocentric understandings of society or of the educational institution are prone to receive negative feedback from students such as “not objective, accusatory, confrontational and unapproachable” (Mukandi & Bond, 2019).
Colonised First Nations academic
First Nations academics who have been colonised, who have limited knowledge and experience with Aboriginal or Torres Strait Islander culture, may struggle with teaching Aboriginal and Torres Strait Islander health courses. While they identify as Aboriginal or Torres Strait Islander, their experiences are reflective of many non-Indigenous peoples.
The lived experience of the colonised First Nations academic impacts their worldview. They will understand the world through a Western or a White lens, and their understanding of Aboriginal and Torres Strait Islander culture will be theoretical rather than developed through lived experience. While teaching an Aboriginal and Torres Strait Islander health course may develop their understanding of their people’s culture, their teaching methods and colonised outlook may also inadvertently be perpetuating a White Western perspective (Hafen, 2024). The academic may not be able to provide insight into the history or culture being examined and may be viewed by learners as not credible due to their lack of lived cultural experience and their cultural disconnect. This may also reduce their ability to foster a sense of belonging and culture with Aboriginal and Torres Strait Islander individuals undertaking the health course. Concepts such as historical trauma and intergenerational trauma may be difficult to comprehend due to not having any experiences of these or not being able to associate these with their own family history. Understanding of traditional knowledge systems and ways of knowing, being and doing may be foreign concepts.
The colonised First Nations academic may be regarded as not truly understanding the concerns of Aboriginal and Torres Strait Islander peoples; they may or may not have experiences with racism, discrimination, poverty or life living in rural, remote or very remote regions. The perceptions of others influence how an Aboriginal or Torres Strait Islander person is treated and whether they are viewed as being First Nations or not. For example, First Nations peoples with fair skin may be asked if they are sure they are Aboriginal or Torres Strait Islander, while those with darker skin may be perceived as being lazy or unintelligent (Doyle et al., 2017).
Although there are many concerns which come from having colonised First Nations academics teaching Aboriginal and Torres Strait Islander health courses, doing so also provides opportunities. It provides an opportunity for First Nations academics to learn about the history and culture of their peoples, but this may also result in new trauma for the individual as they learn the truth. If the academic comes into teaching the course with a growth mind-set, they will benefit from listening to the stories of the Aboriginal and Torres Strait Islander learners. The greatest benefit, however, would come from working alongside a culturally and historically knowledgeable First Nations academic. It presents the opportunity for the colonised First Nations academic to learn about themselves and the culture of their ancestors. This allows them to develop and grow their understanding with the cultural guidance of their First Nations brother or sister. Conversely, the colonised First Nations academic may prefer to keep their Indigeneity unexplored.
Important considerations
Cultural capability and cultural safety
There are many advantages of having culturally and historically knowledgeable First Nations academics teaching Aboriginal and Torres Strait Islander health courses; however, the reality is that there are few First Nations peoples working in academia and even fewer with the requisite understanding to teach a health course (Hutchings et al., 2018). The expectation that a First Nations academic should be the one teaching Aboriginal and Torres Strait Islander health courses needs consideration. As indicated in section 3.3.3 Staff Capacity of the Nursing and Midwifery Aboriginal and Torres Strait Islander Health Curriculum Framework (CATSINaM, 2017), there are a low number of non-Indigenous staff with the requisite knowledge to teach about Aboriginal and Torres Strait Islander peoples and that upskilling all staff and building the cultural safety in the workplace are essential for delivery of this type of curriculum. If there was a greater focus on building the cultural capability and cultural safety of non-Indigenous academics, the potential for re-traumatising and overburdening of First Nations academics could be reduced, freeing them up to utilise their expertise in other areas. It may be better to have a non-Indigenous academic who has experience working with Aboriginal and Torres Strait Islander peoples and who understands the history and culture of First Nations peoples teaching these courses. It should be the right of the First Nations academic to choose whether they teach Aboriginal and Torres Strait Islander health courses and not one which is forced upon them simply because of their Indigeneity.
Colonial load and cultural responsibility
First Nations academics are considered the Indigenous knowledge holders for their specific discipline as well as the person who provides support to Aboriginal and Torres Strait Islander learners within their programmes (Sivertsen et al., 2023). They are expected to be involved in anything “Aboriginal and Torres Strait Islander” at tertiary education institutions including research and any community events. Until recently, the term cultural load was used to describe the burden that they must be involved in everything; however, it is now recognised that culture is not the problem, but rather the legacy of colonialism (Selkirk, 2025; Selkirk et al., 2024).
The expectation that First Nations academics will provide unfettered access to their time and knowledge without a subsequent reduction in other areas is encompassed in what is being termed as “Colonial Load” (Selkirk et al., 2024). Colonial load relies on First Nations academics helping to untie the structured knots from colonisation, Eurocentric practice and systemic racism which are prevalent in our institutions worldwide including tertiary education. These knots include decolonising curriculum, acting as a critical friend for programme accreditation, being an access portal to community and providing staff individually or in groups with education on cultural safety and on Aboriginal and Torres Strait Islander peoples and culture (Jongbloed et al., 2023; Selkirk, 2025). While each of these activities goes towards removing the structural and systems impediments for First Nations peoples, it creates a burden upon First Nations academics which their colleagues do not share. Colonial load or burden is something many Aboriginal and Torres Strait Islander workers have been carrying for decades with limited or no acknowledgement from their employer. First Nations peoples carried this load, as they feel obligated to do this. Not many would even realise this is a “thing” that can cause ill-health and burnout for Aboriginal and Torres Strait Islander peoples. It needs to be acknowledged and recognised by employers.
In addition to the high colonial loads of First Nations academics within tertiary education institutions, they also have obligations to family and community outside of the workplace which are cultural responsibilities (Selkirk et al., 2024). First Nations academics take on high loads as they are driven to improve the health outcomes of their peoples through keeping Aboriginal and Torres Strait Islander peoples engaged in education and striving to move forward (Lloyd et al., 2015; Tesiram, 2022). To add the requirement to teach a course which explores the oppression and differential treatment of your own peoples may be emotionally overwhelming and traumatising to the First Nations academic. While Aboriginal and Torres Strait Islander peoples have shown to be resilient through surviving the colonisation of Australia, the social and emotional wellbeing of the First Nations academic must be prioritised.
Teaching and learning
Due to the distinctive nature of the content being explored and how the aim of both the Aboriginal and Torres Strait Islander Health Curriculum Framework (Department of Health, 2014) and the Nursing and Midwifery Aboriginal and Torres Strait Islander Health Curriculum Framework (CATSINaM, 2017) is to develop cultural capabilities in health programme undergraduates, the question of whether an Aboriginal and Torres Strait Islander health course should be taught by someone with a teaching qualification should be considered. There is a need to recognise that while First Nations academics can be incredibly valuable in teaching health courses, teaching requires not only lived experience but also formal expertise and professional training and understanding of teaching and learning approaches as well as ontological and epistemological approaches (Galea & Rousell, 2022).
The dynamism which encompasses First Nations culture needs to be captured and presented in meaningful ways within Aboriginal and Torres Strait Islander health courses. This ensures that learners not only access knowledge but also reflect on and integrate it into their existing life worlds and worldviews to create new understanding. It is also important in the teaching of Aboriginal and Torres Strait Islander health to consider approaches suitable for teaching about this marginalised group to pre-dominantly non-Indigenous people. The traditional objectivist approach to teaching and learning is not suited to this. This approach emphasises the transmission of information to the learner, often through an acontextual lens, and without consideration for how the learner will perceive or construct meaning from it (Brown, 2009).
Constructivist approaches consider the construction of meaning by the individual and that teaching is a facilitator of this. All people come with differing social worlds, experiences, beliefs and understandings which influence how each individual constructs meaning. “Critical realism” positions itself in the idea that while there is a reality independent of individuals, it is the individual through their experiences who constructs their own understanding of that reality (Brown, 2009; Galea & Rousell, 2022). This philosophical approach lends itself effectively to the teaching of Aboriginal and Torres Strait Islander health. The reality which exists for both First Nations people and for non-Indigenous people is real, but it is their experiences which have created a different understanding of this reality.
Critical ontology is also important for teaching Aboriginal and Torres Strait Islander health courses. Colonisation led to the progressive subjugation of First Nations history, culture and peoples through historical acts, contemporary policies and societal normalisation of White supremacy. Critical ontology recognises how all aspects of society have been shaped by the dominant culture—within Australia, Eurocentrism (Kincheloe, 2011). Indigenous ontologies emphasise relationality and holism. Incorporating Indigenous knowledges, ways of knowing, being and doing within Aboriginal and Torres Strait Islander health courses can challenge non-Indigenous students to question their own beliefs, assumptions and stereotypes, leading to opportunities for mutual respect through relationality (Workman, 2024).
Conclusion
It is important to recognise the fact that just as with any academic, First Nations scholars have diverse areas of expertise. They do not necessarily specialise in Aboriginal and Torres Strait Islander health. Traditional knowledges incorporate all aspects of life—spirituality, history, cultural practices, social interactions, language and healing. Most academics are still very Eurocentric, but First Nations scholars, researchers and lecturers are making some headway in this field. We now have many Indigenous-led institutes established within various universities across Australia. Aboriginal academics are putting traditional knowledges at the forefront and blending it in with Western education as much as possible. This gives Aboriginal and/or Torres Strait Islander peoples the best of both worlds.
While the content for Aboriginal and Torres Strait Islander health courses is guided by the health curriculum frameworks, these courses are run by Australian tertiary education institutions which are overwhelmingly Eurocentric in their scholarship of learning and teaching. The traditional ways of knowing, being and doing which are central to First Nations culture and must be supported in Aboriginal and Torres Strait Islander courses if they are to support the development of the cultural capabilities of undergraduates. The academic who teaches these courses must be culturally and historically knowledgeable or supported to become knowledgeable and culturally safe, regardless of whether they are Aboriginal or Torres Strait Islander or if they are non-Indigenous.
The disparity between the assumptions and the reality of teaching an Aboriginal and Torres Strait Islander health course raises the questions of who the best people are to teach Aboriginal and Torres Strait Islander health courses. If a First Nations academic is teaching these courses, we must consider how can the risks to social and emotional wellbeing be reduced. Further research must be undertaken in several areas: what the teaching of Aboriginal and Torres Strait Islander health courses encompasses; the expectations which tertiary education institutions place on First Nations academics versus that of non-Indigenous academics; how working at tertiary education institution influences the social and emotional wellbeing of First Nations academics and how the colonial load on First Nations academics can be shared and reduced.
Footnotes
Acknowledgements
The authors would like to acknowledge the Aboriginal and Torres Strait Islander peoples as the Traditional Custodians of Australia and the Elders and leaders, past and present, for guiding our peoples through the challenges of the past and who will lead us into the future. The authors would like to acknowledge Faith Griffits for assisting with the development of ![]() and Australian tertiary education institutions for aiding in transforming the understanding of university students through the inclusion of Aboriginal and Torres Strait Islander courses across programmes.
and Australian tertiary education institutions for aiding in transforming the understanding of university students through the inclusion of Aboriginal and Torres Strait Islander courses across programmes.
Authors’ note
This topic is part of a broader research project examining Aboriginal and Torres Strait Islander academic experiences of teaching First Nations courses and making recommendations for support of First Nations academics.
Ethical considerations
No ethical approval was required for this research.
Author contributions
All authors have provided intellectual contribution to the conceptualisation, formal analysis, validation and writing review and editing of the paper and revisions. SM also contributed to the writing of the original draft and visualisation.
Funding
The authors received no financial support for the research, authorship and publication of this article.
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship and publication of this article: Each of the authors is currently or has previously been employed in a tertiary education institution as a teacher for Aboriginal and Torres Strait Islander courses. The topics discussed in the article are applicable to the authors’ experiences.
