Abstract
First Nations peoples in Australia are disproportionately affected by diabetes. We report on a qualitative evaluation of a healthy lifestyle group programme at an Aboriginal Community Controlled Health Service. The programme was designed by an Aboriginal Health Worker and took place in a regional community. Yarning interviews of five participants and four facilitators were conducted followed by a collaborative analysis. The group context provided connecting and relationship-building opportunities, allowing participants to feel that they were seen as an individual. The accidental hybrid approach adopted due to the impact of COVID-19 pandemic lockdown supported transition of healthy activities into the home context while still accessing support and motivation from the group. This paper concluded that the unintentional hybrid programme found promising individual and cross-generational health and wellbeing benefits for First Nations families which suggests that intentional hybrid frameworks may show promise in improving First Nations peoples’ health and well-being.
Keywords
Introduction
The longest continuously existing culture in the world are the Aboriginal and Torres Strait Islander peoples of Australia. Prior to colonisation of Australia, First Nations Australians had no signs of western diseases due to healthy lifestyle and diet and had incredible knowledge about plants, seasons, animals, the ecosystem, and land management (Evans et al., 2021). The current state of health of First Nations Australians has been influenced by intergenerational trauma and dispossession brought on by more than 200 years of colonisation. First Nations Australians’ nutritional and physical activity habits were altered by colonisation, switching from a traditional diet to a western diet, introduction of tobacco, and increasing sedentary behaviour. Other aspects of the health of First Nations Australians are related to the broader social determinants of health, such as income, work, and education (Evans et al., 2021).
Diabetes is a chronic condition with the fastest rate of growth worldwide. The risk of acquiring diabetes is highest in Indigenous peoples and socially disadvantaged individuals worldwide (Ride, 2022). According to Australian Institute of Health and Welfare (2020),
Diabetes is nearly three times as common in First Nations Australians than non-Indigenous people.
Compared to non-Indigenous people, First Nations Australians have four times higher risk of dying from diabetes.
Compared to non-Indigenous children, First Nations Australian children have a 6- to 20-fold increased risk of type 2 diabetes.
Lifestyle risk factors for diabetes include insufficient exercise, smoking, excessive alcohol consumption, poor diet, and poor nutrition. In addition, there are social and emotional issues, including racial discrimination, incarceration, access to resources, housing, poverty, and education. Addressing these issues requires a variety of culturally relevant prevention and management programmes that are designed by and for First Nations Australians (Ride, 2022). Meaningful participation is essential to empower First Nations Australians in health promotion. To achieve this, it is necessary to ensure that First Nations Australians have influence over health promotion activities and that all design components are responsive to cultural differences (Paramenter et al., 2020).
A health and well-being programme was designed by an Aboriginal Health Worker and member of the community for community members with diabetes in a regional location of Australia at an Aboriginal Community Controlled Health Organisation (ACCHO). It was a 10-week healthy lifestyle programme that encouraged community members living with diabetes to increase their physical activity levels and embrace healthier eating through gym-based exercise sessions and group cooking activities called cook-up sessions. This article discusses the key learnings from evaluation of the programme and focuses on the client’s experiences.
Method
A partnership was established, in 2019, between the ACCHO and researchers at a University Department of Rural Health (UDRH) to evaluate the ACCHO diabetes group programme. The first group programme took place in 2019 and a limited evaluation, impacted by the SARS-CoV-2 (COVID-19) pandemic, was completed by a team comprising a non-Aboriginal research lead, a non-Aboriginal researcher (K.F.), and an Aboriginal research liaison. The second iteration of the programme commenced in 2021. Due to staff changes at the UDRH, the opportunity to review the team who would participate in the second evaluation was taken. Reservations about the inherent power differentials experienced during the first evaluation of the programme and acknowledging the history and harm caused to First Nations communities from western researchers doing research to rather than with Aboriginal people, the non-Aboriginal researcher invited an Aboriginal researcher (J.L.), who had been involved in initial discussions about the programme and evaluation, to join her as co-lead of the second programme evaluation. An Aboriginal research liaison (R.W.) was also included in the research team. Participants were acquainted with the research liaison because she was also a healthcare worker at the ACCHO. It was felt that her participation would enable a culturally safe setting for participants.
Researchers’ backgrounds and positionality
This section will provide a brief description of the research team’s backgrounds and positionality. Positionality describes an individual’s worldview which informs how they approach and think about their research (Rowe, 2014). Each paragraph below is written from the perspective of the individual researcher, thus is written in first person.
I (K.F.) am a very recent import into Australia (arriving in 2003). I am of western descent, a physiotherapist and predominantly qualitative researcher. My life and work in Australia have been spent in regional locations, which has provided me with some insights into living in regional areas and the inequities rural communities experience in accessing healthcare. But I am also aware that my western worldview, including my innate privileged experience of healthcare and life, could impact my understanding and interpretation of the Aboriginal participants’ voices in this research. Thus, it was important that the research was conducted collaboratively with an experienced Aboriginal researcher to guide the research team and that we employed research approaches to ensure the authentic voices of the participants were heard and presented. Practically, this meant purposely using a shared and consultative approach in the planning, conduct, and analysis of our research and making sure that our interpretation was well grounded in the data. Our research partnership gave me greater insights into being a trustworthy collaborator: to be guided, to ask questions, and to listen more.
I’d like to start by acknowledging the Wiradjuri people, from central western New South Wales (NSW), as the Traditional Owners of the land that I work, study, and live on. I pay my respect to Elders who have passed and those present and emerging. I also acknowledge the Traditional Owners of the lands that readers live upon. To establish connections and develop relationships, it is customary to introduce and share information about oneself. I am a Cameron and identify as a fair-skinned, blue-eyed First Nations woman. I am a proud descendant from Scottish immigrants and British convicts on my mother’s side, and Wiradjuri nation and Bunjalung nation in northern NSW on my father’s side. I am the youngest of five, raised in a nuclear family with strong values, but removed from my cultural knowledge as my father was a part of the Stolen Generation. However, I am not removed from discrimination and institutional racism in my everyday life. As an experienced registered nurse, registered midwife, academic, researcher, and Wiradjuri woman, it was crucial for me that our research allowed First Nations Australian voices to be heard. I established my identity first as an Aboriginal person and then as a researcher (Martin & Mirraboopa, 2003; Parter & Wilson, 2021). My approach was partly in response to most western-led research that has been done on First Nations land without First Nations people’s consent, consultation, or participation (Martin & Mirraboopa, 2003). Our project included both First Nation and non-First Nation researchers. These researchers brought a variety of skills to the table, including cultural competency, clinical expertise, scientific knowledge, understanding of the health system, and other work and life experiences.
As the Aboriginal research liaison, I (R.W.) think we worked well to pull the information and context out of the interviews. It was culturally safe, and we were generally curious and passionate about what our participants had to say. I felt supported and included in the process and felt we all worked in harmony together.
Timing of research and ethical approvals
This article focuses on data from the second iteration of the programme which ran from July to September 2021. Halfway through the programme, the region in Australia was put into lockdown due to an outbreak of COVID-19 and the programme pivoted to continuing via telehealth. The pandemic and subsequent closures also negatively impacted the amount of quantitative data that were gained post-programme. This article pertains solely to the qualitative data obtained. Approval for the research was gained from the university Human Research Ethics Committee (H20033) and the NSW Aboriginal Health and Medical Research Council (1649/20).
Recruitment
The researchers provided an initial briefing about the research at the end of a cook-up (group cooking session) during an early part of the programme and attended some aspects of the programme to ensure that participants got to meet them prior to asking for their consent to take part in research yarning interviews. All participants (n = 8) and facilitators (n = 4), who took part in the programme, were invited to take part in yarning interviews. Participants and facilitators were contacted by a researcher, provided with further information about the evaluation, and invited to participate either online or face-to-face, dependent on their preference and access due to COVID-19 restrictions and state border controls. First Nations Australians frequently employ yarning. Yarning refers to a discussion or conversation. The sharing and exchange of information during a yarn may take place in an informal or social setting and is a familiar way of exchanging information for First Nations Australians. During interviews yarning was employed to visit places and discuss topics that are interesting and are related to the research project (Bessarab & Ng’andu, 2010). It is a method that necessitates the researcher to forge relationships with Indigenous participants who are trustworthy and accountable.
Data collection
Data were collected between September and October 2021. The yarns were semi-structured to provide opportunities to explore each person’s experience of either taking part or facilitating the programme. Meaning was clarified during the interviews by the researchers paraphrasing participants’ answers to ensure understanding and enable deeper reflection. Five out of eight participants (three women, two men) and all the facilitators (n = 4) took part in yarning interviews.
Data analysis
Initial analysis of the programme participants’ transcripts involved two stages of collaborative yarning (Bessarab & Ng’andu, 2010). First, the researchers and the liaison met twice to identify initial key themes from the transcripts. Second, to conduct member checking and ensure that we had heard their story, programme participants were invited to attend a morning tea at ACCHO, where a preliminary analysis of their experiences was presented to the group. Figure 1 shows the infographic that was presented to participants as part of member checking and data analysis. Programme participants provided feedback on the preliminary analysis, which provided a starting point for the next phase of analysis. Transcripts of the facilitators’ interviews were sent via email to the participants for member checking prior to analysis.
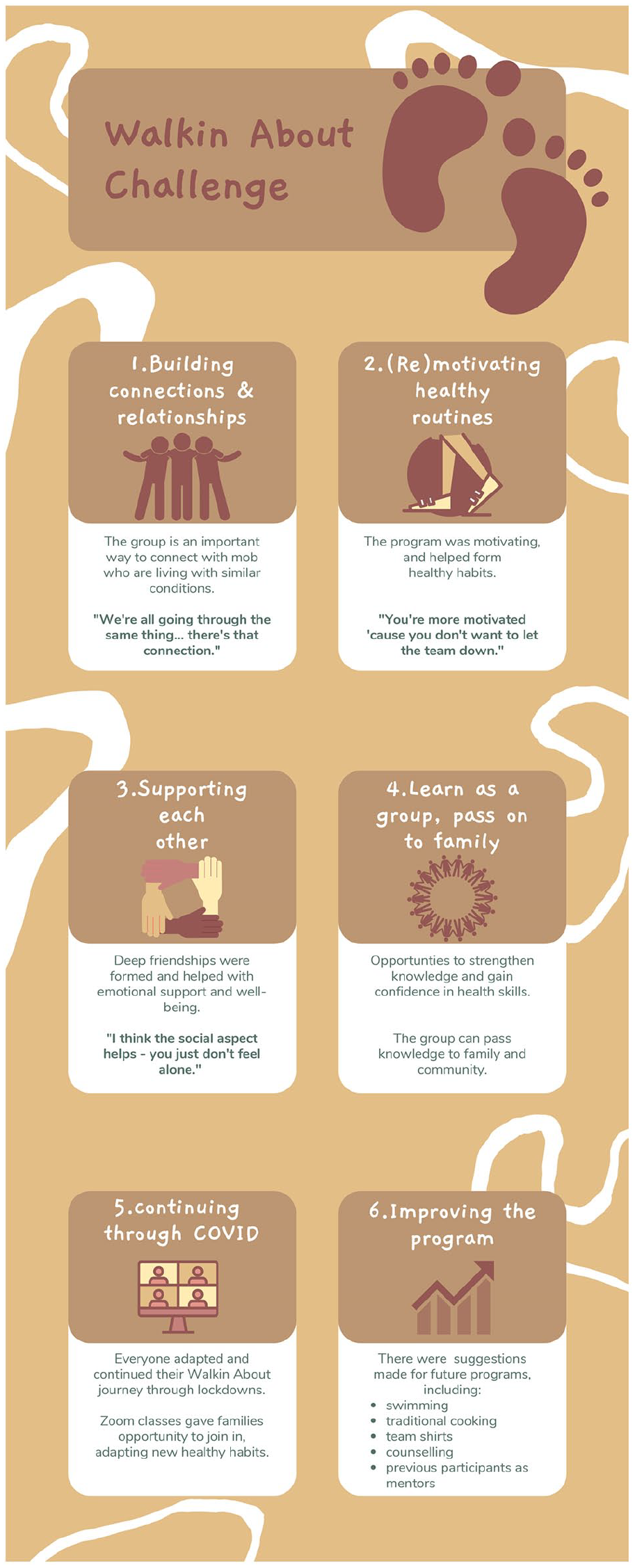
Have we got your story, right? (Created by Holly Hoad (Wiradjuri)).
Subsequent analysis involved two further phases. We identified themes and subthemes by searching for similarities and duplicates across each individual transcript, resulting in the creation of two transcripts: one of programme participants’ voices and one of facilitators’ voices. Themes and subthemes were then refined into a focused thematic analysis. Finally, the participant and facilitator data were combined by identifying similarities and differences across the two transcripts to provide as detailed an account of the programme as possible. Regular analysis meetings were held, which allowed for peer examination of the initial identified themes and enhanced the researchers’ capacity and awareness of their reflexivity through discussion including challenging of interpretations.
This article focuses primarily on the programme participants’ voice with data from facilitator interviews used to augment understanding of the participants’ experiences and examine the impact of an accidental hybrid programme upon those experiences. For this article, a pseudonym was assigned to each participant.
Results
In a group, we’re not just a number
Participants felt that the group programme allowed them to be seen, and understood, as a person. Analysis identified nine aspects that contributed to this feeling:
Shared experience of diabetes
Supporting each other
Supportive groups enabled confidence
Groups enabled learning
Groups provided a cultural experience
Informal style aided rapport
Participants could tell their real story
Group rapport enabled re-engagement with individual appointments
Experiential learning opportunities on multiple aspects of health.
These aspects are discussed below.
Participants appreciated meeting other people who were living with diabetes. The programme provided an opening for connecting with each other. “Because we’re all going through the same thing with the diabetes and all the rest of it, there’s that connection” (Naomi, participant). The participants appreciated these new connections as many of the participants did not have immediate family members who were living with diabetes. The programme provided them with a sense of belonging and a friendship circle of mob who had greater insights into their health experiences and worries.
They enjoyed the supportive group context. “It’s about support, so you support each other, and it helps a lot, especially mentally as well as physically. But mentally because that lets you know you’re not doing it by yourself” (Noah, participant). As this excerpt showed, the sense of belonging that participants gained made them feel that they were not on their health journey alone. They also found opportunities to give each other support during the programme. “It’s that comradery that, as a participant, you’re saying, ‘If you can do this, I can do this’. And we can all support each other in achieving our goals” (Pete, participant).
The supportive context in the group helped participants gain confidence to try new activities, such as exercising in a gym. “It shows us all we’re not doing this alone, that there’s others that have the same issues. It also broadens your horizons. Some of us tried stuff that we’d never tried before” (Pete, participant). The increasing bond between participants led them to feel a commitment to the group as they did not want to disappoint their team: The exercise, the cooking, it’s just easier if you’re not doing it on your own. You’re more motivated “cause you don’t want to let the team down. Like there was one day, I didn’t want to go, and it’s like, “No, I have to go.” (Naomi, participant)
This excerpt suggests that participants’ connection and commitment to the group could be an important factor in their attendance.
Some members of the group continued to meet up once the group had finished. They described how they would meet up in a park, use the outdoor gym equipment, and “just gasbag about what’s goin’ on in our lives” (Ruby, participant). Importantly, their gasbags now included discussions about their diabetes monitoring including glucose levels. “We talk about our sugar levels, which is helping me, ’cause I never understood sugar levels” (Naomi, participant).
Prior to the programme, some of the participants were not engaging regularly with all the health professionals required to manage their diabetes and other health conditions. They explained that their experience of appointments had been unsatisfying because they had a different focus of the health professionals who were concentrated upon monitoring many aspects of diabetes. “You’re sitting there and you’re basically saying, ‘I need help with this’. And they’re saying, ‘No, we need to do this’. It doesn’t work. Why bother?” (Naomi, participant). In contrast, the group programme provided participants with a context that they felt was more suited to their needs including greater duration of time. “You need wriggle room, and with this, we got that with [name of facilitator] ′cause we had an hour and a half, two hours where we were here cooking” (Naomi, participant).
The longer, more informal, nature of the group programme provided opportunities to build rapport and understanding with staff. “It shows that you’re not just someone that comes in, gets this done, and then see you later. It shows that we’re not just a number at the end of the day” (Naomi, participant). Thus, being part of the group allowed participants to feel that they were seen as a person. Facilitators agreed, “They also felt that they got to know the facilitators better, and that the facilitators got to know them as people.” The experience of relationship-building was reciprocal; both participants and facilitators felt they gained insights into the other, as a person.
Progress was also made in the supportive group context because participants felt able to tell their real story. “It’s fine to not tell the truth if you don’t feel safe to tell the truth. If we can create a place where people feel safe to tell the truth, then we’re gonna get somewhere” (Olivia, facilitator). Many of the group activities may have contributed to the feeling of being seen and valued as a person—for example, walking together, preparing food together, and cooking and eating together. These activities not only took time to complete, which allowed greater opportunities to talk, but they also involved doing the same thing together, often side-by-side completing the same or similar task. This created a sense of camaraderie and levelled power differentials. “There’s something about eating together as well, it means that everybody’s equal in a way that I think it’s hard to achieve in any other setting” (Olivia, facilitator).
Thus, despite working towards their individually identified health goals, participants did not feel alone in their quest, as the group context provided connection and support from both fellow participants and the facilitators.
The participants felt that the group experience and rapport gained with the facilitators would help them when they returned to individual health appointments: I know now that it’s finished that I’ll still go back to half hour appointments with [name of facilitator], but it’s gonna be easier. There’s already that rapport there, so it’s not trying to build it in small appointment [times]. (Naomi, participant)
The relationship-building within the group programme led some participants to book appointments with health professionals whom they had not been seeing regularly prior to the programme to help them with their diabetes management. “I’ve booked in with [Name of health practitioner] to re-evaluate, which if I hadn’t had done these groups, I wouldn’t have done” (Ruby, participant).
Finally, the group provided experiential learning opportunities with diet, healthy cooking, physical activity, and living with diabetes. “It really helps you because you know what to feed your body, like what foods, what’s good for you, what’s not” (Pete, participant).
It supported participants to adopt healthier routines, achieve some of their health goals, and then look further into the future for their health: I think my mindset at the start was, “Okay, I’m just participating because of my diabetes.” But, as the weeks rolled on, it was like, “Right, this is a good way of monitoring where I’m at and where I wanna be.” (Noah, participant)
The emphasis of the programme was on making lifelong changes and healthy choices through informal experiential learning opportunities. But one participant felt that their needs were not met with regard to understanding diabetes monitoring. “I don’t even know why I have to monitor my sugars” (Diane, participant). Facilitators also noted that the programme might benefit from a more structured education session to consolidate participants’ understanding of diabetes and its management. “I think that another thing that maybe could be added within the program next time could be some form of education session” (Paula, facilitator).
In addition, some participants thought the 10-week programme was too short to get themselves into a good routine: Ten weeks is good, but if it went longer, if it went—say, if you done it over a 12-month period it would be more beneficial for the participant, simply because you can get into a routine at ten weeks but then you can easily—slip out of it. (Pete, participant)
In summary, this section showed that the group programme provided opportunities for participants to be seen as a person, share their experiences, gain confidence, learn in culturally safe settings, and tell their real story.
Pivoting to home during pandemic lockdown
During the programme, the impact of COVID-19 pandemic resulted in a lockdown midway through the programme for 4 weeks. The programme pivoted to delivery via telehealth. The programme coordinator continued regular contact with participants during this time, individualising communication with participants according to their communication preferences, which meant that participants remained engaged in the programme. “The internet became a barrier because a few of the participants didn’t have internet. That didn’t stop them from participating. I still received photos from them cooking their meals and sending them through” (Emma, facilitator).
Participants appreciated the efforts made to keep the programme going, pointing out that it helped them maintain their momentum. “Because if we’d had a break, I think it would’ve been hard to come back together and pick up and start again” (Pete, participant).
Despite variable access to the Internet, everyone adapted in their own way and continued with the programme at home during the lockdown. Some reframed their inability to participate fully in the online space as another source of motivation. “Not bein’ able to fully participate 100%, was upsetting, but also another form of motivation for me to continue doing as best I can in the program and then looking forward to catchin’ up” (Noah, participant). This excerpt showed, however, that some participants felt that being unable to engage online in the same way as everyone else led them to feel as though they were unable to fully participate.
The facilitator of the cook-ups observed that going into lockdown also had unexpected benefits. Those who had less confidence in a face-to-face context, and therefore engaged less, had to engage more during online cooking in their kitchen: What happened when we went online was every person cooked in their kitchen with their iPad propped up and them going, “Now is this how I chop the onion?” And, “What do I put in next?” It meant that instead of those two to three people taking the lead, everybody got the chance to develop their skills and confidence. (Olivia, facilitator).
Participants were also supported to continue their exercise at home via a home exercise programme and provision of weights and resistance bands. Participants either joined in zoom exercise sessions or discussed via phone their exercise programme with the exercise physiologist: I just sort of had those check-ins over the phone and spoke them through the program. If they had any questions, they would ask away, and we’d try and break down barriers if there were any or try and make it as flexible as possible. Most of the exercises within the home exercise program were things that we may have done in the gym. (Grace, facilitator)
Thus, there was a sense that pivoting the programme to home, participants were continuing with the programme rather than learning new exercises or ways of doing things at home. The transition to home during the lockdown showed participants what exercise they could do at home, with many of them reporting that they were still using their home exercise equipment. “You can do them at home every day, they’re everyday movements you can do. They gave us weights and a band as well, and a printout sheet of what to do. We’ve been doing it at home” (Diane, participant).
In summary, all participants continued with the programme through various telehealth modes, which provided them with experience and confidence to continue with these activities at home.
Sharing knowledge and activities with family
As can be seen from the last excerpt, many participants described how they gained company from their family when doing programme activities. Participants described the online format as “interesting” and “more like real life” because they could see kids milling around in the background, joining in, and offering, sometimes cheeky, commentary to their parents. “It was fun. Some of comments people come out with, and not just us in the program, the kids” (Naomi, participant).
The pivot to continue the programme at home via telehealth provided opportunities for participants to pass on their knowledge and learning to their family. “If you get them in helping you cookin’ or choosing, they’re more likely to eat it” (Diane, participant). Participants gained understandings into how their new knowledge, skills, and recipes would be received by their family, as well as positive insights into cooking together.
Some children joined in the exercise sessions, which resulted in the sessions becoming movement breaks for the whole family at a time when children were spending long hours at the computer for school: Myself and my two girls and when my son’s home, he does it as well. For their movement break. They love it, that I can move again and that we’re doing it together, they just like being together. . . . Just getting out and moving and exercising’s helping them calm down after meetings all day. Sitting in front of the computer all day isn’t helping them and it just makes them turn the TV off or exercise and get some movement, not be so sore. (Diane, participant)
As a result of pivoting to home programme for 4 weeks, participants reported several family benefits. They described how their family had learnt more about healthy living and living with diabetes. “It’s been a whole family involvement . . . . They understand the portion controls and glycemic” (Noah, participant).
Families also formed new exercise routines, from movement breaks in home schooling to cross-generational walks. In the excerpts below, a father described how he and his daughter had created several new routines that they enjoyed together. “It’s routine now, and she looks forward to it. We do the walking in the morning, and the Friday nights is cooking in the fire” (Noah, participant). Their new walking partnership had not only increased their physical activity levels but contributed to their father–daughter relationship too: It’s a father–daughter relationship, just expanding on that and you know that it’s good for us healthy-wise, walking and seeing different parts of the community. We started off walking two blocks, and now we’re up to three and four blocks. (Noah, participant)
As can be seen above, participants began new healthy routines during the programme and felt that they would be able to continue independently or with their family.
In summary, the hybrid model provided opportunities for families to join in and for participants to share their new health knowledge.
Summary of results
This qualitative exploration of a group health behaviour change programme for First Nations peoples living with diabetes in Australia provided the following insights. The group context enabled participants to feel that they were seen and acknowledged as an individual because it provided connecting and relationship-building opportunities. The accidental hybrid approach supported transition of healthy activities into a home context while still accessing support and motivation from the group. Finally, some family members joined in the home-based activities, suggesting possible cross-generational health benefits could be gained from telehealth home-based activities. These aspects will be discussed further in the following section.
Discussion
The group provided a context that allowed participants to feel they were seen as a person, and not just a number. The group programme’s focus on experiential learning and reciprocal support contrasted with their experiences of more regimented individual appointments, where the opportunities to build rapport were restricted by time constraints and a focus upon disease monitoring. These barriers to the individual appointments concur with findings from previous research (Panaretto et al., 2010). The impact of culture on how individual chronic health monitoring appointments are experienced should not be underestimated when the research shows the need to spend more time in relationship development.
We found that the lack of opportunities for connection between client and health professionals during individual appointments had resulted in some First Nations clients ceasing to attend their individual appointments, which is likely to have led to reduced monitoring of health and well-being, and chronic disease management. Basic psychological needs theory provides further insight into this finding. It posits that a person’s psychological well-being and wellness is centred upon three universal needs: relatedness, autonomy, and competence (Deci & Ryan, 2008). Any context that thwarts one of these needs will impact a person’s well-being (Deci & Ryan, 2008). Relatedness is described as the quality of connection a person feels in their social context with a greater sense of relatedness, leading to improved well-being and increased confidence in relationships (Sánchez & Núñez, 2007). Thus, a relationship where clients feel known, valued, and cared for is considered important to support a client’s openness to new information and behaviour change (Ryan et al., 2008).
We found the group context allowed trust and connection between clients and health professionals to grow and was identified as a factor that would help them in future individual health appointments. In addition, engagement in the group and the resultant relationship-building opportunities enabled those participants who had stopped attending individual health appointments with health professionals feeling able to re-engage with individual appointments. In other words, they had gained a greater sense of relatedness and trust in their relationship with their health professionals.
Our findings suggest that the current focus on individual appointments in chronic disease management negates the importance of relationship-building for First Nations Australians. And failing to meet the relatedness requirements of First Nations Australians may result in them withdrawing from essential care with likely poor health sequelae. Several factors of the group context that enabled relationship-building were identified, including longer duration of appointments, the informal context, and doing activities with other people from community with similar conditions and health professionals. All these factors are hard to replicate in individual appointments.
Thus, regular group programmes provide one solution to enable those with chronic health conditions to form, and maintain, culturally appropriate and meaningful therapeutic relationships. We acknowledge the logistics of implementing repeated group programmes for First Nations peoples with chronic disease, particularly in rural and regional areas of Australia, where low staffing, high health professional staff turnover, and long waiting lists can result in a greater focus on individual monitoring appointments rather than group programmes (Haynes et al., 2021; Panaretto et al., 2010). But we also recognise the slow progress in closing the health gap between First Nations Australians and those of western descent, and the high percentage of First Nations Australians living with chronic disease, including diabetes, particularly in rural and regional areas (Australian Institute of Health & Welfare, 2022).
Closing the diabetes gap will need a variety of activities to increase preventive and curative efforts and, in particular, to strengthen First Nation people’s healthcare if the plethora of health issues that First Nation Australians face are to be addressed. This is in line with the more comprehensive First Nation peoples view of health, which recognises that enhancing First Nation people’s health entails enhancing each person’s physical well-being within the context of enhancing the social, emotional, and cultural well-being of the entire community (National Aboriginal Community Controlled Health Organisations, n.d.).
Governments and communities around the world prioritise obtaining evidence to inform ways to enhance First Nation people’s health outcomes. Evidence currently available in Australia indicates that initiatives to enhance the health of First Nation people must consider the root causes of poor health. This includes conceptualising health as biopsychosocial, spiritual, and cultural well-being, as well as being culturally safe, driven by the community, working in conjunction with the community, and giving back to it (Murrup-Stewart et al., 2019; Walker et al., 2021). The success of the programme was due to the way in which the programme used an accidental hybrid approach that enabled inclusion of diabetes management at home. Understanding what prevents or encourages programme participation over time is crucial for ensuring the sustained self-management of chronic disease for First Nations Australians (Paramenter et al., 2020). The results from our study indicated that the participants felt safe both within the ACCHO environment and the sharing of their individual environments via online platforms, including their relationship to Country and family. Our First Nations’ relationship to Country represents one of the main differences to maintain cultural well-being. Country in this context refers to all living things, serves as a place of belonging, and represents a way of thinking (Aboriginal Art and Culture, 2019).
The perception that an individual’s health is shaped by and derived from communal well-being is especially important given the deliberate government policies over decades to break community bonds through removal from Country and breaking up of clans (Terare & Rawsthorne, 2020). The adverse effect of these practices is acknowledged by the Australian Government which “recognises that dispossession, interruption of culture and intergenerational trauma have significantly impacted on the health and well-being of First Nations Australians and that they share a continuing legacy of resilience, strength and determination” (Department of Health and Ageing, 2013). The health inequality gap must be closed by offering services within the ACCHO to ensure that participants feel connected and that the local dynamics are understood, and local ownership encouraged.
The research found that the accidental hybrid programme supported health and well-being activities in two places: the ACCHO and home. Thus, the accidental hybrid programme suggests a possible new framework for behaviour change programmes for First Nations clients with diabetes. An intentional hybrid framework could commence group programmes within the supportive group context at the ACCHO and then once the group had connected, built relationships with health professionals and gained confidence in knowing and doing new health behaviours; home-based activities could be introduced, supported via telehealth. This framework would allow participants to continue with programme activities within their family and home context while still gaining and giving support to each other in the group.
A barrier is that the length of the programme, 10 weeks, was probably too short to facilitate long-term behaviour change, which was an aspect that both participants and facilitators acknowledged. One alternative to longer programmes would be to explore introducing regular booster sessions into the programme design. Booster sessions have been found, albeit in a different context, to re-engage those whose healthy routines have lapsed (Gearing et al., 2013). The impact of providing booster sessions at regular intervals might also meet the need, identified previously, for maintaining relatedness and connection in relationships with treating health professionals but would require further investigation.
This study found that participants passed on their new understanding about healthy diet to their family, for example, teaching their children about the glycaemic index of foods. Children were observed joining in both online cooking sessions and physical activity sessions, and participants reported that this resulted in new cross-generational physical activity routines. The importance of engaging family units to impact an individual’s health has been observed in previous studies in Canada, where family-based collaboration models were found to positively influence diet and physical activity levels (Anand et al., 2007). However, the Anand et al. (2007) study used regular home visits by Aboriginal health counsellors, not telehealth, to engage their families. The finding that family join in programmes when run via telehealth suggests that such programmes have the potential to impact cross-generational health outcomes.
In addition, the relationship benefits of engaging in cross-generational physical activity identified in the current study concur with findings from another qualitative study which explored the experience of regional primary-school-aged children in Australia and their parents of doing physical activity together (Freire et al., 2019). The power of physical activity to elicit bonding and connecting experiences between physical activity partners is rarely mentioned in promoting physical activity, which tends to focus on meeting minimum physical activity requirements, and physical and psychological benefits. However, given the importance of relationships and connectedness for First Nations peoples, focusing on cross-generational physical activity experiences may be mutually reinforcing for families. The unintentional cross-generational positive outcomes from the programme raise the enticing prospect of possible wide-ranging health and well-being cross-generational benefits.
Limitations of the study
This study has privileged programme participants’ voices over facilitator voices because their experiences are limited in the literature. It is acknowledged that different participants are likely to produce differently nuanced results. This study has only presented qualitative data from the programme evaluation because the quantitative data collection was very incomplete due to lockdown restrictions during the COVID-19 lockdown. Thus, the impact of the programme on participants’ physiological measures, such as their glycated haemoglobin, HbA1c, levels are not reported alongside the qualitative findings. All participants resided in a single, regional location of Australia; it is acknowledged that this, the small sample size, and the qualitative nature of the approach limit the generalisability of the results.
Conclusion
This study found that pivoting to online during the COVID-19 lockdown in Australia gave unique insights into the advantages of hybrid contexts for health promotion with First Nations communities. Although drawn from a small sample of participants, the lessons learned indicate an intentional hybrid model might help participants living with diabetes to establish and maintain relationships with healthcare providers, other community members living with diabetes, and their families. Our findings illustrate that for First Nation Australians to successfully manage their chronic illness, it is essential to understand what promotes programme participation.
Footnotes
Acknowledgements
We acknowledge Ms Rebecca Willis (Wonnarua) for valuable assistance as liaison with community at the ACCHO, including assistance in conducting the interviews and initial qualitative analysis of participants’ interviews; all the participants who kindly took part in the study; Ms Holly Hoad (Wiradjuri), Project Coordinator for Indigenous STEM and Entrepreneur Pathways Project, Charles Sturt University, who created the infographic in ![]() ; and Dr Mark Lock (Ngiyampaa) for critically reading the manuscript.
; and Dr Mark Lock (Ngiyampaa) for critically reading the manuscript.
Authors’ note
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and publication of this article: Three Rivers Department of Rural Health, Charles Sturt University is funded under the Rural Health Multidisciplinary Training Program, Australian Government
Glossary
Bunjalung a First Nations people from northern New South Wales, Australia
Wiradjuri a large tribe of First Nations people located in central western New South Wales, Australia.
