Abstract
Objectives
The application of Ophytrium and chlorhexidine (DOUXO S3 PYO Shampoo and Pads; Ceva Santé Animale) in cats for managing cutaneous microbial imbalances was analysed.
Methods
Client-owned cats with microbiota imbalance characterised by Malassezia pachydermatis overgrowth, bacterial overgrowth or both were recruited. The cats were either washed with shampoo, when possible, considering the localisation of the affected zones and the cooperation of the cat, or treated with topical pads on day 0 (D0), and then received daily pad applications for either 2 weeks (D14) or 3 weeks (D21). Microorganisms were assessed on D0, D7, D14 and D21 using quantitative cytological counts, and pruritus was graded by the owner using a pruritus visual analogue scale for cats (VAScat). Satisfaction questionnaires were collected from both the veterinarians and owners on D14 and D21 (end of follow-up [EOF]).
Results
Among the 10 cats that completed the study, cytological resolution, defined as a mean number of bacteria per oil immersion field (OIF) ⩽2 and/or a mean number of yeasts per OIF ⩽1, occurred on D7 and at EOF in 60% and 90% of animals, respectively. Median yeast count per OIF decreased significantly from D0 (6.7) to EOF (0.0). Similarly, the median bacterial count decreased significantly from D0 (18.0) to EOF (0.0). Median highest values assigned using the VAScat decreased significantly from D0 (4.3) to EOF (1.4). Overall, the veterinarians assessed the cytological and clinical improvement as satisfactory, good or excellent in nine cases. The protocol was considered efficient and practical by nine (90%) owners and the pads were considered easy to use by all 10 (100%) owners.
Conclusions and relevance
Pads and an optional shampoo containing Ophytrium and chlorhexidine were well tolerated. These products were effective in achieving cytological resolution and improving clinical signs and discomfort in cats with microbiota disturbances, yielding high satisfaction levels in veterinarians and owners.
Introduction
Significant advancements in feline microbiota research have led to a deeper understanding of the causes and mechanisms of superficial microbial imbalances in cats.1 –4 A retrospective study showed that the incidence of microbial imbalance is lower in cats than in dogs, 5 supported by the fact that there is evidence of reduced adherence of Staphylococcus species to feline corneocytes. 6 Moreover, cats have a more acidic skin pH than dogs, 7 a greater presence of antimicrobial cutaneous peptides and unique grooming habits8,9 that also would help to maintain their skin free from parasites and infections. However, none of these mechanisms is perfect, and disturbances in the feline skin surface microbiota can still occur, leading to discomfort, pruritus and reduced quality of life. 10
Microbial overgrowth is often associated with Staphylococcus pseudintermedius, the most common bacterium found on the feline skin, and Malassezia pachydermatis, the most prevalent yeast. Other coccoid bacteria and rods may be present, particularly under chronic conditions.5,11,12
Recent guidelines have highlighted the importance of prioritising topical therapy as the first-line treatment before considering systemic antimicrobials.13,14 Although effective, antibiotics may not always be necessary, particularly when only small areas are affected or in mild-to-moderate situations. Nonetheless, they are still frequently used as the first-line treatment for managing superficial microbial imbalances. Managing feline patients presents inherent challenges regarding safety concerns, as any applied product is likely to be licked and ingested. Few studies have been conducted on the efficacy and tolerance of topical products in cats,15 –17 except for antiparasitic purposes. 18
Topical formulations are particularly useful for managing microbial overgrowth because they deliver active ingredients directly to the skin where pathogens reside. Among a wide variety of possible antimicrobial agents, the antiseptic chlorhexidine has strong evidence of efficacy,19,20 although only anecdotal reports have evaluated it in cats. 21 Its tolerance and performance in a combined formulation with Ophytrium have been previously assessed in dogs. 22
Ophytrium is a specific purified natural extract of Ophiopogon japonicus, an ornamental plant known as ‘mondo grass’. In vitro models indicate that it acts on the mechanical, microbiological and immunological skin barriers. It increases tight junctions, filaggrin, natural moisturising factor content and ceramides, while diminishing transepidermal water loss in human skin models. 23 It also limited the adhesion and biofilm formation of Staphylococcus aureus and S pseudintermedius, and decreased the secretion of proinflammatory cytokines (thymic stromal lymphopoietin, interleukin [IL]-8 and IL-13) from cultured lymphocytes. 23
The aim of the present multicentre field study was to assess the performance of a protocol combining a commercial shampoo (DOUXO S3 PYO Shampoo; Ceva Santé Animale) and pads (DOUXO S3 PYO Pads; Ceva Santé Animale) containing Ophytrium and chlorhexidine digluconate 3% for managing cats with local bacterial and/or M pachydermatis overgrowth.
Materials and methods
Veterinarians with expertise in feline dermatology in France and Italy conducted this prospective, multicentre, non-controlled study.
Cat population
Client-owned cats of any breed, age, sex, intact or neutered, and exhibiting one to six patches of local skin dysbiosis (each patch not exceeding 10 cm in diameter), regardless of the primary cause, were eligible for recruitment. Dysbiosis, diagnosed by means of showing ⩾1 Malassezia organisms per oil immersion field (OIF) and ⩾2 bacteria per OIF, 24 was confirmed via cytological examination and rapid staining (RAL 555 modified Giemsa stain; Centravet).
The exclusion criteria included lactation, pregnancy, cats with more than six affected areas, generalised bacterial and/or M pachydermatis overgrowth, other fungal infections, deep pyoderma, ectoparasitic diseases and known hypersensitivity to chlorhexidine.
Ectoparasite control was performed at the first visit to ensure that the most recent antiflea treatment was still active and compatible with the shampoo application if necessary. This verification was made by the veterinarian. The washout periods for the previously administered treatments are listed in Table 1.
Washout periods before inclusion

Written informed consent was obtained from the owners or legal custodians of all cats before inclusion.
Study schedule and application protocol
All cats were client-owned and lived with their owners before, during and after the study period. Feeding and housing conditions were maintained as constant as possible during the study period. Topical or oral parasiticides were allowed if their efficacy period had ended within the study’s time frame. At the end of the study, the cats remained with their owners and were managed by their owners and veterinarians.
On day 0 (D0), complete clinical and dermatological examinations were conducted. Veterinarians performed hair combing, tape impressions and skin scraping examinations, when necessary, to confirm the absence of ectoparasites. Skin lesions were mapped and photographs of the cats were captured. After the cytological evaluation of the most severe spot, the veterinarian cleaned the cat with DOUXO S3 PYO Shampoo during the consultation. If a cat was too stressed or the spot was not suitable for shampooing, the veterinarian applied the pads (DOUXO S3 PYO Pads) instead of the shampoo. A box of pads and instructions regarding their daily application at home were provided to the owners (Figure 1). In the case of multiple affected areas, applications started from the most severely affected area, previously visually selected by the veterinarian at D0. A different pad was gently applied for 10 s to each lesion, enough to cover it with the product. At home, the owner recorded in a booklet the days and area(s) of application of the pads. The booklets were checked by a veterinarian at each visit and returned at the end of the study to detect potential deviations from the study protocol.
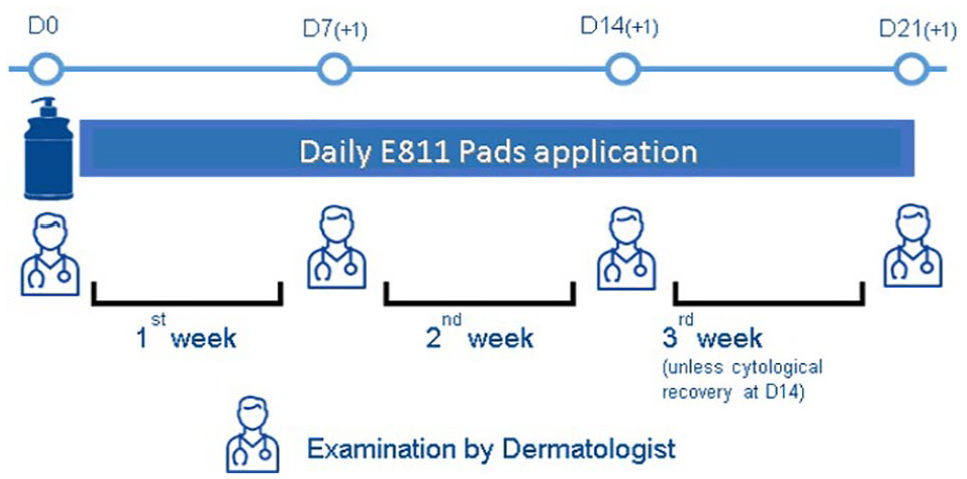
Study protocol
Mandatory visits were scheduled on D7 and D14. On D14, the study was ended if cytological resolution (CR), defined as cytological counts of ⩽2 per OIF for bacteria and/or ⩽1 per OIF for M pachydermatis organisms, was reached. In contrast, if bacterial and/or M pachydermatis overgrowth persisted, the daily application of pads was continued for an additional week and a supplementary (and final) visit was scheduled on D21, when the veterinarian confirmed whether the cat required additional products to manage the initial skin condition, either by continuing the application of the tested pads or by being prescribed a complementary product. Therefore, the end of follow-up (EOF) visit could be at either D14 or D21.
Evaluated parameters
During each visit, the main parameters evaluated (Table 2) were cytological counts performed by the veterinarian and pruritus assessed by the owner (using a pruritus visual analog scale for cats [VAScat]) 25 in terms of frequency of scratching during the consultations.
Evaluated parameters

If cytological resolution not reached on D14
D = day; EOF = end of follow-up; VAScat = pruritus visual analogue scale for cats
Bacteria and/or M pachydermatis counts
The veterinarians determined the most affected patch at D0 based on its visual appearance. The samples were collected by firmly pressing a glass slide on to the patch to allow material to adhere to it. The slides were then air-dried and stained using a quick in-house three-step stain (RAL 555 modified May-Grünwald Giemsa stain; Centravet). Slides were dipped in each solution five to eight times, allowing the excess to drain, gently rinsing the slide with clean water and touching the end of the slide on a paper towel to absorb the excess. The slides were then microscopically examined under magnifications of × 100 and × 400, with a semi-quantitative count as a quick method to grade severity, 26 and a quantitative count of M pachydermatis and/or cocci was made at × 1000 (oil immersion) per mean of six OIFs. Figure S1 in the supplementary material shows the specifications of the procedure.
Each case was classified as a success (CR) or failure based on the yeast and/or bacterial count at the EOF. CR was defined as achieving a mean of ⩽1 M pachydermatis and/or ⩽2 bacteria per OIF. 24
VAScat for licking/scratching assessed by the owner
The owner assessed pruritus using the VAScat. 25 The highest value out of the VAScat licking and scratching scores was defined as the VASmax.
Pruritus assessed by the veterinarian
As the VAScat score can be influenced by owners’ feelings (eg, dissatisfaction and impatience), and it has been shown in dogs that repeatability of scoring is not perfect, 27 pruritus was also assessed by the veterinarian at each visit to provide additional information from objective clinical observations of the frequency of scratching. Grading was as follows: 0 = null; 1 = infrequent; 2 = frequent; and 3 = almost continuous.
Final satisfaction questionnaires
At the EOF, owners and veterinarians were asked a specific set of questions regarding their satisfaction with the products and protocols tested. The protocol efficacy was rated on a scale of 0 (no efficacy), 1 (mild), 2 (satisfactory), 3 (good), 4 (very good) and 5 (excellent). For cats with D21 as the EOF, the veterinarian also had to state whether the cat required additional management (see Table S3 in the supplementary material).
Adverse events and withdrawal from the study
Adverse events and reasons for withdrawal during the study were recorded.
Statistical analysis
The statistical unit for the analysis was the cat. Summary statistics are provided on a per-protocol (PP) basis. SAS 9.4 software was used for all the analyses. Qualitative parameters are presented as numbers and percentages. For quantitative parameters, the mean, median, quartiles (Q1–Q3) and SEM are presented, with 95% confidence intervals when necessary. Missing data were not replaced and were grouped into a category labelled ‘Missing’.
For cytological counts and quantitative pruritus parameters, as data were not normally distributed, Wilcoxon paired tests on absolute changes at D7 and EOF were performed to analyse their evolution from D0. All other parameters are presented descriptively. At the EOF, the responses to questionnaires filled out by veterinarians and owners were analysed.
Results
Cat population
A total of 12 cats were recruited from five investigational centres (four in France and one in Italy); two cats were withdrawn because of major deviations from the protocol and were excluded from the analysis. Thus, the PP population comprised 10 cats. Demographic characteristics are summarised in Table 3.
Demographic characteristics
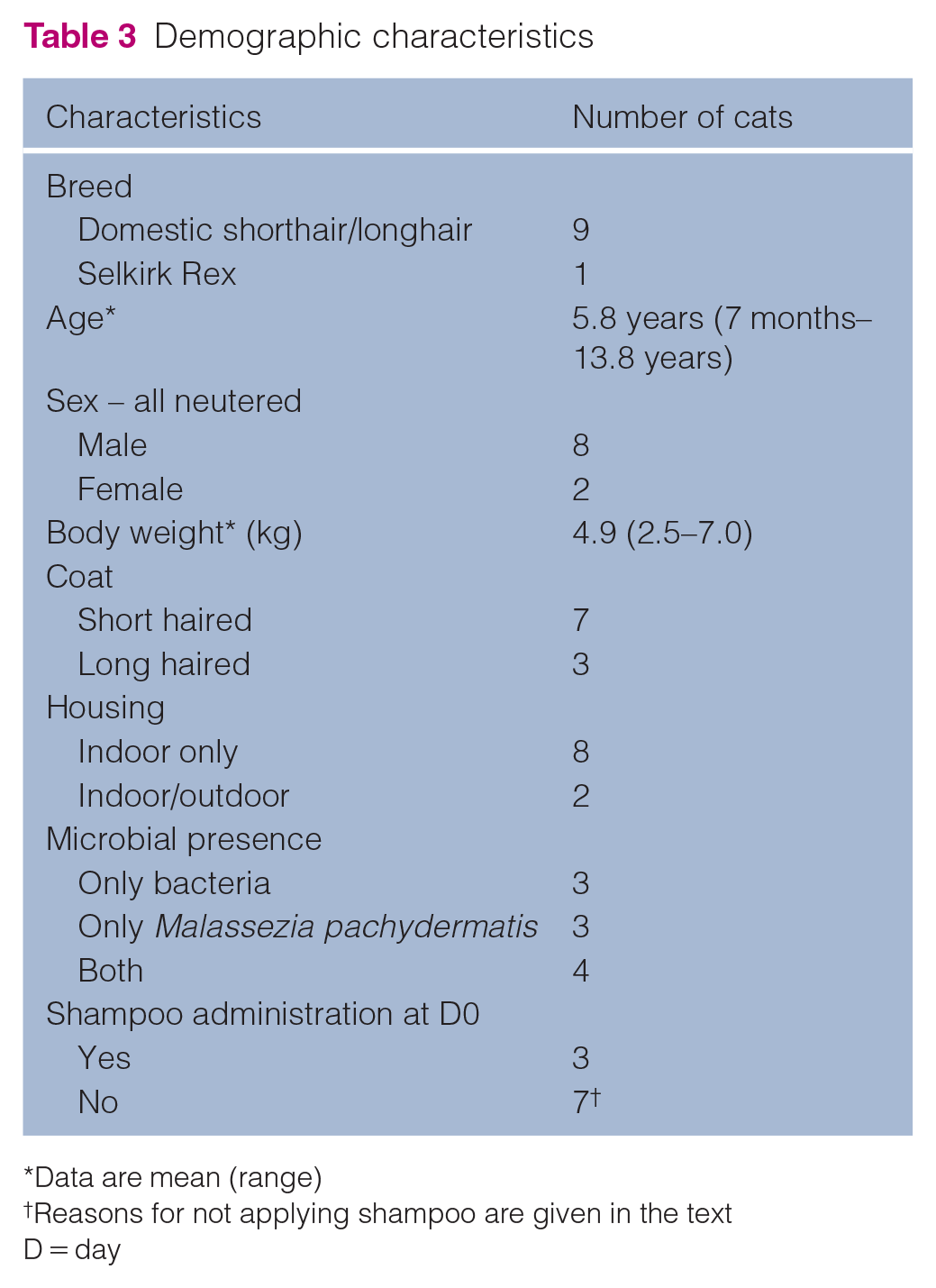
Data are mean (range)
Reasons for not applying shampoo are given in the text
D = day
Based on a clinical examination, all cats were in good overall condition.
The most affected areas were the upper third of the body, including the interscapular, muzzle, chin, ventral neck, post-auricular and periocular areas. This distribution mainly corresponded to the pattern of head and neck pruritus, and the lesions corresponded to excoriations. Eosinophilic plaques and self-induced alopecia were observed on the abdomen. Only one animal showed dermatological signs on its limbs, corresponding to a linear eosinophilic granuloma pattern.
M pachydermatis and bacterial counts
On D7, 6/10 (60.0%) cats reached CR, whereas 9/10 (90.0%) cats reached CR at EOF.
M pachydermatis
Seven cats with M pachydermatis overgrowth on D0 were included in the analysis. The median (Q1–Q3) value on D0 was 6.7 (1.5–8.5) yeast organisms per cat. Mean counts of M pachydermatis decreased significantly at D7 and EOF compared with those at D0; there was a median absolute change of −4.2 points (−7.2 to −1.5) at D7 and −6.2 points (−8.5 to −1.5) at EOF (P <0.05 for both visits). At the EOF, all cats showed a decrease in the mean number of M pachydermatis per OIF >90% compared with that on D0.
Bacteria
Seven cats with evidence of bacterial overgrowth on D0 were analysed. Only cocci were identified. The median number of bacteria per OIF at D0 was 18 (7.0–50.0). The mean number of bacteria per OIF decreased significantly at D7 and EOF compared with that at D0; there was a median absolute change of −16.7 points (–44.7 to −7.0) at D7 and −18.0 points (–45.0 to −7.0) at EOF (P <0.05 for both visits). At the EOF, 5/7 cats showed a decrease in mean number of bacteria by more than 70% compared with D0.
The mean M pachydermatis and bacterial counts on D0 are summarised in Table 4. The evolution of M pachydermatis and bacterial counts over time (D7 and EOF) is shown in Figure 2. More details can be found in Table S1 in the supplementary material.

Evolution of microbial counts at D7 and EOF compared with that at D0. *P <0.05. D = day; EOF = end of follow-up; OIF = oil immersion field
Results for Malassezia pachydermatis and bacterial count at D0 and end of follow-up
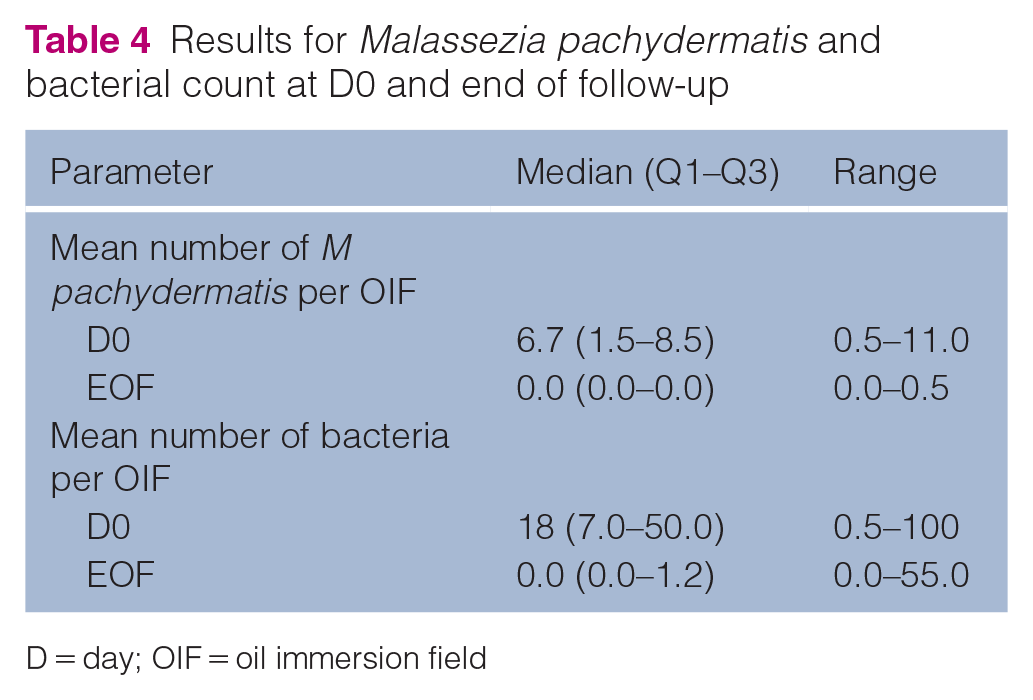

D = day; OIF = oil immersion field
VAScat
The VASmax scores of the 10 cats were analysed. The VASmax score was moderate on D0 (median 4.3, Q1–Q3 3.4–6.0). The test protocol significantly decreased licking and scratching behaviour (P <0.05), with a median absolute change of −1.1 points (–2.0 to −0.5) on D7 and −2.3 points (–4.0 to −1.1) at EOF, corresponding to an average decrease of 41.8% from the baseline (Figure 3).
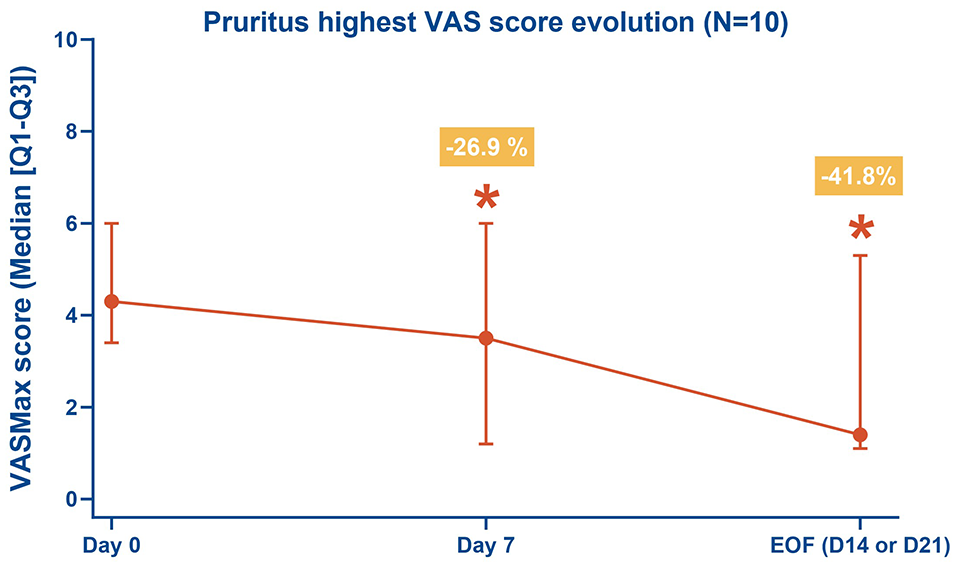
Decrease in maximum value of the VAScat, either scratching or licking, compared to that on D0. The median VASmax on D7 and EOF decreased by 26.9% and 41.8%, respectively, compared to the that on D0. *P <0.05. D = day; EOF = end of follow-up; VAScat = pruritus visual analogue scale for cats; VASmax = highest score recorded per cat on the VAScat
Evolution of pruritus as assessed by the veterinarian during visits
In addition to the improvement in pruritus reported by the owners, veterinarians also observed a decrease in pruritus in terms of frequency during the consultation time at visits (see Figure S2 in the supplementary material). On D0, pruritus was frequent in 5 (50%) cats but persisted in only 2 (20%) cats by the EOF.
Owners’ satisfaction
All the owners completed a questionnaire on global satisfaction at the EOF (Figure 4). Overall, 9/10 (90%) owners considered that the test protocol was effective, and all (n = 10, 100%) considered the pads practical and easy to use. They also appreciated the size, thickness and amount of cotton pad impregnation. Eight owners (80%) were satisfied with the cat’s hair or skin after product application. For other details see Table S2 in the supplementary material.

Owners’ overall appreciation of product characteristics, ease of use and efficiency
Tolerance and safety
No serious adverse events were observed. Veterinarians and owners assessed the local tolerance of the shampoos and pads applied to cats.
Some events occurred during the study, although none of them affected the results. One cat, which should not have been included because of recurrent severe pyoderma, was removed after the D7 visit and was excluded from the PP population. Another cat, whose clinical status deteriorated during the study period, underwent surgery to remove the lesion after the D14 visit. One cat presented with a new location of severe excoriation in the interscapular area between D14 and D21. The protocol was not modified, and this new spot was left untreated, not entering the final data. Finally, one cat had a self-limiting ocular reaction after an out-of-recommendations periocular application of the impregnated pad.
Discussion
The skin is inherently infection resistant owing to its robust mechanical, immunological and microbiological barriers. 7 However, these may still be susceptible to changes that allow overgrowth of pathogenic fungi, bacteria and resident microbiota. These overgrowths appear to be more prevalent in cats than has traditionally been reported.5,12 When natural host defence mechanisms are overcome, notably due to an underlying disease, dermatological manifestations or pruritus may occur, significantly affecting a cat’s quality of life. 10 Various conditions, including allergic dermatoses, keratinisation disorders and parasitic diseases, can lead to such overgrowths. These factors must be carefully considered and managed to ensure positive outcomes.
This study focused on the efficacy of topical treatments on microbial imbalance and pruritus rather than on the possible underlying causes. Having ruled out at D0 the presence of parasites and deep fungal infection, further investigations regarding the underlying causes were left to the professional judgement of the veterinarians. 28
The length of the study was estimated at 3 weeks to allow the animals sufficient time to achieve cytological resolution, although more than half had already recovered by D7. This result can be considered positive as it is comparable to the results obtained by administering systemic antimicrobial treatments, such as amoxicillin/clavulanic acid for bacterial dermatitis and itraconazole for Malassezia species dermatitis in dogs and cats. 29 These results suggest that topical management can control imbalances in the same time frame as systemic treatments. Topical management could therefore be recommended for mild generalised conditions, as skin microbial overgrowths are often secondary to underlying diseases. 30
In this study, the VASmax values for pruritus were significantly reduced at the end of the trial. Ophytrium decreases anti-inflammatory cytokine production in vitro. 30 In a recent study, a protocol combining a shampoo and mousse containing Ophytrium significantly decreased pruritus in cats. 31 In the present study, the rapid and significant reduction in pruritus could be related to the antiseptic properties of chlorhexidine, the mechanical effect of the application of shampoo and/or pads, and the soothing properties of Ophytrium. The use of impregnated pads in humans also offers the benefit of the mechanical removal of microorganisms and debris, 32 and previous in vivo studies have shown similar results in dogs. 22 Chlorhexidine is a widely used antiseptic agent known for its broad-spectrum activity against bacteria, fungi and viruses. In vitro studies have highlighted its efficacy against S pseudintermedius and S aureus. 33 In addition, in vivo studies have reported the importance of a 3% chlorhexidine shampoo as a valuable therapeutic option for combating yeast microbiota imbalances.14,19,34
This prospective field study has some limitations. First, being an open study, each animal was its own control, and statistical parameters were defined based on individual baselines. Ideally, a control group should have been included for comparison of results. Nevertheless, other studies in dogs under similar conditions have demonstrated minimal spontaneous improvement in placebo groups.34–36 Second, a larger sample size might have enhanced the precision and significance of the results. Finally, we are aware that the complete protocol, with all cats receiving one shampoo treatment at D0 followed by subsequent daily pad applications, would have yielded statistically more relevant results. However, in clinical practice, bathing cats remains rare. We should have considered a ‘pads only’ protocol. Still, we appreciate the positive overall results and consider that they may encourage clinicians to consider topical therapy when managing mild and localised microbial overgrowths in cats. Considering the reluctance of many cats to have topical products applied, compliance with the protocol was excellent and the owners reported it as an easy management method. Repeated application did not result in perceived skin dehydration. The owners did not notice any signs of rejection of the product by the cats due to its smell. All owners found the product’s fragrance pleasant and their cat’s skin and fur nice and smooth after application according to the directions.
Conclusions
Given the growing concern regarding antibiotic resistance, finding alternatives to systemic antimicrobials is crucial for the management of skin conditions. The protocol of application of Ophytrium- and chlorhexidine-containing pads with or without shampoo quickly and significantly reduced cocci and M pachydermatis populations in cats with superficial localised cutaneous microbiota imbalances. It also significantly reduced clinical manifestations, including pruritus, leading to high satisfaction among veterinarians and pet owners. However, further studies are needed to provide more scientific evidence on the efficacy and suitability of topical management of feline skin conditions.
Supplemental Material
Figure S1
Microbial counting procedure.
Supplemental Material
Figure S2
Bar plot showing the distribution of the frequency (A) of pruritus observed by the veterinarian over time (n = 10).
Supplemental Material
Table S1
Data for Malassezia and bacterial count.
Supplemental Material
Table S2
Owners’ final questionnaire.
Supplemental Material
Table S3
Veterinarians’ final questionnaire.
Footnotes
Acknowledgements
The authors acknowledge the cooperation of the caregivers who participated in this study. The authors would also like to thank Khnata Lamchemmach and her team for organising the product logistics and transport. The authors would like to thank Charly Matard (data manager) Alexandra Beck, Roxane Kesteman, Léa Lacourty, Charlotte Valade (clinical research associate) and Vanessa Cazeaux (clinical studies assistant) for their valuable contributions to this study.
Author note
This paper was presented as an abstract at the 2023 North American Veterinary Dermatology Forum Conference. Other raw data supporting the conclusions of this study will be available upon request from the corresponding authors.
Supplementary material
The following files are available as supplementary material:
Figure S1. Microbial counting procedure.
Figure S2. Bar plot showing the distribution of the frequency (A) of pruritus observed by the veterinarian over time (n = 10).
Table S1. Data for Malassezia and bacterial count.
Table S2. Owners’ final questionnaire.
Table S3. Veterinarians’ final questionnaire.
Conflict of interest
AC, MG, CB and XDJ are employees of Ceva Santé Animale in Libourne, France. The remaining authors received financial support from Ceva Santé Animale for the research, authorship, and publication of this article.
Funding
This work was supported by Ceva Santé Animale, Libourne, France.
Ethical approval
The work described in this manuscript involved the use of non-experimental (owned or unowned) animals. Established internationally recognized high standards (‘best practice’) of veterinary clinical care for the individual patient were always followed and/or this work involved the use of cadavers. Ethical approval from a committee was therefore not specifically required for publication in JFMS. Although not required, where ethical approval was still obtained, it is stated in the manuscript.
Informed consent
Informed consent (verbal or written) was obtained from the owner or legal custodian of all animal(s) described in this work (experimental or non-experimental animals, including cadavers, tissues and samples) for all procedure(s) undertaken (prospective or retrospective studies). No animals or people are identifiable within this publication, and therefore additional informed consent for publication was not required.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
