Abstract
Objectives
The aim of this study was to investigate a potential association between the COVID-19 pandemic stay-at-home orders and the prevalence of emergency room presentations for urethral obstruction (UO) in feline patients.
Methods
Medical records and hospital census were retrospectively searched to identify the total number of cats and total number of male cats with UO presenting to two academic veterinary medical centers from 22 March to 10 August in the years 2018 (123), 2019 (137) and 2020 (175). Cats were grouped based on the year of presentation and the proportions of UO cases relative to all cats presenting to the emergency rooms during the same time frame. Absolute (year of interest – reference year) and relative ([year of interest – reference year]/[reference year]) change in prevalence was determined. These were compared for each year using a two-sample z-test.
Results
The absolute and relative prevalence of UO presentations across the combined population increased significantly during the COVID-19 pandemic in comparison with 2018 (2.2% and 59%, respectively; P = 0.0003) and 2019 (1.9% and 48%, respectively; P = 0.0021). For the individual institutions, a significant increase in UO presentations was found for institution A when comparing 2020 with both 2018 (P = 0.0072) and 2019 (P = 0.0073), but not for institution B (P = 0.057 and P = 0.18, respectively). No significant differences were found when 2018 and 2019 were compared across the combined population or within institutions.
Conclusions and relevance
The results of this study demonstrate an increased prevalence of UO during the initial months of the COVID-19 pandemic, which may be related to environmental change and stress imposed by stay-at-home orders.
Keywords
Introduction
Urethral obstruction (UO) is a potentially life-threatening disease process that can result in a postrenal azotemia, severe electrolyte and metabolic derangements, and – potentially – permanent kidney damage.1–3 The most common conditions resulting in UO are idiopathic (no apparent cause identified), urolithiasis or the presence of a urethral plug.1–4 For patients with idiopathic obstruction, there may be an association with underlying feline idiopathic cystitis (FIC).1–9 Cats with FIC are suspected of having an imbalance in their sympathetic and hypothalamic–pituitary–adrenal system, making them more susceptible to adverse effects associated with increased stress and anxiety, particularly in the lower urinary tract.1,6,9,10 More specifically, they have an increased number of norepinephrine (noradrenaline) receptors in their bladder, resulting in increased risk of bladder inflammation with the activation of their sympathetic nervous system. 6 Furthermore, cats with FIC have a more sensitive and reactive stress response system and decreased ability to counteract these effects.1,7,8,10 Additional potential risk factors for the development of FIC and UO include an indoor lifestyle, obesity, exclusively dry food diet and spring seasonality.1–4,7,11 Feline UO remains a common cause for presentation to both emergency and primary care veterinary hospitals, accounting for 1–9% of cat presentations to these hospitals.2,12
The COVID-19 global pandemic resulted in government-mandated stay-at-home orders and social distancing. This caused abrupt changes in people’s daily routine and mental health. 13 This increase in time at home would also likely have had an impact of the daily routine of many pets. In the US, the stay-at-home orders for many states started in late March 2020. 14 As it has been recognized that environmental stress plays a role in activating the abnormal neurohormonal system in cats with FIC,6,8 it could be surmised that the stay-at-home orders caused sufficient environmental disruption to increase stress levels, resulting in an increased prevalence of FIC (and, subsequently, UO). However, it is also possible that owners being home more could have had a positive impact on their pets’ stress and environment, thus resulting in a decreased prevalence of FIC and subsequent UO. Recent literature from across the globe has demonstrated an increase in stress behavioral changes in dogs associated with the COVID-19 stay-at-home orders.15–19 To date, there has not been published literature evaluating the potential impact of stay-at-home orders on the stress levels, behavior changes and prevalence of UO in cats.
The specific aim of this study was to identify whether the COVID-19 pandemic and associated stay-at-home orders impacted the prevalence of UO patients presenting to emergency rooms. We hypothesized that there would be a statistically significant increase in the prevalence of UO cases during the initial months of the COVID-19 global pandemic.
Materials and methods
This cohort study was designed as a retrospective investigation. Two collaborating academic institutions, with first-opinion emergency hospitals, searched their respective databases and hospital census to provide information regarding the total number of emergency presentations for cats and the number of cats presenting for UO during the first 20 weeks (~5 months) of the stay-at-home orders related to the COVID-19 global pandemic. Satellite and urgent care facilities were not included. For institution A, the stay-at-home advisory was issued to begin on 24 March 2020 and spanned until 25 May 2020. 14 For institution B, the stay-at-home order was implemented on 23 March 2020 and spanned until 1 May 2020. 14 However, neither state returned to normal business, with many people staying home and working remotely well beyond the mandated orders. 20 The time frame for this study was selected with the notion that the impact would be the greatest at the beginning of stay-at-home and likely a new acclimation would occur. It was also important to span enough time to have sufficient cases and lessen the impact of confounding factors, and so a period of 5 months was chosen. Data from the same dates were obtained from 2019 and 2018, to serve as a control and account for confounding factors, including the impact of seasonality and hospital presentations.
Medical records were searched using the keywords ‘urethral obstruction’, ‘UO’ and ‘feline idiopathic cystitis’. Records were then reviewed to remove any non-feline patients and females, confirm a diagnosis of UO and remove any rechecks not related to an independent obstructive episode. The diagnosis of UO was made based on the presenting clinical picture (physical examination, laboratory abnormalities) and need for urinary catheter placement (either inpatient or outpatient management). Patients that were euthanized without treatment were also included. Patients were excluded if they had UO that was determined to be secondary to cystolithiasis, neoplasia or trauma, or if they were believed to have UO but urinated while in hospital without the need for urinary catheterization. Cats of any breed, age and castration status were included, as well as cats that re-presented for UO during the study period. For patients that had abdominal radiographs performed, the documentation of cystic or urethral calculi as the cause of UO was noted, as well as the reason why radiographs were not performed. As the purpose of this study was solely to assess the prevalence of UO, no other data were extracted from the medical records. A second medical record search was performed for all emergency visit fees (recheck, 24 h returns, referral) and species selection for cats, to provide the total number of cats presenting to the emergency services during the same dates.
Statistical analysis
The prevalence of UO was determined based on the number of cats diagnosed with UO divided by the total number of cats presenting via emergency during that same time period. This was performed within each institution, as well as across the combined populations. Absolute (year of interest – reference year) and relative ([year of interest – reference year]/[reference year]) change in prevalence was also calculated. To determine whether the change in prevalence was significant between the three years assessed, a two-sample, two-tailed z-test was performed comparing 2018 with 2019, 2018 with 2020 and 2019 with 2020 using an online program (Epitools; epitools.ausvet.com.au/ztesttwo). Significance was set at P <0.05. For any insignificant differences in prevalence a post-hoc power analysis was performed to determine the sample size that would have been needed to achieve significance with a power of 80% and confidence level of 95% using Epitools.
Results
The prevalence of UO without documented cystolithiasis, absolute change and relative change at each institution and across the total population are presented in Table 1. There were no significant differences in the prevalence of UO from 2018 to 2019 at either institution, or across the total population (institution A, P = 1.0; institution B, P = 0.56; combined, P = 0.59). The prevalence of UO in 2020 was found to be significantly higher at institution A and across the total population compared with 2018 (institution A, P <0.0072; combined, P = 0.0003) and 2019 (institution A, P = 0.0073; combined, P = 0.0021). While there was a higher prevalence at institution B, the change did not achieve significance compared with 2018 or 2019 (P = 0.057 and P = 0.18; respectively). For this institution, post-hoc power analysis revealed that, to achieve significance, 1746 cats would have needed to present to the emergency room based on the change in prevalence from 2018 to 2020, and 3743 cats based on the change from 2019 to 2020.
Prevalence of urethral obstruction (UO) without cystolithiasis at two separate institutions and combined
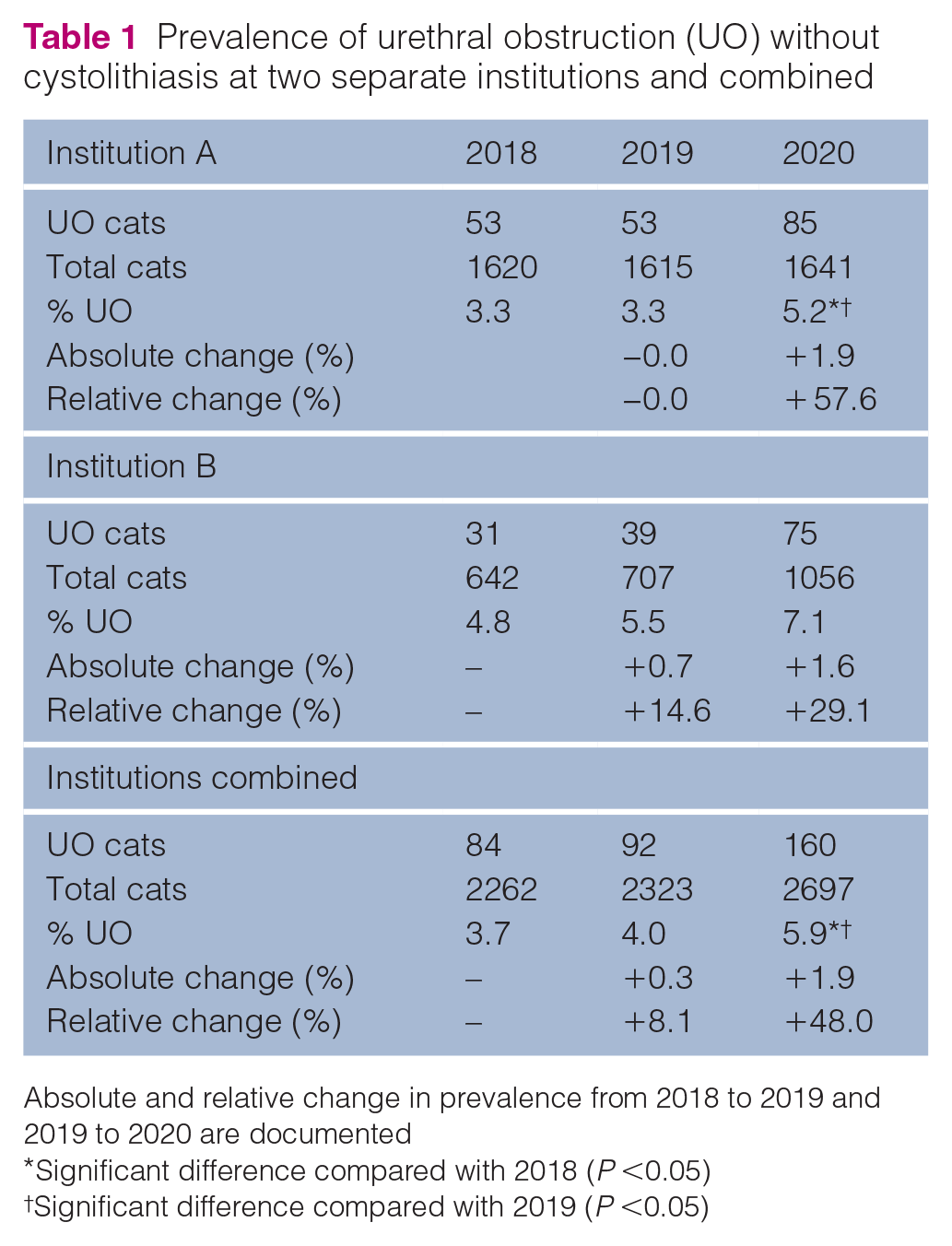
Absolute and relative change in prevalence from 2018 to 2019 and 2019 to 2020 are documented
Significant difference compared with 2018 (P <0.05)
Significant difference compared with 2019 (P <0.05)
Abdominal radiographs were performed in all cats that had a urinary catheter placed with subsequent hospitalization. Radiographs were not obtained in patients that were euthanized without treatment or that were treated on an outpatient basis. From this, the incidence of cystolithiasis was determined among those that had radiographs performed (Table 2).
Frequency of abdominal radiographs, reasons radiographs were not performed and incidence of cystolithiasis as the documented cause of urethral obstruction (UO) in patients that had radiographs performed
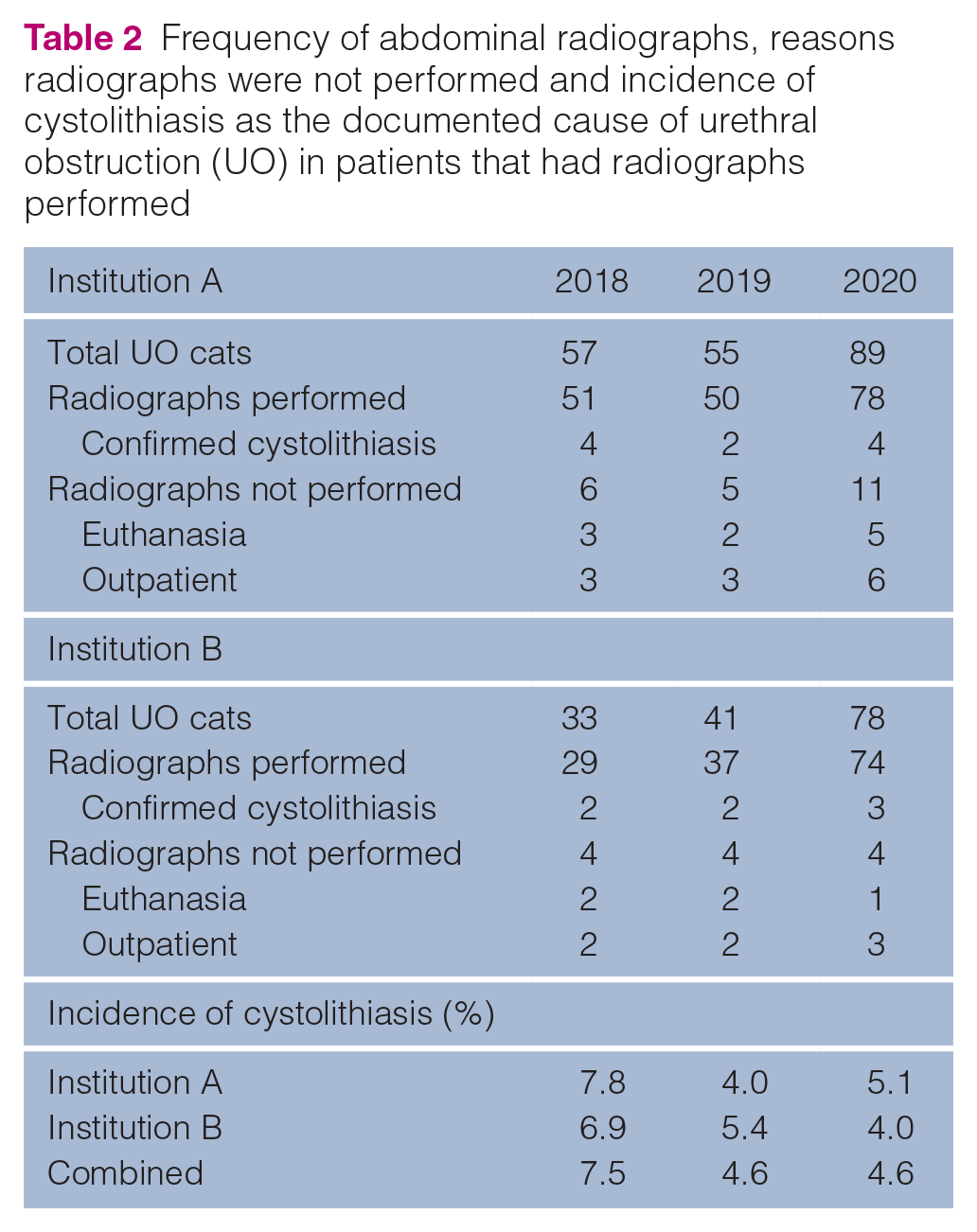
Discussion
The present study evaluated the absolute and relative change in the prevalence of feline UO presenting to two academic emergency rooms during the first 20 weeks of the COVID-19 pandemic vs the previous 2 years. The results indicated a statistically significant increase at one of the institutions, and across the combined populations. This supports our hypothesis that the global pandemic may have increased the risk of UO in cats vs non-pandemic years.
The impact that the stay-at-home orders have had on the mental health and wellbeing of the global human population is an active area of research. There is evidence that humans have suffered increased stress, anxiety and depression as a result of the global pandemic and, more specifically, the stay-at-home orders.21,22 It could be argued that owners being home more with their pets could have a positive effect on their stress level. However, recent reviews have shown a similar increase in behavioral problems associated with stress and anxiety in dogs during the stay-at-home orders.16,18 Cats are known to be sensitive to environmental changes, including changes in frequency or type of interactions with their human caretakers.7,23 With this in mind, it is possible that the COVID-19 pandemic may have resulted in an increase in stress level in cats, and therefore could be related to the increased prevalence of FIC flare ups and, consequently, UO found in this study. It is also possible that more cases presented because owners were at home and able to monitor their pets, and so may have been able to identify clinical signs and thus sought medical care earlier.
This prevalence of presentations for non-obstructive FIC, and potential for increased clinical signs associated with stay-at-home orders, were not evaluated in this study. As the diagnosis of FIC is ultimately one of exclusion, the retrospective nature of this study could have resulted in significant under- or overdiagnosis for patients not having a complete medical work-up performed (eg, urinalysis, urine culture, radiographs and/or lower urinary tract ultrasound). For this reason, the decision was made to not include this subset of data and focus on the more clearly defined population of UO cats. However, this does present a future avenue of exploration.
In this study we elected to exclude UO patients with cystic calculi. Unlike FIC, the presence of calculi does not have a known association with stress or environmental changes, and would be less likely affected by the stay-at-home orders. Further, the overall incidence of urolithiasis was very low in this study population (ranging from 4.6% to 7.5% across the combined institutions) and so these patients were unlikely to have had a significant impact on the findings. Interestingly, this is a much lower incidence of cystolithiasis than previously reported (20–47%).3,24–27 The reason for this difference is not clear, though it is similar to a previous study, which reported that 5.7% of UO cats have cystolithiasis. 28 Several patients that did not have radiographs performed (34/336 total UO cats across the 3 years) were included in the present study, and so it is possible that some of these could have had cystolithiasis. However, given the overall low incidence of cystolithiasis in this study population, it was elected to include those patients in the analysis.
While there were significant increases in both the absolute and relative percentages of UO cats presenting during the pandemic at institution A, and when combining the institutions, there was no statistically significant increase at institution B alone. There was still an absolute and relative increase, but it is suspected that this did not achieve statistical significance because the lower number of patients seen at institution B resulted in a type 2 error. Based on post-hoc power analysis and the detected change in incidence, it would have been necessary to have approximately 1700–4000 cats presenting to institution B’s emergency service each year to reach significance. However, the combined absolute increases comparing both 2018 and 2019 are even more significant than institution A alone (P = 0.0007 vs P=0.0003 and P = 0.0021, respectively), suggesting some contribution from institution B. Other possible explanations for the lack of significant change in institution B may be geographic or policy differences in response to the pandemic resulting in less environmental change for those cats. Additionally, there could be differences in clientele between the two institutions. For example, if more clients from institution B were in healthcare, there may have been little disruption to the daily lives of their cats. Institution B also had a shorter stay-at-home order, which could have influenced the length of time that the cats’ lives were disrupted (6 weeks vs 9 weeks).
The retrospective nature of this study did present some limitations. It was not possible to collect data regarding specific changes to the patients’ environment in relation to the stay-at-home order and pandemic. There was no consideration of other known FIC risk factors, including an indoor living environment, exclusive dry food diet, inadequate litter boxes and multi-cat households, as these could potentially be confounding factors.2,5,8,11 Given the large population included in this study, it can reasonably be expected that these other factors would be consistent from one year to the next. Future studies could involve a specific client questionnaire evaluating changes to the cat’s environment in relation to a pandemic at the time of UO presentation. To more definitively verify if the pandemic and stay-at-home orders resulted in the increase in UO cases, we could have collected data after the pandemic resolved or once the clients’ lives normalized to demonstrate a decrease in UO cases presenting. Unfortunately, this presented a challenge as the COVID-19 pandemic has continued to disrupt the lives of many people. Lastly, during the initial stages of the pandemic many primary care practitioners were closed or overwhelmed, which may have resulted in an increase in patients presenting to emergency services. 29 While the increase in overall caseload would be expected to balance this effect, if there was a disproportionate number of UO cats referred in this regard it could have served to artificially increase the prevalence relative to previous years. This could have been a confounding factor, especially if this had occurred more so for institution A, even though first-opinion emergencies constitute the majority of the emergency caseload for both institutions.
Conclusions
The early months of the COVID-19 pandemic and stay-at-home orders were associated with an increased prevalence of emergency UO presentations compared with a similar time frame in the two previous years. This increase may be related to changes to the home environment and associated stress response experienced during this time, but further investigation is needed. In addition, future studies evaluating a decrease in incidence with the resolution of the pandemic and additional causes of increased incidence in UO are warranted.
Footnotes
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The work described in this manuscript involved the use of non-experimental (owned or unowned) animals. Established internationally recognized high standards (‘best practice’) of veterinary clinical care for the individual patient were always followed and/or this work involved the use of cadavers. Ethical approval from a committee was therefore not specifically required for publication in JFMS. Although not required, where ethical approval was still obtained, it is stated in the manuscript
Informed consent
Informed consent (verbal or written) was obtained from the owner or legal custodian of all animal(s) described in this work (experimental or non-experimental animals, including cadavers) for all procedure(s) undertaken (prospective or retrospective studies). No animals or people are identifiable within this publication, and therefore additional informed consent for publication was not required.
