Abstract
Case series summary
Nasal planum tumors are rare in cats, with squamous cell carcinoma over-represented. Other skin tumors have been reported in this location and though hemangiosarcoma frequently occurs on the skin of the head, these tumors localized to the nasal planum have not been specifically reported. The objectives of this study were to report the clinical findings and outcomes in cats diagnosed with hemangiosarcoma of the nasal planum. Medical records from four different institutions were reviewed to identify cats with a definitive diagnosis of hemangiosarcoma of the nasal planum. Five cats met the inclusion criteria. One cat was treated with palliative radiation therapy (RT) alone, two cats had lesions removed via an excisional biopsy by the primary care veterinarian and two cats had excisional biopsies performed at a referral institution. All four cats that received surgical treatment were treated with adjuvant strontium-90 therapy. The cat receiving palliative RT alone was lost to follow-up 311 days after treatment. At the time of writing, the survival time for 2/3 cats receiving surgery and strontium-90 was 365 days and 1381 days, respectively. One cat receiving this combination of therapy was lost to follow-up immediately after treatment. One cat developed tumor recurrence and a revision surgery via nasal planectomy and upper lip resection was performed 376 days following the initial surgery. Following revision, palliative RT was pursued. The cat was still alive at the time of writing 618 days after the initial procedure, with no evidence of recurrence.
Relevance and novel information
In this case series, surgery was the primary treatment used, but due to the location, only narrow or incomplete surgical margins were possible. RT (strontium-90 and/or palliative) was utilized to decrease the risk of recurrence.
Introduction
Nasal planum tumors are uncommon in cats, with squamous cell carcinoma (SCC) representing the most common feline nasal planum neoplasm. 1 Other reported tumors occurring in this location include fibrosarcoma, melanoma, mast cell tumor (MCT), osteosarcoma and desmoplastic ameloblastoma. 2 This is not unexpected as SCC, fibrosarcoma and MCT are three of the four most common feline skin tumors. 3
Vascular tumors of endothelial origin are generally rare in cats. The malignant variety is more common, accounting for <1.5% to 2% of non-hematopoietic neoplasms.4,5 Feline hemangiosarcoma can be classified into dermal, cutaneous–subcutaneous or visceral varieties. The cutaneous–subcutaneous subset occurs more frequently and with similar aggressive biologic behavior and metastatic potential as the visceral variety.6–9 Cutaneous–subcutaneous lesions in cats occur most commonly on the head; arising mainly from the eyelids, ear tips, nasal planum and non-pigmented skin. 8 Retrospective studies evaluating feline hemangiosarcoma are uncommon in the veterinary literature, with studies often containing low case numbers.5,7–13 Furthermore, only one study evaluating feline cutaneous hemangiosarcoma reported 1/18 cats to have a nasal planum lesion. 13 To our knowledge, no case series exist with a primary focus on hemangiosarcoma of the nasal planum in feline patients or the use of strontium-90 in cases of feline cutaneous hemangiosarcoma. Given the lack of information regarding the outcome of cats with hemangiosarcoma of the nasal planum, the objective of this study was to report the clinical findings and outcomes in cats with a histologic diagnosis of this tumor type.
Case series description
The medical records from four small animal academic referral hospitals (The Ohio State University, University of California-Davis, University of Guelph and University of Florida) were searched for histopathologically confirmed hemangiosarcoma of the nasal planum of cats from 1 January 2010 to 1 September 2021. Cats were excluded from the study if the histopathologic diagnosis was different from hemangiosarcoma, if the site was not the nasal planum or if medical records were incomplete. For all cats, data on signalment, history, physical examination, preoperative imaging, clinicopathologic data, therapy and outcome were collected by medical record reviews.
Data retrieved from the medical records of each cat included age, body weight, breed, sex and neuter status, date of presentation, comorbidities at the time of diagnosis and physical examination findings. Preoperative blood work results were evaluated, and abnormalities were reported. Preoperative thoracic and abdominal imaging, and preoperative cytology or histopathology results of the lesion were also evaluated. Recorded treatments included palliative medical management, surgical biopsy/excisions, radiation therapy (RT) protocols and/or chemotherapy regimens. Intraoperative complications were also recorded. Histopathology reports of primary lesions were reviewed. Immediate postoperative (following recovery from anesthesia to discharge) complications were also evaluated. Longer-term (2 weeks postoperatively) complications, adjuvant treatments pursued, tumor recurrence, and date and cause of death were also reported. Information regarding the follow-up of the cat was obtained from institutional records, referring veterinary records or the cat’s owner.
After review of the medical records from the four institutions, six cats were identified. One case was excluded as the location of hemangiosarcoma was not the nasal planum. The median age at the time of presentation was 11 years (range 3–13). The median body weight of cats in this study was 4.9 kg (range 4.0–6.2). The following breeds were represented: domestic shorthair (n = 3) and domestic mediumhair (n = 2). Four cats were male (all castrated) and one was female (spayed). Clinical signs prompting presentation ranged from the presence of a mass on the nasal planum (n = 4) with intermittent bleeding (n = 3) and sneezing (n = 1); one cat demonstrated no clinical signs. Physical examination findings at the time of presentation to the referral hospitals included a mass on the nasal planum (n = 3; with measurements of 11 mm [case 1], 5 mm [case 4] and 6 × 5 × 2 mm [case 5]), a scar on the nasal planum (n = 2), stertor (n = 1), drooping of the left lower eyelid with mild elevation of the third eyelid (n = 1) and bilateral nuclear sclerosis (n = 1).
Complete blood count (CBC) and serum biochemistry were performed and available for review in four cats. CBC abnormalities included a stress leukogram as evidenced by a mild leukocytosis characterized by neutrophilia, monocytosis and lymphocytosis (n = 1). Serum biochemistry revealed hyperalbuminemia (n = 1), hypercholesterolemia (n = 1) and elevated amylase (n = 1). No abnormalities were detected in two cats. Consistent CBC or biochemistry abnormalities were not recognized.
Three-view thoracic radiography was performed on four cats. There was no evidence of pulmonary metastasis in any cat. Other findings included mild bronchitis, which was suspected to be allergic in origin (n = 1). Abdominal ultrasonography was performed on three cats. There was no evidence of metastatic disease, but other findings included bilateral age-related renal changes (n = 1) and urinary bladder debris (n = 1). Advanced imaging of the primary mass was not performed on any cat. Preoperative cytology of the lesion was performed in one cat (case 2) and findings were consistent with hemorrhage. Preoperative incisional biopsy was performed on two cats (cases 1 and 5). Histopathology results were not available for review for case 1. For case 5, the results were consistent with cutaneous hemangiosarcoma, which was characterized by expansion of the submucosa by an unencapsulated, infiltrative neoplasm composed of plump neoplastic spindle-shaped endothelial cells lining the anastomosing vascular spaces and dermal collagen bundles. The mitotic count was two per ten ×40 fields. Preoperative cytology or biopsy of the regional lymph nodes was not performed for any cat.
Two cats had lesions removed via an excisional biopsy with a punch performed by the primary care veterinarian (cases 2 and 3). The biopsy size was not recorded for case 2, while a 3 mm biopsy punch was used for case 3. Both cats had dental procedures performed concurrently. No intraoperative complications were reported for either case. Samples of the primary lesion were submitted for histopathology in both cases, confirming a diagnosis of cutaneous hemangiosarcoma. The lesions were composed of spindle-to-polygonal cells forming interlacing streams and bundles supported by a thin fibrovascular stroma. The spindle cells often had indistinct borders, moderate eosinophilic fibrillar cytoplasm, oval nuclei of varying size containing stippled chromatin and 1–2 variably distinct nucleoli. Anisocytosis and anisokaryosis were described. The mitotic count was <1 (case 2) and <5 (case 3) in 10 high-power fields. The narrowest lateral resected margin was 1.5 mm for case 2, with neoplastic cells extending from the superficial to deep dermis for case 3.
Following diagnosis, one cat (case 1) was treated palliatively with hypofractionated RT. The protocol consisted of a single weekly treatment for 4 weeks at a dose of 8 Gy per fraction for a total dose of 32 Gy. This was performed as a single field manual set-up using 6 MeV electrons with a 5 cm cone and 0.8 cm tissue-equivalent bolus. At the time of the third treatment, the cat was reportedly bothering the mass more and the mass was described as fluctuant in nature. A fine-needle aspiration of this area was performed, and the findings were consistent with blood. Following sampling, the area immediately became swollen with a blood-filled vesicle-like lesion. At the fourth treatment, ulceration was noted in the radiation field. The ulceration was not present on examination 18 days later. Otherwise, no acute or late complications were reported. The cat was treated concurrently with propranolol (2.5 mg PO q12h) and meloxicam (0.6 mg PO every other day). The mass was still visible after treatment, though final measurements were not obtained. Stable disease was noted at 19 days following completion of RT, though the cat was then lost to follow-up.
Surgery was performed on two cats at the referral academic institution. An excisional biopsy was performed on one cat (case 4), while an excision with 0.5 cm margins around the tumor (deep margin not reported) was performed initially for case 5, followed by revision surgery via nasal planectomy and upper lip resection 376 days later. No cats experienced intraoperative complications.
Samples of the primary lesion were submitted for histopathology in both cases, confirming a diagnosis of hemangiosarcoma for both cats. The lesions were described as an unencapsulated mass composed of bundles and anastomosing streams of densely packed spindle cells forming channels containing red blood cells. The cells often had indistinct cell margins, a small amount of wispy eosinophilic or basophilic cytoplasm, ovoid-to-elongated nuclei, finely granular chromatin and a single small basophilic nucleolus. Anisokaryosis was frequently reported. Lymphocytes were also noted often throughout the mass. Immunohistochemistry for CD31 was performed for case 4, which demonstrated variable immunoreactivity, especially in regions with abundant channels, most suggestive of hemangiosarcoma. The mitotic count was two per ten ×400 fields for case 4, and four per ten ×400 fields for case 5. Histopathology submitted following revisional surgery for case 5 revealed a mitotic count of eight per ten ×400 fields. Margins were incomplete following both the initial surgery and revisional surgery for case 5, and were not reported for case 4.
Both cats were discharged 24 h postoperatively with no reported postoperative complications. There were also no concerns prior to the 2-week recheck, with all incisions reportedly healing within normal limits.
Four of five cats received adjuvant RT therapy following biopsy or surgery (cases 2, 3, 4 and 5). Three cats were treated with strontium-90 (cases 2, 3 and 4). Cases 2 and 3 received a total dose of 130 Gy using a 1 cm probe. One cat (case 5) was treated with strontium-90 following the first surgery and palliative RT following the revision surgery. Case 2 was additionally prescribed a 4-week course of meloxicam (0.3 mg PO q24h); initiation of systemic chemotherapy (doxorubicin) was recommended but declined by the owners. No other pertinent treatments were received.
Case 5 developed tumor recurrence 363 days following the initial surgery, prompting revision surgery. Tumor recurrence was noted 23 days following the revision and RT was started 20 days thereafter. Otherwise, neither recurrence nor distant metastasis was reported in any other case. Continued follow-up every 3 months (case 2) and every 9–12 months (case 3) was recommended to include three-view thoracic radiographs. At the time of writing, restaging was not performed at any time for either case.
The outcomes of the five cats are summarized in Table 1. Of the five cats in this study, three (cases 2, 3 and 5) were alive at the time of follow-up at 365, 1381 and 618 days following initial treatment, respectively. Two of the five cats (cases 1 and 4) were lost to follow-up at 311 days and 1 day after the initial treatment. However, stable disease was reported for one cat (case 1) following completion of the RT protocol.
Case characteristics, therapy and outcome in five cats with hemangiosarcoma of the nasal planum
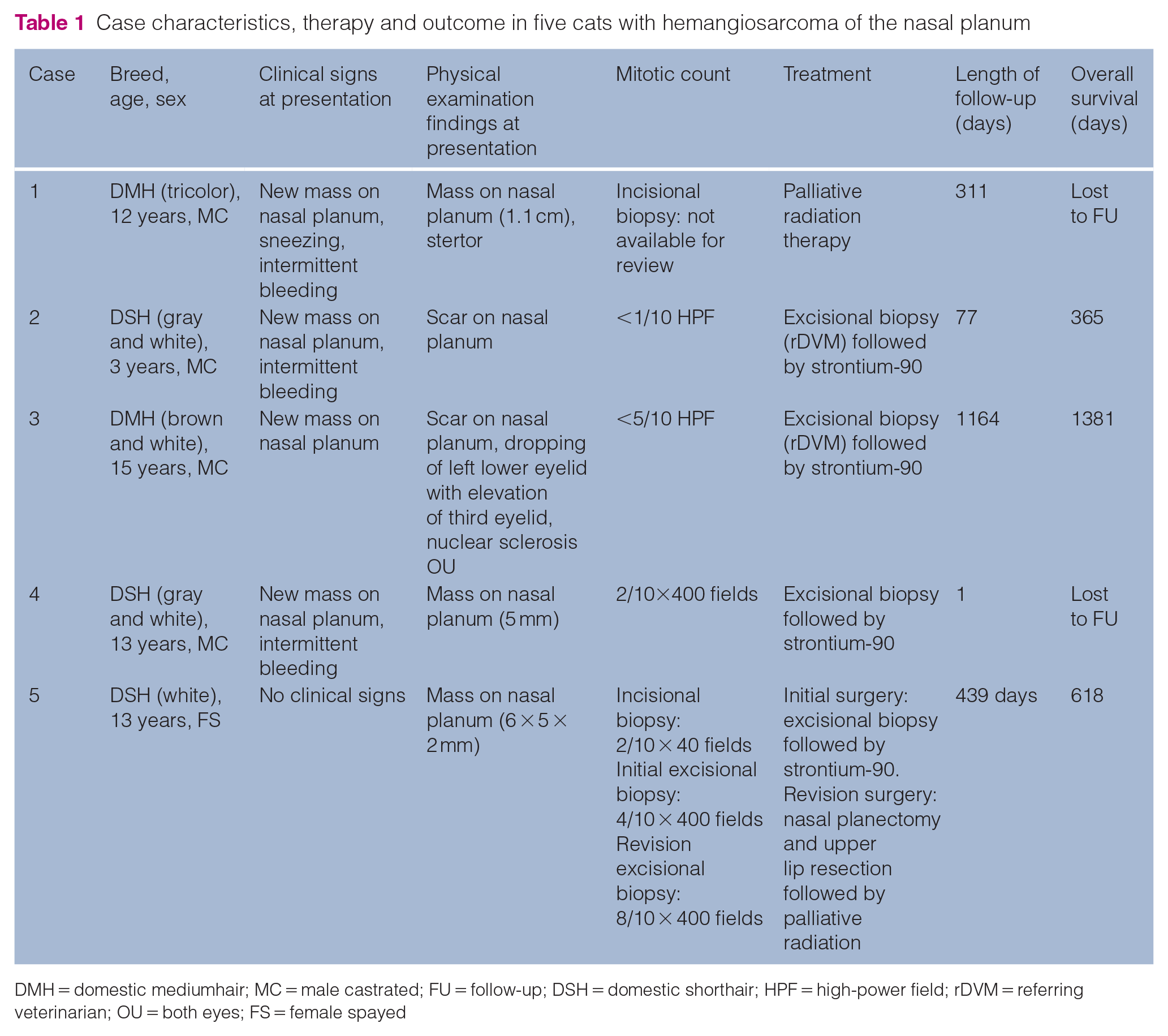
DMH = domestic mediumhair; MC = male castrated; FU = follow-up; DSH = domestic shorthair; HPF = high-power field; rDVM = referring veterinarian; OU = both eyes; FS = female spayed
Discussion
Compared with dogs, vascular tumors of endothelial origin, particularly hemangiosarcoma, are rare in cats. 5 Several primary sites of origin, including cutaneous and subcutaneous tissues, mesentery, spleen, liver, mediastinum and lung have been reported, though cutaneous is the most common in cats.6,9 Based on our literature review, this is the first case series to specifically characterize hemangiosarcoma of the nasal planum in cats.
As with other reports evaluating feline cutaneous, subcutaneous and/or visceral hemangiosarcoma, our data suggest that hemangiosarcoma of the nasal planum is primarily a disease of middle-aged to older cats.7,8,9,12,13 In one study with 18 cats that had a diagnosis of hemangiosarcoma, 70% had a sudden onset of clinical signs, including a visible or palpable mass. 5 Similarly, in the present study, all cats were initially presented for further evaluation due to the development of a mass along the nasal planum with bleeding of the mass reported in 3/5 cats.
The specific etiology of these tumors is unknown; however, the prevalence of cutaneous lesions on the head, pinna and in areas of hypopigmentation make ultraviolet radiation a suspected risk factor. 12 A retrospective study evaluating cutaneous vascular neoplasia in 15 cats found that hemangiosarcoma occurred primarily in white-haired areas, specifically on the pinna or elsewhere on the head. 8 In the current study, one cat was tricolor, two were gray and white, one was brown and white, and one cat was all white, which could support the occurrence of hemangiosarcoma in areas of hypopigmentation. However, it is important to note that retrospective record review precluded identification of the pigmentation status of the nasal planum specifically. In humans, angiosarcoma occurs commonly on the scalp, as well as sites of previous RT, which further supports the suspicion that the effects of radiation might be involved in the development of hemangiosarcoma.14–19 Other potential predisposing factors in the etiology of hemangiosarcoma in humans include chronic lymphedema and vascular stasis.15,17
Surgical excision was the primary treatment modality used in our study (4/5 cats). In a retrospective study evaluating 18 cases of feline cutaneous hemangiosarcoma, cats that underwent surgical resection were found to have a significantly longer median survival time compared with those that did not receive surgery. 13 In a study by Johannes et al, 7 this finding was further supported, and improved survival times with complete excision of tumors vs those that were incompletely excised were also documented. Surgical margins were more likely to be incomplete with a greater risk of local recurrence in those diagnosed with subcutaneous hemangiosarcoma vs cutaneous hemangiosarcoma. 7 Similar findings were reported in a study that evaluated 31 cases of feline hemangiosarcoma that received surgery, 10 where completeness of excision was found to be the most important factor in predicting the clinical outcome in cases of non-visceral hemangiosarcoma. 9 Unfortunately, in the present study, all documented margins were narrow or incomplete. However, adjuvant therapy with strontium-90 was pursued in all four cases receiving surgery, to improve local tumor control.
The potential benefit of adjuvant therapy following surgical excision of feline hemangiosarcoma has not been well documented. In dogs, a study evaluating the effects of palliative RT on non-splenic hemangiosarcoma reported that 15/20 dogs (75%) benefited from RT, with 4/20 total dogs (20%) having complete responses and most dogs tolerating RT well. 20 In humans diagnosed with angiosarcoma of the scalp, surgery is the treatment of choice and postoperative RT has been used to reduce the risk of local recurrence. 21 Definitive RT is also a treatment option when surgery is contraindicated. 21 One cat in the current study underwent palliative RT alone, which was well tolerated. However, this cat was lost to follow-up 311 days after treatment. Owing to the low number of cats receiving each treatment modality, statistical comparison of median survival times for those receiving palliative RT alone with those treated with a combination of surgical excision and RT (either strontium-90 or a combination of strontium-90 and palliative RT) could not be performed. No cats in the present study received chemotherapy as an adjuvant. In humans, chemotherapy has been used in conjunction with RT to improve survival by reducing the rate of distant metastasis following RT. Similarly, chemotherapy has resulted in prolonged survival in dogs with subcutaneous hemangiosarcoma. 22 However, studies are needed to further evaluate the potential benefits of chemotherapy as a sole agent or adjunctive in feline cutaneous hemangiosarcoma.
The metastatic potential for cats diagnosed with cutaneous hemangiosarcoma was historically found to be low compared with visceral varieties with tumor recurrence more likely.8,9 In this study, no cats were found to have distant metastasis at the time of diagnosis or at later follow-up, and a single cat was diagnosed with recurrence. The authors recognize that 2/5 cats could not be reached for follow-up; therefore, these cats may have undetected metastasis or local tumor recurrence. Additionally, one cat did not have staging performed at the time of diagnosis, further limiting the conclusions regarding metastatic potential. However, more recent reports have identified that the cutaneous–subcutaneous forms may behave more aggressively with higher metastatic potential than previously thought. 6 Therefore, complete staging via thoracic radiography, abdominal ultrasonography and a minimum database (CBC, serum biochemistry and urinalysis) should be performed prior to treatment.
This case series had low case numbers owing to the infrequency of diagnosis of this disease, which precluded multivariate analysis. Case accrual was increased by a multi-institutional collaboration, but there are some associated limitations, including the retrospective nature of the study and the lack of standardized follow-up.
Conclusions
Based on this small case series, hemangiosarcoma should be considered a differential diagnosis in cats with tumors of the nasal planum. Acute signs, such as a visible or palpable mass, were common at presentation. Surgery in combination with strontium-90 was the most commonly used treatment modality and resulted in adequate disease control with recurrence noted in one cat. Early surgical excision is recommended for local tumor control. Adjuvant therapy, such as RT, can be considered in cases where complete surgical excision is not possible, or in cases of recurrence. However, these findings are based on a small case series and further evaluation of these tumors is required.
Footnotes
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The work described in this manuscript involved the use of non-experimental (owned or unowned) animals. Established internationally recognized high standards (‘best practice’) of veterinary clinical care for the individual patient were always followed and/or this work involved the use of cadavers. Ethical approval from a committee was therefore not specifically required for publication in JFMS. Although not required, where ethical approval was still obtained, it is stated in the manuscript.
Informed consent
Informed consent (verbal or written) was obtained from the owner or legal custodian of all animal(s) described in this work (experimental or non-experimental animals, including cadavers) for all procedure(s) undertaken (prospective or retrospective studies). No animals or people are identifiable within this publication, and therefore additional informed consent for publication was not required.
