Abstract
Objectives
The aim of this study was to describe the sedative and some physiological effects of tiletamine–zolazepam following buccal administration (BA) in cats.
Methods
Seven healthy spayed European shorthair cats (three males, four females) were studied twice in this randomized, blinded, crossover study. Each cat received two doses of tiletamine–zolazepam by BA: the low-dose (LD) group consisted of 5 mg/kg of each drug, and the high-dose (HD) group consisted of 7.5 mg/kg of each. Baseline systolic blood pressure (SAP), heart rate (HR), respiratory rate (RR) and a sedation score were recorded prior to administration of each treatment. The same variables plus the percentage of hemoglobin saturated with oxygen as measured by pulse oximetry (SpO2) were recorded at predefined intervals for the next 2 h.
Results
All cats completed the study. No retching or vomiting were observed. Hypersalivation was observed in 0/7 and 3/7 for LD and HD groups, respectively (P = 0.2). There were significant changes in scores over time for posture, response to clippers and response to manual restraint for both groups, without differences between groups. RR, HR and SAP changed significantly over time. SAP and RR were significantly lower for the HD than for the LD group. No values for hemoglobin saturation <95% were observed.
Conclusions and relevance
BA of tiletamine–zolazepam at the doses studied here is a simple and effective method for chemical restraint in cats, where the LD group had a lower impact on SAP and RR than the HD group.
Introduction
Intramuscular (IM) or subcutaneous (SC) routes are commonly used to administer sedatives and analgesics in veterinary medicine. In cats, however, these routes of injection require technical skill and proper restraint, 1 and may cause pain and stress. 2 Additionally, aversive reactions to such injections, especially in fractious animals, could result in injuries to the cat or the operator. Aversive reactions to injections are among the most frequent reasons why cat owners find visits to the veterinarian a highly stressful experience for the animal and themselves. 3 Alternative routes for drug administration that avoid such reactions but provide good effects are therefore desirable.
Buccal administration (BA), also referred to as the oral transmucosal route, consists of the application of drugs into the oral cavity in contact with the cheek mucosa and might be attractive to veterinarians and their clients because it is simple and painless.4–6 If drug characteristics are favorable, there is a potential for rapid uptake, and first-pass elimination by the liver may be minimized. 5 This technique also eliminates the risk of needle-stick injury to the animal or the operator, and in most animals it can be performed by a single operator.1,7 BA has been successfully used to administer drugs to different animal species.8–18
Tiletamine–zolazepam (TZ) is an injectable anesthetic mixture of equal concentrations of both agents. Tiletamine belongs to the cyclohexamine family and provides rapid immobilization, but also causes muscle rigidity. Zolazepam is a benzodiazepine with sedative, muscle relaxant and anti-seizure effects. The mixture has been used in cats for chemical restraint and short surgeries in combination with analgesics, and can be administered IM, SC, intravenously (IV) or by the intranasal route (extra-label).19–22 It has also been used in combination with alpha2-adrenergic agonists, ketamine and/or opioids, to augment the depth of anesthesia, analgesia or to extend its duration.23–25
To our knowledge, the effects of TZ after BA in cats have not been reported. Thus, the aim of this study was to evaluate sedation, systolic arterial blood pressure (SAP), heart rate (HR) and respiratory rate (RR) following BA of two doses of TZ to healthy cats
Materials and methods
Animals
All procedures were carried out in accordance with Animal Welfare Policy (Act 087/02, Faculty of Veterinary Sciences, UNCPBA, http://www.vet.unicen.edu.ar). Seven European shorthair cats (three castrated males, four spayed females; mean ± SD age 6.0 ± 0.8 years and weighing 3.96 ± 0.56 kg), belonging to the research colony of the Faculty of Veterinary Science, National University of the Center of Buenos Aires Province, Tandil, were included in the study. The animals were housed individually under controlled temperature (22ºC) and lighting (12 h light–dark cycle) and were adapted to human contact, including manual restraint in lateral recumbency, Doppler arterial blood pressure measurement and BA of water for 8–10 weeks prior to data collection. All cats were classified as American Society of Anesthesiologists’ status I based on physical examination, including HR, RR and systolic blood pressure measurements (Parks Doppler Ultrasound Model 812; Parks Medical), and complete blood count, serum chemistry profile and urinalysis.
Experimental design
Each cat was studied twice with a washout period of 1 week, in a blind, crossover design, with the order of treatment groups selected at random using a list randomizer. 26 Food and water were withheld for 12 h and 2 h, respectively, prior to the beginning of each study. Treatment administration was performed in a quiet area. Two different doses of TZ were evaluated: the low-dose (LD) group received TZ hydrochloride (Zelazol; Zoetis Brasil) 5 mg/kg each, and the high-dose (HD) group received the same formulation at a dose of 7.5 mg/kg each, by BA. In each case, the formulation was deposited into the cheek pouch of each cat’s mouth using a syringe. TZ was reconstituted with 5 ml sterile water as recommended by the manufacturer. A final concentration of 10% w/v of TZ combination was used and 0.1 ml/kg or 0.15 ml/kg was administrated to cats in the LD or HD groups, respectively.
Gastrointestinal, sedative and cardiorespiratory variables (see below) were measured prior to drug administration (baseline), and at 15, 30, 45, 60, 120 and 240 mins after administration. All variables were recorded by two veterinarians unaware of treatment allocation.
Gastrointestinal side effects
Each cat was observed for the presence of hypersalivation, retching or vomiting. These variables were recorded as all-or-none.
Sedative effects
A sedative score was completed by observations of posture, response to clipper sound and response to manual restraint for catheterization, using a modified scale from Santos et al (Table 1). 1 Response to clippers was only evaluated after drug administration and was avoided at baseline to prevent stress to the cats.
Criteria for evaluating level of sedation in cats (adapted from Santos et al) 1

Effects on HR, RR and SAP
SAP, HR and RR were measured at baseline and at every predefined interval after drug administration. In addition, rectal temperature and the percentage of hemoglobin saturated with oxygen as measured by pulse oximetry (SpO2 ) were recorded following administration of TZ. SAP was measured using a Doppler monitor (Parks Doppler Ultrasound Model 812; Parks Medical Electronics) placed over the palmar digital artery. A suitably sized cuff (width of approximately 30% of the limb circumference) was placed over the ulna/radius.27,28 All SAP measurements were performed by a single operator. At each time point, blood pressure was measured five times; the average of these values was used for analysis. HR was determined by auscultation using a pediatric stethoscope (Littman Classic II Pediatric). SpO2 was measured using a probe placed on the front paw on each cat and was automatically measured by a multi-parametric monitor (Goldway UT 4000 F). Supplemental oxygen via a facemask was to be administered to any cat with SpO2 values <95%. RR was counted from visualization of chest excursions over a period of 1 min. Blankets and hot water bottles were used to maintain the rectal temperature between 36–38ºC.
Statistical analysis
The incidence of hypersalivation, retching and vomiting was compared between groups with Fisher’s exact tests. Normal distribution for SAP, HR and RR was confirmed with the Shapiro–Wilk test, and the effects of treatment and time (and their interaction) on those variables were evaluated using linear mixed-effect models for repeated measures. Sedation scores were non-parametric and analyzed with a generalized linear mixed-effect model, using a log-Poisson as link function. All analyses were performed using the software SAS version 9.3 (SAS Institute), with significance set at <0.05. Results are summarized as mean ± SD and median, minimum and maximum (range) for parametric and non-parametric data, respectively.
Results
Gastrointestinal side effects
All cats completed the study. No differences in hypersalivation, retching or vomiting were observed between groups (P >0.2). Hypersalivation was observed in 3/7 cats immediately after administration of the high dose, and in 0/7 of the animals receiving the low dose. Neither retching nor vomiting were observed in any cat.
Sedative effects
Scores for posture, response to clippers and response to manual restraint are shown in Table 2. There were significant changes over time for all three variables (P <0.01) for both groups, where the scores at baseline and 240 mins were significantly lower than the scores at other time points, except for posture, where the score at 120 mins was lower than 15, 30 and 45 mins, but higher than baseline. No differences between doses were observed (all P >0.2). The interaction between time and treatment was not significant for any variable (all P >0.8).
Median (range) behavior sedation scores in cats following buccal administration of tiletamine–zolazepam hydrochloride at 5 mg/kg each (low dose [LD]) and 7.5 mg/kg each (high dose [HD])

There were no differences in the overall sedation score between groups (all P >0.2). Time effect was statistically different for each category (all P <0.01). The interaction time × treatment was not significant for any variable (all P >0.8)
Effects on HR, RR and SAP
RR, HR and SAP changed significantly over time (P <0.0001, P = 0.023 and P = 0.016, respectively) (Figures 1–3). SAP and RR were significantly lower for cats in the HD group compared with cats in the LD group (P = 0.004 and P = 0.028, respectively); there were no differences for HR between groups (P = 0.4) (Figure 2). There was no significant interaction between time and treatment for any variable (all P >0.5). No values for SpO2 <95% were observed. Unfortunately, measurements at 240 mins post-treatment were not assessed because cats were reluctant to instrumentation.
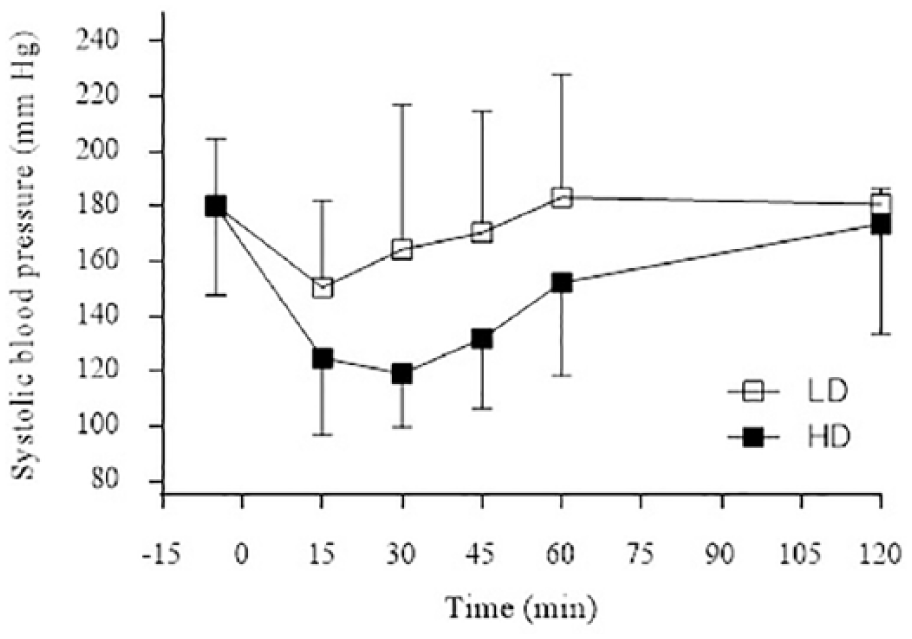
Mean ± SD systolic blood pressure (SAP; mmHg) in cats following buccal administration of tiletamine–zolazepam hydrochloride at 5 mg/kg each (low dose [LD]) and 7.5 mg/kg each (high dose [HD]). Overall SAP was lower in cats in the HD group (P = 0.004)

Mean ± SD heart rate (HR) in cats following buccal administration of tiletamine–zolazepam hydrochloride at 5 mg/kg each (low dose [LD]) and 7.5 mg/kg each (high dose [HD]). There were no differences in the overall HR between groups (P = 0.4)

Mean ± SD respiratory rate (RR) in cats following buccal administration of tiletamine–zolazepam hydrochloride at 5 mg/kg each (low dose [LD]) and 7.5 mg/kg each (high dose [HD]). Overall RR was lower in the LD group (P = 0.028)
Discussion
The main observation of this study is that TZ (5 mg/kg [LD] and 7.5 mg/kg [HD]) by BA in cats effectively produced sedation that occurred approximately 15 mins after administration and lasted for 120 mins.
Chemical restraint is necessary for many procedures in cats; however, aversive reactions to IM injections often occur. 29 The BA route offers an alternative way to administer drugs; the lack of discomfort from this route of administration may improve the overall experience of the cats and the owners when medication is administered. The BA route differs from oral administration in that the first-pass hepatic effect is avoided. The rich blood supply to the oral mucosa allows for therapeutic circulating concentrations to be reached promptly. 6 Drug uptake via the oral mucosa is a passive diffusion process; permeation is superior with lipophilic compounds. 30
Tiletamine and zolazepam are highly lipophilic (logP 2.7 and 1.68, respectively) 31 weak bases and, hence, are well suited for BA. 30 The pH of the cat mouth is reported to be alkaline, which would favor the unionized form of basic compounds and improve its uptake.32,33 Despite that, Pypendop et al demonstrated a weak correlation between bioavailability and unionized calculated fraction for opioids (weak bases) following buccal administration in cats. 34 The buccal pH of the animals was not measured in the present study. TZ is available in an acidic formulation (pH 3.5) and its administration might decrease the buccal pH. The resulting buccal pH, following the administration of these drugs, could affect the uptake process. 33 Unfortunately, the effect of those changes on the uptake of the agents is unknown. While we did not measure plasma concentrations of TZ after BA, a level of sedation that produced lateral recumbency and abolished the reaction to manual restraint and clipping was achieved in all animals for the two doses evaluated in this study, suggesting that effective concentrations of both drugs for a clinically useful level of sedation was achieved. Specific pharmacokinetic studies are needed to correctly characterize TZ uptake following buccal administration in cats.
In this study, both doses resulted in similar sedation, based on observed behavioral responses. From a clinical point of view, we cannot comment on whether this level of sedation would be sufficient to allow other more stimulating or painful procedures than those described in this study. Sedation was not assessed at the 240 min point, as recovery in some cats was accompanied with signs of dysphoria, complicating assessment. For both groups, the highest median sedation scores for each category were obtained between 15 and 60 mins post-administration but had decreased at the 120 min time point; a similar observation was reported when these drugs were used IV. 35 In that study, doses of 9.7, 15.8 and 23.7 mg/kg were evaluated. Our observations suggest that BA produced sedation of similar duration to that of the IV route, albeit with a slower onset.
A dose-dependent decrease in SAP, HR and RR was observed in our investigation. The decrease of these variables over time mirrored the increase in depth of sedation that also occurred. In all cats SAP was ⩾100 mmHg, with the nadir occurring between 15 and 30 mins after administration. A similar trend was observed for HR. However, the decrease in RR lasted for up to 60 mins in cats receiving the highest dose of TZ. Because measurements between 60 and 120 mins were not collected, it is uncertain at which point between those times the RR began to increase. Unfortunately, neither end-tidal, nor arterial CO2 pressures were measured and, hence, we cannot comment on the adequacy of ventilation of these animals. However, no SpO2 values <95% were recorded; hence, if hypoventilation did occur, its magnitude was not such to result in clinically relevant hemoglobin desaturation.
It is known that various medications and toxins may cause ptyalism as a result of their disagreeable taste. In this study, increased salivation was observed in three cats in the HD group immediately after administration. Considering this temporal relation, we speculate that this was caused by the taste of the drugs, and not by a centrally mediated mechanism, as may occur with emetogenic substances. Hypersalivation is commonly accompanied by increased swallowing. Both hypersalivation and swallowing could interfere with buccal absorption, as the agent could become diluted with the secretions, or could be ingested. 32 This could explain the variation in sedation scores obtained between animals for a same dose. However, a similar effect was observed in most cats, showing a predictable response to treatment.
Conclusions
TZ administered at two doses, 5 mg/kg and 7.5 mg/kg, each by BA in cats, produced sedation sufficient to tolerate manual restraint and clipping without any aversive reactions that lasted more than 30–45 mins. For these drugs, and others with similar characteristics, the BA might be useful for replacing IM injections and improve the overall experience of the cat and the owners during veterinary visits.
Footnotes
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
