Abstract
Objectives
The aim of this study was to compare the quality of sedation and recovery, and ease of venipuncture following sedation for feline blood donation using two intramuscular (IM) sedation protocols: alfaxalone/butorphanol (AB) and dexmedetomidine/butorphanol (DB).
Methods
This was an experimental randomized, blinded, crossover study. Ten client-owned healthy cats were recruited to participate in the study. Cats were sedated with AB (alfaxalone 2 mg/kg and butorphanol 0.2 mg/kg) for one donation and DB (dexmedetomidine 10 μg/kg and butorphanol 0.2 mg/kg) for another. Reaction to injection, quality of sedation and quality of recovery were assessed by a blinded observer. Time to lateral recumbency, number of venipuncture attempts, time required for blood collection and time to return to sternal recumbency were recorded. Cats were monitored for evidence of gastrointestinal distress. Each donation consisted of a maximum of 53 ml whole blood drawn over 3–22 mins. Donors received 100 ml subcutaneous lactated Ringer’s solution in recovery. Owners, unaware of sedation protocol, were asked to complete a questionnaire evaluating their cat’s behavior following sedation.
Results
IM injections were well tolerated by both treatment groups. There was no significant difference between treatment groups in sedation scores for posture (P = 0.30) or behavior (P = 0.06). Cats sedated with DB had significantly higher muscle relaxation scores (P = 0.03) compared with AB. There was no significant difference between treatment groups in time to lateral recumbency (P = 0.12), number of venipuncture attempts (P = 0.91) and time for blood draw (P = 0.29). There was no difference in quality of recoveries between treatment groups based on simple descriptive scores (P = 0.18) and owner evaluation 24 h following sedation. One cat vomited following administration of DB.
Conclusions and relevance
Alfaxalone is a suitable alternative to dexmedetomidine when combined with butorphanol and used as part of an IM sedation protocol for cats undergoing blood donation.
Introduction
Anemia is a common clinical finding in critically ill cats. 1 As a result, blood transfusion has become more common as part of the care of critically ill cats, and the development of specialized veterinary facilities has increased the demand for readily available blood products. 2 Many hospitals acquire blood from in-house donors, or from client-owned cats enrolled in a voluntary feline blood donor program. 3
Donors frequently give blood multiple times, and the restraint required for donation can become increasingly challenging. 4 To minimize stress, as well as to facilitate phlebotomy, donor programs routinely sedate cats for donation.4–6 The success of voluntary donor programs relies on owner satisfaction of the donor experience. To limit donor side effects both in hospital and at home, an ideal sedation protocol would have minimal cardiovascular impact on the donor, allow for a rapid recovery, cause minimal residual side effects and allow cats to quickly resume normal behaviors.
Numerous sedation protocols have been proposed for feline blood donation,4–6 many of which include drugs such as dexmedetomidine, medetomidine, ketamine or inhalant anesthetics. The current sedation protocol utilized by the Foster Hospital for Small Animals blood bank involves an intramuscular (IM) injection of dexmedetomidine and butorphanol. Advantages of dexmedetomidine include ease of administration, short onset of action, good quality sedation and an available reversal agent, 7 allowing donor cats to quickly resume normal behaviors. Butorphanol is administered along with dexmedetomidine to enhance sedation. 8 Disadvantages of dexmedetomidine include emesis, bradycardia, increased peripheral resistance and decreases in cardiac output.5,9 One hospital found that sedation with medetomidine, a racemic mixture of levomedetomidine and dexmedetomidine, 6 resulted in several cats becoming pale and bradycardic, and that phlebotomy was difficult, resulting in several donations being aborted. 4
Alfaxalone is an injectable drug approved for anesthetic induction and maintenance in cats.10,11 In Australia, alfaxalone is also approved for IM administration in cats. 10 Reported advantages of alfaxalone include minimal discomfort on injection, good quality of sedation, and rapid and smooth recovery. 10 Unlike some drugs commonly used for feline blood donation, alfaxalone is thought to have minimal cardiovascular effects at clinically relevant doses.10,11 These features make alfaxalone an appealing choice to facilitate feline blood donation.
The objective of this study was to investigate whether alfaxalone and butorphanol (AB) is a suitable alternative to dexmedetomidine and butorphanol (DB) when used as part of an IM sedation protocol for cats undergoing blood donation.
Our hypothesis was that the combination of AB administered IM would provide adequate sedation and good-quality recovery for cats undergoing blood donation. We also hypothesized that venipuncture and blood collection would be easier to perform, and there would be fewer instances of gastrointestinal upset (GIU) in cats administered AB vs cats administered DB.
Materials and methods
Animals and study design
Ten adult domestic shorthair cats from the Foster Hospital for Small Animals feline blood donor program were recruited for the study. Health status was assessed by physical examination, as well as results from the donor screening process, including serum biochemical analysis, complete blood count, blood type, N-terminal pro-brain natriuretic peptide level and infectious disease screening in accordance with the Consensus Statement of the American College of Veterinary Internal Medicine on Feline Blood Donor Screening for Blood-Borne Pathogens. 12 Inclusion criteria consisted of cats between 1 and 8 years of age who were indoor only and weighed >4.0 kg (8.8 lb). Cats that would not tolerate handling for pre-sedation health assessment were excluded from the study.
The study protocol was approved by the Institutional Animal Care and Use Committee at Tufts University. Following owner consent, each cat was enrolled in the study and scheduled to participate in two blood donation events. To allow for hematologic recovery and washout from the first event, there was a minimum of 6 weeks between each blood donation. At the first blood donation, cats were randomly assigned to one of two sedation protocols using an online randomization tool (http://emerald.tufts.edu/~gdallal/assign.htm) in a cross-over study design. At the second blood donation, each cat received the second of the two sedation protocols. All investigators were fully blinded to treatment assignments, except for the blood bank technician who drew up and administered treatment drugs in accordance with the randomization plan.
Sedation
Sedation consisted of one of two IM protocols: AB (alfaxalone 2 mg/kg [Alfaxan; Jurox] and butorphanol 0.2 mg/kg [Torbugesic; Fort Dodge Animal Health]); or DB (dexmedetomidine 10 μg/kg [Dexdomitor; Zoetis Services] and butorphanol 0.2 mg/kg). Treatment drugs were drawn up in accordance with the randomization plan and combined into a single 3 ml Luer Lock syringe. Saline was added to the DB syringes so that the total volume of treatment drugs were equal. Treatment drugs were injected using a 25 G needle into the lumbar epaxial muscles.
Reaction to injection was recorded (0 = none; 1 = mild; 2 = moderate; 3 = severe) and cats were observed in a quiet room by a blinded observer (RCR). A scoring system adapted from Ribas et al 10 was used to evaluate the level of sedation in respect to posture, behavior and muscle relaxation (see supplementary material) at 2, 5, 10, 15 and 20 mins post-injection or until the cat reached a posture score of 3. Once each cat reached a score of 3 for posture, or 20 mins after initial injection, sedation scoring was discontinued and cats were placed in right lateral recumbency (LR) for blood collection. Time (mins) from injection to LR was recorded.
GIU
The same blinded observer (RCR) monitored cats for evidence of GIU. GIU was defined as behaviors suggesting gastrointestinal distress, including salivation, lip smacking or vomiting, at any time point following sedation until discharge.
Blood collection
Once each cat reached a score of 3 for posture, or 20 mins after initial injection, cats were placed in right LR and eye lubricant was administered. Cats that did not achieve LR on their own were gently placed in right LR and their necks extended to facilitate blood collection. If a cat was not amenable to gentle restraint for blood collection, the procedure was aborted and the cat was moved to recovery. Blood collection was performed by the same person each time using a procedure modified from Killos et al. 5 Briefly, after sterile preparation of the jugular vein, a 21 G butterfly needle was inserted into the vessel and attached to a collection system previously described. 5 A maximum of 53 ml blood was collected from each donor. The number of venipuncture attempts, volume of blood collected (ml) and time required (mins) for blood donation were recorded. Once blood collection was complete, a pressure bandage was placed over the venipuncture site, and cats were administered 100 ml lactated Ringer’s solution (Hospira) subcutaneously.
Recovery
Cats were positioned in LR on a blanket in their personal travel carrier with the door open, and placed in a quiet location for observation. Quality of recovery was assessed by the same blinded observer (RCR) using a simple descriptive scale adapted from Caines et al (see supplementary material), 13 as well as through owner evaluation via email survey (see supplementary material). Time taken (mins) to recover from sedation, defined as return to sternal recumbency, was also recorded.
After recovery for the first cat was prolonged, the study protocol was amended to require that cats administered DB that did not return to sternal recumbency within 1 h of initial injection would be administered atipamezole 0.1 mg/kg IM (Antisedan; Zoetis Services) by a non-blinded observer. Cats administered AB that did not return to sternal recumbency within 1 h of initial injection would be administered an IM injection of saline to ensure that investigators remained blinded to the treatment groups. Once the cat achieved sternal recumbency, or once a reversal agent was administered, direct observation by study investigators was discontinued and the cat was returned to the owner or temporarily housed in a hospital ward until the owner was available.
Statistical analysis
Statistical analysis was performed with commercially available software (SAS). The non-parametric Wilcoxon rank sum test was used to compare the distribution of continuous variables between treatment groups. Categorical data were analyzed using a likelihood ratio χ2 test. A multinomial logistic model was used to analyze the effect of treatment group on quality of sedation scores (SS). Significance level was set at P ⩽0.05. Normally distributed data are presented as mean ± SD; non-normally distributed data are presented as median (range).
Results
Eleven cats were identified from the Foster Hospital for Small Animals blood donor program as eligible for participation and underwent pre-sedation assessment. One cat was excluded due to bradycardia identified during physical exam. The remaining 10 cats were enrolled in the study. Five cats were castrated males and five were ovariohysterectomized females. Median age was 4.3 years (range 1.8–7.2 years) and median body weight was 5.2 kg (range 4.4–7.0 kg). Time between donation sessions for each cat ranged from 12–35 weeks.
No significant difference in reaction to injection between treatment groups was identified (P = 0.77). One cat became fractious during the study period and obtained minimal sedation under both protocols. This cat scored a 3 (severe) reaction to injection for both protocols. Aside from this cat, IM injections were well tolerated by the other nine cats. The median score for reaction to injection was 0 for both treatment groups (range: AB 0–3, DB 0–3).
All cats showed some sedation following IM injection, therefore SS were analyzed for all cats. The results of SS for each treatment group with respect to posture, behavior and muscle relaxation are illustrated in Figures 1, 2 and 3, respectively. Based on the multinomial logistic models, there was a significant effect of time on the probability of achieving higher posture (P = 0.005), behavior (P = 0.003) and muscle relaxation (P = 0.004
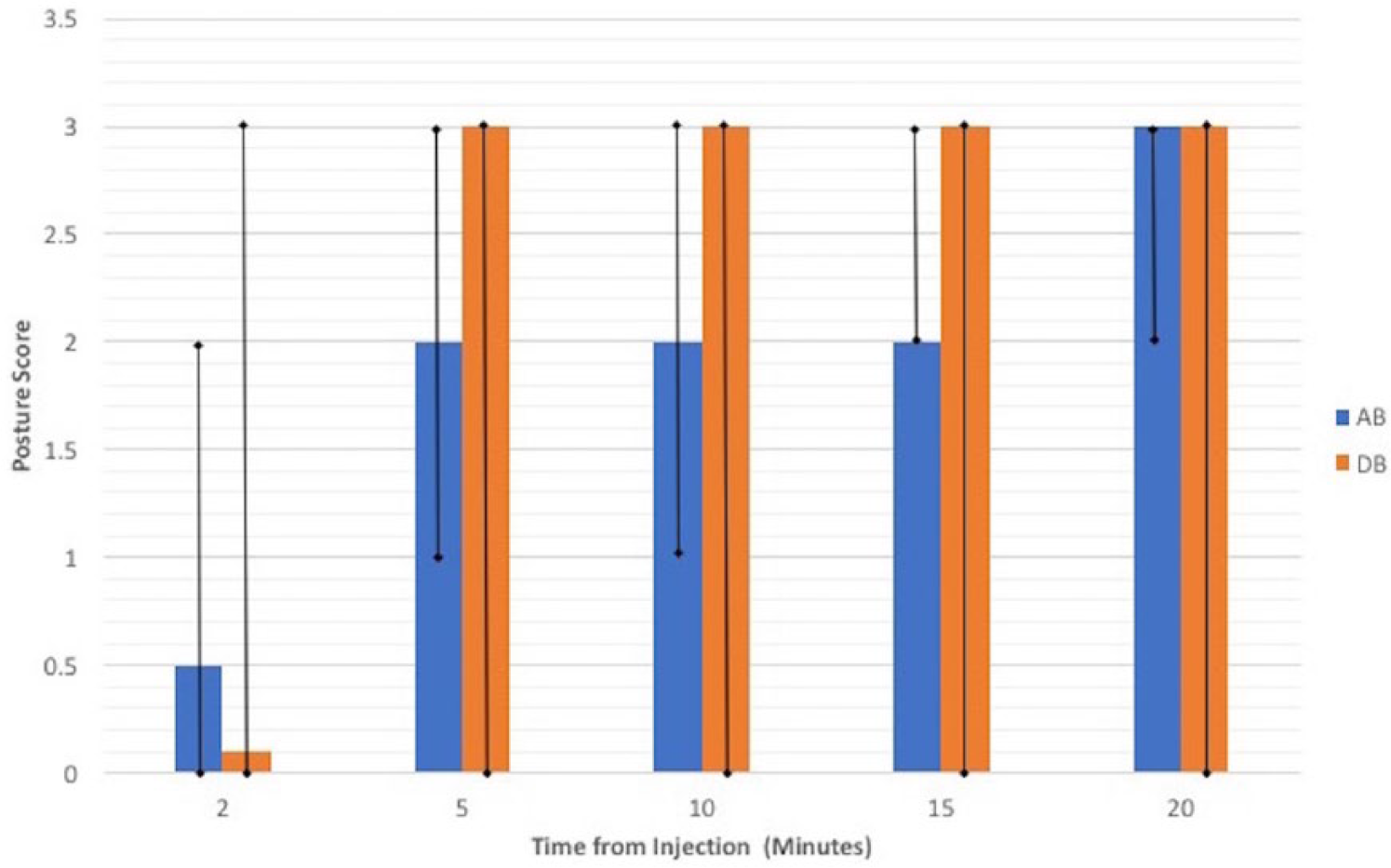
Median posture scores over time for 10 cats receiving alfaxalone and butorphanol (AB) or dexmedetomidine and butorphanol (DB). There was no significant difference (P = 0.30) between AB and DB. Data are reported as median. Vertical bars represent range
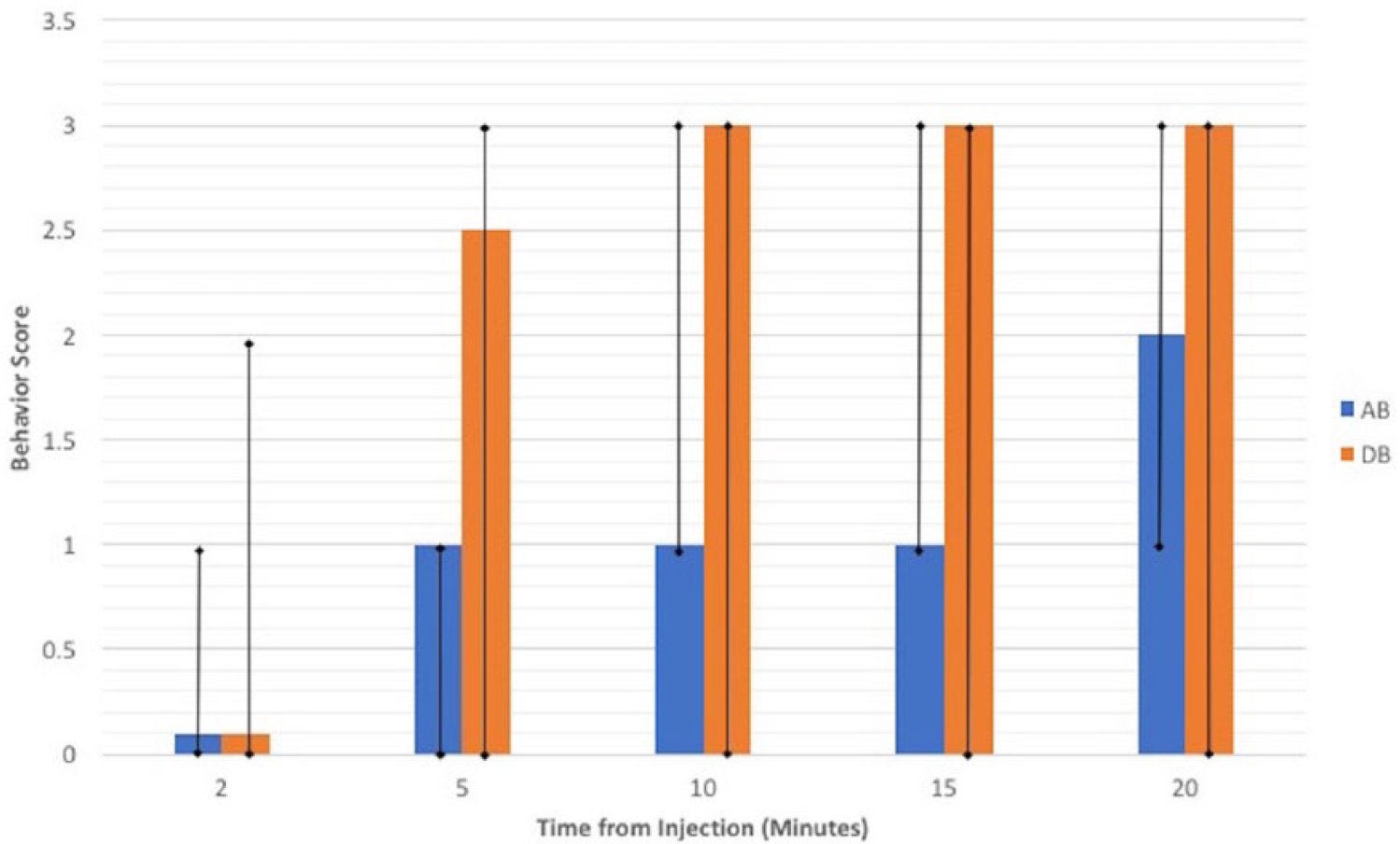
Median behavior scores over time for 10 cats receiving alfaxalone and butorphanol (AB) or dexmedetomidine and butorphanol (DB). There was no significant difference (P = 0.06) between AB and DB. Data are reported as median. Vertical bars represent range

Median muscle relaxation scores over time for 10 cats receiving alfaxalone and butorphanol (AB) or dexmedetomidine and butorphanol (DB). Cats sedated with DB had significantly higher muscle relaxation scores (P = 0.03) compared with cats sedated with AB. Data are reported as median. Vertical bars represent range
No cat in the AB group demonstrated signs consistent with GIU. One cat administered DB vomited 13.5 mins after IM injection but then showed no additional signs consistent with GIU.
Seven cats administered AB achieved a sufficient level of sedation to allow for blood collection compared with eight cats in the DB group. Four cats administered AB attained LR, with a median time from injection to LR of 8.7 mins (range 5.5–12.6 mins); the remaining three cats in the AB group that donated blood did not achieve LR on their own, but tolerated being placed into LR for the blood draw. Eight of the cats administered DB attained LR, with a median time from injection to LR of 4.8 mins (range 3.1–22.5 mins). Of the cats that achieved LR (AB, n = 4; DB, n = 8), there was no significant difference in time to obtain LR between the two treatment groups (Figure 4).

Comparison of times required to attain lateral recumbency for 10 cats receiving alfaxalone and butorphanol (AB) or dexmedetomidine and butorphanol (DB). Horizontal bars represents medians, and diamonds represents mean values
Three cats administered AB and two cats administered DB did not achieve a sufficient level of sedation to allow for blood collection. Of these cats, two cats administered AB and one cat administered DB allowed venipuncture but moved before the total donation volume was collected. One cat in each treatment group did not sedate enough to allow for venipuncture.
Of the cats that achieved sufficient sedation for blood collection (AB, n = 7; DB, n = 8), there were no significant differences between treatment groups in the number of venipuncture attempts (P = 0.91) and the total time for blood draw (P = 0.29). The median number of venipuncture attempts for cats administered AB was two (range 1–4) and one (range 1–4) for cats administered DB. The median time for blood collection was 4.8 mins (range 3.5–5.9 mins) in cats administered AB and 3.5 mins (range 2.4–6.4 mins) in cats administered DB.
All cats showed some sedation following IM injection; therefore, recovery scores (RS) were analyzed for all cats. There was no difference in quality of recoveries between treatment groups based on both simple descriptive scores (P = 0.18) and owner evaluation of the cat’s behavior for 24 h following sedation (see Table 1). The median simple descriptive score for recovery was 0 (range 0–1) for both treatment groups, indicating a calm, smooth recovery. The median values for all owner-assessed behaviors were 3 (same as normal) for both treatment groups.
Results of comparison of effects of alfaxalone and butorphanol (AB) vs dexmedetomidine and butorphanol (DB) on owner-assessed behavior in 10 cats for 24 h following sedation for blood donation

Behaviors are reported on an ordinal scale of 1–5, where 1 is much less than normal, 3 is the same as normal and 5 is much more than normal. Values are reported as median (range)
The median time from injection to sternal recumbency for cats administered AB was 32.1 mins (range 28.9–57.6 mins). One cat administered DB took 111.6 mins to return to sternal recumbency, at which time the protocol was amended and seven cats in the DB treatment group were administered atipamezole 0.1 mg/kg IM. Because seven cats administered DB required reversal, the median time to sternal was not analyzed for this treatment group.
Discussion
The results of this study demonstrated that the combination of AB administered IM provides comparable sedation and good-quality recovery for cats undergoing blood donation when compared with cats administered DB. Cats administered AB had similar SS, time to onset of sedation and RS to cats administered DB. Additionally, the number of venipuncture attempts were similar between the two groups, and no cat administered AB demonstrated GIU.
Cats sedated with AB had similar RS compared with cats sedated with DB, and all scores were consistent with good-quality recoveries. There were no instances of prolonged ataxia or hyperkinesis, as has been reported following IM administration of alfaxalone to cats.14,15 The good recovery quality may be owing to the lower dose of alfaxalone used in this study, or the addition of butorphanol to the protocol. Ribas et al 10 found that cats administered the same dose of alfaxalone in combination with butorphanol had good-quality recoveries, and another study found that premedication with butorphanol and acepromazine prior to administration of alfaxalone improved RS. 16
While seven of the cats administered DB in this study remained in LR for up to 1 h, dexmedetomidine has an easily accessible reversal agent, atipamezole. Alfaxalone does not have a reversal agent, but its effects are short-acting, 11 and the median time for recovery from sedation in this study was just over 30 mins. These results are consistent with what has been reported with similar doses of IM AB. 10
Additionally, owner perception of recoveries for both sedation protocols were good, with the majority of all behavior categories being scored a 3 (normal) for both treatment drugs. Good-quality, rapid recoveries are an important part of sedation protocols used to facilitate feline blood donation, as it is important to owners that the donation process have minimal impact on the behavior of the donor.
One surprising finding of this study was that, excluding the cat with a fractious temperament, two cats in the AB group and one cat in the DB group did not achieve adequate sedation to allow for blood donation. One possible explanation for the lack of sedation could be inadvertent, partial administration of the treatment drug subcutaneously, resulting in erratic absorption. However, this is unlikely as the same trained person administered the IM injections to each cat.
Another explanation could be that cats in the Foster Hospital for Small Animals blood donor program are typically sedated and bled as soon as they arrive at the hospital. Owing to logistics surrounding the study protocol, many cats arrived at the hospital and waited before being sedated. It is possible that some cats became agitated during this time, and achieved less sedation as a result. An important quality that hospitals look for in donor cats is a calm demeanor. The lower doses of treatment drugs used in this study may not be suitable for cats that are agitated or have a fractious temperament.
Finally, it is possible that the dose of treatment drugs chosen for this study were too low. The dose of dexmedetomidine used in this study is below conventional doses of dexmedetomidine or equivalent alpha2 agonists;4,7 however, this dose of dexmedetomidine has been used to consistently provide sedation at the Foster Hospital for Small Animals blood bank for several years and therefore it was selected as the study dose.
Doses of 5 mg/kg alfaxalone IM combined with butorphanol have been reported to result in significantly better SS than a dose of 2 mg/kg. 17 The higher doses also led to significantly longer recovery times, 17 which is undesirable for the aims of the current study. The dose of alfaxalone used in this study was chosen based on data indicating that the same combination of AB provided sufficient sedation for echocardiograms without clinically significant changes in cardiovascular variables. 10 A study evaluating the use of alfaxalone as part of a sedation protocol for the treatment of hyperthyroid cats found that cats administered the same dose of AB required additional doses of alfaxalone (increments of 0.1 mg/kg IV) in order to achieve sufficient sedation for administration of 131I. The authors of that study increased the dose of alfaxalone to 3 mg/kg in combination with 0.2 mg/kg butorphanol, and found that the remaining cats attained sufficient sedation for treatment with minimal additional restraint. 18
Further studies are needed to determine if 3 mg/kg alfaxalone in combination with 0.2 mg/kg butorphanol IM would provide improved sedation for cats undergoing blood donation while continuing to provide a rapid recovery with minimal negative effects.
Both alfaxalone and dexmedetomidine are reported to result in muscle relaxation.19–21 The results of this study found that cats administered DB had significantly increased muscle relaxation scores compared with AB. This likely played a role in facilitating LR. Four cats administered AB achieved LR on their own vs eight cats administered DB. Deutsch et al 17 compared two different IM doses of alfaxalone in combination with butorphanol in cats and found that only half of the cats administered 2 mg/kg alfaxalone achieved LR; our results are consistent with this finding. The dose of alfaxalone used in this study was selected because cats do not have to achieve LR to allow for blood donation, they simply have to be sedate enough to allow being restrained for blood draw. While only four cats in the AB treatment group attained LR on their own, the majority of cats sedated with AB tolerated positioning in LR to allow for blood donation.
One cat had a severe reaction to IM injection of both sedation protocols. In the remainder of cats, IM injections were well tolerated for both treatment groups with scores of 0 (none) and 1 (mild). There are conflicting reports in the literature regarding IM administration of alfaxalone resulting in discomfort on injection in cats.10,14,15 Many of these studies evaluated doses of alfaxalone that resulted in a volume of administration as high as 5 ml/cat, 15 which is not feasible to administer IM to a cat. The average volume of alfaxalone administered to cats in this study was much lower, approximately 1 ml/cat. It is likely that alfaxalone was well tolerated by cats in this study owing to the lower volume of administration, as well as the use of the epaxial muscles for injection. Saline was added to the DB syringes so that the total volume of treatment drugs were equal. Had it not been diluted, the average volume of dexmedetomidine administered to cats in this study would have been 0.1 ml/cat. It is important that any drug protocol used for feline blood donation result in minimal pain on injection, otherwise donors may become conditioned to resent restraint for subsequent donations. 4
One cat in the study demonstrated signs consistent with GIU. The cat vomited shortly after receiving DB. This same cat did not demonstrate evidence of GIU with AB. This is not surprising, as vomiting is a reported side effect associated with IM administration of α2 agonists to cats, 7 but not of alfaxalone. The apparent lack of GIU increases the appeal of alfaxalone as part of a sedation protocol for feline blood donation.
The primary findings of this study did not support our hypothesis that venipuncture and blood collection would be easier to perform in cats administered alfaxalone than in cats administered dexmedetomidine. There was no significant difference in the number of venipuncture attempts or total time for blood collection between the two treatment groups. One possible explanation for this is the dose of dexmedetomidine used. The previous study that found phlebotomy difficult under α2 agonist-mediated sedation evaluated medetomidine at a dose of 40–50 μg/kg IM. 4 Dexmedetomidine is the pharmacologically active enantiomer of medetomidine, and is reported to result in comparable sedation at half of the medetomidine dose. 22 The dose of dexmedetomidine used in this study (10 μg/kg) was lower than what would be considered equivalent to the dose of medetomidine used in the previous study. Vasoconstriction is a dose-dependent side effect of dexmedetomidine, 22 and it is possible that the dose used in this study was not high enough to result in enough vasoconstriction to make phlebotomy from the jugular vein difficult.
One possible limitation of this study is that while the investigator who evaluated the quality of sedation and recovery was blinded to the treatment protocols, it is possible that observer-expectancy bias was introduced based on prior knowledge of the differences in effect between the two drugs. Additionally, the failure to detect any significant differences between the two treatment groups may have been influenced by the study’s small sample size.
Conclusions
Several cats in both treatment groups did not achieve adequate sedation to allow for blood donation. Any failure of sedation is not ideal, as cats are often called in for donation as the need for blood products arises. However, the results of this study found that AB is a suitable alternative to DB when used as an IM sedation protocol for cats undergoing blood donation. This combination of AB appears to provide donor cats with a minimally stressful, efficient donation experience with no apparent negative side effects. Further studies are needed to determine if 3 mg/kg alfaxalone in combination with 0.2 mg/kg butorphanol IM would further enhance the quality of sedation in donor cats while continuing to have minimal negative side effects.
Supplemental Material
Feline Blood Donor Sedation Study Follow up owner questionnaire – Supplemental material for Comparison of two intramuscular sedation protocols on sedation, recovery and ease of venipuncture for cats undergoing blood donation
Supplemental material, Feline Blood Donor Sedation Study Follow up owner questionnaire for Comparison of two intramuscular sedation protocols on sedation, recovery and ease of venipuncture for cats undergoing blood donation by Rebecca C Reader, Bruce A Barton and Amanda L Abelson in Journal of Feline Medicine and Surgery
Supplemental Material
Feline Blood Donor Study Recovery Score – Supplemental material for Comparison of two intramuscular sedation protocols on sedation, recovery and ease of venipuncture for cats undergoing blood donation
Supplemental material, Feline Blood Donor Study Recovery Score for Comparison of two intramuscular sedation protocols on sedation, recovery and ease of venipuncture for cats undergoing blood donation by Rebecca C Reader, Bruce A Barton and Amanda L Abelson in Journal of Feline Medicine and Surgery
Supplemental Material
Feline Blood Donor Study Sedation scoring system – Supplemental material for Comparison of two intramuscular sedation protocols on sedation, recovery and ease of venipuncture for cats undergoing blood donation
Supplemental material, Feline Blood Donor Study Sedation scoring system for Comparison of two intramuscular sedation protocols on sedation, recovery and ease of venipuncture for cats undergoing blood donation by Rebecca C Reader, Bruce A Barton and Amanda L Abelson in Journal of Feline Medicine and Surgery
Footnotes
Acknowledgements
The authors would like to thank Jurox Animal Health for the supply of the alfaxalone, and Kristen Barstow BS, CVT, VTS (ECC) for coordination and implementation of the blood donation sessions.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The study was funded by the Companion Animal Health Fund at Tufts University.
Supplementary material
The following files are available:
Feline blood donor study sedation scoring system
Feline blood donor study recovery score
Feline blood donor sedation study follow-up owner questionnaire
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
