Abstract
Objectives
The objective was to describe the use of a bipolar vessel sealant device for complete ovariohysterectomy in cats (ie, removal of both the ovarian pedicle and the uterine body and vessels) and to report on the feasibility of ovariohysterectomy in cats with pyometra.
Methods
Cats with confirmed pyometra and whose owners agreed to the surgical procedure were prospectively included in the study. Ovaries were visualised and the vessel sealant device was used to coagulate and cut the suspensory ligament, the ovarian pedicle and the broad ligament up to the level of the uterine body. Once the uterine body was measured, it was grasped, coagulated and transected just proximal to the cervix using the vessel sealant device when its diameter was <0.9 cm. Immediate postoperative and short-term follow-up were evaluated by clinical examination.
Results
Thirteen cases were initially included between November 2015 and February 2017. Three cases were subsequently excluded because of a uterine body diameter >0.9 cm. Of the 10 cats finally included, all were intact females, with a median age of 2.7 years (range 0.9–9 years). Median weight was 3.7 kg (range 2.6–6.7 kg). The median surgery time was 10.9 mins (range 9.8–15.2 mins). Median uterus diameter was 0.51 cm (range 0.45–0.64 cm) and median skin incision was 4.1 cm (range 3.6–5.1 cm). No complications during the procedures occurred in any patient. All cases were discharged from the hospital 1 day after surgery, without any abnormality. No complications were noted during the postoperative period.
Conclusions and relevance
The findings suggest that the bipolar vessel sealant device used in this study is safe in performing ovariohysterectomy for pyometra in cats, when the uterine body is <0.9 cm in diameter, without short-term complications.
Introduction
Surgical sterilisation of cats is one of the most commonly performed procedures in veterinary surgical practice. Ovariohysterectomy (OHE) can be used as a surgical method of contraception or as a way to prevent or treat diseases associated with the reproductive system, such as pyometra. 1 Pyometra is a disease affecting 2.2% of non-sterilised female cats in their first 13 years of life, with a notable increase in frequency after 7 years. 2 The clinical presentation is similar in dogs and cats, with vulvar discharge, anorexia or inappetence, and a decrease in general health being the most frequently described clinical signs.2–4 The cause of pyometra is identical in dogs and cats: a bacterial infection settling in the uterus under the influence of progesterone.5,6 This hormonal influence is directly related to ovulation in these two species, explaining the lower incidence of pyometra in cats. 6 Indeed, in cats, ovulation induced by coitus exposes cats to a lesser progesterone influence. In both species, OHE surgery remains the treatment of choice considering the vital risks associated with pyometra.
OHE in cats with pyometra is most frequently performed by ventral coeliotomy. Haemorrhage is considered the greatest intraoperative complication during OHE when the suture ligation technique is used.7,8 In our opinion, ligation of the ovarian pedicle and also that of the uterine body are delicate steps in the OHE procedure in cats. Use of a vessel sealant device (VSD) for ovarian pedicles in both dogs and cats is well described and considered as a safe procedure, but it has not been used in vivo to seal and cut the uterine body.9–11 A previous study, using cadaveric uteri of dogs, describes the possibility of using a VSD to safely seal and cut uterine tissue <0.9 cm in diameter. 12 Other studies report a feline uterine body diameter of 0.34 cm and 0.88 cm when classified as normal and pathological, respectively.13,14 Bearing all this in mind, our hypothesis was that VSD could be safely used to seal both feline ovarian pedicles and uterine bodies <0.9 cm in diameter.
Our study describes the use of a VSD for OHE in cats with pyometra, both for the ovarian pedicles and the uterine body (<0.9 cm in diameter) and vessels. The objective of this study was to describe the technique and report its feasibility for OHE in cats with pyometra.
Materials and methods
Cats with confirmed pyometra and that had owner consent for the surgical procedure were prospectively included in the study. The in-house ethical committee approved the study protocol and written owner consent was obtained for each case. Pyometra was suspected after clinical presentation by our board-certified internist. Definitive diagnosis was made by abdominal ultrasound, which was performed in each case by our board-certified radiologist. Blood analysis was carried out in each case before surgery and in the postoperative period if necessary. Medical stabilisation was performed, if needed, before surgery.
Anaesthesia and surgical procedure
Food and water were withheld for, respectively, 8 and 2 h before surgery. As premedication, cats received diazepam (Valium 0.5 mg/kg; Teva) and morphine (0.1 mg/kg; Lavoisier) intravenously (IV). Cats were anaesthetised IV with propofol (Propovet 1–3 mg/kg; Zoetis) given to effect. Maintenance was under inhalation anaesthesia with isoflurane (Vetflurane; Virbac) vaporised in 100% oxygen (200 ml/kg) in a non-rebreathing system. The animals received prophylactic amoxicillin–clavulanic acid antibiotics (Augmentin 20 mg/kg; Glaxosmithkline) IV preoperatively.
All surgeries were performed individually by a first-year surgery resident (J-FB) or a board-certified surgeon (DL).
Cats were routinely prepared for the aseptic surgery procedure and the urinary bladder was manually emptied if necessary. A midline approach was decided in each case. The cat was placed in dorsal recumbency. The incision was started just caudal to the umbilicus and extended 2 cm caudally. The incision was extended during the procedure if necessary. The skin and subcutaneous fat were incised in the midline exposing the rectus abdominis muscles and the linea alba. An incision was made through the linea alba. A spay hook was used to identify and exteriorise the first uterine horn. The ovary was visualised and the bipolar VSD Caiman 12 mm for open surgery instrument (Aesculap), connected to a generator (Lektrafuse RF generator; Aesculap), was used to coagulate and cut the suspensory ligament and ovarian pedicle. The broad ligament was then coagulated and transected with the same device to the level of the uterine body. The second uterine horn was identified at the uterine body and traced cranially to the ovary, and the same procedure was used for this suspensory ligament, ovarian pedicle and broad ligament. Once both uterine horns and associated ovaries were exteriorised, uterine body circumference was measured with a ribbon, a few mm cranial to the cervix. A sterilised measuring suture ribbon was created to measure the uterine body perimeter intraoperatively. A mark was created to determine a maximum diameter by measuring the uterine body circumference. When the measurement was <2.8 cm, corresponding to a diameter <0.9 cm, the uterine body was grasped, coagulated and cut just proximal to the cervix using the VSD (Figure 1). The sealing cycle of the VSD was applied 2–3 times across the same location on the uterine body to achieve complete sealing of tissue. The abdominal wall incision and skin incision were both closed using a 3-0 monofilament suture material in a simple continuous pattern.
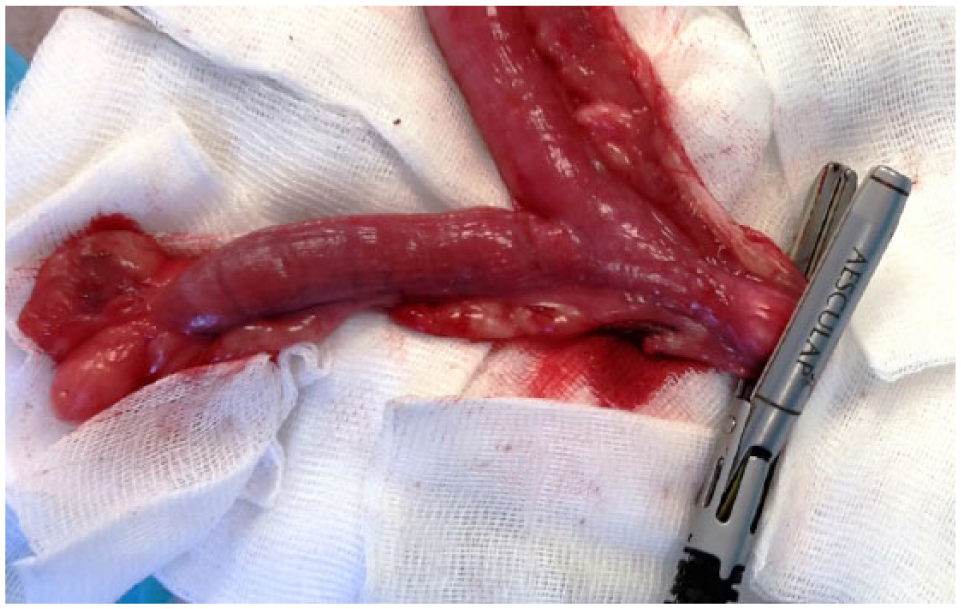
Uterine body, uterine horns and ovaries during the ovariohysterectomy procedure performed with a bipolar vessel sealant device
Operative time recorded for all surgeries was the time elapsed between the first incision and the placement of the last suture. Intraoperative complication was also recorded. Skin incision was measured at the end of the procedure.
Analgesia was provided with morphine (0.1 mg/kg; Lavoisier) injected IV every 4–6 h, from 4 h to 24 h postoperatively. Oral amoxicillin–clavulanic acid antibiotics (Kesium 12.5 mg/kg [Ceva] q24h for 6 days) and meloxicam (Metacam 0.1 mg/kg [Boehringer] q24h for 5 days) in cases without blood renal abnormalities were administered from 24 h postoperatively. Clinical examination was carried out during follow-up at 7 days postoperatively to assess the skin healing and 2 weeks after surgery to remove the cutaneous suture. Postoperative complications such as haemorrhage, peritonitis and abdominal wall closure abnormality, that eventually occurred during follow-up, were also recorded.
Results
Thirteen cases were initially included in the protocol between November 2015 and February 2017. Eight cases showed vulvar discharge at clinical examination and all of them were definitively diagnosed by abdominal ultrasound. Three cases were excluded perioperatively because of a uterine body diameter of >0.9 cm. Finally, 10 cats completed the study. All the cats were intact female domestic shorthairs.
Concerning the three cases excluded owing to the large uterus diameter, median age was 3.2 years (range 2.6–3.2 years), median weight was 4.7 kg (range 4.4–5.6 kg) and median uterus diameter was 1.04 cm (range 0.97–1.12 cm).
Concerning the cats included in this study, median age was 2.7 years (range 0.9–9 years) and median weight was 3.7 kg (range 2.6–6.7 kg). Median uterus diameter was 0.51 cm (range 0.45–0.64 cm), median surgery time was 10.9 mins (range 9.8–15.2 mins) and median skin incision length was 4.1 cm (range 3.6–5.1 cm). No complication during procedure occurred in any cat. All cases were discharged from the hospital 1 day after the surgery, without any abnormality. Clinical follow-up at 7 and 14 days did not show any problems. All results are reported in Table 1.
Results in detail
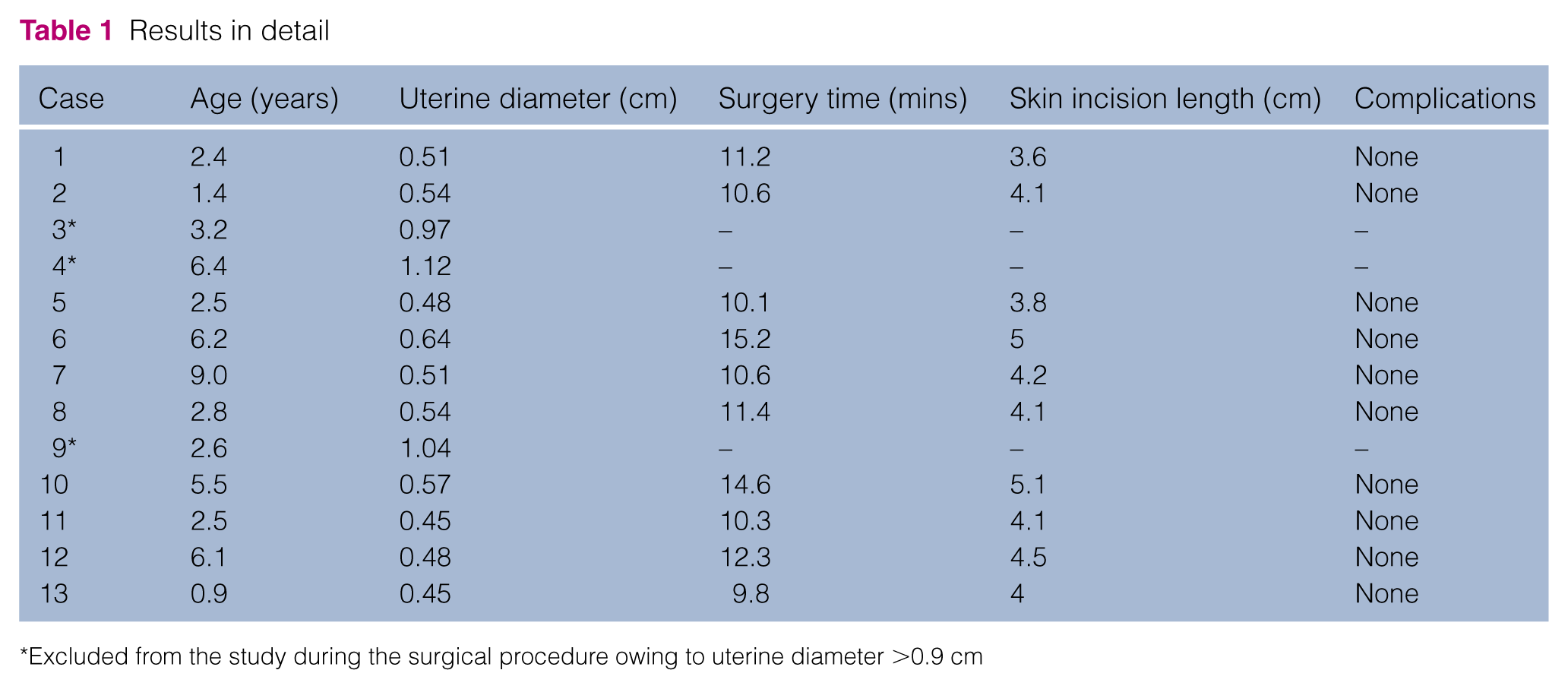
Excluded from the study during the surgical procedure owing to uterine diameter >0.9 cm
Discussion
This study investigated the feasibility of using a 12 mm bipolar VSD to perform OHE for the surgical treatment of pyometra in cats with a uterine body diameter of <0.9 cm. The skin incision length was relatively short and surgery was performed quickly, without any preoperative or postoperative complications.
Although the initial skin incision length in our study was 2 cm, extension was required in all cats to a median final incision length of 4.1 cm (range 3.6–5.1 cm). These values are comparable to those previously reported for midline OHE in cats, showing that the use of the VSD did not require greater access than a traditional three-clamp technique.9,15–17 Following completion of this study, we now recommend an initial incision length of 4 cm for pyometra in cats, to avoid the need to extend the incision during the procedure.
Surgery time was at the lower end of a range previously reported for midline OHE in cats of 8.9–21 mins for an experienced surgeon and 43 mins for a veterinary student.9,15–17 Our surgeries were carried out by experienced surgeons, but measuring the circumference of the uterus or realising photographic illustrations increased the total surgical time. In our opinion, using a VSD to seal and cut ovarian pedicles, broad ligament and uterine body is the major reason why the time of surgery is shorter with this technique. Another explanation could be the reduction of surgical procedures and changes of instruments during surgery. Indeed, the intra-abdominal surgery can be performed using only DeBakey forceps and the VSD instrument.
There were no complications in the immediate perioperative period or during short-term follow-up in our case series. Other studies have also reported a low complication rate after conventional OHE, using or not using a VSD to seal and cut the ovarian pedicles.7,9,16 Haemorrhage has been described by some authors as the most common complication associated with OHE. In studies of OHE in dogs, intraoperative haemorrhage was most commonly associated with ovarian pedicle rupture after manipulation or insufficient knot-tying technique. 18 Although complications concerning ovarian pedicles in cats should be lower than in dogs, postoperative death due to haemorrhage occurred in approximately 1 in 1500 cats undergoing surgical sterilisation.19,20 Manipulation of the ovarian pedicle and problems related to the knots, such as slipping or loosening, are avoided using our surgical technique. No peritonitis or stump abscesses were reported during the postoperative follow-up in this study; however, our follow-up time was short and longer follow-up information is lacking. Further studies assessing long-term stump adhesions and infections would be useful.
Using a VSD for OHE in cats is a simple and effective technique, without foreign material left in the patient. This technique is also faster but more expensive than ligatures for OHE in cats. Use of a VSD has also been reported for laparoscopic-assisted OHE, which is considered as a minimally invasive technique with a smaller skin incision; however, surgical time is longer and complication rates are higher.7–9 The use of a VSD in open surgery is therefore recommended as a good compromise by the authors for OHE for pyometra in cats.
Regarding the VSD equipment used in our study, numerous technical characteristics could be considered as advantages for this kind of surgery. The VSD forceps consist of a 12 mm instrument with a sealing length of 50 mm, a cutting length of 46 mm, a 360° shaft rotation and a pistol-type handle. 21 The distal extremity of the forceps has a 80° orientation that increases range of motion. Quality and reliability of blood vessel sealing strongly depends on the pressure in the instrument’s jaws.21,22 An evaluation of this VSD showed even pressure distribution with only a slight maximum pressure at the middle of the jaw length, as was shown with pressure measurements in the instrument jaws, owing to the hinged jaw. 21 Only the 5 mm forceps were evaluated, but, in our opinion, the design and principle of use is the same for the forceps used in this study. 21 All this could explain the short time of surgery and the correct tissue sealing.
The VSD had to be applied 2–3 times across the same location on the uterine body in our study to achieve a complete seal of tissue. Such use may have influenced the strength of the seal described because of local heat production, compared with a single sealing cycle use.12,21 Nevertheless, the average measured thermal spread beyond the instrument jaws was <1 mm for the corresponding 5 mm VSD. 21 We suspect that this thermal spread is relatively minimal for the forceps used in our study and that VSD could manifestly be used safely for surrounding soft tissues, even with multiple sealing cycle use.
One of the limitations of our study was the low number of cases included. The first goal of this study was to describe the technique and to show its clinical application. Another study with more clinical cases to report peroperative and postoperative complications could be interesting. Another limitation was the absence of a control group to compare, for example, a clamp-ligature technique or a tissue sealing technique. A comparative study between this technique and a conventional OHE technique with the same surgeon could be interesting in order to compare operative time, surgical complication and cutaneous incision length, notably due to personal variation of these parameters. An investigation of the long-term complications, such as adhesions to the stump, and comparison with a suture ligation technique group could also be interesting. Another limitation of the study was the inclusion of only cases with uterine bodies of <0.9 cm in diameter. This limit was applied because of reported uterine tissue sealing up to 0.9 cm. 12 As pyometra in cats could lead to a uterine body >0.9 cm in diameter, an experimental study of bipolar VSD for sealing bigger uterine bodies could be interesting before clinical application.
Conclusions
The findings of the present study suggest that the bipolar VSD used in this study is safe to use in OHE for pyometra in cats, when the uterine body is <0.9 cm in diameter, without short-term complications.
Footnotes
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
