Abstract
A 7-month-old, female, domestic shorthair, indoor/outdoor cat on the island of St Kitts was presented to the Veterinary Teaching Hospital at Ross University School of Veterinary Medicine as part of a student training spay–neuter program. Observation of diarrhea prompted a double centrifugation fecal analysis. Ova of Mammomonogamus species, in addition to Ancylostoma species, Trichuris species and Platynosomum species, were found. Mammomonogamus ierei is a parasitic nematode found on many Caribbean islands for which treatment is not well documented. Five days of fenbendazole (50 mg/kg bodyweight) was administered, and fecal analyses gave negative results for Mammomonogamus species eggs 1 week after the last fenbendazole treatment.
Case Report
A 7-month-old, female, domestic shorthair, indoor/outdoor cat presented to the Ross University School of Veterinary Medicine (RUSVM) Veterinary Teaching Hospital (VTH) for an initial history, physical examination, hemogram and serum biochemical profile before being included in a student training spay–neuter program. The owner had acquired the cat 6 months previously. Two weeks prior to the visit, the cat had been lethargic, and was coughing and sneezing. More recently, the cat had no evidence of coughing or sneezing. During the initial examination, all vital signs were within normal limits, and there was no evidence of respiratory signs. Three days later, the cat returned to the VTH for preoperative assessment. During this second examination, the cat appeared healthy, and there were no signs of respiratory or other infections. However, as part of a drop-off service, the cat remained in the clinic for several hours. During this time, observation of moderate-to-severe diarrhea prompted a fecal analysis. For analysis, 2 g of feces were mixed with water in a 15 ml centrifuge tube and centrifuged for 5 mins at 600 g with a swing-head centrifuge. The supernatant was poured off and Sheather’s sugar flotation solution (specific gravity 1.27) was mixed with the sediment. A coverslip was placed on the centrifuge tube, centrifuged as described previously and allowed to sit for 10 mins before removing the coverslip and placing on a slide to count the ova.1,2 All ova seen on the coverslip were identified, counted, recorded and divided by two to obtain the eggs per gram of feces (EPG).1,3 Results were positive for ova of Ancylostoma species, Trichuris species, Platynosomum species and Mammomonogamus species. While no specific test for Giardia duodenalis was conducted, it also was suspected as a potential cause of the diarrhea.
Fenbendazole (FBZ) (Panacur 10% oral suspension; Intervet) at 50 mg/kg bodyweight (BW) daily for 5 days was chosen as treatment as benzimidazoles have been used to treat Mammomonogamus species in other host animals, is effective against Ancylostoma species and is registered for use in cats. For clinical infection in cats, the product label recommends 50 mg/kg BW for 3 days; however, two additional days of treatment were administered owing to suspicion of a Giardia infection. 4 The first dose was administered the afternoon after the spay procedure. The cat was kept overnight at the VTH, and several minutes of repetitive sneezing was observed the following morning. However, no other respiratory or systemic signs were observed, and the cat was sent home with instructions to continue administering the FBZ. Follow-up fecal samples (Table 1) were analyzed periodically, from the start of treatment to 15 days after administration of the last dose of FBZ, to assess treatment efficacy. For all fecal analyses, the EPG was calculated for Mammomonogamus species ova; for other parasite ova, the EPG was calculated pretreatment, and on days 7 and 15 post-treatment.
Results of serial fecal examinations
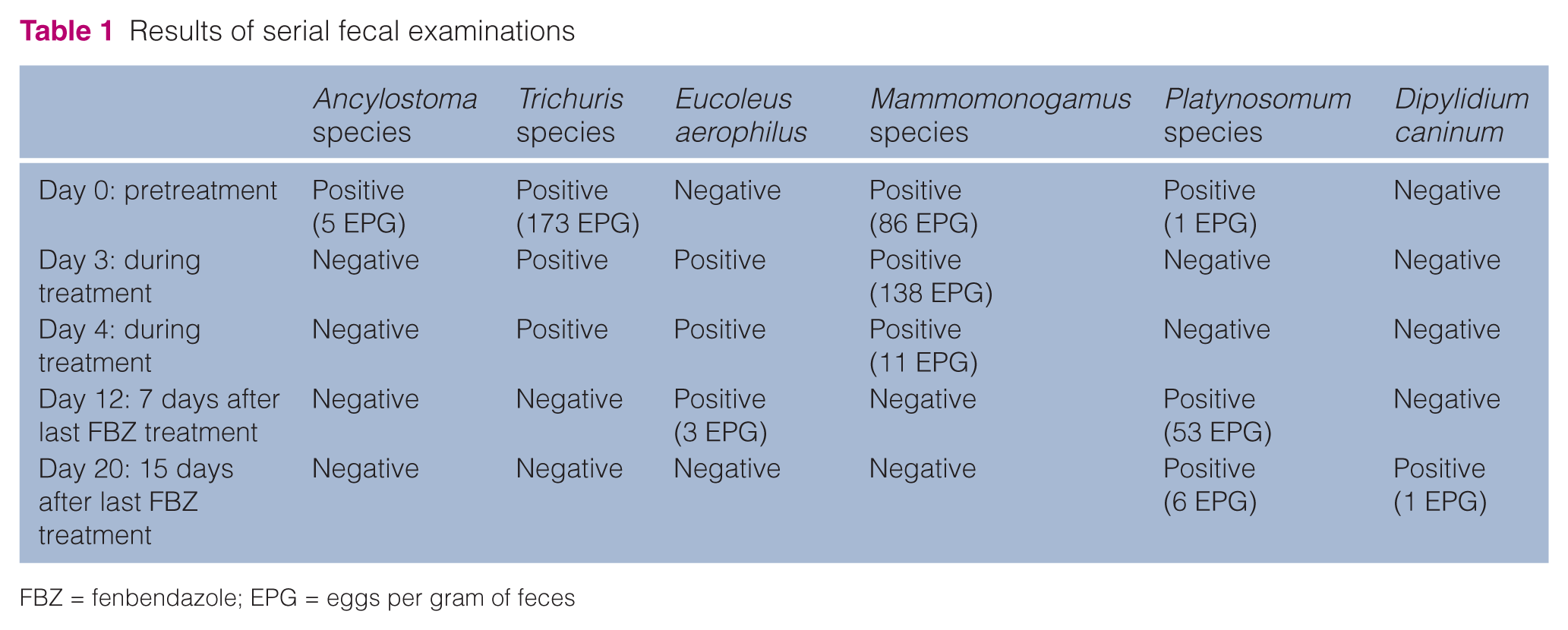
FBZ = fenbendazole; EPG = eggs per gram of feces
Ancylostoma species and Platynosomum species ova were absent on the third day after the treatment was initiated, but ova from Trichuris species, Eucoleus aerophilus and Mammomonogamus species (Table 1) were present. By day 4 of FBZ treatment, the number of Mammomonogamus ova had decreased from 138 EPG to 11 EPG; the egg count was negative by 7 days post-treatment. After FBZ treatment was completed, the owner noted that the cat’s feces appeared firmer. No further coughing or sneezing was observed.
Mammomonogamus (Syngamus) species are parasitic nematodes commonly known as gapeworms. Two species have been reported in cats: Mammomonogamus auris and Mammomonogamus ierei. M ierei is found on many of the Caribbean islands, and Mammomonogamus species eggs have been reported in the feces of 45% of feral cats on St Kitts.5,8 One male and one female parasite are permanently joined in copulation in the nares and nasopharynx of cats. Because the female’s vulva is in the middle of her body and because the males are shorter, a distinctive Y-shape formation occurs. The female is a red color and approximately 20 mm in length, while the male is more of an orange-red or brown-red color, and approximately 5–7 mm in length. 7 Our patient had a brief history of coughing and sneezing, which would fit with infection by M ierei. 8 Based on the history of respiratory signs and the fact that no other Mammomonogamus species have been identified in cats in the Caribbean, it is likely that this cat was infected with M ierei. Ova of Eucoleus aerophilus were not identified until after treatment with FBZ was started. While E aerophilus infection might have contributed to the reported coughing1,3 obtained in the history, most infections are asymptomatic. In addition, such infections are usually in the tracheobronchial tree and normally would not cause sneezing. The low EPG would also suggest that the infection level was not severe enough to have caused significant clinical signs.
Little is known about the life cycle of Mammomonogamus species, although the nematodes are similar to those in the genera Syngamus, in which eggs are coughed up, swallowed and passed in feces. M ierei eggs are ovoid and have a clear shell with irregular transverse striations. They are similar in appearance to eggs of Ancylostoma species, which may be one reason why so few reports of Mammomonogamus species in cats exist. 8 Mammomonogamus species eggs are larger and thicker, approximately 49.5 × 92.0 µm,3,7–10 than Ancylostoma species eggs, but without measuring the size, it is difficult to distinguish between the two ova. Outside the host, Mammomonogamus species eggs undergo development into infective larvae. 6
The route of infection in cats has not yet been determined. Based on unsuccessful attempts of experimental infections with eggs and larvae, it is likely that a paratenic or intermediate host, such as an earthworm, arthropod or snail, is required.7,9 Because M ierei may be related to the species that infects ruminants, 9 Mammomonogamus laryngeus, and because this cat lived on the same property as two sheep, the feces of the two sheep were analyzed and were negative for Mammomonogamus species ova. An alternative source of the infection could have been the 20 cats living next door in a semi-feral colony. However, it was not possible to obtain fecal samples from those cats making it difficult to eliminate or confirm them out as a source of infection.
The pathogenicity of M ierei is unclear. Clinical signs of infections in cats, if any, have not been confirmed. 9 However, Cuadrado et al 8 found that chronic inflammation of the nasopharynx, producing mucoid nasal discharge and sneezing episodes, is possible. Coughing has also been reported in humans that have M laryngeus infections. 6 Infected humans have been cured of the infection if the worms are coughed up or removed manually or via bronchoscopy. The cat in this case had a history of coughing and sneezing 2 weeks prior to initial examination. The repetitive sneezing on the day after the first dose of FBZ was administered could have been related to death of the worms. The worms also could have been sneezed out or coughed up without detection. However, based on the rise in EPG noted on day 3 of treatment, it is more likely that dead or injured worms were swallowed and their eggs released in the gastrointestinal tract. The decrease in count by day 4 would also fit this scenario.
The proper treatment for this parasite is unknown. No anthelmintic has been approved for use against this worm. Thiabendazole, mebendazole and ivermectin have been effectively used to treat Mammomonogamus species infections in cattle and humans.6,9–11 We chose to use FBZ as it is a standard treatment in the RUSVM clinic and affordable for most of our clients. However, as ivermectin is an effective treatment in cattle, potential alternative treatments to FBZ for Mammomonogamus species infections in cats include those containing macrocyclic lactones (eg, ivermectin, moxidectin, milbemycin oxime). Based on the results of the follow-up fecal examinations, we believe that FBZ at 50 mg/kg BW daily for 5 days was effective in eliminating the Mammomonogamus species infection. Diarrhea, sneezing and coughing were not noted by the cat’s owner after treatment. This, in conjunction with the post-treatment fecal examinations, indicate that the other parasitic infections were treated effectively. Further fecal collections could have been beneficial in confirming efficacy of treatment, but proved challenging as the cat was an indoor/outdoor cat. The Dipylidium and Platynosomum species infections were subsequently treated with praziquantel.
Conclusions
This case report highlights the importance of routine fecal examinations in cats. This cat appeared healthy during its first visit and the preoperative visit for the RUSVM student spay–neuter program. If not for the diarrhea observed while the cat was waiting for collection by the owner, the internal parasitic infections would not have been diagnosed. Owners of indoor/outdoor cats might find it challenging to collect feces for analysis. Keeping the cat in the clinic before or after examination, or fecal collection by rectum could be alternatives to having the owner bring in feces. Alternatively, deworming cats on a routine basis (eg, every 3–4 months) could decrease the risk of infection.
Footnotes
Acknowledgements
We thank Charles Pemberton for performing fecal analyses and Jerome Davis for collection of samples.
Conflict of interest
The authors do not have any potential conflicts of interest to declare.
Funding
The authors received no specific grant from any funding agency in the public, commercial or not-for-profit sectors for the preparation of this case report.
