Abstract
Overview:
Leishmania infection is less known in cats than in dogs and humans; felids were traditionally considered a resistant species, and canids as the main reservoir. Only sporadic cases of feline disease have been reported worldwide, mainly caused by L infantum. Epidemiological investigations have confirmed, however, that feline infections are not rare and that disease occurrence might be underestimated in endemic areas.
Infection:
Cats are infected by the same Leishmania species that infect dogs and humans in tropical and subtropical areas worldwide. Sand fly vectors take blood meals from cats and are competent vectors for L infantum, as shown experimentally.
Disease signs:
Skin lesions (ulcerative, crusty, nodular or scaly dermatitis) are the most frequent clinical manifestations and sometimes the only findings on physical examination. Lymph node enlargement, weight loss, ocular involvement (nodular blepharitis, uveitis, panophthalmitis), decreased appetite, chronic gingivostomatitis and lethargy are the most frequent non-cutaneous findings, alone or in combination.
Diagnosis:
Direct confirmation can be obtained by cytology, histology, isolation or polymerase chain reaction (PCR) on samples of skin, lymph nodes, blood or any affected tissue. Serology using a validated immunofluorescence test, ELISA, direct agglutination or Western blot has been used to assess infection frequencies.
Disease management:
Little information is available about treatment with follow-up reports. Long-term administration of allopurinol (10–20 mg/kg q12h or q24h) is usually clinical effective. Vaccines are licensed for dogs only.
Agent
After malaria and lymphatic filariasis, leishmaniasis is the third most important vector-borne disease of humans; it is caused by several Leishmania species, most of zoonotic concern. 1 In veterinary medicine, canine leishmaniosis caused by L infantum is of primary interest, because dogs are the main reservoir of the parasite for humans, and management of the canine disease may be challenging. 2
Cats are naturally infected by the same Leishmania species that affect dogs and humans in tropical and subtropical areas worldwide: L infantum in the Mediterranean basin, Iran and Brazil; L mexicana in Texas, USA; L braziliensis in Brazil and French Guiana; L amazonensis in Brazil; L venezuelensis in Venezuela.3–10
The susceptibility of cats has been confirmed by experimental studies [

Life cycle and transmission
Leishmania species are protozoan parasites, the natural history of which involves two hosts: the phlebotomine sand fly and a vertebrate. The vector harbours flagellated extracellular promastigote forms and transmits them to a vertebrate host; there, the parasite changes into the amastigote form that is able to survive and replicate in intracellular vacuoles within macrophages. Haematophagous female sand flies transmit the promastigotes or may take up amastigotes from an infected vertebrate host.
There is no evidence that ticks and fleas are involved in natural Leishmania transmission.1,2 The risk of transmission in the absence of sand flies is negligible, but transplacental infection occurs as a rare event in both dogs and humans.1,2 Venereal transmission is a potential means of infection. 13 Other types of direct transmission have been suggested to explain the spread of the infection among kennel dogs in the USA in the absence of sand fly vectors.1,2 The risk of transmission by blood transfusion is important for humans and dogs in endemic areas.1,2,14
Many studies have demonstrated that sand flies take blood meals from cats; experimentally, sand flies have been found to be competent vectors for L infantum in cats [
Epidemiology
Leishmaniosis caused by L infantum is an emerging disease globally.1,2 Using molecular diagnostic techniques on dogs in endemic areas, it was shown that the prevalence of the infection is much higher than that of the disease.
17
The same is true for people: in some endemic areas, latent infections approach 30% of the population, based on a positive leishmanin skin test.
14
Leishmaniosis in cats is sporadically reported worldwide, usually from the same areas where the disease occurs in dogs or humans.
3
Cases have been seen in Switzerland, in cats imported from Spain; increased pet movement throughout Europe will lead to more disease, including in non-endemic areas [
Epidemiological studies have been performed during the past 15 years in endemic areas using serological (immunofluorescence, ELISA, Western blot, direct agglutination) and/or parasitological methods (cytology, immunohistochemistry, PCR). The rates of infection vary widely, which may be due to the methodology used, the geographic area and population under study. Positive blood PCR rates range between 0.43 and 61% of the population tested, and antibody prevalence between 3 and 59%. 3
Pathogenesis
Disease development is influenced by immunological factors, which are linked to the complex genetic background of the hosts, as demonstrated by studies in laboratory animals, dogs and humans. 2 In people, L infantum can induce anything between a local skin lesion and a severe visceral disease. The latter form is the typical presentation in immune-incompetent patients. 14 In dogs, leishmaniosis is a multisystemic disease with a wide spectrum of severity that reflects the balance between the protective cell-mediated and the non-protective humoral immune response. In both humans and dogs there is a dynamic range from subclinical infection to self-limiting mild and non-self-limiting severe disease.1,2
In all host species, macrophages play a central role in the control of the infection. Cytokines such as IFN-γ, IL-2 and TNF-α, secreted by activated T cells, stimulate intracellular killing of Leishmania amastigotes by macrophages. The presence of Leishmania-infected macrophages is usually associated with a granulomatous inflammatory reaction. 2 Lymphoid hyperplasia is also common. A massive antibody response is responsible for immune complex deposition in the kidney, with glomerulonephritis and subsequent renal failure.1,2
Histopathology of feline skin lesions mainly shows a diffuse granulomatous dermatitis with macrophages containing many Leishmania parasites, or a granulomatous perifolliculitis and lichenoid tissue reaction/ interface dermatitis, with a lower parasite load.19,20 Granulomatous inflammation has also been seen in the liver and kidney. 20
Epidemiological studies have shown that Leishmania infection of cats is more common than the associated disease; cats may remain PCR and antibody positive for a long time. 3 Cats may be more resistant than dogs to developing disease.
Clinical signs
Canine leishmaniosis is usually chronic and progressive, with an incubation period lasting for months or even years. Any tissue or organ may be involved, but skin lesions are most suggestive, and renal disease is most important prognostically. 1
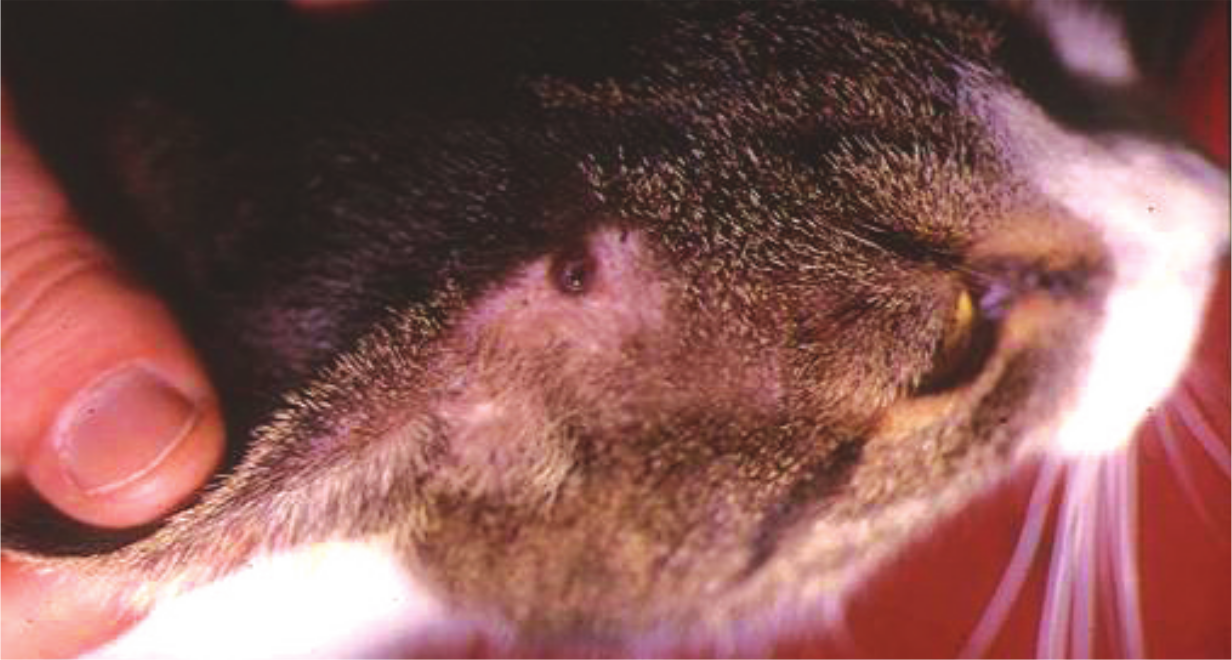
Feline leishmaniosis caused by L infantum has been documented mainly in the past 20 years in Europe and Brazil. 3 Cases have been reported in cats of all ages, almost all domestic shorthair, with no gender predilection. Skin lesions are the most frequent clinical manifestation, and sometimes the only finding on physical examination. Ulcerative, crusty, nodular or scaly dermatitis is found mainly on the head and neck (Figures 1 and 2), less often on the trunk and legs. Pruritus is usually absent; alopecia or a poor coat condition are reported. Lymph node enlargement, weight loss, ocular involvement (nodular blepharitis, uveitis, panophthalmitis), decreased appetite, chronic gingivostomatitis and lethargy are the most frequent non-cutaneous findings. Dehydration, pale mucous membranes, vomiting, hepatomegaly, fever, jaundice, polyuria/polydipsia, spleen enlargement, nasal discharge, recurrent abortion and dyspnoea are also found, although less often.

L infantum-associated ulcerative dermatitis in a cat. Courtesy of Maria Grazia Pennisi
L infantum-associated haemorrhagic nodule in a cat. Courtesy of Maria Grazia Pennisi
Information on clinicopathological abnormalities is scarce; in a few cases followed up until death or euthanasia, glomerular disease and chronic renal failure have been seen to develop [
Data from complete blood counts and serum protein electrophoresis are available but the results may have been influenced by concurrent disease as well as retroviral infection. Various haematological abnormalities have been described in three cats suffering from pancytopenia; in one of them, a retrovirus-negative patient with myelofibrosis, 4% of the circulating neutrophils contained Leishmania parasites.
22
Hyperglobulinaemia and gammopathy are found in most investigated cases [
Immunity
Leishmania immunity is complex. In the dog, a susceptible species, protective immunity against L infantum is CD4 T cell mediated, and the release of gamma-interferon, IL2 and TNF-α is associated with anti-Leishmania activation of macrophages. A combination of high antibody levels and a reduced cellular, mixed Th1 and Th2 response is found in dogs developing the disease.1,2
All sick cats possess specific antibodies, and hyperglobulinaemia is often found. As reported for dogs, Leishmania PCR-positive healthy cats may be seronegative for anti-Leishmania antibodies.3,23
Infection experiments with L braziliensis have shown that the development of skin lesions precedes antibody appearance, and seroconversion occurs when the lesions are healing. 12
An association between feline immunodeficiency virus (FIV) and L infantum infections was found in endemic areas. Most cats developing clinical signs are suspected to have an impaired immune system because of concurrent FIV infection, FIV plus feline leukaemia virus (FeLV) infection, cancer (squamous cell carcinoma), diabetes mellitus, autoimmune disease (pemphigus foliaceus), and treatment with corticosteroids or other immunosuppressive drugs [
Diagnosis
The diagnosis can be accomplished by parasitological (cytology, histology, PCR, isolation) and serological methods (immunofluorescence test, ELISA, direct agglutination, Western blot). In most feline cases where cytology, isolation and PCR were performed, they confirmed the diagnosis obtained using lymph node, skin, bone marrow or blood samples (Figure 3). Ocular disease caused by L infantum was diagnosed by histology after enucleation of the affected eye. On post-mortem examination, parasitological evidence of infection was also obtained from samples of spleen, liver, kidney, pancreas and gastrointestinal organs. 3 Immunohistochemistry has been used on skin biopsies.19,20

Lymph node smear from a cat, showing Leishmania amastigotes in a macrophage (MG-G stain; x64 objective). Courtesy of Maria Grazia Pennisi
Serological tests for leishmaniosis are not commercially available. Recently, immunofluorescence testing has been validated for use in feline samples [
Treatment
The available information on treatment is mostly based on single case reports, not always with an appropriate follow-up (
Prevention
Information is not available on the prevention of feline leishmaniosis. In dogs, the disease is prevented by means of application of repellent agents against sand flies and, more recently, also by vaccination. 1


Footnotes
Key Points
Funding
The authors received no specific grant from any funding agency in the public, commercial or not-for-profit sectors for the preparation of this article. The ABCD is supported by Merial, but is a scientifically independent body.
Conflict of interest
The authors do not have any potential conflicts of interest to declare.
