Abstract
The Cosmetic Ingredient Review (CIR) Expert Panel (Panel) assessed the safety of 14 tocopherols and tocotrienols and concluded these ingredients are safe as used in cosmetics. The tocopherols are reported to function in cosmetics as antioxidants or skin-conditioning agents; in contrast, tocotrienols are not reported to function as an antioxidants in cosmetics but as a light stabilizer, oral care agent, or skin-conditioning agent. The Panel reviewed the new and existing animal and clinical data to determine the safety of these ingredients and found it appropriate to extrapolate the existing information to conclude on the safety of all the tocopherols and tocotrienols.
Introduction
In 2002, the Cosmetic Ingredient Review (CIR) Expert Panel (Panel) published a review on tocopherol, the component most commonly associated with vitamin E. As a part of its procedures, the Panel rereviews the conclusion of prior safety assessments, 15 years after the issuance of a final report. Although it had not been 15 years since the original report on the tocopherols was published, the Panel opened a rereview of the tocopherols to include tocotrienols (a 2013 priority) as well as a few additional tocopherols that were not a part of the original report. In the original safety assessment of tocopherols, the Panel concluded that the following ingredients are safe as used in cosmetics
1
: Tocopherol Tocopheryl acetate Tocopheryl linoleate Tocopheryl linoleate/oleate Tocopheryl nicotinate Tocopheryl succinate Dioleyl tocopheryl methylsilanol Potassium ascorbyl tocopheryl phosphate Tocophersolan
In this study, the Panel stated the following cosmetic ingredients should be included in this safety assessment: Tocotrienols Ascorbyl tocopheryl acetate Ascorbyl tocopheryl maleate Tocopheryl phosphate Sodium tocopheryl phosphate
All relevant published literature that has become available since the CIR safety assessment was issued on tocopherols, and all relevant literature on tocotrienols and the tocopherols that were proposed for addition to this report, are presented in this review. For the purpose of this review, relevant literature refers to that which applies to the safety of tocopherols and tocotrienols as used in cosmetics. Health claims have been made for vitamin E; that information is not relevant to the safety of vitamin E in cosmetics, and therefore, the studies investigating those claims are not included in this review.
Tocopherol and tocopheryl acetate are generally recognized as safe (GRAS) food ingredients. Because systemic exposure resulting from cosmetic use is not expected to exceed the levels found safe for food use, oral toxicity data on tocopherol and tocopheryl acetate are not included in this review.
Some of the ingredients included in this report are ascorbyl-containing compounds. In 2005, the Panel concluded that
Chemistry
Definition and Structure
Tocopherols and tocotrienols are amphiphilic lipids that share in common a substituted chromanol core (Figure 1).
3
Together, the tocopherols and tocotrienols comprise vitamin E, differing structurally by substitution on the polar, chromanol core by either a lipophilic saturated, phytyl side chain or an unsaturated, isoprenoid (geranylgeranyl) side chain, respectively. Tocopherols have 3 stereocenters (*) which are all of the R configuration (
In addition to possible stereochemistries and double-bond geometries, vitamin E comprises 8 naturally occurring structural analogs: 4 tocopherols (α-, β-, γ-, and δ-analogs) and 4 tocotrienols (α-, β-, γ-, and δ-analogs; Figure 2). 4 These analogs differ structurally by the presence and placement of additional methyl groups around the aromatic ring of the chromanol core. All 4 of the tocopherol analogs are listed in the definition for tocopherol. According to the definition for the cosmetic ingredient, however, tocotrienols only contain the α-, γ-, and δ-analogs (ie, no β-tocotrienol).
Further substituted tocopheryl ingredients, including tocopheryl acetate, tocopheryl linoleate, tocopheryl linoleate/oleate, tocopheryl nicotinate, tocopheryl succinate, dioleyl tocopheryl methylsilanol, potassium ascorbyl tocopheryl phosphate, tocophersolan, ascorbyl tocopheryl acetate, ascorbyl tocopheryl maleate, tocopheryl phosphate, and sodium tocopheryl phosphate, involve ester linkages of the corresponding acid to the free alcohol of tocopherol (eg, tocopheryl nicotinate is the tocopheryl ester of nicotinic acid; Figure 3).
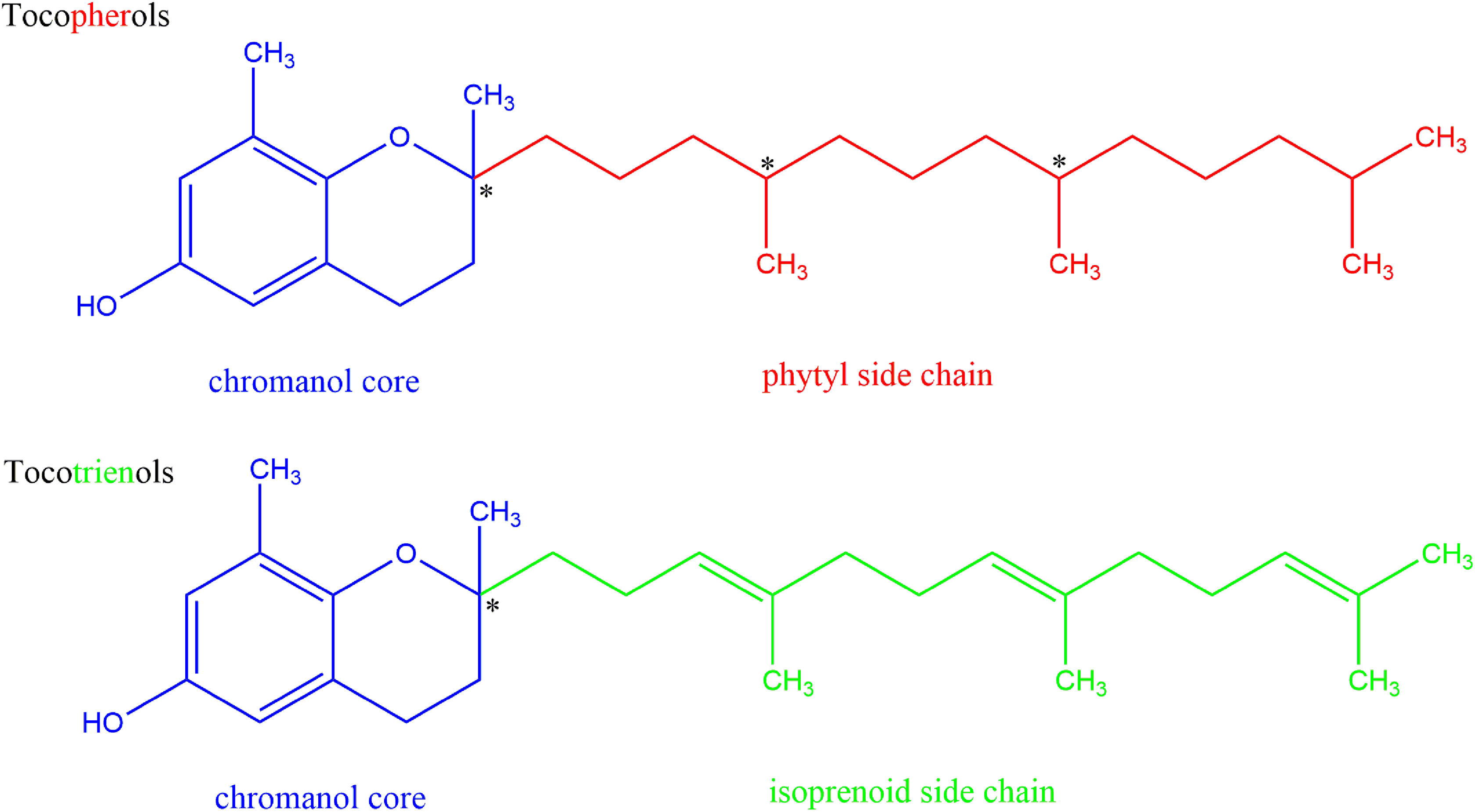
Tocopherols and tocotrienols.
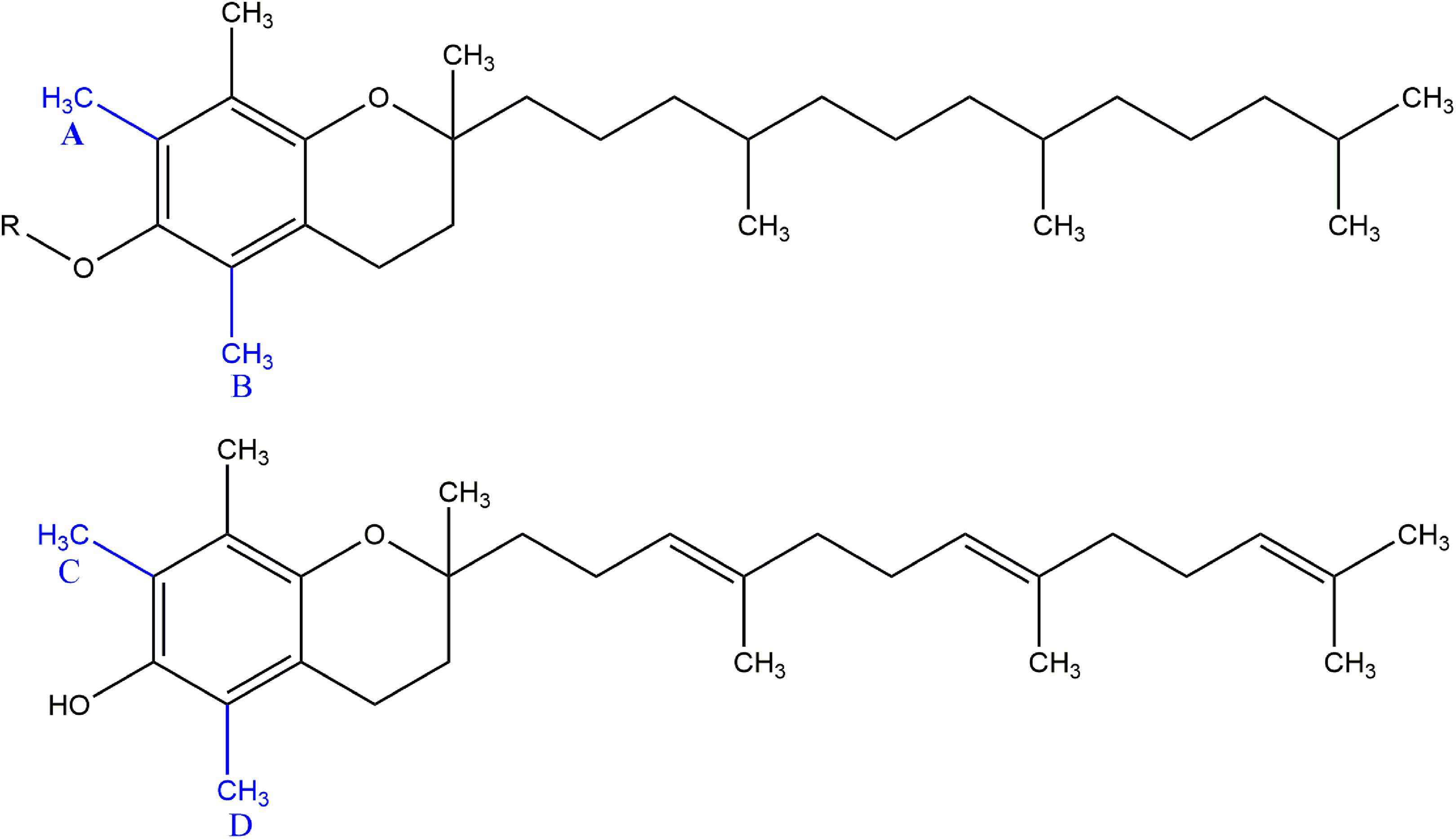
α-, β-, γ-, and δ-analogs—wherein methyl groups A and B are present in the case of α-tocopherol, only B for β-tocopherol, only A for γ-tocopherol, and neither for δ-tocopherol—wherein methyl groups C and D are present in the case of α-tocotrienol, only D for β-tocotrienol, only C for γ- tocotrienol, and neither for δ- tocotrienol—wherein R is hydrogen or, in the case of the tocopheryl ingredients, constitutes together with the attached oxygen, an ester.
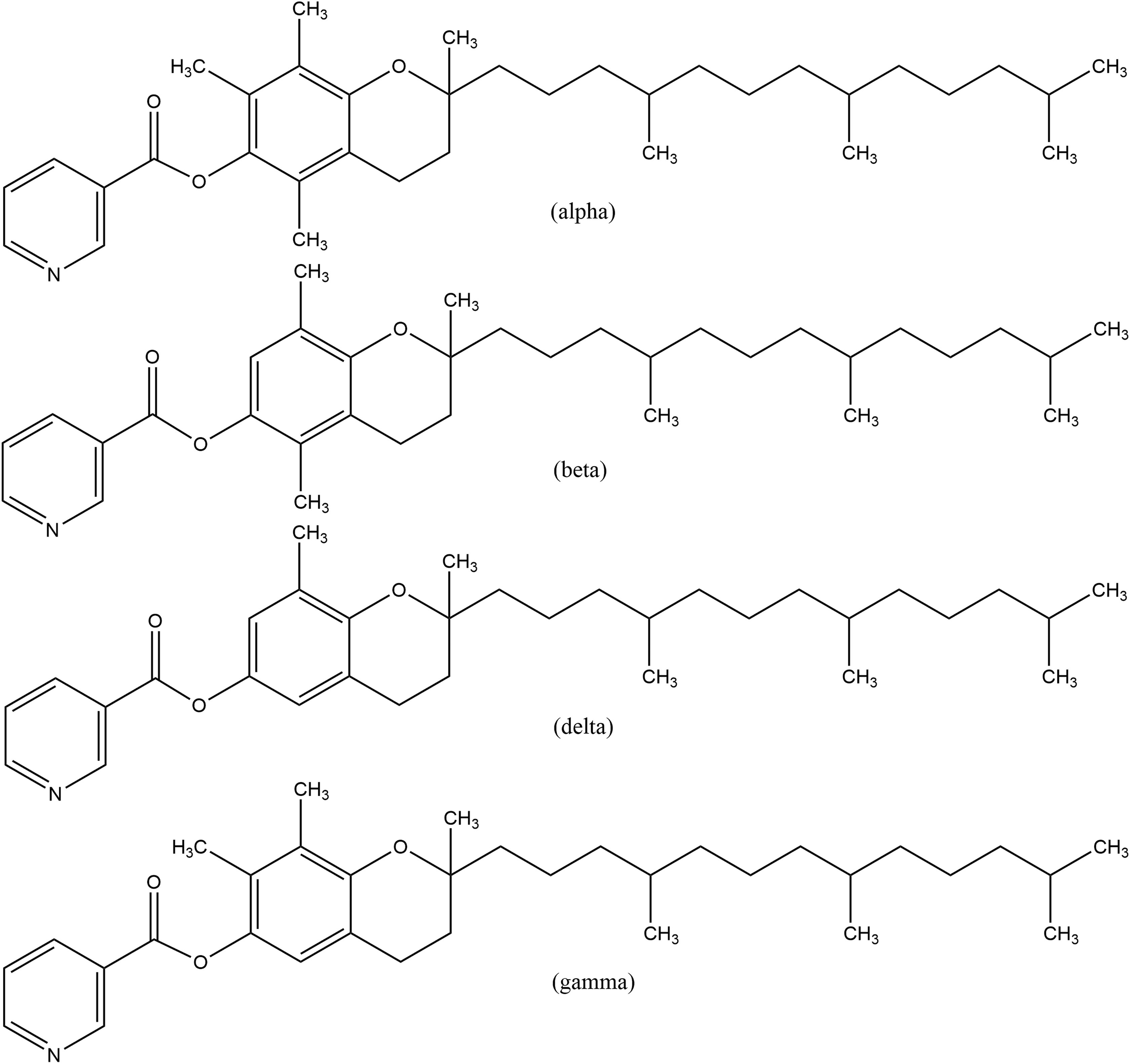
Tocopheryl nicotinate.
The definitions and structures of each ingredient are found in Table 1.
Definitions, Structures, and Functions.
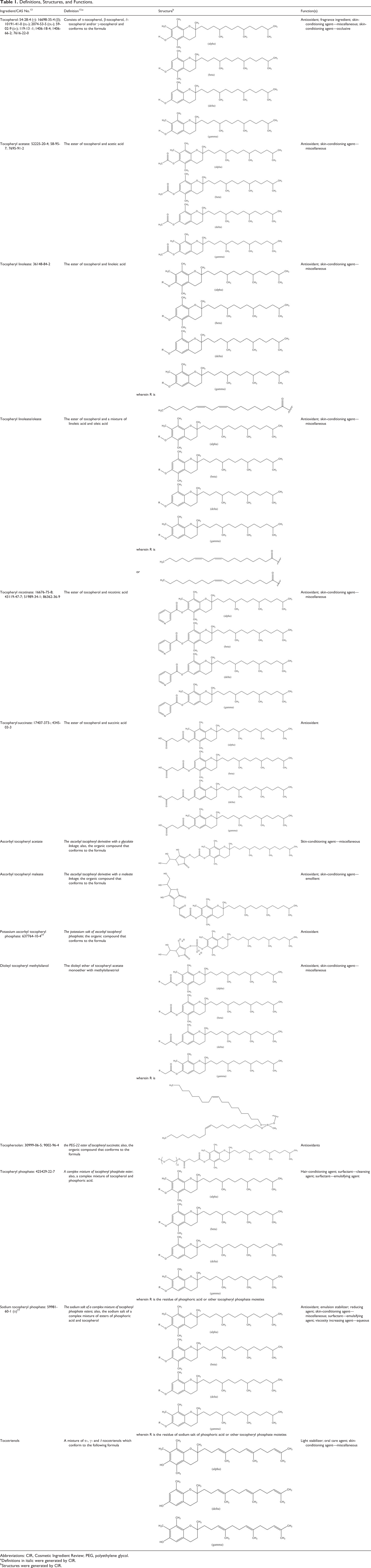
Abbreviations: CIR, Cosmetic Ingredient Review; PEG, polyethylene glycol.
a Definitions in italic were generated by CIR.
b Structures were generated by CIR.
Physical and Chemical Properties
α-, β-, γ-, and δ-Tocopherols and tocotrienols are lipophilic molecules. 5 Tocopherol is readily oxidized upon exposure to atmospheric conditions or light, but the oxidation propensity varies among α-, β-, γ-, and δ-analogs because of differences in oxidation potential and reactivity with molecular oxygen. Limited physical and chemical properties are provided in Table 2.
Physical and Chemical Properties.

Method of Manufacture
The original report on tocopherols describe the commercial manufacture from vegetable oils. 1 Tocotrienols can be isolated from a number of plant sources, including Vitis vinifera and Avena sativa. 3 The extraction method with the highest efficiency is Soxhlet extraction using hexane. Tocotrienols can also be synthesized via a multitude of synthetic pathways, most of which involve multistep processes to alkenylate the chromanol core. 6
Natural Occurrence
Tocopherols and tocotrienols are synthesized by photosynthetic organisms, and because this synthesis is accomplished stereospecifically via enzymes, the resulting tocopherols always possess the same stereochemical configurations, with the R configuration at C-2 (ring-sidechain junction) and the sidechain methyl substituents. 7 –10 Tocotrienols are present in seeds, fruits, and latex. Tocopherols are the exclusive form of vitamin E in leaves of plants and the seeds of most dicots; tocotrienols are found in the seed endosperm of a limited number of dicots. Tocotrienols are the primary form of vitamin E found in the seed endosperm of most monocots, including wheat, rice, and barley, and tocotrienols are also found in coconut oil, cocoa butter, and soybeans.
Natural sources of tocopherols include sunflower, peanut, walnut, sesame, and olive oils; tocotrienols are not found in these oils. 9 γ-Tocopherol is often the most prevalent form of vitamin E in plant seeds and the products derived from them: Corn, soybean, and sesame oil and walnuts, pecans, and peanuts are good sources of γ-tocopherol. 11 Tocopheryl phosphate has been identified in various seeds and nuts, dairy products, green vegetables, fruits, and cereals. 12
Palm oil is one of the richest sources of tocotrienols; tocotrienols compose up to 70% of the vitamin E in palm oil. 9 Crude palm oil extracted from the fruits of Elaeis guineensis contains up to 800 mg/kg tocotrienols. 8 Different analogs are more abundant in some plants than others; for example, rice bran oil is a major source of γ-tocotrienol but not α-tocotrienol. 7 Some other examples of plants containing significant amounts of tocotrienols are provided in Table 3.
Plants Containing Tocotrienols.a
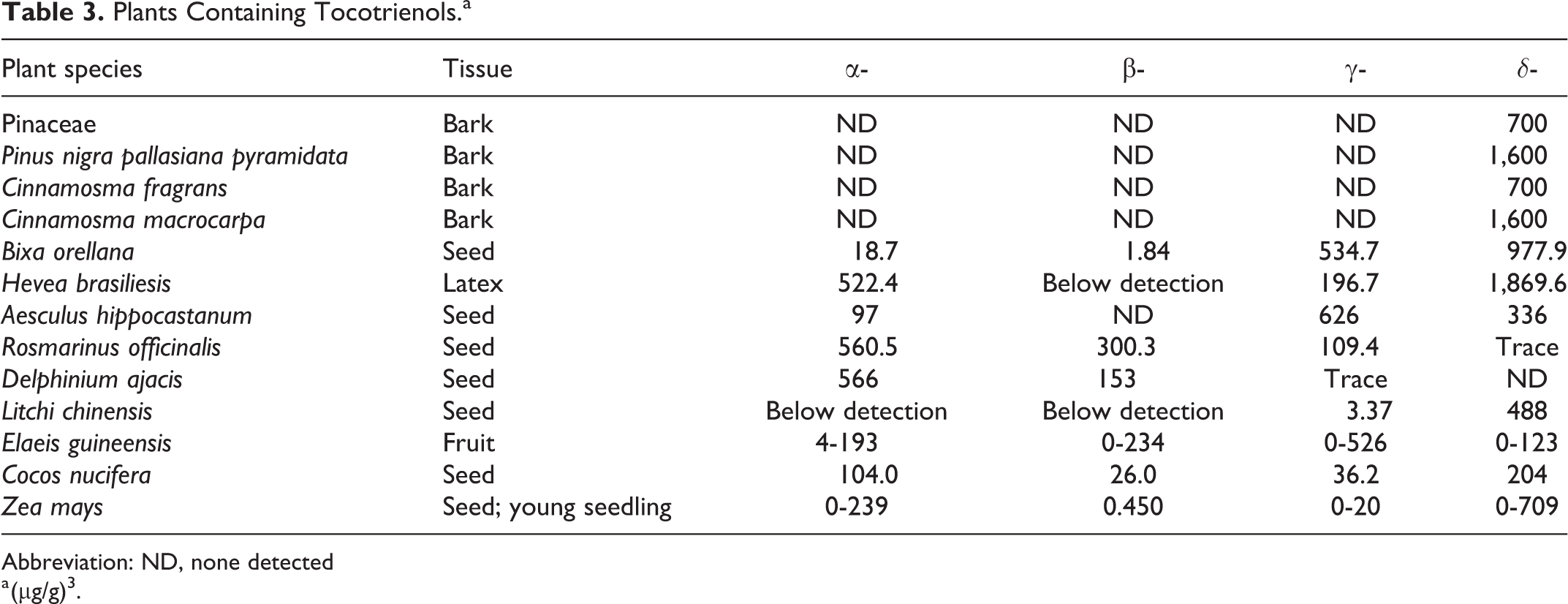
Abbreviation: ND, none detected
a (μg/g) 3 .
Ultraviolet Absorbance
According to the orginal report, tocopherols absorb light in the mid-wavelength ultraviolet (UVB) range. 1 The λ max is reported to be 296 nm.
Use
Cosmetic
Most of the tocopherols are reported to function in cosmetics as antioxidants or skin-conditioning agents.
13
In contrast, tocotrienols is not reported to function in cosmetics as an antioxidant but instead as a light stabilizer, oral care agent, or skin-conditioning agent (Table 1.) The Food and Drug Administration (FDA) collects information from manufacturers on the use of individual ingredients in cosmetics as a function of cosmetic product category in its Voluntary Cosmetic Registration Program (VCRP). The VCRP data obtained from the FDA report that the frequency of use increased considerably for both tocopherol and tocopheryl acetate since the issuance of the original report. The reported use of tocopherol increased from 1,072 (1998 data) to 6,635 uses (2014 data), and the reported use of tocopheryl acetate increased from 1,322 (1998 data) to 9,677 uses (2014 data).
14
For both of these ingredients, the 2014 VCRP data include uses under more than 1 name. Tocopherol has 6,470 reported uses as tocopherol, 119 reported uses as tocopherol
The use concentration of tocopherol, but not of tocopheryl acetate, has increased since the original assessment. According to the survey conducted by the Personal Care Products Council (Council), the concentration of use of tocopherol in leave-on products increased from 2% in 1999 to 5.4% in 2013. 15 Tocopheryl acetate continued to have the highest reported use concentration; it is used at up to 36% in leave-on formulations and that use is in cuticle softeners. The original safety assessment reported that tocopheryl acetate was used at 100% in “vitamin E oil.”
Ascorbyl tocopherol acetate and tocopheryl phosphate are not reported to be used according to VCRP data and Council survey data. 14
The current and historical frequency and concentration of use data for the previously reviewed tocopherols are provided in Table 4. Table 5 provides the frequency 14 and concentration 15,16 of use data for the ingredients that have been included in this rereview. The tocopherols are used in baby product formulations (0.1% tocopheryl acetate in baby lotions, oils, and creams) and formulations that can be incidentally ingested (3% tocopheryl acetate in lipsticks).
Current and Historical Frequency and Concentration of Use of Tocopherols and Tocotrienols According to Duration and Exposure.
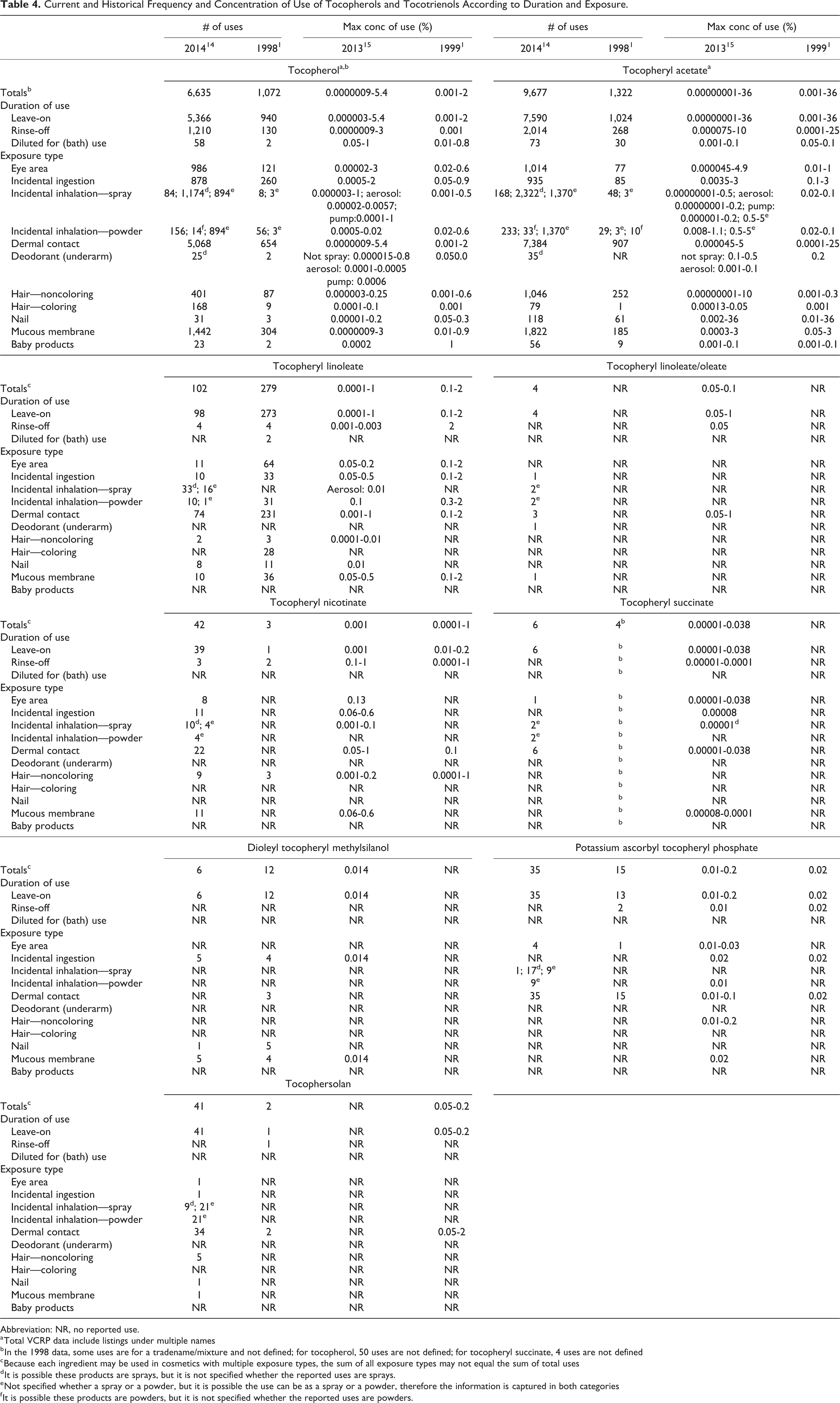
Abbreviation: NR, no reported use.
a Total VCRP data include listings under multiple names
b In the 1998 data, some uses are for a tradename/mixture and not defined; for tocopherol, 50 uses are not defined; for tocopheryl succinate, 4 uses are not defined
c Because each ingredient may be used in cosmetics with multiple exposure types, the sum of all exposure types may not equal the sum of total uses
d It is possible these products are sprays, but it is not specified whether the reported uses are sprays.
e Not specified whether a spray or a powder, but it is possible the use can be as a spray or a powder, therefore the information is captured in both categories
f It is possible these products are powders, but it is not specified whether the reported uses are powders.
Frequency and Concentration of Use According to Duration and Type of Exposure—Added Ingredients.
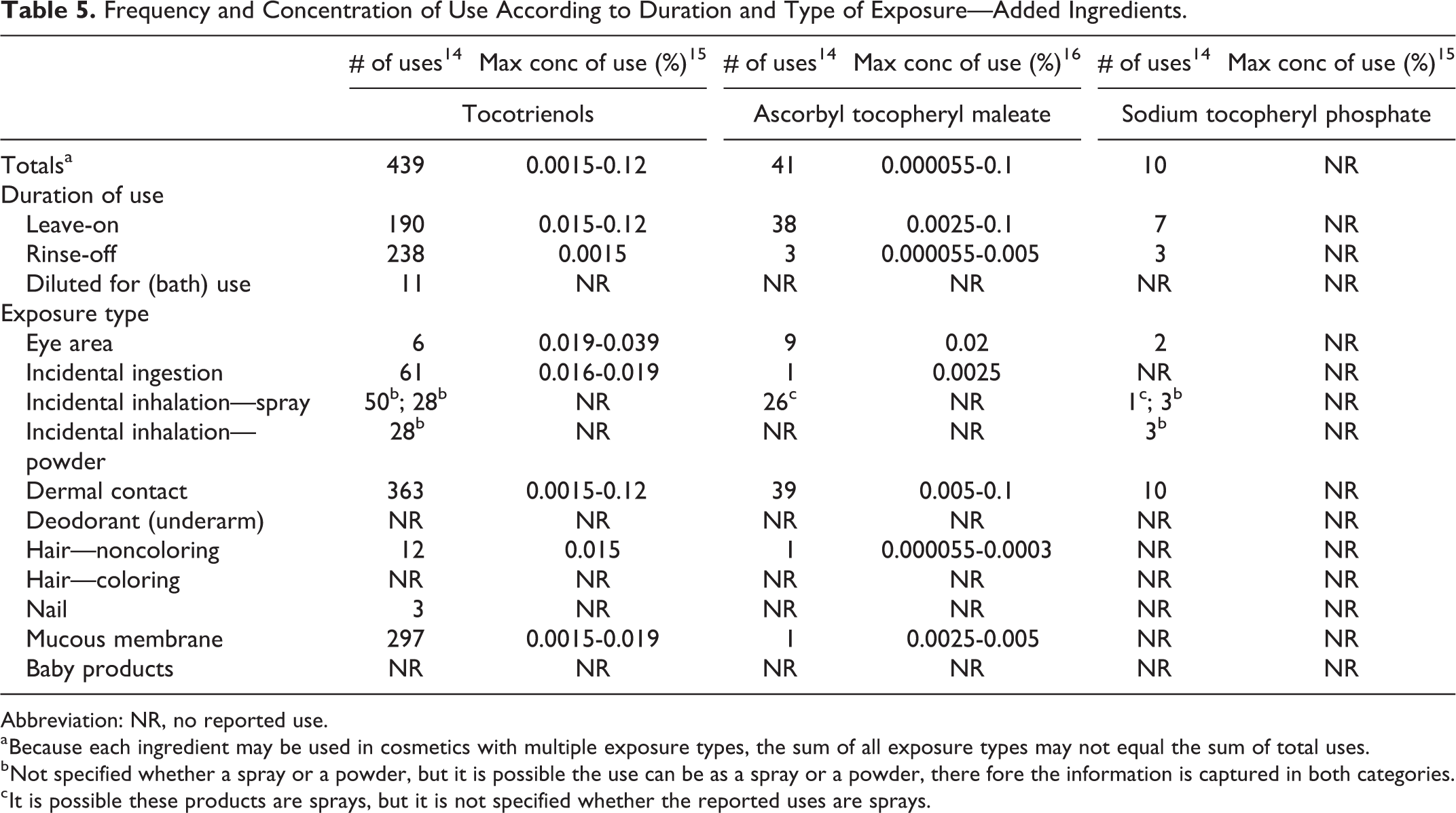
Abbreviation: NR, no reported use.
a Because each ingredient may be used in cosmetics with multiple exposure types, the sum of all exposure types may not equal the sum of total uses.
b Not specified whether a spray or a powder, but it is possible the use can be as a spray or a powder, there fore the information is captured in both categories.
c It is possible these products are sprays, but it is not specified whether the reported uses are sprays.
Several of the tocopherols that are used in products can possibly be inhaled. For example, tocopheryl acetate is used at up to 5% in foot powders and sprays and up to 0.2% in aerosol hair spray formulations, and tocopherol is used at up to 1% in pump hair spray formulations. In practice, 95% to 99% of the droplets/particles released from cosmetic sprays have aerodynamic equivalent diameters >10 μm, with propellant sprays yielding a greater fraction of droplets/particles <10 μm compared to pump sprays. 17,18 Therefore, most droplets/particles incidentally inhaled from cosmetic sprays would be deposited in the nasopharyngeal and thoracic regions of the respiratory tract and would not be respirable (ie, they would not enter the lungs) to any appreciable amount. 19,20 Tocopheryl acetate is used at up to 0.1% in aerosol deodorants, and there is some evidence indicating that deodorant spray products can release substantially larger fractions of particulates having aerodynamic equivalent diameters in the range considered to be respirable. 19 However, the information is not sufficient to determine whether significantly greater lung exposures result from the use of deodorant sprays, compared to other cosmetic sprays.
All tocopherols named in this report are listed in the European Union inventory of cosmetic ingredients. 21 α-Tocopherol acetate is the most common form of vitamin E used in commercial sunscreen and skin care products. 22
Noncosmetic
α-Tocopherol and α-tocopheryl acetate are GRAS food ingredients when used as a nutrient, and α-tocopherol is GRAS as a chemical preservative in food when used in accordance with good manufacturing practices (21CFR182.8890; 21CFR182.8892; 21CFR182.8390). The Joint FAO/WHO Expert Committee on Food Additives established a group allowable daily intake of 0.15 to 2 mg/kg for
Toxicokinetics
Absorption, Distribution, Metabolism, and Excretion
Oral
The structural differences between tocopherol and tocotrienols result in a difference in the penetration of these compounds into the tissues. The presence of 3 unsaturated bonds in the carbon sidechain allows tocotrienols to penetrate tissues with saturated fatty layers, such as the brain and the liver, more readily than tocopherol, which has a fully saturated side chain. 8,9
Many studies have been conducted on the distribution of tocopherols and tocotrienols with oral administration, and the studies demonstrate that tocopherols distribute to almost all tissues in the body, and the distribution and metabolism varies among the tissues. α-Tocopherol is the predominant form of vitamin E in human and animal tissues, and it has the highest oral bioavailability, and
The distribution and intracellular trafficking of vitamin E may be modulated by tocopherol regulatory proteins; 3 have been identified that specifically bind tocopherols.
35
Tocopherol transfer protein (TTP) is a cytosolic lipid-binding and transfer protein that has been found in rat brain, spleen, lung, and kidney, in some human brains, and in the mouse uterus. Tocopherol-associated protein, also a cytosolic lipid-binding and transfer protein, is found in bovine and human tissues; the greatest levels in human tissues were in the adult liver. The third protein, tocopherol-binding protein, is found in rat liver and heart, rabbit heart, bovine heart, and human placenta. Only TTP has been shown to influence plasma and tissue α-tocopherol concentrations. Relative affinities of purified TTP for α-tocopherol, as determined by competition between vitamin E analogs for transfer between liposomes and membranes in vitro, were 100% for
Tocopherols and tocotrienols were found in the skin of female hairless mice fed a chow containing 29.7 mg α-tocopherol, 10.3 mg γ-tocopherol, 3.1 mg α-tocotrienol, and 7.4 mg γ-tocotrienol per kg chow. 36 However, the distribution in the chow was different than that found in the skin; approximately, 58% of the vitamin E in the chow was α-tocopherol and 20% was tocotrienols, but approximately, 89% of the vitamin E found in the skin was α-tocopherol.
A procedure was developed that allowed for the simultaneous determination of tocopherols and tocotrienols, and the presence of these cogeners in tissues of the hairless mouse was determined. 37 The skin contained mostly α-tocopherol (5.4 nmol/g; 85.6%), but α-tocotrienol (0.24 nmol/g; 3.4%) and γ-tocotrienol (0.76 nmol/g; 10.4%) were also found. Tocotrienols were also identified in the skin + subcutis but to a lesser extent. The brain contained primarily α-tocopherol (5.4 nmol/g; 99.8%), and it contained no tocotrienols. The heart, kidneys, and liver also contained primarily α-tocopherol, but some tocotrienols were present, and the highest amount of α-tocopherol was found in the heart (24.2 nmol/g; 98.1%).
Groups of 10 female CF-1 mice were fed a basal diet (containing 75 IU/kg vitamin E) or basal diet supplemented with 0.3% a γ-tocopherol-rich mixture of tocopherols for 4 weeks. 38 One gram of the mixture contained 900 mg total tocopherols with 13.0% of α-tocopherol, 1.5% β-tocopherol, 56.8% γ-tocopherol, and 24.3% δ-tocopherol. Pooled urine and fecal samples were collected for each group during the last 4 days of the study, and at study termination, blood and liver samples were collected. High pressure liquid chromatography (LC)/electrochemical detection and LC-electrospray ionization mass spectrometry were used to analyze the major metabolites of the different tocopherols and tocotrienols in the samples. The major route of excretion was fecal; 18 tocopherol-derived metabolites and α-, γ-, and δ-tocopherol were identified in the fecal samples of the mice fed the tocopherol diet. Short-chain degradation metabolites, particularly γ- and δ-carboxyethyl hydroxychromans and carboxymethylbutyl hydroxychromans, were detected in urine, serum, and liver samples, and tocopherols were detected in serum and liver samples. The majority of the urinary metabolites were excreted as glucuronide conjugates.
The researchers also examined the metabolite profile of pooled samples of feces, blood, and urine from a study in which male CF-1 mice were fed a basal diet or the basal diet supplemented with 0.17% of a tocotrienol preparation for 21 weeks; the preparation was a 65% oil suspension that contained 20.2% α-tocotrienol, 4.0% β-tocotrienol, 16.1% γ-tocotrienol, 24.3% δ tocotrienol, 14.8% α-tocopherol, and 3.1% γ-tocopherol. 38 Twenty-four tocotrienol-derived side-chain degradation metabolites were identified in fecal samples as were parent α-, γ-, and δ-tocotrienols; more short-chain than long-chain tocotrienol-derived metabolites were present in the feces. Short-chain degradation metabolites, particularly carboxyethyl hydroxychromans, carboxymethylbutyl hydroxychromans, and carboxymethylhexenyl hydroxychromans, were detected in urine.
The metabolism of a tocopherol supplement was evaluated in humans. 38 Two male subjects were given 6 softgels containing γ-tocopherol-rich dietary supplements at 0 hour, and 6 more softgels at 10 hours. Each softgel contained 200 mg β tocopherol, 78 mg δ-tocopherol, 133 mg α-tocopherol, and 2 mg tocotrienols. Fecal and urine samples were collected at 0, 12, 24, and 48 hours, and blood samples were taken at 0 and 12 hours. At 24 hours, almost all the side-chain degradation products that were identified in mouse fecal samples (described previously) were found in human fecal samples, and the metabolite concentrations increased over time. γ-Tocopherol-derived metabolites were more prominent than δ- and α-derived metabolites at 24 hours. The major metabolites found in the urine were carboxyethyl hydroxychromans and carboxymethylbutyl hydroxychromans.
Eight-day pregnant rats were dosed by gavage with 1 g/kg tocotrienol-rich fraction (1.23 mmol α-tocotrienol and 0.94 mmol tocopherol per g; isolated from palm oil) suspended in vitamin-E-deficient corn oil for 9 days. 39 The rats were killed on day 17 of gestation, and tissues were collected from the dams and the neonates. In the maternal brain, the α-tocopherol content and α-tocotrienol content changed by 0.1-fold and 5-fold, respectively. In the fetal brain, α-tocotrienol content increased more than 20-fold. Subsequent testing with lower doses of tocotrienols (5 mg/kg bw) over a longer time period (not specified) supported the finding that dietary tocotrienol was distributed to the brain.
Tocopherol depletion by UV in the skin
Tocopherol
Female C3H/HeN Tac mice were treated topically with 5.3 μmol
With the 15-minute tocopherol exposure prior to UV, the researchers found that α-tocopherol was most likely not absorbed into the epidermis prior to irradiation and that photooxidation occurred on the skin surface. The vehicle that was used did not have an effect on the depletion of topically applied tocopherol, but it did have an effect on the products of photooxidation; more polar products occurred when DMSO was used as the vehicle.
Tocopherol acetate
The hydrolysis of α-tocopheryl acetate to α-tocopherol was determined in nonirradiated and irradiated mouse skin. 41 Without UV, d3-α-tocopheryl acetate in an inert cream (50 mg of a 5% cream, 5.3 μmol d3-α-tocopheryl acetate) was applied to the shaved dorsal skin of female C3H/HeN Tac mice. With UV, either shaved mice were irradiated for 60 minutes with a total dose of 13 kJ/m2 UVB and then treated with 5.3 μmol d3-α-tocopheryl acetate in either the inert cream or d3-α-tocopheryl acetate was applied 15 minutes before UVB irradiation. All animals were killed 1, 3, 6, 24, or 48 hours after dosing, and the epidermis was isolated. At 24 and 48 hours postdosing with d3-α-tocopheryl acetate in nonirradiated mice, d3-α-tocopherol increased up to 10 times that of endogenous α-tocopherol. Application of d3-α-tocopheryl acetate 60 minutes after irradiation resulted in a 40-fold increase in epidermal α-tocopherol. In both cases, hydrolysis was <1% of the total applied dose. Hydrolysis of α-tocopheryl acetate increased with increased UVB dose. Application of d3-α-tocopheryl acetate prior to irradiation eliminated hydrolysis.
A dose–response effect of UVB on d3-α-tocopheryl acetate hydrolysis was then examined. Shaved mice were exposed to UVB for 60, 90, or 120 minutes, corresponding to 13, 19.5, or 26 kJ/m2, respectively, in a single dose or in multiple 30 min/d doses, and the mice were treated with 5.3 μmol d3-α-tocopheryl acetate in the inert cream. The animals were killed 24 hours after dosing, and the epidermis was isolated. The UVB exposure, as a 30-minute multiple day dose, potentiated UVB-induced hydrolysis of d3-α-tocopheryl acetate to d3-α-tocopherol.
The researchers also examined the effect of rate of absorption into the skin on hydrolysis by applying 5.3 μmol d3-α-tocopheryl acetate in 50 μL DMSO, following the same procedure described earlier. In nonirradiated mouse skin, hydrolysis was maximal at 3-hour posttreatment with d3-α-tocopheryl acetate in DMSO, which was earlier than what was observed using the inert cream, suggesting that hydrolysis was limited by absorption in these mice. The researchers commented that although maximal absorption occurred earlier than when d3-α-tocopheryl acetate was applied in an inert cream, the maximal capacity for hydrolysis was the same (ie, ∼80 pmol d3-α-tocopherol/mg epidermis). In mice irradiated for 1 hour prior to dosing, a time-dependent increase in hydrolysis was observed at 6 ad 24 hours posttreatment, which was similar to the response observed with the inert cream, suggesting that absorption is not the limiting factor in UVB-induced hydrolysis of d3-α-tocopheryl acetate. These conclusions were supported by the fact that a 10-fold greater dose of d3-α-tocopheryl acetate resulted in a 4- to 6-fold increase in d3-α-tocopherol levels in nonirradiated mice, but only a 2- to 3-fold increase in irritated mice. Further testing led to the suggestion that the esterase activity at the surface of the skin was capable of converting d3-α-tocopheryl acetate to d3-α-tocopherol.
Tocopherol phosphate
One study found that following UV exposure, reduction in endogenous α-tocopherol in the skin was not inhibited by pretreatment with α-tocopheryl phosphate. 42 Pretreatment of SKH-1 mouse skin cultures with 0.5% α-tocopheryl-6-O-phosphate produced a 2 to 3 times greater amount of endogenous α-tocopherol than that found in control skin, and the UV-induced reduction in cutaneous α-tocopherol was inhibited.
Dermal Penetration
In vitro
The effect of vehicle on the dermal penetration of α-tocopherol was determined in micro-Yucatan pig skin. 43 The dermal penetration of 1% tocopherol was evaluated in several vehicles, and α-tocopherol permeated into the receptor fluid regardless of the vehicle used. The greatest permeation found in viable skin + the receptor was from an emulsion vehicle that contained 10% isopropyl myristate; 12.24% of the applied dose was found in the viable skin and receptor fluid. The lowest penetration, 6.47% applied dose, was observed with an alcoholic vehicle that was 96% SD alcohol.
The researchers also examined the kinetics of permeation and metabolism of α-tocopheryl acetate across micro-Yucatan pig skin. 44 Formulations containing a 5% tocopheryl acetate solution in isopropyl myristate, a 5% tocopheryl acetate emulsion, and a 1% solution of α-tocopherol in isopropyl myristate were studied, and permeation was measured at 2, 6, 12, and 24 hours. Any presence of tocopheryl acetate in the receptor fluid was below the limit of detection. Tocopheryl acetate was converted into tocopherol within the viable skin tissue.
In vitro skin penetration data on tocopheryl acetate were obtained from a robust summary of data submitted to the European Chemical Agency (ECHA) as part of the REACH chemical registration process. These data are available on ECHA’s website. 45 The in vitro skin absorption study, performed according to Organisation for Economic Co-operation and Development (OECD) guideline 428, indicated that tocopheryl acetate in an α-hydroxy acid (AHA) vehicle (composition not defined further) penetrated into and through intact and stripped pig skin, and the total skin penetration rates were time- and formulation dependent; the differences were not statistically significant. First, intact skin was exposed to 6 mg/cm2 of 5% [3 H]-tocopheryl acetate cream (300 μg active substance/cm2) in 1 of 3 AHA vehicles for 1, 6, or 18 hours. After 1 hour, 1.1% to 1.3% of the dose (based on penetration in the stratum corneum, remaining skin tissues layers, and chamber liquid) was absorbed. After 6 hours, absorption was 2.6% to 4.2%, and after 18 hours, 3.1% to 4.2% of the dose absorbed. Using stripped skin (stratum corneum removed), higher absorption rates through the remaining skin tissue was observed for all 3 formulations.
The dermal penetration of tocopheryl acetate in human skin samples was measured using 4 different vehicles, and the bioconversion of tocopheryl acetate to tocopherol was determined. 5 Tocopheryl acetate was (1) delivered in a triglyceride oil (caprylic/capric acid triglyceride); (2) surfactant-solubilized in water (PPG-26-buteth-26 and polyethylene glycol [PEG]-40 hydrogenated castor oil); (3) encapsulated in soybean phosphatidylcholine liposomes; or (4) encapsulated in nanotopes. The final concentration of tocopheryl acetate was 2%. A dose of 11 mg/cm2 of each test formulation (corresponding to 220 μg/cm2 tocopheryl acetate) was applied to skin samples under occlusive and nonocclusive conditions. The distribution of tocopherol acetate and tocopherol at the skin surface, in the horny layers, and in the underlying skin was determined after 8 hours.
The recovery rate of tocopheryl acetate–tocopherol (vitamin Etotal) exceeded 90% in each experiment. Tocopheryl acetate in the triglyceride oil was only deposited at the skin surface and in the horny layers. With the other 3 formulations, differences were found with occlusive versus nonocclusive applications; more vitamin Etotal was found in the underlying skin with the nonocclusive application. The conversion to free tocopherol only occurred in the underlying skin layer, and the percentage of bioconversion was greater with occlusive application. The distribution of vitamin Etotal and the bioconversion of tocopheryl acetate to tocopherol from each formulation are summarized in Table 6.
Tocopherol and Tocopheryl Acetate Recovery (mol %) and % Bioconversion Tocopheryl Acetate to Tocopherol in Human Skin In Vitro.
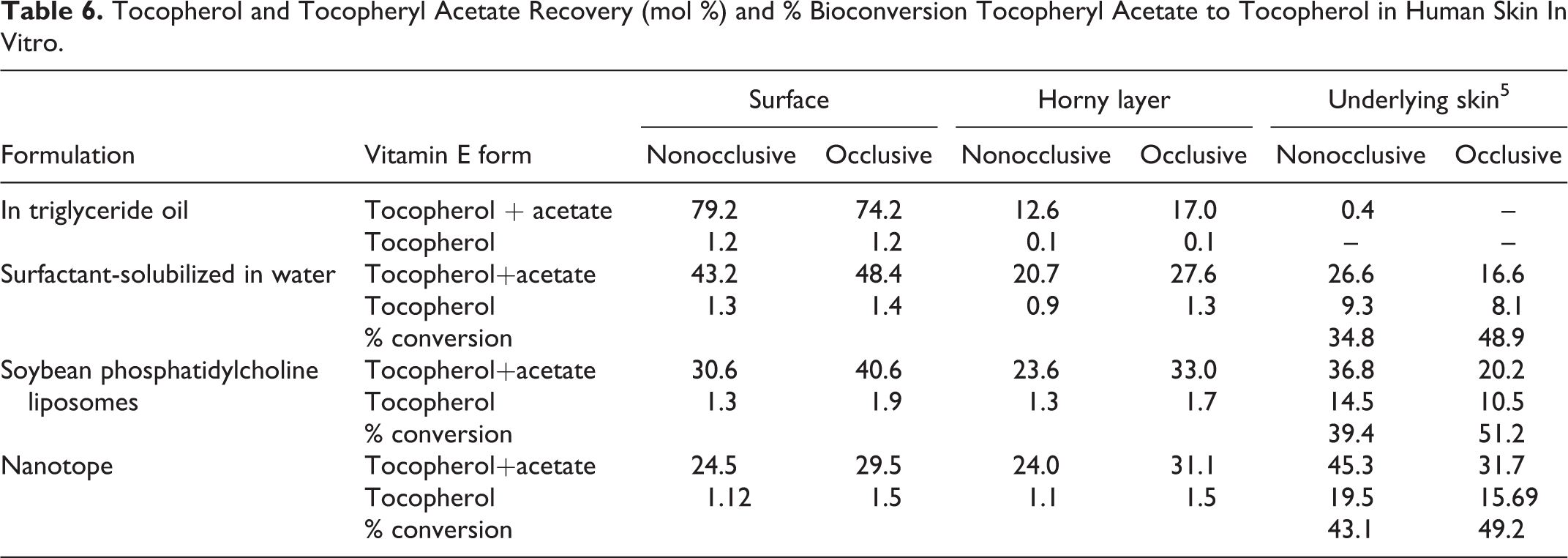
An in vitro study using human cadaver skin was conducted to determine the absorption of tocopheryl acetate from various vehicles. 46 Modified Franz diffuser cells, and 95% degassed ethanol, as opposed to modified phosphate-buffered saline, was used in the receiver compartment. Sampling times ranged from 2 to 48 hours. Tocopheryl acetate, as a 5% solution, was prepared in ethanol, isopropyl myristate, and mineral oil; 5% gel formulations were prepared in a 1% or 3% water-soluble polymer. Isopropyl myristate was the only vehicle that statistically significantly increased permeation through the skin. The calculated permeabilities (using a mathematical model) of the 5% tocopheryl acetate formulations were 1.0 × 10−4 cm/h with ethanol; 1.1 × 10−2 cm/h with isopropyl myristate; 1.4 × 10−4 cm/h with mineral oil; 2.1 × 10−4 cm/h with the 1% water-soluble polymer gel; and 4.7 ×10-4 cm/h with the 3% water-soluble polymer gel.
In vivo
Tocopherol
Dermal application of 5 mg/cm2 α-tocopherol to the backs of female hairless SKH-1 mice for 24 hours resulted in a 62-fold increase in α-tocopherol in the epidermis and a 22-fold increase in the dermis. 47
Tocopheryl acetate
An ointment containing 2% or 20% tocopheryl acetate was applied to the backs of 5 male Wistar rats for 24 hours, and a 2 cm-diameter skin punch was then taken to determine the content of vitamin E in the skin. 48 (The ointment contained 15% squalane.) Application of 20% tocopheryl acetate, but not 2%, resulted in a statistically significant increase in vitamin E in the skin. Vitamin E increased by 2.9 μg/g skin with the 20% ointment but only by 0.8 μg/g skin with the 2% ointment.
Tocopherols and tocotrienols
A 5% w/v solution containing a tocotrienol-rich palm oil fraction (TRF) in PEG-400 was applied to the skin of 4 female hairless mice. 36 The distribution of 4 analogs in the TRF was approximately 35% α-tocopherol, 10% γ-tocopherol, 25% α-tocotrienols, and 30% γ-tocotrienols. Four test sites were marked using polypropylene plastic rings, and 20 μL of the test mixture were applied to the area marked by 2 of the rings, and 20 μL of PEG-400 were applied to the other 2 areas. After 2 hours, the excess substance on the treated area was removed, first by rinsing 3 times with ethanol/water (95:5) and then twice with water alone. Half of the test sites were shielded, and the skin on the back of each animal was then irradiated for 29 minutes using an Oriel 1000-W solar simulator with an output of 2.8 mW/cm2 of long-wave ultraviolet light (UVA) and UVB light; this corresponded to 3 times the minimal erythema dose (MED). The animals were then killed.
Baseline values of each analog in PEG-400-treated skin were determined first; approximately 8.5 nmol/g skin α-tocopherol, 3 nmol/g skin γ-tocopherol, 7.5 nmol/g skin α-tocotrienols, and 7 nmol/g skin γ-tocotrienols were present in the skin. Dermal application of the TRF resulted in a 28-fold increase in α-tocopherol, an 80-fold increase in α-tocotrienol, a 130-fold increase in γ-tocopherol, and a 51-fold increase in γ-tocotrienol in the skin. The percentage of distribution of each of the analogs in the TRF mixture was compared to its percentage of distribution in the skin. The percentage of distribution of each analog that penetrated the skin was significantly different from its distribution in the mixture; higher percentages of α-tocopherol, similar amounts of γ-tocopherol, and lower percentages of α- and γ-tocotrienols were found in the skin, compared to the distribution in the TRF mixture.
In the skin from the UV-irradiated sites, approximately 40% of the vitamin E remained in the TRF-treated skin; there were no significant differences in the degree of destruction of the various analogs. Approximately, 80% of vitamin E remained in the PEG-treated skin. The researchers examined the effect of UV-irradiation on the breakdown of the analogs in the TRF solution itself; 86% α-tocopherol, 83% γ-tocopherol, 83% α-tocotrienol, and 84% γ-tocotrienol remained after irradiation.
The distribution of tocopherol and tocotrienol in the skin was also examined. 49 Forty μL of a 5% (w/v) solution α-tocopherol, α-tocotrienol, or γ-tocotrienol in PEG-400 was applied to the backs of SKH-1 hairless mice for 0.5, 1, 2, or 4 hours using a 2 cm2 polypropylene plastic ring, and the animals were killed after the skin was rinsed. Four animals were used per group. The concentration of each test article was measured in the skin layers. Application of all 3 analogs significantly increased the concentrations of vitamin E in the skin; application of the 5% α-tocopherol solution resulted in a 200- to 2,000-fold increase in skin α-tocopherol content. The concentration of each analog in the skin increased with time, but the relationship between the analogs and the content of each skin layer did not change. When expressed per μ, the highest concentrations of vitamin E was found in the uppermost layer of the stratum corneum (5 μm), and the concentration of α-tocopherol was statistically significantly greater than that of α- or γ-tocotrienol. When the thickness of each skin layer was considered, the lower skin layers contained appreciable amounts of vitamin E. The largest fraction of vitamin E in the skin following topical application was found in the deeper subcutaneous (SC) layers; the papillary dermis (31-130 μm) and the dermis (131-530 μm) contained the major portions of vitamin E if the total amount of each analog in each of the layers was summed and expressed as a percentage per its respective total. At 0.5 hours, significant increases in vitamin E were found in the SC fat, suggesting rapid penetration of vitamin E through the skin.
Toxicological Studies
Single Dose (Acute) Toxicity
Dermal
Tocopheryl acetate
According to robust summary data submitted to ECHA, the dermal LD50 of tocopheryl acetate is > 3 g/kg bw in albino rats. 45 Five animals per group were dosed with 1 or 3 g/kg bw undiluted tocopheryl acetate in vegetable oil under an occlusive patch for 24 hours. Slight erythema was observed 24 to 48 hours after exposure. Slight abrasion was observed in 1 low-dose female, 2 high-dose females, and 2 high-dose males.
Tocopheryl phosphate
The acute dermal toxicity of mixed tocopheryl phosphates (MTPs) was determined in New Zealand rabbits; the dermal LD50 was greater than 1,130 mg/kg bw MTP in female rabbits.
50
Mixed tocopheryl phosphate is a mixture of α-tocopheryl phosphate and α-di-tocopheryl phosphate and is produced by phosphorylating
Oral
Tocopheryl phosphate
The oral LD50 of MTP is >1,130 mg/kg bw in Wistar rats. 50 Groups of 5 male and 5 female were dosed by gavage with 1,130 mg/kg bw MTP (918 mg/kg bw α-tocopherol equivalents) in distilled water and killed after 14 days. All animal survived until study termination.
Repeated Dose Toxicity
Oral
Tocophersolan
Groups of 5 male Sprague-Dawley rats were dosed by gavage with an aqueous solution of 0.5, 1, or 2 g/k g tocophersolan once daily for 5 days, and the animals were then killed. 51 No signs of toxicity were observed, and all animals survived until study termination. Heart, kidney, liver, and spleen weights were not affected by dosing with tocophersolan, and there were no dose-dependent or statistically significant changes in hematology, clinical chemistry, or urinalysis parameters.
Tocopheryl phosphate
Groups of 10 male and 10 female Sprague-Dawley rats were fed a diet containing 0, 1, 3, or 5% MTP for 90 days; this MTP was composed of 72% α-tocopheryl phosphate and α-ditocopheryl phosphate, 13% α-tocopherol, 6% water, 7% phosphoric acid, and 2% other. 12 No clinical signs of toxicity, adverse effects on body weights, or test article-related mortality were reported. There were some statistically significant changes in hematology and clinical chemistry parameters, but generally these changes were dose dependent and not considered toxicologically significant. No statistically significant, dose-dependent changes in organ weight were observed compared to controls. There were no gross changes observed at necropsy; changes in relative heart and epididymal organ weight were considered incidental. The only significant microscopic finding was the presence of foreign material in sinusoidal macrophages associated with mild inflammatory changes in the mesenteric lymph nodes in male- and female-treated animals that occurred in a dose-dependent manner; the foreign material was identified as tocopheryl phosphate. In the mid- and high-dose groups, but not the low-dose groups, the foreign material often had a crystalline appearance. Foreign material was also present in the small intestines of the mid- and high-dose animals. The no-observable-adverse-effect-level (NOAEL) was 1% MTP in the diet.
Three repeated-dose oral toxicity studies of MTP were performed in rats, and no test article-related toxicity was observed. 50 The animals were dosed by gavage for 28 days in each of the studies. In the first study, 10 to 11 Sprague-Dawley rats/gender/group were dosed with 0, 368, 735, or 982 mg/kg bw/day MTP in a medium-chain triglyceride vehicle (corresponding to 0, 45.9, 229.5, and 458.8 mg/kg bw/day tocopherol equivalents, respectively). In the second study, groups of 4 to 5 Sprague-Dawley rats/gender/group were dosed with 0 or 869 mg/kg bw/day MTP (corresponding to 00 and 642 mg/kg bw/day tocopherol equivalents, respectively). And in the third study, groups of 5 Wistar rats/gender/group were dosed with 0, 56.5, 282.5 or 565 mg/kg bw/day MTP (corresponding to 0, 45.9, 229.5, and 458.8 mg/kg bw/day tocopherol equivalents, respectively). The animals were killed on day 29 in the first and third studies, and after a 14-day recovery period in the second study. No test article–related mortality, no signs of toxicity, and no microscopic or gross lesions were observed in any of the studies.
Tocotrienols
Groups of 10 male and 10 female F344/DuCrj rats were fed a diet containing 0%, 0.19%, 0.75%, or 3% of a tocotrienols preparation for 13 weeks; the preparation consisted of 21.4% α-tocotrienol, 3.5% β-tocotrienol, 36.5% γ-tocotrienol, 8.6% δ-tocotrienol, 20.5% α-tocopherol, 0.7% β-tocopherol, 1.0% γ-tocopherol, and 0.5% δ-tocopherol. 52 Another group was fed a diet containing 0.69% α-tocopherol. No remarkable changes in general appearance and no morality were reported. Body weight gain was decreased in the males fed with the 3% tocotrienols diet when compared to the other groups, but feed consumption was similar to the other groups. Relative adrenal glands to body weights were dose dependently increased in all treated males, and lung weights were statistically significantly decreased in all treated females. In the 3% tocotrienols group, statistically significant increases were observed in brain, heart, liver, kidneys, and testes weights of males and liver and spleen weights of females, and statistically significant decreases in ovary and uterus weights were observed in females. Statistically significant changes were noted in various hematological parameters, and most of these changes were thought to have little toxicological significance; however, the statistically significant decrease in platelets in males, but not females, in a dose-dependent manner was thought to be a physiological response. Several hematology parameters were statistically significantly decreased in females of the 0.75% and 3% tocotrienol group. Effects on several serum biochemistry values were also considered of little toxicological significance. The NOAEL was 0.19% tocotrienols preparation in the diet; a no-observable-effect-level could not be determined.
Ocular Irritation
Tocopheryl acetate
According to robust summary data submitted to ECHA, tocopheryl acetate was not irritating to rabbit eyes in 1 study, but it produced weak-to-moderate conjunctival irritation in another study. 45 Undiluted tocopheryl acetate was instilled into the conjunctival sac of 3 Vienna white rabbits, and the eyes were not rinsed. The eyes were scored at 1, 24, 48, and 72 hours after instillation. Slight irritation was observed at 1 to 48 hours, and the eyes were normal at 72 hours.
In a modified Draize test, the same protocol was followed as above, and undiluted
Tocopheryl phosphate
Mixed tocopheryl phosphate was not irritating to rabbit eyes. 50 One-tenth mL of an aqeous gel containing 47.5 mg MTP (38.4 mg/kg bw α-tocopherol equivalents) was instilled into the conjunctival sac of 1 eye of 1 male and 2 female New Zealand rabbits; the contralateral eye served as a control. The eyes were scored for irritation 1, 24, 48, and 72 hours after dosing.
Reproductive and Developmental Toxicity
The original report on tocopherols indicated that tocopheryl succinate, up to 75 mg/d in the diet did not have reproductive or developmental effects in rats. And, tocopheryl acetate, ≤1.6 g/kg/d, generally did not have any reproductive or developmental effects in rabbits, hamsters, rats, or mice. 1
Genotoxicity
In Vitro
Tocopherol
According to robust summary data submitted to ECHA, tocopherol was not genotoxic in a mammalian cell assay.
45
The genotoxic potential of
Tocopheryl acetate
According to robust summary data submitted to ECHA, tocopheryl acetate was not genotoxic in Ames tests or a chromosomal aberration assay. 45 Two Ames tests were performed; the first was performed with Salmonella typhimurium TA1535, TA97, TA98, TA100, and TA102, with and without metabolic activation, at test concentrations of 0, 50, 158, 500, 1,580, and 5,000 μg/plate all-rac-α-tocopheryl acetate in ethanol. The second was performed using S. typhimurium TA1535, TA1537, TA98, and TA100 at concentrations of 0, 20, 100, 500, 2,500, and 5,000 μg/plate tocopheryl acetate in DMSO, with and without metabolic activation. Vehicle and appropriate positive controls were used in each study. Tocopheryl acetate was not mutagenic.
In the chromosomal aberration assay, human peripheral lymphocytes were exposed to
Tocopheryl phosphate
Mixed tocopheryl phosphate was not mutagenic in the Ames test nor genotoxic in a chromosomal aberration assay. 50 Two Ames test were conducted with S typhimurium TA98, TA100, TA1535, and TA1537 and Escherichia coli WP2 uvrA. The test concentrations were 0.9 to 2,825 μg/plate aqeous MTP (0.73-2,294 μg tocopherol equivalents/plate) in the first study and 88.3 to 2,825 μg/plate MTP (71.7-2,294 μg tocopherol equivalents/plate) in the second study. The tests were conducted with and without metabolic activation, and positive and negative controls gave valid results.
Two assays for chromosomal aberrations were conducted using CHO cells; the test article was suspended in 1% carboxymethyl cellulose. Concentrations of 13.4 to 40.8 and 15.5 to 37.9 μg/plate MTP (10.9-33.1 and 12.6-30.8 μg tocopherol equivalents/plate, respectively) were tested with metabolic activation, and concentrations of 26.1 to 40.8 and 3.7 to 67.8μg/plate and MTP (21.2-33.8 and 3.0-55.1 μg tocopherol equivalents/plate, respectively) were tested without metabolic activation in the 2 studies. The only difference in protocol between the 2 studies was that, in the second study without metabolic activation, the cells were exposed continuously for 20 hours as opposed to a 3-hour exposure and 17-hour recovery period.
Tocopheryl succinate
Tocopheryl succinate was weakly positive in a sister chromatid exchange assay in the presence of metabolic activation and was negative for genotoxicity in a chromosome aberration assay.
53
Two trials were performed. In the first trial, concentrations of 5, 7, 10, and 50 μg/Ml
In the chromosomal aberration assay,
Carcinogenicity
Oral
Tocopherol
Female Sprague-Dawley rats were given a single intraperitoneal (IP) injection of 50 mg/kg bw N-methyl-N-nitrosourea, and 1 week later, the animals were fed AIN-93 M diet alone or supplemented with 0.1, 0.3, or 0.5% mixed tocopherols (57% γ-, 24% δ-, 13% α-, and approximately 0.5% β-tocopherol) for 9 weeks, and the animals were then killed. 55 After 9 weeks of supplementation with tocopherols, serum γ- and δ-tocopherol levels were statistically significantly increased. A dose-dependent inhibition in tumor growth was observed, and a statistically significant decrease in tumor burden and tumor multiplicity was reported at necropsy. Tumor burden was inhibited by 80% in the highest dose group. The researchers reported that γ- and δ-tocopherol, but not α-tocopherol, activated peroxisome proliferator-activated receptor-γ.
A mixed tocopherol diet statistically significantly reduced azoxymethane (AOM)-induced colonic aberrant crypt foci in male F344 rats. 56 Male F344 rats were fed a modified AIN-76A diet at 5 weeks of age, and then, at age 7 weeks, were given SC injections of 15 mg/kg bw AOM once weekly for 2 weeks. One day after the second injection of AOM, groups of animals were maintained on the AIN-76A diet alone or supplemented with 1,000 ppm mixed tocopherols; the mixed tocopherols consisted of 58% γ-tocopherol, 21% δ-tocopherol, and 12% α-tocopherol. All animals were killed 8 weeks after the second AOM injection. Azoxymethan-induced colonic aberrant crypt foci was reduced approximately 55% in the mixed tocopherol-fed rats when compared to the controls.
Tocopheryl succinate
The effect of tocopheryl succinate on benzo(a)pyrene (B[a]P)-induced forestomach tumors was studied in Kunming mice. 57 Thirty female mice were used per group. Negative and vehicle (corn oil) control groups were dosed with 1 g/kg bw succinic acid by gavage 4 times per week for 4 weeks. The vehicle controls and all other mice were dosed with 1 mg/animal B(a)P, 2 times per week for 4 weeks. The test groups were dosed with 1.25 or 2.5 g/kg bw tocopheryl succinate by gavage 4 times per week or with 20 mg/kg bw tocopheryl succinate via IP injection 2 times for week, for 4 weeks. The positive control group was dosed with B(a)P only. The animals were killed 11, 16, or 29 weeks after the first dose of B(a)P.
The incidence of forestomach tumors was 100% in the positive controls, and there was an average of 5.4 tumors/mouse at week 29. Similar results were observed in the vehicle control group. With tocopheryl succinate, tumors were seen in only 81.8% and 76.9% of the mice dosed orally with 1.25 and 2.5 g/kg bw tocopheryl succinate, respectively, and only 50% of the mice dosed IP with tocopheryl succinate. The number of tumors per mouse was inhibited by 68.5% with 1.25 g/kg bw oral, 70.4% with 2.5 g/kg bw oral, and 79.6% with 20 mg/kg bw IP tocopheryl succinate. Tocopheryl succinate significantly affected total tumor volume per mouse. Total tumor volume per mouse was decreased by 63.5% and 81.1% with 1.25 and 2.5 g/kg bw tocopheryl succinate, respectively. With IP administration, total tumor volume was decreased by 84.1%.
Tocotrienols
Groups of 10 female FVB/N HER-2/neu transgenic female mice were dosed by gavage, 3 times per week, with 0, 50, or 100 mg/kg tocotrienols (10% γ-tocotrienol and 90% δ-tocotrienol) in olive oil to determine the effect of tocotrienols on the development of mammary tumors. 58 The appearance of tumors was significantly delayed in high-dose animals, and a statistically significant decrease in week 26 tumor volume was also observed in this group. There were no statistically significant differences in the incidence of metastasis or the kinetics of tumor incidence on tumor volume and multiplicity between the treated and control groups.
Photocarcinogenicity
Tocopherol
Female SKH-1 mice were exposed dorsally to 2,250 J/m2 UVB (equivalent to 1 MED) 3 times per week for 10 weeks, and the animals were then dosed topically with vehicle (Surgilube; n = 20) or 5 mg
Tumor Promotion
Dermal
Tocopherol
The ability of dermally applied Protocol A: A single topical application of 10 nmol of the tumor initiator 7,12-dimethylbenz[a]anthracene (DMBA) was applied; 1 week later, the proposed tumor promoter was applied topically 2×/week. Test groups were exposed to 80 μmol tocopherol, with and without 80 μmol vitamin C. Protocol B:A single topical application of 10 nmol DMBA; 1 week later, the proposed promoter was applied topically 2×/week. Test group were exposed to 8 or 80 μmol tocopherol, with and without 80 μmol vitamin C. Protocol C: Tocopherol was applied topically 2×/week for 4 weeks; a single topical application of 10 nmol DMBA followed; 1 week later, 4 μg of the weak tumor promoter mezerein was applied topically 2×/week. The test group was exposed to 80 μmol tocopherol. Protocol D: The proposed promoter or the promoter and90Sr/90Y β-radiation were applied topically 2×/week for 4 weeks; a single topical application of 10 nmol DMBA followed; 1 week later, 4 μg mezerein was applied topically 2×/week. Test groups were exposed to 8 μmol tocopherol without vitamin C and to 80 μmol tocopherol with and without 80 μmol vitamin C.
Protocols A and C determined the number of tumors/animal (tumor multiplicity) 98 days after initiation with DMBA; protocols B and D determined tumor multiplicity 153 days after initiation with DMBA. With protocols A and B, tocopherol caused a statistically significant increase in tumors. Using protocol B, the low concentration of tocopherol did not produce tumors, with or without vitamin C.
Following protocols C and D, application of tocopherol prior to initiation with DMBA and then promotion with mezerein statistically significantly increased the tumor multiplicity. The increase in tumor multiplicity compared to controls was greater when measured after 98 days than after 153 days. β-Radiation amplified the effect of high-dose tocopherol; however, using protocol D, vitamin C did not. The difference in tumor multiplicity in groups exposed to β-radiation → DMBA → mezerein, 8 μmol tocopherol → DMBA → mezerein, or tocopherol, 8 μmol + β-radiation → DMBA → mezerein was not statistically significant from the group exposed to DMBA → mezerein. Also, tumor multiplicity in the group exposed to tocopherol, 80 μmol + vitamin C, 80 μmol → DMBA → mezerein was not significantly different from the group exposed to 80 μmol tocopherol → DMBA → mezerein. Pretreatment with tocopherol prior to DMBA reduced tumor latency.
Antiproliferative Effects/Proapoptotic Effects
The effect of α- and γ-tocopherol and α- and γ-tocotrienols on proliferation and apoptosis was examined in rat normal hepatocyte (RLN-10) and hepatoma (dRLh-84) cells. 61 γ-Tocotrienols had the greatest effect in rat hepatoma cells; 50 to 100 μmol/L γ-tocotrienols strongly decreased cell number in a dose-dependent manner after 24 hours; γ-tocotrienols strongly suppressed proliferation of dRLh-84 cells, and 25 mmol/L γ-tocotrienols induced DNA fragmentation in dRLh-84 cells. α-Tocotrienols also exerted effects, but to a lesser extent. α- and γ-Tocopherol did not affect cell number, proliferation or DNA fragmentation. The researchers stated that the results suggested that caspase-8 activity was involved in the induction of apoptosis by tocotrienols.
Dermal Effects
Dermal Irritation and Sensitization
Nonhuman
Tocopherol
Tocopheryl acetate
According to robust summary data submitted to ECHA, tocopheryl acetate is not irritating to rabbit skin. A 2.5 cm2 semiocclusive patch containing 0.5 mL undiluted tocopheryl acetate was applied to a shaved area on the back or the flank of 2 male and 1 female Vienna white rabbits, and no erythema or edema was observed. The test sites were scored 30 to 60 minutes after patch removal and at 24, 48, and 72 hours after application. In a similar study using 6 New Zealand white rabbits, application of an occlusive patch containing 0.5 mL tocopheryl acetate to intact and abraded skin did not result in erythema or edema, and the PII was 0.
Tocopheryl phosphate
Mixed tocopheryl phosphate was not a dermal irritant in New Zealand rabbits. 50 A dose of 0.5 g/site of an aqeous gel containing 88 to 101 mg/kg bw MTP (38.4 71-82 mg/kg bw α-tocopherol equivalents) was applied to a 10 cm2 area of clipped dorsal skin of 1 male and 2 female rabbits. The semiocclusive patch was removed after 4 hours, and the test site was scored for irritation at 1, 24, 48, and 72 hours after patch removal. The only observation was a barely perceptible erythema observed in the male at 60 minutes.
An LLNA was performed to evaluate the sensitization potential of MTP, and no evidence of sensitization was observed. 50 Groups of 5 female CBA/J mice were dosed with 25 μL of 5%, 10%, or 25% MTP in reverse osmosis water (corresponding to 1.13, 2.26, or 5.65 mg MTP, respectively); the test article was applied to the dorsal aspect of the ear daily for 3 consecutive days. On day 6, the animals were given a single intravenous injection of [H3]-thymidine, and then killed 5 hours after the injection. Several negative controls and a positive control (25% hexylcinnamaldehyde in acetone/olive oil) were used.
Tocotrienols
Undiluted TRF(composed of 50% tocotrienol/tocopherol complex, with 20%
Human
Tocopherol
The Mayo Clinic, Arizona, compared its positive patch-test reaction rate to tocopherol between June 1987 and December 1997 to that observed during 1998 and 2007. 65 From 1987 and 1999, various concentrations of α-tocopherol in petrolatum were tested; these concentrations were not specified. In 2000 to 2005, patients were patch tested with 10% α-tocopherol acetate in petrolatum; from 2005 onward, undiluted α-tocopherol was used. During the period June 1987 to December 1997, 1,136 patients were patch-tested with tocopherol; 6 (0.53%) patients had a positive patch-test reaction to tocopherol. A total of 1,814 patients were patch-tested in 1998 to 2007, 11 patients had a positive reaction to α-tocopherol in petrolatum, and 1 reacted to undiluted tocopherol for a positive reaction rate of 0.66%. The difference in positive reactions was not statistically significant.
The North American Contact Dermatitis Group (NACDG) patch tested 4,454 patients in 2005 to 2006.
66
Finn Chambers were applied for 48 hours, and the test sites were read 48 to 72 hours and 72 to 186 hours after patching. The frequency rate of positive patch-test reactions to undiluted
The reaction rate to undiluted
Tocopheryl acetate
A cuticle softener containing 36% tocopheryl acetate was essentially nonirritating in clinical testing. 68 A 24-hour single-insult occlusive patch test was conducted in 19 participants. One participant had a + reaction, and the PII was 0.03.
According to robust summary data submitted to ECHA,
Tocotrienols
At concentrations ≤5%, TRF was not an irritant in a patch test or a sensitizer in human repeated insult patch test (HRIPT); irritant reactions were observed at higher concentrations. 64 The patch test was performed by applying Finn chambers containing 0%, 1%, 2.5%, 5%, 7.5%, 10%, and 20% TRF in petrolatum to the backs of 30 participants for 48 hours. The test sites were evaluated 48 and 96 hours after application of the test material using the methods of the International Contact Dermatitis Research Group\. No irritation reactions were observed with 1, 2.5, or 5% TRF at 48 or 96 hours. However, reactions were observed upon patch removal with higher concentrations, ranging from doubtful erythema with 7.5% TRF to moderate-to-well-defined erythema (total skin reaction score of 9) with 20% TRF. These reactions subsided by 96 hours of reading. Sodium lauryl sulfate was highly irritating, with total skin reaction scores of 44 and 32 at the 48 and 96 hours, respectively.
An occlusive HRIPT of 2.5% and 5% TRF in petrolatum was conducted in 25 participants. Sodium lauryl sulfate was used as a positive control, and an untreated site as a negative control. The induction patches were applied for 24 hours; the test site was evaluated 30 minutes after patch removal, and the site was then repatched. A 2-week nontreatment period followed the 21-day induction period, and then a 48-hour challenge patch was applied to a previously unexposed site. Challenge readings were made 48 and 96 hours after patch removal. Both 2.5% and 5% TRF had cumulative irritation scores that were lower than the negative control (4 and 7 for 2.5% and 5% TRF, respectively, compared to 14 for the negative control). After challenge, 2 participants had transient reactions at the 48 hours of reading; no reactions were observed after 96 hours.
Contact Allergy: Case Reports
Numerous case reports were presented in the original CIR report on tocopherol-containing products, and additional reports have been published since the original CIR report was issued (Table 7). 69 –73
Case Reports.
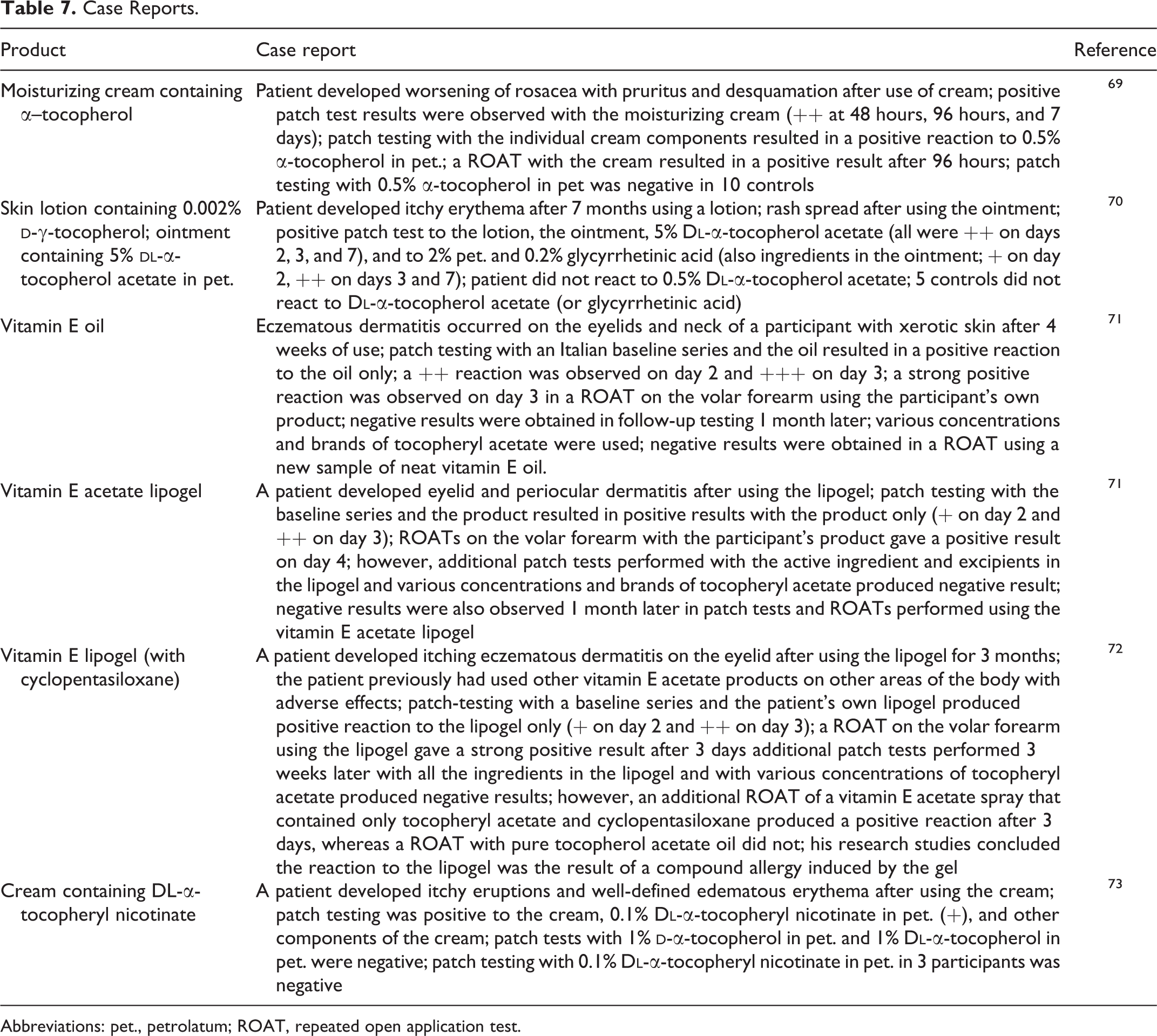
Abbreviations: pet., petrolatum; ROAT, repeated open application test.
Phototoxicity and Photoallergenicity
According to the original CIR report on tocopherols, tocopheryl acetate, 0.2 mL applied under an occlusive patch for 24 hours prior to irradiation, was not phototoxic in a study in 11 participants. 1
Nonhuman
Tocopheryl acetate
According to robust summary data submitted to ECHA,
A slight erythematous skin reaction was observed in 2 of the 20 test animals following challenge; no consistent or significant differences were detected between the irradiated and the nonirradiated test sites, and the reactions were not clearly dependent on the test article concentration. It was stated that the reactions most likely resulted from cutaneous hyperirritability. No reactions were observed in the control group.
Photoprotective Effects
Nonhuman and human studies have been conducted to examine whether tocopherols have a photoprotective effect (Table 8). Generally, the nonhuman studies have assessed the protection against oxidative damage in the skin. The human studies examined phototoxic effects and changes in MED.
Photoprotective Effects.
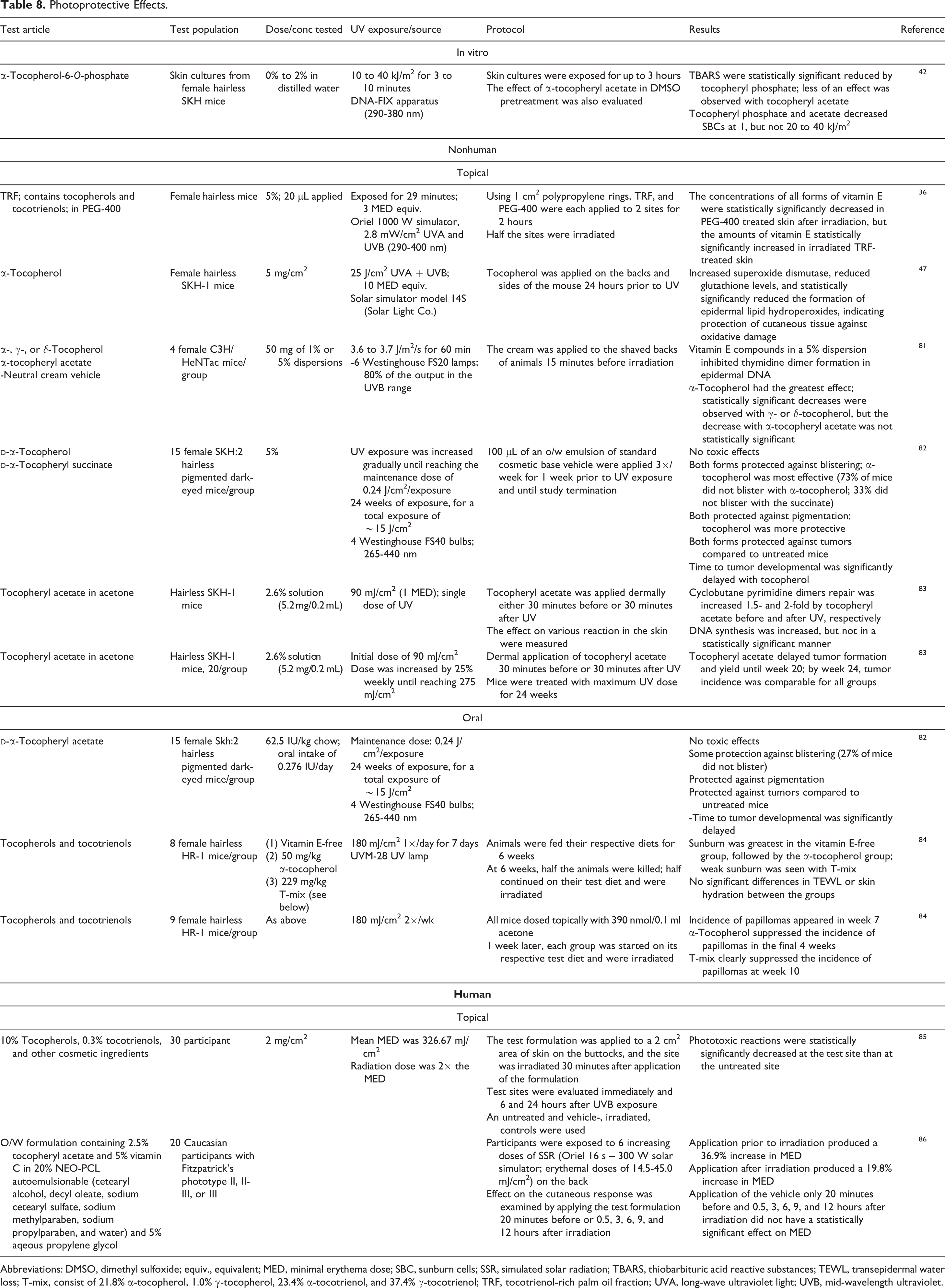
Abbreviations: DMSO, dimethyl sulfoxide; equiv., equivalent; MED, minimal erythema dose; SBC, sunburn cells; SSR, simulated solar radiation; TBARS, thiobarbituric acid reactive substances; TEWL, transepidermal water loss; T-mix, consist of 21.8% α-tocopherol, 1.0% γ-tocopherol, 23.4% α-tocotrienol, and 37.4% γ-tocotrienol; TRF, tocotrienol-rich palm oil fraction; UVA, long-wave ultraviolet light; UVB, mid-wavelength ultraviolet.
Effect on Irritated Skin
Nonhuman
Tocopheryl acetate
The effect of tocopheryl acetate ointment containing 15% squalane on allergic contact dermatitis was investigated in male Wistar rats. 48 Allergic contact dermatitis was induced with 2,4-dinitrochlorobenzene (DNCB)-acetone, and 0.1 g tocopheryl acetate ointment was applied to the test site after the initiation of inflammation. The ointment was applied using a 2 cm diameter film, and the film was covered with gauze and a bandage. The tocopheryl acetate ointment inhibited allergic contact dermatitis in a dose-dependent manner, with significant inhibition of erythema observed with 20% to 40% tocopheryl acetate. An ointment with 2% to 10% tocopheryl acetate had an inhibitory effect on erythema. The inhibition was confirmed microscopically in keratinocytes from skin samples taken from the treated area.
The researchers then examined the effect of the tocopheryl acetate ointment on DNCB-acetone-induced irritant contact dermatitis on the backs of male Wistar rats; the ointment was applied in the same manner as described previously. The ointment with 20% tocopheryl acetate significantly reduced erythema.
The researchers also examined the effect of the ointment on irritant contact dermatitis in mice. Irritant contact dermatitis was induced in male ddY mice by applying phorbol 12-myristate 13-acetate-acetone to the ears of each animal; 20 mg of the tocopheryl acetate ointment was then applied to both sides of the ear. The 20% tocopheryl acetate ointment significantly reduced ear swelling.
Tocotrienols
Tocotrienols reduced allergic dermatitis in mice. 74 Allergic dermatitis was induced in male NC/Nga mice using picryl chloride, with and without oral administration of 1 mg/d/animal tocotrienols in vitamin E-stripped corn oil for 1 week prior to sensitization. Scratching behavior, dermal thickening, and serum histamine levels were statistically significantly reduced by tocotrienol administration. Subsequent studies concluded that tocotrienols significantly suppressed degranulation of mast cells and significantly reduced histamine release, and it also suppressed protein kinase C activity.
Effect on Barrier Function of Damaged Skin
Nonhuman
Tocopheryl acetate
Skin barrier function in male Wistar rats was damaged using a detergent and DNCB, and the effect of tocopheryl acetate on the damaged skin was evaluated. 48 The damaged test site was covered for 18 hours with 0.1 g tocopheryl acetate ointment; ointments containing 2% to 40% tocopheryl acetate were used. Ointment containing 2% tocopheryl acetate had little effect on damaged skin. However, concentrations of 5% to 40% tocopheryl acetate statistically significantly reduced the increase in transepidermal water loss; the maximum effect was observed with 20% tocopheryl acetate. The 20% ointment also statistically significantly decreased the erythema intensity.
Epidemiology and Dietary Supplementation
Health claims exist in the literature regarding vitamin E supplementation 75 ; however, the benefits of vitamin E supplements are still being debated. The original CIR safety assessment on tocopherol referred to numerous studies in which tocopherol appeared to have protective effect in carcinogenicity modulation studies. 1 However, as an example of possible negative effect of vitamin E, dietary supplementation with α-tocopherol was reported to significantly increase the risk of prostate cancer among healthy men in the Selenium and Vitamin E Cancer Prevention Trial. 76 Although the CIR recognizes that there is a large body of literature on the effects of vitamin E supplementation, these articles are not relevant to the cosmetic use of the tocopherols.
Summary
Tocopherol is the component most commonly associated with vitamin E. This assessment report addresses the safety of tocopherol, tocopherol-derived ingredients, and tocotrienols as used in cosmetics. In 2002, the Panel published a report assessing the safety of tocopherol and some of these tocopherol-derived ingredients, concluding these are safe as used in cosmetics. However, in this current assessment, tocotrienols and some additional tocopherol-derived ingredients, as used in cosmetics, are assessed for the first time. Accordingly, this report includes only information that has become available since the 2002 CIR safety assessment was issued on tocopherol and the originally assessed tocopherol-derived ingredients for the ingredients that were previously reviewed and all information (ie, data search not date restricted) on tocotrienols and the newly added tocopherols.
Most of the tocopherols are reported to function in cosmetics as antioxidants or skin-conditioning agents; tocotrienols are not reported to function as an antioxidant, instead it is reported to function as a light stabilizer, oral care agent, or skin-conditioning agent. Voluntary Cosmetic Registration Program data obtained from the FDA in 2014 report that the frequency of use increased considerably for both tocopherol and tocopheryl acetate. The reported use of tocopherol increased from 1,072 (1998 data) to 6,635 uses (2014 data), and the reported use of tocopheryl acetate increased from 1,322 (1998 data) to 9,677 uses (2014 data). The use concentration of tocopherol, but not of tocopheryl acetate, has increased since the original assessment. According to the survey conducted by the Council in 2013, the concentration of use of tocopherol in leave-on products increased from 2% in 1999 to 5.4% in 2013. Tocotrienols is used in 433 formulations, with a reported maximum leave-on concentration reported of 0.12%.
Tocopherols and tocotrienols are distributed throughout the body, and the distribution and metabolism varies among the tissues. Tocopherol is the predominant form of vitamin E in human and animal tissues, and it has the highest bioavailability; natural vitamin E has approximately twice the systemic availability of synthetic tocopherol. The distribution and intracellular trafficking of vitamin E may be modulated by tocopherol regulatory proteins, but only one of the proteins, TTP, has been shown to influence plasma and tissue α-tocopherol concentrations.
The structural differences between tocopherol and tocotrienols result in a difference in the penetration of these compounds into tissues. The presence of 3 unsaturations in the carbon side chain benefits tocotrienols to penetrate tissues with saturated fatty layers, such as the brain and the liver, more readily than tocopherol, which has a fully saturated carbon side chain. However, the tocotrienols are not as prevalent in the body as the tocopherols, and oral absorption of the tocotrienols has been reported to be incomplete. Orally administered tocopherols and tocotrienols are distributed in the skin and adipose tissue. Dermally applied tocopheryl acetate is hydrolyzed to tocopherol upon exposure to UV. Dermally applied tocopherols penetrate the skin.
Toxicity of dermally applied (single-dose) tocopheryl acetate and tocopheryl phosphate and orally administered tocophersolan (repeated dose) or tocopheryl phosphate (single and repeated-dose) is not remarkable. In rats fed a diet containing ≤3% tocotrienols for 13 weeks, a statistically significant decrease in platelets in males, but not females, was interpreted to be a physiologic response.
Undiluted tocopheryl acetate was not irritating to rabbit eyes in 1 study, but it produced weak-to-moderate conjunctival irritation in another study. Undiluted MTP was not irritating to rabbit eyes.
Numerous genotoxicity studies were conducted with tocopherol, tocopheryl acetate, MTP, and tocopheryl succinate. The only remarkable result was tocopheryl succinate with only a weak positive in a sister chromatid exchange assay in the presence of metabolic activation.
Topical treatment of SKH-1 mice with 5 mg
Undiluted tocopheryl acetate was not irritating to rabbit skin, and tocopheryl acetate did not have photoallergenic effects in guinea pigs. A cuticle softener containing 36% tocopheryl acetate was essentially nonirritating in a single-insult occlusive patch test in 19 subjects, and undiluted tocopheryl acetate is not a sensitizer in humans.
An aqueous gel containing 88 to 101 mg/kg bw MTP was not irritating to rabbit skin nor was undiluted palm TRF. No evidence of sensitization was observed in an LLNA with MTP. In clinical testing, TRF was not an irritant in humans at concentrations up to 5%; however, reactions were observed at higher concentrations, ranging from doubtful erythema with 7.5% TRF to moderate-to-well-defined erythema (total skin reaction score of 9) with 20% TRF. Tocotrienol-rich palm oil fraction, 2.5 and 5%, was not a cumulative irritant or a sensitizer in an HRIPT in 25 participants.
Tocopherol, tocopheryl acetate, and tocopheryl phosphate had some photoprotective effects in mice, and tocopherol and tocopheryl acetate were shown to have a photoprotective effect in humans. Tocopheryl acetate inhibited contact dermatitis in rats and reduced erythema, and tocotrienols reduced allergic dermatitis in mice.
The CIR recognizes that many articles on the effects of vitamin E supplementation can be found in the published literature; however, these articles are not included in this safety assessment because they are not relevant to the cosmetic use of the tocopherols.
Discussion
The Panel determined that the 2002 safety assessment on tocopherols should be expanded to include tocotrienols (a 2013 CIR priority ingredient) and 4 additional tocopherols. Although data were not available on all of the ingredients, the Panel found the existing data on the tocopherols are sufficient to support the safety of this entire family of ingredients.
The Panel noted that the current reported maximum use concentration of tocopherol (ie, 5.4%) is higher than what was reported in the original assessment (ie, 2%) and that irritation and sensitization data at these higher concentrations are not available for tocopherol. The Panel discussed the issues of irritation and sensitization during both the original and the current review of tocopherols and, in both instances, determined that the irritation and sensitization potentials of the ingredients included in this review were not of concern. In the 2002 safety assessment, the Panel was initially concerned with possible irritation and sensitization because of a large number of occurrences reported in Switzerland with the release of a new line of cosmetics that contained tocopheryl linoleate; however, the researchers thought the occurrences were due to either a contaminant or a metabolite. Other safety data in the 2002 report indicated that tocopherol was not an irritant or a sensitizer. Irritation and sensitization data that are available since the 2002 review was issued indicate that tocopheryl acetate is not an irritant or a sensitizer, and tocopheryl phosphate is not a sensitizer. Additionally, the Panel commented that although moderate sensitization potential was reported in a guinea pig maximization test of
Tocopherol has some absorption in the UV range. However, the Panel noted that according to animal and clinical testing, tocopheryl acetate was not photoallergenic or phototoxic.
During the original review of tocopherols, the Panel did carefully consider that the tumor promoting ability of tocopherol, tocopheryl acetate, and tocopheryl succinate had been extensively studied. In most studies, tocopherol is reported to inhibit tumor promotion, and studies published since the original tocopherol report seem to support this conclusion. The general experience of the Panel is that tocopherol is not a tumor promoter. Additionally, photocarcinogenicity testing with tocopherol did not raise any concerns for the Panel.
The Panel also noted that results of epidemiology and dietary supplementation studies are inconclusive; positive and negative results on the health effects of vitamin E have been observed with the use of vitamin E supplements. The Panel stated that the systemic exposure of vitamin E supplementation is much higher than that expected during cosmetic use; therefore, any adverse conclusions made during these studies did not cause concern for the cosmetic use of these ingredients.
Tocopherols and tocotrienols can be plant derived. However, these ingredients are specific, purified, highly enriched lipid compounds, and the tocopherols often are produced synthetically. For these reasons, the usual concerns expressed during the discussion of botanical ingredients did not apply to the ingredients in this report.
Finally, the Panel discussed the issue of incidental inhalation exposure to tocopherols. The Panel stated that although there were no inhalation data available, the tocopherols are used at relatively low concentrations in products that could incidentally be inhaled; for example, tocopheryl acetate is used at up to 5% in foot powders and sprays and up to 0.2% in aerosol hair spray formulations, and tocopherol is used at up to 1% in pump hair spray formulations. The Panel noted that in aerosol products, 95% to 99% of droplets/particles would not be respirable to any appreciable amount. Furthermore, droplets/particles deposited in the nasopharyngeal or bronchial regions of the respiratory tract present no toxicological concerns based on the chemical and biological properties of these ingredients. Coupled with the small actual exposure in the breathing zone and the concentrations at which the ingredients are used, the available information indicates that incidental inhalation would not be a significant route of exposure that might lead to local respiratory or systemic effects. A detailed discussion and summary of the Panel’s approach to evaluating incidental inhalation exposures to ingredients in cosmetic products is available at http://www.cir-safety.org/cir-findings.
Conclusion
The Panel concluded that the following 14 ingredients are safe in cosmetics in the present practices of use and concentration described in this safety assessment: Ascorbyl tocopheryl acetate*
Ascorbyl tocopheryl maleate Dioleyl tocopheryl methylsilanol Potassium ascorbyl tocopheryl phosphate Sodium tocopheryl phosphate Tocopherol Tocophersolan Tocopheryl acetate Tocopheryl linoleate Tocopheryl linoleate/oleate Tocopheryl nicotinate Tocopheryl phosphate*
Tocopheryl succinate Tocotrienols
Footnotes
Author Contributions
Monice M. Fiume and Bart Heldreth contributed to conception and design, contributed to acquisition, analysis, and interpretation, drafted manuscript, and critically revised manuscript; F. Alan Andersen, Wilma F. Bergfeld, Donald V. Belsito, Ronald A. Hill, Curtis D. Klaassen, Daniel C. Liebler, James G. Marks, Ronald C. Shank, Thomas J. Slaga, and Paul W. Snyder contributed to conception and design, contributed to analysis and interpretation, and critically revised manuscript. All authors gave final approval and agree to be accountable for all aspects of work ensuring integrity and accuracy. Unpublished sources cited in this report are available from the Executive Director, Cosmetic Ingredient Review, 1620 L Street, NW, Suite 1200, Washington, DC 20036, USA.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The articles in this supplement were sponsored by the Cosmetic Ingredient Review. The Cosmetic Ingredient Review is financially supported by the Personal Care Products Council.
