Abstract
Tavaborole is a topical antifungal agent approved by the US Food and Drug Administration for the treatment of toenail onychomycosis. The effects of tavaborole on gestation, parturition (delivery, labor), offspring development, and survival during the perinatal and postnatal periods were assessed in mated female rats. Females (F0 generation) were administered single daily oral (gavage) doses of 15, 60, or 100 mg/kg/d from gestation day 6 through lactation day 20. The females were allowed to deliver naturally and rear their offspring until lactation day 21, at which time the F0 females were euthanized. One male and female from each litter were selected (F1 generation) and retained for assessments, including growth, neurobehavior, fertility, and their ability to produce an F2 generation. Reproductive and offspring parameters were determined for the F1 and F2 generations, as applicable. F1 females and F2 pups were euthanized on postnatal day 7. In the F0 females, decreased activity was observed in the 100 mg/kg/d dose group. Excess salivation was observed in the 60 and 100 mg/kg/d dose groups (slight to moderate), however, this finding was not considered adverse. There were no tavaborole-related effects on the growth, viability, development, neurobehavioral assessments, or reproductive performance of the F1 generation. Survivability and mean body weight of the F2 pups were unaffected. The no observed adverse effect level (NOAEL) for maternal toxicity (F0 generation) was 60 mg/kg/d, based on the decreased activity observed in the 100 mg/kg/d dose group. The NOAEL for the offspring effects was ≥100 mg/kg/d, based on the lack of test article-related changes.
Introduction
Onychomycosis is a fungal infection of the nail unit (primarily the nail bed and often involving the nail plate and less frequently the nail matrix), most commonly occurring in the toenails. Typically, the infection is caused by dermatophytes, which are ubiquitous in the environment and are the same organisms associated with athlete’s foot, jock itch, and ringworm. A large proportion of the population is susceptible to dermatophyte infections and there does not appear to be a protective adaptive immune response, so reinfection is common in the susceptible population. 1,2
Treatment options include oral and topical drugs. Limitations of the currently approved oral therapies include drug–drug interactions and systemic adverse effects, including hepatotoxicity. 3 -7
Tavaborole (CAS #174671-46-6) is a topical antifungal agent approved by the US Food and Drug Administration (FDA) indicated for the topical treatment of onychomycosis of the toenails due to Trichophyton rubrum or Trichophyton mentagrophytes.
Tavaborole topical solution, 5% (Kerydin; Anacor Pharmaceuticals, Inc, Palo Alto, California), is a cyclized boronic acid complex (5-fluoro-1,3-dihydro-1-hydroxy-2,1-benzoxaborole; Figure 1). This novel, low-molecular-weight (152 Da) pharmaceutical compound demonstrates potent antifungal activity against dermatophytes with minimum inhibitory concentration values in the low mg/mL range. 8
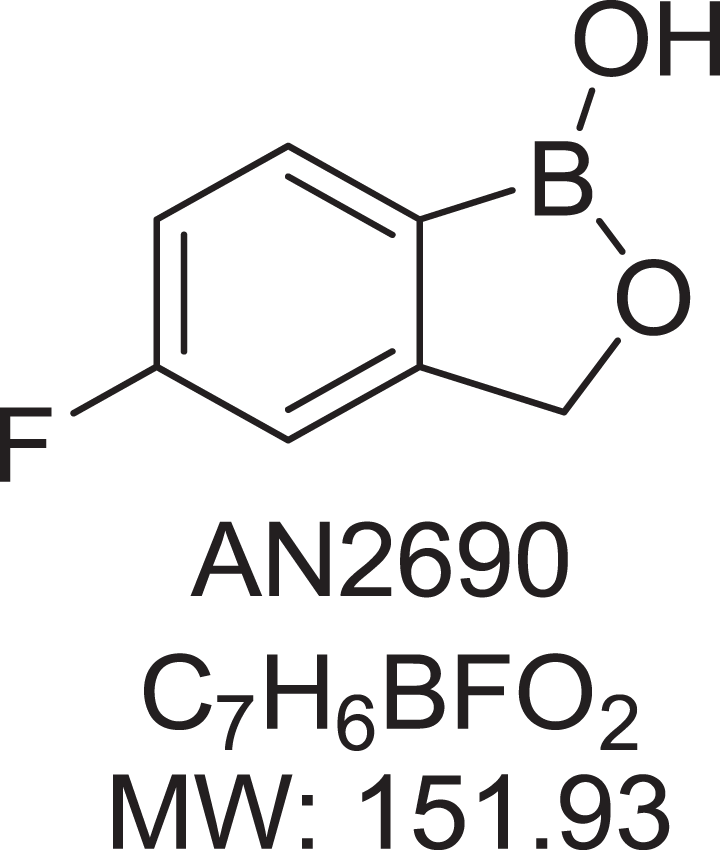
Chemical structure of tavaborole (AN2690).
The mechanism of action of tavaborole is the inhibition of fungal protein synthesis through inhibition of leucyl-tRNA synthetase, an aminoacyl-tRNA synthetase (AARS). 9 Although tavaborole inhibits an AARS, its mechanism of action is different from that of known AARS inhibitors and represents a new class of inhibitors that exert their action on AARSs via the editing domain. Preclinical studies, including a battery of genetic toxicology studies 10 and carcinogenicity studies, 11 have demonstrated the safety of this compound. For women of childbearing potential, there is a high level of concern for the unintentional exposure of an embryo or fetus. In support of the clinical development of tavaborole, reproductive and developmental toxicity studies were conducted to provide information on the potential hazard, if any, to the unborn that may arise from drug exposure of the mother during pregnancy and lactation.
As part of the nonclinical development program, reproductive and developmental toxicity studies were conducted (rat fertility and early embryonic development, rat and rabbit embryo–fetal development [oral and dermal administration]), 12 and as reported here, a rat prenatal and postnatal development study. There were no effects on fertility or reproductive performance at doses up to 300 mg/kg/d (107 times the maximum recommended human dose [MRHD] based on the mean area under the curve [AUC] comparisons). In an oral embryo–fetal development study in rats, oral doses of 30, 100, and 300 mg/kg/d tavaborole were administered to pregnant female rats. In the presence of maternal toxicity, embryo–fetal toxicity (increased embryo–fetal resorption and/or deaths) and drug-related skeletal malformations and variations suggestive of delayed development (ie, a delay in ossification) were noted in fetuses at 300 mg/kg/d tavaborole (570 times the MRHD based on AUC comparisons). No developmental toxicity was noted in rats at 100 mg/kg/d tavaborole (29 times the MRHD based on AUC comparisons). In an oral embryo–fetal development study in rabbits, oral doses of 15, 50, and 150 mg/kg/d tavaborole were administered to pregnant female rabbits. In the presence of maternal toxicity, excessive embryo–fetal mortality due to postimplantation loss was noted at 150 mg/kg/d tavaborole. No drug-related malformations were noted in rabbits at 150 mg/kg/d tavaborole. No embryo–fetal toxicity was noted in rabbits at 50 mg/kg/d tavaborole (16 times the MRHD based on AUC comparisons). In a dermal embryo–fetal development study in rabbits, topical doses of 1%, 5%, and 10% tavaborole solution were administered to pregnant female rabbits. A dose-dependent increase in dermal irritation at the treatment site was noted at 5% and 10% tavaborole solution. A decrease in fetal bodyweight was noted at 10% tavaborole solution. No drug-related malformations were noted in rabbits at 10% tavaborole solution. No developmental toxicity was noted in rabbits at 5% tavaborole solution (26 times the MRHD based on AUC comparisons).
The objective of this study 13 was to evaluate the potential effects of tavaborole on the survival, development, and reproductive capabilities of pups (F1 generation) when administered orally by gavage to Crl: CD(SD) pregnant rats (F0 generation) from implantation through lactation. This study also evaluated potential adverse effects on gestation, parturition, lactation, and maternal behavior of the F0 female rats.
Materials and Methods
This study was conducted in an Association for Assessment and Accreditation of Laboratory Animal Care (AAALAC) accredited facility in accordance with the NRC Guide for the Care and Use of Laboratory Animals and the Animal Welfare Act, as well as in compliance with Good Laboratory Practice (GLP) Regulations 21 CFR Part 58 and the regulations of the US FDA. The study procedures were also based on the International Conference on Harmonisation (ICH) S5 guidance. 14 Analyses for homogeneity and concentration verification were conducted and found to be homogeneous and within ±15% of target concentrations.
Animals and Husbandry
One hundred nulliparous mated female rats (Crl: CD[SD]) from Charles River Laboratories, Inc (Raleigh, North Carolina) were 60 days old and weighed 188 to 226 g at arrival and were approximately 77 days old and weighed 237 to 303 g at the initiation of dosing.
The rats had been bred with male rats of the same strain and source that were maintained as a breeding colony at the testing facility. Each F0 female rat was permanently identified by a unique animal number when assigned to the study using a Monel self-piercing ear tag. In addition, each cage was labeled appropriately. Female rats (F0) were individually housed in suspended, stainless steel, wire-bottomed cages, except during the cohabitation and postpartum periods, in a room dedicated to this study. During cohabitation, each pair of rats was housed in the male rat’s cage. Beginning no later than gestation day 20, females (F0) were individually housed in nesting boxes containing nesting material. Each dam and her delivered litter were housed in a common nesting box during the postpartum period. Bed-o’cobs bedding (The Anderson’s Industrial Products Group, Maumee, Ohio) was used as the nesting material. After weaning, the F1 rats were individually housed before and after cohabitation and housed in pairs (1 male rat per female rat) during cohabitation. The same type of caging was used as described for the F0 females. Each dam and her delivered F2 litter were housed in a common nesting box during the postpartum period. All cage sizes were in compliance with the Guide for Care and Use of Laboratory Animals. 15
The study rooms were maintained under conditions of positive airflow relative to a hallway and independently supplied with a minimum of 10 changes per hour of 100% fresh air that had been passed through 99.97% high-efficiency particulate absorption filters. Room temperature and humidity were monitored constantly throughout the studies. Room temperature was targeted at 64°F to 79°F (18°C-26°C), and relative humidity was targeted at 30% to 70%. A 12-hour light–dark cycle was maintained, with each dark cycle beginning at 1,900 hours ± 30 minutes.
PMI Nutrition International (St Louis, Missouri), Certified Rodent Diet #5002 (meal) and local water that had been processed by passage through a reverse osmosis membrane (RO water) from an automatic watering system and/or from water bottles attached to the cages were provided ad libitum. Fresh food was presented at food weighing intervals. Chlorine was added to the processed water as a bacteriostat.
Test Substance
Tavaborole powder was manufactured by Anacor Pharmaceuticals, Inc. Tavaborole oral suspensions were prepared in 1% (wt/vol) aqueous carboxymethylcellulose (medium viscosity) United States Pharmacopeia grade (Sigma-Aldrich, St. Louis, Missouri) using reverse osmosis membrane-processed deionized water at appropriate concentrations to meet dose level requirements. Stability of the prepared formulations bracketing the range of concentrations was evaluated prior to the study. Concentration and homogeneity of the formulations were monitored during the study and found to be within acceptable criteria of ±10% of their mean nominal concentrations. For homogeneity, the relative standard deviation for the formulation for the grand mean of the average value for the top, middle, and bottom formulations for each group was ±3%.
Animals and Test Article Administration
Time-mated female Sprague Dawley rats [Crl: CD®(SD)] IGS BR], approximately 11 weeks old at the time of dosing, were received from Charles River Laboratories (Raleigh, North Carolina). There were 25 rats/sex/group. Rats were administered tavaborole at 0 (vehicle control: 1% [wt/vol] carboxymethylcellulose), 15, 60, or 100 mg/kg/d via oral gavage once daily at a dose volume of 5 mL/kg.
Mating and Treatment
Females were placed with untreated male rats (1:1) of the same strain and from the same supplier for mating. Cohabitation continued until positive evidence of mating was found (copulatory plug and/or sperm in a vaginal smear), at which time each mated female was returned to its own cage. The cohabitation period consisted of a maximum of 5 days. Formulations (suspensions) of tavaborole were prepared daily until stability of the prepared formulations was established, after which formulations were prepared at least once weekly at the testing facility. Prepared suspensions were stored refrigerated (2°C-8°C) and stirred continuously during dose administration. F0 female rats were dosed orally via gavage once daily from gestation day 6 through lactation day 20 (lactation day 0 = day of parturition; rats that delivered a litter) or gestation day 24 (rats that did not deliver a litter). Any dam in the process of parturition was not dosed until the following day. The actual volume administered to each rat was calculated from the most recent body weight data, which was measured, when scheduled, prior to dose administration. F1 generation pups were not directly given the test article and/or control article but may have been possibly exposed to the test article and/or control article during maternal gestation (in utero exposure) or via maternal milk during the lactation period. F2 generation pups were not given the test article and/or control article. The study design and treatment regimen for the F0 generation and F1 generation are presented in Table 1.
Study Design.
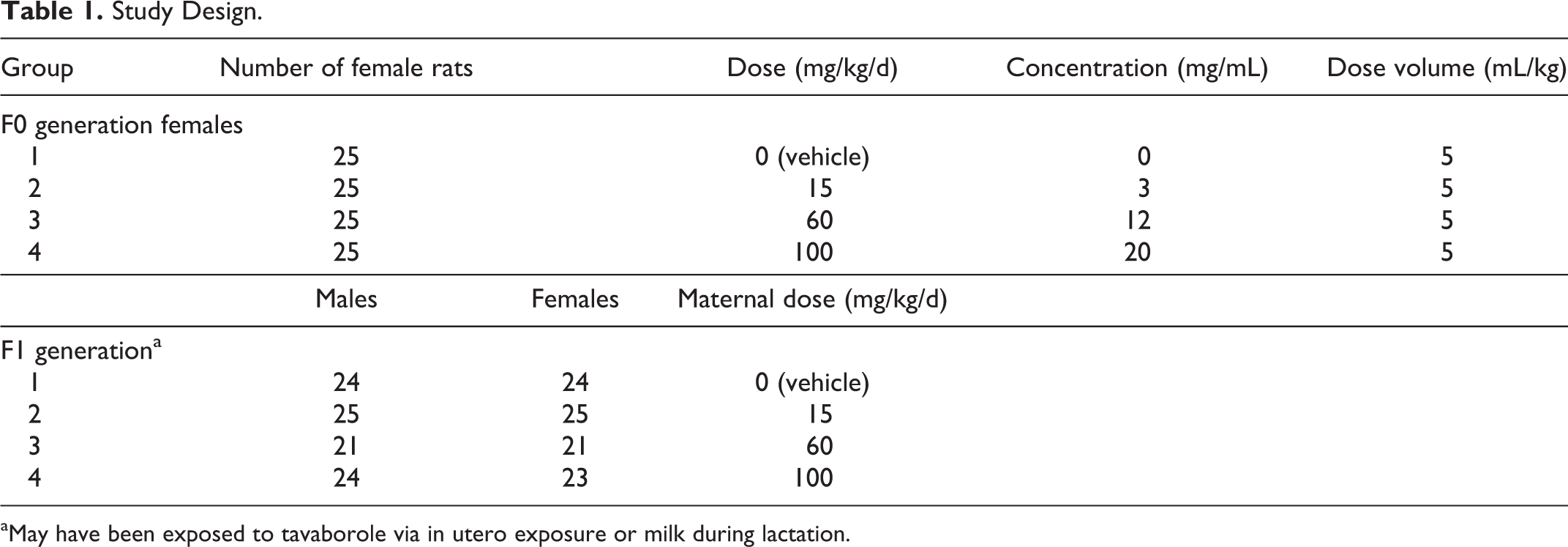
aMay have been exposed to tavaborole via in utero exposure or milk during lactation.
Observations and Measurements—F0 Generation
All rats were observed for viability at least twice daily. All F0 female rats were examined at least weekly for changes in appearance and behavior during the acclimation period and on gestation day 0. During the dosing period, clinical observations were recorded before dosing and 15 (±5) minutes postdose (oral gavage). Maternal behavior was recorded at least daily.
F0 female rats were weighed at least weekly during the acclimation period, on gestation days 0, 6, 9, 12, 15, 17, 21, and 25 (when necessary), and on lactation days 1, 4, 7, 14, and 21 (terminal weight). F0 female food consumption was recorded for gestation days 0 to 6, 6 to 12, 12 to 17, 17 to 21, and 21 to 25 (when necessary) and lactation days 1 to 4, 4 to 7, 7 to 10, 10 to 14, and 1 to 14. F0 female rats were observed daily for the following natural delivery parameters: clinical observations during parturition, duration of gestation, length of parturition, litter size, and pup viability at birth.
Necropsy—F0 generation
F0 female rats were euthanized by CO2 inhalation on lactation day 21. All rats were examined for external and visceral changes. A gross necropsy of the thoracic, abdominal, and pelvic viscera was performed. A table of random units was used to select 1 control group rat from which all tissues examined at necropsy were retained, in order to provide control tissues for any possible histopathological evaluations of gross findings. Females that did not produce litters were euthanized on gestation day 25. The uteri of apparently nonpregnant rats were examined for evidence of implantations by ammonium sulfide staining. 16 Uteri and ovaries of nonpregnant rats were retained in neutral-buffered 10% formalin and were discarded at the end of the study upon authorization of the study director. Uteri and ovaries of pregnant females were not preserved.
Observations and Measurements—F1 Generation Preweaning
On day 1 postpartum, F1 generation pups were individually identified within the litter by tattoo indicating their respective sequence numbers on that day. Ink was injected under the skin of the paws to mark the pups. F1 rats selected for continued observation were identified by a Monel self-piercing ear tag (Gey Band and Tag Co, Inc, Norristown, Pennsylvania) and a tail tattoo (using AIMS Black Pigment #242; AIMS, Inc, Piscataway, New Jersey) at weaning.
Pups in each litter were counted at least once daily during the preweaning period (until lactation day 21). Litters were also observed twice daily for viability.
Pups were sexed externally on postnatal days 1, 4, 7, 14, and 21. Pups were observed for viability at least twice daily during the postweaning period. Clinical observations were recorded once daily during the preweaning period (from postnatal day 0 until postnatal day 21) for changes in appearance and behavior and possible test article-related effects. Maternal nursing/litter behavior was recorded daily during the lactation period. Pups were individually weighed on postnatal days 1 (after all pups were delivered and groomed by the dam), 4 (prior to culling), 7, 14, and 21 during the preweaning period.
When possible, the F1 litters were culled to 8 pups per litter, preferably 4 per sex, on lactation day 4, to allow uniform pup growth. This was done by separating the pups by sex and randomly and blindly selecting 4 pups per sex using a table of random units. The remaining pups were euthanized by an intraperitoneal injection of sodium pentobarbital and given a gross external and visceral examination. These pups (F1) not selected for continued observation (culled pups) were examined for gross findings and confirmation of sex. Necropsy included a single cross-section of the head at the level of the frontal–parietal suture and examination of the cross-sectioned brain for apparent hydrocephaly. Pups found cannibalized were recorded as such, and the remains were discarded without necropsy.
Selection F1 Generation for Postweaning Evaluation
On lactation day 21, 1 male and 1 female pup were randomly selected from each litter and retained for postweaning measurements and for later breeding to produce an F2 generation. All F1 rats were weaned at the same age, based on observed growth and viability of the rats, on postnatal day 21. At weaning, a table of random units was used to select 1 male and 1 female per group for continued evaluation. The remaining rats were euthanized by CO2 inhalation and given a gross external and visceral examination. Pup sex was confirmed by internal examination. Necropsy included a single cross-section of the head at the level of the frontal-parietal suture and examination of the cross-sectioned brain for apparent hydrocephaly.
F1 Postweaning Measurements (Maturational and Behavioral Evaluations)
Clinical observations were recorded weekly during the postweaning period and on gestation days 0, 6, 9, 12, 17, 21, and 25 (when necessary; female rats only), lactation days 1, 4, and 7 (female rats only), and prior to euthanasia (all rats). Body weights were recorded weekly, on days of acoustic startle habituation, on the day of positive vaginal patency or preputial separation, on gestation days 0, 6, 9, 12, 17, 21, and 25 (when necessary, female rats only), lactation days 1, 4, and 7 (female rats only), and prior to euthanasia (all rats). Food consumption values were recorded weekly during the postweaning period (except during cohabitation) and on gestation days 0, 6, 9, 12, 17, and 21 (female rats only) and lactation days 1, 4, and 7 (female rats only). The following postweaning tests were conducted: Motor activity was evaluated on postnatal days 22 and 61 (±2 days) in 1 male and 1 female rat from each of 20 litters per dose group. Acoustic startle habituation was conducted on postnatal days 23 and 62 (±2 days) in 1 male and 1 female rat from each of 20 litters per dose group. F1 rats were tested on both days for their reactivity to auditory stimuli and habituation of responses with repeated presentation of stimuli. Passive avoidance testing was conducted beginning on postnatal day 24 ± 1 in the same rats selected for motor activity and acoustic startle habituation (when possible). The F1 females were checked daily for vaginal patency from postnatal day 28 until all females tested positive. Females were weighed on the day they tested positive for vaginal patency. The F1 males were checked daily for preputial separation from postnatal day 39 until all males tested positive. Males were weighed on the day they tested positive for preputial separation.
Estrous cycles of F1 females were evaluated by daily examination of vaginal cytology beginning 14 days prior to mating and during the mating period, until a copulatory plug and/or sperm in the vaginal smear was detected.
F1 Cohabitation and Mating
At 94 to 97 days of age, 1 F1 female from each litter was placed with 1 F1 male from a different litter within the same dose group based on a computer-generated random units table (sibling matings were avoided). Cohabitation continued for 2 weeks, until positive evidence of mating was found, at which time the mated female was returned to its own cage. When a pair of rats failed to mate, the female was paired for up to 1 more week with another nonsibling male (preferably a male that had already successfully mated) from the same dose group.
F1 Parturition
F1 females were allowed to deliver naturally and were observed daily for the following natural delivery parameters: clinical observations during parturition, duration of gestation, length of parturition, litter size, and pup viability at birth.
Necropsy—F1 Generation
Pups that died before examination of the litter for pup viability were evaluated for vital status at birth. The lungs were removed and immersed in water. Pups with lungs that sank were identified as stillborn; pups with lungs that floated were identified as liveborn and to have died shortly after birth. Pups with gross findings were preserved in Bouin solution for possible future evaluation. Pups that were found dead or were euthanized before scheduled termination were examined for gross findings and for the cause of death or condition on the day the observation was made. Pups with gross findings found on postnatal days 2 to 4 were preserved in Bouin solution for possible future evaluation; gross findings of pups found on postnatal days 5 to 21 were preserved in neutral-buffered 10% formalin.
The F1 males were euthanized after cohabitation, and the F1 females were euthanized after completion of the 7-day postpartum period by CO2 inhalation and given a gross external and visceral examination. Testes and epididymides of male rats were excised, and paired organ weights were recorded. The epididymides were retained in neutral-buffered 10% formalin. The testes were fixed in Bouin solution for 48 to 96 hours and then retained in neutral-buffered 10% formalin.
For female rats, the number of implantation sites was recorded. Rats that did not deliver a litter were euthanized on gestation (presumed) day 25 or 26 and examined for gross findings. A gross necropsy of the thoracic, abdominal, and pelvic viscera was performed. The number of implantation sites was recorded. Tissues with unusual findings were saved in 10% neutral-buffered formalin for possible histopathological examination. The rats were examined for gross findings.
Observations and Measurements—F2 Generation
Litters were examined twice daily for number alive and dead until euthanasia. Survival was calculated until lactation day 7. Pups in each litter were counted at least once daily during the postpartum period. Pups were sexed on postnatal days 1, 4, and 7. Pups were observed for viability at least twice daily and for clinical observations once daily. Body weights were recorded on postnatal days 1, 4, and 7. F2 pups were individually identified within the litter by tattoo indicating their respective sequence numbers on postnatal day 1. Ink was injected under the skin of the paws to mark the pups. Appropriate parameters were evaluated for the individual pups.
Necropsy—F2 Generation
All surviving pups were euthanized on postnatal day 7 by an intraperitoneal injection of sodium pentobarbital and examined for gross findings. Gross lesions were preserved in neutral-buffered 10% formalin. Necropsy included a single cross-section of the head at the level of the frontal–parietal suture and examination of the cross-sectioned brain for apparent hydrocephaly. Pups that died on postnatal day 1 before examination of the litter for pup viability were evaluated for vital status at birth. The lungs were removed and immersed in water. Pups with lungs that sank were identified as stillborn; pups with lungs that floated were identified as liveborn and to have died shortly after birth. Pups that were found dead or euthanized before scheduled termination were examined for gross findings and for the cause of death or condition on the day the observation was made. Pups with gross findings found on postnatal days 2 to 4 were preserved in Bouin solution for possible future evaluation; gross findings of pups found on postnatal days 5 to 7 were preserved in neutral-buffered 10% formalin.
Data Analysis
Averages and percentages were calculated. Litter values were used where appropriate. Comparative statistical analyses were performed only on body weight, body weight change, food consumption, reproductive parameters, pup viability, and postweaning developmental observations. Adult data were evaluated with the individual rat as the unit measured. Litter values were used in the evaluation of pup data, as appropriate.
Variables with interval or ratio scales of measurement, such as body weights, food consumption values, and percentage mortality per litter were analyzed as described under the parametric heading of the schematic. Bartlett’s test of homogeneity of variances 17 was used to estimate the probability that the dose groups had different variances. A nonsignificant result (P > 0.001) indicated that an assumption of homogeneity of variance was not inappropriate, and the data were compared using the analysis of variance test. 18 If that test was significant (P ≤ 0.05), the groups given the test article were compared with the control group using Dunnett’s test. 19 If Bartlett’s test was significant (P ≤ 0.001), the analysis of variance test was not appropriate, and the data were analyzed as described under the nonparametric heading of the schematic. When 75% or fewer of the scores in all the groups were tied, the Kruskal-Wallis test 20 was used to analyze the data, and in the event of a significant result (P ≤ 0.05), Dunn’s test 21 was used to compare the groups given the test article with the control group. When more than 75% of the scores in any dose group were tied, Fischer’s exact test 22 was used to compare the proportion of ties in the dose groups. Data from the motor activity and acoustic startle habituation tests, with measurements recorded at intervals (blocks) throughout each test session, were analyzed using an analysis of variance with repeated measures, 23 as described under that heading in the schematic. A significant result (P ≤ 0.05) in that test can appear as an effect of dose (differences among dose groups in the totals of all measurements in a session) or as an interaction between dose and block (differences in the patterns of dose group values across the measurement periods). If the dose effect was significant, the totals for the control group and the groups given the test article were compared using Dunnett’s test. If the dose × block interaction was significant, an analysis of variance test was used to evaluate the data at each measurement period, and a significant result (P ≤ 0.05) was followed by a comparison of the dose groups using Dunnett’s test.
Results
F0 Generation
Mortality (F0)
There was no mortality. All dams survived to scheduled euthanasia (Table 2).
Summary of Pregnancy and Mortality for F0 Generation Females.
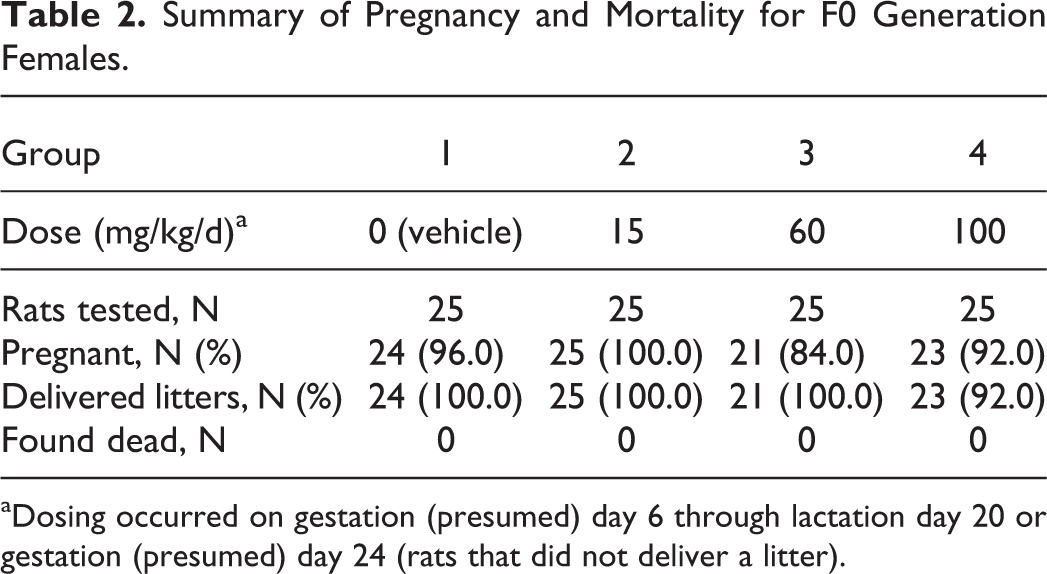
aDosing occurred on gestation (presumed) day 6 through lactation day 20 or gestation (presumed) day 24 (rats that did not deliver a litter).
Clinical observations (F0)
Clinical observations are summarized in Table 3.
Summary of Clinical Observations: F0 Generation Female Rats.a,b,c
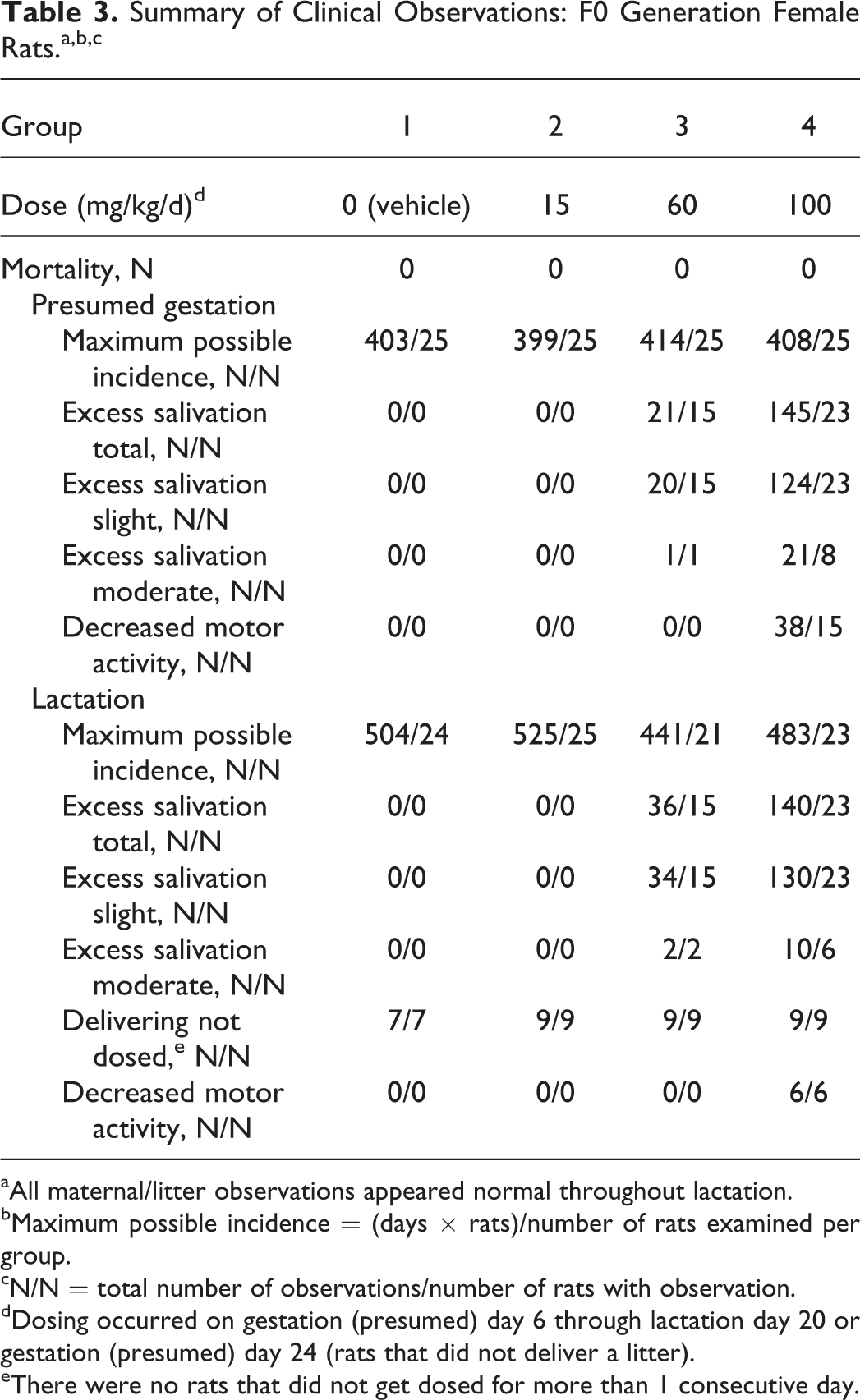
aAll maternal/litter observations appeared normal throughout lactation.
bMaximum possible incidence = (days × rats)/number of rats examined per group.
cN/N = total number of observations/number of rats with observation.
dDosing occurred on gestation (presumed) day 6 through lactation day 20 or gestation (presumed) day 24 (rats that did not deliver a litter).
eThere were no rats that did not get dosed for more than 1 consecutive day.
Test article-related and incidental findings (F0)
During the gestation and lactation periods, decreased motor activity was observed in rats in the 100 mg/kg/d dose group and was considered adverse. During these periods, excess salivation (slight to moderate) was observed in rats in the 60 and 100 mg/kg/d dose groups, however, this finding was not considered adverse because the predominant observation in the majority of the rats was graded as slight.
Other clinical observations did not occur in a pattern indicative of a dose–response relationship and were considered incidental and/or were considered common findings in laboratory rats and were unrelated to administration of tavaborole.
Body weight (F0)
Body weight data for F0 generation rats are presented in Figure 2. There were no tavaborole-related effects on mean body weight or body weight gains for either the gestation or lactation periods. All differences from control body weights and body weight gains were considered incidental and unrelated to tavaborole. The typical fluctuations in body weight gains that occur in lactating rats occurred in all dose groups.
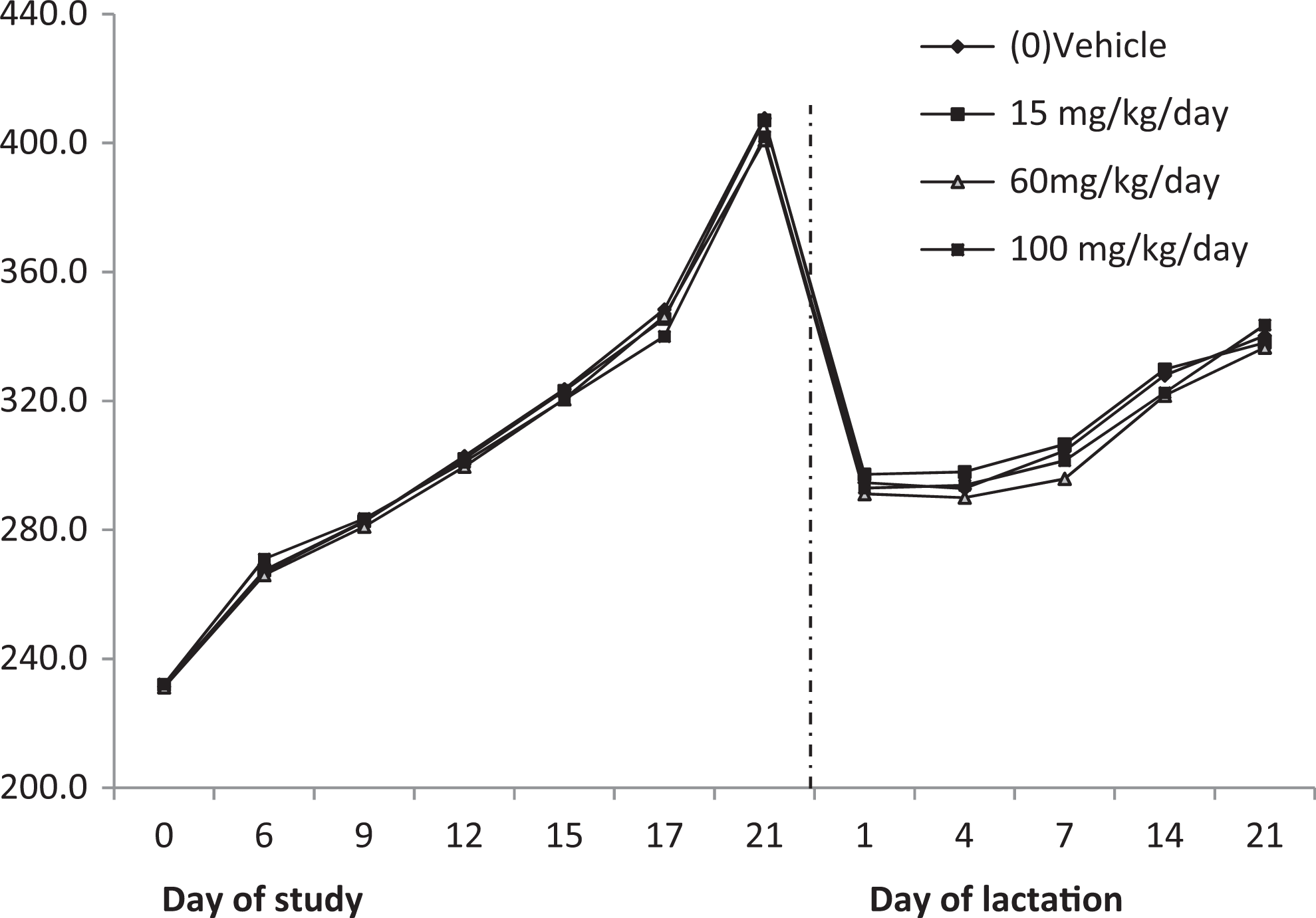
Maternal body weights: F0 generation.
There were no tavaborole-related effects on mean food consumption during the gestation or lactation periods. All differences from control food consumption values were considered incidental and unrelated to administration of tavaborole.
Natural delivery observations for F0 rats are summarized in Table 4. There were no tavaborole-related effects on parturition. All changes from control in parturition were considered incidental and unrelated to tavaborole. The significant but slight increase (P ≤ 0.01) in the duration of gestation in the 100 mg/kg/d dose group (23.0 days vs 22.6 days in the control group) was considered incidental because the increase in duration was minimal and the duration was within the range observed historically at the testing facility (22.5-23.0 days). The length of parturition, in terms of number of dams delivering over 2 days, was comparable among the groups.
Summary of Natural Delivery Observations: F0 Generation Female Rats/F1 Pups.a
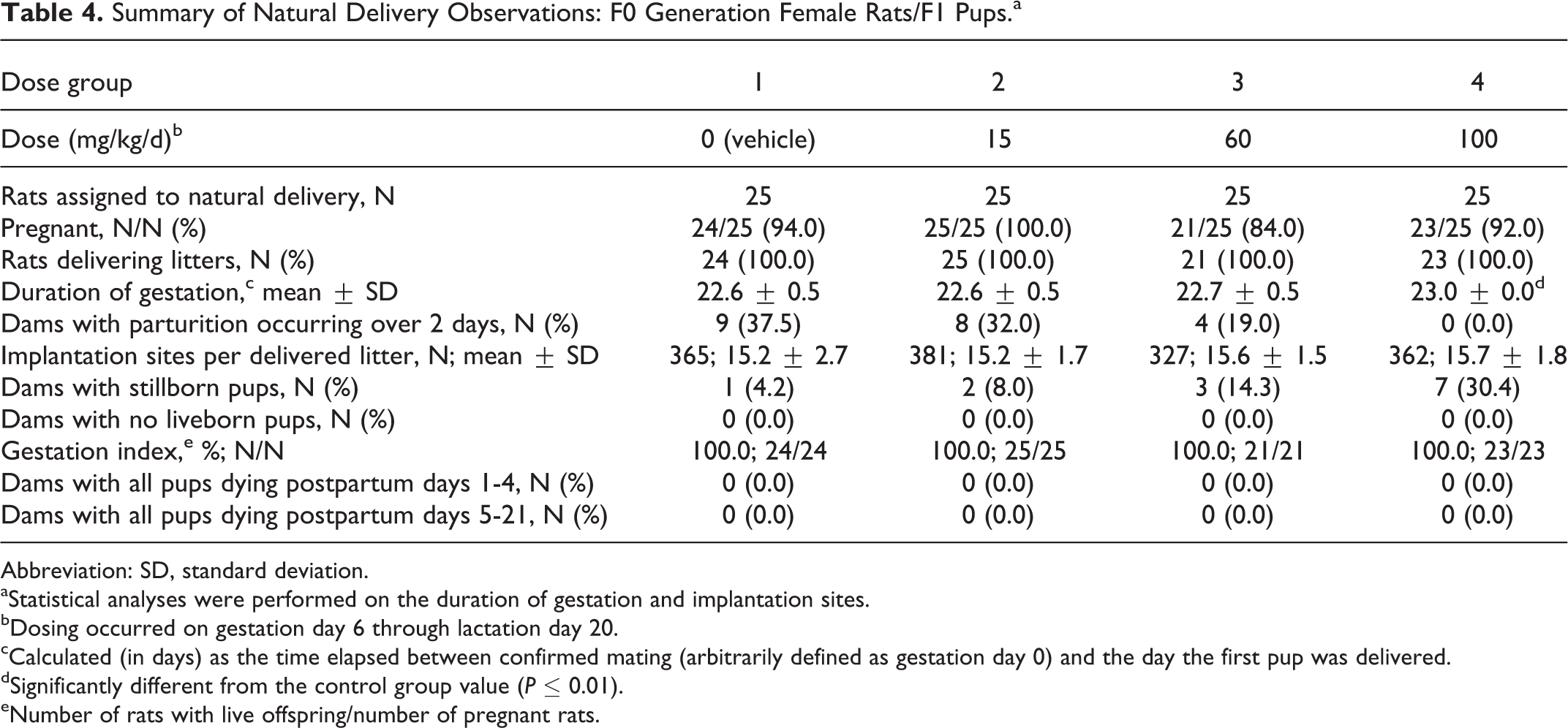
Abbreviation: SD, standard deviation.
aStatistical analyses were performed on the duration of gestation and implantation sites.
bDosing occurred on gestation day 6 through lactation day 20.
cCalculated (in days) as the time elapsed between confirmed mating (arbitrarily defined as gestation day 0) and the day the first pup was delivered.
dSignificantly different from the control group value (P ≤ 0.01).
eNumber of rats with live offspring/number of pregnant rats.
Necropsy observations (F0)
There were no necropsy findings in the F0 generation rats.
Offspring survival (F1)
Offspring survival data are presented in Tables 5 and 6. There were no tavaborole-related effects on pup survival. All changes from control in survivability were considered incidental and unrelated to tavaborole. Both the viability and lactation indices were comparable among the groups.
Litter Observations (Naturally Delivered Pups)—F1 Generation Litters.a,b
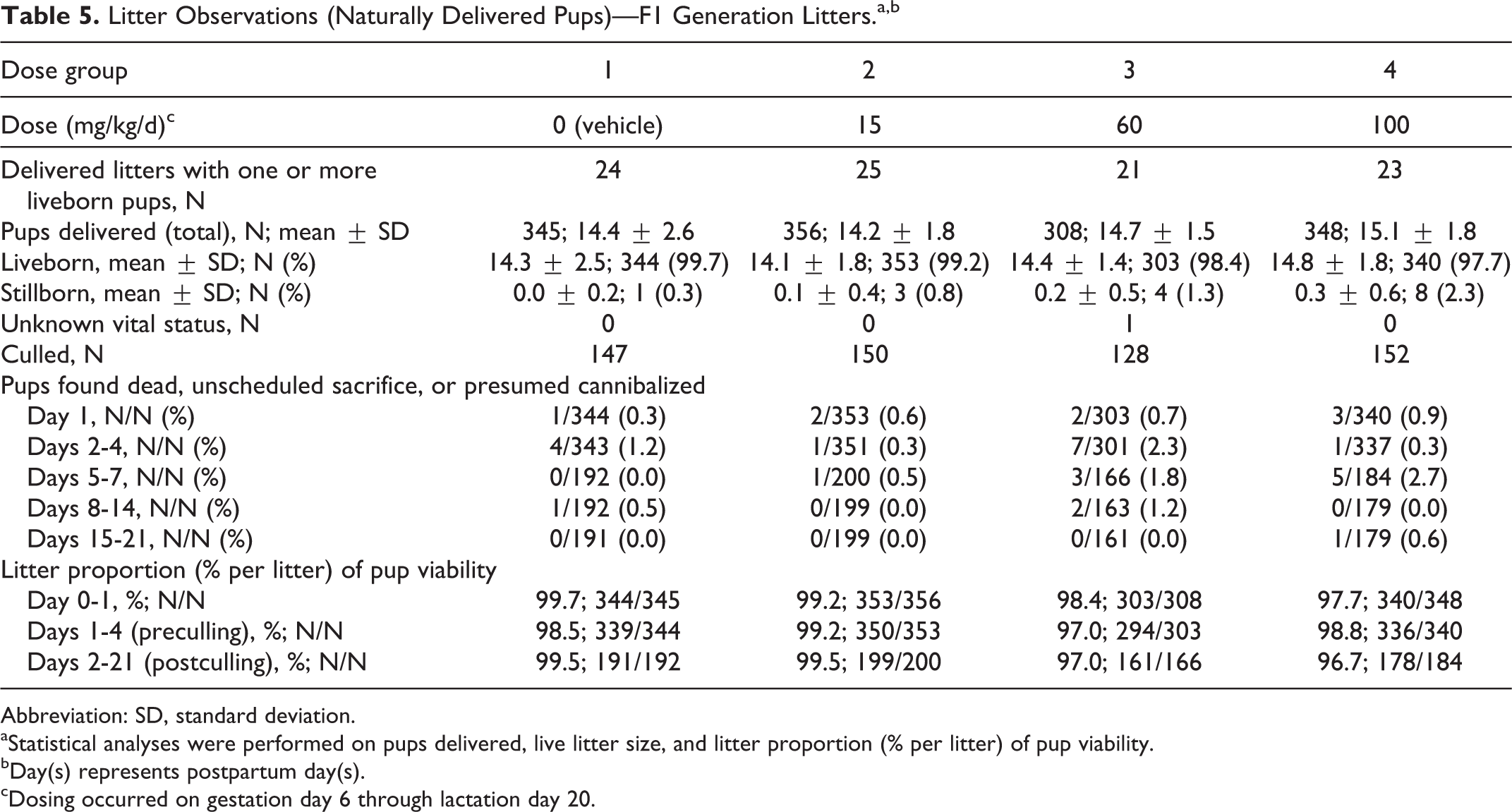
Abbreviation: SD, standard deviation.
aStatistical analyses were performed on pups delivered, live litter size, and litter proportion (% per litter) of pup viability.
bDay(s) represents postpartum day(s).
cDosing occurred on gestation day 6 through lactation day 20.
Litter Viability (Naturally Delivered Pups)—F1 Generation Litters.a,b
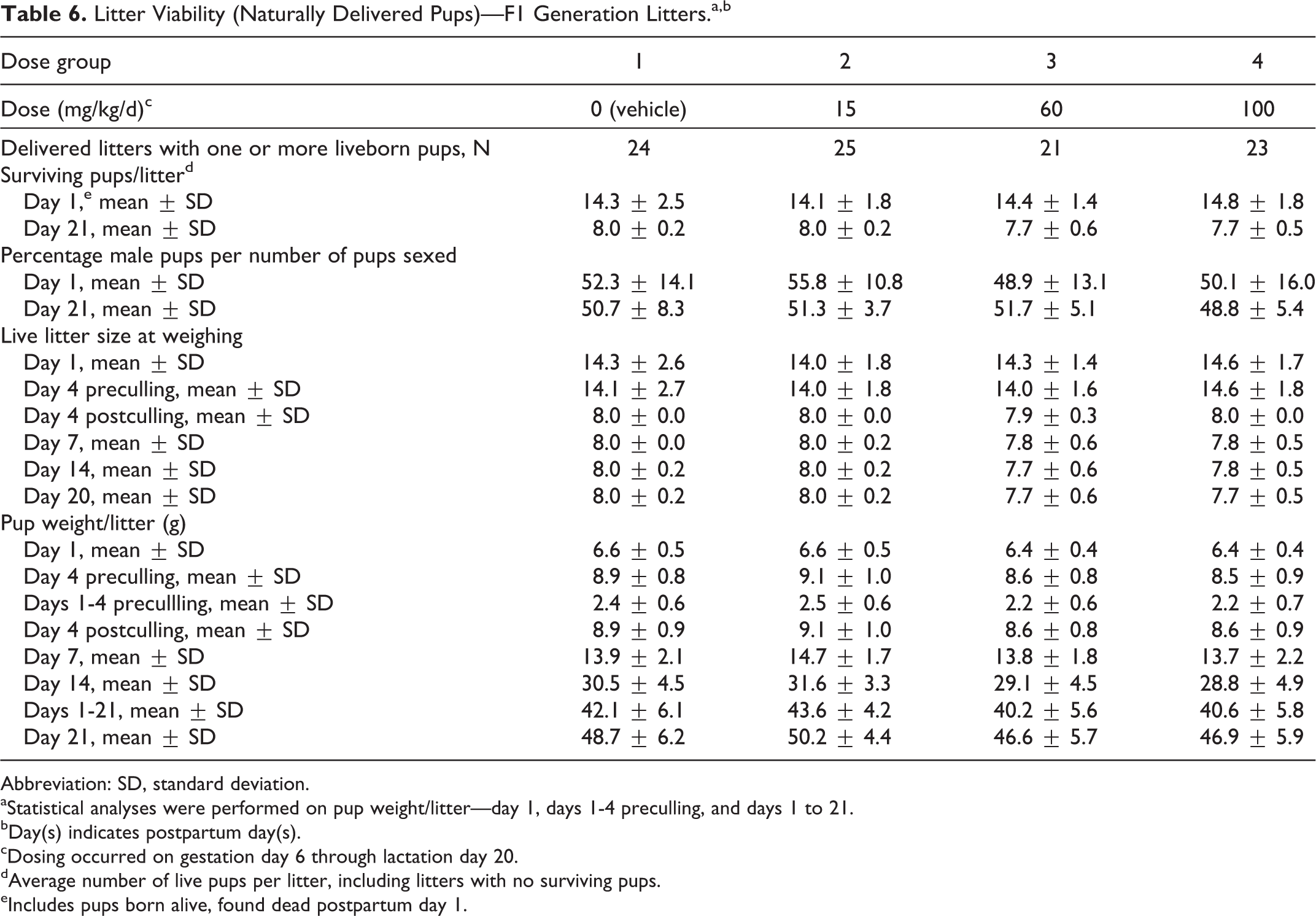
Abbreviation: SD, standard deviation.
aStatistical analyses were performed on pup weight/litter—day 1, days 1-4 preculling, and days 1 to 21.
bDay(s) indicates postpartum day(s).
cDosing occurred on gestation day 6 through lactation day 20.
dAverage number of live pups per litter, including litters with no surviving pups.
eIncludes pups born alive, found dead postpartum day 1.
F1 Generation
Mortality, clinical, and necropsy observations (F1)
There were no tavaborole-related clinical observations in the F1 generation during either the preweaning or postweaning period. All clinical observations were considered incidental and unrelated to tavaborole.
During the postweaning period, a total of 2 male rats, 1 each in the 0 and 100 mg/kg/d maternal dose groups, and 2 female rats, 1 each in the 60 and 100 mg/kg/d maternal dose groups, were found dead or euthanized early. Each early death was related to a small pup that failed to thrive at weaning or due to misaligned incisors or broken palate. All other F1 generation rats that were weaned survived to scheduled euthanasia.
Body weight and food consumption (F1)
There were no tavaborole-related effects on mean body weight (Figure 3), body weight gain, or food consumption for the F1 generation rats during either the preweaning or postweaning period. Any differences from control values were considered incidental and unrelated to tavaborole.
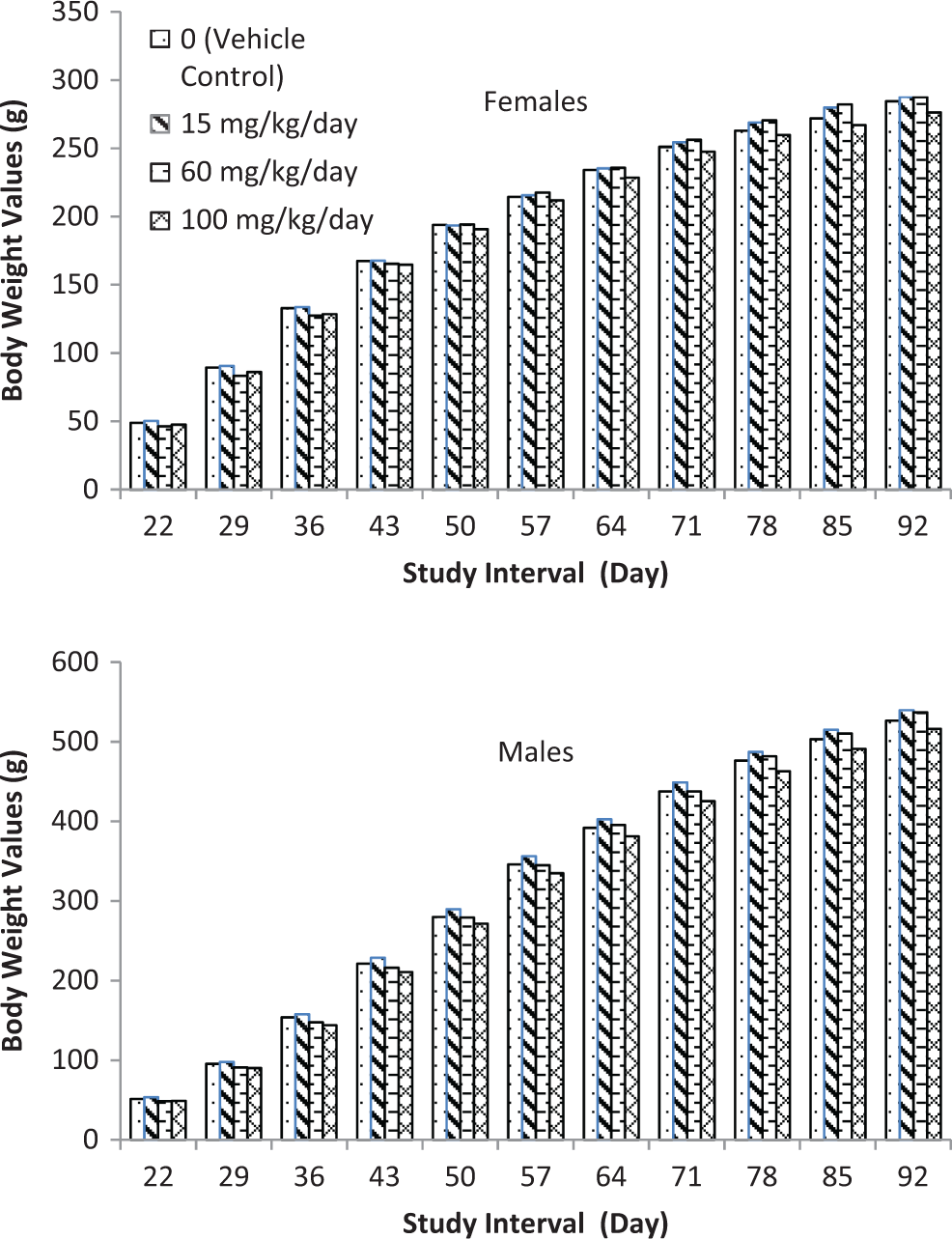
F1 generation body weights.
Maturational and behavioral/developmental evaluations (F1)
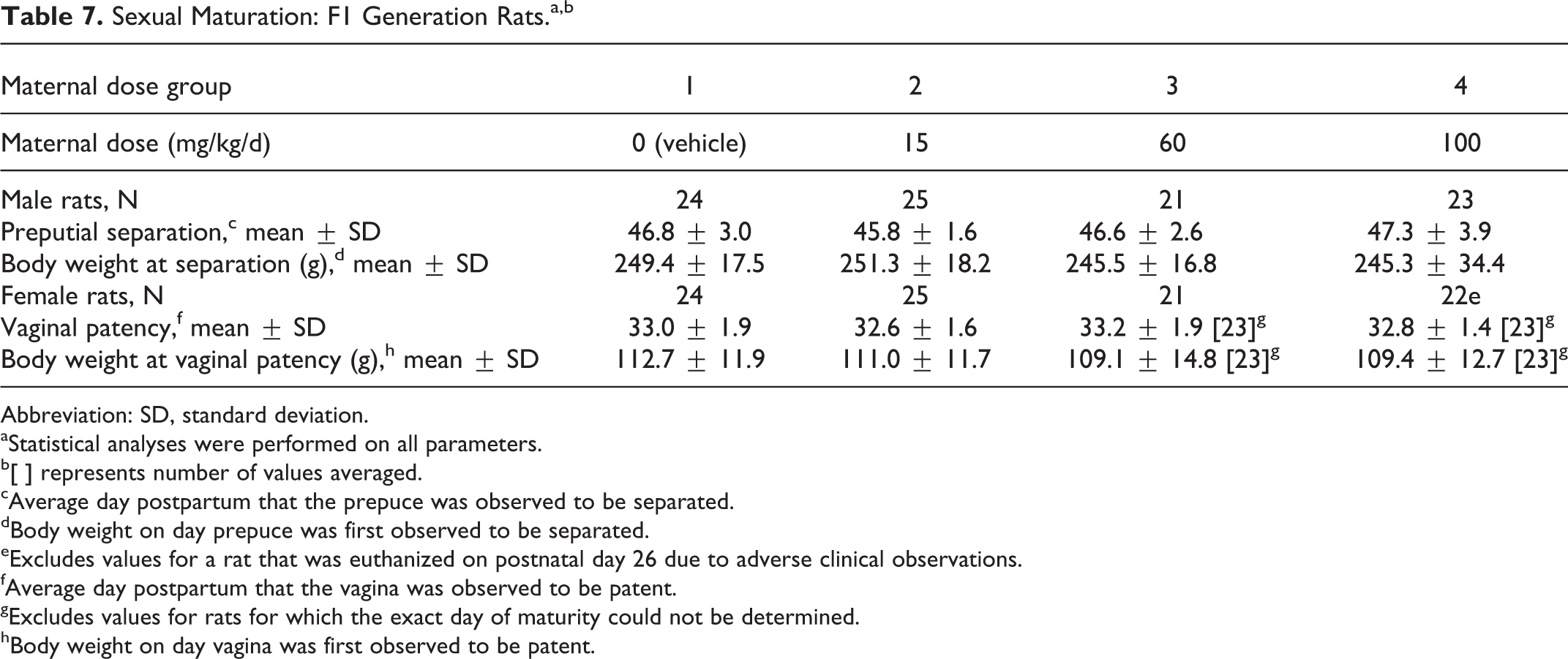
There were no tavaborole-related effects on sexual maturation in F1 generation rats, as measured by the average day of vaginal patency or day of preputial separation (Table 7). Furthermore, there were no tavaborole-related effects on motor activity (Figures 4–5) in the F1 generation rats as measured by the number of movements and time spent in movement, and there were no tavaborole-related effects on acoustic startle habituation (Figure 6), a measure of learning, in F1 generation rats. There were no tavaborole-related effects on memory or learning in the F1 generation rats, as measured by passive avoidance testing (Table 8).
Sexual Maturation: F1 Generation Rats.a,b
Abbreviation: SD, standard deviation.
aStatistical analyses were performed on all parameters.
b[ ] represents number of values averaged.
cAverage day postpartum that the prepuce was observed to be separated.
dBody weight on day prepuce was first observed to be separated.
eExcludes values for a rat that was euthanized on postnatal day 26 due to adverse clinical observations.
fAverage day postpartum that the vagina was observed to be patent.
gExcludes values for rats for which the exact day of maturity could not be determined.
hBody weight on day vagina was first observed to be patent.
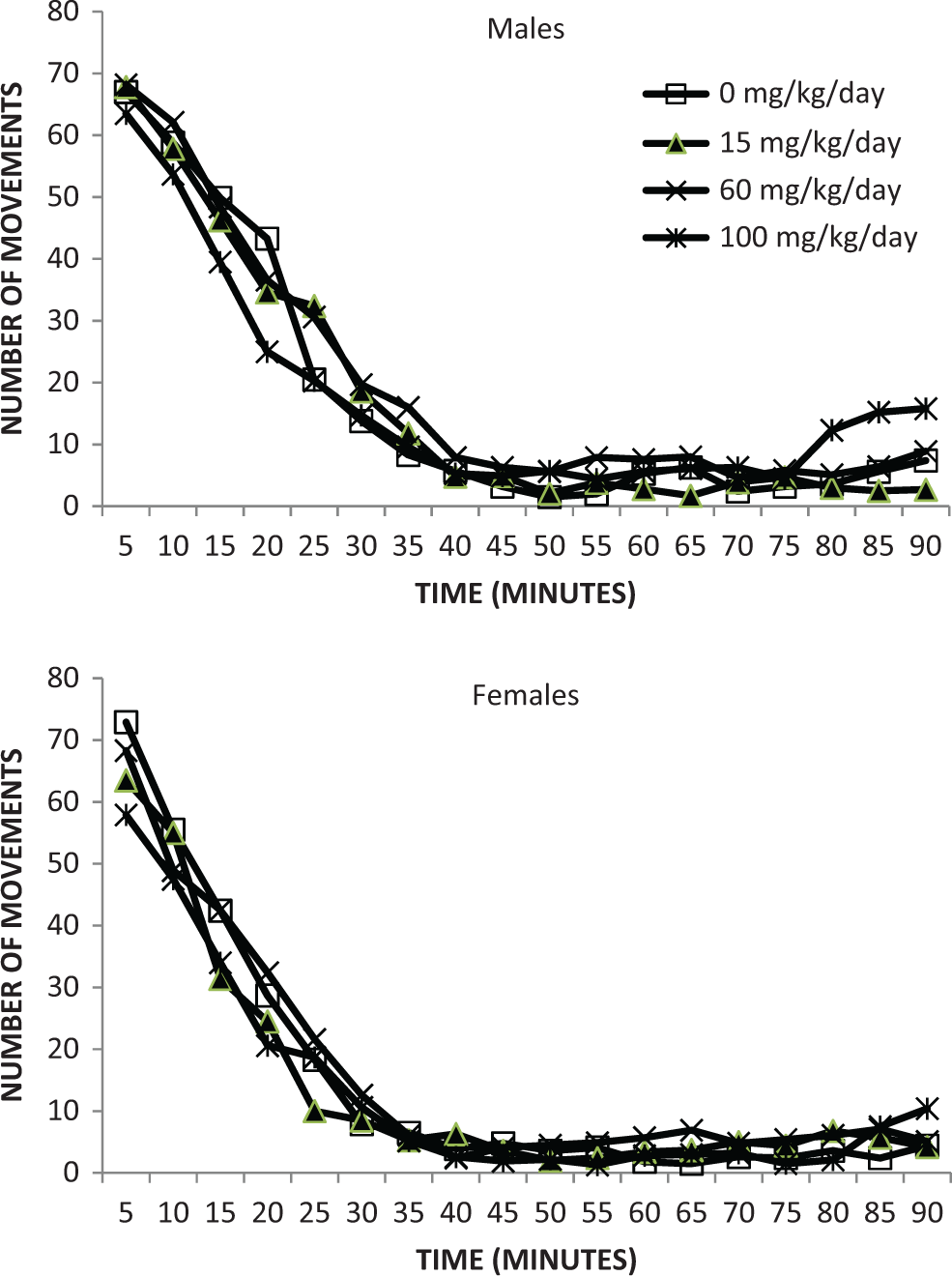
Motor activity—number of movements—F1 generation rats—postnatal day 22.
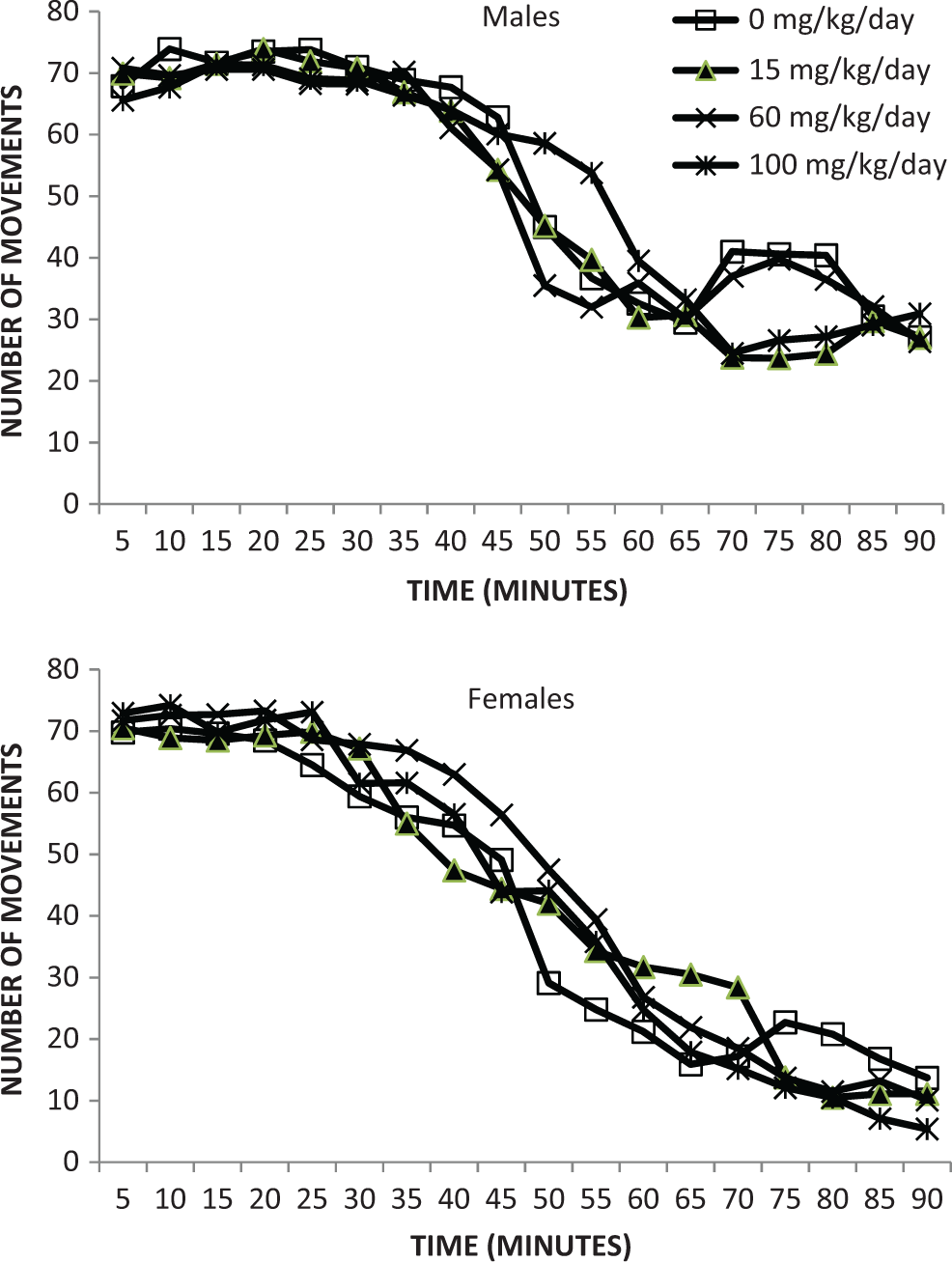
Motor activity—number of movements—F1 generation—postnatal day 61 ± 2.
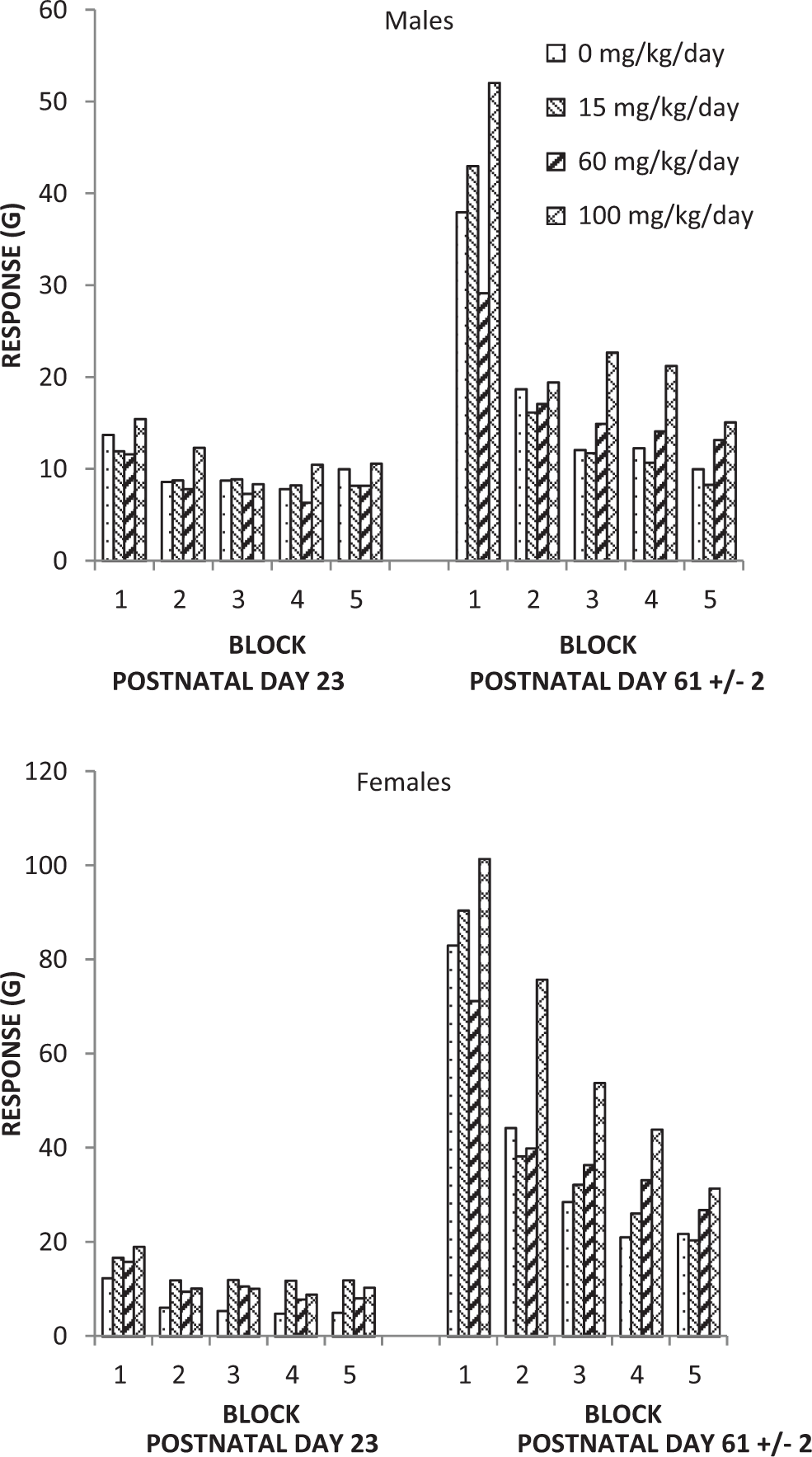
Acoustic startle habituation F1 generation rats.
Passive Avoidance: F1 Generation Rats.a

Abbreviation: SD, standard deviation.
aStatistical analyses were performed on all parameters.
bSessions 1 (learning phase) and 2 (retention phase) of testing were separated by a 1-week interval.
cExcludes values for rats that did not have records for the first session available at the time of data tabulation.
dThe latency was recorded in seconds.
eNumber of rats that did not meet the criterion in session 1 (learning phase); session 2 (retention phase) values for these rats were excluded from summarization and statistical analyses.
fExcludes 1 rat that was not tested.
gSignificantly different from the control group value (P ≤ 0.05).
hExcludes values for 1 rat that was euthanized on postnatal day 26 due to adverse clinical observations.
The latency for session 1 trial 1 for the female rats in the 15 and 60 mg/kg/d maternal dose groups (9.9 and 7.7 seconds, respectively; Table 8) were significantly increased (P ≤ 0.05) compared to the control group (3.6 seconds). These differences were considered incidental because the differences were not dose dependent and the latency times were within the range observed historically at the testing facility (2.6-14.1 seconds). All differences from control for all measures of maturation and neurobehavioral assessment values were considered incidental and unrelated to tavaborole.
Estrous cycles, mating, and fertility (F1)
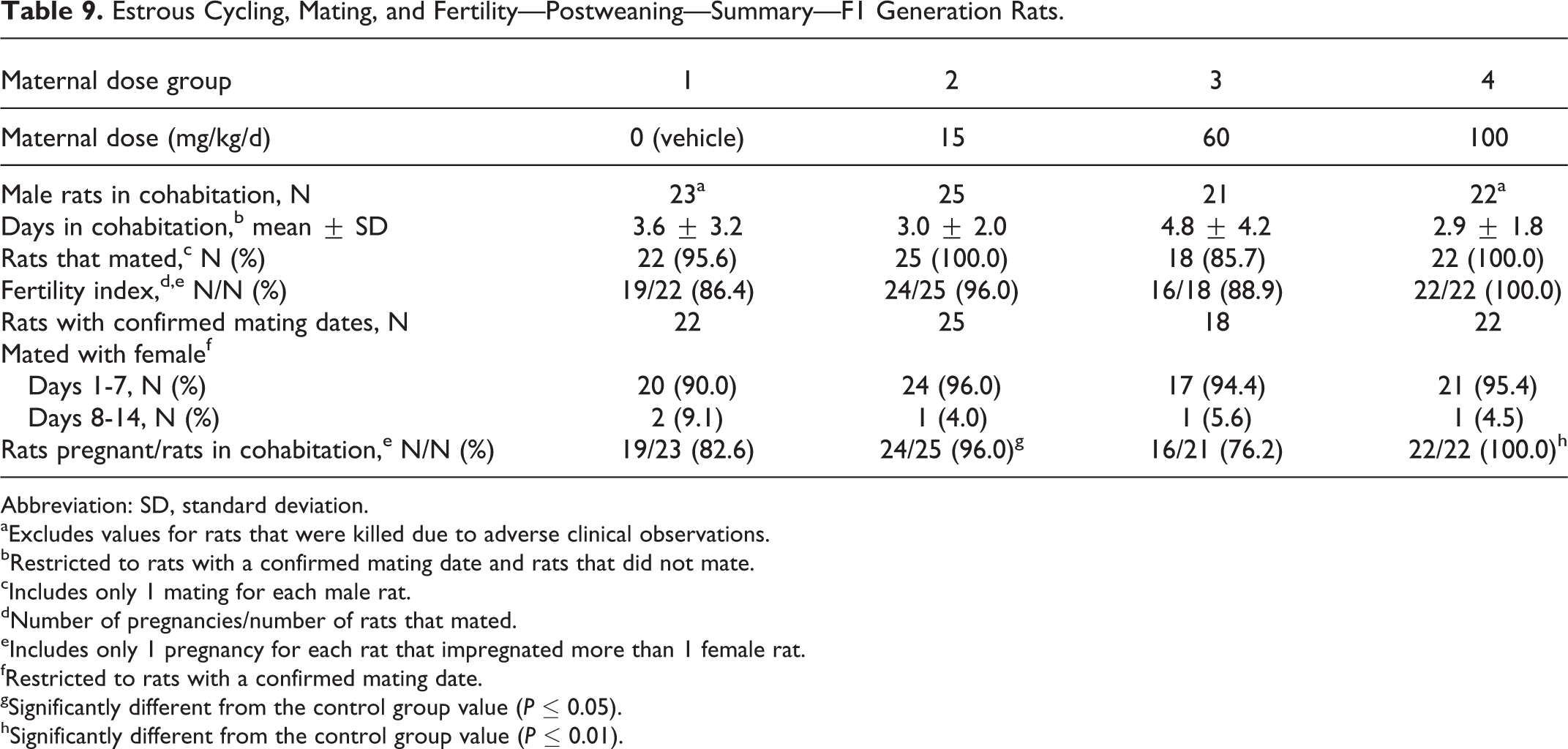
There were no tavaborole-related effects on mating and fertility or estrous cycles in F1 generation rats (Table 9). All changes in estrous cycles, mating, and fertility were considered incidental and unrelated to tavaborole.
Estrous Cycling, Mating, and Fertility—Postweaning—Summary—F1 Generation Rats.
Abbreviation: SD, standard deviation.
aExcludes values for rats that were killed due to adverse clinical observations.
bRestricted to rats with a confirmed mating date and rats that did not mate.
cIncludes only 1 mating for each male rat.
dNumber of pregnancies/number of rats that mated.
eIncludes only 1 pregnancy for each rat that impregnated more than 1 female rat.
fRestricted to rats with a confirmed mating date.
gSignificantly different from the control group value (P ≤ 0.05).
hSignificantly different from the control group value (P ≤ 0.01).
The percentages of rats that were pregnant (of all female rats placed in cohabitation) in the 15 and 100 mg/kg/d maternal dose groups were significantly increased (P ≤ 0.05 or P ≤ 0.01) compared to the control group (96.0% and 100.0% in the 2 respective test article groups vs 82.6% in the control group). The increase was statistically significant due to the low percentage of pregnancy in the control group, and thus, the increase was considered incidental. A decrease in percentage of pregnant rats was noted in the 60 mg/kg/d maternal dose group (76.2%). This difference was also considered incidental because the decrease did not occur in a dose–response manner and the percentage of pregnant rats in this dose group was within the range observed historically at the testing facility (72.0%-100.0%).
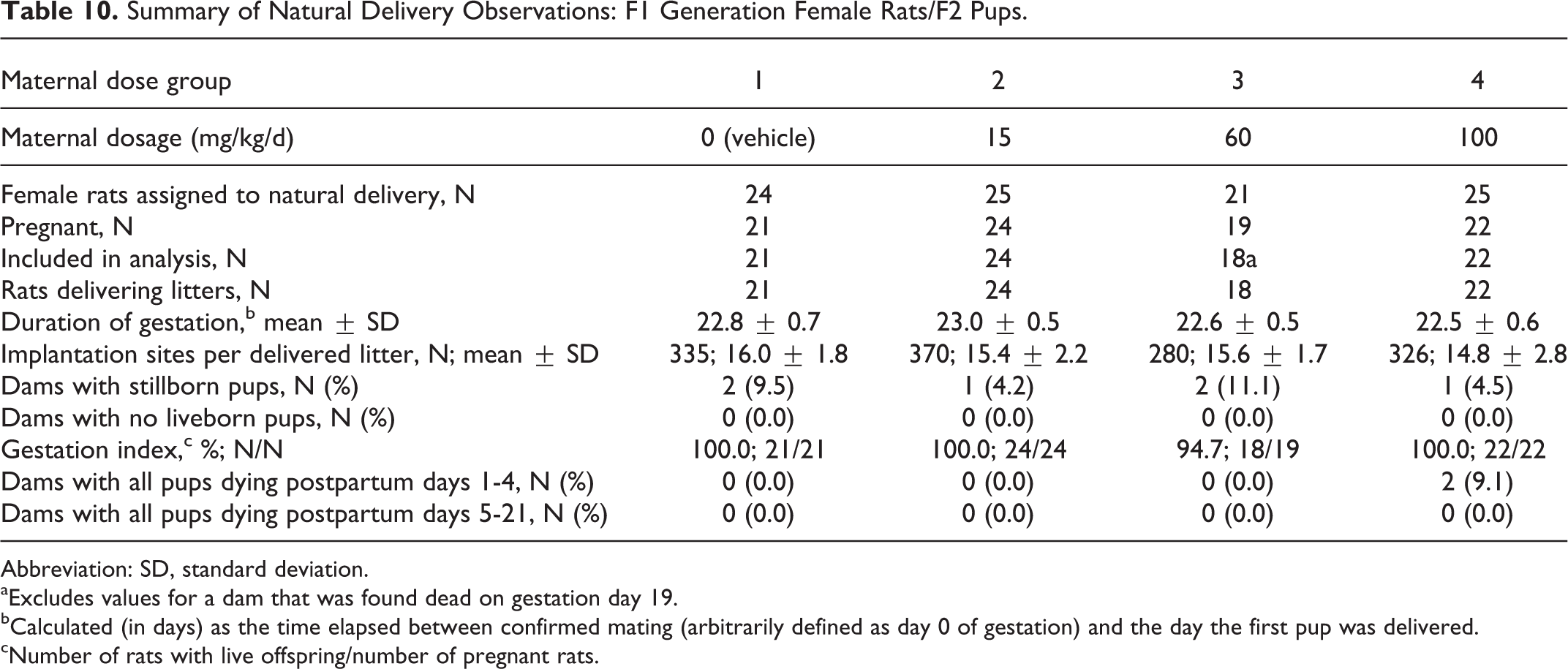
There were no tavaborole-related effects on parturition in F1 generation rats. The duration of gestation was comparable among the groups (Table 10). All changes from control in parturition were considered incidental and unrelated to tavaborole.
Summary of Natural Delivery Observations: F1 Generation Female Rats/F2 Pups.
Abbreviation: SD, standard deviation.
aExcludes values for a dam that was found dead on gestation day 19.
bCalculated (in days) as the time elapsed between confirmed mating (arbitrarily defined as day 0 of gestation) and the day the first pup was delivered.
cNumber of rats with live offspring/number of pregnant rats.
Necropsy observations (F1)
There were no tavaborole-related necropsy findings in the F1 generation rats. All necropsy findings observed in the F1 generation represented common findings in laboratory rats and were considered incidental and unrelated to tavaborole.
Terminal body weights, organ weights, and ratios of organ weights to terminal body weights (F1)
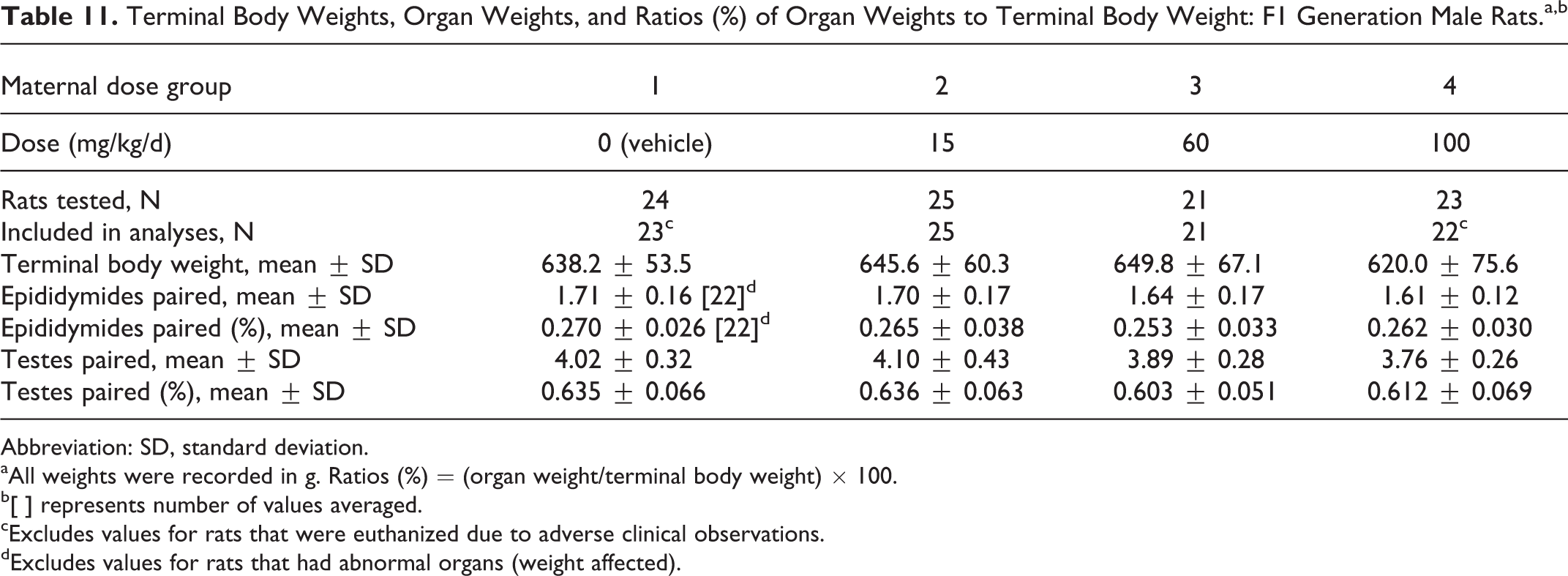
There were no tavaborole-related effects in F1 generation rats on mean terminal body weights, paired testes and epididymides weights, and the ratios of these organ weights to terminal body weights (Table 11).
Terminal Body Weights, Organ Weights, and Ratios (%) of Organ Weights to Terminal Body Weight: F1 Generation Male Rats.a,b
Abbreviation: SD, standard deviation.
aAll weights were recorded in g. Ratios (%) = (organ weight/terminal body weight) × 100.
b[ ] represents number of values averaged.
cExcludes values for rats that were euthanized due to adverse clinical observations.
dExcludes values for rats that had abnormal organs (weight affected).
Offspring survival (F2)
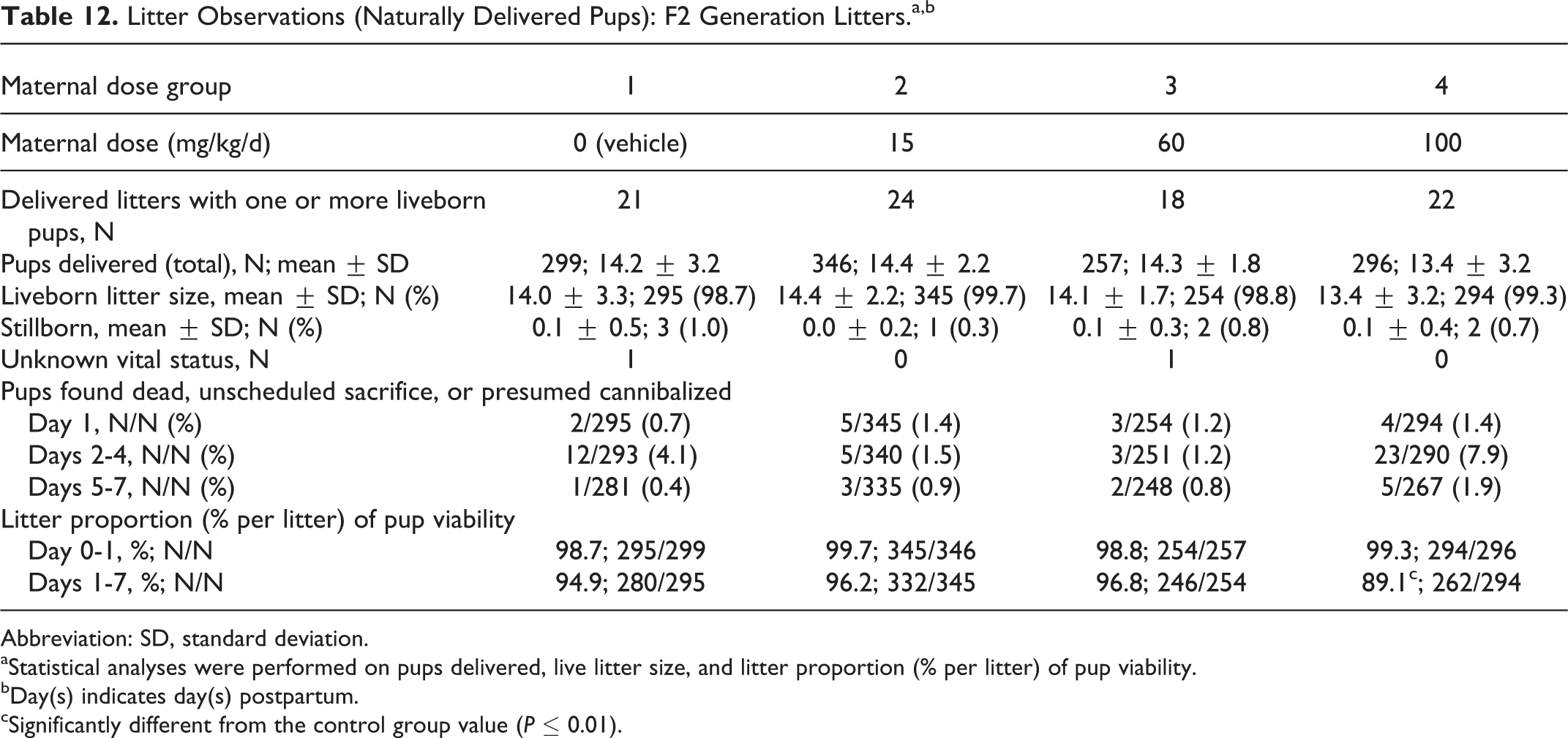
Tavaborole did not affect the survival of F2 pups (Table 12). Although a significant decrease in pup viability was observed in the 100 mg/kg/d maternal dose group (89.1% vs 94.9% in the control group) for days 1 to 7 postpartum, this reduction was considered incidental since the decrease was mainly due to 2 dams with pups dying between days 1 and 2 postpartum and there were no other test article-related findings in F2 generation. One of the 2 dams had mammary masses in the left inguinal area and right flank, and this poor condition led to the deaths of the pups since the pups did not have a milk band present, indicating the pups were not nursing. Masses of the type and location observed in this study are known spontaneous findings in this strain of rat. No plausible explanation was at hand for the demise of pups born to the other dam. All differences from control for all natural delivery and litter observations values were considered incidental and unrelated to tavaborole.
Litter Observations (Naturally Delivered Pups): F2 Generation Litters.a,b
Abbreviation: SD, standard deviation.
aStatistical analyses were performed on pups delivered, live litter size, and litter proportion (% per litter) of pup viability.
bDay(s) indicates day(s) postpartum.
cSignificantly different from the control group value (P ≤ 0.01).
F2 Generation
Body weight (F2)
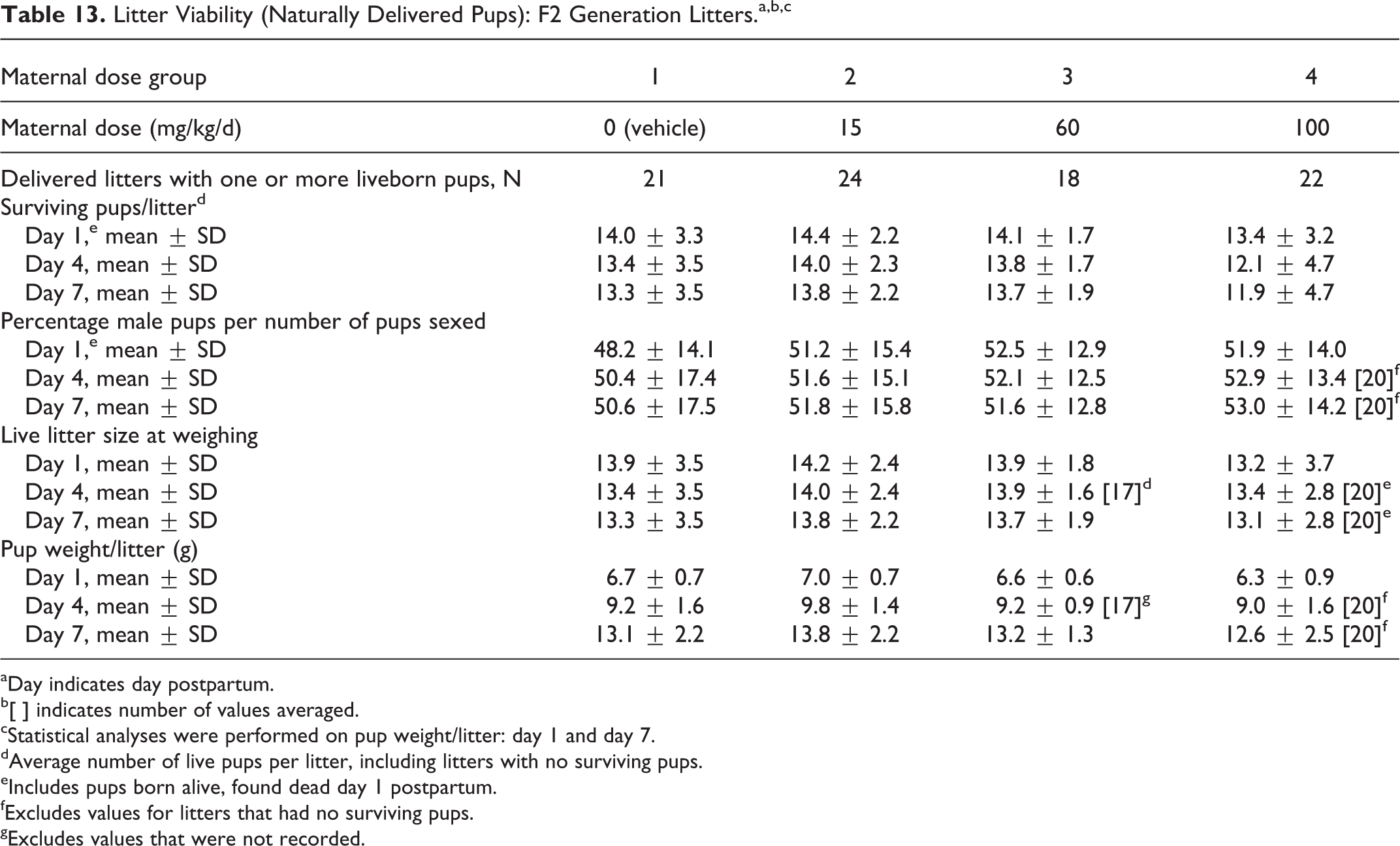
There were no tavaborole-related effects on mean body weight or body weight gains for the F2 generation pups (Table 13). All differences from control body weights and body weight gains were considered incidental and unrelated to tavaborole.
Litter Viability (Naturally Delivered Pups): F2 Generation Litters.a,b,c
aDay indicates day postpartum.
b[ ] indicates number of values averaged.
cStatistical analyses were performed on pup weight/litter: day 1 and day 7.
dAverage number of live pups per litter, including litters with no surviving pups.
eIncludes pups born alive, found dead day 1 postpartum.
fExcludes values for litters that had no surviving pups.
gExcludes values that were not recorded.
Clinical observations (F2)
There were no tavaborole-related clinical observations in the F2 generation. All clinical observations were considered incidental and unrelated to tavaborole.
Necropsy observations (F2)
There were no tavaborole-related necropsy findings in the F2 generation. All necropsy findings represented common findings in laboratory rats and were considered incidental and unrelated to tavaborole.
The no observed adverse effect level (NOAEL) for maternal toxicity (F0 generation) was 60 mg/kg/d, based on the decreased activity observed in the 100 mg/kg/d dose group. The NOAEL for the offspring (through maternal exposure in utero and during lactation) effects was ≥100 mg/kg/d, based on the lack of test article-related changes.
Discussion and Conclusions
As part of the nonclinical development program for tavaborole, a topical antifungal agent approved by the US FDA for the treatment of toenail onychomycosis, reproductive and developmental toxicity studies were conducted (rat fertility and early embryonic development, rat and rabbit embryo–fetal development [oral and dermal administration]), 12 and as reported here, a rat prenatal and postnatal development study. In the prior studies, 12 there were no effects on fertility or reproductive performance at doses up to 300 mg/kg/d (107 times the MRHD based on the mean AUC comparisons). In the rat embryo–fetal development toxicity studies, teratogenicity was not observed at doses up to 100 mg/kg/d (29 times the MRHD). However, several treatment-related skeletal malformations and variations were observed at 300 mg/kg/d (570 times the MRHD). In rabbit embryo–fetal development toxicity studies dosed via oral or dermal administration, the NOAEL for maternal toxicity and embryo fetal toxicity was 50 mg/kg/d (16 times the MRHD) and 5% (26 times the MRHD), respectively.
Under the conditions of the present study, there were no tavaborole-related effects on the growth, viability, development, neurobehavioral assessments, or reproductive performance of the F1 generation. Survivability and mean body weight of the F2 pups were unaffected. The NOAEL for maternal toxicity (F0 generation) was 60 mg/kg/d, based on the decreased activity observed in the 100 mg/kg/d dose group. The NOAEL for the offspring (through maternal exposure in utero and during lactation) effects was ≥100 mg/kg/d, based on the lack of test article-related changes, and was 29 times the MRHD of tavaborole.
Compared to other approved antifungals, the results of the reproductive toxicology studies conducted with tavaborole exhibit higher safety margins. Oral reproduction studies with Lamisil (terbinafine hydrochloride) in rabbits and rats at doses up to 300 mg/kg/d resulted in safety margins that were 12× to 23× the MRHD, respectively, based on body surface area comparisons. 6 Another antifungal, Sporanox (itraconazole) was found to cause a dose-related increase in maternal toxicity, embryotoxicity, and teratogenicity in rats at doses approximately 5 to 20× the MRHD and in mice at doses approximately 10× the MRHD. In rats, the teratogenicity consisted of major skeletal defects; in mice, it consisted of encephaloceles and/or macroglossia. 7 No effects on fertility were observed in male and female rats that were administered subcutaneous doses up to 25 mg/kg/d efinaconazole (279 times the MRHD based on AUC comparisons) prior to and during early pregnancy. Efinaconazole delayed the estrous cycle in females at 25 mg/kg/d but not at 5 mg/kg/d (56 times the MRHD based on AUC comparisons). 24
Patient safety is a primary concern when treating for onychomycosis. There have been a number of safety concerns with oral antifungals. A review was published on the mode of action, pharmacokinetics, tolerability, and safety of the 3 FDA-approved oral drugs griseofulvin, itraconazole, and terbinafine. 25 Comparison of griseofulvin with the antifungal agents terbinafine and itraconazole suggests that griseofulvin is no longer the treatment of choice for dermatophyte onychomycosis. Although itraconazole (Sporanox) was used for years, its major drawback is the high potential for drug interactions since it is a potent inhibitor of CYP3A4 and cannot be conveniently used with statins, antidiabetics, or antihypertensives.
In a review of onychomycosis and the various treatment options, the conclusion is that oral medications are associated with high recurrence rates and treatment failure and are not suitable for many cases due to potential adverse effects. 26 Pharmacokinetic data have shown that terbinafine accumulates in adipose tissue and provides a “drug depot” effect. Within 24 hours of the first dose, terbinafine appears in the stratum corneum and maintains a therapeutically active drug concentration in the nails. The mean active drug concentration persists in the body up to 3 months after termination of oral therapy. 27 The most commonly reported side effects are nausea, vomiting, and other gastrointestinal side effects. Other side effects include taste disturbances and hair loss. Due to potential terbinafine-induced hepatotoxicity, manufacturers suggest performing liver function tests for patients before commencing therapy and after 4 to 6 weeks of therapy. 28 -30
Other studies assessing the reproductive and teratogenic potential of tavaborole revealed that tavaborole was not considered a reproductive toxicant at doses that provided exposures up to 107 times the MRHD nor was it found to be a teratogen at doses that provided up to 29 times the MRHD of tavaborole. 12
In the present study, there were no tavaborole-related effects on the growth, viability, development, neurobehavioral assessments, or reproductive performance of the F1 generation. Survivability and mean body weight of the F2 pups were unaffected. The NOAEL for maternal toxicity (F0 generation) was 60 mg/kg/d, based on the decreased activity observed in the 100 mg/kg/d dose group. The NOAEL for the offspring (through maternal exposure in utero and during lactation) effects was ≥100 mg/kg/d, based on the lack of test article-related changes, and was 29 times the MRHD of tavaborole.
Footnotes
Authors’ Note
The study was conducted at Charles River Laboratories, Horsham, Pennsylvania, and Schering-Plough Research Institute, Summit, New Jersey.
Author Contributions
V. Ciaravino and S. Chanda contributed to conception and design, contributed to acquisition, analysis, and interpretation, drafted the manuscript; and critically revised the manuscript. D. Coronado and C. Lanphear contributed to analysis and interpretation and critically revised the manuscript. A. Hoberman contributed to analysis and interpretation, drafted the manuscript, and critically revised the manuscript. All authors gave final approval and agree to be accountable for all aspects of work ensuring integrity and accuracy.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Vic Ciaravino, Dina Coronado, and Sanjay Chanda are employees of Anacor Pharmaceuticals, Inc, Palo Alto, California.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
