Abstract
Nitric oxide (NO) is a potent signaling molecule that needs to be tightly regulated to maintain metabolic and cardiovascular homeostasis. The nitric oxide synthase (NOS)/dimethylarginine dimethylaminohydrolase (DDAH)/asymmetric dimethylarginine (ADMA) pathway is central to this regulation. Specifically, the small-molecule ADMA competitively inhibits NOS, thus lowering NO levels. The majority of ADMA is physiologically metabolized by DDAH, thus maintaining NO levels at a physiological concentration. However, under pathophysiological conditions, DDAH activity is impaired, in part as a result of its sensitivity to oxidative stress. Therefore, the application of high-throughput chemical screening for the discovery of small molecules that could restore or enhance DDAH activity might have significant potential in treating metabolic and vascular diseases characterized by reduced NO levels, including atherosclerosis, hypertension, and insulin resistance. By contrast, excessive generation of NO (primarily driven by inducible NOS) could play a role in idiopathic pulmonary fibrosis, sepsis, migraine headaches, and some types of cancer. In these conditions, small molecules that inhibit DDAH activity might be therapeutically useful. Here, we describe optimization and validation of a highly reproducible and robust assay successfully used in a high-throughput screen for DDAH modulators.
Introduction
Asymmetric dimethylarginine (ADMA) and monomethyl-L-arginine (L-NMMA) are endogenous competitive inhibitors of nitric oxide synthase (NOS). 1 These methylarginines are generated by the methylation of arginine residues on histones and other proteins by a family of enzymes known as protein arginine methyltransferases (PRMTs). 2 During the hydrolysis of proteins containing methylarginine residues, free ADMA and L-NMMA are released ( Fig. 1 ). The concentration of these methylated arginines is physiologically regulated either by excretion through the renal system or degradation by dimethylarginine dimethylaminohydrolase (DDAH).3,4 Of the two arginine analogues, ADMA is present at roughly 10-fold higher levels in plasma and tissue. Plasma ADMA is increased in patients with cardiovascular risk factors and is predictive of major adverse cardiovascular events, suggesting that it is a pathophysiologically relevant molecule. 5
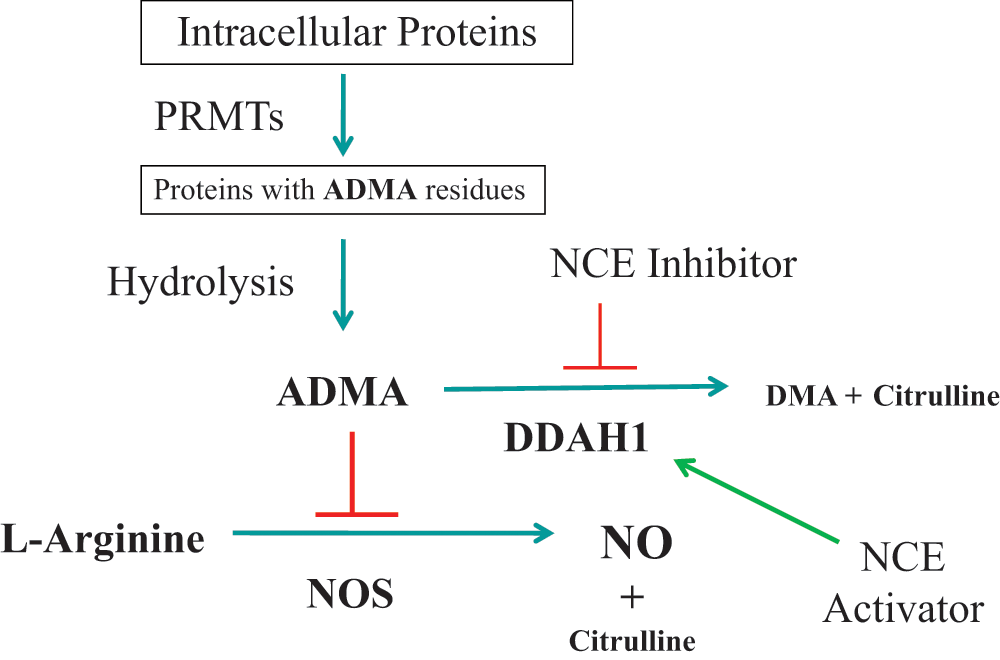
The NO/ADMA/DDAH pathway and the pharmacological inhibition of DDAH1 leading to higher ADMA levels and subsequent regulation of NO production. DMA, dimethylamine; DDAH, dimethylarginine dimethylaminohydrolase; ADMA, asymmetric dimethylarginine; SDMA, symmetric dimethylarginine; L-NMMA, monomethyl arginine; PRMTs, protein arginine methyltransferases; NO, nitric oxide; NCE, new chemical entity.
DDAH is a cysteine hydrolase enzyme that is expressed in all nucleated mammalian cells in one of two isoforms (DDAH1 and DDAH2). 6 About 80% of endogenous ADMA is metabolized by DDAH, principally the DDAH1 isoform.5,7,8 Several studies have provided evidence that disruption of DDAH activity is the major cause by which metabolic perturbations (such as hypercholesterolemia or hyperglycemia) elevate levels of ADMA.4,9 Elevations in plasma ADMA impair vascular function and increase the risk of cardiovascular disease and death. 4 Thus, it seems likely that an activator of DDAH, by reducing ADMA levels, might reduce the progression of vascular disease.4,9
On the other hand, there are conditions where excessive accumulation of NO (primarily driven by inducible NOS, or iNOS) may be associated with disease. For example, overproduction of NO is associated with vascular collapse in sepsis and is implicated in migraine headache, some types of cancer, and defined autoimmune diseases such as rheumatoid arthritis and spondyloarthritis.10,11 In these cases, it seems likely that a DDAH antagonist, by elevating ADMA levels and suppressing NO synthesis, might have therapeutic value. Moreover, a recent study has shown that in an animal model of idiopathic pulmonary fibrosis (IPF), DDAH and iNOS activities are increased. In this model, a small-molecule antagonist of DDAH (L-291) reduced fibrosis and improved pulmonary compliance. 12 Therefore, interest is growing in the regulation of DDAH activity as a promising therapeutic avenue.10,13 A growing number of DDAH inhibitors have been reported in the literature.10,13–21 However, almost all of these compounds, with the exception of the substrate-like competitive inhibitors, are either nonselective or weak antagonists. Furthermore, no allosteric activators of DDAH activity have been reported. Therefore, there is a need for a strategy that will accelerate the search for potent and biologically relevant small molecules that regulate DDAH activity.
To this end, we have developed a sensitive, robust, and highly reproducible assay that differentially detects the breakdown of the endogenous substrate ADMA. In this biochemical assay, ADMA is metabolized by recombinant human DDAH1 into dimethylamine and L-citrulline. The production of L-citrulline can be quantified colorimetrically using a single derivatization step with a ureido-reactive reagent. This previously reported test-tube method 22 was substantially modified and miniaturized into a 384-well format to facilitate the screening of a chemical library of more than 130 000 compounds using a robotic arrayer system. In an orthogonal assay, DDAH activity can be monitored fluorimetrically by using an artificial substrate, S-methyl-L-thiocitrulline (SMTC), that produces a methyl mercaptan molecule (methanethiol; CH3-SH) upon metabolism by DDAH. The release of CH3-SH can be quantified upon the addition of a coumarin-containing reagent (7-diethylamino-3-(4-maleimidophenyl)-4-methylcoumarin [CPM]).
Materials and Methods
The chemical library of the Stanford High Throughput Bioscience Center (HTBC) contains more than 130 000 small molecules selected from diverse sources, including Sigma, ChemDiv, MicroSource, ChemBridge, the National Institutes of Health clinical collection (NIH CC), National Cancer Institute (NCI), natural products, and Food and Drug Administration (FDA)–approved drug libraries using stringent criteria to maximize diversity and medicinal drug-like properties (http://htbc.stanford.edu/). The orthogonal assays, using hits derived from the HTBC, were conducted using chemicals purchased from Sigma-Aldrich (St. Louis, MO) unless indicated otherwise. For generation of DDAH protein, we used an Escherichia coli BL21 strain purchased from Invitrogen (Carlsbad, CA). Dr. Neil McDonald (Birkbeck College, London) kindly provided the plasmid construct pGEX-6P-1-DDAH1. Empty vector control, enzyme purification, and cleavage reagents were from GE Healthcare (Piscataway, NJ). Clear and black 384-well plates were from E&K Scientific (Santa Clara, CA). Antibodies directed against DDAH1 (Abcam; Cambridge, MA) and glutathione S-transferase (GST; GE Healthcare) were obtained from commercial purveyors.
Production of Recombinant Human DDAH1
Human DDAH1 was expressed in E. coli BL21 Star (DE3) strain for protein production. In parallel, cells were also transformed with empty vector. Positive clones were selected by PCR, and the clones harboring DDAH were subsequently inoculated into LB broth. Bacteria were grown at 37 °C (225 rpm) for 36 h, and preinduction samples were removed prior to inducing the remaining culture by adding isopropyl-β-D-thiogalactopyranoside (IPTG; 0.1 mM final concentration) at 25 °C for 18 h. The cells were harvested by centrifugation, and the supernatant was discarded prior to lysing them with cell disruption buffer (containing 20 mM Tris-HCl [pH 8.0], 150 mM NaCl, 2 mM β-mercaptoethanol, 1 mM phenylmethylsulfonyl fluoride [PMSF], 1 mM benzamidine, and 10 mM DNAse 1) 20 and with 1% Triton X-100 and lysozyme to break the peptidoglycan layer. The lysate was centrifuged at 20 000 g for 40 min at 4 °C, and the supernatant was transferred into clean tubes for sodium dodecyl sulfate–polyacrylamide gel electrophoresis (SDS-PAGE) and Western analyses. The protein was purified using glutathione sepharose 4B column in a batch mode according to the manufacturer’s recommendations. The GST-tag was cleaved off the recombinant protein using PreScission Protease. The purified protein was eluted and SDS-PAGE analyzed, and its identity was confirmed by Western and mass spectroscopy.
DDAH Activity Assay
The L-citrulline assay was based on an original test-tube method developed by Prescott and Jones in 1969, 22 which we adapted and optimized for a microplate format (see Results section for details). Subsequently, the activity of DDAH was quantified by detecting its conversion of ADMA to citrulline using the optimized protocol. The assay was scaled up to a 384-well format for high-throughput chemical screening.
High-Throughput Screening of Small Molecules
More than 130 000 small molecules deposited in the Stanford HTBC were screened using the enzymatic assay to identify chemicals that regulate DDAH activity. In brief, recombinant human DDAH1 (rhDDAH1) was mixed with ADMA in the presence of screening buffer in 384-well plates using a Staccato multidrop. Small molecules (100 nL each) were then added to the wells using a robotic arrayer to yield a final compound screening concentration of up to 50 µM. Plates were incubated at 37 °C for 4 h. Subsequently, color-developing reagent (containing two volumes of antipyrin and one volume of 2,3-butanedione oxime reagents) was added using the Velocity 11 (Menlo Park, CA) system, and the plates were sealed using an automated plate sealer. Finally, color was developed by incubating the plates at 60 °C for 90 min prior to spinning them at 1500 rpm for 5 min. In this assay, absorbance was proportional to the concentration of citrulline generated by DDAH and was measured using an AnalystGT plate reader (Molecular Devices, Sunnyvale, CA) at 485 nm using a dichroic beam splitter. The signal-to-noise ratio of separation was calculated using an established formula. 23
Identification of Primary Hits
Inhibitors were defined as compounds that reduce absorbance by at least 30% compared with control wells. The hits were validated using an 8-point full dose-response study (50 µM to 0.39 µM in serial dilutions). A total of more than 150 compounds, about 0.12% of the total compounds, caused a reduction in absorbance of at least 30%. To determine which of these hits were true inhibitors of DDAH activity, we used a modification of a newly validated secondary fluorimetric assay 18 as described below. In parallel, compounds were also cross-validated by adding them in reaction mix containing all the components described above with the exception of the enzyme to rule out the possibility that their apparent activity was caused by nonspecific reaction quenching and not by directly inhibiting DDAH.
Secondary Assay to Validate Potential DDAH Inhibitors
For the secondary assay, we adapted a fluorimetric assay that uses SMTC as a substrate. DDAH metabolizes SMTC into L-citrulline and methanethiol (CH3-SH). 18 In brief, DDAH (30 nM final concentration) was mixed with SMTC (100 µM final concentration), CPM (50 µM final concentration), and screening buffer (containing a final concentration of 0.01% Triton-X100 and 1 mM EDTA). The reaction mix was added to black 384-well plates to validate primary hits that modulate DDAH activity. The release of CH3-SH was monitored fluorimetrically by adding CPM as described. 18
Application of the L-Citrulline Assay to Cells
The feasibility of the citrulline assay in cell culture was validated by measuring the levels of L-citrulline in cell lysates applying a protocol similar to that described above. First, primary microvascular endothelial cells (HMVECs) were seeded in 75-cm2 cell culture flasks until confluency. The cells were exposed to 1 mM L-arginine for 24 h in the presence of vehicle control. The cells were washed with phosphate-buffered saline (PBS) and then dissociated with 3 mL Accutase for 3 min at 37 °C/5%CO2. The cells were then pelleted down by centrifugation and lysed by adding lysis buffer (containing 100 mM Na2HPO4, 1% NP-40, 1× protease and phosphatase inhibitors). The suspension was kept on ice for 30 min prior to centrifugation at 13 000 rpm for 30 min at 4 °C. Finally, the cell debris was removed and the supernatant was collected for the citrulline assay. The citrulline assay was performed in a microplate assay as described above by transferring equimolar amounts of cell lysate and adding 0.5 volume of color-developing reagent. The mix was incubated at 60 °C for 90 min, and absorbance was measured as described above. Known concentrations of commercial citrulline were used to construct standard curves and to estimate the concentration of citrulline in the samples.
Results
Human DDAH1 (858 bp) encoding plasmid was successfully transformed into an E. coli system, and the PCR-positive clones were used for the production of rhDDAH1. Western blot analysis using both anti-DDAH1 and anti-GST antibodies confirmed that rhDDAH1 tagged with GST (56.5 kDa) was expressed only in the cells transformed with the vector encoding DDAH and induced by IPTG ( Fig. 2 ). Sepharose column purification and subsequent SDS-PAGE ( Fig. 3A ) and Western blot analyses ( Fig. 3B ) revealed that the protein can be purified to a single band for use in screening experiments. Despite earlier reports of difficulties producing soluble protein in an E. coli (BL 21) system, 24 our protein yield was consistently above 2 mg/L culture, probably due to optimal induction time, RNase, and the major protease-deficient production system used in our experiments.
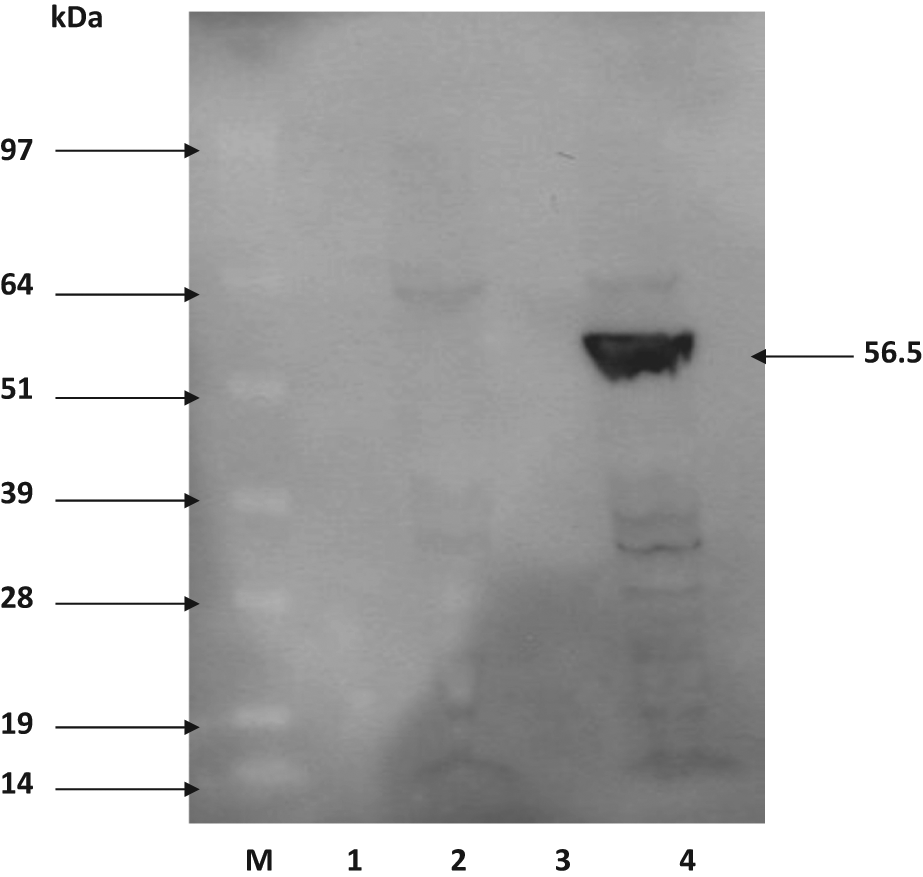
Western blot analysis showing the production of glutathione S-transferase (GST)–dimethylarginine dimethylaminohydrolase (DDAH) (56.5 kDa). Lanes 1 and 3, preinduction; lane 2, postinduction sample of an empty vector; lane 4, isopropyl-β-D-thiogalactopyranoside (IPTG) induction of DDAH vector; lane M, SeeBlue Plus molecular weight marker.
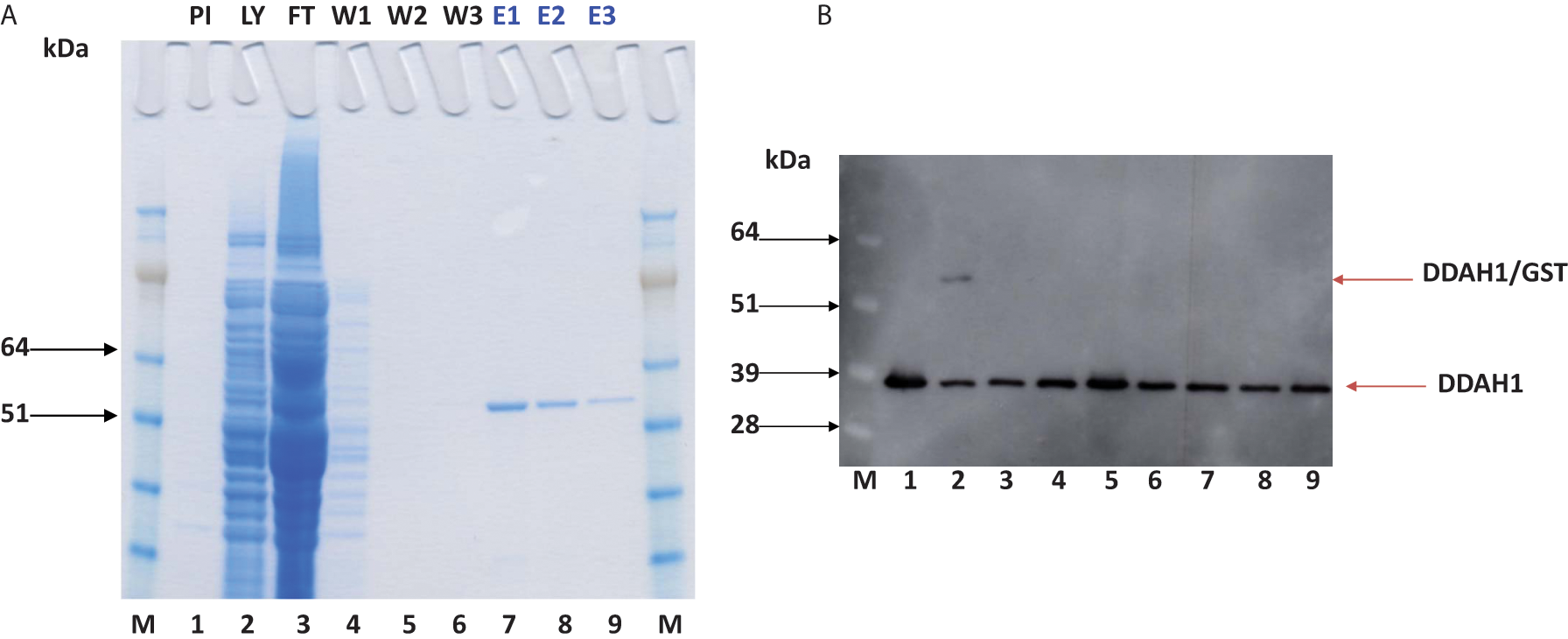
(
To find small-molecule modulators of DDAH activity, we first developed an enzymatic assay that would lend itself to high-throughput screening (HTS). A microplate-based L-citrulline assay to measure DDAH activity has been previously reported,
25
but this protocol requires harsh conditions, including heating the plates to a temperature of ~100 °C. In a high-throughput format, these conditions could cause sample evaporation and deformation of the reaction plates, and thus this assay is not practical for the purpose of comprehensive screening. Accordingly, we optimized the conditions, including the amount of enzyme, substrate, incubation time, and temperature, for a high-throughput assay (
Fig. 4
). In brief, various amounts of rhDDAH1 (0.1–10 µM) were incubated with various concentrations of ADMA (1 µM to 8 mM) for various time points (30 min to 10 h) at room temperature or 37 °C. In the final screening assay, we used near-catalytic activity (kcat ~ 0.7 min−1) conditions at 0.3 µM DDAH, 500 µM ADMA (Km = 180 µM), and 4 h of incubation time at 37 °C. The reactions were stopped and color was developed as described above followed by incubation at 60 °C for 90 min. Absorbance, proportional to DDAH activity, was measured at 485 ± 20 nm. To screen the entire library, we first optimized the biochemical properties of the assay as described above. We modified the technique so as to reduce the number of steps and facilitate robotic handling and throughput. Subsequently, HTS was performed using 384-well plates. The Stanford HTBC is equipped with a Caliper Life Sciences (Hopkinton, MA) workstation for sample preparation and analysis, Titertek (Huntsville, AL) multidrops, microplate dispenser, automated liquid handler and laboratory robotics for screening of chemical libraries. The Z′ score was consistently found to be between 0.7 and 0.8, indicating the robustness of the assay. Furthermore, the feasibility of the assay was demonstrated in cell culture study by quantifying the amount of L-citrulline in endothelial cells treated with L-arginine or vehicle. As expected, pretreatment with L-arginine increased the amount of intracellular L-citrulline significantly (
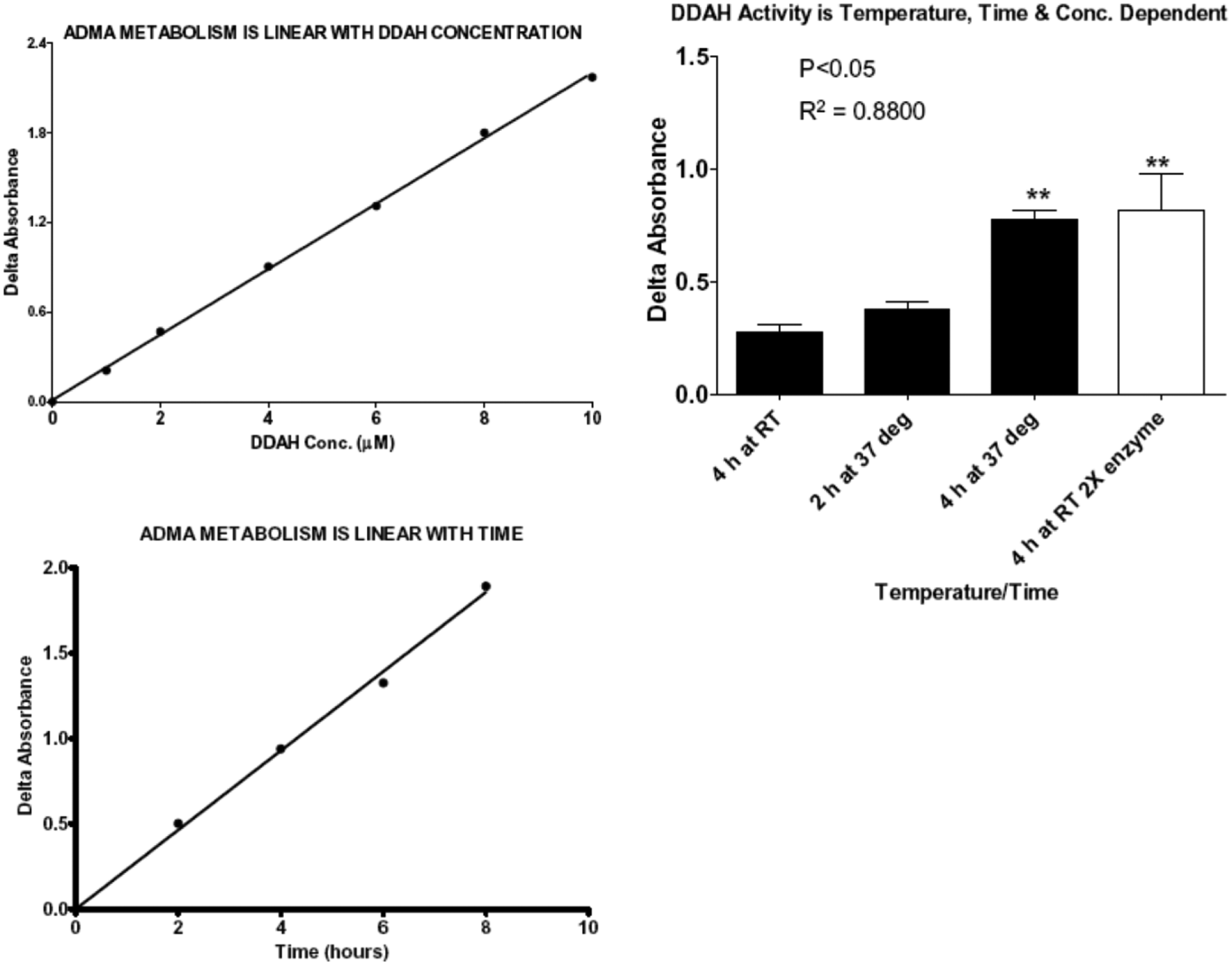
Citrulline assay showing that the conversion of asymmetric dimethylarginine (ADMA) to L-citrulline by dimethylarginine dimethylaminohydrolase 1 (DDAH1) is proportional to time, temperature, and enzyme concentration. Data are averaged from at least duplicate experiments. RT, room temperature.
Validation Assay
We first optimized the concentration of SMTC as a substrate in the colorimetric citrulline assay described above. Subsequently, we used this substrate in the fluorimetric assay near its kcat (kcat ~1 min−1) at a 100-µM substrate concentration (Km = 0.37 µM), 18 detecting the metabolite methanethiol (CH3-SH) using the CPM reagent. This study, in conjunction with the citrulline assay, narrowed down the number of hits by reducing potential false positives, such as pan-assay interference compounds (PAINS). 26 About 70% of the selected hits validated in the primary assay (about 35 compounds were retested in the secondary assay) were also inhibitors in the secondary fluorimetric assay. In addition, the validation assay also confirmed known DDAH inhibitors such as chloromercuribenzoate 7 and ebselen 14 and identified several new, potent inhibitors of human DDAH1. Not surprisingly, these include other mercury-containing compounds such as phenylmercuric acetate (IC50 <0.78 µM) and quinone-type compounds such as ChemDiv 2548-0707 (IC50 = 5.5 µM) and 2548-0703 (IC50 = 9.0 µM). However, it also includes more structurally novel compounds such as 4-mercapto-5-methoxy-2-phenyl-3(2H)-pyridazinone (4-MMP, IC50 = 12.7 µM) and SCH-202676 (IC50 = 13.3 µM) ( Fig. 5 ). In addition, our time-dependence kinetics study with two of the compounds (phenylmercuric acetate and 4-chloromercuribenzoic acid) indicates progressive inhibition, suggesting that their mode of inhibition might be irreversible ( Fig. 6 ). Furthermore, our follow-up study on selected inhibitors using the citrulline assay also confirmed the activity of these inhibitors against human DDAH1. Given their structure, it is possible that many of the compounds inhibit DDAH by reacting with the active-site cysteine. 13 Additional inhibitors of human DDAH1 and their potencies are shown in Table 1 .
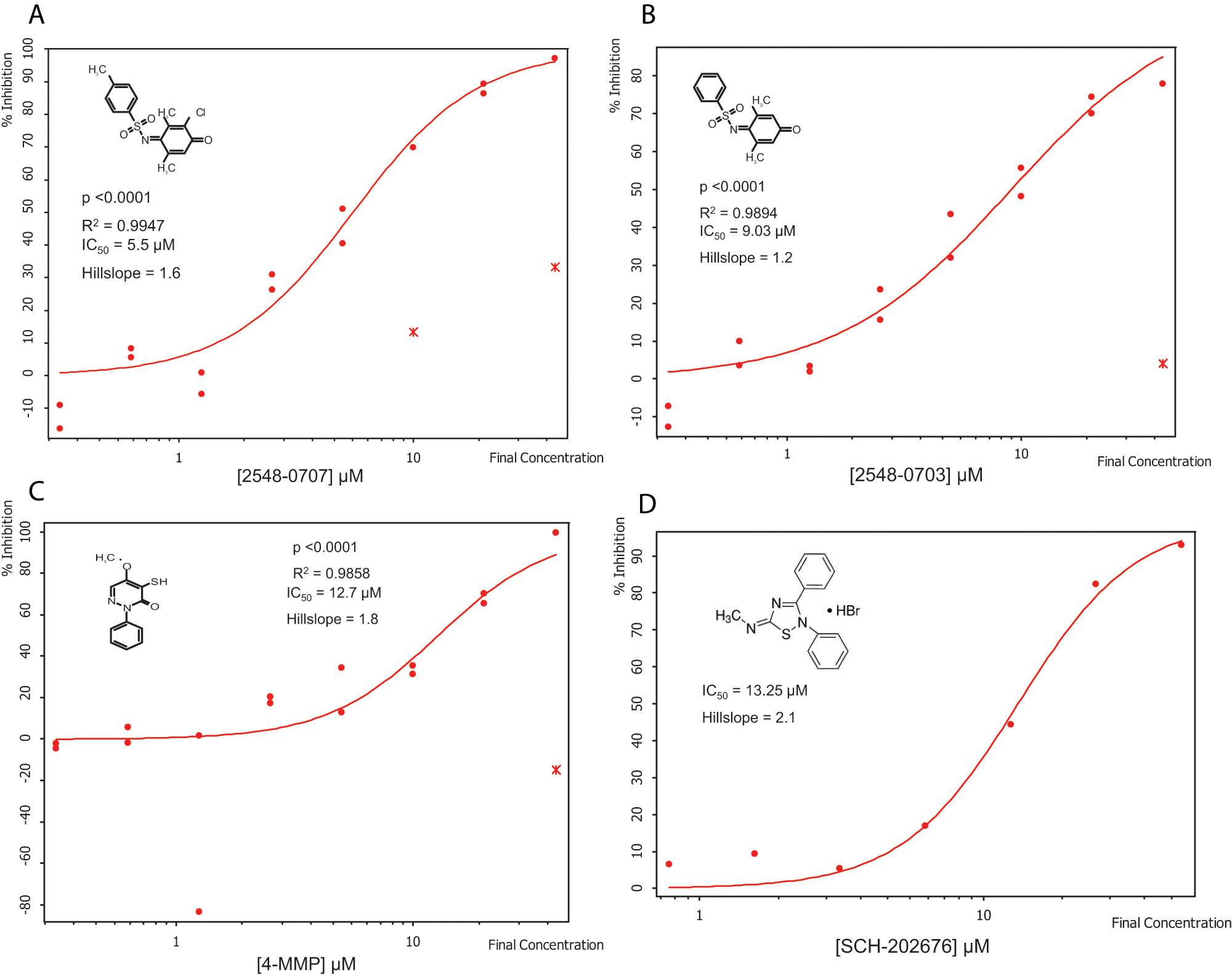
Curve fit data showing inhibition of human dimethylarginine dimethylaminohydrolase 1 (DDAH1) activity by selected small molecules using the 7-diethylamino-3-(4-maleimidophenyl)-4-methylcoumarin (CPM) assay: (
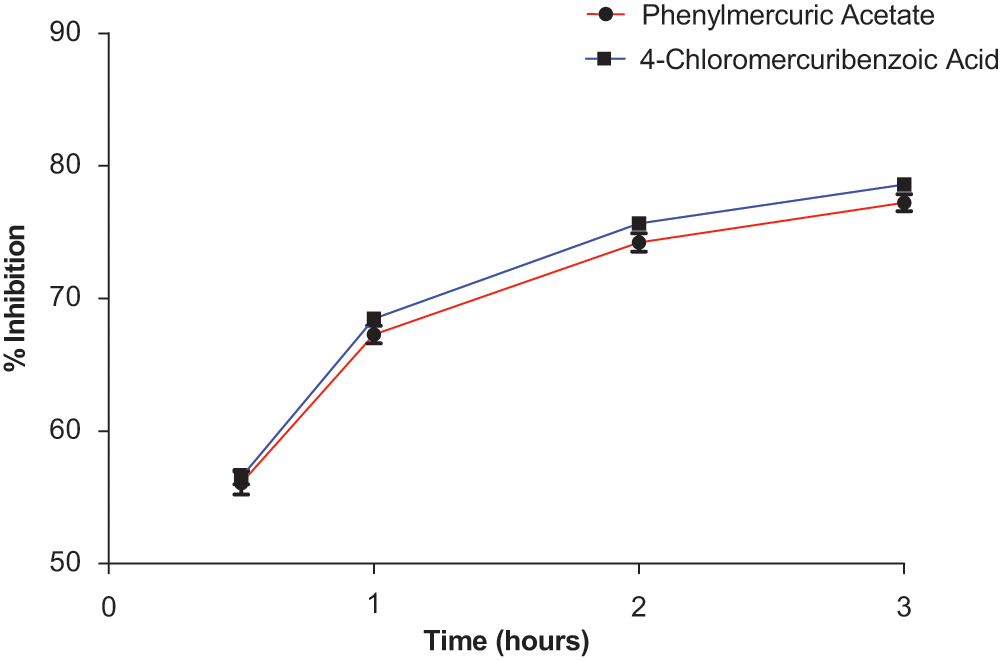
Time-dependent inhibition study of two small molecules, phenylmercuric acetate and 4-chloromercuribenzoic acid (each at 50 µM final concentration), using the fluorimetric 7-diethylamino-3-(4-maleimidophenyl)-4-methylcoumarin (CPM) assay (30 nM final enzyme concentration). Values are mean ± SEM. Experiments were performed in triplicates.
Novel Inhibitors of Human Dimethylaminohydrolase 1 (DDAH1)
The compounds listed in the table were validated in full dose-response curves. The inhibitory concentration at 50% (IC50) was calculated using Assay Explorer software (Accelrys, Inc., San Diego, CA).
Discussion
Small molecules that regulate the production of NO would be good molecular probes as well as potential therapeutics for cardiovascular and metabolic diseases. One possible mechanism to regulate NO is by controlling the activity of DDAH using small molecules ( Fig. 1 ). Toward this end, we have developed a high-throughput assay, as well as adapted a sensitive orthogonal assay, to detect small molecules that modulate the activity of this enzyme. Our HTS was conducted near Km concentration, a condition that ensured appreciable separation between the noise and signal to provide a good Z score in our hands using the described colorimetric assay. We found that the concentrations used allowed reproducible linearity over the period of time that our screen was conducted. In addition, our primary assay has an added advantage of using an endogenous substrate over the secondary assay that uses an artificial substrate.
Potential applications of DDAH agonists
Drug development programs are not typically directed toward enzyme activators. Nevertheless, DDAH represents a compelling target for allosteric activation. The ADMA/NO/DDAH pathway is involved in a number of pathophysiological conditions characterized by elevated ADMA and impaired NO function as a result of direct or indirect impairment of DDAH activity. These conditions include hypercholesterolemia, hyperhomocysteinemia, hypertriglyceridemia, stroke, erectile dysfunction, peripheral and coronary artery diseases, systemic and pulmonary hypertension, atherosclerosis, primary dysmenorrhea, cytomegalovirus infection, preeclampsia, chronic kidney disease (CKD), nonalcoholic steatohepatitis (NASH), nonalcoholic fatty liver disease (NAFLD), insulin resistance, and diabetes mellitus.5,9,27,28 These pathologies could potentially be ameliorated or reversed using small molecules that activate DDAH.
Potential applications of DDAH antagonists
In contrast, small molecules that inhibit DDAH activity could potentially be useful in diseases where an overly active DDAH needs to be reduced and ADMA levels need to be elevated as in pulmonary fibrosis 12 and conditions where NO production is principally driven by iNOS as in sepsis. 10 Our screening effort using a recombinant protein has revealed a number of small molecules that modulate human DDAH1 activity. Among these, we have observed that DDAH is very sensitive to organomercury compounds such as phenylmercuric acetate (IC50 < 0.78 µM), thimerosal (IC50 = 0.46 µM), and cumertilin (100% inhibition at 25 µM). This is consistent with the discovery by Ogawa et al. 7 of DDAH in 1987, at which time they observed that the enzyme (isolated from rat kidney homogenates) was sensitive to the mercury-containing compounds p-chloromercuribenzoate and mercury chloride, leading them to correctly predict the involvement of a thiol-containing motif in the active site of the enzyme. This hypothesis was later confirmed in human DDAH1 (which shares 93% homology with rat DDAH).9,20 Furthermore, we suspect that electrophilic compounds such as ChemDiv 2548-0707 and 2548-0703 ( Fig. 5 ) could also react with the active-site cysteine.
The presence of a cysteine residue (Cys 273) in the catalytic site of DDAH1 appears to have created a vulnerability of DDAH to inhibition by small molecules that contain a sulfhydryl group. Many of the compounds listed in Table 1 contain sulfur, and it seems likely that their inhibition of DDAH is by the formation of a disulfide bond with the catalytically active site. Indeed, the isothiazolo[5,4-b]pyridin-3-one core found in many of the molecules ( Table 1 , last 13 entries) bears a striking resemblance to ebselen, which has been previously shown to inhibit DDAH by covalently reacting with the active-site cysteine. 14 Similarly, 4-(2, 5-dioxo-2,5-dihydro-1H-pyrrol-1-yl)benzoic acid ( Table 1 , 2nd entry) contains a maleimide moiety, which is known to react with cysteine residues. Although these inhibitors could conceivably be used as probes for in vitro characterization of DDAH, such potentially nonspecific inhibitors could have off-target effects via their reaction with other cysteine-containing proteins. Nonetheless, several marketed drugs are covalent inhibitors, and about 5% of these drugs are in use in cardiovascular medicine. 29 For example, aspirin (to reduce the risk of heart attack and stroke) and Plavix (for coronary artery disease, cardiovascular disease, and peripheral vascular disease) are examples of widely used covalent inhibitors. However, DDAH inhibitors that possess other functionalities may confound an understanding of their actions in vivo. For example, the seleno-organic compound ebselen strongly inhibits DDAH activity in vitro, as shown by others 14 and in our present screening (IC50 = 3.9 µM). However, ebselen is also known to be an antioxidant 30 and thereby could protect DDAH from oxidative stress, 9 complicating any simple interpretation of the biological effects of the drug. In addition to these likely covalent inhibitors, some of the molecules, such as 3-(1-azepanyl)-1-(1-naphthyl)-2,5-pyrrolidinedione and 3- [5-(4-methylphenyl)-2-furyl]propanoic acid ( Table 1 , 1st and 6th entries), do not contain obvious electrophilic moieties and could thus be acting noncovalently.
In summary, we have developed a robust DDAH assay that uses the natural substrate ADMA and is suitable for HTS to find chemicals that modulate DDAH activity in vitro and in cell-based assays (
Footnotes
Acknowledgements
The authors are grateful to Prof. Neil McDonald (Birkbeck College, London) for providing human DDAH1 plasmid and to Dr. David Solow-Cordero and Jason Wu of the High Throughput Bioscience Center for their technical assistance. We are also grateful to the Stanford PAN facility and Chemistry Department for their DNA sequencing and mass spectrometry services, respectively.
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported in part by grants to JPC from the NIH (RC2HL103400, 1U01HL100397, and K12HL087746), AHA (11IRG5180026), Stanford SPARK Program, and the Tobacco-Related Disease Research Program of the University of California (18XT-0098). YTG was a recipient of the Stanford School of Medicine Dean’s fellowship (1049528-149- KAVFB) and is currently supported by the Tobacco-Related Disease Research Program of the University of California (20FT-0090). Keisuke Yamada was a visiting scholar.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
