Abstract
There is a heightened focus on the need for interprofessional collaboration (IPC) to improve person-centered care. The unique challenges of the home healthcare context are not reflected in existing frameworks. The purpose of this work was to develop an interprofessional competency framework for home healthcare and to identify enablers and barriers to implementation. The framework was co-designed with home healthcare clients, providers and leaders through a 5-step process: a rapid literature review, “Design Day,” iterative co-design, shareback meetings, and refinement. Seven competencies were identified around the core value of patient-centered care, supported by 4 guiding principles. The framework was designed to promote individual-, team- and organization-level competency through identifying required elements at each level. Three months after clinical leaders were introduced to the IPCC Framework, 38 participated in workshops in which they provided insights on enablers and barriers to implementation. These were analyzed thematically with reference to the COM-B theory of change model. Major themes reflected capabilities to implement practice changes, opportunities enabling the integration of IPC, barriers to implementing IPC, and motivation to practice interprofessionally. Most identified barriers existed structurally at the team and organizational levels, limiting or disincentivizing interprofessional collaboration. This framework provides an approach that home healthcare organizations can use to guide the advancement of IPC, identifying how competencies may be enacted at the individual, team, and organizational levels within the relatively autonomous and geographically disparate context of home healthcare.
Keywords
Introduction
Internationally, there is a heightened focus on the need for interprofessional collaborative practice to improve person-centered care. 1 The World Health Organization defines interprofessional practice as the state in which “. . .multiple health workers from different professional backgrounds provide comprehensive services by working with patients, their families, caregivers and communities to deliver the highest quality of care across settings.” 2 This requires clear, efficient communication and collaboration between healthcare providers of different disciplines as they care for shared clients. 3 Without this collaboration, clients and families must assume responsibility for communicating clinical information with and between healthcare providers 4 – placing substantial burden on the client or caregiver, increasing the risk of inaccurate information sharing, and limiting opportunities for clarification and follow-up between healthcare providers. 5
Accordingly, there have been considerable efforts in many countries to study the contributing factors that may influence interprofessional collaboration (IPC) between healthcare team members, with theoretical frameworks or models developed in Canada6,7 and Norway 8 based on reviews of the literature, and in Finland, 9 New Zealand, 10 the United Kingdom, 11 and the United States 12 based on primary data (interviews, group discussions, and observational studies with providers and leaders). These models have addressed factors at the individual through system levels that are required as facilitators of interprofessional practice. While they provide a broad understanding of concepts and relationships, further work is needed to support operationalization and measurement of IPC behaviors in practice. This practical step is advanced through 3 additional frameworks which explicitly identify measurable behaviors associated with specific competencies.13 -15 Common competencies identified across all 3 were shared decision making/collaborative leadership, communication, and knowledge of roles and functions; 2 frameworks13,14 also contain a focus on inclusivity, interprofessional conflict resolution, and continuous quality improvement.
In Canada, as in many international contexts, there is also a growing focus on the potential contributions of home healthcare to broader health systems 16 – as the setting in which the vast majority of people prefer to receive care and as an opportunity to manage costs and improve access to care.17,18 In Canada, 6% of the population receives home care and an additional 3% have been identified as needing but not receiving it. 19 Home healthcare encompasses a broad range of services, including nursing, personal support, and allied health services (e.g., occupational therapy, physiotherapy, social work, speech language therapy and nutrition/dietetics).
In the unique practice context of home healthcare, there are practical considerations for implementing interprofessional collaboration which extend beyond those seen in institutions. In Ontario, Canada, most publicly funded home healthcare is coordinated by a quasi-governmental organization which contracts individual homecare services to provider organizations on a fee-for-service basis. This structure can result in clients receiving home healthcare services from multiple organizations and limits the availability of paid hours to engage in indirect care activities. Even when a home healthcare client receives multiple services from 1 organization, the providers’ varying work schedules and lack of co-location create few opportunities for interprofessional collaboration. This challenge is not unique to the Ontarian or Canadian context; earlier work by Landers et al. 20 identified similar challenges in communication and coordination across providers working within the US Medicare-funded system.
To date, comprehensive IPC frameworks have been developed for the practice contexts of acute and primary care settings, as identified above. However, as previously identified by Ritchie et al. 21 in their work to develop a care quality framework for home healthcare, while frameworks from other contexts serve as useful inspiration, there is a need for context-specific adaptation in order to ensure that developed frameworks are appropriate for and usable within a homecare context. Two studies presenting homecare-specific conceptual frameworks related to IPC focus more narrowly on communication 22 and shared decision-making, 23 providing greater depth related to enabling these competencies in homecare contexts. Additional insights are provided by a qualitative study of home healthcare nurses, which found that collaboration was influenced by outreach and ongoing relationship maintenance, care coordination practices, and congruence between organizational values and nurses’ personal values. 12
In addition to the differences in practice context, there are also substantial differences in the composition of the home healthcare workforce as compared to acute and primary care settings. Current IPC frameworks have primarily been informed by engagement with physicians, physician assistants, nurses/nurse practitioners, midwives, or social workers. The inclusion of physical and occupational therapists, which disciplines each support over 30% of homecare clients, 24 has been rarer. To our knowledge, only Légaré et al’s study of interprofessional decision making in homecare has included the insights of personal support workers, 23 who provide >70% of paid homecare services in Ontario. 24
Given the unique nature of the work context and workforce composition in home healthcare, and the current lack of comprehensive, homecare-focused interprofessional collaborative competency frameworks to support IPC, there is an opportunity to build on existing work by developing such a framework. This could be used to inform home healthcare provider organizations’ work to create the enabling conditions for successful implementation of interprofessional collaboration practices which are widely recognized as improving person-centered care.
Purpose
Develop an Interprofessional Collaboration Compe-tency Framework tailored to the unique context of home healthcare, and
Identify barriers and enablers for implementation into practice, from the perspective of clinical homecare leaders.
Phase 1: Framework Development
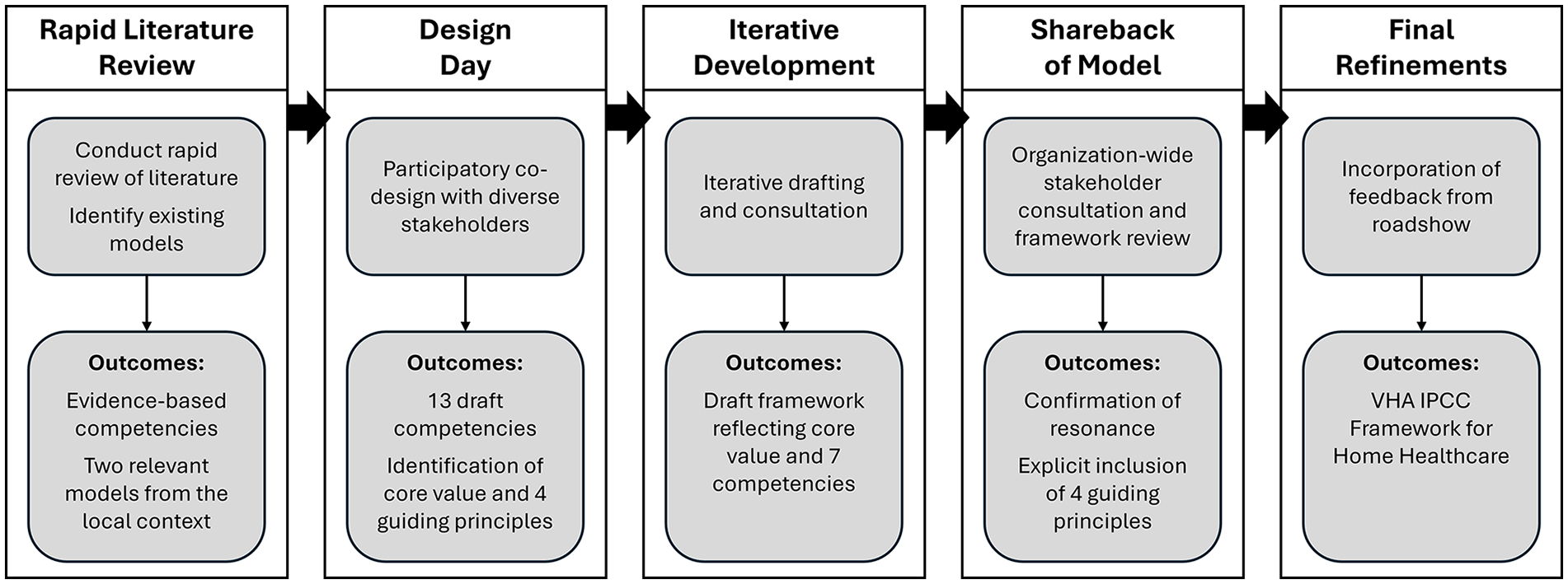
Iterative participatory co-development process.
Step 1: Rapid Literature Review
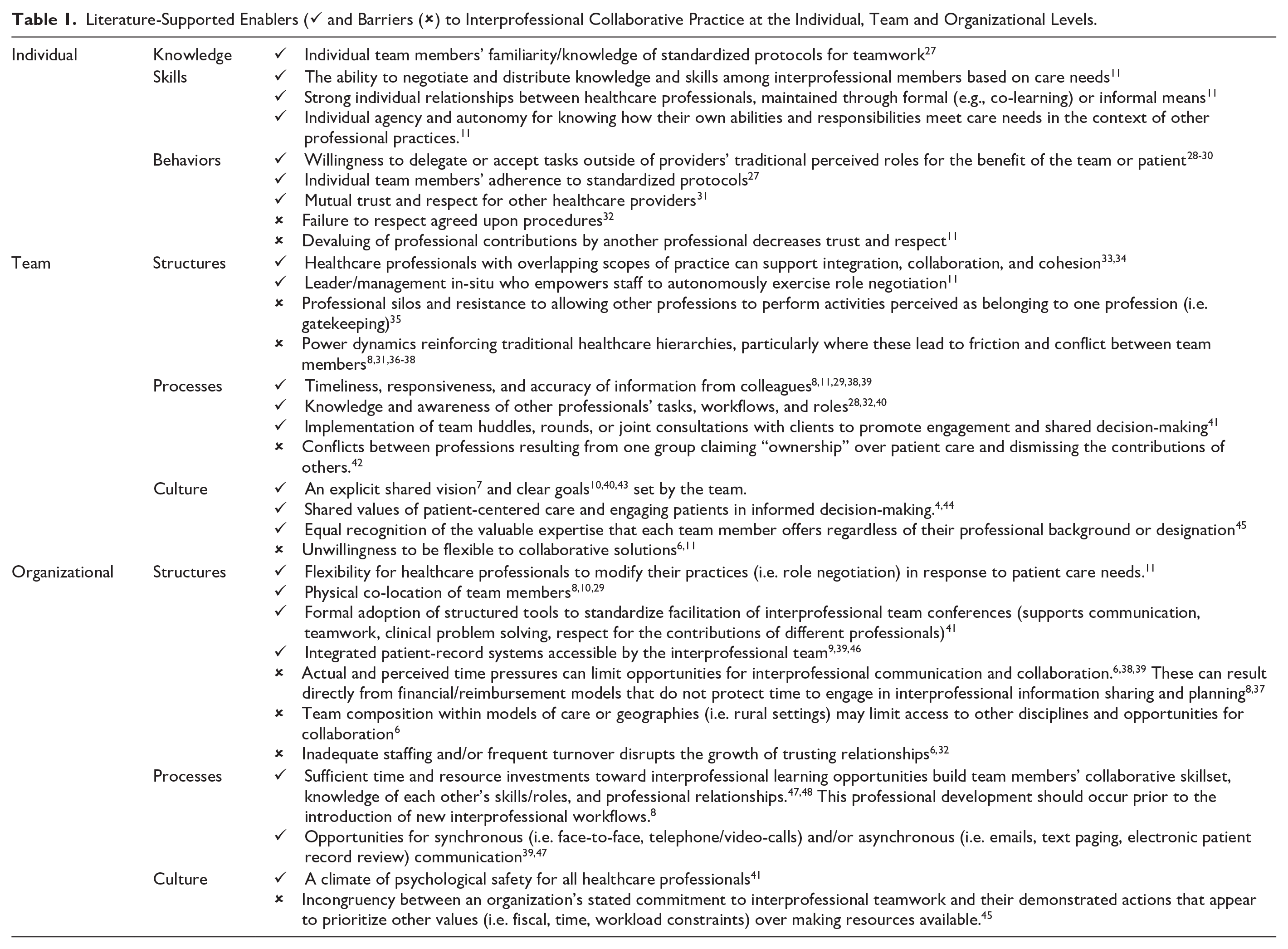
A rapid literature review 25 was used to identify evidence-based competencies and existing frameworks for supporting interprofessional collaboration. Details regarding the search, screening and data abstraction, conducted in Covidence®, 26 are available in Appendix A. Key findings (Table 1) highlight competencies of individual healthcare providers, the interprofessional team, and the provider organization that are required to support interprofessional collaborative practice. The majority of evidence-based competencies were reflected within the Canadian Interprofessional Health Collaborative (CIHC) Framework 13 and Sunnybrook’s Interprofessional Collaboration Framework. 14 Findings from this review, including the 2 identified example frameworks, provided an evidence-based foundation for future steps.
Literature-Supported Enablers (✓ and Barriers (✗) to Interprofessional Collaborative Practice at the Individual, Team and Organizational Levels.
Step 2: “Design Day”
The foundational co-design event was a day-long “Design Day” which engaged 94 stakeholders to seek broad perspectives on core interprofessional collaboration competencies in home healthcare. Contributors included client partners (3); point-of-care providers of personal support (5), nursing (9), allied health (9) and social support services (1); clinical leaders and supervisors directly supporting each discipline (27); senior clinical leaders (8); scheduling coordinators (8); and specialists with expertise in information technology (3), clinical practice and education (4), quality (3), human resources (1), communication (3), innovation (2) and operations (8). Participants were introduced to the project vision to co-design the future of interprofessional home healthcare. As background, they were presented with an evaluation of the organization’s current state, the WHO’s definition of interprofessional care, 2 2 example interprofessional competency frameworks,13,14 and a summary of literature-based interprofessional care concepts. Smaller (6-8 person) mixed-perspective groups then discussed values, competencies and practices that they believed were most important for interprofessional collaboration. Note-takers at each table recorded the ideas raised during these discussions, with a focus on interprofessional population health-based care, interprofessional competencies, and leadership competencies in interprofessional care. Synthesis of the notes from each group identified 13 priorities: team development, safety and care, collaboration and growth, a person-centered approach, organizational consistency, interdepartmental collaboration, culture shift and standardization, championing team investment, team empowerment, cross-disciplinary communication, service integration & access, skills development, and navigating high-pressure situations.
Step 3: Iterative Development
To create the draft framework, the Design Workstream team held 5 virtual meetings to prioritize and define key competencies based on the literature review, CIHC and Sunnybrook frameworks,13,14 and Design Day findings. These were used to create an initial map of behaviors, actions and skills that participants identified as necessary for interprofessional collaboration. Design Workstream members used collaborative strategies including group discussion and asynchronous voting and ranking exercises to review, prioritize, rank, redefine, and customize these competencies to address the needs of the Ontario homecare context. The workstream leads (GP, JDS) synthesized the outcomes of these meetings and proposed 2 potential draft frameworks based on the identified priorities. These were discussed, compared to the CIHC and Sunnybrook frameworks, and iteratively refined. Throughout this process, meeting and asynchronous engagement records including minutes, presentations, collaborative documents (e.g., digital collaboration boards, spreadsheets), and iterative framework drafts were used to track team processes, reasoning and decisions. Twice during the development process, progress was reviewed with the One Team Project Team which provided oversight and direction.
Step 4: Shareback of Model
Shareback meetings with leaders throughout the organization were used to ensure resonance and support refinement of the framework language and definitions. Four large group meetings invited feedback from clinical leaders across all disciplines and regions (60); senior leadership of digital solutions, communications, research, finance and legal/privacy (6); and leaders from clinical practice (1), quality (1), and client engagement (1). Two One Team Project representatives also sought feedback directly from point of care through individual meetings with allied health (1), nursing (1) and personal support (1) providers and from 2 client and caregiver partners. Feedback from the shareback sessions provided confirmation that the proposed framework resonated, suggested opportunities to clarify language, and identified a preference to include 4 “guiding principles” in the graphic depicting the framework.
Step 5: Final Refinement
In the sixth and final meeting of the Design Workstream, this team reviewed feedback from shareback meetings, added the guiding principles, and adjusted the wording of the competencies and definitions. Final refinements and clarifications were approved by the leaders and senior sponsors of the One Team Project Team and Design Workstream.
Result: VHA’s Interprofessional Collaboration Competency (IPCC) Framework for Home Healthcare
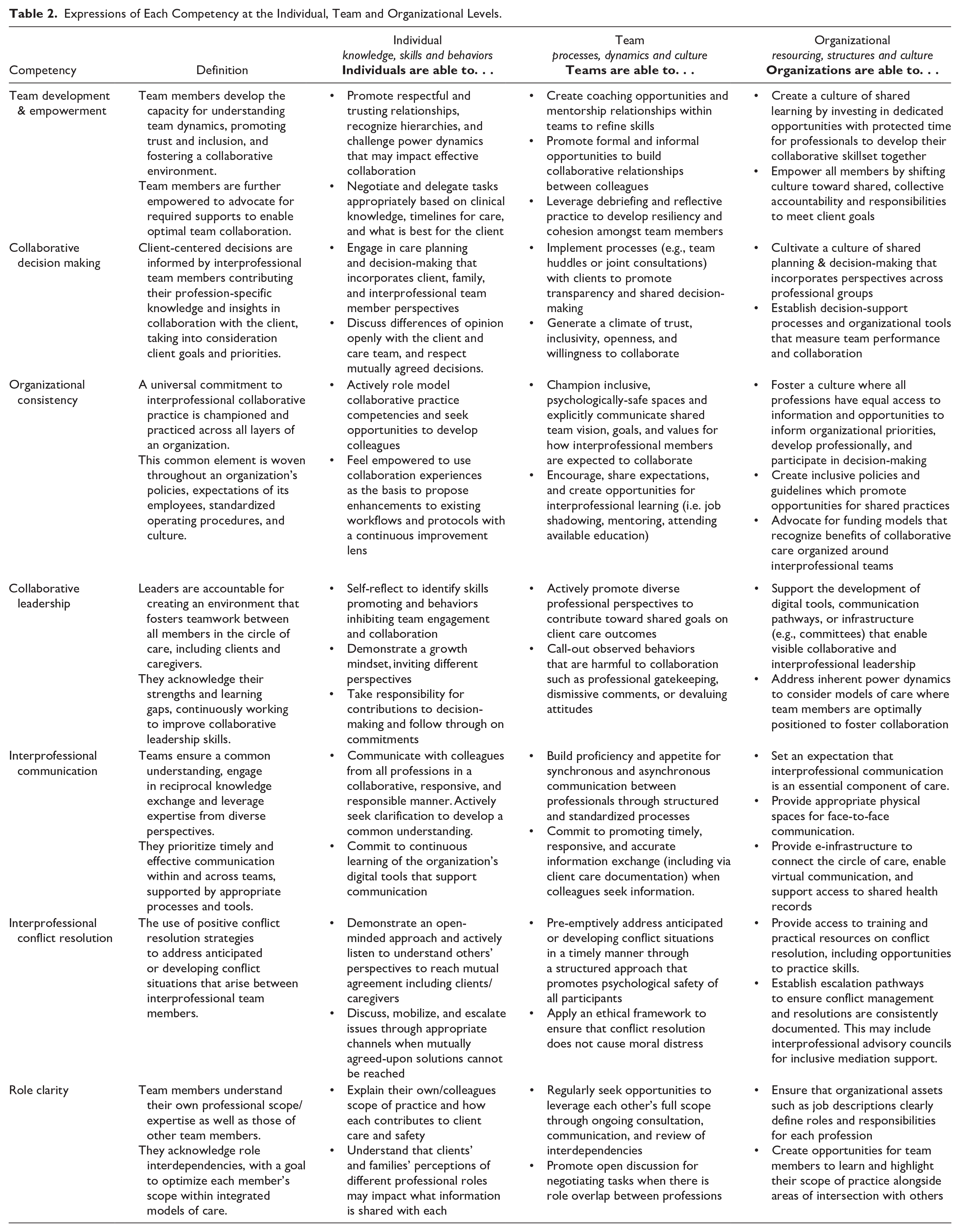
VHA’s IPCC Framework for Home Healthcare (Figure 2) aims to enhance person-centered care – the core value at the center of the framework. This is supported by a commitment to 4 guiding principles that influence how the framework is applied: (1) creativity and innovation, (2) the quintuple aim, 49 (3) diversity, equity and inclusion, and (4) best practice, research and education. The framework is designed to promote individual competency through clearly identifying requisite knowledge, skills and attitudes, and to promote team- and organization-level competency through identifying structures, workflows and culture that support interprofessional practice. The identified competencies for interprofessional collaboration in home healthcare are: (1) team development and empowerment, (2) collaborative decision making, (3) organizational consistency, (4) collaborative leadership, (5) interprofessional communication, (6) interprofessional conflict resolution, and (7) role clarity. These competencies are further defined in Table 2.
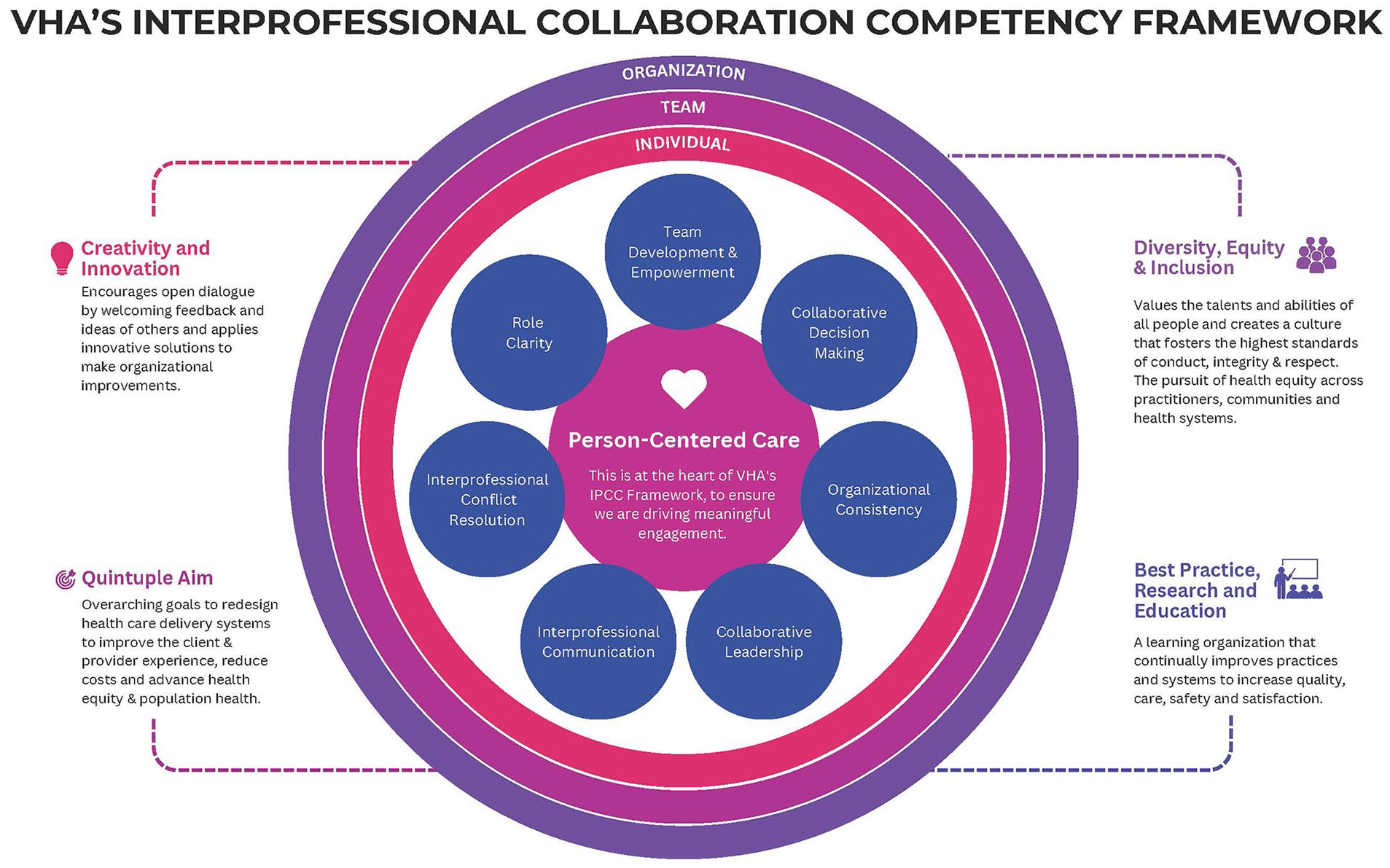
VHA’s Interprofessional Collaboration Competency Framework for home healthcare.
Expressions of Each Competency at the Individual, Team and Organizational Levels.
Phase 2: Clinical Leadership Perspectives on Implementation Requirements
To prepare for organization-wide implementation of the IPCC Framework, clinical leaders were provided with comprehensive training and education. To assess practice readiness and identify barriers and enablers of framework implementation, these clinical leaders were surveyed immediately after the training and invited to participate in 3-month follow-up workshops.
Recognizing that adoption of the IPCC Framework would require practice change from all individuals at the organization, the COM-B theory of change model 50 was used to map leaders’ insights regarding: perceived Capabilities (C) surrounding individual-level knowledge and skills, and team- and organization-level structures and processes related to the IPCC Framework; Opportunities (O) for enabling interprofessional competencies within the home healthcare context; and Motivation (M) to practice interprofessionally – all of which are required to influence the intended Behavior change (B) of practicing interprofessional collaboration.
Methods
Results
Post-training surveys
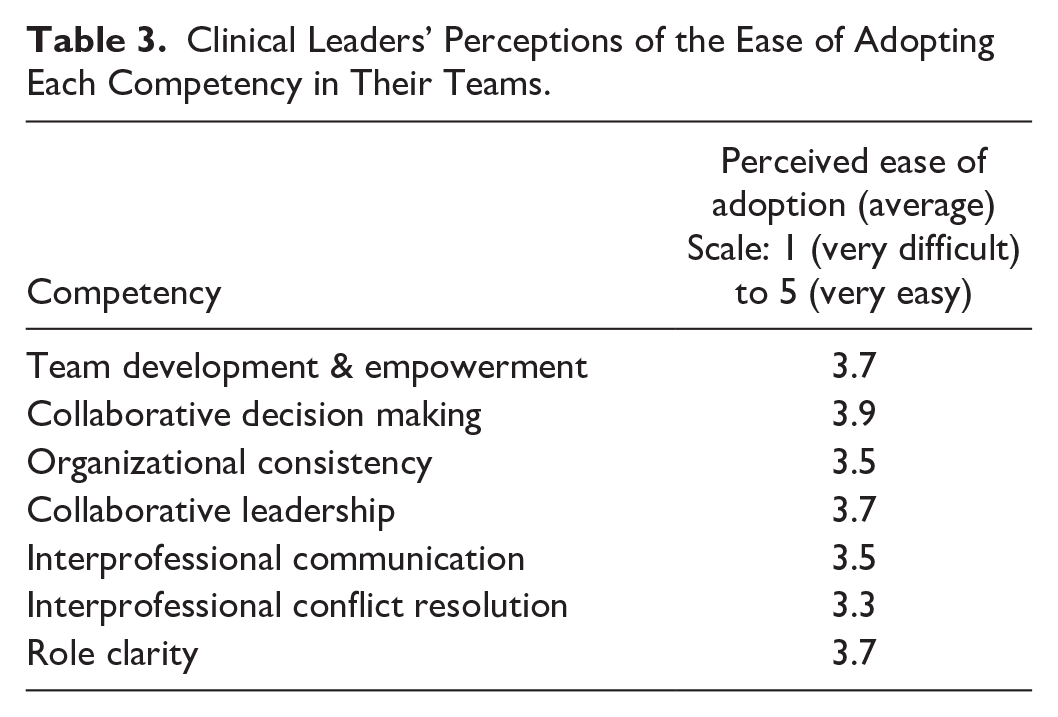
In post-training surveys (n = 52), clinical leaders from nursing (n = 10), personal support (n = 10), allied health (n = 27) and social support (n = 5) reported that they expected most competencies to be relatively easy to adopt within their teams (Table 3). The greatest challenges were anticipated with respect to interprofessional conflict resolution, interprofessional communication, and organizational consistency.
Clinical Leaders’ Perceptions of the Ease of Adopting Each Competency in Their Teams.
Post-training workshops
Three workshops were held with a total of 38 clinical leaders representing nursing (n = 5), personal support (n = 8), allied health (n = 21) and social support (n = 4) services. Clinical leaders across the workshops identified enablers and barriers to framework implementation at the individual, team, and organizational levels (Table 4). Most leaders perceived individual-level strengths in capability and motivation, while discussion of team- and organization-level factors had a greater emphasis on structural barriers or factors which disincentivized interprofessional collaboration.
Summary of Clinical Leaders’ Perceived Enablers (✓) and Barriers (✗) to Applying VHA’s IPCC Framework.
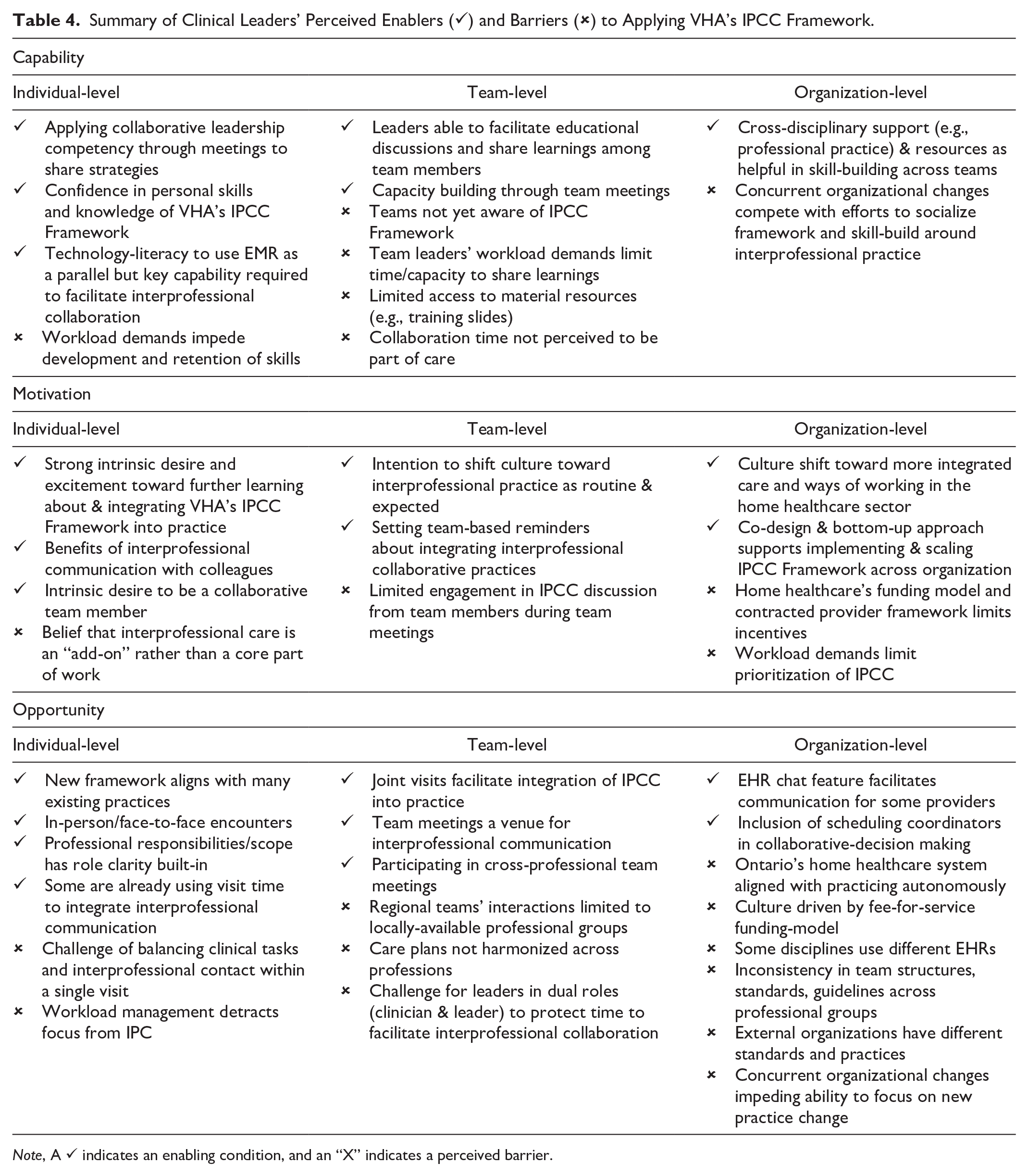
Note, A
Theme 1: Capability to Implement Practice Change
Most leaders reflected on their experiences implementing strategies from the framework to build capacity within their point-of-care teams. They shared how their teams applied competencies such as collaborative leadership, interprofessional communication, and role clarity through interprofessional team meetings at the team and leadership levels. In those meetings, team members shared personal learnings and healthcare providers from different professional teams were invited to speak about their roles: We come together as leaders on that [geographic] team and share ideas and supports and learn from each other about ways to support our teams and collaborate and it’s actually been really helpful. (Allied health leader)
Some allied health leaders shared how their teams were adjusting their workflows to leverage features within the electronic health record (EHR) platform that facilitated interprofessional communication: [In my team,] we were able to focus on some of the strategies on interprofessional communication wherein we could use the [EHR] chat function to communicate with other members. So that was received very well by the team. (Allied health leader)
Some leaders whose teams had struggled to make progress on implementation shared a need for practice-based learning resources (e.g., presentation slides, booklets) to support socialization of the framework and encourage interprofessional practice. Similarly, others suggested client-facing resources to clarify provider roles: I know one of the things that we’re talking about is the [client-facing web interface]. . . possibly [we could include] a blurb about our roles for clients and families because I think that’s also helpful. (Personal support leader)
Additionally, some leaders shared that they had not yet worked with their teams on implementing the IPCC Framework due to competing demands related to other ongoing organizational changes.
Theme 2: Opportunities Enabling Integration of IPC
Many leaders shared environmental factors which enhanced their ability to facilitate IPCC Framework implementation. Several competencies, such as role clarity and interprofessional communication, were viewed as more innate and built into clinical care, providing natural opportunities to engage. In these cases, the framework validated approaches to interprofessional practice such as conducting client visits jointly with other care team members, including scheduling coordinators in collaborative decision-making, and participating in cross-professional team meetings: We’ve always worked in collaboration with our other multi-disciplinary teams, but now that it’s official and you know that it’s recommended, . . . It wouldn’t be viewed as a waste of time because all of us are working for the same client who’s in the center of all. (Allied health leader)
Allied health leaders specifically highlighted the organization’s digital communication platforms, including the EHR’s chat feature, as valuable in-workflow tools for interprofessional communication.
Theme 3: Barriers to Implementing IPC
Various elements of the organization of home healthcare work, team workloads, and the time required to change practices were identified as barriers to creating a work culture that prioritizes interprofessional collaborative practice. The majority of leaders expressed that these barriers were often driven by the conditions of the dominant home healthcare sector fee-for-service funding model, which generally encourages a narrower task focus within time-limited visits. This model was perceived to exacerbate the siloing of care delivery and disincentivize interprofessional collaboration. Several leaders shared the perception that the opportunities for point-of-care healthcare providers to practice interprofessional communication were not built into the timing of clinical encounters; instead, providers felt that they needed to cut care visits short or contribute unpaid time after client visits to practice interprofessional collaboration: I’m still really challenged with this area because ultimately the system is not there to support this interprofessional collaboration . . . For me to communicate with the nurse that’s involved . . . I don’t even know who the nurse is. . . there’s certainly no remuneration associated with that extra work. (Allied health leader)
Additionally, organizational consistency to enable collaborative decision-making was noted by most participants to be lacking between professional groups; specifically, difficulty identifying all care team members, a lack of harmonized care plans in a centralized EHR, and inconsistent scheduling practices across discipline-specific teams were identified as limitations of the existing team and organizational structures.
I feel like we are missing that opportunity for the nurse and the occupational therapist to reach out to each other instead of going through a supervisor. [Who is assigned to a client] is available in [the nursing EMR], but our [allied health] providers don’t have access to it . . . there needs to be a mechanism for more direct communication with [all] service providers. (Nursing leader)
Lastly, several leaders shared their difficulties collaborating interprofessionally with members of the client’s care team from external provider organizations – a challenge which stemmed from differing processes, standards, and scopes of practice across organizations: It’s very hard to navigate across multiple organizations and [the funder] has a different process than care coordinators and it’s just hugely difficult (Allied health leader)
Theme 4: Motivation to Practice Interprofessionally
All leaders were intrinsically motivated to practice interprofessional collaboration and believed that their teams shared this motivation. Some leaders shared optimism that the IPCC Framework could contribute to sector reform in ways that would minimize siloed work, while others shared their strong desire to see IPCC Framework competencies embedded into day-to-day practice: Giving [interprofessional practice] more visibility so that the nurses know this is an option and the direction we’re going as an organization. And not to feel like this is extra work because this is what you would be expected to be doing. This is not just a ‘by the way’ but actively seeking those opportunities for collaboration. (Nursing Leader)
However, previously discussed challenges relating to capability and opportunity also affected team- and organization-level motivation. Most participants discussed how perceptions of current workplace processes, priorities and compensation models disincentivized implementation of the IPCC Framework at an individual level.
The culture hasn’t changed, it’s still very much driven by the funding model . . . Client care is really important and it’s the bulk of our work . . . I can see a client or three clients, compared to me sitting in the whole day of a workshop. (Allied health Leader)
Discussion
This paper presented the development of VHA’s Interprofessional Collaboration Competency Framework for Home Healthcare. Inspired by the Sunnybrook framework 14 and the Canadian Interprofessional Health Collaborative Competency Framework, 13 VHA’s IPCC Framework incorporates insights from home healthcare clients and providers. It identifies 7 competencies required at the individual, team and organizational levels to support interprofessional collaborative practice. In addition to previously identified competencies, the framework contains an emphasis on organizational consistency, which must be fostered very deliberately in this relatively autonomous and geographically disparate context (c.f., Chow et al 6 ). To this end, VHA’s IPCC Framework emphasizes the structural advantage of organizing work such that teams include point-of-care providers across disciplines rather than reinforcing professional silos, as has also been proposed for hospital-based care. 54
In considering IPCC Framework implementation, clinical leaders identified existing strengths, practices that could readily be integrated into team workflows, and anticipated barriers. Leaders perceived an intrinsic desire from point-of-care providers to be collaborative practitioners, reflecting a broader shift away from task-focused approaches toward team-based, holistic care. 4 They also shared some existing structures and practices, such as cross-disciplinary supports and EHR chat features, which facilitate the application of IPCC Framework competencies. Identified barriers largely centered on team and organizational structures which would need to change in order to align workflows and fully implement the IPCC Framework. Leaders also identified elements of broader health system structures that impact how completely the framework can be implemented.
Existing strengths of individual providers aligned with many identified competencies – particularly interprofessional communication, role clarity, and collaborative leadership. Individual-level barriers were identified related to high workloads, limited time with clients, and challenges balancing time for direct clinical care with interprofessional communication. These were exacerbated by a commonly held perception that interprofessional activities, while important, are not a core part of a client visit. This barrier was attributed to the contracted fee-for-service model which dominates home healthcare provision in Ontario; however, this prioritization challenge exists across healthcare settings (c.f., Allen et al 46 ). Within the fee-for-service model, there is a potential to support a shift in perception by ensuring that all parties – including clients and families – understand that interprofessional communication is part of the services expected within a client visit. Such a shift must be supported by organization- and health system-level recognition that allows appropriate time and resources for clinical collaboration.6,8 Concurrently, the broader adoption of interprofessional communication tools embedded within providers’ workflows (e.g., within the EHR) is a common recommended enabler of interprofessional collaboration 39 that may reduce the time required for effective communication.
Paid team meetings were understood to be important professional development and learning opportunities. Participants highlighted that more such opportunities were needed. For client cases requiring more extensive interprofessional communication, interprofessional joint visits have been highlighted in the present work and by Kushner and Strasser 41 as important for enabling shared decision-making; similarly, case-focused interprofessional huddles or rounds have been identified as useful opportunities to support collaboration. 41 Creating and engaging in these interprofessional opportunities requires time and coordination from healthcare providers, emphasizing a need to ensure that organizational expectations recognize and account for this time.6,8
At the organizational level, leaders identified some progress toward socializing IPCC Framework concepts, while highlighting a need for structural change. A particularly high priority, reinforced by the literature, was the availability of an integrated patient record/EHR system accessible by all members of the interprofessional team.9,39,46 A shared EHR would also provide a platform for the creation of care plans that could be harmonized across professions, enhance the utility of in-workflow tools for interprofessional communication, and enable transparency regarding all healthcare providers’ scheduled visits to each client.
While these organizational measures would address many barriers to interprofessional collaboration within a service provider organization, the current reality that a client may receive home healthcare from many organizations may limit their impact. If care integration at the broader system level could be designed in a way that is sensitive to required organization-level IPCC Framework competencies, this could help to bridge current challenges and create shared expectations for communication and collaboration. 3
Strengths and Limitations
VHA’s home healthcare-specific IPCC Framework is grounded both in the academic evidence base and in extensive consultations with home healthcare clients, care providers, and leaders. The rapid review which informed the model development was limited to articles published in English since 2015 found within the Ovid MEDLINE database and would not have captured earlier literature or works not indexed in MEDLINE. All parties involved in the framework’s development were from a single large provider organization which provides service within southern Ontario, Canada. Developers reflected the organization’s experience in delivering care under both traditional fee-for-service and diverse integrated models of care. Allied health and nursing leaders were most vocal in sharing their perspectives on enablers and barriers to implementation; further work to elicit the perspectives of personal support and social care leaders may help to identify additional existing strengths and opportunities specific to those groups. Similarly, increased engagement with point-of-care providers could uncover further practical insight into enablers and barriers that may affect implementation. Broad consultation within the originating organization has supported the framework’s face validity in this context; perspectives from outside the organization are necessary to validate its potential generalizability. Work to date has been largely conceptual; rigorous evaluation of future implementations will support further understanding of its utility.
Current Status of the Framework
Since the creation of VHA’s IPCC Framework in 2023, the organization has made a deliberate effort to implement the Framework, build capacity, and embed the 7 competencies in its culture and operations. Pilot projects to create an enabling context and culture for interprofessional collaborative practice at the team and organization levels are being designed, implemented and evaluated. Examples include an integrated interprofessional care model, interprofessional rounds, shared scheduling and a digital coordinated care plan. Plans for scale and sustainability are under development.
Implications for Homecare Policy and Practice
The importance of enabling IPC is being emphasized across many health systems, including in Ontario, Canada where this framework was developed.1,2,55 VHA’s IPCC Framework provides a blueprint for home healthcare organizations to follow in pursuit of enabling interprofessional collaborative practice. It identifies and describes competencies to present a target for updating collaboration approaches within organizations. Current interest in reforming homecare and moving toward more integrated care models presents an opportune time to test the changes required to implement the framework as a strategy for enhancing IPC.
Conclusion
As a home healthcare-specific product, VHA’s IPCC framework provides an approach that home healthcare organizations can use to guide the advancement of interprofessional collaborative practice. As the first home healthcare-specific interprofessional collaboration framework, it contributes insights on how competencies may be enacted at the individual, team, and organizational level within the relatively autonomous and geographically disparate context of home healthcare delivery. This framework provides guidance on how interprofessional care can be advanced within an organization while highlighting opportunities to address system-level barriers in the creation of new models of integrated care.
Footnotes
Appendix A
Acknowledgements
Data Availability
Not applicable
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: All authors are employed by the organization at which the framework was developed.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Considerations
Ethical approval was not required for the work reported in this manuscript, which was conducted as part of an organizational quality improvement initiative.
Consent to Participate
Not applicable
Consent for Publication
Not applicable
