Abstract
The study focuses on the acceptance of remote monitoring (RM) in the home environment among elderly neurological patients during the pre-implementation phase of RM. Conducted at the neurosurgery outpatient clinic of Kuopio University Hospital in Finland’s North Savo region, the study included 30 patients. The participants were introduced to the prospective implementation of RM at home, and they completed a structured survey that recorded sociodemographic data and RM acceptance levels, informed by the literature on telemedicine homecare acceptance. Analysis using the SPSS 29.0 program featured chi-square tests to explore associations between RM acceptance and six sociodemographic variables: age, gender, education, living arrangement, place of residence, and caregiver presence during clinic visits. The major findings indicated that 80% of patients (24 out of 30) were receptive to RM at home. Statistically significant associations were found between living arrangement and RM acceptance (p = .007, OR = 0.357), and between education and RM acceptance (p = .025, OR = 0.667). The association between caregiver presence during clinic visits and RM acceptance (p = .088, OR = 4.857) showed a trend but did not reach statistical significance. No associations were found concerning place of residence, age, and gender. These findings highlight the need to consider sociodemographic elements in the design and implementation of RM solutions for elderly neurological patients. As a conclusion the study highlights the importance of tailoring RM to the specific sociodemographic characteristics of these patients in the pre-implementation phase to enhance adoption and effectiveness.
Keywords
Introduction
The adoption of remote monitoring (RM) solutions has the potential to transform home healthcare by enabling continuous health tracking and timely interventions, thereby reducing the burden on healthcare systems. 1 For RM solutions to be effectively implemented, understanding patients’ willingness to adopt RM prior to its implementation in the home environment is critical.2 -4
In this study, acceptability is defined as the likelihood of an individual adopting and using a technology, system, or solution.5,6 Prior research suggests that factors influencing acceptability vary between the pre- and post-implementation phases and differ across quantitative and qualitative research findings. 3 Previous studies suggested exploring how specific patient groups perceive RM before adoption, particularly the factors influencing their willingness to be monitored at home. 3 There is the need for acceptability studies tailored to diverse neurological conditions to better understand factors shaping acceptance levels in these populations. 4 Older adults prefer aging in place to maintain independence, familiarity, and identity, a choice underlined by the need for supportive services and accessible environments, especially as physical or cognitive limitations emerge.7,8 For elderly neurological patients, who require continuous monitoring for conditions like cognitive decline and mobility impairments, RM technologies provide crucial support by enabling real-time health tracking and reducing hospital visits. 4 However, the adoption of RM technologies remains underexplored, highlighting the importance of understanding RM acceptance to effectively tailor it to the needs of the elderly.8,9
Prior research has found that age, gender, and education affect telemedicine homecare acceptance among elderly individuals at risk for hypertension and diabetes, with telemedicine knowledge mediating these effects in the post-implementation phase. 10 Age negatively influences RM acceptance in elderly populations with chronic illnesses, while gender and education have a positive impact, with women and those with higher education showing greater receptivity. Rural residence was reported to negatively influence technology acceptance due to barriers such as limited access to devices and poor internet connectivity. 4 Additionally, living with caregivers was found to positively influence acceptance of telemonitoring solutions among neurological patients.4,11
Previous research highlights a gap in understanding RM acceptance among elderly patients with chronic neurological disorders. 4 Idiopathic normal pressure hydrocephalus (iNPH) is such a disorder, characterized by a triad of gait disturbance, cognitive impairment, and urinary incontinence. The primary treatment for iNPH is the surgical implantation of a cerebrospinal fluid shunt, which may be prone to malfunctions. 12 The cognitive impairment developed in iNPH can affect patients’ ability to accurately assess their symptoms, emphasizing the need for objective assessment methods. 13 Routine annual follow-up visits are often insufficient, leading to delays in necessary interventions. 14 Because the progression of motor symptoms can be effectively monitored in a home setting,4,12 this patient group was identified as potentially benefiting from RM. This study explores RM acceptance by iNPH patients. We also acknowledge the role of caregivers in facilitating RM adoption and managing care for patients with neurological conditions.4,11
Reflecting on this background, this study focuses on six sociodemographic variables (age, gender, education, living arrangement, place of residence, and caregiver presence during clinic visits) to assess their influence on RM acceptance in the pre-implementation phase among elderly patients. The research question of the study is: What are the associations between the selected sociodemographic factors and the acceptance of RM among iNPH patients in the pre-implementation phase?
Methods
Study Setting and Participants
This pilot study was based on a quantitative survey conducted at the neurosurgery clinic of Kuopio University Hospital (KUH) in Finland between September 2022 and January 2023. The study was approved by the Research Ethics Board of the North Savo Hospital District, where the KUH is located. The survey targeted patients attending the clinic for iNPH diagnosis or follow-up.
We randomly selected 30 patients. During the visit to the clinic, they were invited to participate in the survey-based study, together with 19 caregivers accompanying them. All agreed to participate and provided their informed consent. The purpose of the survey was explained to the patients and caregivers by a healthcare professional. To accommodate the patients’ cognitive needs and ensure comprehension of the survey questions in the study, it was conducted by a healthcare professional, who presented all questions orally to the patients and their caregivers.
Cognitive Assessment and Professional Evaluation
During the clinic visits, all patients except one (due to a lack of time) underwent a Mini-Mental State Examination (MMSE) to assess cognitive function. As a standard dementia screening tool, the MMSE evaluates orientation, memory, attention, language, and visuospatial skills on a scale from 0 to 30, where higher scores indicate better cognitive performance. 15 The 29 tested patients showed questionable, mild or moderate dementia symptoms (Table 1), and none were excluded for severe dementia (scores below 11). While the MMSE did not determine study eligibility, a neurosurgery professional evaluated each participant’s orientation to ensure their understanding of the study and interview questions.
Patients Mini-Mental State Examination (MMSE) Scores.
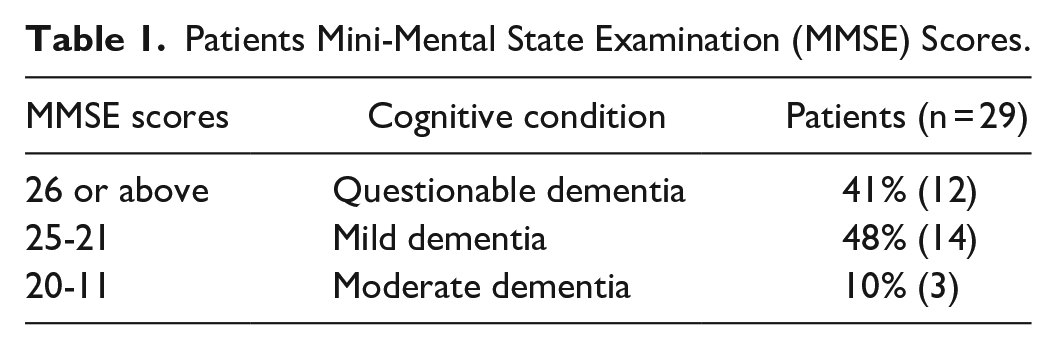
Sociodemographic Section of the Survey
In this study, we focused on the sociodemographic data of the broader survey. The data used were collected in categorical scales regarding patients’ age, gender, education, living arrangement, place of residence, and caregiver presence during the clinic visit. The acceptance of RM was surveyed using a binary (Yes/No) question.
Statistical Analysis
Statistical analyses were conducted using the Statistical Package for the Social Sciences (SPSS) version 29.0. Descriptive statistics (mean and range) were calculated for the age variable. To assess patients’ acceptance of RM, chi-square tests were employed to examine associations between patients’ sociodemographic information (age, gender, education, place of residence, living arrangement, and caregiver presence during clinic visits) as independent variables, and acceptance of RM as the dependent variable. p-Values ≤0.05 were considered statistically significant.
Because of the small sample size, we grouped two independent variables (education and place of residence) into broader categories. For education, the collapsed variable “pre-higher education” comprised of basic, middle, high school and vocational education, and “higher education” comprised of university and college degrees. For place of residence, the collapsed variable “urban area” included city/municipal center and suburbs, and “non-urban area” included rural and sparsely populated regions.
Results
Sociodemographic Information
Table 2 provides the patients’ sociodemographic information. Thirty patients (mean age 78, age range 64-87) participated in the study. Fifty-seven percent (17 out of 30) of the patients were 78 years old or younger, while 43% (13 out of 30) were older than 78 years. Among them, 67% (20 out of 30) were male and 33% (10 out of 30) were female. Regarding education, 60% (18 out of 30) of patients had completed pre-higher education, while 40% (12 out of 30) had attained higher education. Regarding place of residence, 77% (23 out of 30) lived in urban areas, while 23% (7 out of 30) resided in non-urban areas. Additionally, 53% (16 out of 30) lived with a family caregiver, and 47% (14 out of 30) lived alone. Sixty-three percent (19 out of 30) of the patients were accompanied by a caregiver during their clinic visit, while 37% (11 out of 30) attended the visit alone.
Sociodemographic Information of the Patients.

Acceptance of RM at Home
Of all patients, 80% (24 out of 30) expressed their acceptance of RM at home, while 20% (6 out of 30) did not accept RM. Also, 95% of the accompanying caregivers (18 out of 19) expressed their acceptance of the patient adopting RM.
The Influence of Sociodemographic Factors Contributing to the Acceptance of RM
The results of the chi-square tests in Table 3 showed varying levels of association between the chosen sociodemographic factors and RM acceptance. A statistically significant association was found between living arrangement and RM acceptance (p = .007, p ≤ .05), with a strong effect (Cramér’s V = 0.636). The association between education and RM acceptance was also statistically significant (p = .025, p ≤ .05), with a moderate effect (Cramér’s V = 0.408). The presence of a caregiver during the clinic visit showed a potential trend toward influencing RM acceptance, but this relationship was not statistically significant (p = .088, p > 0.05) with a small effect (Cramér’s V = 0.118). This can be caused by the small sample size, which limits detecting potential associations despite small effect sizes (Cramér’s V). Place of residence was not associated with RM acceptance (p = .517, p > .05), despite a small effect size (Cramér’s V = 0.173). Age did not show a statistically significant relationship with RM acceptance (p = .713, p > .05), and the effect size was negligible (Cramér’s V = 0.067). Similarly, there was no association between gender and RM acceptance (p = 1.000, Cramér’s V = 0.000). Table 3 provides the results of the chi-square test, including the p-value, Cramér’s V, and confidence intervals (CIs), and odd ratios (ORs) for each variable.
The Cross-Tabulation of Patient’s Sociodemographic Factors and Remote Monitoring (RM) Acceptance.

Note. Statistical significance was determined at a threshold of p ≤ .05. Cramér’s V = 0.10 to 0.30: Small or weak effect; Cramér’s V = 0.30 to 0.50: Moderate effect; Cramér’s V ≥ 0.50: Strong effect. OR = odds ratios; CIs = confidence intervals.
Living Arrangement
Fifty-eight percent (14 out of 24) of patients who reported living with a family caregiver accepted RM, while 67% (4 out of 6) of patients who rejected RM were living alone. The results of the chi-square test in Table 3 showed that cohabiting was significantly associated with higher RM acceptance (p = .007, p ≤ .05).
Education
Of the 24 patients who accepted RM, 50% (12 out of 24) had higher education. In contrast, all 6 patients (100%) who refused to participate in RM had not completed higher education. The chi-square test results in Table 3 showed a statistically significant association between education and RM acceptance (p = .025, p ≤ .05). Patients with higher education were more likely to accept RM compared to those with lower education.
Caregiver Presence During Clinic Visit
The caregiver presence during clinic visits influenced RM acceptance. Seventy-one percent (17 out of 24) of the patients who accepted RM were accompanied by a caregiver at the clinic, while 67% of those who rejected RM (4 out of 6) were not accompanied by a caregiver. The results of the chi-square test in Table 3 indicate a potential trend toward an association between caregiver presence and RM acceptance, though it is not statistically significant at the conventional 0.05 level (p = .088, p > .05). However, the effect size (Cramér’s V = 0.118) suggests a small relationship, which could be further explored with a larger sample size.
Place of Residence
Seventy-nine percent (19 out of 24) of the patients who accepted RM and 67% (4 out of 6) of those who rejected RM lived in urban areas. The results of the chi-square test in Table 3 showed no significant association between place of residence and RM acceptance (p = .517, p > .05). The small effect size (Cramér’s V = 0.173) indicates that further research with a larger, more diverse sample is needed to explore potential trends.
Age
The majority of patients who accepted RM (58%, 14 out of 24) were 78 years old or younger. Additionally, 50% of the patients (3 out of 6) who rejected RM were over 78 years old. The results of the chi-square test in Table 3 revealed no statistically significant difference in patient age and RM acceptance (p = .713, p > .05). The effect size was negligible (Cramér’s V = 0.067), indicating that age is unlikely to influence RM acceptance. A study with a larger sample size is required to further explore and validate these findings.
Gender
Of the 24 patients who accepted RM, 33% (8 out of 24) were female, and 67% (16 out of 24) were male. The results of the chi-square test in Table 3 showed no significant association between gender and acceptance of RM (p = 1.000, p > .05). Table 3 shows the cross-tabulation of gender with respect to RM acceptance or rejection. However, the small sample size and uneven gender distribution limit the generalizability of these findings. A study with a larger sample size and a well-balanced gender representation is needed to validate these results.
Discussion
The study showed that 80% of patients (24 out of 30) expressed acceptance of RM at home prior to implementation. Furthermore, 95% of the accompanying caregivers (18 out of 19) expressed their acceptance of the patient adopting RM. These findings are consistent with previous research reporting high levels of RM acceptance among patients with neurological conditions and their family caregivers.2,4 Our findings indicate that living arrangement and education showed statistically significant association with RM acceptance among elderly neurological iNPH patients. Caregiver presence during clinic visits also had a positive influence. These findings support other research emphasizing caregivers’ vital role in decision-making and overcoming technological barriers for patients. Additionally, the neurological condition of our patient population may contribute to this outcome, as cognitive and motor impairments are linked to greater support for adopting technology. 4 Variations in our findings with other studies likely reflect differences in patient populations, healthcare systems, cultural contexts, and study design. Also, using a small, geographically localized sample in research limits generalizability and increases the risk of sample bias, meaning the findings may not reflect broader populations. This can skew results and reduce statistical power, hindering the ability to detect accurate effects.
Living Arrangement
Our findings indicate that cohabiting with a family caregiver positively impacts patients’ willingness to accept RM at home. This is consistent with previous research highlighting the significant role caregivers play in supporting neurological patients with eHealth adoption.4,11 The beneficial effects of caregiver support of telemedicine homecare adoption among elderly patients with chronic conditions have been noted. These studies document how caregivers provide emotional and technical support, boosting patients’ confidence in using RM tools.10,16,17
Education
We found that higher education was positively associated with RM acceptance, consistent with studies reporting that higher education levels positively influence receptiveness to digital solutions.10,18,19 Individuals with higher education are better equipped to understand and navigate technology, providing them with better digital literacy and making them more likely to support RM. 20
Caregiver Presence During the Patient’s Clinic Visit
The presence of caregivers during clinic visits was associated with RM acceptance. While previous findings confirmed that caregivers play a crucial role in providing emotional support and alleviating concerns about technology use after implementation, 19 our study demonstrates that caregiver’s presence during the clinic visit positively influences patient’s willingness accept RM in the pre-adoption phase. Our findings underscore the pivotal role of caregiver involvement in facilitating RM acceptance prior to RM use.
Place of Residence
Contrary to previous studies that found rural residency to hinder technology acceptance due to limited access to digital devices and unreliable internet connectivity, 4 our results showed no significant impact of place of residence on RM acceptance.
Age
Unlike previous studies, 10 which found that age influences technology acceptance, we observed no clear correlation, although trends were noted. RM acceptance peaked among patients aged ≤78 years and then declined after age 78. This aligns with research indicating varied technology acceptance among different elderly age groups. 21
Gender
Contrary to previous findings that observed gender differences in technology acceptance,7,8 our data showed no significant gender impact on RM acceptance. This is consistent with studies reporting no gender differences in acceptance of healthcare technology. 22
Limitations and Future Research
This study’s limitations include the reliability of patient responses, potentially affected by factors like cognition, health status, and prior experience with technology. The small sample size, uneven gender distribution and limited geographical scope restricted the generalizability of our findings to elderly neurological patients. Future studies should use larger, gender-balanced samples that have broader diversity (e.g., geographic, place of residence) to improve generalizability. Improved gender-balance clarifies gender-specific acceptance patterns and reduces biases in RM research. Including participants from diverse locations enhances understanding of RM acceptance across different contexts, ensuring wider applicability of findings. Future research should also examine additional factors influencing RM acceptance in the pre-adoption phase, such as technological, cultural, and contextual variables. Previous studies indicate that elderly patients’ rejection of eHealth solutions often stems from concerns about usability, lack of knowledge, and apprehension about learning new technologies, which are prevalent among this demographic. 23
The role of caregivers in the pre-adoption phase of RM in the home environment should be studied in future research to better understand its influence on RM acceptance among elderly neurological patients. The inclusion of family caregivers in RM studies for these patients has been highlighted in several studies, underscoring their crucial role in supporting the use of RM devices.4,24,25 RM solutions can provide significant benefits for both patients and caregivers, enabling better management of neurological conditions in the home environment. While many studies explored the role of family caregivers in facilitating RM acceptance during or after implementation, primarily through providing emotional and technical support, our study demonstrates that caregiver presence during clinic visit and cohabiting with a caregiver positively influences patient acceptance of RM in the pre-implementation phase.
Conclusions
We examined RM acceptance during the pre-adoption phase among elderly neurological patients, showing acceptability linked to cohabiting with caregivers, higher education of the patient and caregiver’s presence during clinic visit. Our practical recommendations include implementing educational initiatives that are tailored to different educational backgrounds of elderly neurological patients. Health policies should ensure that caregiver support is integrated into RM programs by training caregivers alongside patients, providing them with resources to assist with technology management, and recognizing their role in RM with appropriate support and resourcing. For technology developers, collaboration with patient advocacy groups should be encouraged to ensure that RM solutions are designed with input from both patient and caregiver perspectives. This collaboration would help tailor RM solutions to the needs of specific patient populations, such as elderly neurological patients.
Footnotes
Acknowledgements
The authors thank Tiina Laaksonen for performing the MMSE to the patients as part of the study.
Data Availability Statement
The data supporting the findings of this study are not publicly available due to privacy restrictions to protect the confidentiality of the participants.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was conducted in cooperation with the Doctoral Programme in Neuro-Innovation (The Marie Skłodowska-Curie Actions co-fund number 101034307) at the University of Eastern Finland Business School, Kuopio University Hospital VTR fund [grant number 5252614], the Research Council of Finland [grant numbers 339767 and 348202], the Sigrid Juselius Foundation (no specified grant number), and the Strategic Neuroscience Funding of the University of Eastern Finland.
Ethical Considerations
This study was approved by the Research Ethics Board of the North Savo Hospital District, Finland (Approval number: 276/2016 (5/2008)), with approval updated on June 22, 2021. The study adhered to the ethical principles outlined in the Declaration of Helsinki and complied with the EU General Data Protection Regulation (GDPR).
Consent to Participate
Informed consent was obtained from all patients and caregivers participating in the study prior to their participation, including consent to participate and consent to publication.
Consent for Publication
Informed consent was obtained from all patients and caregivers participating in the study for their participation, including prior consent to participate and consent to publication.
