Abstract
The Desired Sensation Level (DSL) Method was originally developed in the early 1980s to provide clinicians with a systematic, science-based approach to pediatric hearing instrument fitting that ensures audibility of amplified speech by accounting for factors that are uniquely associated with the provision of amplification to infants and young children who have hearing loss. This review identifies and describes several of the primary factors that have been considered in the development of the DSL Method. Specifically, the issues discussed relate to: (1) the definition and measurement of relevant acoustic, electroacoustic and audiometric variables; (2) how the external ear acoustics of infants and young children are accounted for in the DSL Method for both audiometric assessment and in the fitting of amplification; and (3) how the DSL Method has evolved concurrently with developments in hearing instrument and electroacoustic measurement technologies. Finally, current issues in the field are identified that have motivated the development of version 5.0 of the DSL Method for hearing instrument fitting.
Introduction
It started with the measles. In the early 1970s, Richard Seewald and Patricia Stelmachowicz were young clinical audiologists working at the Children's Hospital in Halifax, Nova Scotia, Canada. A rubella outbreak in 1973–1974 rapidly created an unexpected caseload of more than 30 infants with hearing loss as well as additional handicapping conditions. At the time, Seewald and Stelmachowicz did not have the resources that are used in audiology clinics today, such as electrophysiologic test systems, probe microphone systems, computers, programmable hearing aids, or prescriptive algorithms to help them to fit infants with appropriate amplification. Also, they did not have universal newborn hearing screening.
Consequently, fitting hearing instruments to babies was very rare in those days. They realized that the behavioral comparative procedures (e.g., aided sound field threshold testing) that were used for fitting hearing instruments in older children and adults were not useful when working with young infants. With a great deal of uncertainty and with very little science, they and their colleagues did their best to provide these babies with adequate hearing instrument fittings. Eventually, Seewald and Stelmachowicz pursued doctoral studies and have dedicated their careers, often collaboratively, to developing systematic, science-based procedures for fitting amplification to infants and young children.
In 1976, Seewald enrolled at the University of Connecticut to work with Prof. Mark Ross, and together they began the development of the Desired Sensation Level (DSL) Method for pediatric hearing instrument fitting. Work on the DSL Method evolved from innovative approaches to pediatric hearing instrument fitting that had emerged in the 1970s and was based on the premise that the process of hearing instrument fitting for infants and children differs in several important ways relative to fitting amplification in adults (Gengel et al., 1971; Erber, 1973; Byrne and Fifield, 1974; Ross, 1975). The DSL Method was originally developed to provide clinicians with a systematic, science-based approach to pediatric hearing instrument fitting that ensures audibility of amplified speech by accounting for factors that are uniquely associated with the provision of amplification to infants and young children who have hearing loss (Seewald et al., 1985; Ross and Seewald, 1988; Seewald and Ross, 1988). This general objective is still in place today as work continues on the development of the DSL Method.
The Linear Gain Era
As explained within the initial publications outlining the development of the DSL Method, the electroacoustic fitting goal was to define frequency/gain characteristics that would deliver to a child amplified speech that was audible, comfortable, and undistorted across the broadest relevant frequency range possible (Seewald et al., 1985; Seewald et al., 1987; Ross and Seewald, 1988; Seewald and Ross, 1988). The early versions of the DSL Method used tables of values that specified target sensation levels for amplified speech as a function of frequency and hearing level. These desired sensation levels, or DSLs, were based on data describing the speech sensation levels that were associated with comfortable listening levels across hearing levels (e.g., Kamm et al., 1978; Pascoe, 1978) and ceiling speech recognition performance in children with sensory hearing impairment (e.g., Gengel et al., 1971; Erber and Witt, 1977; Macrae, 1986; Smith and Boothroyd, 1989).
The relationship between hearing threshold level and the levels of amplified speech as prescribed by the DSL Method v3.1, for the 1000 Hz region, can be seen in Figure 1. It should be noted that all variables shown in this figure are plotted in dB SPL ear canal level as a function of hearing level in dB HL. In this way, the important inter-relationships among the variables shown (i.e., hearing threshold, target levels for amplified speech and target levels for hearing instrument output limiting) can be studied. In addition, these theoretical target values could be used to generate the desired frequency/gain prescription. For example, if the child had a hearing threshold of 50 dB HL at 1000 Hz, the DSL Method v3.1 would prescribe an ear canal hearing instrument output of 85 dB SPL for an average conversation speech input within the 1000-Hz frequency region. The required gain was then simply calculated by subtracting the assumed speech input from the target output. This calculation was repeated at each frequency at which audiometric threshold data were available.
Because young children's loudness discomfort levels (LDLs) are not typically measured, targets for hearing instrument output limiting were proposed that also varied as a function of frequency and hearing level (Seewald, 1991; Seewald et al., 1993). These output-limiting levels were chosen to allow headroom for the peaks of conversational speech, and as much as possible, to avoid peak clipping distortion. The relationship between the recommended output-limiting levels and hearing threshold from the DSL Method v3.1 is also shown in Figure 1. These prescribed real-ear output-limiting criteria are approximately one standard deviation below the mean LDL data reported by Pascoe (1978) and agree closely with the maximum output target values recommended by other hearing instrument prescriptive procedures (e.g., Dillon and Storey, 1998; Storey et al., 1998).
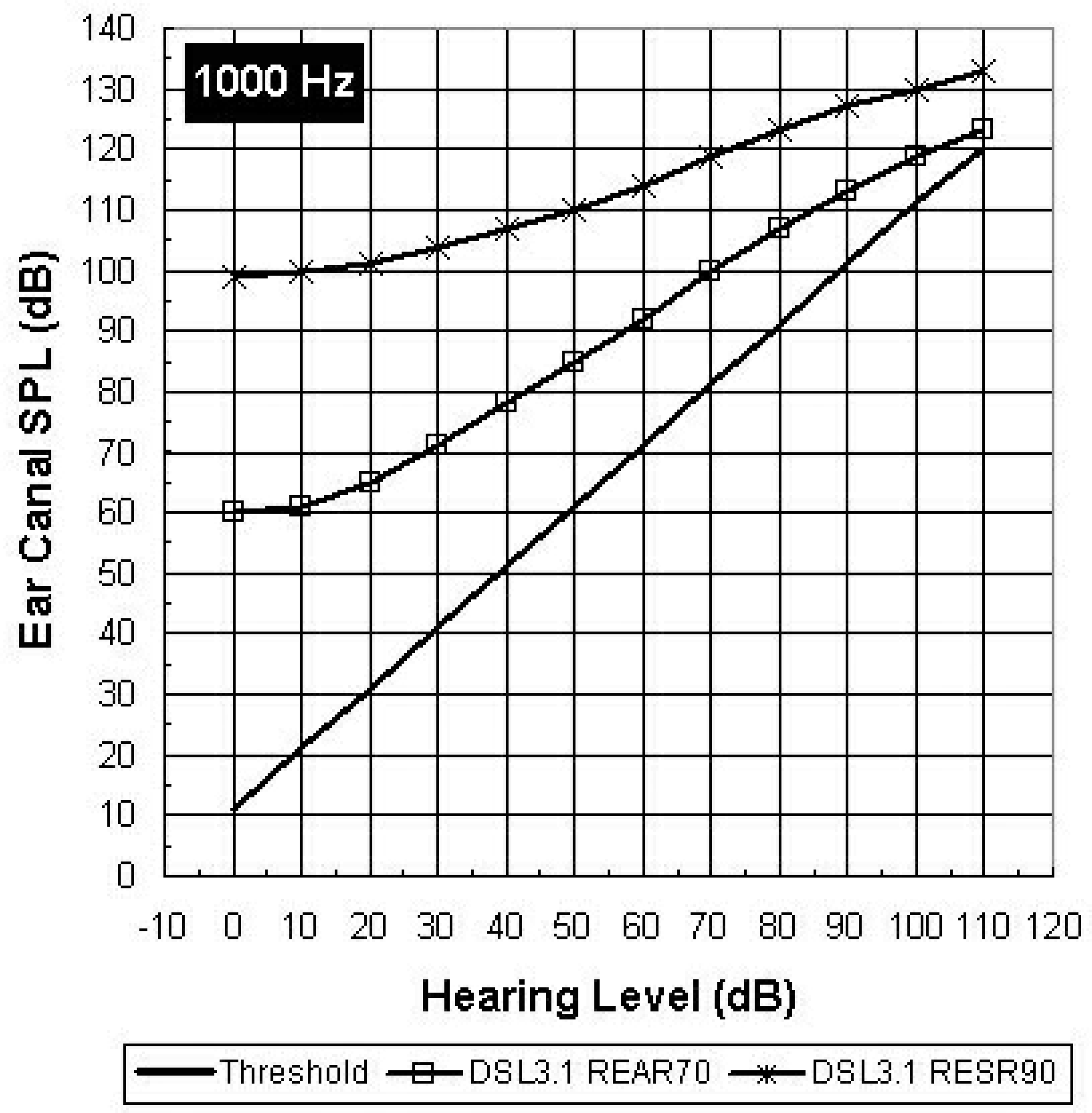
Threshold, target values for amplified speech and target values for hearing instrument output-limiting, in dB SPL ear canal level, as a function of the measured hearing level in dB HL at 1000 Hz. The values shown in this figure were applied in the DSL Method (v3.1) for hearing threshold data collected at 1000 Hz.
The linear version of the DSL Method was first distributed as a software system in 1991 (Seewald et al., 1991), making it the first published computer-assisted implementation for hearing-instrument fitting for young children. DSL v3.0 offered several unique pediatric features:
First, it accounted for acoustic variables in the fitting of amplification that are known to vary as a function of age. Two such factors are the real-ear unaided gain (REUG) and real-ear-to-coupler difference (RECD). For children younger than 37 months old, the default REUG values applied in the DSL Method were derived from data reported by Kruger (1987). In addition, for all infants and children younger than 60 months old, the default RECD values were derived from data reported by Feigin et al (1989). Current versions of the DSL Method continue to use the Kruger data to predict the REUG by age, but the RECD data have undergone some revision, as will be described by Bagatto et al in Chapter Two of this edition.
Second, the DSL Method converted audiometric and electroacoustic variables to the sound pressure level (SPL) scale in the ear canal as a function of frequency. This ear canal SPL approach had two advantages: it brought the audiometric data and hearing instrument performance data onto the same graphical display, and it removed age-related variance in ear canal acoustics from the calculations. The strategy of using a common display format for both audiometric and electroacoustic data was originally proposed by audiologists at the Central Institute for the Deaf, who used a carefully calibrated sound field for the same purpose (Erber, 1973; Skinner, 1988). With the advent of clinical probe microphone systems, however, the DSL Method modified the CID approach to create the now well-recognized SPLogram display. The advantage of the SPLogram approach is that it allows a close examination and understanding of the important inter-relationships among relevant auditory and amplification characteristics, facilitating the aural habilitation /rehabilitation process. Figures 2 through 4 illustrate how these graphic displays were used in v3.1 of the DSL Method.
Figure 2 presents an unaided SPLogram from the early linear versions of the DSL Method (versions up to and including v3.1). This type of display was recommended for use in counselling caregivers regarding candidacy for the use of amplification. Audiometric data were collected using traditional audiometric transducers (i.e., insert phones, TDH headphones, or sound field loudspeakers) in dB HL as a function of frequency. The audiologist would enter the audiometric thresholds, the child's age, and the results of any probe microphone measurements that had been made. The computer program would retrieve and apply the appropriate measured or age-predicted average transform values (see Bagatto et al., Chapter Two in this volume), and calculate the predicted ear canal SPL threshold values. These thresholds were then compared against the unaided levels of speech that had also been converted to ear canal SPL levels using age-appropriate open ear resonances. The unaided speech spectrum was displayed as the 30 dB dynamic range of speech (i.e., peaks and valleys), with the long-term average levels also indicated. The clinician could discuss the displayed audibility and inaudibility of speech with caregivers before fitting the hearing instrument and introduce them to the goals of the amplification fitting process. It can be seen in Figure 2 that, in the unaided condition, the peak levels of speech are audible from 250 through 1000 Hz for speech, with an overall level of 70 dB SPL.
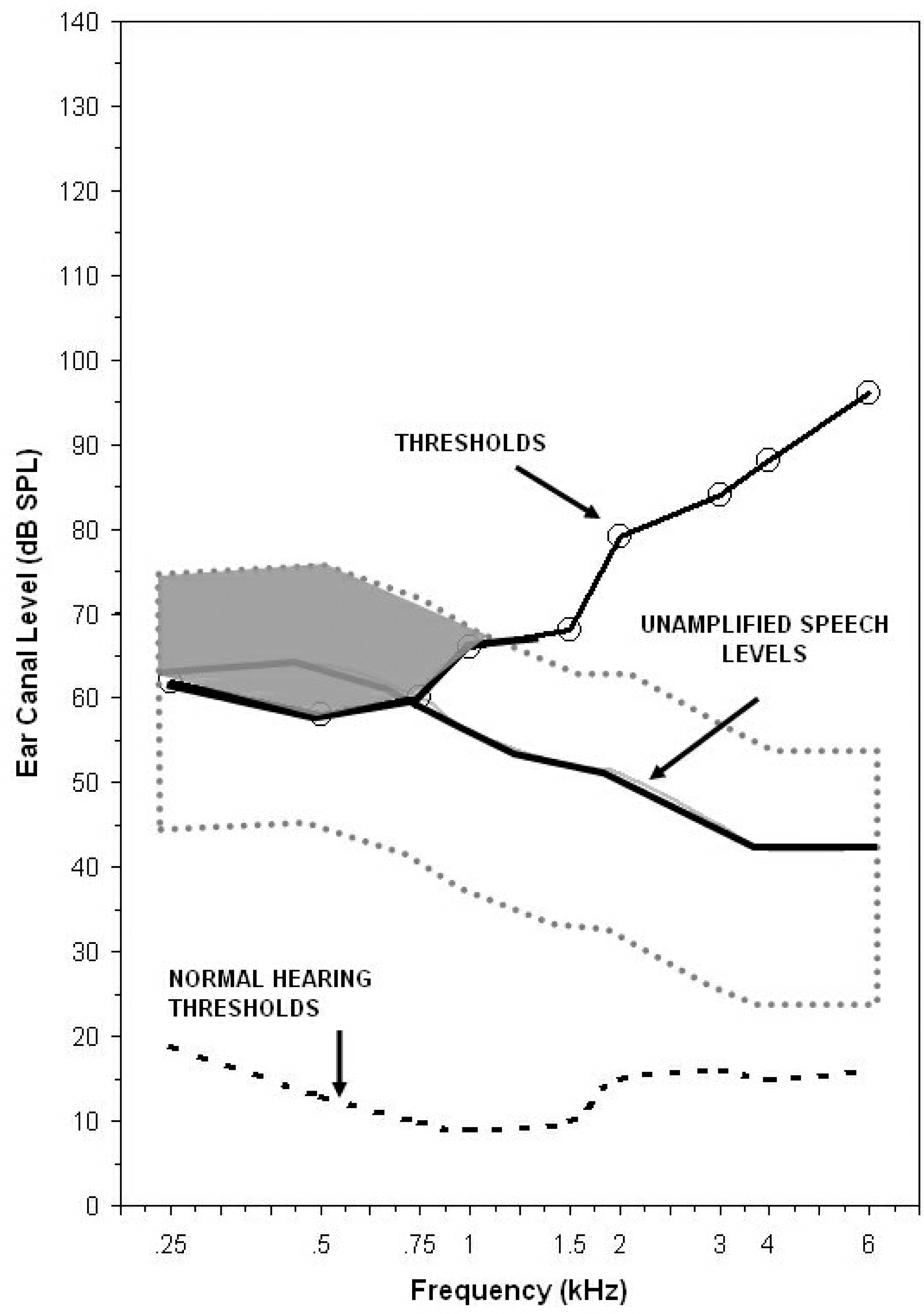
Pure tone air conduction thresholds plotted in dB SPL (ear canal level) as a function of frequency. All other variables, including average normal hearing sensitivity and the average unamplified long-term average speech spectrum level with its associated range of approximately 30 dB, have also been plotted. The portion of the unamplified speech spectrum that would be audible for this child has been shaded.
When it was decided that the child would be fitted with amplification, the DSL prescriptive algorithm would predict a set of frequency-specific target values for hearing instrument output-limiting in addition to target levels for amplified average conversational speech. These targets assumed an input speech spectrum with an overall RMS level of 70 dB SPL. Figure 3 presents the DSL targets for the amplified long-term average speech spectrum and the real-ear saturation response from v3.1 of the DSL Method. These values would be used to select the frequency-gain and output-limiting characteristics of the hearing instrument to be fitted. Further, these ear canal SPL target values were then converted to the 2 cc coupler equivalent to allow coupler-based fitting, which is often more feasible with the infant and toddler population.

The unaided SPLogram with target criteria for amplified long-term average speech (real-ear aided response [REAR]) and for real-ear saturation response (RESR) are plotted as a function of frequency (in Hz).
Figure 4 presents the results of electroacoustic selection and real-ear electroacoustic verification in the SPLogram format. Results show good agreement between the measured performance characteristics and the electroacoustic performance criteria specified by the DSL Method. From these electroacoustic findings, it could be predicted that an infant or young child fitted with these electroacoustic characteristics would derive significant benefit from amplification for auditory learning. Specifically, advocates of the habilitative audibility approach recommend providing audibility of the full bandwidth and envelope of conversation-level speech so that phonemic patterns can be learned (e.g., Ling, 1989; Scollie, 2005). Over time, of course, the validity of this prediction would require systematic assessment.
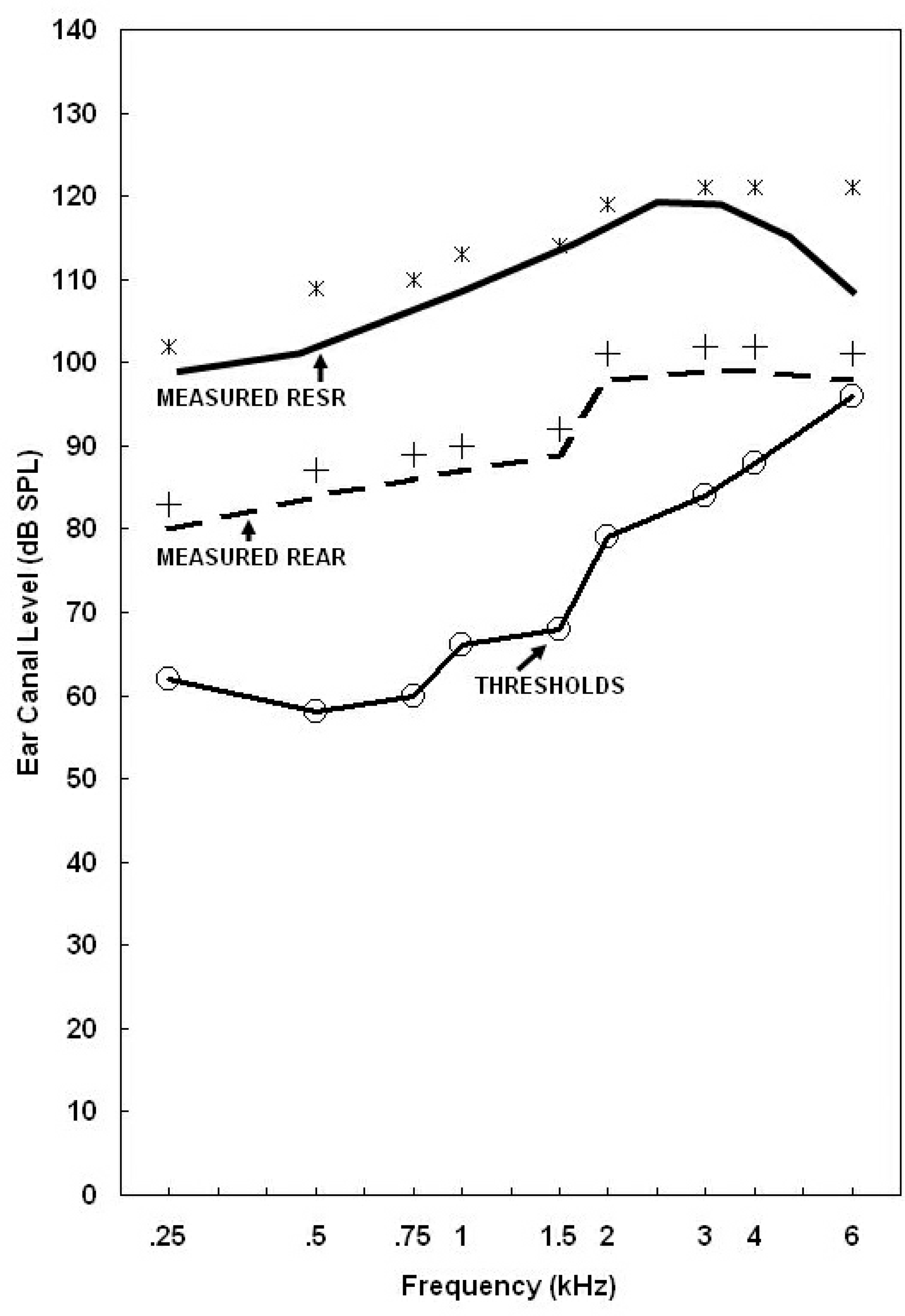
The results of real-ear aided response (REAR) and real-ear saturation response (RESR) verification measures plotted in ear canal SPL as a function of frequency (Hz). The REAR and RESR target criteria and thresholds are also plotted for comparison purposes.
The Role of Clinical Protocols
During the early design and development stages of the DSL Method, attention was focused on the clinical problem of electroacoustic selection. However, it soon became clear that electroacoustic selection could not be isolated from the manner in which audiometric assessment data were collected or from the verification procedures that would be applied at the time of fitting. Therefore, the DSL electroacoustic prescriptive strategy became embedded within a set of recommended clinical procedures for application in pediatric audiology settings.
Over time, the DSL Method has come to reflect the philosophy that DSL is more than just an algorithm for electroacoustic selection, but rather a method consisting of sequential stages in a well-integrated pediatric hearing instrument fitting process. This process includes audiometric assessment, hearing instrument selection, and verification and evaluation of aided auditory performance (Seewald, 1995; Seewald et al., 1995). Over the years, our research program on the development of the DSL algorithm has therefore been coupled with the research and development of clinical procedures and protocols to assist with appropriate pediatric assessment and verification procedures that can be implemented in routine clinical practice (Seewald et al., 1993; Moodie et al., 1994; Seewald, 1995; Bagatto, 2001).
The Nonlinear Era
In 1995, Cornelisse, Seewald and Jamieson described an electroacoustic fitting algorithm called the DSL input/output formula (DSL[i/o]). This device-independent enhancement of the DSL Method provided prescriptive targets for the fitting of wide-dynamic-range compression (WDRC) hearing aids. The DSL[i/o] algorithm applied loudness data and a curvilinear fit to map a wide range of input levels to target hearing instrument output levels across frequencies. It has been used in DSL software systems for v4.0 and v4.1 and in most hearing instrument and real-ear system manufacturers software implementations.
The DSL v3.1 linear gain and DSL[i/o] curvilinear compression prescriptions are shown in Figure 5, for a wide range of inputs across frequencies. The output level is plotted as a function of frequency for input levels ranging from 20 to 90 dB SPL in sound field, in 10-dB steps. The thresholds for the individual with hearing impairment (THhi) and corresponding upper limits of comfort (ULhi) are also plotted. It can be seen in this figure that when the linear gain algorithm (DSL v3.1) is applied, less of the input dynamic range fits into the residual auditory area as the dynamic range of hearing decreases. However, the entire input dynamic range fits into the auditory area when the DSL v4.1 curvilinear [i/o] compression mapping is applied (Cornelisse et al., 1995). The DSL[i/o] algorithm has been applied in several laboratory and clinical trials, as summarized by Scollie et al. in Chapter Three of this issue.

The DSL Method prescribed output for (
Comparisons Among Hearing Instrument Prescriptive Formulas
Two other “generic” prescriptive approaches currently available for use in hearing instrument fitting are the National Acoustic Laboratories (NAL) prescription (Byrne et al., 2001) and the CAMFIT procedure (Moore et al., 1999). Target-to-target comparison studies among algorithms have been published (e.g., Keidser et al., 2003).
One limitation associated with such target-to-target comparisons is that most have been done using a real-ear insertion gain (REIG) reference, which is not recommended for use with children. The REIG format typically uses average adult real-ear unaided gain (REUG) values when deriving target criteria, which is inappropriate for use with infants and young children.
A second limitation with published comparisons is the modification of the original target from the prescriptive algorithm before performing the target-to-target comparisons. For example, one strategy for target modification is the “normalization” of target responses at 1000 Hz (e.g., Keidser et al., 2003). The “normalization” strategy mathematically increases or decreases each target response so that all responses are forced to meet at 1000 Hz regardless of the actual prescribed target value at that frequency. This approach may not provide accurate estimates of inter-prescription agreement, because the prescriptions may differ markedly at 1000 Hz and therefore may not accurately reflect how infants or young children will wear their hearing instruments at a fixed volume-control setting.
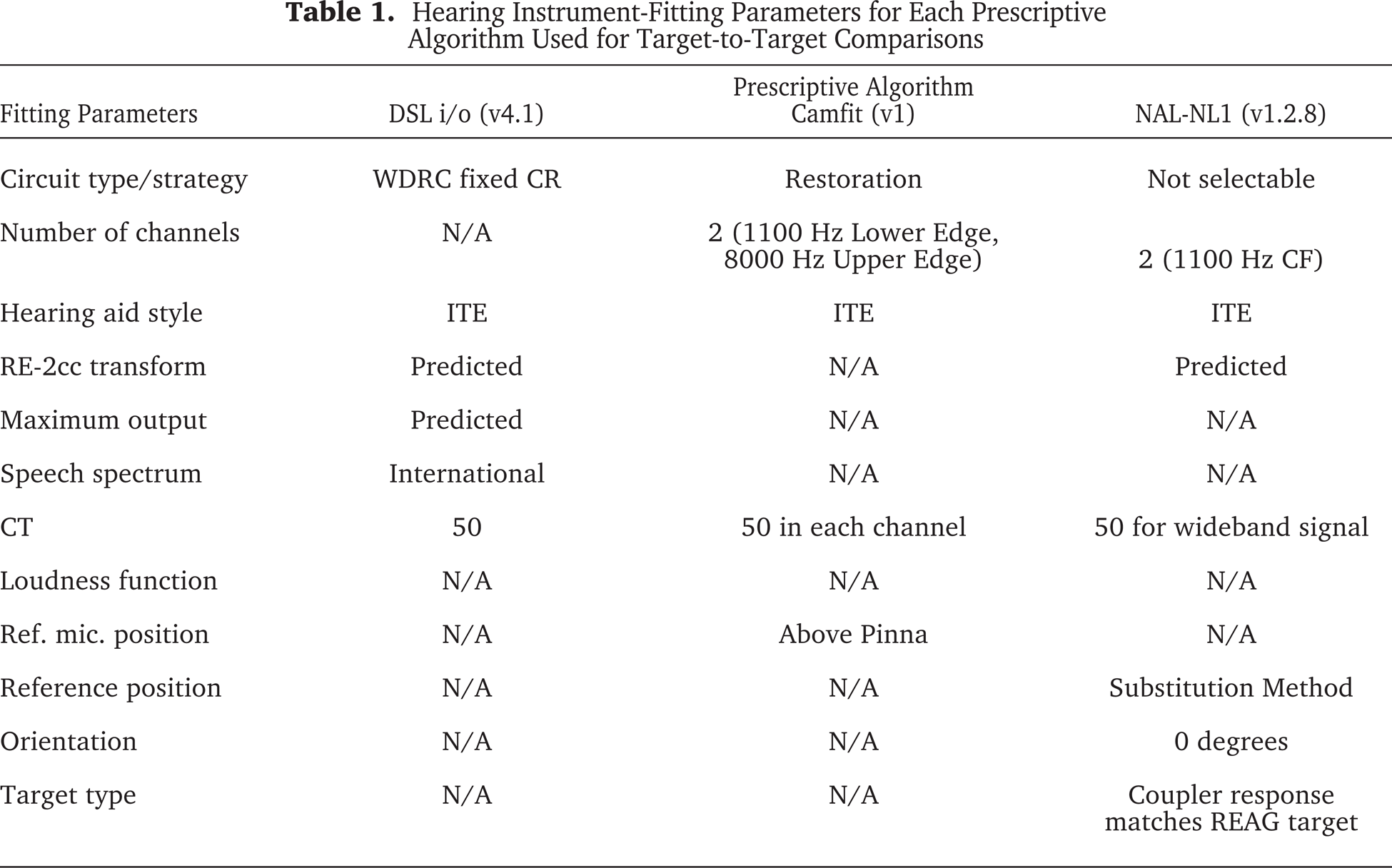
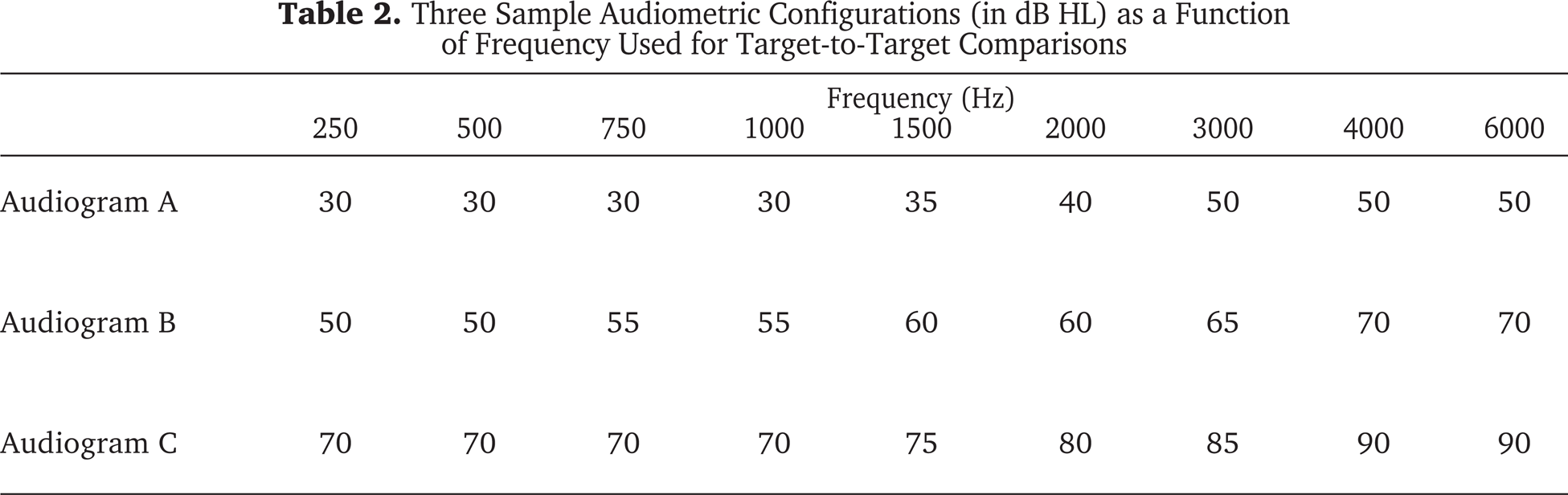
To quantify the true differences among contemporary generic algorithms for the fitting of WDRC instruments, NAL-NL1 (2 channel), DSL[i/o] fixed ratio and CAMFIT Restoration target-to-target comparisons were performed in our laboratory using NL1 v1.2.8, DSL v4.1a, and CAMFIT v1 computer-assisted implementations. Sixty-one theoretical audiogram configurations were generated for threshold values from 30 to 90 dB HL for 250 to 6000 Hz and included configurations covering a variety of slope cut-off frequencies. The age of the theoretical subject was adult, the transducer for threshold measurement procedures was set for TDH headphone, and any HL-to-SPL transform values were set to use age-appropriate average adult values. For comparative purposes, hearing instrument-fitting parameters for each prescriptive algorithm were matched as closely as possible (see Table 1). Real-ear aided gain (REAG) targets were calculated for 50, 65, and 80 dB pure-tone input levels. Table 2 shows three sample audiometric configurations (from the possible 61) used to generate the data for these target-to-target comparisons. Measurement results for the three audiometric configurations are shown in Figure 6, panels a, b, and c. Specifically, the prescribed NAL-NL1, DSL[i/o] and CAMFIT REAG targets for 50, 65, and 80 dB SPL inputs are shown as a function of frequency for the three audiometric configurations.
Hearing Instrument-Fitting Parameters for Each Prescriptive Algorithm Used for Target-to-Target Comparisons
Three Sample Audiometric Configurations (in dB HL) as a Function of Frequency Used for Target-to-Target Comparisons

Measured REAG as a function of frequency for three audiometric configurations derived using the CAMFIT Restoration, DSL v4.1 fixed and NAL-NL1 software.
General conclusions that can be made from this target-to-target comparison work are:
for most of the audiometric configurations, the real-ear aided gain targets were similar in shape for the three prescriptive algorithms;
in contrast to popular assumptions, the DSL[i/o] algorithm did not always generate the maximum REAG target for a given audiometric profile;
consistent with the habilitative audibility approach (Ling, 1989; Scollie, 2005), the DSL algorithm generated the maximum REAG target the greatest percentage of time for the high frequencies; and finally,
consistent with the effective audibility approach (Ching, Dillon, Katsch, and Byrne, 2001), the NAL-NL1 prescriptive algorithm did not generate targets for all frequencies, especially for more severe-to-profound hearing losses.
Is It Time for a New Version of the DSL Method?
Several factors have made our laboratory consider development of a new version of the DSL[i/o] algorithm along with several modifications and elaborations to the fitting method. First, newborn hearing screening programs are becoming more common worldwide (Hayes, 2002). Children with hearing loss are being identified at birth, and amplification is being provided to infants by 6 months of age in many locations throughout the world (Joint Committee on Infant Hearing, 2000; American Academy of Audiology, 2003).
In the context of early intervention, infants will wear their hearing instruments at settings determined by the clinicians for at least the first few years of life. This increases the importance of continued research and development on an objective, evidence-based procedure like the DSL Method for hearing instrument fitting for application with the infants and children.
Second, improvements in electrophysiologic testing procedures and advances in hearing instrument technology, including new digital signal-processing algorithms and multichannel/multistage technology and multimemory programs, make continued development both desirable and necessary. In addition, since the release of the computer-assisted implementation of DSL v4.1 in 1997, anecdotal reports from clinicians, research studies in our laboratory, and published studies indicated some modifications could be applied to the algorithm for more appropriate adult application (e.g., Moore et al., 2001).
Finally, although many hearing instrument manufacturers offer proprietary fitting algorithms in their fitting software, clinicians still desire access to generic prescriptive algorithms, especially for their pediatric clients. This is understandable in light of recently published studies showing that adult clients with similar hearing losses might be fitted with substantially different amplification characteristics depending on the hearing instrument proprietary fitting method chosen (Smeds and Leijon, 2001; Keidser et al., 2003; Killion, 2004). In the case of a 6-month-old infant who can neither manipulate the gain of the hearing instrument nor express concerns regarding the quality of their auditory perceptions through amplification, these research findings would seem to be clinically important.
Given all these considerations, work was initiated in the late 1990s on a new version of the DSL Method that includes the DSL multistage input/output algorithm, referred to as DSL m[i/o]. Although modifications to the DSL algorithm continue to be made into the 21st century, the goals and objectives expressed in the initial publications have not changed, nor has the belief that the hearing instrument fitting process is a series of well-integrated stages that include audiometric assessment, hearing instrument selection, and verification and evaluation of aided auditory performance.
This edition of Trends in Amplification describes the background research and development activities that have resulted in the most recent version: DSL m[i/o] v5.0 for hearing instrument fitting in both children and adults. This description is divided into two parts: (1) the clinical procedures that can be used to fit amplification in the pediatric population (Bagatto et al., Chapter Two in this issue); and (2) a revised prescriptive algorithm (Scollie et al., Chapter Three in this issue).
Footnotes
Acknowledgment
We gratefully acknowledge the assistance of Carol Van Evera, Jeff Crukley, Andreas Seelisch, and Julianne Tenhaaf in the preparation of this chapter.
