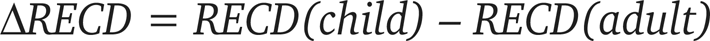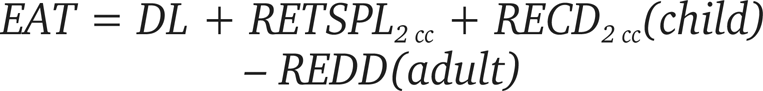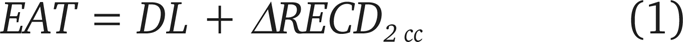Abstract
Considerable effort has recently been dedicated towards early detection of hearing loss in infants. The goal is to subsequently fit hearing aids to hearing-impaired infants so that they can develop speech and language as early and as well as possible. The responsibility of the audiologist is to provide the child with the optimal amplification from the hearing aid. This paper gives an overview of aspects involved in correctly assessing the hearing loss and optimally fitting and verifying the performance of the child's hearing aids. Special emphasis is directed towards differences that exist between children and adults, and how these differences can be considered during a pediatric fitting. We suggest a stringent terminology that can help avoid ambiguous terms and connotations in the child's domain which are derived from those that have become established in adult audiometry and hearing aid fittings. The quantification of hearing thresholds and their appropriate representation is reviewed. An appropriate threshold-based prescription of gain or output of the hearing aid is described. Issues of verification and the actual programming of the hearing aid are discussed.
Introduction
In recent years, much support has been given to the early detection and intervention of hearing impairment. The first years of life are critical in the development of speech and language abilities of young children. It is during this period that infants will construct meaningful representations from audible sequences of sounds. Furthermore, the young child will be required to accurately reproduce sequences of speech sounds in order to communicate with others (Wilcox and Tobin, 1974; Robinshaw, 1995; Downs and Yoshinaga-Itano, 1999). It has been widely documented that children with hearing loss do not acquire speech and language skills comparable to normal hearing peers (Davis et al., 1986; Kuhl and Meltzoff, 1988; Geers and Moog, 1989; Blamey et al., 2001). A delay in speech and language development typically occurs as a result of the inability of hearing-impaired children to perceive a sufficient proportion of speech signals in their auditory environments. However, evidence shows that hearing-impaired infants who are provided with proper amplification within the 6 first months of life are able to develop speech and language to a level similar to that of normal-hearing infants (Yoshinaga-Itano et al., 1998). Nevertheless, a delay in the onset of amplification that exceeds the time of 6 months of age could very likely lead to permanent delays in speech and language development.
Several challenges may cause a delay in diagnosis and intervention of the hearing-impaired child. The initial procedural difficulty with the diagnostic process is apparent. Until a certain age is reached, infants are unable to verbalize or communicate their perception of certain auditory events. This inability affects the ease in which hearing thresholds and hearing aid fitting results are collected. Fortunately, audiometric information can be collected objectively via electrophysiologic methodologies, where hearing thresholds can be estimated following waveform analysis of auditory evoked potentials (Stapells et al., 1995; Lins et al., 1996). These threshold estimations provide an inferred diagnosis of the integrity of the cochlea and central auditory structures. Thresholds can also be collected with traditional behavioral audiometry once the child is able to participate during these tasks. In the event of a positive diagnosis of hearing loss and subsequent prescription of hearing aids, these threshold estimations will also be the basis of the calculation of hearing aid gain and/or output characteristics.
An appropriate assessment and intervention with the hearing-impaired child is critical. An assessment and intervention that results in the provision of a hearing aid that does not deliver sufficient amplification may prevent certain elements of speech to be perceived and result in suboptimal development of speech and language skills. Furthermore, a delivery of an excessive amount of gain/output from a hearing aid could cause further hearing loss (Macrae, 1991, 1993, 1995). Although hearing-impaired adults are capable of assisting in the subjective validation of a hearing aid fitting, an infant cannot and thus depends on the knowledge of the audiologist to ensure a proper fitting. Hence, amplification must be as precise and accurate as possible.
In this article, we will address the various variables affecting the accuracy during the quantification of hearing thresholds for children at ages of 0–5 years, focus on the application of these thresholds during the calculation of output characteristics for these children's hearing aids, and suggest solutions in order to promote an effective intervention.
Variables Affecting the Quantification of Hearing Thresholds and Hearing Aid Amplification in the Pediatric Population
Ear Canal Properties
A frequently overlooked variable affecting the hearing assessment and the calculations of hearing aid gain/output is the physical change in ear canal dimensions that occurs rapidly during the first 20 months of life and continues until the age of approximately 5 years (Bentler, 1989). The external ear canal is a complex sound resonator that modifies the spectral amplitude characteristics of an incoming sound wave. The resulting imprint from the ear canal is dependent on its shape, volume, length, and on properties of its surrounding tissues. It is known that the shorter and smaller ear canal of the child results in a higher resonance frequency of the unoccluded ear than that of the adult (Kruger, 1987). This means that the resonance amplification found around 3 to 4 kHz in adults is not yet present in this frequency range in very young children, leading to a higher (worse) free-field threshold in this region. Instead, infants have a resonance amplification at frequencies between 4 and 7 kHz (Westwood and Bamford, 1995). Figure 1 illustrates the physical changes in ear canal length and resonance frequency during childhood. At the age of approximately 5 years, the ear canal has almost come to its final dimensions and is therefore acoustically equivalent to that of an average adult. For this reason, the use of the word “children” in this article will refer to children under the age of 5 years.
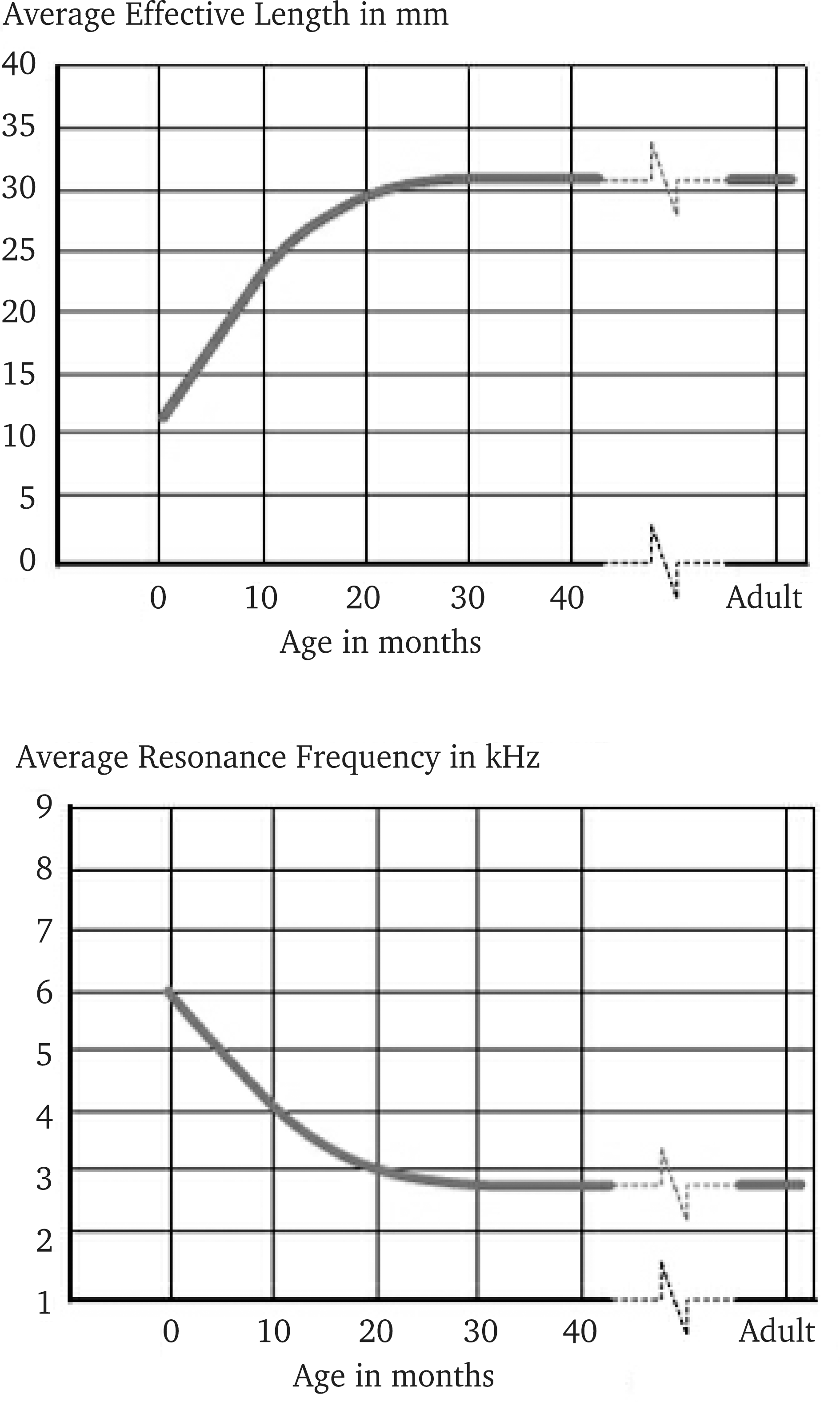
Average effective ear canal length (top panel) and average ear canal resonance frequency (bottom panel) of the human ear canal as a function of the age. Adapted from Kruger, 1987.
Because of the smaller volume, a greater sound pressure level will typically develop in the occluded ear canal of the child compared to that generated by the identical acoustic signal introduced into the adult's occluded ear canal (Feigin et al., 1989). This will lead to a seemingly lower (better) hearing threshold in the child when the same electrical input is presented during audiometric testing using insert earphones calibrated for average adults. It will also mean a higher output level in the ear canal of the child compared to an adult, when a hearing aid set at identical settings is placed on the ear of a child.
Research has indicated that infants have higher (worse) pure-tone thresholds than adults. This elevation in hearing threshold does not reflect properties of the external ear and cannot be explained by nonsensory factors, such as inattention or inappropriate motor responses (Nozza and Henson, 1999). This elevation in thresholds has been observed both behaviorally (Trehub et al., 1980; Werner et al., 1993) and with electrophysiologic measurements (Sininger and Abdala, 1996).
The auditory system of infants is approximately 10 to 20 dB less sensitive than the sensitivity reached in adulthood (Sininger and Abdala, 1996). Poorer sensitivity has been partly explained by the immaturity of the infant middle ear (Keefe et al., 1993). Infants have lower ear canal conductance for regions above 1000 Hz and higher ear canal conductance below 1000 Hz. Thus, high frequency tones would be attenuated by the infant middle ear before reaching the cochlea; however, this effect is not of sufficient magnitude to account for the total discrepancy in sensitivity. The remaining effect is likely due to neural immaturity, as evidenced by the auditory brainstem response (ABR). Various models have been proposed, where effects of neuronal myelination (Moore et al., 1995), axonal conduction, and synaptic transmission (Ponton et al., 1996) are evidenced.
Other research has dismissed the ability of the ABR to account for nonsensory discrepancies in sensitivity (Werner and Boike, 2001). This line of research has suggested that children are not equipped to monitor the output of single input auditory filters that are centered on specific frequencies (Bargones and Werner, 1994). Thus, thresholds for broadband stimuli are more adult-like than thresholds for narrow-band stimuli (Werner and Boike, 2001).
Unlike for the external ear, normative data are not available in order to account for variability in audiometric measurements that originate from the middle ear, the central auditory system, and nonsensory factors. Perhaps a more accurate pediatric fitting and intervention could be ensured if the sources and time course of this variability were documented. Nevertheless, it can be concluded that the time course of this maturation will gradually cause a change in an infant's measured threshold during the first years of life. It can also be concluded that a higher perceived output may gradually result over time when a hearing aid set to constant settings is placed on the ear of an infant.
Audiometric Equipment
Audiometric equipment and other equipment used to estimate hearing thresholds is usually calibrated so that an average adult with normal hearing will obtain a threshold reading of 0 dB. All transducers, including free-field loudspeakers, supra-aural headphones, and insert earphones, are calibrated to maintain this consistency. The process of measuring hearing thresholds in dB HL is thus rather simple with adults because, after thorough calibration, the hearing threshold level in dB HL is found directly on the audiometer dial. As a result of this correspondence between hearing threshold and the dial reading on the audiometer in adults, it is simple to imagine how one could come to generalize this correspondence in all individuals. However, using the same transducers as for adults, the 0 dB value does not represent an average group of children with normal hearing. Because of physical differences between ear canal dimensions of an infant and of individuals older than 5 years of age, different SPL levels will develop in different ears for the same dial reading in dB on the audiometer when using the same transducer. The following example illustrates this effect. Consider an adult and child with identical hearing loss. Both require the same sound pressure level at the eardrum in order to reach threshold. Consider that the child has a smaller and shorter ear canal which increases the sound pressure level of a stimulus delivered by an insert phone by 10 dB relative to the adult. Assume that the adult has a hearing loss of 20 dB HL at a particular frequency. Then, at the eardrum of the child, when the audiometer dial is set to 20 dB, the transducer will actually produce a sound pressure of 20 + 10 = 30 dB relative to the threshold of normal hearing adults. The audiologist will need to reduce the audiometer setting by 10 dB in order to maintain the same real-ear SPL. The lower dial reading of 10 dB may be misleading to the unaware audiologist if the necessary correction of +10 dB is not added to yield the “correct” threshold of 20 dB HL. Figure 2 illustrates this manifestation.
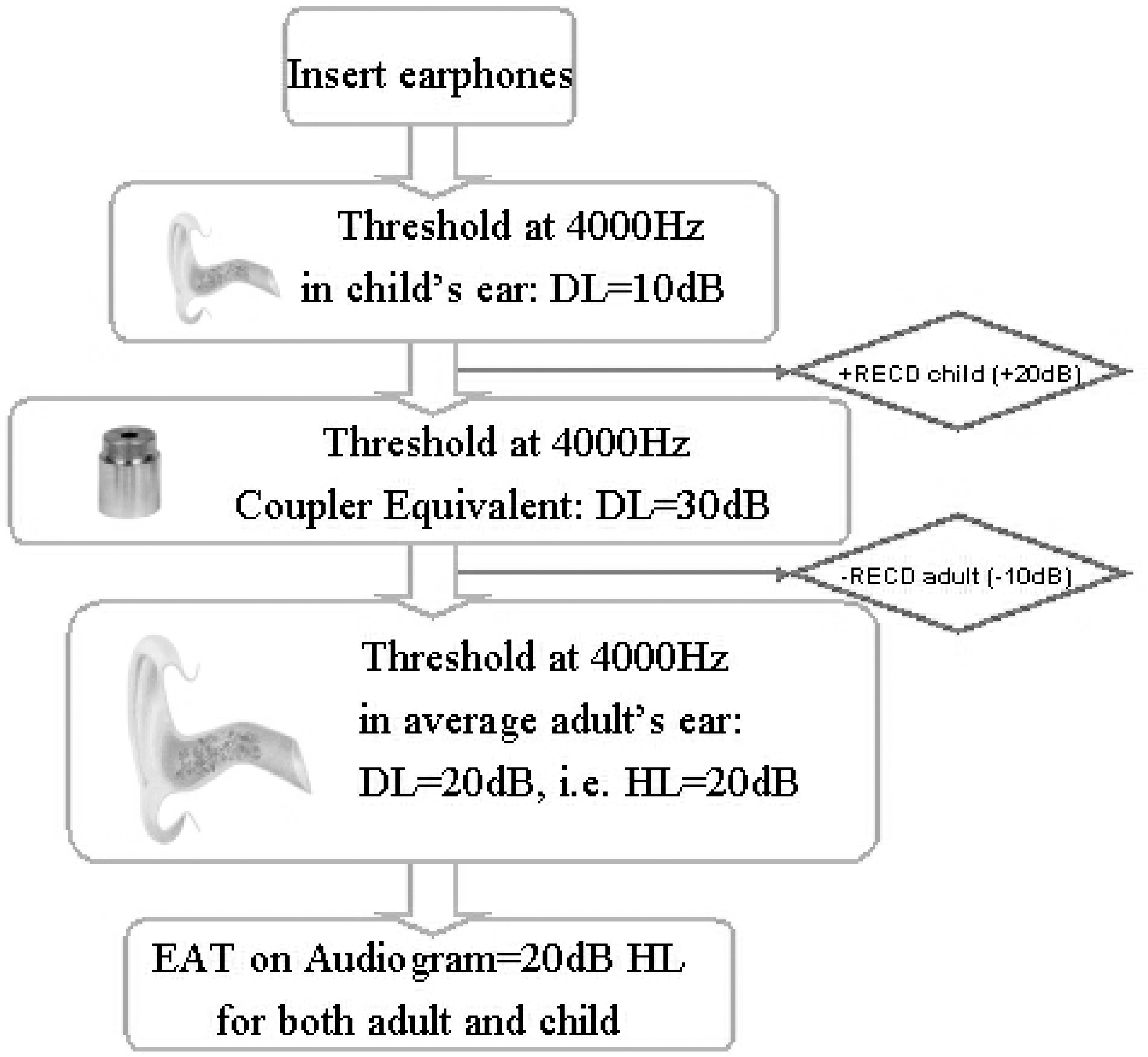
Representation of calculations involved in determining the equivalent adult threshold (EAT) based on an example where the air conduction threshold is being measured at 4000 Hz by using insert earphones for a child younger than 1 year of age. If threshold is reached at 10 dB DL for the child, then the transducer needs to receive an amount of RECD (child) = 20 dB more electrical input in order to reach the same sound pressure level in the coupler, resulting in a dial level of 30 dB DL. In order to produce the same sound pressure level in the ear of an average adult instead of the coupler, the transducer needs to receive an amount of RECD(adult) = 10 dB less of (electrical) input, resulting in a dial level of 20 dB DL. Because of the calibration of the audiometer to average adults, this corresponds to a hearing level of 20 dB HL. The hearing threshold of the child (the EAT) is therefore equal to EAT = 20 dB HL. Average RECD values are taken from Seewald et al., 1993, and Dillon, 2001.
Furthermore, a different SPL will develop in the ear of the same child, depending on the transducer used to obtain threshold measurements. Thus, transducers cannot be interchanged during a pediatric hearing assessment because threshold will be reached at rather different dB readings on the audiometer for each transducer type. Not only does the threshold of normal-hearing children only seldom correspond to the dial reading of 0 dB, but the choice of one transducer instead of another will also have a significant frequency-dependent effect when recording a child's hearing thresholds. Figure 3 illustrates the variability in results when assessing the same child with different transducers by erroneously only reading the audiometer dial.

Predicted monaural air conduction thresholds in dB HL for the same 9 month old child using different signal transducers. Adapted from Seewald and Scollie, 1999.
It becomes apparent that threshold information entered into a prescriptive gain formula in order to estimate the required hearing aid gain requires special consideration when used with children. The clinician must give special attention to the child's outer ear in relation to the audiometric transducer selected during audiometry in order to ensure that the values entered into a prescriptive gain calculation are reflective of the child's ear (ie, dimensions) and the condition under which a hearing threshold was obtained (ie, transducer). Strategies to overcome the calibration problem for children are presented in the following sections.
The gradual evolution of hearing aids has permitted hearing-impaired children to experience their auditory environments with clarity and comfort. However, a wide range of hearing aid types are available as well as a wide range of technology that can be implemented within these hearing aids. Many features are available in order to permit the provision of a hearing aid capable of optimal performance for a particular hearing-impaired individual's auditory needs. Yet, no clear consensus exists on how to select the most appropriate hearing aid, with all the necessary features, that will meet these objectives.
A recent survey by Tharpe and colleagues (2001) reveals that less than 50% of pediatric audiologists provided nonlinear hearing aids to children with severe and profound hearing loss. However, the reasons for choosing a linear or nonlinear instrument were not based on facilitation of the intervention process or optimization of speech and language development. Evidence indicates that nonlinear amplification with digital signal processing (DSP) has potential in facilitating speech recognition in various listening environments (Stelmachowicz et al., 1993) and enhancing the development of expressive and receptive speech of children (Gou et al., 2002). Many features, such as compression with a low compression kneepoint, multichannel processing, and speech enhancement/noise reduction, have been implemented and endorsed for this purpose (For review refer to Kuk and Marcoux, 2002). The combination of these features facilitates the ease at which an accurate amplification of all levels of speech and of all speech elements, including the softer ones and those found in competing noise environments, is achieved. Nevertheless, further studies are required in order to determine optimal fitting strategies for hearing-impaired children.
Following the selection of hearing instruments for the hearing-impaired child, several generic prescriptive formulae can be used to determine the gain and output to be delivered from hearing aids. The gain and output characteristics for a nonlinear instrument can, for example, be specified by the desired sensation level (DSL [i/o]) method (Seewald et al., 1993), or the National Acoustics Laboratories nonlinear method (NAL-NL1). It should be noted that these two methods have been used with success during pediatric fittings (Seewald et al., 2002), although they prescribe different frequency-specific values of gain and output depending on the child's hearing loss.
Lastly, generic prescriptive fitting procedures may provide target values expressed as either insertion gain or aided gain (or, directly equivalent, output level at the eardrum). As an example, the DSL[i/o] method has promoted the expression of target values as aided gain. In contrast, target values provided by NAL have until recently been expressed as insertion gain. While both types of targets can be used to prescribe an accurate amount of gain for the hearing-impaired child, the verification of real-ear gain may be problematic when prescriptive target values are expressed as insertion gain, and vice versa. Still, similar conclusions can be reached from the comparison of the respective target values with the insertion gain or the aided gain from a hearing aid fitted on an adult ear. However, when the same hearing aid is placed on a child, there can be large and age-dependent differences between verification measurements on the child and those made on the adult.
The following sections present an approach to promote an accurate fitting procedure of hearing aids to children. These steps will give close consideration to the physical changes of the child's ear that influence accuracy of pediatric hearing aid fittings. All steps will apply equally to linear and nonlinear hearing aids.
Steps in Ensuring an Accurate Pediatric Hearing Aid Fitting
When dealing with pediatric assessments and fittings, the terminology can easily become confusing because the meaning of many terms (levels, gain settings, etc.) are often implied from their use with adults. Simply adding a prefix such as “corrected” in front of a term does not necessarily make it less ambiguous. We therefore suggest a new consistent terminology in order to clarify the differences between the pediatric and adult populations with regard to the documentation of threshold information and hearing aid fitting. This new terminology will also prevent the ambiguous meaning of audiologic terms used during adult hearing aid fittings. All level and gain values used in the following sections are frequency dependent. The gain of a nonlinear hearing aid will also be dependent on the input signal level. This dependence on frequency and level has been omitted in the following formulae in order to increase their readability. Each of the following formulae is valid in any one single-frequency band, and in case of gains, at any one constant input level.
Reviewing the Definition of Hearing Level
The amount of gain a child should receive from a hearing aid can be calculated using prescriptive formulae. Prescriptive gain formulae typically require at least a measurement of hearing threshold level (HTL) in order to calculate gain targets in various frequency bands. In order to ensure an accurate prescription of gain, it is crucial that the hearing thresholds are valid. Simply stated, it is important to ensure that these thresholds are descriptive of the ear from which they were collected. However, following the previous discussion, it is not sufficient to use the dB reading on the audiometer as input into a prescriptive gain calculation because an erroneous estimation of gain/output will result.
Hearing levels (ie, hearing thresholds expressed in dB HL) are defined as the difference in sound pressure level at threshold between an individual and an average group of normal-hearing adults. The advantage of the dB HL scale lies in its independence from the point of measurement. That is, the same value is repeated whether it is obtained in the free field or with insert earphones. This is not fulfilled for the dB SPL scale, which only makes sense if the place of measurement is mentioned (eg, in free field, or at the eardrum) or at the place of the hearing aid microphone. In an audiometer, the independence of the dB HL scale from the measurement point is ensured by an appropriate calibration of the measurement equipment to average adult persons so that 0 dB on the audiometer dial is equivalent to 0 dB HL. As mentioned earlier, this leads to the following notable effect: The audiometer reading in children, when expressed to the same reference (ie, 0 dB), would suggest that even normal-hearing children possess “different” or “abnormal” hearing. This is due to the developmental difference in the physical properties of the child's external ear. Furthermore, assuming that there is no progression in hearing loss, the audiometer reading at threshold will change with age. Of course, suggestions that a group of children with no anomalies of the auditory system have “abnormal” hearing and that their hearing threshold levels change with age in the absence of progression in hearing loss are unacceptable.
As a means of ensuring an accurate documentation of children's thresholds, it is therefore recommended that measurement conventions be revised in order to avoid confusion during the hearing assessment. In order to reach this objective, it is important to refer to dB readings from an audiometer as dial level or dB DL.
DL: Dial level (Unit: dB). The dial reading on the audiometer. The DL is typically not the correct hearing threshold of the child and 0 dB DL typically does not indicate normal hearing for a child. The mismatch between 0 dB DL and the DL at the threshold of the normal hearing threshold in children is age-, frequency- and transducer-dependent. Note that there can also be such a mismatch in individual adults because of their individual ear canal dimensions. However, the mismatch amongst adults will be “unbiased” (it will be zero on average), while the mismatch between children and an average adult has a clear bias depending on age, frequency, and transducer.
The conversion of a child's hearing thresholds (eg, from dB DL to dB SPL or to dB HL) makes use of some well-known acoustic transforms. These transforms include the free field-to-eardrum transform, also called real-ear unaided gain (REUG) for thresholds collected in the free field, the real-ear-to-dial difference (REDD) for thresholds collected using supra-aural headphones or the real-ear-to-coupler difference (RECD) for thresholds collected using insert earphones. These acoustic transforms should be measured on an individual ear using probe-tube measurements in order to consider the unique spectral amplification properties of the individual ear during the fitting. As mentioned previously, this measurement is important because of individual differences in the ear canal transfer functions among children and adults. However, during the measurement of these acoustic transforms, the sound pressure level recording in the ear canal may have considerable variability. Error sources originate from the probe-tube depth, position, azimuth, stability, and location of the sound source during measurements with children and adults (Dirks and Kincaid, 1987; Valente et al., 1990; Dirks et al., 1996). In addition, the reliability of the technique will likely decrease with an agitated, vocal, or uncooperative child. For these reasons, in the absence of an effective and reliable technique, average age and transducer-dependent corrections are available. Average transforms are available for various age groups as a result of many studies that have recorded the difference in real-ear measures (RECD, REDD, REUG) between the child and adult (Kruger, 1987, Kruger and Ruben, 1987; Bentler, 1989, 1991; Feigin, et al., 1989; Dempster and MacKenzie, 1990; Dillon, 2001; Bagatto et al., 2002). Despite the fact that these can also be used to conveniently expedite the fitting process, the tabulated average values should be viewed as an inferior replacement for the individually collected data.
We now introduce the following terminology:
ΔRECD, ΔREDD, ΔREUG: Difference of real-ear differences between child and adult (Unit: dB), ie,
At the child's eardrum, the sound level will be different by an amount equal to ΔRECD, or ΔREDD or ΔREUG relative to the sound level at the average adult eardrum for the same equipment and setting (same hearing aid + coupler, or headphones, or free field, etc.). As an example, if ΔRECD = 5 dB at a certain frequency, the same hearing aid will produce a sound of x dB SPL at the eardrum of an adult and of (x + ΔRECD) = (x + 5) dB SPL at the eardrum of the child, ie, 5 dB higher compared to the average adult. If, as another example, ΔREUG = −6 dB, the same free field will, in the unoccluded ears, produce a sound level of x dB SPL at the eardrum of an adult and of (x + Δ REUG) = (x − 6) dB SPL at the eardrum of the child.
Ensuring an Accurate Documentation of Hearing Thresholds in Children
There are two established methods to accomplish the task of expressing a child's hearing threshold in a well-defined way. The first method is to express hearing threshold information in dB SPL at the eardrum instead of dB HL. The SPLogram, such as used with the desired sensation level prescriptive formula (DSL [i/o]) (Seewald, 1995) can be constructed as a result of a level conversion. The advantage of using the SPLogram is that threshold information can appear along with electroacoustic coupler gain estimates on one single graph, and threshold information can be compared between age groups. The SPLogram is a valuable tool within the DSL software but may be difficult to achieve outside of the DSL framework. The SPLogram may be initially unfamiliar in its adaptation for counseling or dissemination purposes, mainly because normal hearing does not coincide with 0 dB SPL at any audiometric frequency, neither for adults nor for children.
The second method also accounts for the properties of the child's ear; however, it achieves a representation of the child's threshold information by providing an equivalent adult threshold (EAT) expressed in dB HL. We present here the same definition of EAT as given by Dillon (2001, Chapter 15):
EAT: Equivalent adult threshold (Unit: dB HL). The EAT is defined as the hearing threshold level that an average adult would have if the adult had the same threshold in dB SPL at the eardrum as the child. For the purpose of this definition it is assumed that the threshold measured in dB SPL at the eardrum is the same in a normal hearing adult and in a normal hearing child. In other words, the EAT relates the threshold level at the child's eardrum to the normal threshold level at the eardrum of an average adult, ie, MAP (minimal audible pressure). Note that EAT and HTL (hearing threshold level) are identical in average adults. It follows therefore that an EAT of 0 dB HL indicates normal hearing regardless of the age of the child and independent from the frequency or transducer chosen.
The EAT for a child cannot be directly read from audiometric equipment. Instead, it can be calculated in a variety of ways, each leading to the same EAT value. These calculations make use of the same acoustic transforms that are used for the SPLogram method. In addition, they also use a common coupler (eg, 2 cc coupler) as a reference for both the child's and adult's ear canal properties. Following Dillon (2001), the EAT at any frequency when using insert phones, a 2 cc coupler, and standard audiometric equipment can be calculated as:
An EAT-based method is used by the NAL-NL1 procedure. The main advantage of the EAT is that it provides a direct comparison between the hearing thresholds of the child and that of a normal hearing adult (0 dB HL in both cases), which is the primary reference point in diagnostic audiology and counseling. Initially, the dB HL scale holds more familiarity for most clinical audiologists.
By again considering the example illustrated in Figure 2, one can observe that both the child and the adult with identical hearing loss have a hearing threshold level or EAT of 20 dB HL. This EAT corresponds to 10 dB DL in the child and 20 dB DL in the adult. The one-to-one correspondence between dB HL and dB DL values in the adult, is not valid during audiometry with children. In sum, the distinction between EAT and DL is necessary to retain the original intent of the definitions of hearing level (HL) and hearing threshold level (HTL). This distinction is illustrated in Figure 4. By directly plotting the audiometer's dial level at threshold on the skewed audiogram and by extrapolating to the dB HL axis of the standard audiogram, the EAT is provided. Consider the example where a child under the age of 1 year is assessed with insert earphones. Threshold at 4000 Hz reveals a dial level of 40 dB DL. By placing this value on the skewed audiogram in Figure 4 (top panel), and extrapolating to the standard audiogram, an EAT of approximately 50 dB HL is revealed. Now consider the same child assessed in the free field. Threshold at 4000 Hz is now obtained at 65 dB DL. By placing this value on the skewed audiogram in Figure 4 (bottom panel), and extrapolating to the standard audiogram, the same EAT of 50 dB HL is revealed. These skewed audiograms can also determine the dial levels required to obtain an EAT 0 dB HL and determine normal hearing for children of a particular age group, assessed with a selected transducer. However, these skewed representations are mostly for illustrative purposes and would be of limited clinical value since the transformation between dB DL and dB HL is different for different age ranges and for different transducers. Therefore, a different skewed audiogram would be required for each age increment and for each transducer type. Furthermore, these illustrations were constructed based on average acoustic transforms from published data (Kruger, 1987; Bentler and Pavlovic, 1989; Seewald et al., 1993; Dillon, 2001) and may only approximate the relation between the dB DL and dB HL scales for an individual child. The transformation between these scales, and hence the calculation of the EAT, should be performed using individual data of the child's acoustic transforms. For an insert phone or for a free field these calculations were given earlier in equations 1 and 2.

Illustration of DL and HL audiograms for a child under the age of 1 year assessed with insert earphones (top panel) or in the free field (bottom panel). The calculations of DL values are based on average RECD and REUG values taken from Seewald et al., 1993, and Dillon, 2001.
The audiologist using the audiogram for the purpose of diagnosis and documentation should adopt the use of the dB DL notation and the application of acoustic transforms to dial levels in order to obtain the accurate hearing thresholds. This being said, it could also be useful for generic prescriptive gain methods to reinforce the importance of obtaining an accurate audiogram by permitting the audiologist to enter threshold information expressed in either dB DL, or in another form, (EAT or SPLogram). It may also be useful for fitting softwares to calculate and illustrate the EAT or the SPLogram, based on the application of average or individual acoustic transforms to thresholds in dB DL, in order to avoid the audiologist's task of calculating these conversions manually.
Another benefit from displaying the EAT (or the SPLogram) alongside the DL in the fitting software is that confusion in the diagnosis of minimal hearing loss is avoided. It has been stated that an EAT of 15 dB HL should be strongly considered as the lower limit of normal hearing in children (Northern and Downs, 1991). This criterion should of course not be mistaken with 15 dB DL. Consider the following example, where an audiologist assumes that an 8-month-old child has normal hearing because he obtained thresholds at 15 dB DL with insert earphones. His assumption is wrong, as, at 4 kHz for example, this threshold may correspond to an EAT of as much as 25 dB HL and provide evidence of a mild high-frequency hearing loss. Thus, it should be emphasized that an EAT of 15 dB HL should be considered as the lower limit of normal hearing in children. The calculation of the EAT might be important when considering the impact of minimal hearing loss on academic and social development in children (Bess et al., 1998). For this purpose, the dB DL values necessary to reach the EAT of 15 dB HL criterion are documented in Table 1, based on age and transducer-dependent average acoustic transforms (Kruger, 1987; Bentler and Pavlovic, 1989; Seewald et al., 1993; Dillon, 2001).
Dial levels corresponding to minimal hearing loss of 15 dB HL for audiometry in free field or with insert earphones for different age groups. The dial level of the audiometer is assumed to be calibrated for use with average adults. Note that all dial level values are rounded to the nearest 5 dB, which is the common step size in many audiometers. If the threshold dial levels of the child equal or exceed those in the table, an indication is given that the child may have at least a minimal hearing loss. Data are based on average RECD and REUG values are taken from Seewald et al, 1993, and Dillon, 2001
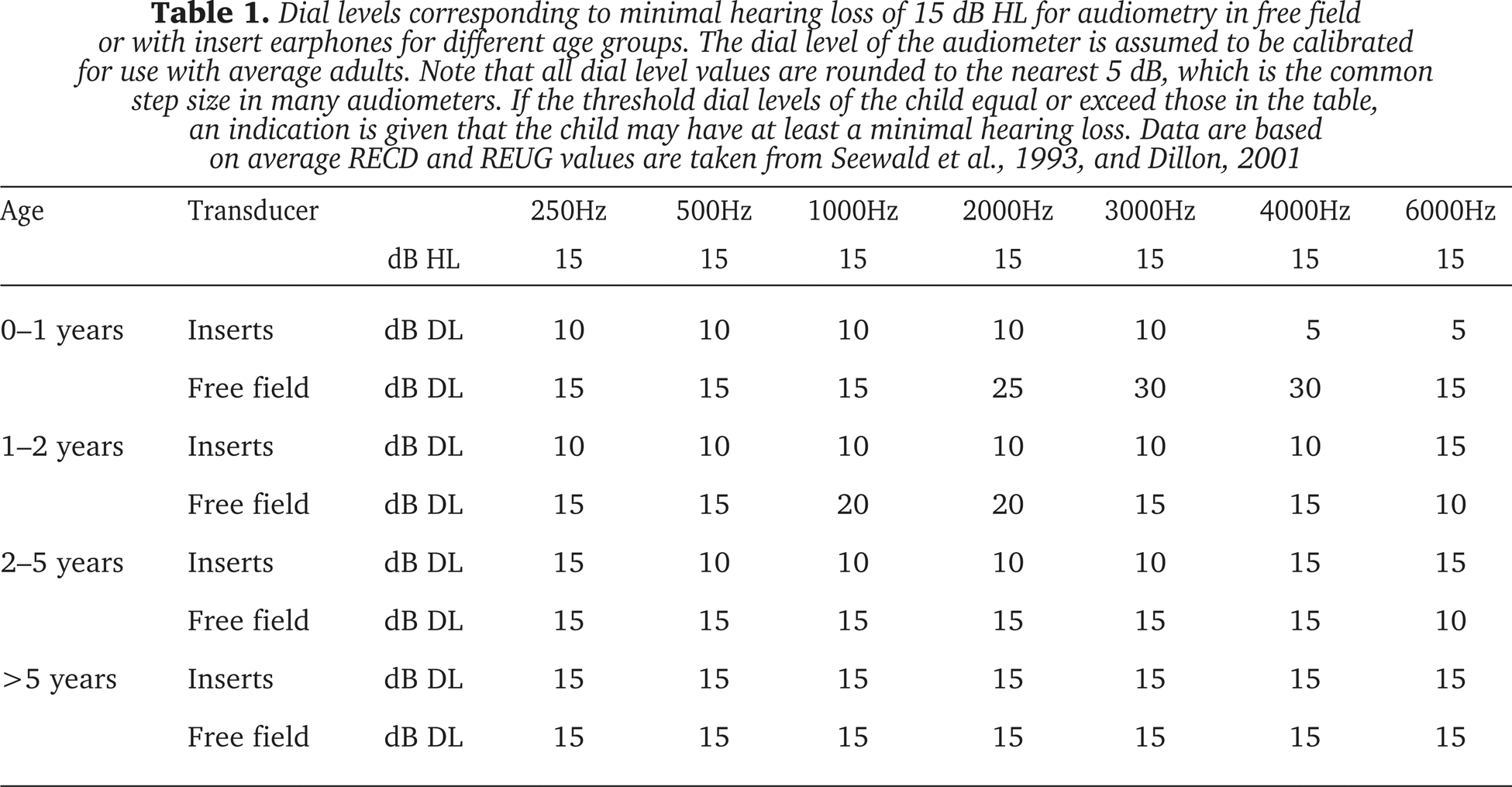
Dial levels corresponding to minimal hearing loss of 15 dB HL for audiometry in free field or with insert earphones for different age groups. The dial level of the audiometer is assumed to be calibrated for use with average adults. Note that all dial level values are rounded to the nearest 5 dB, which is the common step size in many audiometers. If the threshold dial levels of the child equal or exceed those in the table, an indication is given that the child may have at least a minimal hearing loss. Data are based on average RECD and REUG values are taken from Seewald et al, 1993, and Dillon, 2001

Special attention should be given to whether or not the chosen prescriptive gain calculation requires that thresholds be entered in the dB DL format. In fact, if an audiologist were to obtain the EAT values during a pediatric assessment and enter them into some prescriptive gain calculations, this could lead to a second transformation and an erroneous calculation of gain.
Producing the accurate value of hearing thresholds is a prerequisite to the next section, which deals with the accuracy of prescriptive gain calculations.
Certain studies have documented unique loudness requirements of hearing-impaired children (Serpanos and Gravel, 2000; Leibold and Werner, 2002). Nevertheless, there is no conclusive evidence that fundamentally different specific pediatric prescriptive gain formulae should be implemented during pediatric fittings (Ching et al., 1997).
In the following, we derive the necessary steps for an appropriate pediatric prescription of hearing aid performance. We start with hearing thresholds expressed as EAT. Once the EAT has been determined, the following gain can be calculated:
EAIG: Equivalent adult insertion gain (Unit: dB). The EAIG is a function of a set of EATs. The EAIG is the insertion gain that a prescriptive fitting rule will calculate for an adult with a hearing loss as specified by the EAT values of a child. The EAIG is thus identical for all individuals independently of their age and individual characteristics of the ear canal. It is however not the insertion gain that should be prescribed for the child (see below).
Most fitting rules calculate a target insertion gain, ie, gain values. This is true for both older rules (half-gain rule or POGO) and for modern rules (NAL-NL1). An exception is DSL[i/o], which effectively prescribes real-ear output levels as the primary target. With modern fitting software, a conversion from IG to output level and vice versa can be achieved conveniently. The question that thus arises is whether a child should be prescribed the identical amount of IG or the identical output at the eardrum (or aided gain). As the child's REUG differs from that of an adult, it is not possible to provide both an identical IG and identical aided gain to children and adults with equivalent hearing loss. The choice will then depend on the definition of normal hearing in children. The intuitive definition, labeled definition 1 in the following, defines a child to be normal hearing if it shows the same hearing thresholds as an average group of children of the same age group without any hearing problems or pathology of the auditory structures. However, if we consider that maturation of the middle ear and central auditory structures may affect perceptual sensitivity of the inner ear and cause a shift in threshold, it would be rather difficult to determine an accurate representation of normal hearing in infants as these maturational effects are neither well understood nor accurately quantified.
Both the SPLogram method and the EAT-based approach consider a more practical definition of normal hearing in children, labeled definition 2, which applies when a child shows the same hearing thresholds as a normal hearing adult, as measured by the sound pressure level at the eardrum. The practicality of this definition is appealing as normal hearing is well defined in the adult population and this criterion applies to most individuals.
According to definition 1, the logical prescription rationale could be that the child should receive the same IG as an average adult with equivalent hearing loss. This is so because the child should be given some amount of gain relative to the unaided gain that all normal-hearing children of the same age group get from their ear canals, just as the adult with equivalent hearing loss will be given the same amount of gain relative to the unaided gain that all normal-hearing adults gets from their ear canals. In sum, the identical IG should be given to the child and the adult with identical EATs. However, according to the more practical definition 2, the logical rationale is that the child should receive the same real-ear output level as the adult with equivalent hearing loss. This is so because a normal-hearing child and adult have the same hearing thresholds, as measured at the eardrum. They should therefore receive the same real-ear output at the eardrum. Both possible prescription rationales differ to a similar extent to which the REUG of the child and the adult differ. The following example illustrates the effect that this rationale has on the IG. We consider a 6-month-old child with a flat hearing loss of 50 dB HL (EAT). For simplicity, we assume the use of a linear hearing aid and we use the half-gain rule which prescribes an amplification of IG = 50/2 dB = 25 dB at all frequencies. For a linear aid, it is sufficient to consider sinusoids as input signals, eg, sinusoids at 60 dB SPL. For an adult with a flat hearing loss of 50 dB HL, this would result in a prescribed real-ear output level or real-ear aided response (REAR) of:




Illustration of the application of equal insertion gain or equal aided gain (ie, equal output level at the eardrum) for an adult and a 6 month old child with identical hearing loss of EAT = 50 dB HL. The real-ear unaided gains appear on the bottom of both graphs, the real-ear aided gains appear on the top portion of each graph, whereas the insertion gains appear as the vertical lines between the unaided and aided gain curves. The upper graph shows the case where the child receives the same 25 dB insertion gain as the adult would be prescribed. The lower graph shows the case where the child receives the same aided gain as prescribed to the adult, resulting in IG = 25 dB for the adult, but not for the child.
The following can be seen from these equations: Because the calculation of insertion gain takes into account the individual REUG, an identical prescription of insertion gain to a child and to an adult with identical hearing loss will result in an unequal amount of output sound pressure level at the eardrum, at most frequencies (see Eq. 3 and 5). Furthermore, as the REUG of the child changes over time, the resulting prescribed output sound pressure level at the eardrum of the child will change over time.
On the other hand, an identical prescription of output sound pressure level at the eardrum to the child and to an adult with identical hearing loss will result in a prescription that is independent of age if the hearing loss stays constant (see Eq. 4). However, this rationale will result in an unequal amount of insertion gain for the child and the adult at most frequencies (see Eq. 7). From the prescribed output level, it is possible to calculate the corresponding insertion gain for the child which will be appropriate for this rationale, ie, the delivery of the same output level measured at the eardrum of the adult with equivalent hearing loss. We define:
IGRO: Insertion gain for restored output (Unit: dB). The IGRO is the insertion gain which the hearing aid needs to produce for a child in order to give the same “restored” output sound pressure level at the eardrum of the child as would be measured at the eardrum of an average adult with the hearing aid set to the corresponding EAIG prescribed to the adult. The IGRO can be calculated from the EAIG as:

Using the real-ear unaided response REUR and real-ear aided response REAR, the expression for IGRO (6) can be deduced as follows:

Generally, if IG(adult) is the insertion gain of the hearing aid necessary to reach a specific output REAR(adult) in the adult ear, then IG(child) = IG(adult) – ΔREUG is the necessary insertion gain of the same hearing aid to be prescribed for the child, if the intention is to reach the same output level REAR(adult) at the eardrum of the child.
Considering the previous numeric example once again, where the child given the same output level at the eardrum as the adult (Eq. 4) will need to be provided with an insertion gain that is:

From Eq. 8 it can be seen that the prescribed IGRO needs to change with age if the EAT of the child, and correspondingly the EAIG of 25 dB from this example, remains constant. A frequent recalculation of gain is therefore necessary over time in order to provide an accurate pediatric fitting. This notion should also be considered during any verification procedure, which will be discussed in a later section.
Having determined that equal real-ear output should be provided to children and adults with identical hearing loss, a hearing aid must be adjusted or programmed to produce a specific output. The previous section proposes that an amount of gain equal to IGRO should be prescribed to a child. This value of IGRO should also be measured on the child, eg, during a verification with real-ear measurement equipment. In the event where verification takes place with the hearing aid mounted to a coupler rather than to the real-ear, an appropriate coupler gain target should be determined. Just as the prescribed insertion gain for the child and for the adult with identical hearing loss will differ, so will the prescribed coupler gain.
A hearing aid which is set to give a certain output level in the ear of an adult will typically produce a higher output level in the child's ear canal because of its smaller dimensions. The same phenomenon was also discussed in the section about pediatric audiometry. Therefore, the prescribed coupler gain for an adult fitting must be corrected in order to be appropriate for a pediatric fitting. We introduce the following definition:
CGRO: Coupler gain for restored output (Unit: dB). The CGRO is the coupler gain which the hearing aid needs to produce in order to give the same “restored” output sound pressure level at the eardrum of the child as would be prescribed and measured at the eardrum of an average adult with the hearing aid set to the corresponding EAIG prescribed to the adult. The CGRO can be calculated either from the EAIG or from the adult's coupler gain2
cc
(adult) corresponding to that EAIG by:


Using the output level in the coupler, p2 cc , and the input level in the free field, p FF, the expression for CGRO (Eq. 9 and 10) can be deduced as follows (see Eq. 11 and 12):


Verification of the pediatric hearing aid fitting aims to determine whether the prescribed performance of hearing aid gain can be measured in the ear of the child. Insertion gain measurements are often produced for this purpose. Also, since many prescriptive gain calculations are expressed as insertion gain values, it is logical to verify the insertion gain of the hearing aid in order to obtain a direct comparison between the prescribed and real-ear performance. As discussed previously, the calculation of insertion gain of the child's hearing aid requires an initial measurement of his or her REUR in the unoccluded ear canal. The insertion gain can then be obtained by measuring the REAR and subtracting the child's REUR. The resulting insertion gain would then be compared to the prescribed insertion gain in order to determine whether the amount of available gain is adequate for the child's hearing loss.
At this point, it is vital for the verification process to actually compare the measured IG in the child's ear with the correct IG prescribed for the child. This is not the same insertion gain as EAIG which would have been prescribed to an adult with identical hearing loss as the child. Instead, recall that the prescribed IG for the child is given by Eq. 6, if the rationale is to prescribe the same output level, REAR, for the child and adult with equivalent hearing loss.
Consider the following example, where a child has a flat 50 dB HL (EAT) hearing loss. Assume a fitting rule that would provide an adult with this hearing loss with EAIG = 25 dB of insertion gain at 3000 Hz. That insertion gain is calculated based on the knowledge that the average adult REUG is 14.5 dB at this frequency. During the verification of insertion gain, the REUG of the child is only 0.5 dB SPL at this frequency. If the hearing aid would mistakenly be “fitted” by adjusting the measured insertion gain of the hearing aid for the child until it reaches the value EAIG = 25 dB, that value would then be too low by 14 dB. Instead, the measured insertion gain should equal the IG which is appropriate for the child, ie, IGRO (see Eq. 6):
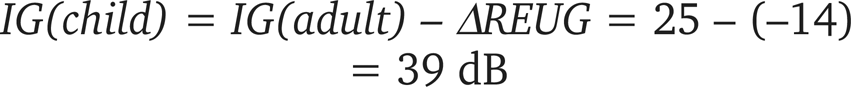
In order to circumvent the calculation of insertion gain to be measured during verification (see Eq. 6), it has also been suggested to assess the performance of a hearing aid in the ear of the child by defining a verification strategy based on real-ear aided gain (Seewald, 1995; Ching et al., 2002). Regarding verification, the advantage of the aided gain for the child is that it does not have to consider the REUG of the child nor its RECD. Instead, the prescribed aided gain is the same for all individuals with identical hearing loss, regardless of their age. The aided gain measured in a child of any age should equal the aided gain that would be prescribed and measured in an adult with identical EATs. Otherwise, in order to minimize real-ear measurements with the child, a verification of coupler gain is feasible when incorporating the RECD of the child (see Eq. 9 or 10).
Adjusting an Internal Gain Parameter of the Hearing Aid
With the above terminology, the necessary insertion gain or coupler gain of a hearing aid can now be accurately determined. Finally, during the actual programming, the hearing aid or its programming software will typically offer a handle that allows one to set the hearing aid gain. Let us assume that this handle is internally calibrated to show the insertion gain that the hearing aid will provide in an average adult person. This may be the case for many manufacturers. Then, special awareness is necessary in the following case: If the hearing aid does not posses a distinct pediatric fitting mode, it will always assume a fitting to an average adult person. In this case, the reading of the gain handle will only reflect the measured IG for an average adult person, but not for a child.
We now introduce the formal concept of an internal hearing aid gain handle Gint. .
Gint. : The setting of a hypothetical internal gain handle of the hearing aid (Unit: dB), indicating the insertion gain of the hearing aid for an average adult. Such a handle might be provided in the fitting software if it assumes an average adult value for REUG and RECD. In an average adult, the amount of insertion gain that the hearing aid actually provides will equal the value of Gint. , which is also equal to EAIG, while a mismatch between the two values will be observed in a child.
Attempting to set the insertion gain of the child's hearing aid simply by moving the gain handle Gint. to a value equal to EAIG, will result in an erroneous pediatric fitting. The reason for this is that the internal gain handle must consider the amount of natural amplification from the ear canal as expressed in REUG and RECD, which is not equivalent to that measured in children. Unless the fitting software is prepared for pediatric fittings and considers the correct REUG and RECD values of the child, the calibration of the internal setting of the gain handle will be incorrect. In order to adjust the hearing aid to actually deliver the correct amount of intended insertion gain, Gint. needs to be manipulated to account for the mismatch before it is input into the hearing aid programming software.
If the aim of the fitting is to prescribe the same hearing aid output as for an adult, and if no specific pediatric fitting mode is available, the Gint. needs to be corrected by the value ΔGRO:
ΔGRO: Difference in internal gain parameter for restored output (Unit: dB). In the case where the hearing aid offers a handle for Gint.
and if no pediatric fitting mode is available, that hearing aid gain handle needs to be set to the value Gint.
= EAIG + ΔGRO in order to produce the same output at the eardrum of the child that the hearing aid produces for an average adult with the hearing aid set to Gint.
= EIAG. The difference equals ΔGRO = ΔRECD, ie, the internal gain handle needs to be set to Gint.
= EAIG – ΔRECD. This can be seen as follows:


Note that the necessary correction is the same as the one calculated for the coupler gain (see Eq. 9). Of course, the hearing aid must only be adjusted to Gint. = EAIG – ΔRECD in the case that the aid possesses the mentioned Gint. handle calibrated for adult fittings (ie, the hearing aid assumes an average adult value of REUG and RECD). Still, when measured via real-ear probe-tube microphone equipment, the hearing aid should provide an insertion gain of IGRO. If the hearing aid does indeed possess a pediatric fitting mode, the above mismatch will most probably be taken into account by the manufacturer. In this case, one should consult the hearing aid fitting manual in order to determine whether the gain handle is calibrated either to reflect the actual pediatric situation, or the average adult situation.
For completeness we also discuss the necessary pediatric correction for Gint. if the aim of the fitting would be to achieve the same hearing aid insertion gain in the child as in the adult with identical hearing loss, although we discourage the reader from doing so. For this rationale, if no specific pediatric fitting mode is available, the Gint. has to be corrected by the value ΔGRIG:
ΔGRIG: Difference in internal gain parameter for restored insertion gain (Unit: dB). In the case that the hearing aid offers a handle for Gint.
, that gain handle needs to be set to the value Gint.
= EAIG + ΔGRIG in order to result in an insertion gain for the child that equals the EAIG for the adult. The difference equals ΔEAIG = − ΔRECD + ΔREUG. This can been seen in the same way as explained for ΔGRO when continuing in equation 14:
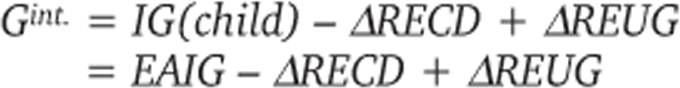
Note that the hearing aid must only be adjusted to an Gint. = EAIG – ΔRECD + ΔREUG in the case that the aid possesses the mentioned Gint. handle calibrated for adult fittings. Still, when measured via real-ear probe-tube microphone equipment, the hearing aid should give an insertion gain of EAIG. Again, if the hearing aid does indeed possess a pediatric fitting mode, the above mismatch will most likely be taken into account by the manufacturer.
Many benefits are associated with the early detection and intervention of pediatric hearing loss. However, hearing aid fittings must be performed using the highest level of accuracy in light of the various risk factors associated with either over- or under-amplification. A number of generic and nongeneric fitting softwares ease the prescription of an accurate hearing aid output. It is nevertheless important to understand the many factors which influence the hearing aid performance of a pediatric fitting in the event where corrections are absent or unclear within a particular fitting protocol.
The most important steps of a pediatric hearing aid fitting are:
Be aware of the distinction between the DLs (which are misleading) and the expression of hearing threshold levels in terms of the EATs or the SPLogram.
Use the EATs as input to most generic prescription fitting rules (except for, eg, DSL[i/o] which uses the SPLogram data).
Identify the insertion gain prescribed from an adult fitting rule as the EAIG.
Calculate the IGRO. This is the insertion gain that should be measured/verified in the child using real-ear equipment. It is the insertion gain that is necessary for the child in order to yield the same output level at the eardrum as for an adult with identical hearing loss (see Eq. 6).
If necessary, calculate the appropriate coupler gain CGRO which should be measured/verified in a hearing aid coupler (see Eq. 9 and 10).
In case you are fitting a hearing aid without a specific pediatric fitting mode, but with an internal gain handle calibrated to indicate the insertion gain for an average adult, adjust that gain handle by ΔGRO to the value Gint. = EAIG – ΔRECD (see Eq. 14).
During verification, make sure to compare the measured IG in the child with the IGRO, and not with the EAIG.