Abstract
Introduction
Pelvic fractures pose a significant treatment challenge in the prehospital environment, often resulting from high-energy trauma and concurrently presenting with life-threatening hemorrhage necessitating immediate intervention. Commercial pelvic binders such as the Structural Aluminum Malleable (SAM) Pelvic Sling II have become commonplace in prehospital care, especially in military medicine. However, given limitations to carried equipment and the scarcity of pelvic fractures, medics in austere conditions may opt to carry just one or even no commercial pelvic binders.
Objective
This study explored an innovative approach using 2 Combat Application Tourniquet II (CAT II) devices tandemly connected to stabilize pelvic fractures. The primary aim was to assess whether this technique will generate comparable intrapelvic pressure to the SAM Pelvic Sling II.
Methods
This study employed a human cadaveric model for which pelvic fractures were surgically created to generate an open-book fracture. Intrapelvic pressure was measured via a Foley catheter. The SAM Pelvic Sling II was applied in standard fashion 3 times, each with intrapelvic pressure recorded. Similarly, 2 CAT IIs were applied in tandem to the pelvis 3 times to generate 3 pressure measurements.
Results
There was a small yet statistically significant increase in intrapelvic pressure generated by the CAT II method than by the traditional method.
Conclusion
The use of 2 CAT II devices connected in the fashion described in this study appears to offer a potentially feasible and effective alternative for stabilizing pelvic fractures. Yet, further investigation is required before this concept is ever applied to real patients.
Introduction
Pelvic fractures, often resulting from high-energy trauma such as vehicle accidents, falls from height, or battlefield injuries, represent a significant and challenging medical emergency in both civilian and military settings.1–6 These injuries are associated with high morbidity and mortality rates, primarily due to secondary hemorrhagic shock and the potential for associated organ damage.1,2,4,7–9 The complexity of pelvic fractures requires immediate and effective stabilization to prevent further hemorrhage, mitigate pain, and attempt to improve patient outcomes.2–4,6,8 Thus, the current standard of care remains to perform pelvic stabilization despite recent evidence suggesting that it may not provide a benefit to mortality. 10 Traditionally, stabilization techniques have relied on the Structural Aluminum Malleable (SAM) Pelvic Sling II (SAM Medical, Tualatin, OR) and similar devices, which have been shown to effectively reduce pelvic volume and decrease hemorrhage by stabilizing the pelvic ring.6,7,9,11,12 However, the prehospital environment, especially in austere settings, demands equipment that is not only effective but also lightweight and compact.
The physical burden carried by wilderness medical providers is substantial, with every additional piece of equipment potentially impacting their mobility, conspicuity, efficiency, and, ultimately, the survival of their patients and themselves. 13 While effective, the SAM Pelvic Sling II adds to this burden with its significant bulkiness, which may be a factor in why some active-duty combat medics opt not to carry it within their aid bags at all. 14 Therefore, an opportunity to identify a stabilization method that is both effective in its clinical outcomes and pragmatic in its application and transport is warranted. There is growing interest in identifying such alternative methods, especially to apply in mass-casualty situations and other scenarios where prolonged casualty care is paramount due to the looming threat of large-scale combat operations.1,15–19 The Combat Application Tourniquet II (CAT II, Gen VII; North American Rescue, Greer, SC), a mainstay in austere medical kits for extremity hemorrhage control, presents as an intriguing alternative due to its widespread use and availability as well as its lightweight and compact design. 12 Connecting 2 CAT II devices in tandem to form a circumferential pelvic stabilization device would offer a novel approach to managing pelvic fractures in the field, potentially streamlining equipment needs without compromising care.
The primary aim of this study was to evaluate the feasibility and efficacy of using 2 CAT II tourniquets connected as an alternative method for stabilizing pelvic fractures in prehospital austere settings. Specifically, we sought to compare the intrapelvic pressure generated by this technique with that achieved by the traditional SAM Pelvic Sling. By doing this, we aimed to assess whether the CAT II-based method can offer comparable pelvic compression while reducing the equipment burden on military medical providers. This investigation was driven by the hypothesis that the CAT II device, when applied in such a manner, can provide an effective stabilization force across the pelvic region, potentially revolutionizing pelvic fracture management in the prehospital and military environments.
Methods
This study employed a controlled cadaveric model to simulate patients who have sustained pelvic ring fractures. The primary objective was to assess the generated intrapelvic pressure by each pelvic binding method, simulating the application in a prehospital military setting. The cadaver underwent fracture induction and stabilization procedures sequentially using an osteotomy made by a sagittal saw (Stryker System 7; Stryker, Portage, MI) through both the pubic symphysis and the right sacroiliac joint, followed by application of each stabilization method (SAM Pelvic Sling II and CAT II) to facilitate pressure measurement and allow for direct comparative analysis. The primary outcome measure was the intrapelvic pressure generated by each stabilization method measured using a pressure transducer inserted into the cadaver's urinary bladder. Data were recorded at the time of maximum applied pressure for both the CAT II devices and the SAM Pelvic Sling II.
One human cadaver was selected as a convenience sample at the study location. The following demographics were obtained: The cadaver was a 74-y-old female, 168 cm in height, and 89 kg in weight. Cadavers with any history of pelvic surgery or trauma were excluded from the study to maintain uniformity in the sample and to ensure the validity of the fracture induction and stabilization processes. Following fracture induction, a Foley catheter was inserted into the urethral meatus of the cadaver until its proximal tip rested within the urinary bladder. The bladder was filled with 200 mL normal saline. The distal, or external, tip of the catheter was attached to a Bourdon tube style small pressure gauge (Figure 1). The pretest pressure in the gauge was subtracted from the subsequent readings prior to recording the readings. An Abdominal Aortic Junctional Tourniquet–Stabilized (AAJT-S; North American Rescue, Greer, SC) was applied with a pressure of 300 mm Hg to stabilize abdominal viscera and mitigate anatomically cephalic organ translocation during the pelvic compression and facilitate pressure measurements (Figure 2). 20
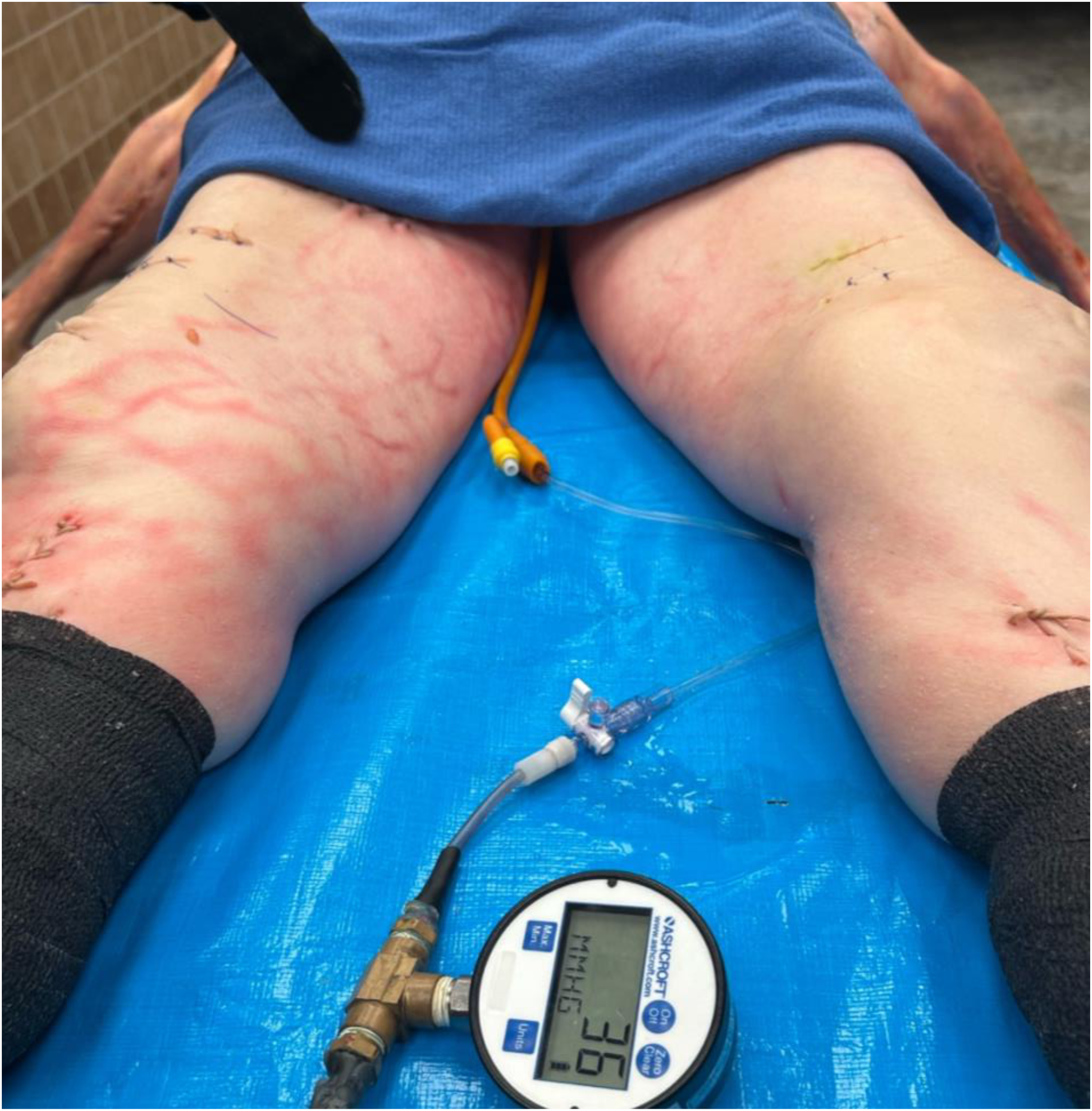
Foley catheter in situ and attached to manometer.
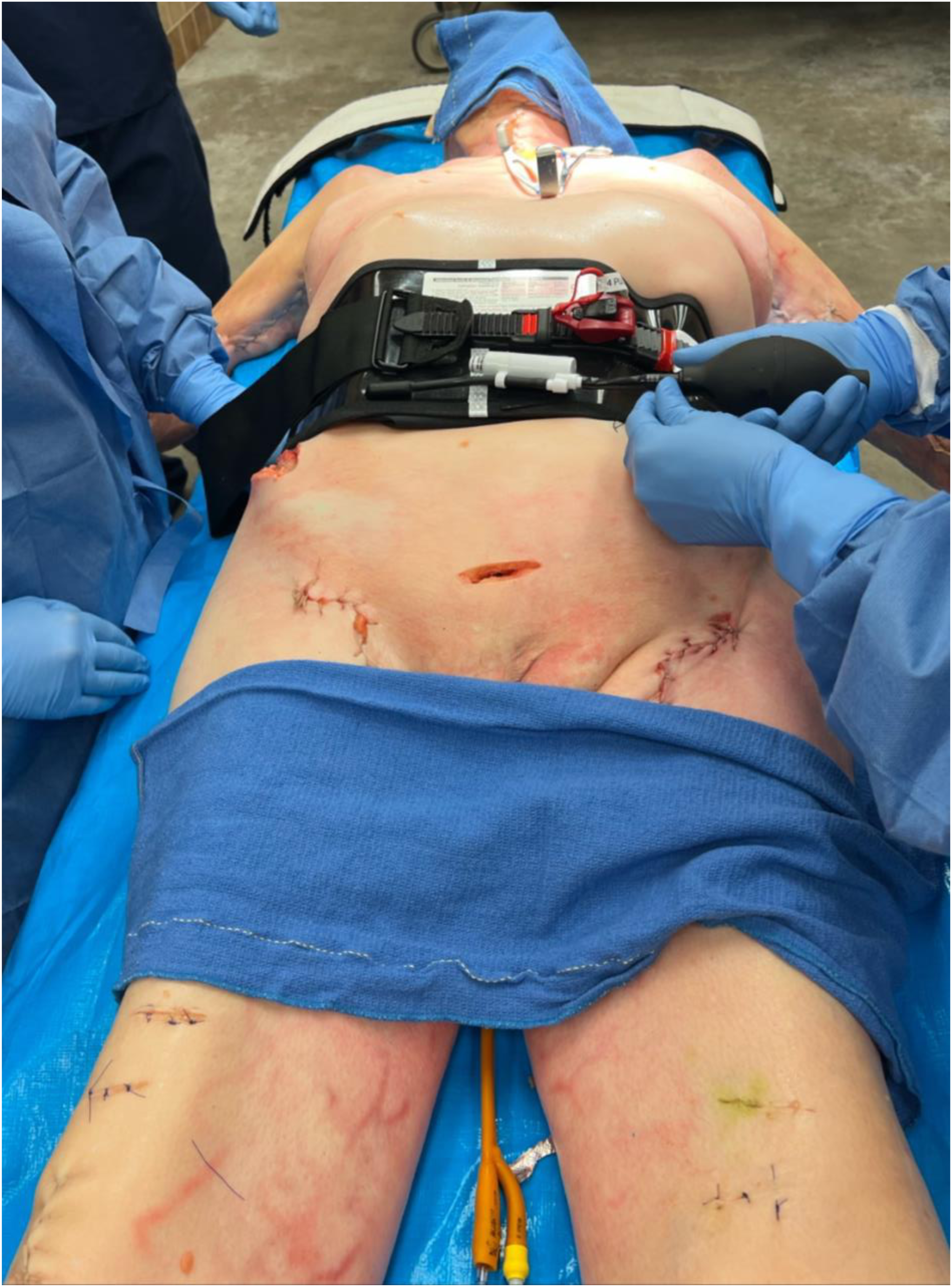
Abdominal aortic and junctional tourniquet stabilized in situ and being inflated.
The SAM Pelvic Sling II was applied according to the manufacturer's instructions. The binder was positioned around the pelvis overlying the femoral greater trochanters and secured to achieve the recommended stabilization pressure, indicated by an audible click of its buckle (Figure 3). The manometer reading was recorded before pressure was released. This process was repeated twice more to generate a total of 3 intrapelvic pressure readings, and then the SAM Pelvic Sling II was removed from the cadaver.
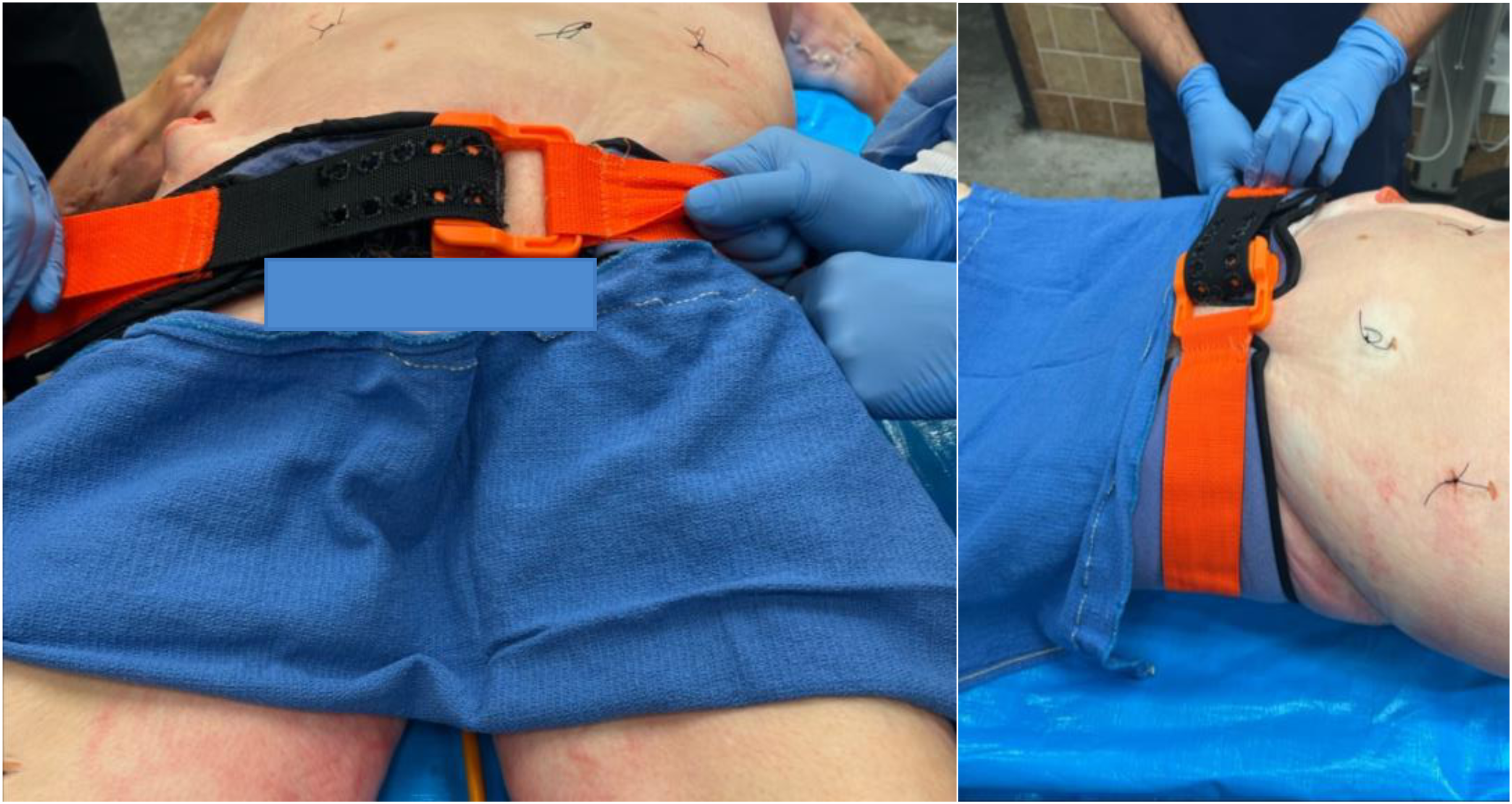
SAM Pelvic Sling II in situ.
Subsequently, 2 CAT II devices were connected end to end by running the Velcro-lined strap of tourniquet 1 through the buckle of tourniquet 2 and folding it back onto itself before being applied circumferentially around the cadaver's pelvis. More specifically, the optimal length of the tourniquet assembly was measured by holding it across the cadaver’s pelvis and adjusting it so that it was only long enough to reach the surface of which the supine cadaver rested. The assembly was passed beneath the cadaver and placed atop the greater trochanters to extend across the pubic symphysis. Pulling as hard as the operator could with just the index finger and thumb on the tourniquet, the Velcro was secured at this point. Further tension was applied by turning each of the 2 windlasses placed symmetrically over the lateral aspect of the cadaver's hips 3 half-turns, totaling 1.5 complete 360-degree rotations on each side before securement (Figure 4).
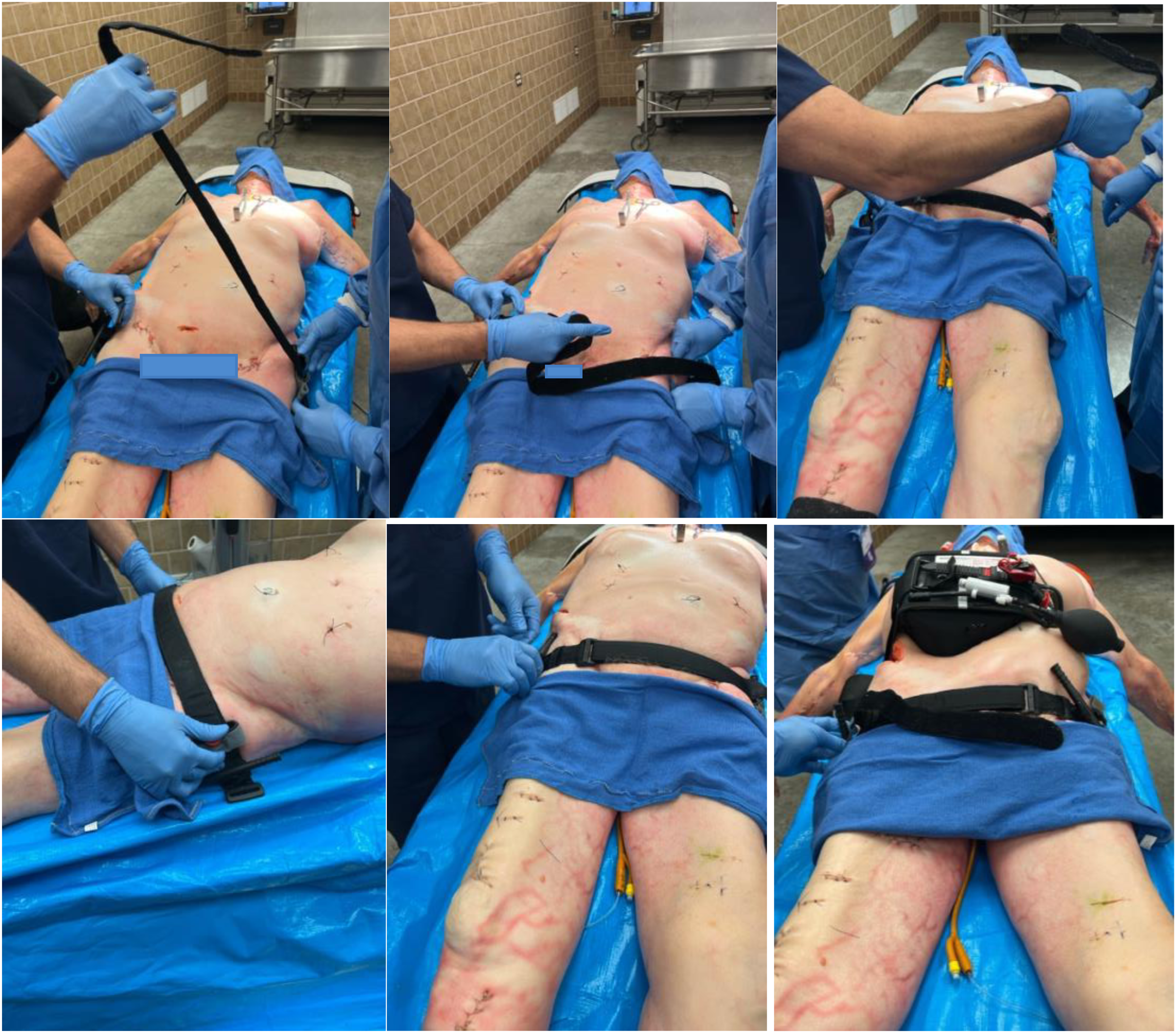
Application of Combat Application Tourniquet II devices connected in tandem and encircling the pelvis.
Statistical Analysis
Statistical analysis was conducted using statistical software SAS 9.4 (SAS Institute, Cary, NC), with the results intended to identify any significant differences in the efficacy of pelvic fracture stabilization between the 2 methods. Intrapelvic pressures generated by the SAM Pelvic Sling II and the CAT II devices were compared using a paired t test owing to the same cadaver providing repeated measures. Descriptive statistics were used to summarize the pressure measurements, and differences were considered statistically significant at a 2-tailed P value of <0.05.
Results
Six pressure measurements were acquired from the 1 cadaver in this study. The SAM Pelvic Sling II accounted for 50% (n=3) of the measurements with mean 34.00 mm Hg (SD 1.00 mm Hg), and the in-tandem CAT II devices generated the other 50% (n=3), with mean 37.67 mm Hg (SD 0.6 mm Hg), as shown in Table 1. All measurements recorded were included in the analysis. There was a significant increase in pressure generated by the in-tandem CAT II devices compared with the SAM Pelvic Sling II (t(2)=5.50; P=0.032).
Intrapelvic pressure measurements generated for each method tested.

Discussion
This study investigated the feasibility and efficacy of using 2 CAT II tourniquets connected in tandem as a novel approach for stabilizing an open-book pelvic fracture in a cadaveric model. The findings demonstrated that the in-tandem CAT II-based method generates an intrapelvic pressures comparable with that achieved by the SAM Pelvic Sling II, a widely used device for pelvic fracture stabilization. Moreover, the CAT II method produced slightly higher mean intrapelvic pressures (37.67 vs 34.00 mm Hg); while statistically significant, it is unclear whether this difference is clinically significant. However, these results should be considered hypothesis generating because they suggest that the CAT II-based method potentially may serve as an effective alternative for pelvic fracture management in austere environments.
This comparable efficacy of the CAT II method highlights its potential advantages in military and prehospital settings. The compact and lightweight design of CAT II tourniquets offers significant logistical benefits, reducing the equipment burden on military medical personnel without compromising pelvic compression effectiveness. This is particularly relevant in combat scenarios where every ounce of weight and space in a medic's kit is critical to mobility and survival. The widespread availability and familiarity of CAT II tourniquets further enhance their practicality, streamlining training requirements and underscoring the versatility of the CAT II device by demonstrating its utility beyond extremity hemorrhage control. By repurposing a device already ubiquitous in military kits, this approach could minimize the need for additional specialized equipment, thus simplifying inventory management and potentially reducing costs.
Limitations
Using a cadaveric model limits the findings’ applicability to living human subjects. The physiologic responses to injury and intervention, such as blood flow dynamics and tissue elasticity, cannot be exactly replicated in cadaveric models. This discrepancy is particularly relevant in the context of military medicine, where patients are often young, physically fit, male, individuals who may respond differently to pelvic stabilization techniques compared with the average population represented in cadaveric studies. Another limitation of this study was that despite achieving statistical significance, the technique was only tested on a singular cadaveric model. We also used only 1 provider/operator to conduct the study and only 1 commercial product for comparison. Likewise, time required for application and the effectiveness of each method under different environmental conditions outside of a laboratory setting were neither investigated nor compared.
Similarly, in real-world scenarios, pelvic fractures can vary widely in location, type, and severity. The fractures introduced in this study were complete transections at the pubic symphysis and the right sacroiliac joint, which only represents a small subset of possible injury patterns that each may respond to stabilization in different manners. Consequently, the efficacy of the CAT II devices in stabilizing fractures of different types or multiple locations remains to be determined. Furthermore, although the CAT II method demonstrated the capability to generate an intrapelvic pressure comparable with that of the SAM Pelvic Sling, it is crucial to consider the distribution of this pressure and strap tension of each device. The narrower structure of the CAT II devices means that the pressure is not distributed over as wide an area as with the SAM Pelvic Sling. This difference in pressure distribution and strap tension could impact the clinical efficacy of the CAT II device, particularly in stabilizing the pelvic ring and mitigating potential intrapelvic hemorrhage as well as potentially contributing to increased skin breakdown injury.1,21 Likewise, pressure associated with each method was not measured over time, which is critical in prolonged casualty care scenarios because it may decrease over time even without patient movement. 1 Further clinical studies are warranted to assess the feasibility and practicality of implementing this technique in real-world scenarios.
Conclusion
The CAT II method described in this study generates slightly higher intrapelvic pressure than the SAM Pelvic Sling II when applied to a cadaveric model with fractures at the pubic symphysis and right sacroiliac joint. Thus, this study provides preliminary evidence supporting the feasibility of using CAT II devices for pelvic stabilization, and the method may offer an alternative to carrying large, bulky pelvic binders for practitioners operating in austere environments or other resource-scarce scenarios such as mass-casualty incidents in the setting of disaster relief or those brought about from large-scale combat operations.16,18 However, due to the extensive limitations of this study, further investigation into matters especially including the resiliency of the CAT II method to maintain efficacy throughout diverse means of patient evacuation is necessary before such a technique may be recommended for real patient scenarios. Thus, this study should serve as an introduction to the concept of pelvic stabilization using the CAT II method rather than a proof of concept.
Previous Presentation
Data from this study were presented at the Special Operations Medical Association Scientific Assembly, Raleigh, NC, May 14, 2024.
Footnotes
Acknowledgments
The investigators extend their profound gratitude to the men and women who generously donated their remains to advance scientific research and medical education. Their selfless contributions have not only facilitated this study but also continue to support the ongoing pursuit of knowledge that benefits humanity.
Author Contribution(s)
Funding
No external funding was used or required for this study.
Disclaimer
The views expressed in this paper reflect the results of research conducted by the author(s) and do not necessarily reflect the official policy or position of the Department of Defense, the Defense Health Agency, or the United States government. The Institutional Review Board for the University of Texas Health Science Center, San Antonio, TX, reviewed and waived this study as nonhuman subject research (IRB No. 00000525NHR). The cadaveric specimen was requested and approved through the Texas State Anatomical Board (Texas Funeral Commission) and the University of Texas Southwestern Willed (UTSW) Body Program for research and procedural training.
