Abstract
Introduction
Traumatic injuries and medical emergencies are common in skiing and snowboarding, often occurring in remote alpine areas where ski patrols provide only basic trauma care. This pilot study, conducted at the Livigno Carosello 3000 Ski Area in Northern Italy, evaluated the impact of adding a healthcare-enhanced ski patrol team that included a critical care nurse and an on-call medical consultant.
Methods
A retrospective observational study compared rescue operations across 2 ski seasons: 2022–23 (basic team only) and 2023–24 (basic and enhanced team). Data were collected from all rescue operations conducted from Sundays to Thursdays, excluding logistical transports and refusals. Patient characteristics, injuries, treatments, evacuation methods, and dispositions were analyzed by season and by team composition.
Results
Among 595 cases (281 in Season 1, 314 in Season 2), the enhanced team managed 61% of rescues in Season 2 and handled significantly more medical emergencies (P<0.01). The enhanced team administered pharmacologic therapy in 27% of cases and applied spinal motion restriction more often (12 vs 2%; P<0.01). Their involvement also was associated with increased snowmobile evacuations (62 vs 49%; P<0.01) and decreased referrals to trauma clinics (48 vs 60%; P<0.01), alongside more on-site discharges and private transports (11 vs 5%; P<0.01).
Conclusions
Adding healthcare professionals to ski patrol teams improved case management, enabled prompt treatment, and optimized evacuation strategies. These findings support integrating clinical expertise into ski patrol operations and warrant further study of long-term impacts on system efficiency and patient outcomes.
Keywords
Introduction
Recreational skiing and snowboarding rank among the most popular winter sports worldwide, but these activities are associated with significant risks, as evidenced by the high number of accidents and injuries recorded each year at ski resorts.1,2 Ski resort medical problems span a broad spectrum, ranging from minor bruises to major trauma, and also include nontraumatic medical emergencies such as metabolic imbalances, neurologic disorders, gastrointestinal issues, and cardiac arrests.3,4
Given the remote locations of many ski resorts, transportation to properly equipped hospitals for trauma care can be both complex and prolonged, potentially resulting in a high workload for the local emergency medical services and emergency departments.5,6 Moreover, the high incidence of traumatic events on ski slopes, often accompanied by severe pain, makes early and effective pain management particularly beneficial. The optimal approach therefore involves delivering critical care and timely, effective analgesia at the point of injury.7–10
Italian law mandates that ski area operators provide technical rescue and transportation services to injured individuals, ensuring their transfer from the slopes to locations accessible to the nearest healthcare or first aid centers. 11 In our setting, ski patrollers, including volunteers and professionals, are trained in basic life support but cannot perform medical assessments or give medications. Including healthcare providers as members of the rescue team may enhance care, allow advanced interventions, and support better training and protocol development.12–15
Starting from the 2023–24 ski season, the Livigno Carosello 3000 Ski Area introduced an enhanced healthcare ski patrol service staffed by an onsite critical care nurse and an on-call medical consultant. Accordingly, the aim of this study was to describe the characteristics of this service and its operations and evaluate its impact on evacuation and patient disposition process, as well as on the early administration of medical interventions, including advanced analgesia.
Methods
Study Setting
This observational retrospective study was conducted at the Carosello 3000 Ski Area, located in Livigno, Italy, a major ski area in the Italian Alps. The resort spans elevations from ∼1816 m at the base to 2800 m at the summit, offering a vertical drop of almost 1000 m. Skiers and snowboarders can explore ∼20 km of trails categorized into blue (easy), red (intermediate), and black (difficult) runs. The resort has no dedicated first aid room or medical facility. A heated room at the base is available for patients awaiting transport, but it is not equipped or staffed as a treatment area and lacks medical resources.
Rescue Operations
A ski patrol service operates throughout public hours, with three rapid-response teams based at a summit hub to ensure full resort coverage. In Season 1, the first team included 2 ski patrollers (basic team). In Season 2, from Sunday to Thursday, it was staffed by 1 ski patroller and 1 critical care nurse (enhanced team). The second and third teams—2 ski patrollers and 1 ski patroller, respectively—remained unchanged.
Basic teams are trained in basic life support and patient transport. Although in other countries this training may follow structured programs such as Outdoor Emergency Care (OEC) or equivalent wilderness protocols, no such nationally recognized qualifications exist in Italy. Consequently, training is delivered through local or regional courses, and under Italian law, team members do not have clinical medical training or authorization to administer medications or perform diagnostic assessments. 16
In Season 2, team dispatch was based on the lead ski patroller's assessment of call details (eg, severity, location, and availability), without formal triage criteria. In some cases, the enhanced team was dispatched directly, whereas in others, a basic team may have responded initially and subsequently requested nurse involvement. However, this escalation process was not standardized and was not recorded consistently in the operational dataset. In our setting, the lead ski patroller is designated based on experience, seniority, and demonstrated coordination skills, as per regional regulations, without a national certification process.
In this setting, transport mode was determined by patient condition: Snowmobiles were used for patients who did not require immobilization or supine transport, whereas patients needing spinal precautions or supine evacuation were transported with a toboggan. Snowmobiles were not used to tow toboggans, which may differ from practices in other resorts.
All teams carry emergency gear appropriate to their roles, with the nurse additionally equipped for advanced care, including an automated external defibrillator, medications, an airway kit, and a nitrous oxide cylinder, which were transported via snowmobile or sled, when possible, or carried in backpacks on inaccessible terrain. Communication is maintained via radio, and collaboration with law enforcement ensures coordinated response and incident investigation. Equipment details are described in Table 1. An overview of the territory and resources is provided in Figure 1.
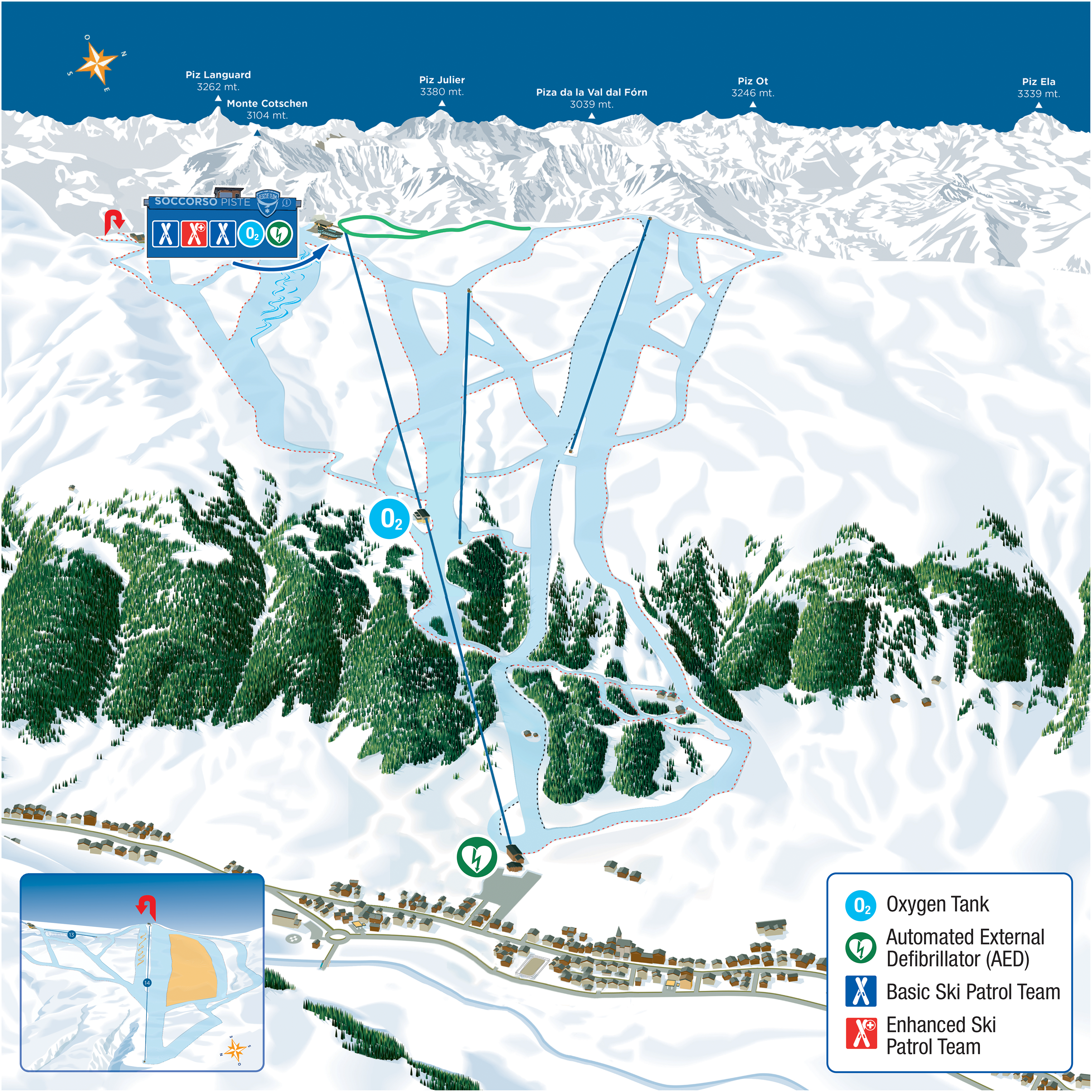
Representation of the Catchment Area of the ski Patrol Teams and Resources Available.
Equipment Available to ski Patrollers and Critical Care Nurses and at Fixed Stations at the Livigno Carosello 3000 Ski Area.

Enhanced Team Protocols and Procedures
The enhanced team operates through close collaboration between the onsite critical care nurse and on-call medical consultant. Nurses were selected from a pool of experienced critical care professionals with advanced skiing proficiency and were required to have at least 1 y of experience in critical care settings as well as valid certifications in Advanced Cardiovascular Life Support, Pediatric Advanced Life Support, and Prehospital Trauma Life Support. Predeployment training included both medical protocols (ie, procedures and algorithms) and slope rescue techniques, including simulation training at a rope access facility and high-fidelity scenarios on the ski slopes.
The scope of practice of the onsite nurses is defined by an operational document listing predefined clinical algorithms, developed and approved by the medical director of the rescue team and a senior emergency physician from the regional Emergency Medical Services (EMS) agency responsible for clinical governance. These were adapted from the portfolio of nurse-led prehospital emergency protocols used in the local EMS system, modified to meet the specific operational needs of a ski resort. The algorithms provide structured guidance on clinical management, including drug administration and other therapeutic interventions that nurses can perform following discussion with the on-call medical consultant. This ensures standardized, high-quality care while remaining within the legal and professional framework of advanced nursing practice. 17 The on-call medical consultant is a senior emergency physician from the regional EMS agency, selected for expertise in prehospital medicine or ski area operations. The physician was available for consultation throughout the day and was consulted by the nurse in all cases, ensuring both timely intervention and clinical oversight.
Although treatment protocols were standardized, there were no formal algorithms for patient disposition; decisions such as whether to discharge on site or initiate EMS transport were made jointly by the nurse and the physician. A list of clinical algorithms is provided in online Supplemental Table A1.
Data Collection
We included all data from rescue operations that happened during the 2022–23 (December 3–April 19) ski season (Season 1) and the 2023–24 (December 3–April 30) ski season (Season 2). We excluded rescues related to logistical reasons (eg, patients requiring transport by ski patrol for nonmedical issues), rescues where patients refused either the rescue or transport, and rescues performed on Fridays and Saturdays. The exclusion of the latter was due to contractual constraints because the critical care nurse, and hence the enhanced team, was available only from Sunday to Thursday in Season 2. Therefore, we compared data only from these weekdays across the 2 seasons.
Data were collected via paper forms for cases attended by the basic team and via electronic patient care records (ePCR; MAMBU SRL, Reggio Emilia, Italy) for those attended by the enhanced team. Paper forms were deidentified and manually transcribed into an Excel spreadsheet, whereas ePCR data were exported directly. All records were merged chronologically into a single dataset. Collected variables included event date/time, patient age, gender, presenting complaint, evacuation method, disposition (ie, EMS, Helicopter EMS, private ambulance, or own vehicle), and administered therapies.
Data Analysis
We compared baseline characteristics between the 2 seasons to rule out significant differences. In Season 2, we analyzed cases attended by ski patrollers vs the enhanced team to describe their respective activities. We then compared evacuation methods and patient disposition between Season 1 and Season 2 to assess the enhanced team's impact. Continuous variables were summarized as means and standard deviations. Normal distribution was assessed using the Shapiro-Wilk test and QQ plots. Nonnormally distributed variables were compared using the Mann-Whitney U test. Categorical variables were reported as counts and percentages and compared using χ2 or Fisher's exact tests as appropriate. All tests were 2 tailed with a significance threshold of P<0.05. Statistical analyses were conducted using Stata 17 (StataCorp, College Station, TX) and R (version 4.3.2; R Core Team, 2023; R Foundation for Statistical Computing, Vienna, Austria).
Ethics
This study was conducted in compliance with the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) checklist. 18 Ethical approval for this study was granted by the Comitato Etico Territoriale Lombardia 5 (Protocol 02-25, Milan, Italy) and all study procedures were performed in accordance with the principles of the Declaration of Helsinki.
Results
Patients
Of the 871 total rescues recorded, 595 (68%) met the inclusion criteria and were included in the study (Figure 2). The mean age was 40 y; most patients (89%) were on skis, whereas the remaining were snowboarding. Nearly all patients were rescued following a traumatic event (94%), with the remainder being assisted for medical conditions. Regarding injury patterns, the most common injuries affected lower limbs (55%), followed by upper limbs (26%) and traumatic brain injuries (7%), based on data from both seasons combined.
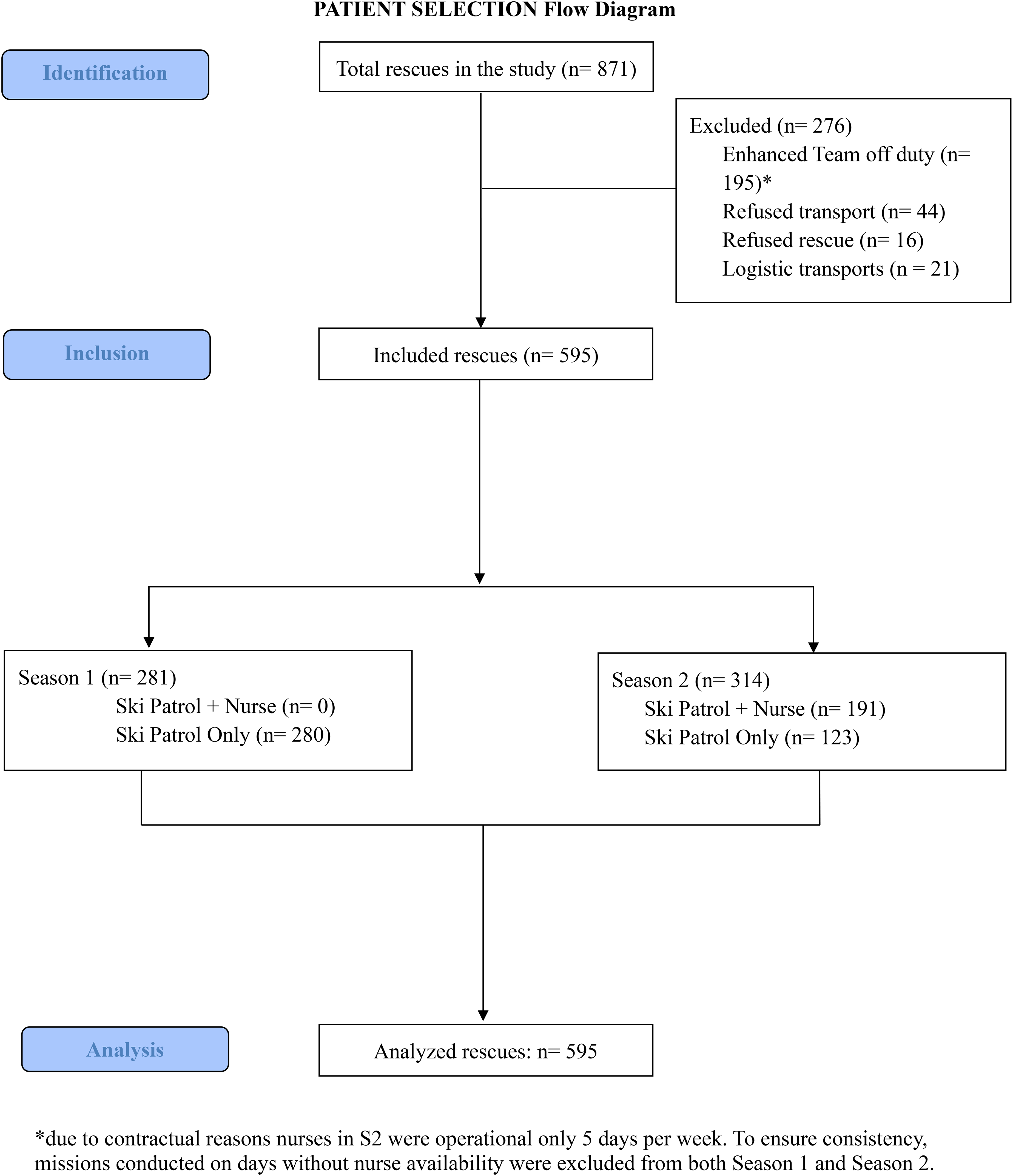
STROBE Flow Diagram of Patients Included in the Study.
A total of 281 patients were rescued during Season 1, and 314 were rescued during Season 2. Rescue operations were most concentrated between 1000 and 1400, with the peak occurring during the 1000–1200 time slot. The primary methods of activating the ski patrol were either through ski lift operators or other resort personnel or via calls placed by skiers to the regional EMS dispatch center (112), which then notifies the ski patrol. Additionally, some patients self-presented at the ski patrol hut. No significant differences in patients’ baseline conditions were observed between the 2 seasons (Table 2).
Demographic and Operational Features by Season.
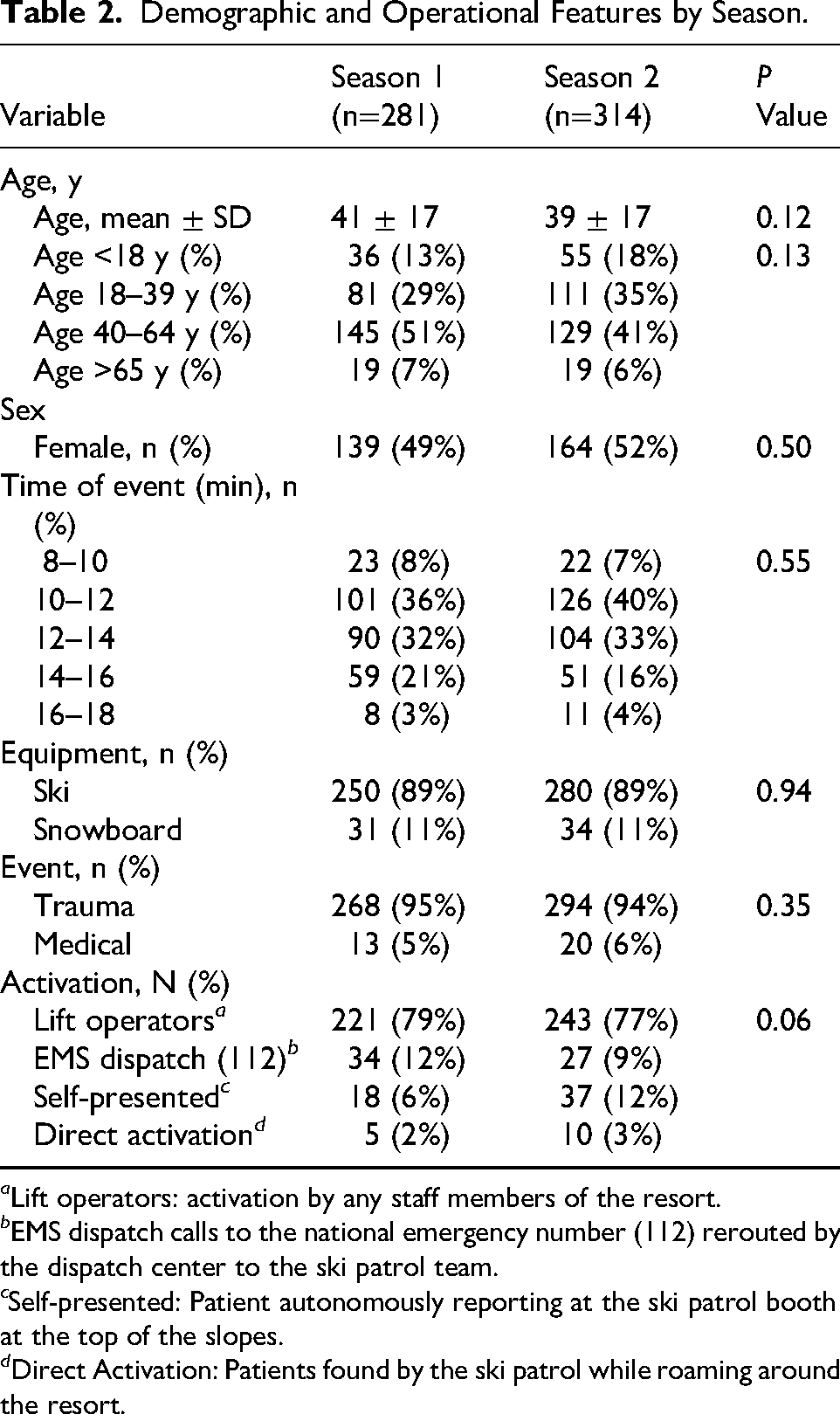
a Lift operators: activation by any staff members of the resort.
b EMS dispatch calls to the national emergency number (112) rerouted by the dispatch center to the ski patrol team.
c Self-presented: Patient autonomously reporting at the ski patrol booth at the top of the slopes.
d Direct Activation: Patients found by the ski patrol while roaming around the resort.
Activities
Among the 314 patients rescued during Season 2, 191 (61%) were managed by the enhanced team, whereas the remaining 123 patients were assisted by ski patrollers only. All patients in Season 1 were attended exclusively by ski patrollers. When comparing the use of the enhanced team vs the regular ski patrol in Season 2, the most reported injury was lower limb trauma, which also was the least attended by the former (P<0.01). The enhanced team was significantly more involved in assessing medical cases (P<0.01), and there also was a trend toward greater involvement in head trauma cases (9 vs 4%; P=0.06). No significant differences were observed for other trauma sites, including face, thorax, abdomen, upper limb, and spine. To further characterize head injuries and neurologic events, we analyzed the 21 patients with head trauma or related conditions during Season 2, 17 of whom (81%) were managed by the enhanced team. Most had mild presentations, with 82% diagnosed with concussion (Glascow Coma Scale score=15 in 88%), whereas seizures (18%) and transient loss of consciousness (12%) were less frequent (see online Supplemental Table A2).
The most applied treatment was splinting of fractures, and there was no difference between the 2 levels of attendance. The enhanced team implemented thermal protection more frequently than the basic team, although this was not significant. They were, however, significantly more likely to implement spinal precautions (12 vs 2%; P<0.01) and perform helmet removal (4 vs 0%; P=0.02).
Oxygen and pharmacologic interventions were administered exclusively by the enhanced team. A total of 51 patients (27% of all attended by the enhanced team) received at least 1 pharmacologic therapy, and 3 patients required oxygen. Details are presented in Table 3.
Events, Treatment, and Therapy During Season 2 by Team Attendance.
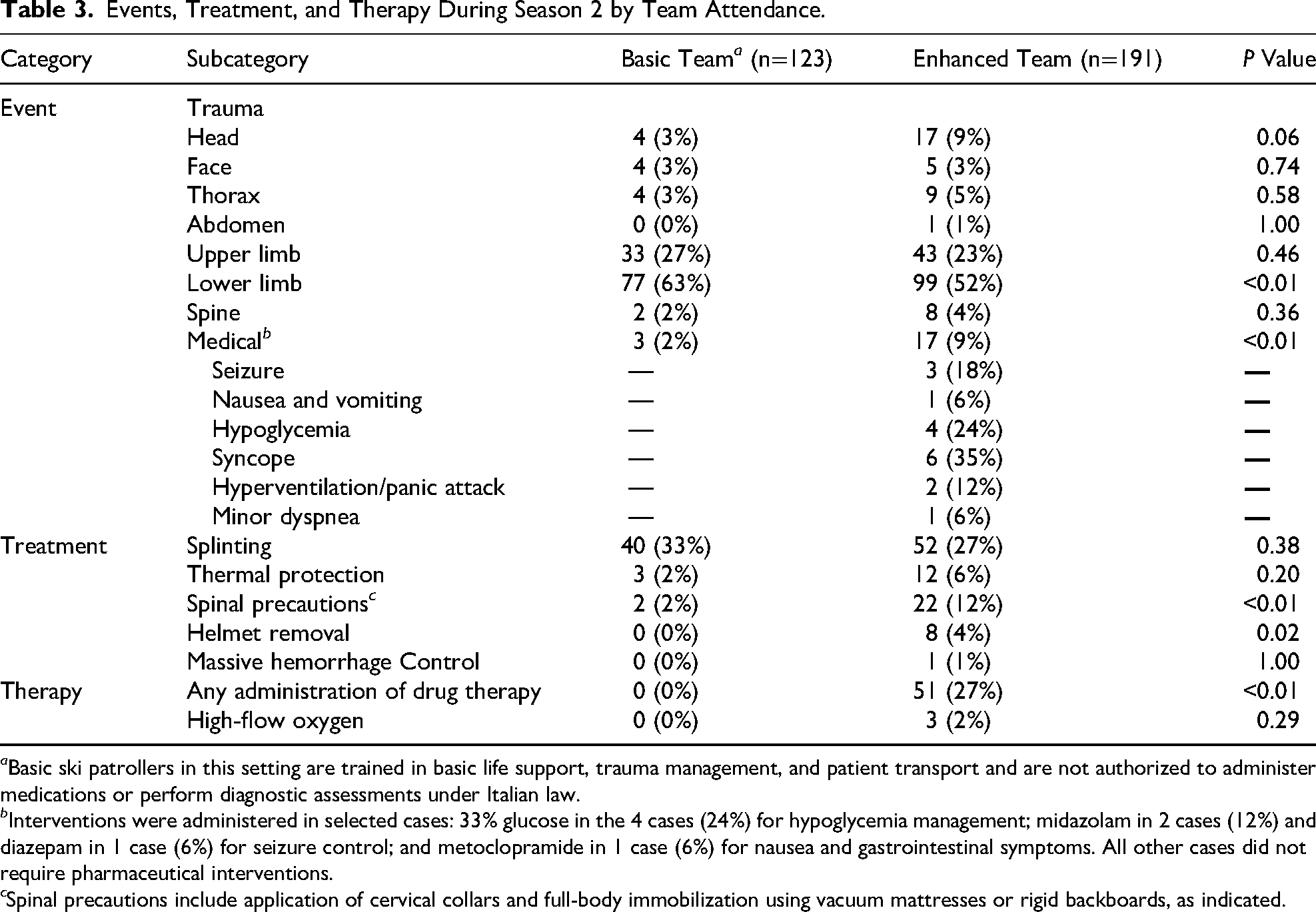
a Basic ski patrollers in this setting are trained in basic life support, trauma management, and patient transport and are not authorized to administer medications or perform diagnostic assessments under Italian law.
b Interventions were administered in selected cases: 33% glucose in the 4 cases (24%) for hypoglycemia management; midazolam in 2 cases (12%) and diazepam in 1 case (6%) for seizure control; and metoclopramide in 1 case (6%) for nausea and gastrointestinal symptoms. All other cases did not require pharmaceutical interventions.
c Spinal precautions include application of cervical collars and full-body immobilization using vacuum mattresses or rigid backboards, as indicated.
Therapy
A total of 66 drug administrations were performed in the 51 patients receiving medical therapy during Season 2. Analgesia was the most common intervention, with oral transmucosal fentanyl citrate (OTFC) used in 32 cases (48%). Other analgesics used were ketorolac both intravenously or orally (17%), acetaminophen both intravenously or orally (8%), LIVOPAN (6%; Linde AG, Pullach, Germany), and oral ibuprofen (3%). Eleven patients received combination therapy, most commonly OTFC with oral ketorolac. Intravenous access was generally avoided due to environmental constraints, such as low temperatures and time pressure, and used only when clearly indicated (eg, significant trauma or prolonged extrication). Carrying multiple analgesic options allowed the nurse to adapt pain management to injury severity, expected evacuation time, ambient temperature, and feasibility of intravenous access in challenging alpine conditions. Additional medication classes were administered based on clinical indications. These included a 33% glucose solution (6%) for hypoglycemia management and midazolam (3%) and diazepam (2%) for seizure control, all of which were attributed to presumed medical rather than traumatic causes, and metoclopramide (2%) for nausea and gastrointestinal symptoms, and tranexamic acid (2%) for hemorrhage control. A breakdown of the administered medications is provided in online Supplemental Table A3.
Outcomes
In both seasons, the most common evacuation method was ski lift (ie, gondola), accompanied by ski patrol, and followed by snowmobile and toboggan. Snowmobile use increased significantly from 49% in Season 1 to 62% in Season 2 (P<0.01), whereas gondola and toboggan use remained stable. Most patients required at least 2 transport methods.
Regarding disposition, transport to private trauma clinics decreased from 60 to 48% (P<0.01), whereas the proportion of patients who did not require hospital transport and left by private means rose from 5 to 11% (P<0.01). HEMS transfers remained unchanged (5% in both seasons; P=0.81). Details are presented in Table 4.
Evacuation and Disposition by Season.
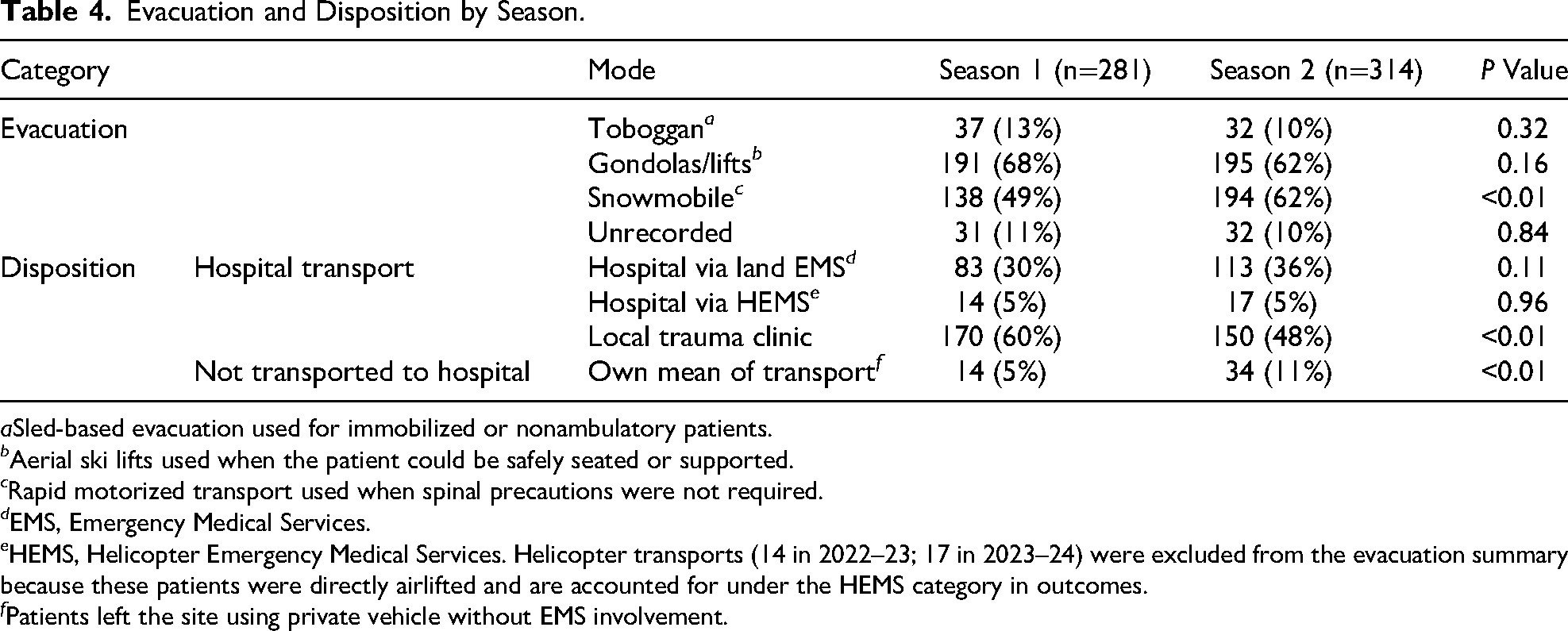

aSled-based evacuation used for immobilized or nonambulatory patients.
b Aerial ski lifts used when the patient could be safely seated or supported.
c Rapid motorized transport used when spinal precautions were not required.
d EMS, Emergency Medical Services.
e HEMS, Helicopter Emergency Medical Services. Helicopter transports (14 in 2022–23; 17 in 2023–24) were excluded from the evacuation summary because these patients were directly airlifted and are accounted for under the HEMS category in outcomes.
f Patients left the site using private vehicle without EMS involvement.
Discussion
This pilot retrospective observational study evaluated the impact of a healthcare-enhanced ski patrol team on the medical response to incidents at the Livigno Carosello 3000 Ski Area during the 2023–24 ski season. Outcomes were compared with those of the previous season, when only basic ski patrol teams were involved.
The main findings included 1) the enhanced team attended nearly two thirds of all cases during their operational hours, 2) trauma was the most common pathology and was regularly attended by both teams, but the enhanced team specifically focused on medical cases (P<0.01) and traumatic brain injuries (9 vs 4%; P=0.06), 3) the presence of the enhanced team enabled the administration of medical therapies, including early analgesia, and 4) the enhanced team's involvement facilitated on-slope triage, which may have improved evacuation time and methods.
Integration of Healthcare Professionals into ski Patrol Teams
Although evidence is mostly anecdotal,19–21 the inclusion of healthcare professionals in ski patrols has been hypothesized to enhance operational effectiveness. Being involved in a high number of cases, nurses frequently assumed leadership roles at the scene, acting as both first responders and clinical providers when appropriate. 22 In this capacity, their assessments of injury severity and triage decisions guided the initiation of immediate care protocols, subsequent treatments, and evacuation strategies. Additionally, nurses consistently collaborated with snow patrollers, actively participating in patient search, handling, and transfers, thereby directly supporting on-slope rescue efforts. Our deployment model was chosen to minimize time to clinical contact and enable early medical interventions at the point of injury. Alternatives such as stationing nurses at base or training patrollers to paramedic level were considered but are not permitted under the current Italian regulatory framework. Although our study was conducted at a single-base resort, this model could be adapted to larger ski areas through mobile or sector-based deployment of healthcare professionals. 16
Injury Patterns
Our case mix aligns with existing literature, identifying lower limb injuries as the most common on ski slopes.2,23 These occurred at similar rates across both seasons and were managed primarily by the basic team, reflecting both the high frequency and relative simplicity of lower limb injuries, which typically did not require advanced interventions. The enhanced team, while also treating isolated injuries, was more involved in cases requiring analgesia or complex triage or involving multiple injury sites. For instance, head injuries, which often demand specialized evaluation, were more frequently managed by the enhanced team.24,25
Pain Management
Effective prehospital pain management is particularly important in ski slope traumas, where evacuation may be prolonged. 26 Analgesia was the most frequent intervention given by the enhanced team, delivered using a multimodal, stepwise approach aligned with the World Health Organization analgesic ladder and guided by numerical pain scores. 27 Commonly used medications included OTFC, nonsteroidal anti-inflammatory drugs, and acetaminophen, administered alone or in combination. OTFC provided rapid analgesia without requiring intravenous access, an advantage in cold, remote environments.28,29 Intranasal administration, although noninvasive, may be less effective in low temperatures due to delayed mucosal absorption. 30 The team also had access to a portable cylinder of a 50:50 nitrous oxide-oxygen mixture that offered rapid-onset analgesia and was effective in both hospital and prehospital settings. 31
Impact of The Enhanced Team on Evacuation Procedures
The observed increase in snowmobile use (49–62%; P<0.01) likely reflects the integration of nurses into ski patrol teams, enabling more selective application of spinal precautions. Although traditional protocols employed by ski patrollers required full immobilization for suspected traumatic injuries—often resulting in slower toboggan evacuation—nurses were able to perform on-site cervical spine assessments using validated tools such as the NEXUS criteria or the Canadian C-Spine Rule. 32 This allowed timely identification of low-risk patients who could be safely transported via snowmobile, a faster and more resource-efficient method.
Although the enhanced team applied spinal precautions more frequently overall, this likely reflects their greater involvement in complex or high-risk cases, such as traumatic brain injuries. Simultaneously, their ability to clinically clear low-risk patients may have reduced unnecessary immobilizations in others, promoting more nuanced triage decisions and expedited evacuations.
However, attributing higher snowmobile use solely to team composition is interpretative because injury severity and operational factors also may have influenced transport decisions. Moreover, although structured decision tools were included in the enhanced team protocols, their use was not consistently documented, limiting retrospective evaluation of immobilization appropriateness. 33
On-Slope Triage, Patient Disposition, and Resource Utilization
The presence of the enhanced team enabled on-slope triage, which is crucial for rapidly categorizing patients by injury severity and matching them with the most efficient evacuation method. Mountain triage remains challenging due to hostile environments, limited resources, and varying levels of responder training. 34 Nurse integration, supported by dedicated triage protocols, can facilitate on-site decision making, improve communication with the Agenzia Regionale Emergenza Urgenza (AREU) EMS dispatch center, and ensure more appropriate allocation of rescue resources. 12
In Season 2, helicopter transport was reserved for life-threatening cases and transfers to the regional Level 1 trauma center, representing 5% of all ski area transports. Compared with Season 1, fewer patients were referred to trauma clinics, whereas more were discharged on site or left by private means, suggesting more individualized triage and resource use. This pattern aligns with prior findings that only 8% of winter resort patients meet objective criteria for helicopter transport, whereas provider judgment alone can lead to overtriage rates >85%. 35 Overall, patient disposition was influenced by both clinical and logistical factors, underscoring the value of structured triage protocols in optimizing EMS resource use in alpine settings.
Limitations and Future Directions
This retrospective study reflects a specific local setting and should be viewed as hypothesis generating. Several important descriptors—such as injury severity, clinical outcomes, use of protective equipment, and environmental conditions (eg, weather, snow, HEMS availability)—were unavailable, limiting generalizability. Fridays and Saturdays were excluded due to the absence of the enhanced team, introducing potential selection bias. It also should be noted that the enhanced team was not involved in all rescue missions, possibly due to operational constraints (eg, simultaneous incidents) or because certain cases were deemed not to require advanced medical support. No data were available in the dataset to clarify the rationale guiding team deployment. Another limitation is the use of different documentation systems (eg, paper forms for the basic team and ePCR for the enhanced team), which may have affected the level of detail recorded, particularly regarding interventions. This difference should be considered when interpreting group comparisons. Additionally, the lack of standardized decision-making criteria and consistent documentation in certain areas (eg, team dispatch and immobilization) reduces the ability to determine whether observed differences were due to team composition or to patient or contextual factors. Lastly, ski patroller training and scope of practice vary internationally; in our setting, basic ski patrollers are limited to basic life support, trauma management, and patient transport, whereas in other systems, they may perform advanced interventions. Future studies should adopt prospective designs with detailed patient-level data from the slopes through hospital discharge. Particular attention should be given to tracking patient disposition, including on-site discharges and transfers, to identify secondary transfers and better assess outcomes.
Conclusions
In conclusion, the integration of healthcare professionals, such as critical care nurses, into ski patrol teams has the potential to significantly enhance the medical response to on-slope incidents. This study suggests that the enhanced team was particularly useful in managing complex cases including medical events, administering early analgesia, and improving triage and evacuation procedures. Although traumatic injuries remained the most common, the presence of healthcare professionals allowed for a more comprehensive approach to patient care, potentially reducing time to definitive treatment and optimizing resource use.
Supplemental Material
sj-docx-1-wem-10.1177_10806032251389927 - Supplemental material for Transforming Emergency Care on the Slopes: A Study on the Integration of Nurses in Ski Patrol Teams
Supplemental material, sj-docx-1-wem-10.1177_10806032251389927 for Transforming Emergency Care on the Slopes: A Study on the Integration of Nurses in Ski Patrol Teams by Martina Longobardi, Federico Emiliano Ghio, Laura Leuci, Matteo Sala, Barbara Mantellini, Gabriele Perotti, Giulia Vinciguerra, Massimo Lombardo and Luca Carenzo in Wilderness & Environmental Medicine
Supplemental Material
sj-docx-2-wem-10.1177_10806032251389927 - Supplemental material for Transforming Emergency Care on the Slopes: A Study on the Integration of Nurses in Ski Patrol Teams
Supplemental material, sj-docx-2-wem-10.1177_10806032251389927 for Transforming Emergency Care on the Slopes: A Study on the Integration of Nurses in Ski Patrol Teams by Martina Longobardi, Federico Emiliano Ghio, Laura Leuci, Matteo Sala, Barbara Mantellini, Gabriele Perotti, Giulia Vinciguerra, Massimo Lombardo and Luca Carenzo in Wilderness & Environmental Medicine
Supplemental Material
sj-docx-3-wem-10.1177_10806032251389927 - Supplemental material for Transforming Emergency Care on the Slopes: A Study on the Integration of Nurses in Ski Patrol Teams
Supplemental material, sj-docx-3-wem-10.1177_10806032251389927 for Transforming Emergency Care on the Slopes: A Study on the Integration of Nurses in Ski Patrol Teams by Martina Longobardi, Federico Emiliano Ghio, Laura Leuci, Matteo Sala, Barbara Mantellini, Gabriele Perotti, Giulia Vinciguerra, Massimo Lombardo and Luca Carenzo in Wilderness & Environmental Medicine
Footnotes
Acknowledgments
We express our gratitude to Stefano Cusini and Luigi Viviani, respectively, general manager and technical director of the Livigno Carosello 3000 Ski Area, and the entire team for their strong belief in this project. Their investment of time and resources in strengthening the team and their collaborative support with data and expertise in ski patrol operations have been invaluable.
Consent to Participate
Retrospective observational research performed by Istituto di Ricovero e Cura a Carattere Scientifico is waived from the requirement of obtaining informed consent, as specified under the Italian Data Protection Code (Legislative Decree No. 196/2003) and the General Data Protection Regulation (GDPR), when the research involves data that are anonymized and do not involve any intervention with the participants. Because this study adheres to these legal and ethical standards, informed consent is not required.
Author Contribution(s)
Disclosures
FEG owns shares of I-Help SRL, the medical service provider of the Carosello 3000 enhanced team. The other authors have no conflicts of interest to disclose.
Availability of Data
All data generated or analyzed during this study are included in this published article (and its online Supplemental Files).
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
