Abstract
Mycobacterium marinum is an acid-fast bacillus. Human infection can occur when damaged skin is exposed to an aqueous environment that is contaminated by the organism. An infection with M marinum can present as painless purple nodules that spread along the lymphatics. Sporotrichosis presents similarly. We present a case of cutaneous M marinum infection in a patient from rural central Texas who developed lesions initially suspected to be sporotrichosis after she sustained a splinter wound of her right hand. Despite empirical treatment for sporotrichosis with itraconazole, the patient's condition worsened, prompting further investigation. A positive culture for M marinum altered the treatment plan. After a course of minocycline, the patient's cutaneous lesions resolved. This case highlights the diagnostic challenge of M marinum infections, which can mimic conditions such as sporotrichosis. M marinum is an incredibly slow-growing organism in culture and requires a high degree of foresight for accurate diagnosis. Clinicians should consider M marinum in the differential diagnosis for patients with apparent sporotrichosis lesions, particularly those with a history of appropriate environmental exposure, even in regions distant from bodies of water or occupations not routinely in contact with aquatic organisms.
Introduction
Mycobacterium marinum is an acid-fast bacillus that causes a tuberculosis-like illness in freshwater and saltwater fish. Human infection with M marinum can occur when damaged skin is exposed to an aqueous environment that is contaminated with this organism. As with a sporotrichosis infection, an infection with M marinum manifests clinically as painless purple nodules that can spread along the lymphatic system. Cutaneous sporotrichosis, caused by fungi in the genus Sporothrix, classically presents with painless erythematous papulonodular lesions that spread along the lymphatic system after exposure of damaged skin to the fungus. 1 Several microorganisms that can be acquired through environmental exposure can cause infections that clinically mimic cutaneous sporotrichosis. These include Nocardia (cutaneous nocardiosis), Leishmania (cutaneous leishmaniasis), Francisella tularensis (tularemia), and M marinum.2,3 We present a case of M marinum infection with an unusual etiology that mimicked the classical presentation of sporotrichosis.
Case Report
A 53-y-old woman presented to the emergency department complaining of a rash over the dorsum of her right hand and forearm. The patient reported that 3 wk prior she was walking outdoors with her dog, fell, and got a wood splinter at the metacarpophalangeal joint of her right fourth finger (Figure 1).
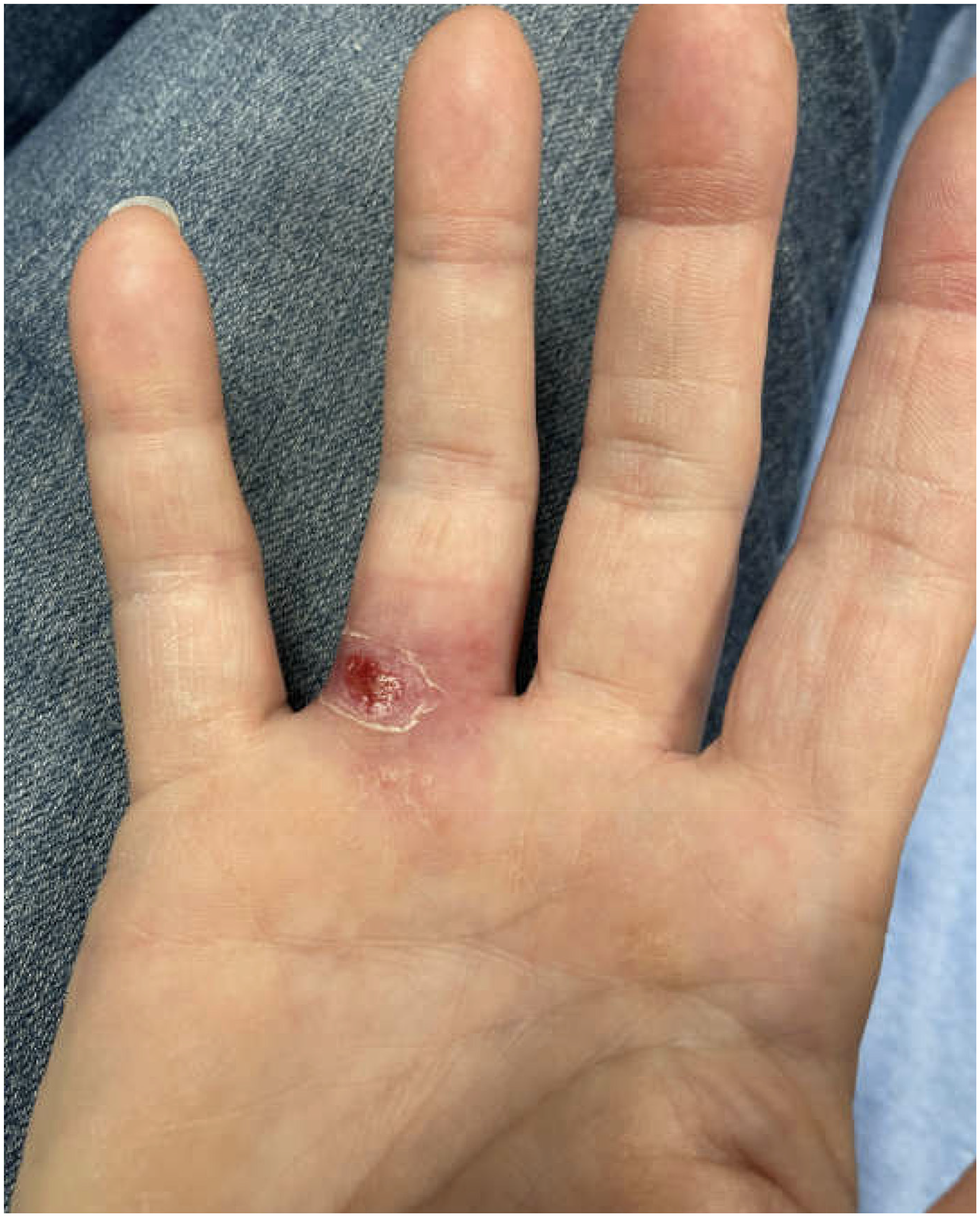
Nonhealing wound from a wood splinter in emergency department 3 wk after initial exposure.
She reported that the wound had not healed. The patient also reported that 2 wk after the fall, she noticed a painful, erythematous line that traveled continuously up her arm. The patient presented after developing erythematous nodular lesions that had progressed proximally up her arm over the past week. These nodular lesions were in a lymphatic chainlike distribution and were painful to touch (Figure 2).
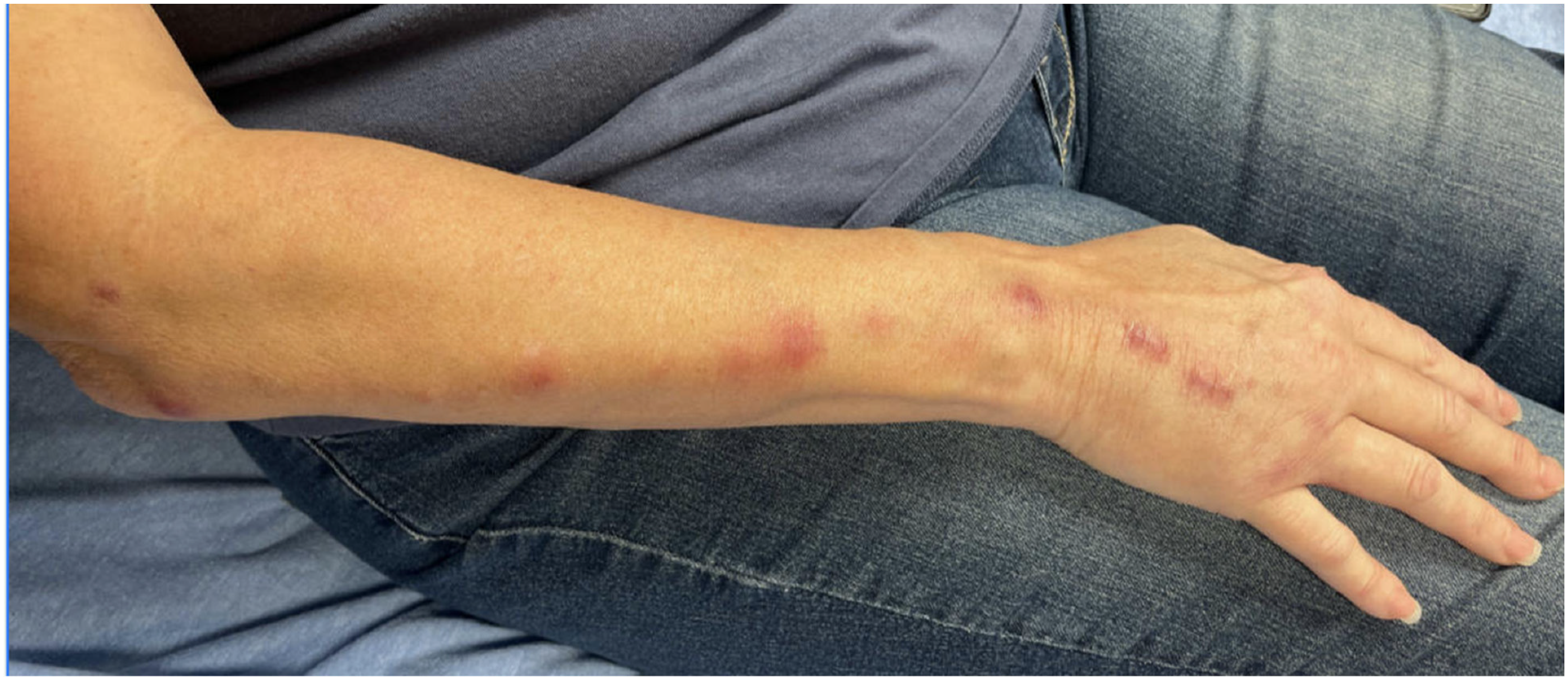
Cutaneous nodules tracking proximally up the arm in emergency department 3 wk after initial exposure.
The patient reported losing her appetite for 5 d before presentation but denied fever, chills, or other systemic symptoms. She also denied any history of recent travel. She reported living and working on a farm with chickens, dogs, cats, and horses. The patient reported taking amoxicillin at home without improvement. At that point, she decided to present to the emergency department. On examination, the patient was afebrile, hypertensive (blood pressure 176/89 mm Hg), and tachycardic (heart rate 106 beats/min). Otherwise, her vital signs were normal. The initial lesion was present over the palmar surface of the fourth finger, with surrounding erythema and edema (Figure 1), which were concerning for cellulitis. Additional erythematous tender lesions were present in a linear distribution along the arm (Figure 2). The remainder of the physical exam was unremarkable. The exam findings were consistent with possible sporotrichosis. The patient reported working with hay bales after the initial lesion, which aligned with an appropriate timeline for a sporotrichosis infection. Laboratory work-up, including a complete blood count and comprehensive metabolic panel, was unremarkable. Blood and wound cultures were collected. A right-hand x-ray showed no evidence of osteomyelitis or gas in the soft tissues. We consulted the infectious disease service. The consultant agreed that the most likely diagnosis was sporotrichosis and recommended treatment with itraconazole. The internal medicine service admitted the patient to the hospital for intravenous ceftriaxone treatment for the potential development of secondary cellulitis. Both infectious disease and dermatology services saw the patient on admission. Dermatology biopsied the lesions. In addition to intravenous ceftriaxone, the patient also was started on intravenous sulfamethoxazole-trimethoprim for potential Nocardia infection. Additional history obtained while the patient was in the hospital revealed that she had been exposed to farm animals and to fish tanks. The patient requested to be discharged the next day. She was instructed to continue the itraconazole and sulfamethoxazole-trimethoprim and to follow up within 2 wk with the infectious disease service.
The patient could not follow up 2 wk after discharge, and her subsequent visit was with her primary care physician 3 mo later. At that visit, the patient was still taking her course of itraconazole. However, the lesions had worsened and had spread proximally over her right arm (Figure 3). The patient continued taking itraconazole and sulfamethoxazole-trimethoprim. Her primary care physician urgently referred her to the dermatology service.
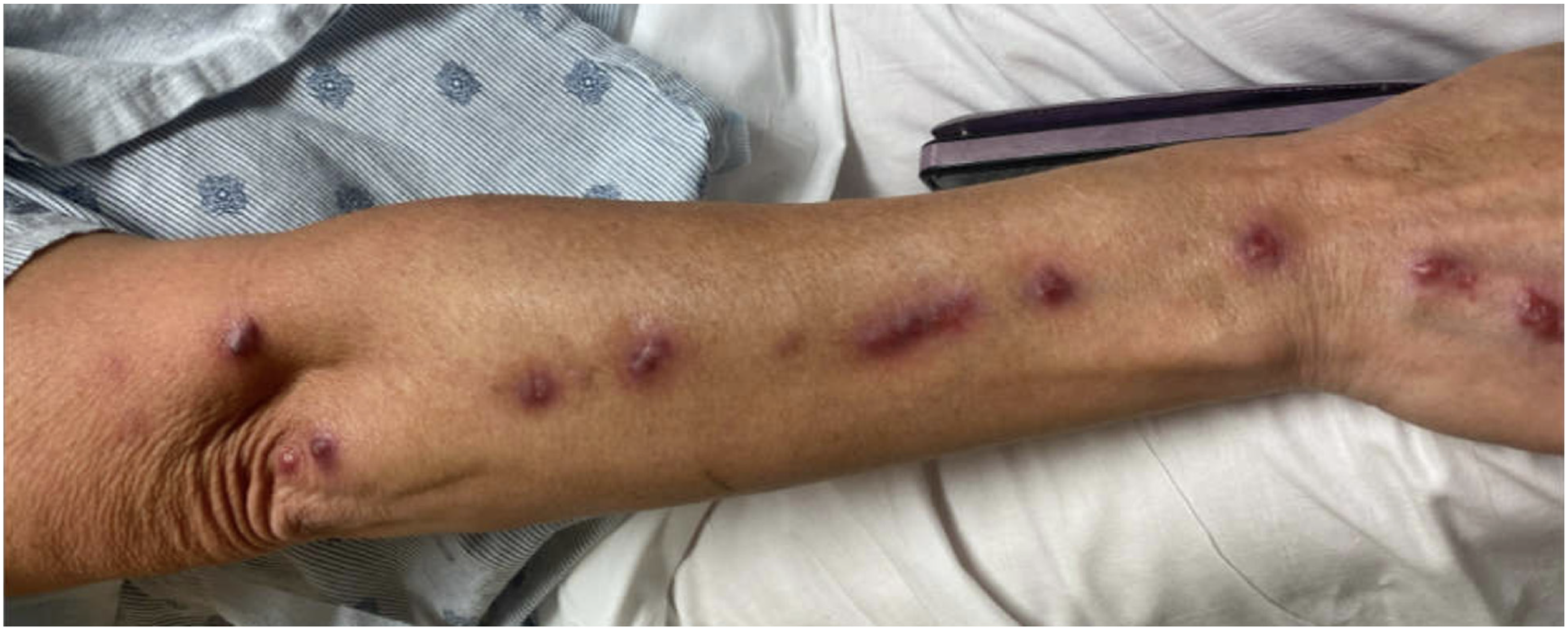
Lesions advancing proximally 3 mo after initial exposure.
Dermatology contacted the patient 1 wk later and informed her that the acid-fast bacillus culture collected on her admission date had grown M marinum after 3 mo. The patient was unaware of any aquatic exposures except cleaning her fish tank before developing the lesions. The dermatology service initiated a 3-mo course of minocycline.
After 1 mo on minocycline, the patient followed up with dermatology and reported significant improvement in her symptoms. Physical examination showed healing cutaneous nodules in a lymphatic distribution with improved erythema, pain, and nodularity. The dermatology service advised the patient to finish the 3-mo minocycline course and follow up. The patient did not return for dermatology follow-up. It is unknown if the patient completed the full 3-mo course of minocycline.
Discussion
Human infection with M marinum commonly occurs because of trauma in an aquatic environment that disrupts the skin barrier. 4 The disruption often can be subtle, like a small cut or abrasion that may be difficult for patients to notice or remember. 4 Historically, a common source of M marinum infections was from home aquariums or swimming pools, giving M marinum another name, “fish-tank granuloma.” 4 These cases have decreased as widespread chlorination and sanitation techniques have improved. Now, the most common mode of infection of M marinum occurs through contaminated aquariums and the handling of infected fish and shellfish. Infections with M marinum are rare. Most studies suggest that the incidence is between 0.4 and 1.3 per 1,000,000 individuals annually. 3
M marinum is an aerobic acid-fast bacillus that grows optimally in temperatures around 25 to 35°C. 4 M marinum is a very slowly growing organism. The incubation time ranges from 2 to 4 wk. Most human infections are confined to the skin, with rare cases progressing to tenosynovitis, arthritis, and osteomyelitis.5,6 There also have been cases of disseminated infection in immunocompromised patients.5,6 Most infections occur in immunocompetent patients and are susceptible to rifampicin, amikacin, tetracyclines, clarithromycin, and some quinolones. 4 Currently, there are no definitive guidelines for treating M marinum infection. 7 Antibiotics, given either as monotherapy or in combination, are effective. In either treatment strategy, antibiotic therapy should be continued for 1 to 2 mo following resolution of the cutaneous lesions. 7 This results in a course ranging from 3 to 6 mo. 4
Diagnosis can be difficult and delayed because of the slow-growing nature of the organism, the rarity of the overall condition, and the variable nature of the presentation. Cutaneous plaques, papules, or nodules (with or without ulceration) typically appear after the incubation period of 2 to 4 wk. 4 Cutaneous lesions in a sporotrichoid pattern are observed in up to a third of reported cases. 4 Lesions are normally painless. Systemic symptoms are usually absent. Accurate diagnosis can be made by history, physical examination, and bacterial culture. A major obstacle to diagnosis is the high degree of foresight needed because the organism is very slow growing. Cultures may not become positive for several months.
Conclusion
We present a case of an infection that started after the patient sustained a wound from a splinter outdoors. With a clinical presentation consistent with sporotrichosis, this was high on the list of differentials for the initial diagnosis. The patient lived in rural central Texas and worked as a farmer. Farmers are particularly susceptible to sporotrichosis because of the high risk of disruption of the skin barrier and exposure to soil, hay, and vegetation.8,9 Given the lengthy amount of time needed for a positive culture of M marinum and the potential for infectious progression, it is critical that the differential diagnoses for sporotrichosis-pattern cutaneous lesions, especially lesions in the upper extremities not responding to anti-fungal treatment, be broad to make a timely diagnosis. 10 M marinum should be included in the list of differential diagnoses even if the patient lives far from marine environments. If the patient has had an aquatic exposure, M marinum should be included in the list of differential diagnoses and a bacterial culture should be obtained.
Footnotes
Patient Consent
The patient provided written consent for her images and health information to be used for publication in medical literature.
