Abstract
Introduction
Frequent human–cattle interactions in high-density livestock regions expose farm workers to a significant risk of traumatic accidents, which range from minor to severe and life-threatening injuries. This study aimed to assess the incidence, mechanisms, and clinical impact of cattle-related injuries in a high-livestock-density area to inform preventive and healthcare strategies.
Methods
This monocentric retrospective observational study was conducted at Santa Croce e Carle Hospital, Cuneo, Italy, between January 1, 2018, and December 31, 2024. All patients aged ≥18 y presenting to the emergency department with cattle-related trauma were included. Injury severity was assessed using the Injury Severity Score (ISS), need for total-body computed tomography, intensive care unit admission, and 30-d mortality.
Results
A total of 182 patients (male:female ratio 4.5) were included, with a median age of 55 y (interquartile range, 45–64). The primary injury mechanisms were kicks (43.4%), charges (29.1%), and trampling (9.9%). Most cases (67.6%) were low priority at triage; 5.5% required intensive care unit admission. The median ISS was 1 (interquartile range, 1–4), and 3.3% had an ISS of >15. No trauma-related mortality was observed within 30 d.
Conclusions
Cattle-related injuries pose a substantial burden on farm workers and healthcare services; injuries range from minor to severe trauma. Given the high-energy potential of cattle-related impacts, improved safety measures and specific clinical management protocols are warranted to mitigate risks and enhance occupational safety in agricultural settings.
Introduction
Livestock farming represents one of the most significant economic activities in the province of Cuneo, a region in northwestern Italy characterized by a long-standing agricultural tradition. The area, home to 580,161 inhabitants, 1 hosts a substantial cattle population of 443,851 animals distributed across 3524 farms. 2 This high livestock density underscores the pivotal role of cattle farming in the local economy, providing employment for a considerable portion of the workforce and contributing significantly to both agricultural production and the food industry.
The close and frequent interaction between humans and cattle, particularly in the context of farming activities, inevitably carries risks. 3 Direct human–cattle contact during routine tasks such as feeding, milking, and veterinary procedures can result in traumatic injuries. These incidents can arise from accidental kicks, charges, trampling, and other unpredictable animal behaviors, which may be triggered by stress, fear, or environmental factors. Such injuries have the potential to range from minor abrasions and contusions to more severe outcomes, including fractures, head injuries, and, in rare cases, life-threatening trauma. 4
In the United States, agriculture is among the most hazardous occupations, with a fatal injury rate of 28.7 per 100,000 workers—8.5 times higher than the average across all other industries. 5 Injuries resulting from human–animal interactions represent a considerable risk, especially in areas where cattle farming is widespread. These incidents not only pose a direct threat to the health and safety of individuals working in the sector but also place a considerable burden on local healthcare services, particularly emergency departments (EDs) and Emergency Medical Services (EMS), which are often the first level of care for such injuries. Understanding the epidemiologic patterns and clinical consequences of bovine-related trauma is therefore crucial to designing effective preventive strategies and ensuring that adequate healthcare resources are allocated to address this issue.
This study aimed to assess the incidence and clinical consequences of cattle-related injuries in patients presenting to the ED. By analyzing the characteristics of these cases, the research sought to provide insights into the burden of bovine-related trauma, ultimately informing occupational safety measures and healthcare management strategies in regions with high livestock density.
Methods
This study was designed as a monocentric observational retrospective analysis, and it was conducted at the Santa Croce e Carle Hospital in Cuneo, in northwestern Italy, in the Piedmont region, between January 1, 2018, and December 31, 2024. The methodology followed the STROBE (Strengthening the Reporting of Observational studies in Epidemiology) Statement guidelines for reporting observational studies. 6 The Cuneo Hospital is a regional trauma center. We reviewed the medical records of all patients aged ≥18 y who presented to the ED during the study period. Only those with trauma resulting from contact with a bovine were enrolled. Patients were identified by entering specific keywords (eg, “cow,” “bull,” “livestock,” and “cattle”) into the hospital's electronic medical record system. Variables collected included sex, age, season of injury, mechanism of injury, triage level, mode of presentation to emergency services, pain scores, injury type, and disposition. The state of frailty related to comorbidities was described with the Charlson Comorbidity Index (a validated method of predicting mortality by classifying and weighting comorbid conditions). 7 To assess the severity of trauma, the following parameters were considered: number of patients undergoing total-body (CT) scans in the ED, the Injury Severity Score (ISS, a widely used anatomic scoring system that quantifies trauma severity by assessing injuries across multiple body regions), 8 the need for admission to the intensive care unit (ICU), and 30-d mortality.
In our setting, the decision to perform a total-body CT scan (ie, head, chest, abdomen, and pelvis) was based on the primary evaluation conducted in the ED, taking into account the mechanism of trauma, vital signs, laboratory tests, and first-level imaging findings (x-ray and point-of-care ultrasound) in accordance with Advanced Trauma Life Support guidelines. 9
Two independent reviewers extracted data from medical records. Discrepancies were resolved by consensus. Complete records were required for inclusion; no cases with missing key variables were included in the analysis. Statistical analysis was performed using R software (R for macOS X Cocoa GUI; R Foundation for Statistical Computing, Vienna, Austria). Normally distributed continuous variables were expressed as means and standard deviations; nonnormally distributed variables were expressed as medians and interquartile ranges. The normality of the distribution was assessed with the Shapiro-Wilk test, considering variables with a P value of <0.05 to this test as nonnormally distributed. Categorical variables were expressed as absolute number and percentage. The study was conducted in accordance with the Declaration of Helsinki and was reviewed and approved by the local ethics committee. The identity of the patients was kept anonymous, and the data were treated confidentially.
Results
A total of 182 patients were included in the study (Table 1), with a male:female ratio of 4.5. The median age of the cohort was 55 y, with an interquartile range (IQR) of 45 to 64 y. The incidence of injuries was distributed relatively uniformly across the seasons, with 24.7% of cases (n=45) occurring in spring, 26.9% (n=49) in summer, 27.5% (n=50) in autumn, and 20.9% (n=38) in winter. The most common mechanism of injury was kicks, reported in 43.4% of cases (n=79). Charges or headbutts were responsible for 29.1% of injuries (n=53), whereas trampling accounted for 9.9% (n=18). Most cases (67.6%; n=123) were classified as low priority at ED triage, 22.5% (n=41) as intermediate priority, and 8.8% (n=16) as high priority; 15.9% of patients (n=29) arrived at the ED via EMS. The median numeric rating scale score for pain on admission was 5 (IQR, 3–7). The median Charlson Comorbidity Index was 1 (IQR, 0–2).
Characteristics of the Study Cohort (N=182).
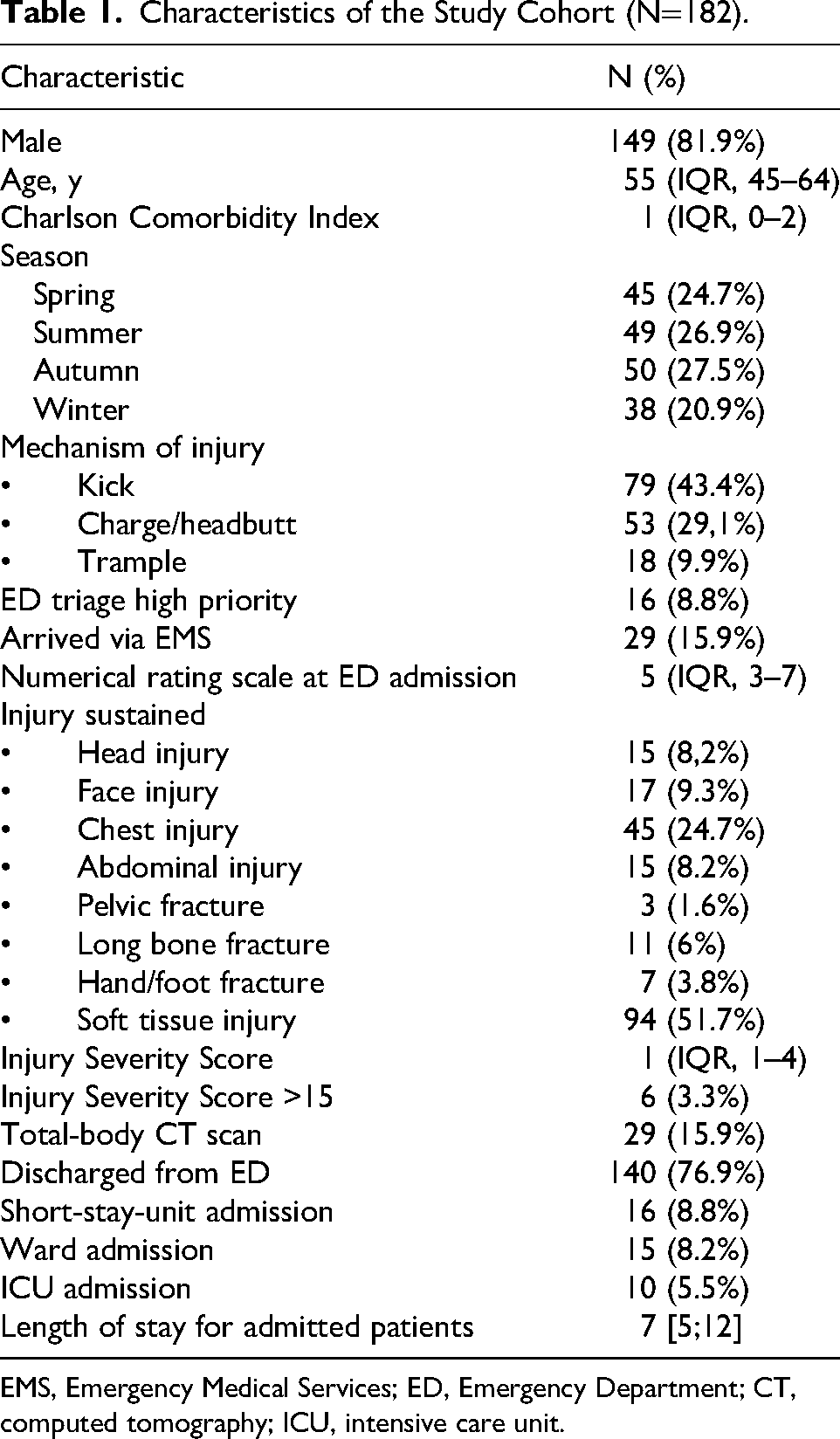
EMS, Emergency Medical Services; ED, Emergency Department; CT, computed tomography; ICU, intensive care unit.
Soft tissue injuries represented the most commonly reported type of injury, occurring in 51.7% of cases (n=94). Other injuries included chest injuries (24.7%; n=45), facial injuries (9.3%; n=17), head injuries (8.2%; n=15), and abdominal injuries (8.2%; n=15). Long bone fractures occurred in 6% (n=11), hand or foot fractures in 3.8% (n=7), and pelvic fractures in 1.6% (n=3). The median ISS was 1 (IQR, 1–4), and 3.3% of patients (n=6) had an ISS of >15; among the 6 patients with an ISS of >15, 66.7% (n=4) arrived via EMS. A total-body CT scan was performed in 15.9% of cases (n=29).
Most patients (76.9%; n=140) were discharged following evaluation in the ED. A total of 8.8% (n=16) were admitted to a short-stay unit for observation, 8.2% (n=15) were hospitalized in general wards, and 5.5% (n=10) required ICU admission. Among admitted patients, the median length of hospital stay was 7 d (IQR, 5–12). No trauma-related mortality was observed within 30 d of ED admission.
Discussion
The findings of this study highlight the significant burden of cattle-related injuries in a high-livestock-density area, emphasizing their impact on both occupational health and healthcare services. For instance, during the study period, the ED evaluated 69,595 adult trauma patients. Cattle-related trauma therefore accounted for ∼0.26% of all traumatic presentations, suggesting that although these injuries are relatively uncommon, they represent a recognizable and specific subset of rural trauma. The relatively high frequency of trauma among farm workers aligns with existing literature, which identifies livestock handling as a major occupational hazard in agricultural settings.
Regarding the demographic characteristics of our study population, the data consist primarily of male individuals in their prime working years. This aligns with figures from the Agricultural Registry of Piedmont, which estimate that ∼85% of farm owners are over the age of 41 y, with women accounting for less than a quarter of cases. This distribution confirms that our sample is representative of the broader agricultural workforce, which is predominantly composed of experienced, middle-aged individuals. Such demographic consistency strengthens the validity of our findings and highlights the need to focus preventive measures on this specific subgroup.
The occurrence of incidents does not follow a clear seasonal pattern, suggesting that risk factors are more closely linked to routine farming activities than to specific periods of animal reproduction. Tasks such as feeding, milking, and grazing pose more frequent injury risks than occasional breeding-related activities. This highlights the inherent dangers of daily agricultural work, underscoring the need for proactive safety measures. Regulatory bodies should develop and implement guidelines that account for livestock behavior, promoting tailored risk-mitigation strategies; one potential intervention could involve incorporating specific training on bovine-related injury risks into mandatory first aid courses for agricultural workers and rural communities, thereby raising awareness and promoting safer handling practices. Such measures could reduce the frequency and severity of livestock-related injuries significantly, enhancing occupational safety in agriculture.
As one of the largest case series on cattle-related injuries, our study presents some data consistent with previous studies, whereas others show discrepancies (Table 2). Male sex and an average age of around 50 y are common findings across most studies, reflecting the typical profile of livestock industry workers.4,10,12 However, a study on bull-related injuries conducted in India reported a younger patient population due to the fact that most incidents occurred during a traditional sporting event. 13
Summary of Findings From Studies on Cattle-Related Injuries.
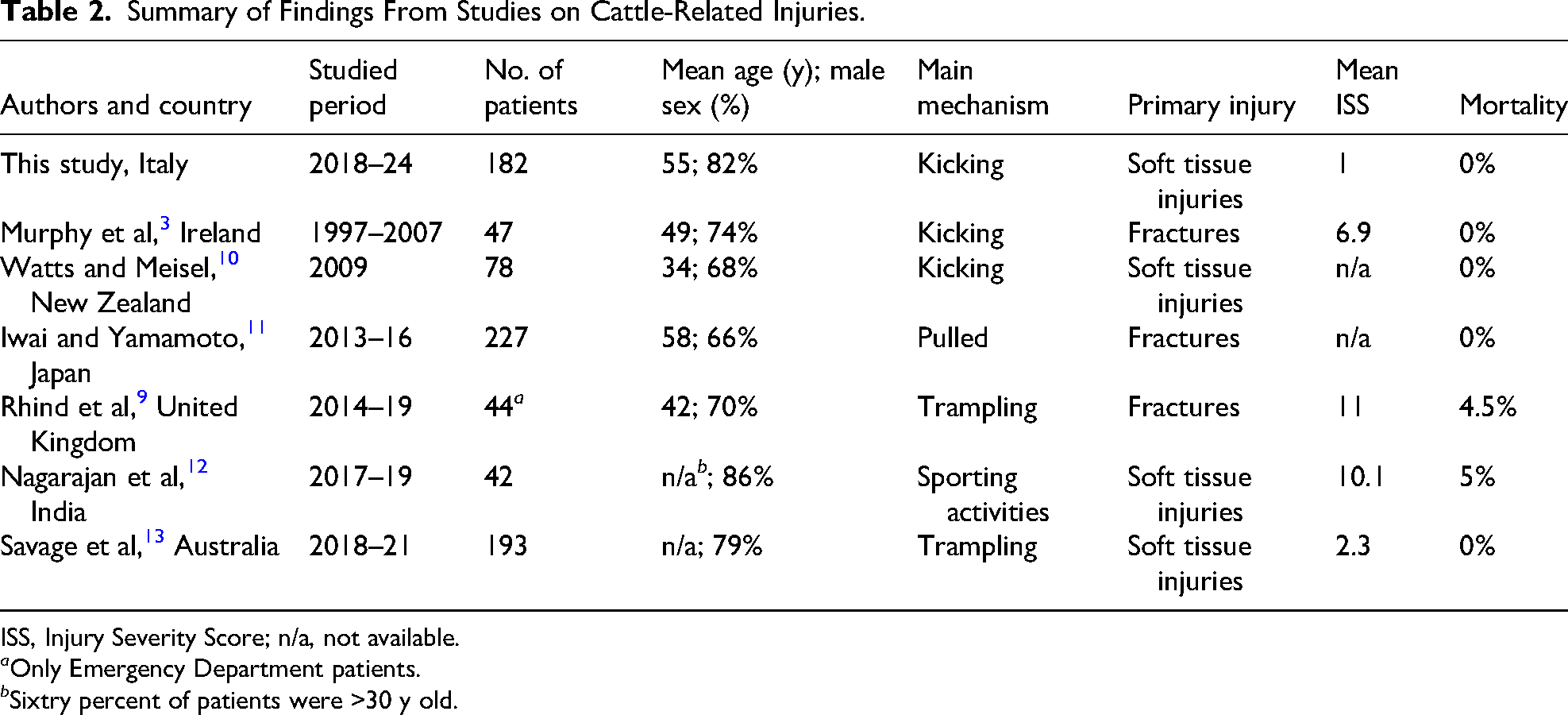
ISS, Injury Severity Score; n/a, not available.
a Only Emergency Department patients.
b Sixtry percent of patients were >30 y old.
In this study, kicking was the most common cause of injury, consistent with findings from Ireland and New Zealand.4,14 However, trampling was the leading cause in studies from the United Kingdom and Australia, suggesting potential differences in handling practices and cattle behavior across regions.10,15 Regarding injury patterns, soft tissue injuries were the most frequent type in this study, aligning with findings from India, New Zealand, and Australia.13‐15 Conversely, fractures were more common in Japan, the United Kingdom, and Ireland.4,10,12 The lower incidence of fractures in our cohort may reflect differences in farming practices, cattle handling techniques, or the average size and temperament of livestock. It is also possible that our cohort had a higher proportion of injuries resulting from defensive rather than aggressive interactions, such as kicks during routine handling, rather than full trampling or charges. Mortality remained low across all studies, with the exception of India (5%) and the United Kingdom (4.5%), likely due to higher ISS values and more severe injuries in these cohort.10,13
When assessing a patient with a cattle-related injury in the ED, it is essential to recognize that these animals often weigh as much as a car. Consequently, particularly incidents involving bulls or trampling should be classified as high-energy trauma, necessitating a high index of suspicion for severe injuries. Notably, a study of more than 1000 farm-related trauma cases found that most fatal incidents were associated with attacks by bulls or cows. 11 Additionally, a study conducted in Poland demonstrated that among a large cohort of patients presenting to the ED with animal-related injuries, the most severe cases were those caused by cattle. 16
Although this study was conducted in a regional trauma center with access to multidisciplinary teams and advanced imaging modalities, it is important to consider that many cattle-related injuries may present to smaller, nontrauma hospitals. In such settings, early recognition of the high-energy nature of certain mechanisms (eg, trampling and bull attacks) is critical. Prompt referral or transfer protocols to trauma centers may be warranted when clinical suspicion of polytrauma exists, particularly in the absence of whole-body CT capabilities or ICU support.
Limitations
Although this study included a relatively large case series for a topic that is underexplored, certain limitations must be acknowledged. As a single-center study conducted in a rural region of northwestern Italy, the findings may not be generalizable to other healthcare settings or geographic areas. The lack of precise standardization for classifying cattle-related injuries may have led to the exclusion of some cases despite a thorough keyword search in medical records; additionally, fatalities that occurred at the scene and injured individuals who sought initial care from their general practitioners could have been excluded from our analysis. Future studies integrating EMS intervention records could improve the accuracy and completeness of the collected data substantially. In addition, it is worth noting that cattle-related trauma represents only one category of farm-related injuries. Other frequent mechanisms include falls from height, machinery accidents, and exposure to chemicals. 17 However, due to the unique biomechanical profile and high-energy nature of bovine-related injuries, we chose to focus specifically on this trauma subset. Lastly, patients with incomplete records may differ from those with complete records in ways that could not be assessed in this study.
Conclusion
In conclusion, although the absolute frequency of livestock-related trauma is relatively low, their potential severity and unique injury mechanisms justify dedicated attention. Most injuries arise from routine activities rather than from exceptional events. Although many cases involve minor trauma, some incidents result in severe injuries requiring management strategies similar to those used for high-energy trauma. Given the substantial weight and unique characteristics of these animals, there is a clear need for heightened awareness, improved injury classification, and the implementation of specialized guidelines to enhance prevention and treatment.
Footnotes
Acknowledgments
The authors express their gratitude to Sergio Aimar for his valuable support in analyzing and understanding the demographics of cattle in our area. His contribution has been highly valuable to the development of this study.
Author Contribution(s)
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
