Abstract
Introduction
With point-of-care ultrasound (POCUS) use in austere environments comes the challenge of having an ever-available coupling medium for image generation. Commercial gel has numerous drawbacks that can limit its utility in these settings, and no studies have evaluated the potential for a reusable coupling medium. This study aimed to determine whether 3M™ Defib-Pads could be utilized as a reusable alternative to commercial gel for image generation in resource-limited settings.
Methods
A descriptive, cross-sectional survey of Canadian physicians with POCUS interest was conducted to evaluate the interpretability of various POCUS images in a blinded fashion. Three anatomic regions (cardiac, abdominal, and nerve) were utilized, and image generation from the commercial gel and 7 Defib-Pad conditions were evaluated. These included pads that were 1) newly opened, 2) dirtied then rinsed, 3) air dried, 4) rinsed after being air dried, 5) frozen then thawed, 6) used in double thickness, and 7) used with a probe cover.
Results
Compared to commercial gel, 3M™ Defib-Pads performed similarly, with adequate image interpretability of up to 100% in some conditions. The exception was pads that had prolonged air exposure, which produced images that were never interpretable. However, subsequent rinsing of these pads with water resulted in restored image generation.
Conclusion
3M™ Defib-Pads were found to produce interpretable POCUS images under multiple environmental stressors and with different modalities of use, suggesting that 3M™ Defib-Pads can perform as a reusable gel alternative in resource-limited settings.
Introduction
Point-of-care ultrasound (POCUS) has become a very useful tool in emergency departments around the world. With improvements in the size, portability, and affordability of hand-held ultrasound devices, POCUS use has also increased in prehospital and wilderness settings.1–3 For an ultrasound device to produce images, it requires a coupling agent such as commercial ultrasound gel, and without this medium, a hand-held device quickly transforms into an expensive, bulky paperweight. In remote and low-resource settings where all equipment must be carefully selected for maximum efficiency, the potential loss of utility of a device is unacceptable. It is within these environments that several limitations of commercial ultrasound gel become apparent. Commercial gel is heavy and bulky, which makes carrying it on your person a much more cumbersome task, especially if using body heat to prevent the gel from freezing in subzero conditions. It leaves behind a wet-sticky residue, which is undesirable when clothing is limited, and the potential for hypothermia is a concern. It is also relatively expensive and has the added disadvantage of being a finite resource, which may be problematic if repeat or multiple scans are desired.4–7
Other studies have evaluated the feasibility of homemade ultrasound gel. While they significantly reduce cost, these recipes create products that still suffer from being finite, leave behind a wet-sticky residue, require preparation, and are bulky and heavy once made.4–7 Therefore, the search began for an alternative that would be easier to transport, ready to use, minimize residue, withstand environmental extremes, and, most importantly, have the potential to be reusable.
3M™ Defibrillator Pads, 2345N (Defib-Pads), were a logical option to investigate given their conductive nature, compact packaging, light weight, preexisting use as a medical-grade product, and structure that may lend itself to reusability. Of note, these Defib-Pads are created for use with traditional metal paddle electrodes and are not self-adhesive pads, meaning repositioning would be possible without undesired hair removal. Additionally, Defib-Pads are marketed as having a low potential for skin irritation and do not leave behind residue, suggesting that if they worked as a gel alternative, almost no clean-up would be required after image acquisition. Despite these promising qualities, it is worth noting that there are two main limitations to Defib-Pads: cost and availability. Currently, Defib-Pads cost roughly $7.50 each if bought in a box of 10, versus a 250 mL bottle of commercial gel that can be bought as cheap as $2.50. Additionally, Defib-Pads may not always be available for purchase due to supply shortages or limited baseline availability in various countries. Advanced purchase and storage may be required to ensure availability at the time of need. 3M™ Defib-Pads are marketed as a single-use product; however, when employed in an off-label context (POCUS) in resource-poor settings, their repeat use may be reasonable, especially when involving the same patient.
The objectives of this study were to (1) determine whether ultrasound images generated using 3M™ Defib-Pads would be interpretable and (2) explore the impact of various environmental stressors or methods of use on image interpretability.
Methods
Ethical Considerations
This study received approval from the Western Health Science Research Ethics Board.
Study Design and Population
This study was a descriptive, cross-sectional survey of Canadian physicians who are interested in and training in POCUS and are associated with the Canadian Association of Emergency Physicians Emergency Ultrasound (CAEP EUS) Committee.
The target population was Canadian physicians who subscribe to the CAEP EUS listserv. Approval was given to utilize this listserv by the CAEP EUS Committee Chair, who maintains and has regular communication through this e-mail list. Physician members of this listserv are interested in POCUS education, news, and research; however, they are not required to have any specific degree of POCUS training. Thus, it was felt that utilizing this listserv would provide a generalizable population of POCUS users while being able to presume these individuals could meaningfully answer the survey questions. Additionally, the 55 recipients receiving an email invitation to participate were also welcome to share the survey with their POCUS-inclined colleagues.
Image Creation
The ultrasound images used to create this survey had been previously created by a single POCUS fellow at Western University (London, Ontario) and were stored in the local commercially available cloud-based storage system (Qpath, Telexy Healthcare Inc.). All 24 scans were obtained from a healthy volunteer and generated using a Mindray ME8 (Mahwah, NJ) cart-based system with three standard probes: phased array 1–5 MHz, curvilinear 1–5 MHz, and linear 5–20 MHz. Images were initially created with the main goal of evaluating and documenting the idea of using Defib-Pads as a gel alternative for personal use in wilderness settings. Discussions with mentors resulted in the decision to create a formal study using the images.
A total of 8 different conditions were trialed. The first condition utilized Aquasonic 100 (Parker Laboratories, Inc., Fairfield, NJ), a commercial ultrasound gel. The remaining 7 conditions utilized 3M™ Defibrillator Pads, 2345N, 3 M ID 7000002724 (3M™ Health Care, St. Paul, MN) as the coupling agent and included the following: (1) newly open, (2) freeze-thaw, (3) dirt-rinse, (4) air-dry, (5) wet post air-dry, (6) double-thickness, and (7) probe cover. Following is a description of each condition.
The “freeze-thaw” condition involved placing an unopened Defib-Pad package in a standard kitchen freezer (−18 °C) for 8 h and was thawed prior to use. The “dirt-rinse” condition involved burying an opened Defib-Pad without packaging in a garden for 1 h before it was rinsed with tap water until no visible debris was present (Figure 1). The “air-dry” condition involved leaving an opened Defib-Pad without packaging on a towel for 4 h until it had lost moisture but had not become brittle. The “wet post air-dry” condition involved briefly rinsing this air-dried pad under tap water prior to use. The “double-thickness” condition involved two newly opened pads placed together to increase thickness. The “probe cover” condition employed two newly opened pads, one on the skin and the second between the probe cover (TIDI Shield MICK-P432, TIDI Products, LLC, Neenah, WI) and probe—essentially utilizing a probe cover as per usual protocol except replacing commercial gel with Defib-Pads (Figure 1).

(A) Probe-cover set up using Defib-Pads (not pictured: additional pad placed directly on skin), and (B) Defib-Pad as part of the “dirt-rinse” condition, during dirt exposure.
Each condition was used to image 3 anatomic windows to assess for interpretability across various tissue types and depths. These windows included the cardiac parasternal long axis, the hepato-renal interface, and the mid-forearm ulnar nerve. Both cardiac and abdominal scans consisted of 6 s clips, whereas the ulnar nerve scans were still images. Random letters were assigned to each condition and used to label the corresponding scans.
With respect to a utilization protocol, Defib-Pads were placed on the anatomic area to be scanned based on traditional anatomic landmarking and adjusted as needed to find the sonographic landmarks and areas of interest prior to clip generation. Translational movements of the probe were conducted as normal.
Data Collection
A 28-question survey was developed and reviewed by all authors of this study, as well as experienced research faculty. The survey was created in English on Qualtrics software (version: March 2023, https://www.qualtrics.com) and was open for data collection over a four-week period. Two emails were sent requesting study participation, with the second being a reminder e-mail one week before data collection would close. Data was collected during April 2023.
Outcome Measures and Analysis
Participants were surveyed to collect relevant demographic information, including their highest level of POCUS training achieved, their areas of practice (emergency physician, intensivist, family physician, internist, other), their work environment (academic, community, rural/remote), and the region (province or territory) in which they work. Respondents could select multiple options within each of: area of practice, work environment, and region of work, as applicable. They were then asked to review a series of 24 ultrasound scans, which were presented in an anonymized and randomized fashion. Participants were asked to make a dichotomous decision (interpretable or non-interpretable) on the quality of the scans.
For the purposes of this study, an “interpretable scan” implied all sonographic landmarks and anatomy were visualized with enough clarity and quality that clinical questions could be confidently answered. This was defined at the beginning of the survey, and further clarification was provided for each question. For example, the right upper quadrant scans were accompanied by the following prompt: “Is this right upper quadrant view interpretable (are you able to confidently tell whether or not there is free fluid in this clip)?” The ulnar nerve images were accompanied by the following prompt: “Is this ulnar nerve image interpretable (are you able to confidently identify the ulnar nerve, ulnar artery, and ulna)?” The cardiac scans were accompanied by the following prompt: “Is this parasternal long axis clip interpretable (are you able to confidently assess for pericardial effusion or LV systolic function)?”
It was clarified that the scan might not be complete (ie, not a full sweep of the entire hepato-renal interface) but could still be interpretable. If the participant found a scan to be uninterpretable, they would be prompted to elaborate on what made the scan uninterpretable (artifact, resolution, etc).
Descriptive Statistics
Demographic information and interpretability of each scan were calculated and presented using percentages. All data analyses were performed in SPSS version 29 (IBM Corp. Released 2022. IBM SPSS Statistics for Windows, Version 29.0. Armonk, NY: IBM Corp).
Results
A total of 39 responses were recorded; however, 5 participants provided incomplete responses to demographic or ultrasound scan questions and, therefore, were excluded from the final analysis. The demographics of the remaining 34 respondents can be found in Table 1.
Respondent demographics.
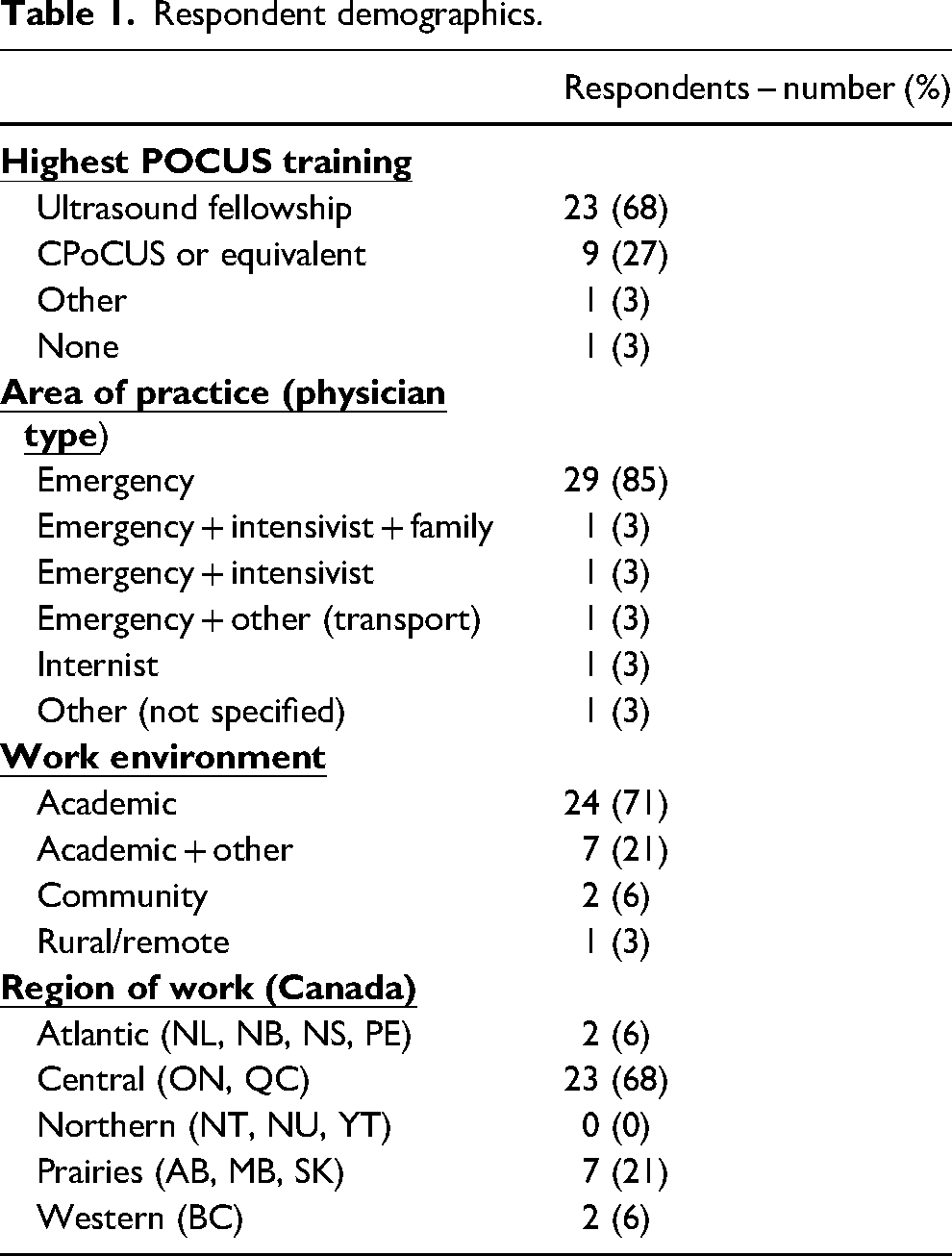

Both commercial gel and 3M™ Defib-Pads scans were rated as interpretable by the vast majority of respondents across all variables except for the Defib-Pad “air-dry” condition. With respect to the 7 Defib-Pad conditions, the following were interpretable by over 94% of participants across all three anatomic windows: newly open, dirt-rinse, and freeze-thaw. A direct comparison of the three anatomic windows across all eight conditions and the percentage of interpretability can be found in Table 2.
Percentage (%) of respondents who rated the POCUS scans interpretable from each anatomic window across each coupling agent condition.
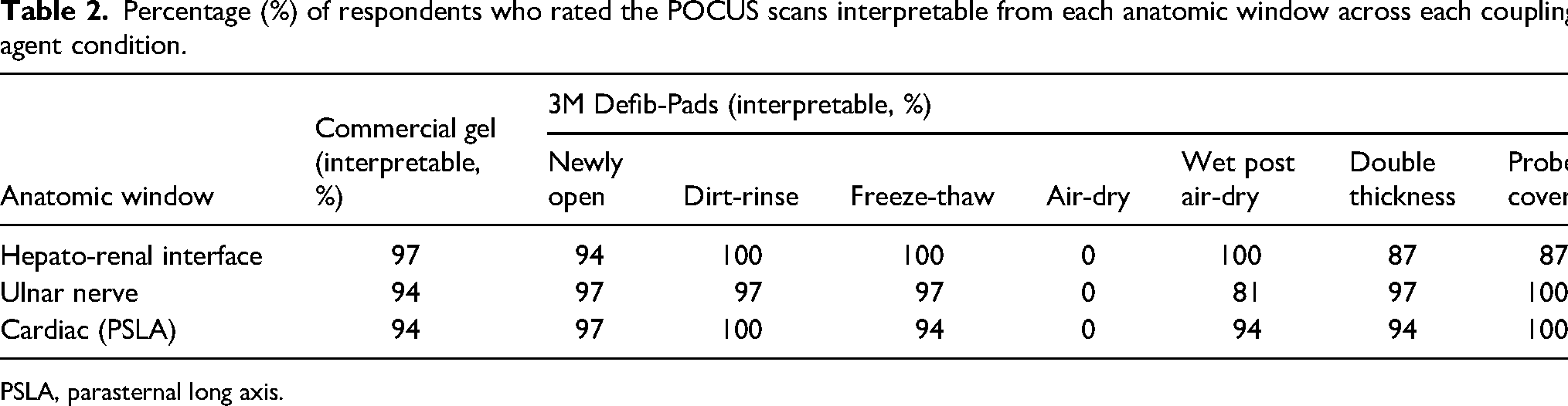
PSLA, parasternal long axis.
The air-dried Defib-Pads generated extremely poor images and were interpretable by 0% of respondents. Figure 2 provides a comparison of the images generated across all conditions using the ulnar nerve window. Comments pertaining to the uninterpretable scans were reviewed to determine what made images uninterpretable. For the ulnar nerve scans, most concerns were related to the scan being a still image or the respondent being unsure whether the nerve presented was indeed ulnar rather than there being concerns regarding image quality. In the hepato-renal interface scans, some participants commented on not seeing the full hepato-renal interface rather than image quality. For the cardiac scans, some rated the clip uninterpretable due to the view being incomplete but stated that the structures were interpretable.
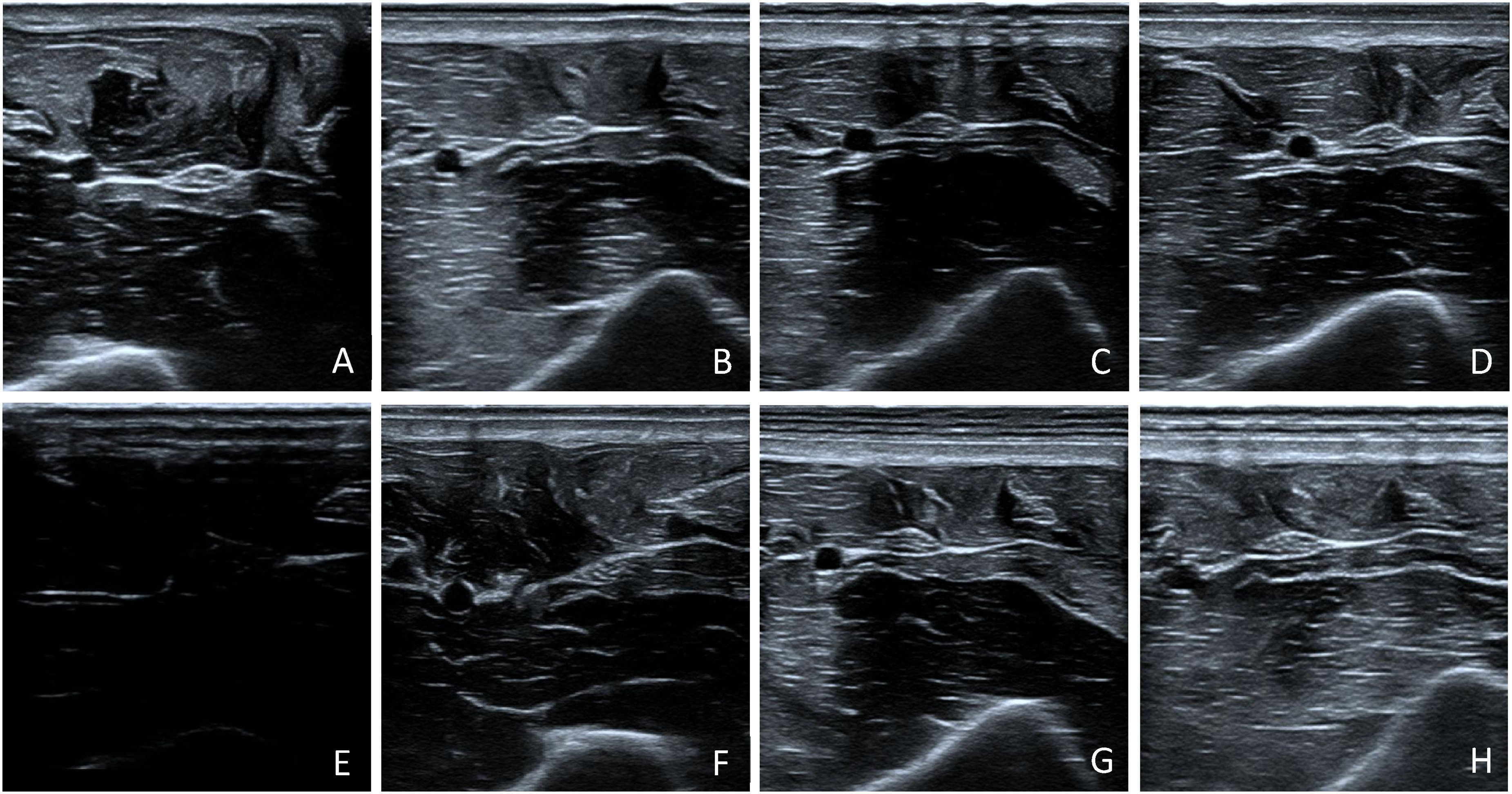
Comparison of the ulnar nerve images generated across all testing conditions. (A) commercial gel. B-H are all Defib-Pad conditions: (B) newly open, (C) freeze-thaw, (D) dirt-rinse, (E) air-dry, (F) wet post air-dry, (G) double thickness, (H) probe cover.
Discussion
Interpretation of Findings
This study found that 3M™ Defib-Pads can function as a coupling agent to produce interpretable scans, even when subjected to various environmental stressors or used in different applications, with one exception. The pads that were exposed to air drying never produced interpretable images. However, once these pads were rinsed with water, their ability to act as a coupling agent returned, and the images they generated were rated as interpretable by 81–100% of participants, depending on the anatomic window. With respect to all remaining conditions, 87–100% of participants rated the scans presented as interpretable across all anatomic windows.
At first, the results presented in Table 2 may provide the impression that Defib-Pads outperformed commercial ultrasound gel; however, this is not necessarily the case. What may seem like a large difference in percentage may actually represent the subjective opinion of one or two participants given the small sample size of the study. Also, the threshold for an “interpretable” image was relatively basic, including the ability to identify anatomy with enough clarity and quality that simple clinical questions could be answered (eg, a pericardial effusion, free fluid, or nerve identification). Additionally, no positive findings were included in the survey to determine the accuracy of the interpretation. It is more likely that using Defib-Pads on this single person created images that were good enough to answer basic questions. Had different body habitus, body hair, or variable anatomy been present or other scanning locations used (sub-xiphoid), these results may have been more skewed in favor of commercial gel.
Each Defib-Pad condition in this study was created with real-world exposure and application in mind. The “freeze-thaw” condition was included for mountaineering or freezing environments where the coupling agent should be able to survive those conditions with functionality intact. The “dirt-rinse” condition was included as Defib-Pads may be exposed to debris in wilderness settings and, if adequate debris removal is unattainable, then they pose a risk of 1) creating artifacts within the image generated and 2) potentially damaging the device's protective membrane. The “air-dry” condition was included because of the potential for prolonged air exposure either by accident or from performing multiple scans. If this exposure rendered the gel alternative permanently useless, then its practicality would be limited. However, if this deterioration in image quality could be restored using water, then this would strengthen the potential for Defib-Pads to be a reusable gel alternative, hence the “wet post air-dry” condition. The “double-thickness” condition was included because some anatomic regions or low BMI patients can pose a challenge to image generation in normal environments and require a larger volume of commercial gel for adequate coupling. Hence, a thicker Defib-Pad may be of benefit. The concern with a double-thickness pad is that air may become trapped between the two layers, causing impedance mismatching and making the image uninterpretable. The “probe cover” condition was included because the use of hand-held ultrasound devices in certain environments has the potential to damage the probe, and utilization of a probe cover may provide valuable protection in these contexts. Some examples may include salt water exposure in marine settings or small particulate exposure in desert environments.
Comparison to Previous Studies
A handful of studies have looked at various gel alternatives in both in-hospital and out-of-hospital settings. Cheap, homemade gel alternatives such as glucomannan powder, cornstarch, and cassava flour have been shown to produce adequate ultrasound images and are currently being employed in the real world with success.4–7 However, these require preparation with water and sometimes heat to create a gel that would be single use and must be used within days of creation. No reports currently exist of these mixtures causing damage to the ultrasound probe.
Other studies have evaluated premade, everyday products such as hand sanitizer, shampoo, and even maple syrup as gel alternatives.8,9 Although these mediums have produced adequate ultrasound images and clearly work in a pinch, they come with the downside of being single use and of limited quantity. When considering their use in the wilderness context, these mediums serve other important functions and are brought in small quantities; thus, they are not ideal to rely on as a long-term solution. Additionally, there is limited data to suggest these gel alternatives will not damage ultrasound probes in the long term. In fact, many manufacturers warn against utilizing certain hand sanitizers and cleaning agents with their products because of the concern of membrane breakdown. Furthermore, these studies have only evaluated gel alternatives at room temperature and without contamination. This may be acceptable when being used in a rural ED or clinic setting but is not as realistic for a prehospital environment.
Lastly, water has been shown to be a useful gel alternative when used for vascular access or as an immersion medium for digits.10,11 It has the benefit of largely being a ubiquitous resource; however, its lack of viscosity makes it more challenging for utilization in other applications such as FAST and cardiac views.
Clinical Implications
3M™ Defib-Pads show promise as a reusable gel alternative in POCUS when commercial gel is not available. Although this is off-label use, it may allow the continued use of POCUS in situations that would otherwise render the hand-held device useless and the sonographer unable to generate images that could change patient management.
Research Implications
Future studies would evaluate the use of 3M™ Defib-Pads as a reusable gel alternative on more than one individual with more than one sonographer. Ideally sonographers would be from various POCUS training backgrounds to assess for general usability. Additionally, further research should be done on whether these Defib-Pads could be cleaned or disinfected without compromising the pad's functionality and would thus allow for potential storage and use over multiple patients.
Limitations
There are a few limitations to this study. The ultrasound scans were generated using a cart-based system, which typically has better image quality at baseline compared to a hand-held POCUS device. Additionally, the scans were obtained on a single healthy individual, so image acquisition may not be generalizable to different body types or pathology. The scans were also all acquired by a single ultrasound fellowship-trained physician, and therefore, the ability to acquire images with this gel alternative may not be generalized to the average POCUS user. Lastly, this study also had a small sample size and suffered from a degree of selection bias, given the disproportionate number of respondents with POCUS fellowship-level training.
Conclusion
In conclusion, 3M™ Defib-Pads were found to produce interpretable POCUS images regardless of whether they were newly opened, subjected to environmental stressors (freezing, dirtying, and drying with rewetting), or employed in different ways (double thickness and with a probe cover). Images were uninterpretable after a period of air drying but regained their image acquisition ability after reexposure to water. Of note, the idea to use Defib-Pads was not intended to completely replace commercial gel or other gel alternatives but rather to provide a reasonable alternative where its properties may be favored over the existing options. This study demonstrated the potential for 3M™ Defib-Pads as a reusable gel alternative for POCUS in resource-limited settings.
Footnotes
Author Contribution(s)
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
