Abstract
The Wilderness Medical Society convened a panel to review available evidence supporting practices for medical direction of search and rescue teams. This panel included of members of the Wilderness Medical Society Search and Rescue Committee, the National Association of EMS Physicians Wilderness Committee, and leadership of the Mountain Rescue Association. Literature about definitions and terminology, epidemiology, currently accepted best practices, and regulatory and legal considerations was reviewed. The panel graded available evidence supporting practices according to the American College of Chest Physicians criteria and then made recommendations based on that evidence. Recommendations were based on the panel's collective clinical experience and judgment when published evidence was lacking.
Introduction
Wilderness search and rescue (SAR) is performed by a variety of organizations that exist to locate, access, stabilize, and evacuate subjects to a place of safety. Typically, in the vast regions of the American West, SAR agencies are smaller and volunteer based and work under the local sheriff's department to perform SAR services. The Mountain Rescue Association (MRA), founded in 1959, is an agency that accredits SAR teams in search; low- and high-angle rock rescue; and snow, ice, and avalanche rescue for ∼100 US and a few Canadian teams. The MRA does not provide specific certifications besides team accreditations and other than recommending cardiopulmonary resuscitation (CPR) and basic first aid training and does not give guidance for medical direction of SAR activities. The National Association of Search and Rescue, formed in 1972, provides a wide variety of training courses and certifications for individual rescuers and focuses on larger statewide responses. It does not currently provide recommendations regarding medical direction in its curricula.
Two reviews of SAR medical direction and capabilities in the western unites States (the Pacific Northwest region and the Intermountain region, respectively) demonstrated that nearly all teams (99%) had medically trained members.1,2 Only 34% of teams required medical training as a prerequisite for membership, with first aid and CPR the most frequently required certifications. These studies found that 84% of surveyed teams do provide medical care to lost and injured subjects both with and without the assistance of other Emergency Medical Services (EMS) or Health EMS agencies, yet less than half have physician medical direction. 2 Furthermore, these studies found that despite 77% reporting that they provide patient care alongside EMS, only 23% of teams reported joint training with local EMS.
While most SAR organizations in the United States rely on volunteers to provide the services, other countries and regions use career-based professionals to provide these services. Most of the developing world relies on the military for SAR, when available. Although the Wilderness Medical Society (WMS) is an international organization, given the heterogeneity of EMS services, healthcare, and insurance coverage worldwide, we will focus on the North American experience for these clinical practice guidelines.
In the United States there are hundreds of SAR organizations that cover a broad spectrum of rescue services including the US Coast Guard for open-water and coastal rescue services, the US National Park Service with both paid and volunteer rescue specialists, fire departments, state park rangers, state police, highway patrols, county sheriffs, and rescue squads, among many others. Our focus and the teams that will benefit the most from clinical practice guidelines regarding medical direction are the volunteer agencies that work under the various jurisdictional authorities but often operate independently as nonprofit organizations. Additionally, we will not address military, federal, or larger state-run SAR operations because they generally work closely with established EMS systems and work within their medical protocols. Similarly, we will not cover urban SAR (USAR) medical direction, although these and other WMS clinical practice guidelines may be useful to any of the organizations mentioned here.
In Canada, the vast majority of wilderness SAR is performed under the authority of Parks Canada, an agency similar to the US National Park Service. The rangers responsible for SAR undergo extensive training and preparation for their career-based activities. There are also several provincial parks and volunteer SAR teams in Canada to cover areas not serviced by Parks Canada. These volunteers have local medical direction, with Parks Canada having broader medical direction for the entire park system.
The limited SAR activities in Mexico largely fall under the purview of the Mexican military. The Mexican Navy operates 5 Estaciones Navales de Búsqueda y Rescate stations tasked with maritime SAR within 50 mi of the Mexican coast. The Mexican Army also conducts some air rescue activities. There are 5 national medium USAR teams in Mexico. There is a private nonprofit rescue organization (Los Topos de Tlatelololco) based in Mexico City that trains mostly for USAR given Mexico's history of natural disasters such as earthquakes. The Air Force Rescue Coordination Center aids with inland SAR in Mexico. Otherwise, there does not seem to be much organized inland SAR in Mexico.
Methods
The author group was identified in 2021 and consisted of representatives of the WMS SAR Committee, the MRA, and the National Association of EMS Physicians (NAEMSP) Wilderness Committee. The authors were identified by the WMS SAR Committee as experts in the topics of operational medical oversight, wilderness medicine education, and SAR organizations. The authors reviewed the literature for the best available evidence. Practice recommendations were assigned a level of evidence according to the methodology proposed by the American College of Chest Physicians. 3 The document is intended to provide guidance to current and potential medical directors of SAR teams, leadership of SAR teams and area jurisdictions, and regulatory agencies.
Definitions
SAR is a heterogeneous field with a great variety of environments and activities that may or may not be considered SAR activities. For the purposes of clarity and consistency in this document, the authors have agreed on the following definitions for which these guidelines apply. These guidelines are specifically intended for local and regional organizations with or without previous medical oversight. They may inform other military, governmental, or medical organizations whose primary function is not SAR but that may be working in a SAR capacity.
Providers, clinicians, and practitioners: First aid and the practice of medicine
In these clinical practice guidelines, we use the term clinician to refer to all healthcare categories sometimes historically referred to as providers. This convention follows the AMA Manual of Style, 11th Edition, in the general equivalence of these terms. 4 More particularly, it follows the AMA/AAMC Center for Health Justice, 5 the National Association of EMS Physicians, 6 Wilderness Medicine Magazine, 7 and the Western Journal of Emergency Medicine 8 —which cite accuracy and respect as their reasons—in privileging clinician for this conglomerate term, which most inclusively yet accurately captures caregivers who work in healthcare settings (including the wilderness). In the United States, all clinicians have some sort of license or certificate issued by the state for their practice level. For the purposes of these clinical practice guidelines and simplicity, we will refer to all these credentials as licenses regardless of the specific term the state uses to reference them. Typical examples would be emergency medical responder (EMR), emergency medical technician (EMT), paramedic, medical doctor (MD), and so on. These license levels and clinician types collectively make up the pathway by which medicine can be legally practiced in the United States.
We use the term practitioner to refer to the subset of clinicians who are licensed to provide direct medical decision-making patient care by a state with varying degrees of independence and without specific protocols and who have prescription-writing authority. This subset includes physicians (MDs and doctors of osteopathic medicine [DOs]), physician assistants (PAs), and various types of advanced practice registered nurses (APRNs).
All medical care delivered outside this framework, if delivered legally, is considered first aid. This also includes numerous certifications that include training but do not include state licensure. Typical examples would be wilderness first responder (WFRs), wilderness first aid (WFA), Stop the Bleed, and advanced wilderness first aid (AWFA). Such certificates do provide medical training but do not provide licensure to practice medicine; correspondingly, in practice and for these clinical practice guidelines, all certificates and practice types that do not carry a state-issued license to practice medicine (independently or in delegated practice) will all be considered first aid–level training regardless of the name or scope of the certificate. Some certificates have state-specific variation as to where they fall in this categorization. A few states, for example, Maryland, identify outdoor emergency care (the National Ski Patrol certification for their ski patrollers) as a state-recognized license, whereas the vast majority do not recognize it, putting it into the overall first aid category in those states.
SAR Organization
SAR at its core refers to the search for someone with the goal of rescuing them. Our literature review did not reveal consensus on one single comprehensive definition of SAR organization, but it appears that the concept is guided by three principal characteristics. First, the group should be organized, as in an organized group of people that operate in an organized fashion. Second, the group should possess a jurisdictional authority agreement to operate within its given location and in a mandated capacity. Third, the organization's goal is to provide location, stabilization, and evacuation of its subjects.
More specifically, SAR organizations exist to locate a person or persons in need of assistance in an environment that possesses a risk to them (generally an austere environment but occasionally an urban environment when the subjects are vulnerable as a consequence of their cognitive capacity or compromises to the urban environment in events such as disasters) and then access, stabilize, and evacuate them to a place of safety. This organization is made up of individuals who are proactively trained for and operate with the primary function of search and rescue. This responsibility typically ends with delivery of the subject to a transporting agency.
Most SAR organizations have a duty to respond that is established through a memorandum of understanding or other agreement with the authority having jurisdiction for SAR in a particular geographic or political region. This definition includes SAR organizations that are in whole or part organized and operated under their local EMS medical directorship.
Medical directors and advisors
A medical director is a state-licensed practitioner who provides medical oversight; their role is necessary if the services offered by the organization's clinicians include the activation of EMS-specific scopes of practice. 9 Such activation is important for clinicians at multiple levels, particularly the Basic Life Support (BLS) level. While it is sometimes maintained that BLS roles do not require or benefit from medical oversight, we feel that the opposite is the case. BLS clinicians (and first aiders) usually have the least amount of training that is measured in hours compared with other clinicians in the EMS or wilderness medicine realm and therefore would logically benefit the most from practitioner-level medical support. The role and qualifications of medical directors are often defined by state regulatory authorities. Medical directors hold practitioner licenses (usually an MD or a DO) and provide the traditional elements of EMS medical oversight. These include education, endorsement of organizational credentialing, quality management, and quality improvement of personnel holding licenses that require medical oversight for activation and the system in which they operate. The National Association of State EMS Officials, 10 consensus documents, 11 major industry textbooks, 9 and standard of care all indicate that every EMS system, including those with wilderness operations, should establish physician-led medical oversight.
The term medical advisor should be confined to situations where healthcare practitioner input is purely advisory and is not being used legally or operationally to activate or support EMS-grade protocols or certifications (ie, protocols or certificate levels that require state licensure/certification beyond the first aid threshold). 9 This includes the medical advisory role for outdoor experiential or adventure groups, summer camps, or fieldwork organizations, for example. A notable exception exists in federal government nomenclature. Both the National Park Service (NPS) and the US Forest Service (USFS) have EMS systems—with the NPS being in place since the origin of EMS in the 1970s and the USFS being very recently established in 2022. Currently, the USFS has a medical director (Dr Michelle Curry as of this publication) who provides national-level medical oversight. However, individual forests or collections of forest properties (within the USFS) and parks or collections of park properties (within the NPS) also have physicians who provide local medical oversight. Despite the fact that these practitioners operate in every way as medical directors, federal requirements result in their labeling as local emergency medical advisors. Advancing this terminology to remove the “advisory” component of this label is a medical oversight goal for practitioners working in these systems. 12
The concept that all SAR organizations should have a medical advisor or medical director is a key component of the theory of medically-directed rescue, a movement originating from the Pittsburgh EMS model for field medical care. 13 Such an approach provides for “a well-coordinated medical and rescue plan that allows for early patient assessment and interventions while extrication proceeds.” More generally, it implies that in the SAR world any subject with a medical condition is automatically a patient and that patient care considerations must direct all levels of a rescue, including the technical or extrication portions.
Medicolegal considerations for medical oversight
Medical directors should understand basic medicolegal principles such as the elements necessary for medical malpractice, rescue and abandonment, and the geographic variability of Good Samaritan laws. Because the majority of SAR personnel including medical directors are volunteers, it is often misinterpreted that Good Samaritan laws will protect the rescuers and medical director from malpractice claims. In general, these laws will immunize individuals who provide emergency medical care if there was no pre-existing duty to treat, no established doctor-patient relationship, no compensation or expectation of compensation, and no gross negligence has occurred. 14 These laws were conceived to encourage assisting others one may encounter who need medical assistance but do not generally apply to rescue teams or EMS agencies. Regardless of whether the medical director or rescuer is paid or volunteer, duty is established by virtue of their position as a public servant, and therefore, they have a duty to rescue. Some states, such as Oregon, have codified laws that specifically add language protecting volunteer rescuers, but in most jurisdictions, there is no difference between a paid or volunteer rescuer or medical director in terms of liability or duty to act.
Malpractice insurance
Although litigation involving medical care in SAR is uncommon, it is recommended that medical directors have adequate malpractice insurance. Malpractice coverage should be specific to the activity being performed and should also cover professional administrative liability. It is important to note that hospital or practice-based malpractice insurance does not cover medical direction of SAR teams or care delivered in the field unless specifically mentioned in the policy. There is only one company the authors could identify that offers this coverage individually at the time of publication. EMS medical director insurance is offered by the NFP Corporation, which is available through WMS membership.
Variations in SAR and EMS systems
There is a great deal of variation in the missions, operational environments, and membership makeup of SAR teams within the United States. On a state-by-state basis, SAR teams may operate under the auspices of sheriff's offices, fire departments, as independent county agencies, as regional intergovernmental units, or as not-for-profit organizations providing their services via delegation of authority from requesting governmental entities. Some states assign responsibility for SAR to their state police or natural resources agencies, whereas others rely on locally operated teams and others yet on private groups. Amalgamations of these models are common.
Similarly, the way traditional EMS services are provided varies dramatically throughout the United States as well. Regionally, service-delivery models include fire-based, hospital-based, privately operated, “third service,” public utility, and law enforcement–based EMS agencies. Adopted and registered as a certification mark by the federal government in 1972, the blue “Star of Life” symbol contains 6 geometric points that represent the 6 functions of an EMS system:
15
Detection of illness and injury Reporting of illness and injury to response agencies Response to report of illness and injury On-scene care of the ill and injured Care in transit to a receiving facility Transfer of the patient to definitive care
An entity involved in all 6 of these functions is most likely an EMS entity, but it need not fulfill all 6 functions to be considered involved in the delivery of EMS. The National Association of State EMS Officials holds that “the EMS system includes the full spectrum of response from recognition of the emergency to access of the healthcare system, dispatch of an appropriate response, pre-arrival instructions, direct patient care by trained personnel, and appropriate transport or disposition. Anyone participating in any component of this response system is practicing EMS.”
16
NAEMSP holds that “an entity that is involved with the response to provide medical care for ill and injured patients in the out of hospital setting constitutes an EMS service, regardless of whether patient transport is provided. EMS services may include, but are not limited to, emergency services call-taking and dispatch, ambulance services, mobile-integrated health services, and non-transport first responders such as fire departments, law enforcement agencies, search and rescue teams, and other first-responder/public safety agencies”. 17
There has been a great deal of controversy regarding the role of SAR teams in the provision of medical care and their relationship with traditional EMS agencies. A recent survey of NPS-affiliated SAR teams in the Pacific West of the United States demonstrated that nearly all teams had members with medical training (99%) and provided medical care (84%). 2 Yet fewer than half the teams reported having medical direction or oversight (45%), and only 23% reported joint training with traditional ambulance-based EMS agencies. 2
Echoing national organizations, Millin, writing for Hawkins, defines wilderness EMS as any entity that is trained, equipped, and holds themselves out as being able to provide any level of patient care at all in the wilderness. 9 Thus, a compelling argument can be made that SAR teams are participants in EMS systems, even if they do not meet the legal definition of an EMS agency within the regulatory framework of their operating environment. Because they are engaged in the delivery of EMS and patient care, SAR teams should operate under physician medical direction. 18
Roles for a physician medical director of a SAR team may include
Quality management Case review Protocol development Establishment of patient care standards Selection of appropriate medical equipment Credentialing of care providers Collection of patient follow-up and outcome information Liaison with the local and regional medical community
Medical direction
As in many areas of SAR, no empirical evidence or high-powered dataset in the North American region seems to exist to suggest the value of medical direction or advising in SAR organizations against the lack thereof. This recommendation comes from an expert opinion that is shared among leadership of various committees and groups extending beyond the WMS.
The NAEMSP released a position statement in 2010 referring to the need of medical directors for operational EMS programs that included wilderness SAR teams. SAR teams in North America in general are not required to be certified or licensed as EMS programs. However, the principle of functioning “within and not outside the mainstream healthcare system” in an effort to maintain established quality and continuity of care draws on the need for qualified medical directors. This should not be exclusive to EMS operations but should extend to SAR operations that function in conjunction with and to complement other EMS operations. Similar standards should be considered both for the benefit of the subjects/patients and also for EMS and SAR rescuers to perform at their optimal potential.
The purpose of these guidelines is to demonstrate the value of qualified medical direction for SAR teams in general. As this subdiscipline of wilderness medicine develops academically, data may continue to accumulate and support specific initiatives and value-based direction for these organizations and individuals involved.
Medical director qualifications, experience, and integration into operations
Medical directors of SAR teams should be physicians licensed to practice medicine in the state where the team operates. The 2012 NAEMSP document, “The Definition of EMS,” states that “EMS is the practice of medicine, and as such any of the activities that constitute EMS require oversight of a physician.” 16 This is further clarified by the NAEMSP 2017 document, “Physician Oversight of EMS Systems,” which states that “an entity that is involved with the response to provide medical care for ill and injured patients in the out of hospital setting constitutes an EMS service, regardless of whether patient transport is provided.” 17 Medical directors should be specialty trained in emergency medical services, emergency medicine, or at least a medical specialty that represents the broad patient base encountered by the team. 18 Medical directors should be familiar with the injuries and illnesses commonly seen in their team's operational environments and should have formal training and credentials in out-of-hospital operational medicine. Medical directors should maintain competency through continuing education specific to out-of-hospital medicine. Medical directors of SAR teams should be familiar with the regulations, laws, and political context regarding the practice of medicine and EMS in their jurisdiction. This necessitates a close working relationship with the local EMS system as well as the agency with responsibility for SAR within the jurisdiction. To ensure that oversight is provided according to best practices, medical directors should have formal training in medical oversight through either fellowship training in EMS or attendance at a national or local medical director's course such as the WEMS Medical Director Course, NAEMSP Medical Directors Course, or equivalent.11,18–20 Medical directors either should be experienced and actively engaged in field operations and training with their teams or should have a designated assistant or associate who is active in the field.17,21
Minimum level of training and certification for team members
Unlike other disciplines in healthcare that have well-established minimum educational and training requirements for licensure or certification to practice, there are no such standards that are applicable to members of SAR teams. Although individual rescue organizations may set their own rules for rescuer background and training such as BLS vs Advanced Life Support (ALS) certification, these rules may not be accepted outside the SAR organization or be legally recognized outside the state where the team is based. However, given the dramatic variation in environments, distance to care, and operational requirements specific to each SAR organization, setting a general recommendation for a minimum level of training that is applicable to all SAR groups is not practical.
Ongoing team medical training
In all medical settings, it is expected that skills and knowledge deteriorate over time. This has been demonstrated specifically in wilderness medicine with WFR training across providers of all levels. Even more notably, responders may overestimate their competence. 22 As leaders of their organization, SAR medical directors are tasked with the maintenance of their rescuers’ knowledge and skills, which requires ongoing engagement and training.
SAR rescuers are typically volunteers and have a variety of medical training and practical experience, so one of the challenges is focusing a limited amount of instructional and practical time on medical skills that are essential for rescuers. This may vary across regions and settings where high-yield injuries and emergencies also vary, for example, water-related injuries being more common in the Pacific Northwest than heat-related injuries. No one unified SAR medical training exists to provide such training, and for this again the medical director of each SAR program is saddled with the responsibility of overseeing in-house medical training specific to their program by identifying which skills are essential to maintaining and providing the training to ensure competence.
One such skill may be medical improvisation, as seen in the educational structure of the National Ski Patrol Outdoor Emergency Care course in which students spend a large amount of time in role-playing scenarios applying basic medical knowledge to a variety of problems. 23 This is one approach to teaching wilderness skills in a practical format rather than a classroom or video format such as standardized CPR training and can be used for ongoing training for SAR programs as well. However, as with the practical sessions in CPR training programs, scenarios do provide opportunity for instructors to provide real-time feedback and for students to recognize areas of deficiency in a safe setting that actively engages them in the learning process before they apply their general knowledge and skills in the field. 23
Provider scopes of practice
The National EMS Scope of Practice Model lists the following recognized levels of prehospital medical providers: emergency medical responders (EMR), emergency medical technician (EMT), advanced EMT (AEMT), and paramedic. Likewise, it has been proposed that the 4 levels of wilderness prehospital providers be recognized as wilderness emergency medical responder (WEMR), wilderness emergency medical technician (WEMT), wilderness advanced EMT (WAEMT), and wilderness paramedic. 21 Many volunteer SAR teams also include practitioners such as PAs, APRNs, and physicians. These individuals often serve as normal operational members of SAR teams who are trained and licensed as medical providers in their normal occupations. While PAs and APRNs are not normally part of the prehospital EMS community recognized and regulated by most states, it is important to realize that all the aforementioned medical providers have essential cognitive, psychomotor, and operational skills that may contribute to the success of SAR teams.
In keeping with the National EMS Scope of Practice Model, to function in their roles as members of SAR teams, recognized prehospital EMS providers must either be members of an EMS team sanctioned by the state having jurisdiction (which includes physician medical direction) or have a formalized individual medical direction arrangement with a physician. In many states, prehospital EMS providers operate under the license of their physician medical director. Independently licensed medical providers may operate within their scope of practice as defined by the state but should coordinate with and adhere to guidelines set forth by the physician medical director of the SAR team.
Medical education and certifications for rescuers
There is no minimum single standard of wilderness education or certification that is universally accepted for wilderness SAR. As the Acronym Reference Chart indicates (Table 1), there are multiple courses and certifications that may provide education and skills specific for SAR functions in a range of wilderness and austere environments. Numerous organizations have emerged that provide a variety of wilderness medical certifications and training offerings that span rescuer education and skill levels. These training opportunities and certifications are acquired through entities outside the SAR organization. Some programs are more established than others and may be subject to some variation in how they are implemented. Selection of the program or certification may depend on the participant's prerequisite medical education, particular roles or duties in SAR, and the degree of involvement in SAR. Of note, the legal recognition of these certifications and the differences in licensure and scope of practice requirements for rescuers are highly variable across state lines and must be determined on a state-by-state basis.
Acronym reference chart.
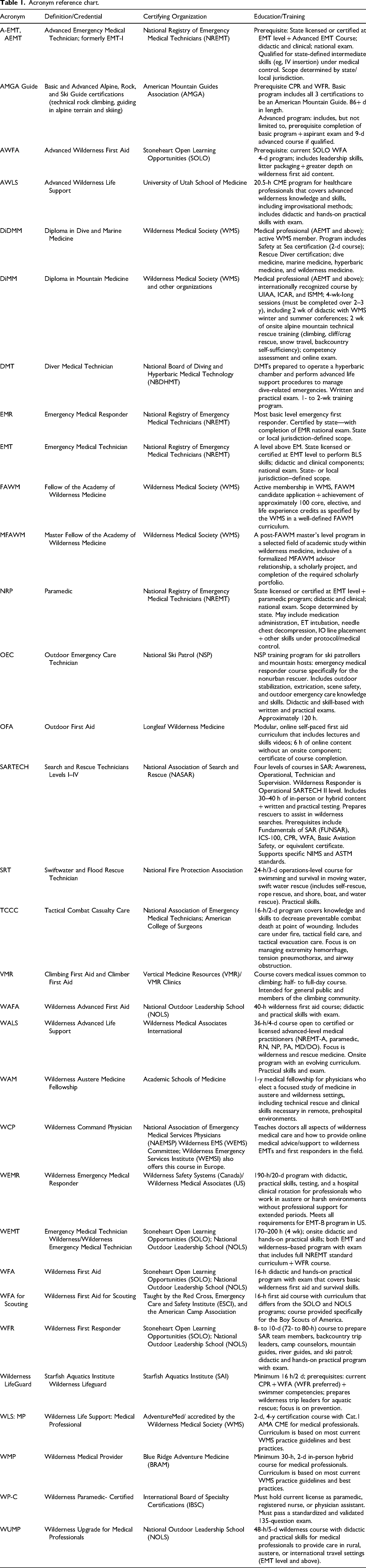
To decode and navigate the multiple acronyms used to describe the more widely encountered training offerings, Table 1 is provided as a reference. This table overviews the meaning of the acronym, identifies the certifying organization, and briefly summarizes the curriculum. Though not intended to be all-inclusive, the table lists the most common certifications and training programs available. Depending on the SAR team practice environment, one or more of these training programs and credentials may be needed to adequately prepare the rescuer to perform in the SAR role safely and effectively.
Expanded scope of practice vs operationally specific scope of practice
Scope of practice refers to what licensed healthcare providers at a specific level are legally allowed to do (the boundaries of their practice), not what they must do. The latter refers more to the standard of care, which involves the provision of care as another prudent individual with similar training and experience faced with a similar care situation would provide. This is often the tool employed in determining the quality of medical care. Scope of practice depends on education, certification, licensure, and credentialing. The scope of practice for the various levels of traditional EMS have been delineated. 24 The scope of practice for the various levels of WEMS also have been proposed. 21 Whereas scope of practice normally varies little at a certain level of certification or licensure within a given jurisdiction, the standard of care can vary greatly depending on the situation.
There are inherent complexities in WEMS vs traditional EMS, such as difficulty in accessing the patient, the need to carry all required equipment on one's person, concerns about exposure, and long evacuation times. For this reason, traditional EMS scope-of-practice restrictions applied to austere environments can significantly limit the delivery of quality patient care by adequately trained medical providers. Prehospital healthcare providers who operate in wilderness environments require specialized skills that go beyond those of traditional EMS. 21
For this reason, the concept of expanded scope of practice has developed in which the medical director trains and credentials the prehospital provider in the use of interventions that are normally limited to providers of a higher level of education or certification or that are not normally employed in the prehospital EMS environment. 18 Examples include the reduction of dislocated joints, the administration of antibiotics, the administration of topical anesthesia for eye injuries, and the advanced care of wounds. 21 The appropriate reduction and immobilization of a dislocated shoulder can allow a wilderness patient to ambulate and participate in their own extraction in a matter of hours. Otherwise, the pain of a dislocated shoulder can require a prolonged carryout that increases the risk to both patient and rescuer in terms of darkness, exposure, fatigue, and decision making. It is important to note that the operational needs in the wilderness are quite different from the needs in the traditional EMS environment. While expanded scope of practice may imply allowing a prehospital provider to do more than they would normally do, the term operationally specific scope of practice emphasizes delivery of the appropriate care for the operational environment. 18
Treatment protocols
Many EMS protocols exist for prehospital and ambulance services for EMR, EMT and paramedic levels. In many cases these provide an excellent model for a SAR organization that provides this level of care. The austere and environmental challenges of a SAR response, not typical in most ambulance-based EMS services, must be addressed prospectively because direct medical control is often impossible due to communication limitations in the wilderness. We recommend that medical directors use the same protocols, with specific exclusions/exceptions mentioned elsewhere, as the agencies receiving and transporting SAR patients to definitive care. The advantages of similar protocols and medication and equipment choices among agencies will simplify handoffs and communication.
Adaptation of general treatment protocols
One of the hallmarks of the remote, austere, and wilderness application of medical care, especially EMS-level medical care, is the need for operationally specific protocols. The historical advent of wilderness medicine and wilderness EMS schools in the 1970s was characterized by the use of existing EMS credentials (eg, EMT) with operationally and environmentally specific adaptations to their training curriculum.
This resulted in operationally or environmentally specific protocol changes. Some of the first of these were the NAEMSP Rural Committee's protocol recommendations for rural EMS published in 1991 and 1993, which were developed by early wilderness EMS leaders such as Peter Goth (whose work in this regard was configured as “rural” but extended into “wilderness”).25–28 These topics included environmentally specific adaptations to CPR (I), dislocation management (II), spine injuries (III), and wounds (IV). This groundbreaking work addressed topics that are still at the forefront of environmentally specific protocols today.
For example, it is widely understood that resuscitation in the wilderness will have different resources and potentially different endpoints. To illustrate this point, laypeople (and BLS personnel) are trained to perform CPR in cardiac arrest until exhausted, more advanced care arrives and care can be transferred, or pulses return. If pulses do not return after 10 min and no advanced care is likely to arrive rapidly, performing CPR until exhausted may put otherwise healthy individuals in danger in the inherently unsafe wilderness environment. It is also not realistic that patients will spontaneously regain pulses after an hour (or many hours) of CPR alone. Finally, in many scenarios where this action will be performed, the real danger is stress injury to survivors and bystanders, many of whom may personally know the patient. In this context, not only may the real patients increasingly become the other surviving individuals in the situation (including rescuers), but setting something subjective as the threshold for stopping CPR such as their own exhaustion when someone's life appears to be on the line invites excessive and potentially inappropriate effort. Considering all this, the WMS published practice guidelines recommending that CPR could reasonably be terminated after 30 min if ALS care was not rapidly available and there were no signs of life. 29 More recently, this guidance has been reiterated in even more specific wilderness environments such as drowning and aquatic emergencies. 30
Perhaps the most widely known and impactful environmentally specific changes have come in the realm of spinal injury management. Most of the surgical and emergency medicine world is familiar with the NEXUS (1998) and Canadian C-Spine (2004) studies, which provided evidence for selectively excluding patients from spinal immobilization. What is sometimes less well known is that the first published protocols on this topic came from the wilderness EMS community and the NAEMSP Rural Committee publication in 1993. About a decade later, the subsequent movement from spinal immobilization to spinal motion restriction and the corresponding principles of spinal cord protection also were heavily influenced by wilderness EMS medical practice. While recognition is growing that spinal motion restriction or exclusion of spinal cord protection is likely relevant for all field medical environments, originally, both the theoretical and operational concepts of spinal immobilization exclusion and spinal cord protection came from the wilderness EMS world and its environmentally specific pressures (specifically the difficulties of immobilizing and carrying out every patient).9,25–28
Other environmentally specific protocols such as dislocation reduction recognize the potential time delays in SAR patients reaching facility-based care or care from a clinician credentialed to perform reductions. Similarly, some operationally specific protocols recognize that an expanded scope might be needed for medications such as intramuscular epinephrine (for anaphylaxis) in remote or wilderness environments. It is worth noting that such measures are sometimes more welcomed by state regulators when they are cast as “operationally specific” protocols (which put the emphasis on the uniqueness of the environment) vs “expanded scope of practice” protocols (which put the emphasis on debates around scope of practice, which can be highly contentious). 21
Finally, from a common sense perspective, protocols need to address the realities of the operational environment of a SAR team, which may entail providing care in freezing temperatures, on cliff faces, or in the water. The modern consensus definition of wilderness medicine, rather than prioritizing time as the defining feature, privileges the environment and its obstacles, which emphasizes their importance.9,31
Online medical control
Online medical control is defined as the medical direction provided directly to out-of-hospital clinicians by the medical director or designee, generally in an emergency situation, either on scene or by direct voice communication. 33 SAR personnel should have the nominal ability to obtain online medical control for medical oversight to be exercised effectively, for patient care to be delivered safely, and for the SAR team to conform to standards of care as participants in EMS systems. 9
With the understanding that connectivity may not be possible on every wilderness response, SAR teams should establish mechanisms and clear policies for connecting with their medical director or designee via phone, radio, or satellite communication. These mechanisms should allow for effective, real-time, two-way communication of patient status, clinician concerns, and implementation of clinical orders. Such mechanisms are of particular importance when emergency care is predominantly delivered by first aid–level and BLS personnel given the limited nature of their training. 9
SAR teams also should establish mechanisms and policies for initiating a field response from their medical director or designee. These policies should consider information that would trigger an automatic response from a medical director as well as the process for requesting a follow-on response when personnel are already deployed and encounter a situation in which the presence of an on-scene medical director would be beneficial.
Quality management
The primary responsibility of a medical director is to ensure continuous improvement of the quality of patient care and to ensure that the medical activities of a SAR team are indeed patient centered. 17 To do so, they must be able to review patient care records and should be made aware of incidents in which patient care deviated significantly from established standards of quality. SAR teams should establish key performance indicators of clinical quality, ensure that each instance of the delivery of medical care is documented and that those records are accessible to their medical director, and establish mechanisms for alerting their medical director to incidents of concern. 34
Conclusions
The current landscape of SAR in North America is heterogeneous, with no universal structure for regulation or oversight. There are currently no established best practices for medical oversight of these teams. While the particular mission and scope of each team are unique, central to all SAR missions is caring for individuals in need of rescue, which predictably involves medical care. This group of experts has summarized the existing evidence and has proposed best practices regarding the medical direction of SAR teams to ensure that the best care possible is delivered to patients who require rescue by SAR teams in North America.
Supplemental Material
sj-pdf-1-wem-10.1177_10806032241249126 - Supplemental material for Wilderness Medical Society Clinical Practice Guidelines for Medical Direction of Search and Rescue Teams
Supplemental material, sj-pdf-1-wem-10.1177_10806032241249126 for Wilderness Medical Society Clinical Practice Guidelines for Medical Direction of Search and Rescue Teams by Christopher A. Davis, Cassie Lowry, Aaron Billin, Linda Laskowski-Jones, Alison Sheets, David Fifer and Seth C. Hawkins in Wilderness & Environmental Medicine
Footnotes
Author Contribution(s)
Disclosures
The authors report the following disclosures: AS is president of the Mountain Rescue Association; SCH is on the faculty of the Wilderness EMS Medical Director Course; and AB, CL, DF, LLJ, and CD have no disclosures to report.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
