Abstract
In this study among a longitudinal cohort of women living with human immunodeficiency virus (HIV) in Metro Vancouver, Canada (2014–2019), we used bivariate and multivariable logistic regression with generalized estimating equations to investigate associations between low, medium, and high relationship power and two outcomes among women in heterosexual relationships: (1) being on antiretroviral therapy (ART); (2) optimal ART use. Multivariable analysis suggested that high and medium relationship power were significantly associated with being on ART and optimal ART use. These findings suggest the critical importance of relationship power screening, strength-focused couples-based interventions and structural approaches to address gendered inequities, norms and HIV stigma.
Introduction
Worldwide, 30% of women ages 15 years or older have experienced intimate partner violence (Bows, 2016). According to the Canadian Centre for Justice and Community Safety Statistics, intimate partner violence is defined as: “all forms of violence committed in the context of an intimate partner relationship” (Cotter, 2021), which includes verbal/emotional violence, physical and/or sexual violence. Compared to men, women are overrepresented among people experiencing intimate partner violence in Canada. When discussing women's experience of intimate partner violence, Indigenous women as well as trans women and nonbinary persons as part of this population experience unique factors surrounding power and sexual violence that benefit from further contextualization. Indigenous women continue to experience ongoing and historical consequences of colonial violence and systemic oppression, including high levels of childhood and adulthood violence (National Inquiry into Missing and Murdered Indigenous Women and Girls, 2019), with prevalence of intimate partner violence being twice as high for Indigenous women (45%) as compared with non-Indigenous women (25%) (Heidinger, 2022). Though much of existing research focuses on the experiences of cisgender women, the Canadian Labour Congress survey reports that trans people are nearly twice as likely to report having ever experienced domestic or intimate partner violence (Bucik, 2016). According to Statistics Canada data, close to 50% of sexual minority women (lesbian, gay, bisexual) have experienced IPV in their lifetime, double that of heterosexual women (Jaffray, 2020).
Evidence suggests that >90% of women living with human immunodeficiency virus (HIV) have experienced intimate partner violence in their lifetimes (Orza et al., 2015). Extensive research further suggests a link between intimate partner violence and sub-optimal access to HIV treatment among women living with HIV (Hatcher et al., 2015; Kouyoumdjian et al., 2013; Trimble et al., 2013), while much less research has been done to understand the relationship between intimate partner violence and reduced access to other health services. Notably, intimate partner violence has been found to be associated with lower antiretroviral therapy (ART) use, decreased self-reported optimal ART use, and decreased likelihood of viral load suppression, as described in a global review of intimate partner violence and HIV (Kouyoumdjian et al., 2013). The ways in which intimate partner violence produces barriers to access to HIV treatment are complex. For example, aspects of needed HIV care including attending appointments, obtaining, and taking medications may serve as reminders of a person's HIV diagnosis and trigger aggression by an abusive partner (Kouyoumdjian et al., 2013). Women living with HIV experiencing intimate partner violence may need to choose between immediate personal safety and care engagement (Hatcher et al., 2015; Kouyoumdjian et al., 2013). Partner control of resources such as finances and transportation may also limit treatment access for women living with HIV (Lichtenstein, 2006). As in other populations, most of the existing research on violence against women living with HIV has focused on the experience of cisgender women, with limited research pertaining to transgender women and nonbinary people. However, evidence shows that stigma and institutional inequities are shared exacerbating factors of both intimate partner violence among trans women, and healthcare access barriers among women living with HIV (Tan et al., 2020).
While intimate partner violence and sexual relationship power are highly linked, comparatively more research has been conducted on the connection between intimate partner violence and accessing HIV treatment than on the role of relationship power. Relationship or interpersonal power may be described by a framework surrounding the ability to influence or control others within a relationship; relationship power specifically describes ‘power over’ (control over others), which is distinct from personal power or the ‘power to’(control over self) (Harvey & Bird, 2004). Determinants of interpersonal power distribution can arise from different sources of power (i.e., education, health, socioeconomic status), operate through processes of power (i.e., assertiveness, persuasiveness), to manifest as the outcomes of power (Harvey & Bird, 2004), notably decision-making dominance, the ability to act against the partner's wishes, and the ability to enforce the actions of a partner (Pulerwitz et al., 2000). These outcomes are assessed to evaluate relationship power of women in intimate and sexual relationships through the standardized Sexual Relationship Power Scale (Pulerwitz et al., 2000). Review of studies evaluating relationship power using the Sexual Relationship Power Scale indicates high relationship power is positively associated with consistent condom use and less risky sexual behavior (e.g., anal sex), and is negatively associated with physical violence and history of forced sex (Matsuda et al., 2012). The relationship control subscale of the SRPS was also shown to demonstrate high levels of reliability in a study demonstrating that sexual relationship power equity is associated with consistent condom use and fewer experiences of recent violence in women living with HIV in Canada (Closson et al., 2022a).
There appears to be a bi-directional relationship between relationship power and intimate partner violence. Intimate partner violence may be a manifestation of an imbalance of relational power within a partnership (Minieri et al., 2014; Muldoon et al., 2015). Low relationship power has been associated with intimate partner violence among sex workers in Canada (Muldoon et al., 2015) and may also mediate the relationship between intimate partner violence and downstream health outcomes such as mental health conditions (Minieri et al., 2014). Experiences of intimate partner violence may also erode the relationship power held by an individual to further contribute to imbalanced relational power (Minieri et al., 2014). For trans women, this relationship may become further complicated. Limited existing literature exploring relationship power in trans women suggest that enacted transphobia and gender discrimination may be leveraged as an additional tool of establishing power (Peitzmeier et al., 2021).
Globally, while robust research has identified the association between intimate partner violence and health outcomes such as ART use and adherence (Hatcher et al., 2015; Kouyoumdjian et al., 2013; Mendoza et al., 2017; Siemieniuk et al., 2013), there is limited research investigating the direct connection between sexual and relationship power and HIV care outcomes. Understanding relationship power at a dyadic level may provide insight to potential relationship-based HIV care interventions, while consideration of how relationship power interacts with social structural factors may aid design of institutional policy and programs. Therefore, this study aims to address this knowledge gap through investigating how relationship power, measured by the three categories of high, medium, or low power as derived from the Relationship Control subscale within the Sexual Relationship Power Scale, is associated with access to HIV care services among women living with HIV in Metro Vancouver, Canada.
Methods
This analysis drew on data from a community based longitudinal cohort: (Sexual Health & HIV/AIDS: Longitudinal Women's Needs Assessment, the SHAWNA Project) that aims to assess the needs and priorities of women living with HIV in Metro Vancouver. Initiated in 2014, with data collection ending at the end of February, 2025, the SHAWNA Project was developed after six months of extensive consultation with community members, policy experts, and care providers; the project continues to be guided a Community Stakeholder Advisory Board of 10 + community organizations, and a Positive Women's Advisory board comprised 8–12 women living with HIV from Metro Vancouver that meet every 2–3 months.
The cohort included women (cis and trans) living with HIV age 14 and older who are living or accessing HIV care in Metro Vancouver. Ethical approval was in place to allow participants under 18 years of age to consent as mature youths. Recruitment was community based through peer navigators, self-referrals, and care provider referrals, as well as through HIV/AIDS organization and clinical outreach programs including clinical partner (Oak Tree Clinic), BC's main referral center for women living with HIV. At enrollment, participants completed an initial baseline questionnaire, and returned semi-annually for follow-up questionnaires administered by an experienced Community Interview Team. Informed consent was obtained at baseline and at each subsequent visit. Participants may choose to complete the interview at the community research office, or at a discreet location of their choosing.
Data collected by baseline and follow up surveys included individual (age, gender identity, sexual orientation, race/ethnicity), biological/behavioral (optimal ART use and care engagement), and socio-structural (gender-based violence, sexual violence, sex work, housing, and income status) variables. Participants also receive voluntary viral load and CD4 count testing conducted by a sexual health nurse at each visit. STI and Hepatitis C serology is also offered, and nurses may provide treatment onsite for symptomatic STIs and facilitate education and referral. Participants are remunerated $80CAD at baseline and $65CAD at each follow-up visit for their time, expertise, and travel expenses. The SHAWNA Project holds ethics approval through the UBC Clinical Research Ethics Board, and Providence Health Research Ethics Boards.
Primary Outcome Variables
The primary outcomes evaluated include ART use and optimal ART use. Time updated ART use was derived from participant self-report of currently being on ART at the time of questionnaire completion (“yes” vs. “no”). Among participants who self-reported currently being on ART, self-reported optimal ART use was evaluated as greater or equal to 95% ART use/adherence within the past 3–4 weeks based on participant self-report, versus less than 95% ART use/adherence.
Primary Explanatory Variable
The primary explanatory variable of interest was self-reported relationship power evaluated through the sexual relationship and power scale (Pulerwitz et al., 2000). The Sexual Relationship Power Scale is a 23-item measure of relationship power dynamics with two subscales: Relationship Control and Decision-Making Dominance. Specifically, the 15-item Relationship Control subscale was used for this study, and analyses was restricted to heterosexual relationship power dynamics of women with men sex partners. Participants were asked to indicate their level of agreement to statements describing power dynamics in a relationship, such as “if I asked my partner to use a condom, he could get angry” or “I feel trapped or stuck in our relationship.” Possible responses include: “strongly agree”; “agree”; “somewhat agree”; “disagree”; “strongly disagree.”. Items on the Relationship Control subscale were scored on a 4-point Likert scale (1 = strongly agree and 4 = strongly disagree). Scores were then summed and divided into tertials of high, medium, and low relationship power, based on the baseline sample distribution. The standardized Cronbach alpha for the relationship control subscale was 0.93 using the first available observation for participants in our study.
Sample Characteristics and Potential Confounders
Additional variables used to define sample characteristics and considered as potential confounders included: sexual orientation was drawn from a survey item asking “In the last six months, which of the following describes your sexual orientation (check all that apply)” and was defined as having minoritized sexual identities at any study visit (lesbian, gay, bisexual, queer, asexual, and/or Two-Spirit) versus only heterosexual at all study visits; a variable measuring gender identities was drawn from a survey item asking “In the last 6 months, which of the following best describe (s) your gender identity (check all that apply)” and was defined as minoritized gender identities at any study visit, inclusive of trans woman (transgender woman, transsexual woman, other transfeminine identity), nonbinary (nonbinary, genderqueer), and/or Two-Spirit versus only reporting cisgender at all visits. Indigenous women were asked if they identified as Two-Spirit. Two-Spirit is an identity among people Indigenous to Turtle Island/North America who identify as having both a masculine and a feminine spirit, and may be used to describe any or all of sexual, gender and/or spiritual identity depending on the individual and context (Pruden, 2019). Based on evidence that minority stress- stress/distress experienced by individuals identifying as sexual or gender minorities-processes affect all individuals who identify as a gender minority relative to individuals who identify as cisgender (Tan et al., 2020), and all individuals who identify as a sexual minority relative to individuals who identify as heterosexual (Meyer & Frost, 2013), for the purposes of analyses, we combined participants with responses to sexual minority identities into one variable and gender minority identities into one variable. These experiences are driven by ‘minority stressors’, including distal minority stressors (e.g., experiences of discrimination) and proximal stressors (e.g., anticipated discrimination related to disclosure of sexual orientation and/or gender identity, perceived discrimination related to negative social attitudes about ones sexual orientation and/or gender identity or internalized transphobia or other discrimination based on gender identity, or heterosexism) (Brooks, 1981; Livingston, 2017). Additional social-structural factors included race (self-report as Indigenous [First Nations, Métis, or Inuit], other racialized persons [African/Caribbean/Black/other women of color including East/South/Southeast Asian and Middle Eastern] versus. White). The term Indigenous is used throughout while recognizing great diversity across and within languages, cultures, nations, and lands. While descriptive data were disaggregated, given the small sample size of Black participants, comparable to the BC population, Black women and women with other racialized identities were combined in modelling to understand experiences of racism for nonIndigenous racialized persons. We included age at study visit (measured continuously, in years), and im/migrant to Canada, including refugee, immigrant, migrant, asylum seekers, and undocumented persons. We also included whether participants had been forcibly removed from their parents as a child/youth. Remaining variables were time-updated factors, which captured events in the last six months at each semi-annual study visit unless otherwise noted. Structural vulnerability factors included housing instability (any living situation aside from living in the same house/apartment for the last six months alone, with intimate partner, or shared with family, e.g., homeless, living with family/friends, supportive housing, moving in the last six months); food insecurity (measured by a version of the Radimer/Cornell Hunger Scale; “often true” or “sometimes true” to at least one item versus “never true” or “not applicable” to all items (Kendall et al., 1995); main source of employment (sex work, full/part-time employment; versus no formal employment); criminalized injection and noninjection (excluding alcohol and cannabis) substance use. Relationship factors of interest included if the participant financially supported dependent (s) (current measure) and having a cohabiting intimate male partner. With respect to their main intimate male partner in the last six months, the participant reported if they provided financial support to their intimate male partner; if they provided nonfinancial support to their intimate male partner in another way (e.g., shelter, food, drugs, or other); if they received financial support from their intimate male partner; and if they received financial support from their intimate male partner in another way (e.g., shelter, food, child support, drugs/alcohol, cigarettes, physical safety, sex work, or other). If the participant was currently parenting any children (has custody and child lives with them) was also captured. Health-related factors (in the last 6 months) included having a physical disability that limits mobility (current measure); major or persistent pain (reporting undiagnosed or diagnosed major or persistent pain); contemplated or attempted suicide; depression, anxiety and/or post-traumatic stress disorder (PTSD) (diagnosis, treatment, or received counselling).
Statistical Analysis
Analyses were restricted to women in heterosexual relationships who answered the Relationship Control subscale of the Sexual Relationship Power Scale for their main intimate men sex partner. Baseline descriptive statistics, including frequencies and proportions for categorical variables and medians and interquartile ranges (IQR) for continuous variables, were calculated for all variables and stratified by the two outcomes. Differences were assessed using Pearson's chi-square test for categorical variables (Fisher's exact test was employed for small cell counts) and the Wilcoxon two-sample test for continuous variables. A complete case approach was used, such that observations with missing data were removed from analysis. To account for repeated measures by the same respondent, bivariate and multivariable logistic regression with generalized estimated equations (GEE) were conducted using an exchangeable correlation structure to examine the independent associations between relationship power and the two outcome variables of ART use and optimal ART use. Variables hypothesized to be confounders of the relationship between the explanatory variable and the two outcomes and those which were significantly associated at p < 0.10 in bivariate analysis were considered for inclusion in the full multivariable GEE confounder models. The most parsimonious models were determined using the method of Maldonado and Greenland (Maldonado, 1993), where reduced models were constructed by removing potential confounders one at a time and excluding the variable that produced the smallest relative change in the effect estimate for the relationship power explanatory variable. This process was repeated until the minimum relative change exceeded 5%. All reported p-values are two sided and odds ratio (ORs) and adjusted odds ratios (AORs) with 95% confidence intervals (CIs) are reported. SAS version 9.4 was used for statistical analyses (SAS Institute Inc., Cary, NC, USA).
Results
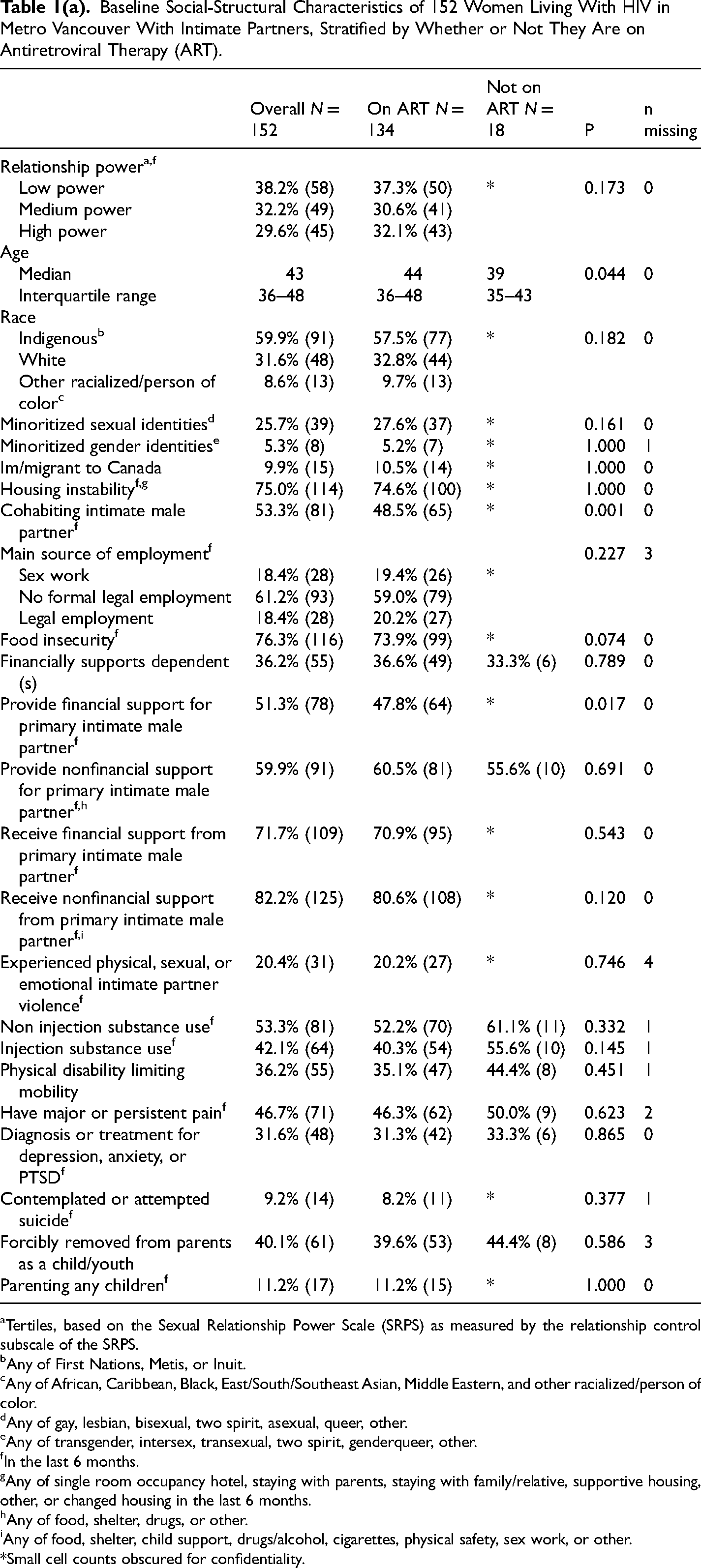
The sample size for the outcome, being on ART, was 408 observations, from 152 participants. The sample size for the outcome, self-reported optimal ART use, was 367 responses, from 143 participants. We drew on data from September 2014 to February 2019. Baseline sample characteristics stratified by being on ART (yes vs, no) and by optimal ART use (optimal, ≥95% vs. suboptimal, < 95%) are shown in Tables 1a and b respectively. Overall, 88.2% (n = 134) of women were on ART at the baseline, and 74.1% (n = 106) of women on ART had optimal ART use at the baseline. Of the entire sample, 38.2% (n = 58), 32.2% (n = 49), and 29.6% (n = 45) of participants were divided into tertiles of low, medium, and high levels of relationship power respectively, as measured by the relationship control subscale of the Sexual Relationship Power Scale. A total of 25.7% (n = 39) of participants had minoritized sexual identities, and 5.3% (n = 8) had minoritized gender identities. Overall, 4.6% (n = 7) identified as trans women, and 1.3% (n = 2) identified as nonbinary. Indigenous persons were overrepresented in this sample at 59.9% (n = 91) relative to the population of British Columbia (5.9% in 2016 by Statistics Canada); 5.3% (n = 8) of Indigenous participants identified as Two-Spirit. The sample also included 8.6% (n = 13) other racialized/persons of color (4.6%, n = 7 African, Caribbean or Black and 4.0% other racialized person/s of color), and 31.6% (n = 48) White participants (Table 1a).
Baseline Social-Structural Characteristics of 152 Women Living With HIV in Metro Vancouver With Intimate Partners, Stratified by Whether or Not They Are on Antiretroviral Therapy (ART).
Tertiles, based on the Sexual Relationship Power Scale (SRPS) as measured by the relationship control subscale of the SRPS.
Any of First Nations, Metis, or Inuit.
Any of African, Caribbean, Black, East/South/Southeast Asian, Middle Eastern, and other racialized/person of color.
Any of gay, lesbian, bisexual, two spirit, asexual, queer, other.
Any of transgender, intersex, transexual, two spirit, genderqueer, other.
In the last 6 months.
Any of single room occupancy hotel, staying with parents, staying with family/relative, supportive housing, other, or changed housing in the last 6 months.
Any of food, shelter, drugs, or other.
Any of food, shelter, child support, drugs/alcohol, cigarettes, physical safety, sex work, or other.
Small cell counts obscured for confidentiality.
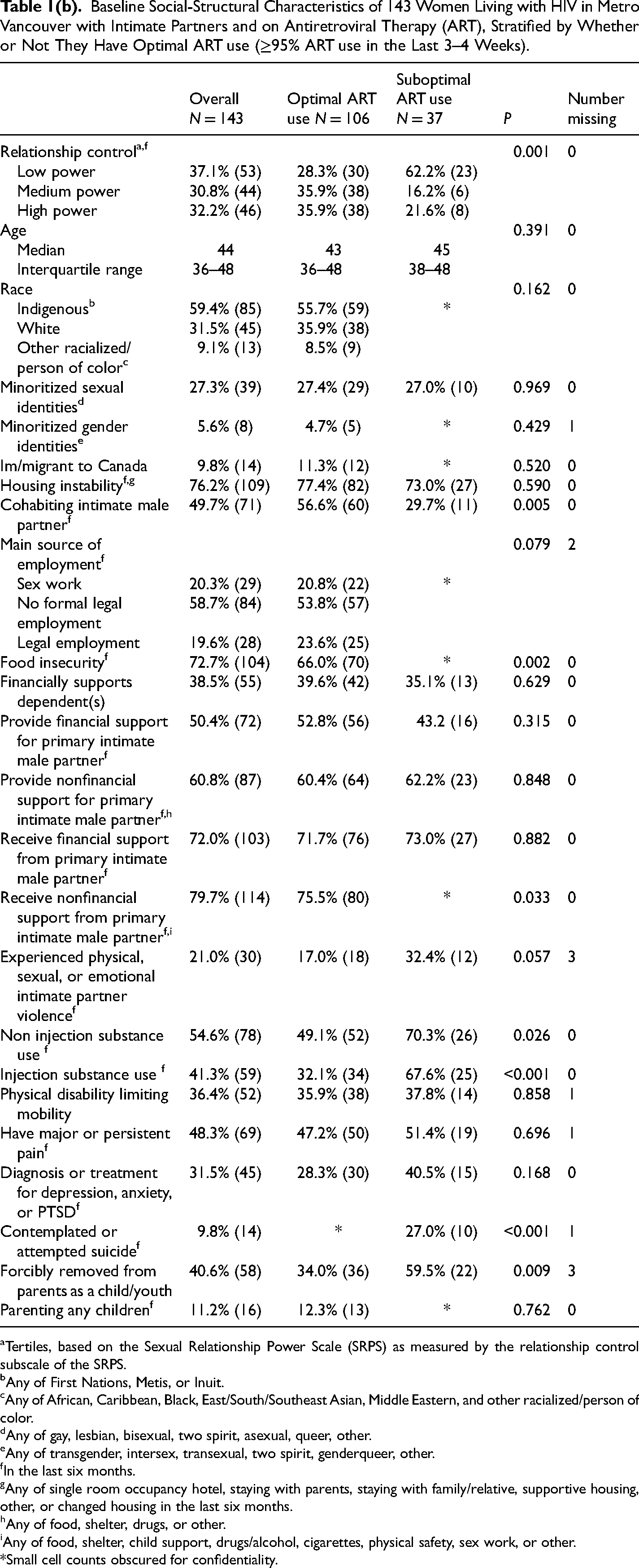
Baseline Social-Structural Characteristics of 143 Women Living with HIV in Metro Vancouver with Intimate Partners and on Antiretroviral Therapy (ART), Stratified by Whether or Not They Have Optimal ART use (≥95% ART use in the Last 3–4 Weeks).
Tertiles, based on the Sexual Relationship Power Scale (SRPS) as measured by the relationship control subscale of the SRPS.
Any of First Nations, Metis, or Inuit.
Any of African, Caribbean, Black, East/South/Southeast Asian, Middle Eastern, and other racialized/person of color.
Any of gay, lesbian, bisexual, two spirit, asexual, queer, other.
Any of transgender, intersex, transexual, two spirit, genderqueer, other.
In the last six months.
Any of single room occupancy hotel, staying with parents, staying with family/relative, supportive housing, other, or changed housing in the last six months.
Any of food, shelter, drugs, or other.
Any of food, shelter, child support, drugs/alcohol, cigarettes, physical safety, sex work, or other.
Small cell counts obscured for confidentiality.
In bivariate GEE analysis (Table 2a), high relationship power (OR: 3.44: 1.34–8.81) and medium relationship power (OR: 1.76: 0.99–3.12) (vs. low relationship power) were associated with increased odds of being on ART. In multivariate GEE analysis, (Table 2a), high relationship power (AOR: 2.85: 1.06–7.69) and medium relationship power (AOR: 1.78: 0.95–3.31) remained significantly associated with elevated odds of being on ART after adjusting for key confounders, including main source of employment and identifying as a sexual minority.
Bivariate (Unadjusted) and Multivariable (Adjusted) Odds Ratios With 95% Confidence Intervals for the Association Between Relationship Power and Being on ART among Women Living with HIV with Intimate Partners a in Metro Vancouver.

Current primary noncommercial men sex partner excluding one-night stand.
The multivariable model was adjusted for the following confounders: race, cohabiting intimate male partner in the last six months, food insecurity in the last six months, injection drug use in the last 6 months, forcibly removed from parents.
Bivariate (Unadjusted) and Multivariable (Adjusted) Odds Ratios with 95% Confidence Intervals for the Association Between Relationship Power and Optimal ART use (≥95% ART Use in the Last 3–4 Weeks) among Women Living With HIV With Intimate Partners and on ART a in Metro Vancouver.

Current primary noncommercial men sex partner excluding one-night stand.
The multivariable model was adjusted for the following confounders: minoritized sexual identities (gay, lesbian, bisexual, Two-Spirit, asexual, queer, other), main source of employment in the last six months.
In bivariate GEE analysis (Table 2b), high relationship power (OR: 2.89: 1.60–5.23) and medium relationship power (OR: 2.69: 1.47–4.95) (vs. low relationship power) were associated with increased odds of optimal ART use. In multivariable GEE analysis (Table 2a), high relationship power (AOR: 2.18: 1.14–4.15) and medium relationship power (AOR: 2.25: 1.11–4.55) remained significantly associated with elevated odds of being on ART after adjusting for key confounders, including race, cohabiting intimate man partner, food insecurity, injection drug use, and having been forcibly removed from parents.
When the outcome is “On ART,”, the full sample size is 152 participants with 408 observations. In multivariable GEE, there are seven missing observations in one confounder variable (“main source of income,” and thus the final sample size for the multivariable model is 151 participants with 401 observations. When the outcome is “≥95% ART adherence,” the full sample size is 143 participants with 367 observations. In multivariable GEE, the sample size is 139 participants with 346 observations. There are 21 missing observations over the study period, across six different variables (three missing observations in the outcome “95% use of ART,” one missing observation in the variable “food insecurity,” three missing observations in the variable “receive nonfinancial support from primary intimate male partner,” one missing observation in the variable “thought of or attempted suicide,” eight missing observations in the variable “forcibly removed from parents as child/youth.” Based on this information, we can see that the missing proportion in the data we use for two multivariable models is small.
Discussion
Our study provides important evidence to suggest that higher sexual relationship power, as measured by the Relationship Control subscale of the Sexual Relationship Power Scale, is associated with more optimal outcomes along the HIV care continuum, including being on ART and optimal (≥95%) ART use amongst heterosexual women living with HIV with their men intimate partners in a Canadian setting.
These findings support the relationship between intimate partner relationship power and HIV care continuum outcomes described by limited existing literature across diverse geographic and socioeconomic contexts (Conroy et al., 2017; Hatcher et al., 2012; Robinson et al., 2017).
Of note, a study conducted by Closson et al. investigating sexual relationship power equity among women living with HIV in Canada found that high levels of relationship control were associated with consistent condom use, and lower odds of recent experiences of violence. Though condom use and experiences of violence are not direct measures of HIV care outcomes, this study supports the association between sexual relationship power and these important health outcomes in the pertinent context of women living with HIV in Canada (Closson et al., 2022a). Other literature provides insight on how relationship power may specifically influence HIV care. For example, a qualitative study investigating how relationship dynamics and partner support influences optimal ART use among heterosexual South African couples found that relationship conflict arose as reason for missed doses, especially among women (Conroy et al., 2017). Conversely, participants also reported that their partner supported their ART use (>96%) by providing instrumental support, reminding them to take their medications, and taking their medications together in the case of couples who are both on ART (Conroy et al., 2017). Though not a direct investigation of relationship power, findings of this study suggests that partners of people living with HIV have to potential to both help or hinder their treatment. Similarly, Hatcher et al. (2012) found that higher relationship power was associated with lower rates of depression and improved mental health status in women living with HIV in Uganda, while Closson et al. found low relationship power to be associated with increased likelihood of intimate partner violence in young women (Conroy et al., 2017). Combined, these findings implicate relationship power as a point of intervention in improving HIV care (Hatcher et al., 2012). A systematic review including studies conducted in North America and Sub-Saharan Africa also found that interventions including HIV knowledge, relationship skill building, and CBT sessions designed to address gender and power inequalities among women living with HIV led improved sexual and reproductive health outcomes, such as increased condom use and condom use self-efficacy (Robinson et al., 2017).
Multiple studies have also found relationship power as a mediator affecting how other factors influence health outcomes (Buelna et al., 2009; Filson et al., 2010; Pulerwitz et al., 2002; Volpe et al., 2012). Given the relationship between depression and suboptimal HIV care outcomes, it is notable that relationship power has been found to mediate the association between intimate partner violence (Filson et al., 2010), or violence perpetrated by a dating partner (Volpe et al., 2012), and depression in girls and women as the outcome (i.e., relationship power transmits the effect of intimate partner violence to influence the outcome of depression). Relationship power has also been noted to mediate the association between other variables, including education and condom use (Pulerwitz et al., 2002) (relationship power transmits effect of education to influence outcome of condom use), as well as violence perpetrated by dating partner and sexually transmitted infections (relationship power transmits effect of dating violence to influence outcome of sexually transmitted infections) (Buelna et al., 2009).
Mechanisms to help explain why higher relationship power may be associated with optimal health services access appear complex. Through the interdependence model, relationship power has been described to affect sexual health and HIV care outcomes among women through three pathways (Blanc, 2001). Power imbalance in favour of partners acts as a direct barrier to functional ability to carry out actions and decisions to improve health, such as negotiating for condom use (Blanc, 2001), or preventing partners from sabotaging/disposing medications (Kouyoumdjian et al., 2013). Power imbalance in favour of partners also influences the ability to use health services, should the dominant partner control the financial or mobility means to do so (Blanc, 2001). Finally, relationship power also acts in association with violence (Blanc, 2001); narrative findings investigating intimate partner violence in women living with HIV describe how the fear of violence often prevents women from disclosing their HIV status, or engaging in HIV care (taking medications, attending appointments, negotiating for safer sex) that may draw attention to their HIV status (Hatcher et al., 2015; Kouyoumdjian et al., 2013; Lichtenstein, 2006). The need for confidentiality, in turn, contributes to avoidance of HIV testing, necessitates concealment of ART medications and potential discontinuation of ART (Kouyoumdjian et al., 2013). Regarding factors mediating the association between relationship power and HIV care continuum outcomes, one study did find that safer sex communication mediated the association between sexual relationship power and condom use in heterosexual young men and women (Li & Samp, 2019). Further study of how relationship power affects access to health services and care outcomes, including investigation of potential mediators, would provide insight for potential relationship power-based interventions.
Implications of the Study
Any intervention, program or policy at individual, interpersonal or structural levels designed to address relationship power and its potential effects on health services access among women living with HIV should encompass Indigenous-led, culturally safe approaches with Indigenous women (Allen et al., 2020; Tujague & Ryan, 2021) and culturally appropriate approaches that respect and celebrate diversity among women living with HIV according to culture and/or ethnic background, alongside trauma-informed principles and practice. Given the over-representation of Indigenous women with HIV in this study, it is crucial to acknowledge the intersections between colonial violence and systemic racism and oppression in Canada, and its role in gender-based violence and relationship power inequities. Recommendations rely on the critical guidance of the Missing and Murdered Indigenous Women and Truth and Reconciliation Commission reports (National Inquiry into Missing and Murdered Indigenous Women and Girls., 2019; Truth and Reconciliation Committee in Canada, 2015), which outline critical guidance and calls to action. Trauma-informed approaches include an awareness of health effects of trauma, creating safe environments, and fosters connection and trust, and can help guide recommendations drawn from this study. Trauma-informed practice is founded upon the understanding that experiences of trauma can influence healthcare interactions and manifest in multiple ways including physically, mentally, and behaviorally (Health Resources and Services Administration, 2018). A trauma-informed approach to care may include encouragement of patient participation, nonjudgmental patient–provider interactions, providing a safe and comfortable care environment, and reducing administrative barriers to care access (Health Resources and Services Administration, 2018). Trauma-informed principles must acknowledge that experiences of trauma can stem from and/or intersect with various forms of oppression and marginalization, including racism, gender discrimination, classism, homophobia and/or transphobia (Health Resources and Services Administration, 2018). For example, gender discrimination may affect the establishment and manifestations of relationship power, particularly for trans women (Peitzmeier et al., 2021).
Safe, supportive and strength-focused relationship power screening, in addition to intimate partner violence screening, may help identify barriers to care. Though intimate partner violence often exists concurrently with low relationship power, relationships with low power does not necessarily include intimate partner violence. However, this does not preclude individuals experiencing lowing relationship power, but not intimate partner violence, from encountering care barriers often associated with intimate partner violence. These findings also highlight the importance of supporting care access for individuals experiencing low relationship power. Screening tools to identify trans-specific intimate partner violence, such as outing a partner, have been described and validated in efforts towards trans-inclusive care (Peitzmeier et al., 2019, 2021). Further adaption of a trans-specific relationship power screening tool may help include trans women in relationship power-based research and intervention.
Research exists to support psychoeducation-based programs that address sexual health risk reduction, STIs, partner communication, and healthy relationship building to support sexual and reproductive health among women living with HIV (Robinson et al., 2017). Concurrently, supporting women and their partners in developing relationships in which there is equitable power dynamics may also contribute to improving optimal ART use among women. All such programs and interventions should incorporate culturally safe approaches that attend to the mental and emotional needs of Indigenous women and their relationships, and include access to elders, traditional healers and ceremonies and land-based programs. Culturally appropriate approaches that take into account diverse interpretations and acknowledgement of mental health issues should be tailored with and according to the needs of specific cultural/ethnic groups. Programs to support the development of couples-focused interventions among Indigenous women need to take into account the effects of colonial violence in shaping relationship dynamics and should be grounded in culturally safe principles to support healing. Existing literature have found that a collectivist relationship orientation was associated with improved HIV care retention (Goldenberg et al., 2013) and that partners of people living with HIV can provide significant support in consistent medication use (Stumbo et al., 2011). Family and couples-based interventions that bolster social support have been known to improve health outcomes in management of other chronic conditions such as diabetes and cancer (Remien et al., 2005). One study (Dworkin et al., 2017) found in a narrative investigation of relationship power among same-sex men couples that some men described that being a part of a supportive relationship helped empower them as individuals in their personal and professional pursuits. These benefits may also translate to health care services access, including HIV care, as highlighted in a randomized controlled trial conducted in New York examining the efficacy of couples-based intervention on consistent HIV medication use. The study found that those who participated in couples-based intervention was more likely to be take medication regularly, though the effects diminished following the intervention (Remien et al., 2005). Though existing research is largely conducted with cis women, trans women may also benefit from couples-based interventions. In a randomized control study involving trans women and their cis men partners, couples-based intervention for HIV prevention reduced higher risk behaviors such as sex without a condom and sex with a casual partner (Poteat et al., 2020). Further study of trans and gender-diverse couples-based intervention to improve HIV care are needed.
Additional institutional and socio-economic changes may help to address the functional-, financial, and violence-related barriers to health care exacerbated by inequitable relationship power, and build empowerment among women to improve health care access. Considerations of the historical and ongoing effects of colonial violence and systemic racism against Indigenous Peoples, as highlighted in item 18 of the Truth and Reconciliation Commission of Canada call to action (National Centre for Truth and Reconciliation, 2015), should be a key priority when developing these strategies. With cultural safety, cultural appropriateness and trauma-informed principles in mind, implementing social policy to address basic health and safety concerns, such as housing insecurity, food insecurity, and mental/physical health care (Closson et al., 2022a; Hatcher et al., 2015; Kouyoumdjian et al., 2013) could provide a source of physical safety and lessens dependence on partners for the necessities of life to alleviate the acute impacts of violence and socioeconomic barriers to care for women experiencing low relationship power. This impact may be bolstered with programs to support care access during times of financial insecurity, such as providing transportation, childcare, and employment support. Additional efforts to optimize the processes of HIV care, such as simplified medication regimens, accessibility of medication and healthcare professionals may lower the functional requirement to seek and participate in care and could help support confidentiality for some women.
Interventions to address societal gender norms alongside HIV-related and other intersectional stigmas (poverty stigma, class stigma, racism, transphobia, homophobia, heterosexism, sexism) may help promote women's relationship power and reduce inequitable power dynamics. Systematic review of studies examining characteristics of successful interventions targeting gender norms and inequality worldwide identified multiple key approaches (Levy et al., 2020). Successful interventions such as the SASA! program to reduce intimate partner violence in Uganda (Kyegombe et al., 2014) utilized multisectoral action involving collaborating with community activists, marriage counselors, religious and cultural leaders outside of the healthcare sector (Heymann et al., 2019; Levy et al., 2020). Other programs incorporating multilevel, multistakeholder interventions involving not only individuals, but also communities, government leaders, and NGOs were more effective in changing entrenched social norms (Heymann et al., 2019; Levy et al., 2020). Employment of diversified programming such as including mass media campaigns in addition to individual/group counselling allowed for greater social participation (Heymann et al., 2019; Levy et al., 2020). Finally, addressing inequitable gender norms, such as through programs that are tailored toward encouraging community members including men and boys to critically reflect on how to participate in systemic change (Heymann et al., 2019; Levy et al., 2020), could help improve equitable social and health care participation among women. Ultimately, a combination of direct care practices (trauma informed patient care, cultural safety), socio-structural changes (access to medication and healthcare resources, addressing housing, food, security concerns), and altering cultural norms are collectively necessary to improve care outcomes for women living with HIV.
Limitations
This study had several limitations as well as strengths. The small sample size may not provide sufficient power to detect other potentially relevant associations. This limitation is mitigated by our study design that was able to draw on longitudinal data available. As this study includes self-reported data, results may be influenced by social desirability bias or recall. However, our community interviewers have extensive training and experience in conducting interviews in a safe and supportive manner, and work to develop good relationships with study participants to minimize such bias.
Additionally, optimal ART use was defined as 95% adherence, though emerging studies indicate that 95% adherence may not be necessary for viral suppression (Bezabhe et al., 2016; O’Halloran Leach et al., 2021). This may have excluded participants who did not achieve 95% adherence, but nonetheless achieved viral suppression. Given the longitudinal nature of data gathered in this study, the 95% adherence threshold was defined at study initiation in 2014, based on standard practice used in HIV research (Lima et al., 2010; Paterson et al., 2000). However, future studies may consider adjusting the threshold of optimal adherence.
Additionally, findings of this study may not be representative of all women living with HIV in Metro Vancouver and may not be generalizable to women living with HIV in other settings. Recruitment of study participants for the SHAWNA Project was conducted across a diverse group of community organizations and clinical settings to reflect as much of the diversity of women living with HIV in Metro Vancouver as possible.
Limitations also exist with regards to evaluating sexual relationship power using the SRPS. Within this study, high, medium, and low relationship power was divided into tertiles based on a normal distribution of scores within our cohort. This was done to better assess the relationship between result variables and relationship power within the cohort population. However, as power level stratification cutoffs are determined based on the study population, it is difficult to compare the relationship power level observed in our study population with others in existing literature. Within our study, of the women who were on ART, 38.2% experienced low, 32.2% medium, and 29.6% high power respectively, while women who had optimal ART use experienced 37.1% low, 30.8% medium, and 32.2% high power respectively. In context of existing literature, Closson et al. stratified relationship power levels based on Pulerwitz et al.'s original scoring cutoffs with SRP scores of 1–2.43, 2.431–2.820, and 2.821–4 corresponding to low, medium, and high relationship power respectively in their study of sexual relationship power and condom use in women living with HIV in Canada (Closson et al., 2022a). With this method of scoring, they found that 80% of their study population experienced high levels of relationship power, and conducted analysis by combining the remaining 20% of low and medium relationship power responses into one group for analysis (Closson et al., 2022a). In comparison, Hatcher et al. divided relationship power scores into tertiles and reported median relationship power score of 2.46 with interquartile range of 2.10–2.85 for N = 270 participants within their study of relationship power and depression among women living with HIV in Uganda (Hatcher et al., 2012). Given that intercomparison of sexual relationship power level is difficult across studies without current data, further investigation may compare how sexual relationship power differs among populations.
Finally, the original SRPS was validated for men intimate sexual partners; but used the term “male” which implies biological sex rather than gender identity and thus may be interpreted by some participants to only apply to cisgender men. However, the SRPS has been used to evaluate sexual relationship power of cohorts across sexual orientation and gender identities with reassuring validity (McMahon et al., 2015). More recent work has adapted and used SRPS across sexual orientations and gender identities (Closson et al., 2019; Closson et al., 2022b; Matsuda et al., 2012; McMahon et al., 2015). Nevertheless, further validation of the SRPS, or creation of a more inclusive relationship power scale that is valid across sexual orientation and gender diversity is recommended.
Conclusion
Our study provides novel evidence to suggest that relationship power plays an important role in supporting optimal HIV care continuum outcomes, including being on ART and optimal ART use. These findings suggest the critical importance of relationship power screening alongside partner violence screening, strength-focused couples-based interventions and structural approaches to address gendered social and health inequities, gender norms and HIV stigma.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by grants from the Canadian Institutes of Health Research (PJT - 169119) and the National Institutes of Health (1R01MH123349-01A1), and the Canadian HIV Trials Network (CTN-333). KD was supported through a Michael Smith Foundation for Health Research Scholar Award.
