Abstract
This study evaluated whether rotational thromboelastometry (ROTEM; Tem International GmbH, Munich, Germany) FIBTEM maximum clot firmness (MCF) can be used to predict plasma fibrinogen level in pediatric patients undergoing cardiac surgery. Linear regression was conducted to predict plasma fibrinogen level using FIBTEM MCF (0.05 level of significance). Scatter plot with the regression line for the model fit was created. Fifty charts were retrospectively reviewed, and 87 independent measurements of FIBTEM MCF paired with plasma fibrinogen levels were identified for analysis. Linear regression analysis suggested a significant positive linear relationship (P < .0001) between plasma fibrinogen levels and MCF. Both MCF intercept and slope were significantly correlated with fibrinogen level (P < .0001). The estimated regression equation (predicted fibrinogen = 78.6 + 12.4 × MCF) indicates that a 1-mm increase in MCF raises plasma fibrinogen level by an average of 12.4 mg/dL. The statistically significant positive linear relationship observed between MCF and fibrinogen levels (P < .001) suggests that MCF can be used as a surrogate for fibrinogen level. This relationship is of clinical relevance in the calculation of patient-specific dosing of fibrinogen supplementation in this setting.
Background
Rotational thromboelastometry (ROTEM; Tem International GmbH, Munich, Germany) is a modification of thromboelastography (TEG; Haemonetics Corp., Braintree, Massachusetts), first described in 1948. 1 Thromboelastography and ROTEM are point-of-care instruments that assess the viscoelastic properties of whole blood during coagulation; they are commonly used to monitor hemostasis and transfusion management in patients undergoing surgery or experiencing trauma. 2,3 Although similar, the devices are different and can yield different results, particularly for fibrin-based clotting. 3,4 The functional fibrinogen (FF) assay (TEG device) and the FIBTEM assay (ROTEM device) purport to ascertain the functional stability of fibrin polymerization, the end product of the enzymatic cascade of blood clotting. To eliminate platelet’s contribution to clot strength, abciximab, a glycoprotein IIb/IIIa platelet inhibitor, is used in the TEG FF assay, while the platelet inhibitor cytochalasin D is used in the ROTEM FIBTEM assay after tissue factor activation. 3,4 Rotational thromboelastometry measurements at the bedside have been previously validated compared to those analyzed in a hospital laboratory; 5 in contrast, plasma fibrinogen levels are not quickly obtained in the operating room using standard laboratory tests. Furthermore, reference values for pediatric age groups have been established for the ROTEM assays. 6
We attempted to correlate the maximum clot firmness (MCF) of the FIBTEM test with plasma fibrinogen levels derived via the Clauss Method. We then devised a mathematical formula to convert the MCF value of the FIBTEM test to a plasma fibrinogen level based on this analysis, thus allowing the MCF to be used as a surrogate of plasma fibrinogen levels.
Methods
After receiving institutional review board (IRB) exempt status from the Research Institute of Nicklaus Children’s Hospital, we retrospectively and consecutively reviewed charts of neonates, infants, and children 5 years old or younger undergoing cardiac surgery, where fibrinogen levels were obtained in the perioperative period. Values at cardiopulmonary bypass (CPB) baseline, on CPB, and after CPB were obtained; this represents a wide range of fibrinogen and FIBTEM MCF values. Dates ranged from May 1, 2015, to November 15, 2015. Plasma fibrinogen levels obtained by traditional laboratory tests (the Clauss method) were compared to the FIBTEM MCF values taken at the same time. The fibrinogen was measured by the Stago STA Compact System, which used a modified Clauss method. The reagents used are; reagent 1: STA-Fibrinogen, reagent 2: STA—Owren-Koller buffer and STA—Coag Control N+ABN Plus (Diagnostic Stago Inc., Mount Olive, New Jersey). Clot detection by the STA-Compact involves an electromagnetic–mechanical system. Essentially, the method involves measuring the clot formation time when adding excess thrombin to plasma samples with standardized fibrinogen concentrations to produce a standard curve. When the patient sample is evaluated, thrombin is added and then the clot formation time is compared to the standard curve to determine the fibrinogen concentration.
Descriptive statistics including mean, standard deviation, minimum, maximum, and median were used to describe plasma fibrinogen levels and FIBTEM MCF values. Kolmogorov-Smirnov test was used to assess whether plasma fibrinogen levels and FIBTEM MCF values were normally distributed. Simple linear regression was performed to determine whether FIBTEM MCF significantly predicts fibrinogen level. Model fit was assessed by distribution of residuals and R 2.
Inferentially, our aim was to develop a regression equation to predict Clauss fibrinogen levels with ROTEM FIBTEM MCF. To do so, we used repeated 10-fold cross validation as is standard for predictive equation development. 7,8,9 First, data (87 subjects) were randomly split into 10 roughly equal-sized parts. Each of kth part, k = 1, 2…10, was left out for testing, while linear regression with robust standard errors, 10 quadratic regression, and cubic regression were employed, respectively, using the 9 remaining parts to train the models. The held out kth block was then predicted and predictions were summarized into mean squared errors. We repeated the process of 10-fold cross validation for 1000 times, and the estimates from a total of 10 000 resamples were averaged; this is commonly known as repeated k-fold cross validation of a predictive equation. 7 Model selection was based on the comparisons of average Akaike Information Criterion (AIC) 11,12 from the linear, quadratic, and cubic training models. Mean R 2, correlation coefficient, and standard errors of correlation coefficients were calculated for the selected model across the 10 000 resamples. Statistical analysis was performed using the statistical software package SAS Enterprise Guide 7.1 and R 3.4.2. A P value of .05 was used for the level of statistical significance.
Results
We retrospectively reviewed 50 charts of neonates, infants, and children <5 years old undergoing cardiac surgery. A total of 87 independent measurements of FIBTEM MCF paired with plasma fibrinogen levels were identified for analysis in 27 patients.
Plasma fibrinogen level ranged from 33.0 to 448.0 mg/dL, with the sample mean of 178.1 and standard deviation of 76.4 mg/dL (Table 1). The mean FIBTEM MCF was 8.0 mm with the standard deviation of 4.3 mm. Both plasma fibrinogen level and FIBTEM MCF were normally distributed according to Kolmogorov-Smirnov test (P > .05).
Descriptive Statistics of the Plasma Fibrinogen Level and FIBTEM MCF (N = 87).

We first offer a basic description of a single linear regression to show a simple linear regression line with all available samples. Results suggest a significant positive linear relationship between plasma fibrinogen levels and FIBTEM MCF measurements. Figure 1 shows the scatter plot of plasma fibrinogen levels on the ordinate (y-axis) scale and corresponding MCF values on the abscissa (x-axis) as well as the basic linear regression line fit to all available samples. However, to ensure a more robust estimate of the predictive equation, we shift our focus to the repeated k-fold cross-validation process to produce a robust predictive model.

Fit plot of linear regression using FIBTEM maximum clot firmness to predict plasma fibrinogen levels (N = 87).
Using repeated 10-fold cross validation, results suggested that linear regression model was the best among linear (mean AIC = 853.3), quadratic (mean AIC = 852.2), and cubic (mean AIC = 854.0) models. The estimated intercept across repeated k-fold cross validation sampling was 78.6 (95% confidence interval [CI]: 52.8-104.4, P < .001; Table 2), and the mean correlation coefficient of FIBTEM MCF was 12.4 (95% CI: 9.6-15.2, P < .001). Estimates from repeated cross validation were consistent with these from simple linear regression, with a slightly increased mean standard error of the intercept. The mean R 2 was 0.375. Figure 2 shows the fit of the averaged regression lines (blue line) and corresponding predictive equation across repeated k-fold cross validation samples and their associated regression lines (pink lines). The final prediction of Plasma Fibrinogen on MCF is:
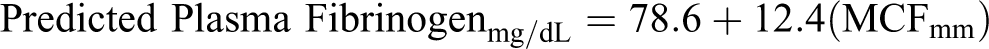
Results from Repeated 10-fold Cross Validation of Linear Regression Using FIBTEM MCF to Predict Plasma Fibrinogen Level.


Repeated 10-fold cross validation results of linear regression. MCF indicates maximum clot firmness.
Discussion
Our results suggest a strong positive correlation between standard plasma fibrinogen levels measured in the laboratory and FIBTEM MCF. Linear regression analysis demonstrated that Predicted Fibrinogenmg/dL = 78.6 + 12.4 (MCFmm) was the best “fit” for the data. Similar results were obtained by other investigators in adult patients. Mace et al demonstrated a strong correlation between ROTEM FIBTEM MCF and fibrinogen levels derived via the Clauss method in a retrospective analysis of 1077 adult cardiac surgery patients. 13 Roullet et al showed a strong correlation between the ROTEM FIBTEM A10 and fibrinogen levels in 23 adult patients undergoing orthotopic liver transplant. 14 Other investigators have likewise demonstrated similar results in adult patients. 15,16 Moreover, Haas et al prospectively demonstrated a good correlation between fibrinogen level and ROTEM FIBTEM MCF in 50 pediatric patients undergoing major surgery. 17 Other investigators have reported similar results. 18 –20 However, none created a predictive formula with this data for future use by clinicians during the ROTEM test.
It has been reported that early ROTEM measurements predict MCF in pediatric patients undergoing cardiac and noncardiac surgery, with clot amplitude at 5, 10, and 15 minutes after clotting time strongly correlating with MCF in all ROTEM assays. 21 Therefore, with ROTEM, coagulation testing can be performed at the bedside, and results can be available in as little as 5 minutes. In contrast, common laboratory fibrinogen tests typically take an hour or more to obtain a result, greatly reducing their utility to clinicians in the operating room. 22 Rotational thromboelastometry allows for early goal-directed hemostatic therapy, potentially improving patient outcomes compared to standard coagulation tests. Indeed, use of ROTEM during cardiac surgery has been shown to reduce transfusion prevalence in pediatric patients compared to conventional testing. 23
It has been widely reported that the coagulation system of neonates is immature. 24 –26 Part of this is due to the fact that neonatal fibrinogen is structurally and functionally different than adult fibrinogen. 27 –29 Use of human fibrinogen concentrate (HFC) at a dose of 70 mg/kg has been shown to reduce the need for transfusion with fresh frozen plasma and cryoprecipitate in neonates, young infants, and other high-risk cardiac surgery patients. 30 In addition, HFC administration to adult patients with fibrinogen levels within the normal range undergoing aortic valve operation and ascending aorta replacement, with the aim of reaching upper-normal levels, led to reduced postoperative bleeding and transfusion requirements. 31 Therefore, with administration of HFC to correct hypofibrinogenemia, previous studies have suggested a possible benefit of HFC when targeting a high-normal fibrinogen level in adults undergoing cardiac surgery. 31 However, subsequent studies did not demonstrate this benefit in adult cardiac surgery patients. 32,33
Goal-directed and individualized HFC dosing in this situation may be more efficacious in reducing transfusion requirements than a standard dose of 70 mg/kg of HFC. Further prospective studies will need to be conducted to investigate the benefits of ROTEM-guided HFC dosing in clinical settings. One noteworthy point, factor XIII (Fibrin Stabilizing Factor), which is essential for final clot stability and responsible for producing cross-linked fibrin strands, affects the ROTEM FIBTEM but not the fibrinogen level as determined by the Clauss method. 34,35 Factor XIII can be deficient after CPB in this patient population, potentially affecting the result.
Using the Predicted Fibrinogen formula determined in this article and the ROTEM FIBTEM, clinicians can ascertain a patient’s plasma fibrinogen level within 5 minutes, with the caveat that prospective studies would further support the validity of our formula. The recommended dosing formula can then be used to calculate the appropriate dose of HFC to be administered in order to reach a target plasma fibrinogen level.
Conclusions
A statistically significant positive linear relationship was observed between MCF values and plasma fibrinogen levels (P < .001), indicating that FIBTEM MCF can be used to determine plasma fibrinogen levels; the simple but robust predictive equation is: Predicted Fibrinogenmg/dL = 78.6 + 12.4(MCFmm). Rotational thromboelastometry provides the advantage of a shorter time to coagulation results, allowing earlier goal-directed hemostatic treatment compared to conventional laboratory tests. The results of this study suggest FIBTEM MCF may be used as a surrogate of the plasma fibrinogen level to calculate patient-specific dosing of HFC. Further prospective studies are needed to investigate the use of FIBTEM MCF and our predicted fibrinogen equation in coagulation testing and HFC dosing in a real-world clinical setting.
Footnotes
Authors’ Note
This retrospective study was approved by the Research Institute of Nicklaus Children’s Hospital. It was granted Institutional Review Board Exempt status. Financial support was provided by CSL Behring. Our institution does not require ethical approval for reporting deidentified retrospectively obtained data. We received IRB exempt status from the Research Institute of Nicklaus Children’s Hospital.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded in part by CSL Behring.
