Abstract
The significance of platelet size indices has not been widely analyzed in anorexia nervosa (AN). It seems important to get more knowledge on the easily available indices of platelet function obtained by routine complete blood count analysis in patients with AN. We analyzed platelet count (PLT), platelet distribution width (PDW), and mean platelet volume using an automated blood cell counter in 25 females with AN and healthy age- and gender-matched nonatopic controls. Mean PLT was significantly lower in patients with AN than in the control group. Platelet distribution width values in patients with AN were significantly higher than those in the controls. Platelet distribution width values significantly correlated with the disease duration and rate of body weight loss in the anorectic patients. Anorexia nervosa in adolescents is associated with a decrease in PLT along with an increased PDW, which may be an indicator of dysregulated thrombopoiesis.
Keywords
Introduction
Anorexia nervosa (AN) is a complex syndrome characterized by changes in eating behavior associated with somatic complications and multiple metabolic, endocrine, immune, and hematological abnormalities. 1,2 All of these disturbances may be accompanied by changes in platelet function. 3 –5 It has been demonstrated that thrombocytopenia is a frequent complication of AN, which often resolves itself with nutritional rehabilitation. 6 –10 Platelet volume measurements, such as mean platelet volume (MPV; an indicator of platelet size) and platelet distribution width (PDW; an index of platelet size heterogeneity), are simple and useful parameters related to platelet function and activation. Platelet size is widely available as part of a full blood count analysis. 11 –13 Therefore, it is important to obtain more information about the parameters characterizing platelet function; these data can be collected from a simple and common laboratory test. Therefore, the aims of this study include (1) evaluating platelet indices such as MPV, PDW, and platelet count (PLT) in adolescent patients with AN and (2) determining the associations between platelet parameters and inflammatory markers as well as body mass index (BMI) in these patients.
Materials and Methods
We recruited 25 females (mean age: 15.2 [1.2] years, range: 13.2-17.1 years) who, following pediatric examination, psychological evaluation, and psychiatric consultation, were diagnosed with a restrictive type of AN in accordance with the classification in Diagnostic and Statistical Manual of Mental Disorders V of the American Psychiatric Association. 14
We assessed the patients using a semistructured interview (The Eating Disorder Examination). 15 Expected body weight was established using normal ranges for a Polish population of females. 16
Our evaluation was based on an analysis of hospital medical documentation regarding patients with AN referred to the Department of Paediatrics and Endocrinology at University Hospital in Zabrze, Poland, prior to refeeding treatment. The patients did not have concomitant diseases (screened by clinical history, physical examination, electrocardiography, chest radiography, spirometry, and urine and blood tests), severe somatic complications of AN (gastrointestinal bleeding, dehydration, peptic ulcer disease, liver and kidney dysfunction), or psychiatric disorders. Additionally, gynecological and orthopedic consultations. On recruitment, none of the patients were taking drugs (including antianxiety medications or psychotropic drugs). The mean duration of the disease prior to hospitalization was 14.9 (17.4) months. In all patients with AN, secondary amenorrhea had been present for a mean duration of 7.3 (7.2) months. We also calculated the mean rate of body weight loss prior to hospitalization (weight loss, kg/duration of the disease, months), which was 1.73 (1.38) kg/month. During hospitalization, patients were placed on bed rest, they were fed a high-calorie diet, and they received psychotherapy.
The control group consisted of 24 age-matched (mean age: 15.2 [2.0] years; range: 13.7-17.5 years), healthy, normal weight, nonsmoking females without signs of infection, or atopy.
All of females who we examined were in Tanner IV to V pubertal stages. Full blood count including platelet indices (PLT, MPV, PDW) was performed using ABX Pentra XL 80 (Horiba, Kyoto, Japan) analyzer.
The study was conducted according to the Declaration of Helsinki and approved by the Bioethics Committee of the Medical University of Silesia in Katowice (registry number KNW/0022/KB/211/12). Informed written consent for participation in the study was obtained from all study participants and their parents or legal guardians.
Statistical Analysis
We prepared the database using Excel 2000 (Microsoft Corporation, Albuquerque, New Mexico). We carried out the statistical analysis using Statistica 6.0 software (StatSoft Inc, Tulsa, Oklahoma). A normal data distribution was assessed using the Shapiro-Wilk test; homogeneity of variance was computed using Levene test. We present the results as means (standard deviation [SD]) for normally distributed variables and as medians and interquartile ranges for nonnormally distributed variables. We used the student t test or the Mann-Whitney U test (if the distribution of data differed from normal) for intergroup comparisons. Spearman correlation coefficients were used to estimate relationships between variables. We used analysis of covariance to remove the effects of parameters that significantly differed between the groups. P Values <.05 were considered to be statistically significant.
Results
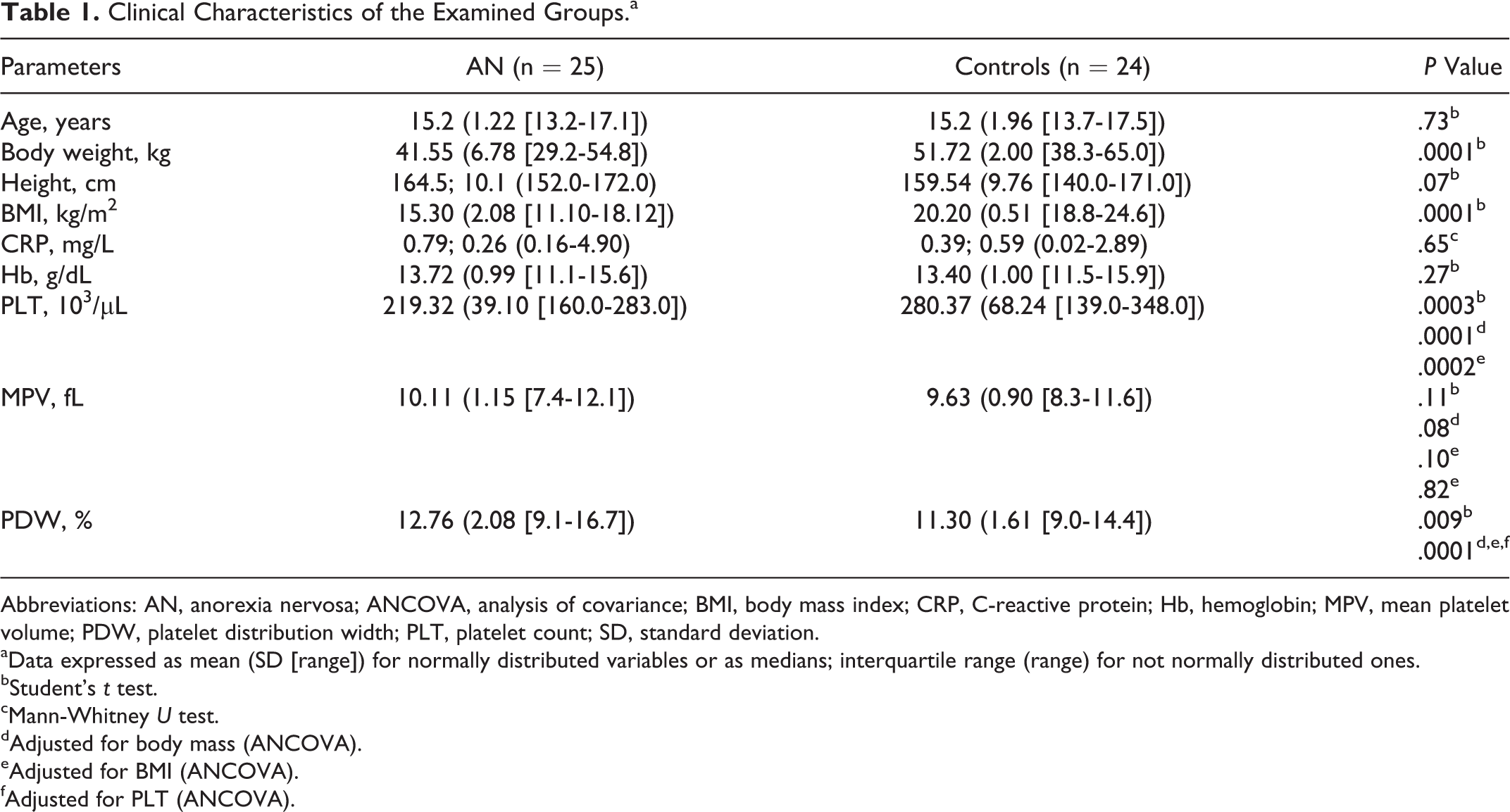
A comparison of the platelet parameters between patients with AN and healthy participants is presented in Table 1.
Clinical Characteristics of the Examined Groups.a
Abbreviations: AN, anorexia nervosa; ANCOVA, analysis of covariance; BMI, body mass index; CRP, C-reactive protein; Hb, hemoglobin; MPV, mean platelet volume; PDW, platelet distribution width; PLT, platelet count; SD, standard deviation.
aData expressed as mean (SD [range]) for normally distributed variables or as medians; interquartile range (range) for not normally distributed ones.
bStudent’s t test.
cMann-Whitney U test.
dAdjusted for body mass (ANCOVA).
eAdjusted for BMI (ANCOVA).
fAdjusted for PLT (ANCOVA).
As expected, anorectic patients had significantly lower body weights and BMIs than the control group, but there were no other differences in the 2 samples in terms of other clinical parameters.
The mean PLT was significantly lower in patients with AN than in the control group, even after adjusting for body mass or BMI (Table 1). However, all values were within normal ranges (according to populational reference values: 130-400 103/μL).
Platelet distribution width values in patients with AN were significantly higher than those in the controls (Figure 1). This difference remained significant after adjusting for parameters that significantly differed between the groups—body mass, BMI, and platelets count (Table 1). Three (12%) patients in the AN group and 4 (16.7%) patients in the control group had PDW lower than normal (according to the reference values in our laboratory: 9.8%-16.2%). Only patients with AN (2 of 25 females) were found to have PDW higher than normal (according to the populational reference values: 9.8%-16.2%).
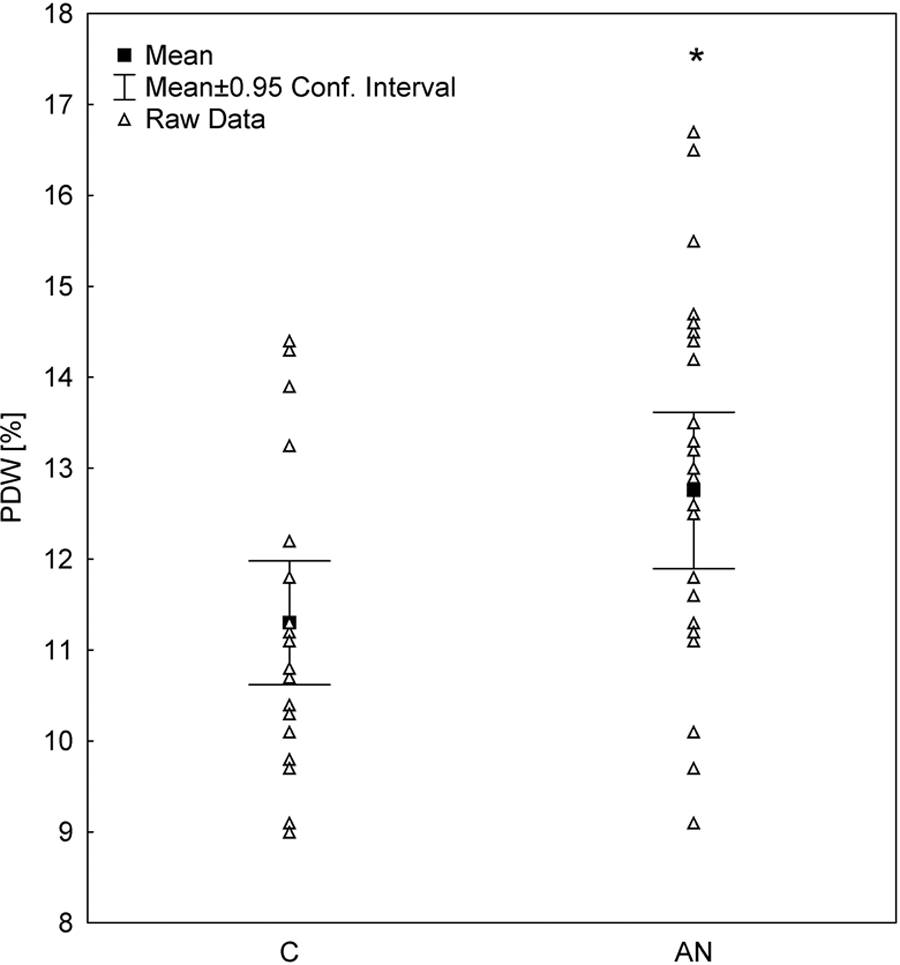
Platelet distribution width (PDW) in the examined groups. AN indicates anorexia nervosa; C, healthy controls. *P < .05.
All MPV values were similar between the 2 groups (also after adjustment for body mass, BMI, and PLT; Table 1) and normal (according to reference values: 7.4-12.4 fL).
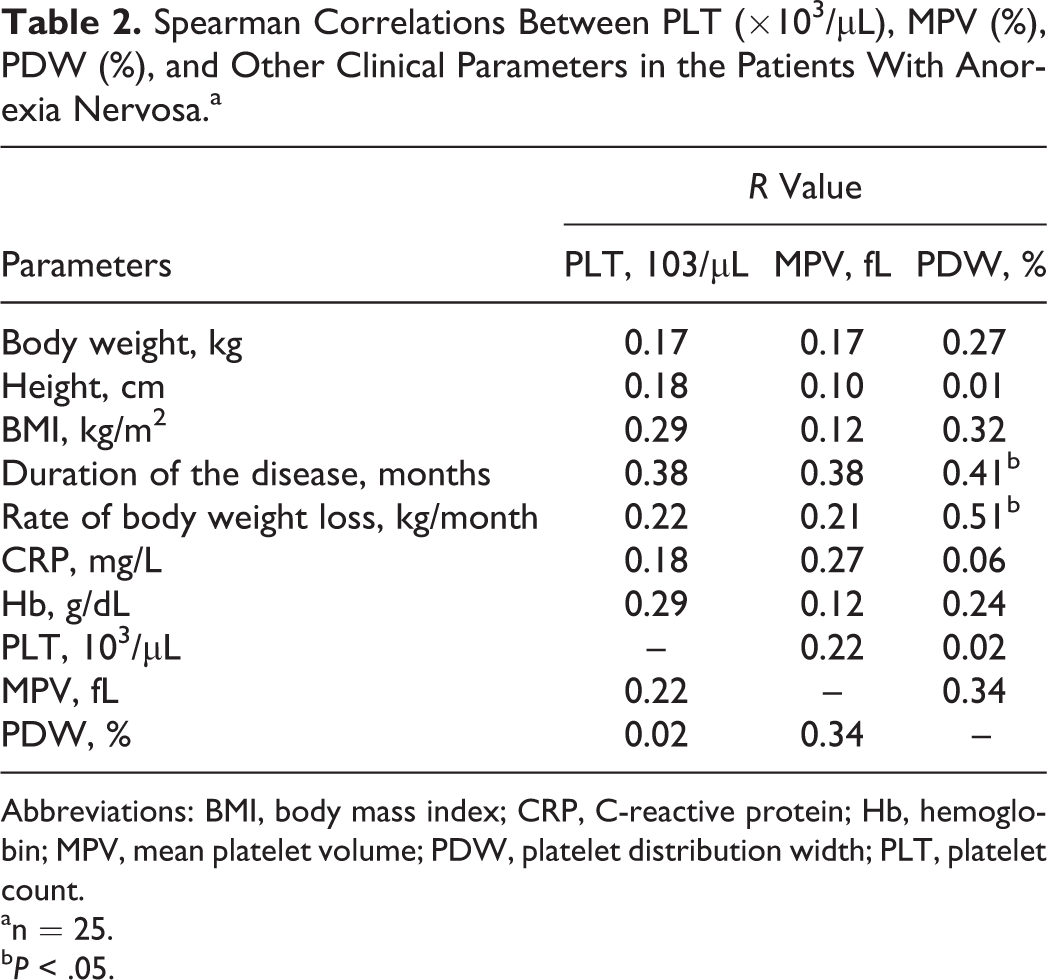
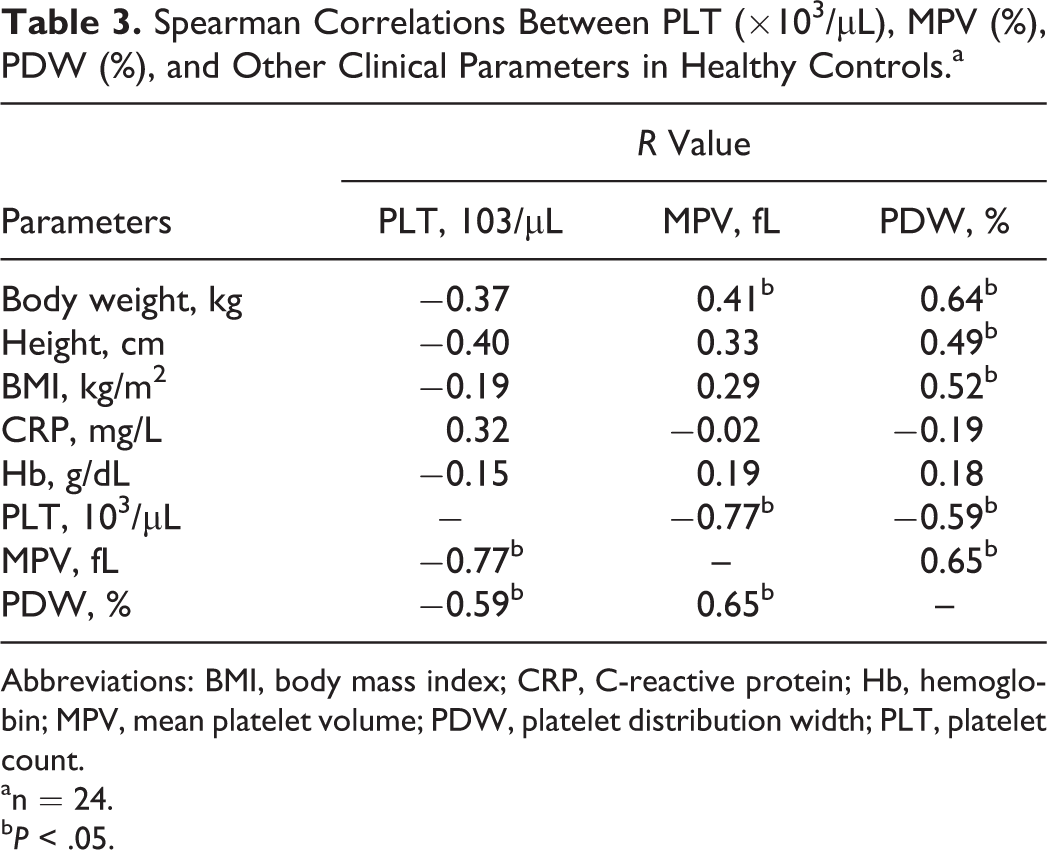
In patients with AN PLT correlated negatively with duration of the disease and rate of body weight loss. Platelet count, MPV, and PDW did not correlate with anthropometric parameters (body weight, height, and BMI) either hemoglobin or serum C-reactive protein (CRP) concentrations. There was not any significant relationship between PLT, MPV, and PDW in this group (Table 2). In the healthy girls, we showed a significant positive correlation between MPV, PDW, and body weight. Platelet distribution width correlated also with height and BMI. We also noted significant negative relationship between PLT and MPV as well as PDW in this group. The last parameter correlated positively with MPV. There were no significant correlations between PLT, PDW, MPV, and hemoglobin as well as CRP in healthy girls (Table 3).
Spearman Correlations Between PLT (×103/μL), MPV (%), PDW (%), and Other Clinical Parameters in the Patients With Anorexia Nervosa.a
Abbreviations: BMI, body mass index; CRP, C-reactive protein; Hb, hemoglobin; MPV, mean platelet volume; PDW, platelet distribution width; PLT, platelet count.
an = 25.
b P < .05.
Spearman Correlations Between PLT (×103/μL), MPV (%), PDW (%), and Other Clinical Parameters in Healthy Controls.a
Abbreviations: BMI, body mass index; CRP, C-reactive protein; Hb, hemoglobin; MPV, mean platelet volume; PDW, platelet distribution width; PLT, platelet count.
an = 24.
b P < .05.
Discussion
The novel finding of our study was that patients with AN exhibited significantly increased PDW compared to the healthy controls. In addition, we confirmed that AN was associated with lower PLT.
We reported previously the incidence of thrombocytopenia in patients with AN ranges from 5% to 11%. 8 Changes in peripheral blood cell count in patients with AN are generally attributed to starvation-mediated gelatinous marrow transformation and bone marrow atrophy; such changes may also be due to multiple vitamin and mineral deficiencies, resulting from inadequate oral caloric intake. 9,17 These deficiencies disappear completely and rapidly following sufficient refeeding. 7,8
Some authors 8 reported correlation between low PLT and duration of the eating disorder. However, this trend was not confirmed in our group of patients.
Our most interesting finding was a significant increase in PDW in the AN group. However, only 2 patients with AN were found to have PDW above the normal range. Lower PLT may explain higher values of PDW in those patients. Production of platelets in the bone marrow is known to increase in response to a decreasing PLT. The newly produced platelets can be larger and more reactive. 11 –13 Interestingly, statistical differences were found for PDW, but not for MPV.
A plausible explanation might be found in the fact that PDW could potentially provide more information on thrombopoiesis than MPV. Since PDW is strongly correlated with differences in the platelet volume, higher PDW may be an indicator of dysregulated thrombopoiesis. 18 –20 Our results are consistent with previous observations of patients with the sickle cell disease (SCD). The PLT in those patients was within normal ranges, while MPV did not differ from the values observed in the non-SCD group. However, PDW was higher, which indicated the production of subfunctional platelets. 21 Moreover, Bowles et al pointed to the association of the platelet size with the degree of bone marrow disease, lower in thrombocytopenic patients with bone marrow disorders compared to thrombocytopenic patients with reduced platelet survival. 22 Therefore, higher PDW values and lower PLTs might confirm dysregulation of thrombopoiesis in AN, which is more likely associated with gelatinous transformation of the bone marrow affecting variability of the platelet size. 8
It has been accepted that bone marrow atrophy and gelatinous transformation are characteristic findings in patients with AN; these findings are likely to be associated with body fat mass index rather than duration of the illness. 8,17 In our study, PDW correlated positively with both, the duration of the illness and the rate of body weight loss, which might define the severity of AN. Under normal circumstances, there is an inverse relationship between platelet size indices and their number, which was confirmed in our control group. 23 This association was not observed in AN patients.
Higher PDW in AN might not reflect the inflammatory response because activation of systemic inflammation, including the acute phase response (APR), does not seem to be a feature of AN; this fact was also confirmed in our study. Serum CRP concentration, the best marker of APR 24 in our patients, did not differ significantly from that of the healthy controls. Furthermore, the decrease in PLT and the increase in PDW were not correlated with serum CRP concentrations.
Platelet size is the indicator of platelet reactivity and production of proaggregating mediators. Both metabolically and enzymatically, larger platelets can be more active than smaller platelets. However, it has not been documented that patients with AN have higher prothrombotic status, 25 which may be partially explained by lower PLTs in patients with AN. 21 Moreover, the relationship between platelet reactivity in vitro and their function in vivo in different diseases is controversial and has not yet been clearly resolved. 26 The role of platelets in atopy and in allergic diseases, especially the atopic dermatitis has been demonstrated. 27,28
Limitations
The main limitation of our study is a relatively small sample size, due to the rare incidence of AN. Furthermore, we only considered the newly diagnosed cases of AN (before therapy). Nevertheless, we were able to observe statistically significant differences in PLT and morphological parameters between patients with AN and the healthy participants. Platelet activation is a well-characterized multistep process, which may be assessed by different methodologies. However, it is not possible to use universal platelet function tests to assess all platelet functions. Increased MPV may reflect either the production rate (the presence of increased number of larger, more reactive platelets) or platelet activation (shape changes from discoid to spherical and pseudopodia formation). The PDW can represent heterogeneity of the platelet volume (anisocytosis). Large platelets are more reactive in vitro and correlate with platelet activity; measured by aggregation, release reaction, and expression of glycoprotein Ib and IIb/IIIa receptors measured by in vivo and in vitro tests. The discussed changes in shape and size of PDW platelets seem to be a more specific marker of platelet activation than MPV. Mean platelet volume and especially PDW increase during platelet activation are easy to be determined by automated hematology analyzers; therefore, they are commonly used upon multiple preliminary evaluations, especially in large populations. However, interpretation of the results should take into consideration limitations of the method itself, including variability in measurement of platelet volume indices and lack of definitive prospective evaluation of cutoff values. 18,29–32
Repeated measurements of platelet indices in the same patients, before therapy and after weight gain, seem essential for accurate interpretation of our results.
Conclusion
Anorexia nervosa in adolescents is associated with decreased PLT along with increased PDW, which may be indicative of dysregulated thrombopoiesis. These findings are likely to result from the changes in bone marrow function, due to starvation-mediated gelatinous transformation. 8 The potential use of platelets as a prognostic biomarker in AN is still to be investigated.
Footnotes
Authors’ Note
Joanna Oświęcimska and Alicja Kasperska-Zajac have contributed equally to the recent work.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
