Abstract
The European Clinical Laboratory and Molecular (ECLM) classification of von Willebrand disease (vWD) is based on the splitting approach which uses sensitive and specific von Willebrand factor (vWF) assays with regard to the updated molecular data on structure and function of
Keywords
Introduction
The classification of congenital von Willebrand disease (vWD) is dominated by the recommendations of the von Willebrand factor (vWF) Scientific Standardization Committee (vWF-SSC) of the International Society on Thrombosis and Haemostasis (ISTH).
1
–5
The ISTH classification of patients with vWD type 1 is based on quantitative measurement of factor VIII coagulant activity (FVIII:C) and vWF antigen (vWF:Ag) and 3 insensitive laboratory tests of vWF ristocetine cofactor (vWF:RCo) activity, ristocetine-induced platelet aggregation (RIPA), and vWF multimers in low-resolution gel.
1
As vWF multimeric analysis in a low-resolution gel has a low sensitivity to distinguish the various variant of vWD type 1 and type 2, the ISTH vWD classification cannot clearly distinguish between the pronounced variants of type 1 from type 2M or 2E vWD at vWF levels below 0.20 U/mL.
2
–5
The ISTH vWD classification mainly used a “lumping” approach for the classification of type 2 vWD.
1
Dominant vWD type 2E is usually present with a laboratory vWD phenotype 1, and diagnostic differentiation of pronounced type 1 vWD from type 2E and type 2M vWD using the SSC-ISTH criteria remains a persistent problem in routine daily practice. The ISTH vWD classification is not based on structural and functional relationship of
Clinical, Laboratory, and Molecular Diagnosis and Classification of vWD 2016
The European clinical laboratory and molecular (ECLM 2016) classification of vWD following the recommendations of Budde and Schneppenheim, Michiels et al, and Gadisseur et al is based on the splitting approach by the use of vWF-specific and -sensitive diagnostic tools in view of new molecular data on structure and function of
Laboratory Characteristics of the European Clinical Laboratory and Molecular (ECLM) Classification of Von Willebrand Disease Type 1 Autosomal Recessive Severe Types 1 and 3, 2C and 2N Versus Autosomal Dominant Type 1 Secretion Defect (SD) and Types 2A, 2B, 2E, and 2D anno 2016.

Abbreviations: CB, collagen binding; GPIb, glycoprotein Ib; vWD, von Willebrand disease; vWF, von Willebrand factor, MM, multimers.
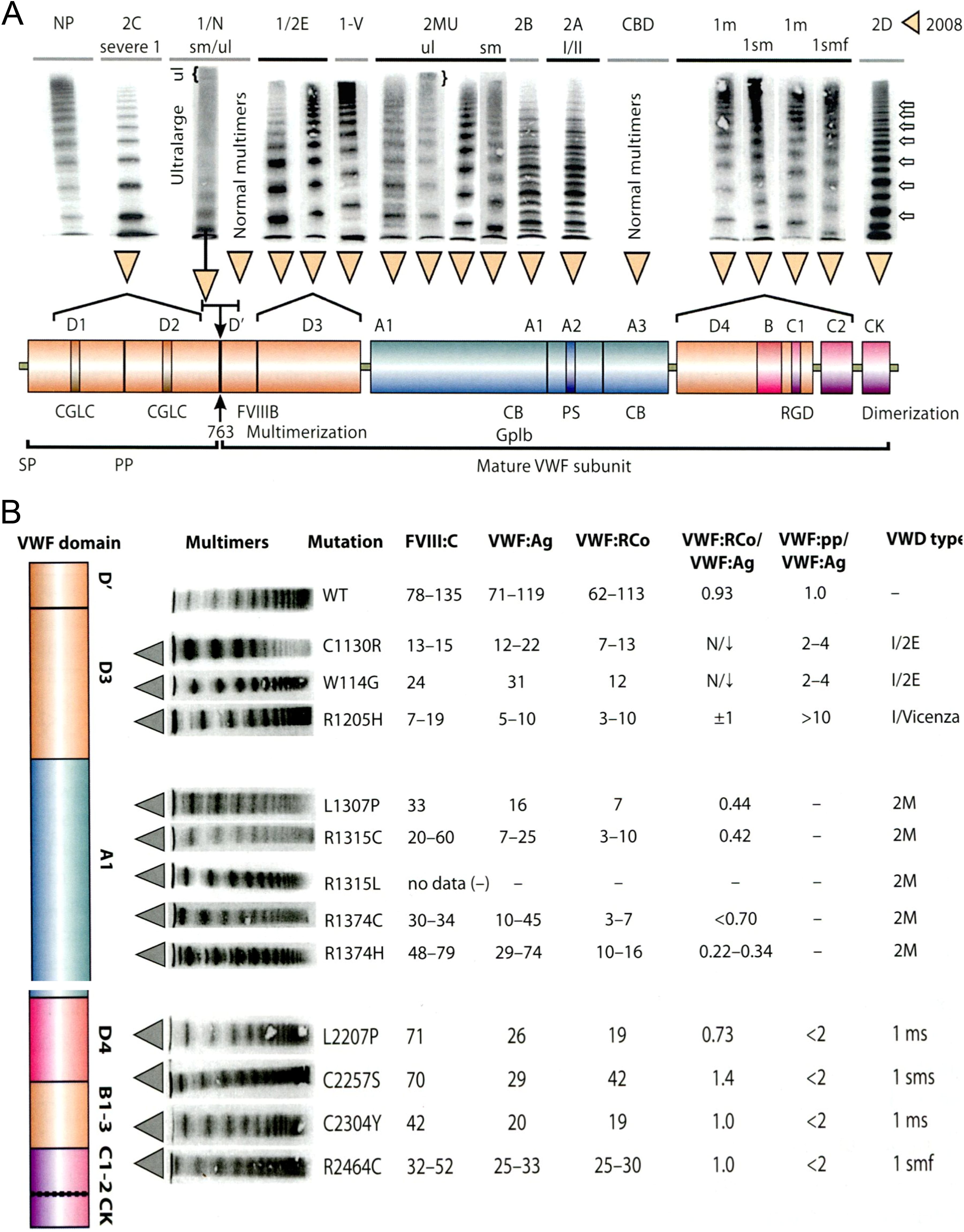
A and B, Clustered distribution of von Willebrand disease (vWD) types 1 and 2 with abnormal von Willebrand factor (vWF) multimers in medium-resolution gels for the classification of types 1 and 2 vWD related to mutations in the D1, D2, D3, A1, A2, D4B1-3, C1-2, and CK domains of vWF (A and B). In vWD 2A due to mutations in the A2 domain (A), there is a lack of large vWF multimers and the outer subbands of the individual triplets are markedly pronounced. von Willebrand disease type 2B due to gain-of-function mutations in the A1 domain cannot be distinguished from vWD 2A because their multimer patterns of pronounced triplet structure of each vWF band are very similar (A). In vWD 2C due to mutations in the D1 and D2 domains (A), there is a lack of large vWF multimers and absence of triplet structure of the individual bands. The first band (dimer) and second band (tetramer) are markedly pronounced. In vWD 2E due to mutation in the D3 domain (A and B), the vWF multimers show lack or relative decrease in large multimers and the absence of the outer subbands of normal triplets, which give the individual multimers a broader appearance. In vWD 2M due to the loss of functional mutations in the A1 domain (A and B), the vWF multimers are variable from normal to smeary pattern with some loss or the presence of large multimers. In vWD type 1 due to mutations in the D4–B1-3–C1-3 domain (A and B), the vWF multimers are normal with some minor smearing pattern (1 m or 1 ms) or with a pronounced smearing pattern (1 sm). The vWF multimers are normal in vWD 2N and vWD collagen-binding defect (CBD). Type 2N mutations that involve a cysteine (C788R/Y, Y795C, and C804F) are associated with aberrant multimerization.
Three main categories of vWD can be distinguished: first autosomal recessive type 3 and severe type 1 vWF:RCo <10U/dL, second dominant types 1 (vWF:RCo 10-30 U/dL) and 2, and third a large group of mild vWD type 1 (vWF:RCo 30-50 U/dL) with no or low penetrance of bleeding manifestations.
7,12,13
The mild, moderate to pronounced vWD type 1 is a quantitative vWF deficiency with equally decreased values of all vWF parameters and a normal ratio of vWF:RCo/Ag and vWF:CB/Ag (>0.70) before and after DDAVP (Table 1). von Willebrand disease type 2 is a qualitative vWF deficiency with normal, near normal, or decreased levels for FVIII:C and vWF:Ag, and much lower values for vWF:RCo and vWF:CB with decreased vWF:RCo/Ag ratio and vWF:CB/Ag ratio (<0.70; Table 1). von Willebrand factor multimeric analysis using low- and medium-resolution gels clearly distinguish vWD type 2A, 2C, 2E, 2D, and 2M (Figure 1A and B).
7,12
–14
The responses of FVIII and vWF parameter to intravenous DDAVP is an essential tool to distinguish pseudo-vWD from mild type 1 and to separate in a much better manner the various variants of autosomal dominant types 1 and 2.
2,5,6
The interpretation of vWF response curves to DDAVP has significant therapeutic implications for the different variants of dominant type 1 and type 2 vWD mutations for both clinicians and patients with vWD.
2,6,15,16
Responses of FVIII:C and vWF parameters to DDAVP related to the structural and functional relationship between laboratory phenotype and expression studies of
The Spectrum of vWD Type 1 and Type 2: The Experience of 1 Center From 1990 to 2010
Between 1992 and 1997, the Rotterdam vWD study group analyzed 295 index cases of patients coded as vWD irrespective of blood O or non-O in the Erasmus University Medical Center, Rotterdam, with a referral region of about 2 million inhabitants. 2 The first group of 128 (46.5%) index patients had vWF antigen and functional levels of around 40% to 60%, a very mild bleeding tendency, no family history, normal Ivy BTs, usually showed normal responses of vWF and FVIII:C to DDVAP when tested on indication, do not have vWD, and were diagnosed as pseudo–von Willebrand (Figure 2, left). 2 –6 The second group of 167 index patients of 94 families were diagnosed diagnosed as ISTH defined mild vWD type 1 in 65 families; severe dominant vWD type 1 in 10 families (of which 2M in 3); types 2A, 2B, and 2N in 10, 4, and 2 families; and recessive type 3 in 3 families, respectively. 2 The diagnosis of mild vWD type 1 was based on a personal bleeding history and decreased values for FVIII:C, vWF:Ag vWF:RCo, and vWF:CB with normal ratios for vWF:RCo/Ag and vWF:CB/Ag. Bleeding manifestation in the proband of 24 index family cases of vWD type 1 was usually mild and occasionally moderate. The Ivy BTs were normal or only slightly prolonged in only a few cases. The values for vWF:Ag vWF:RCo and vWF:CB were between 0.20 and 0.60, with normal ratios for vWF:RCo/Ag (0.62-1.08) in all and also for vWF:CB/Ag in 21 of the 24 cases of mild vWD type 1.
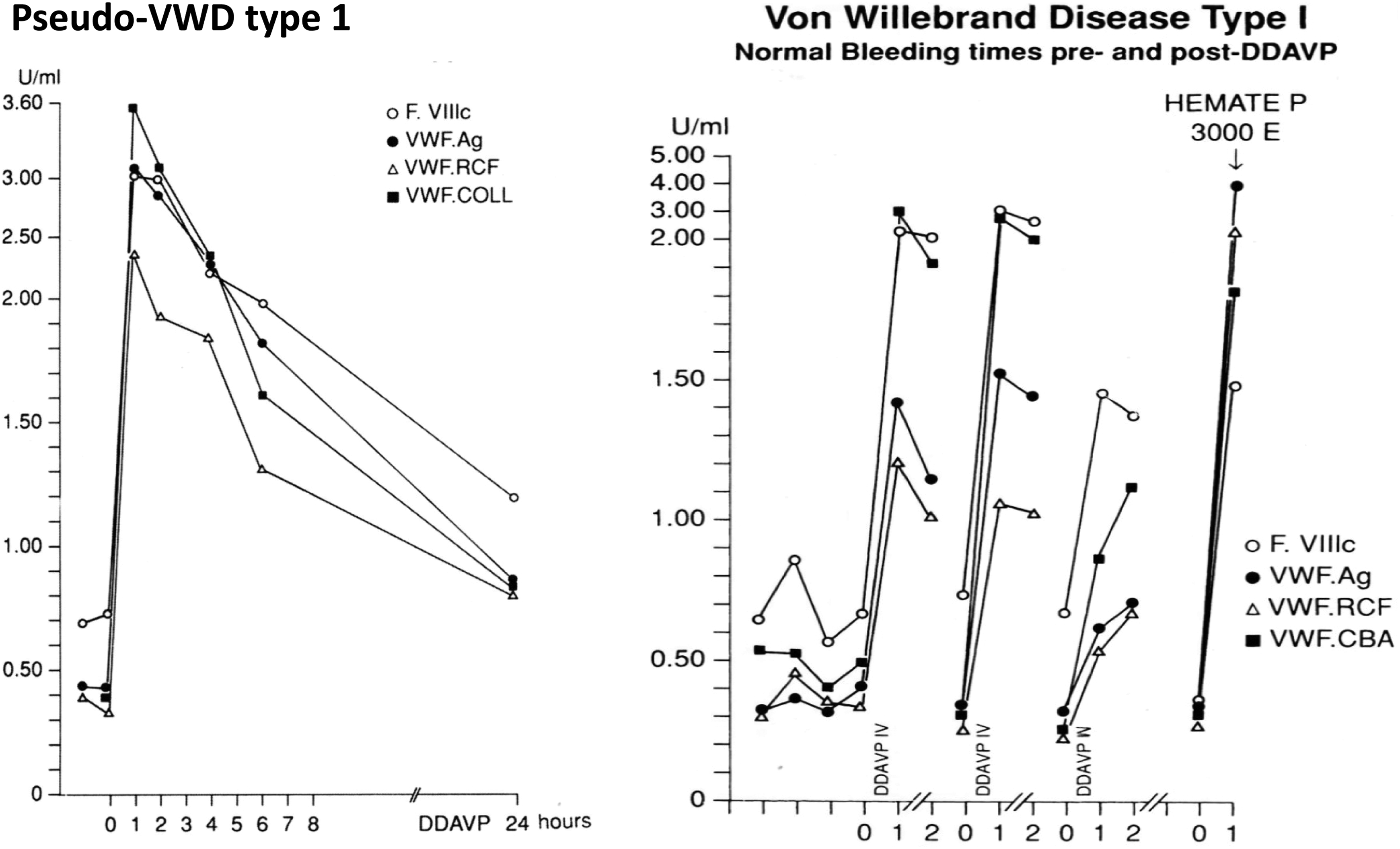
Left: Completely normal responses of FVIII: C and von Willebrand factor (vWF) parameters to DDAVP from around 0.4 U/mL to high levels of 2.5 to 3.6 U/mL followed by normal half-life times of vWF antigen (Ag) and ristocetine cofactor (RCF) and collagen binding (COLL) activities consistent with the diagnosis of pseudo–von Willebrand disease (pseudo-vWD). 2 Right: Restricted responses to DDAVP of vWF ristocetine cofactor (vWF:RCF) and vWF collagen-binding activity (vWF:CBA) as compared to vWF: Ag and FVIIIC consistent with mild vWD type 1.
The responses of the vWF parameters to DDAVP in the 24 probands with mild vWD type 1 were normal, showing a 2- to 10-fold increase in vWF:Ag and vWF:RCo. The vWF:RCo/Ag ratio remained normal (0.65-1.19) after DDAVP in all 24 vWD type 1 patients. The majority of vWD type 1 patients showed significantly higher peak values of vWF:CB immediately after DDAVP, which resulted in significantly higher vWF:CB/Ag ratios (1.4-2.8) after DDAVP. The group of 24 probands of vWD type 1 could be separated in a group of 14 probands with normal biological half-life times of the vWF parameters, which we classified as pseudo-vWD (Figure 2, left) and a group of 10 probands with restricted responses of vWF:RCo as compared to vWF:Ag (Figure 2, right) followed decreased half-life times of vWF parameters. 2 Three patients with suspected mild vWD type 1 but completely normal responses to DDAVP (Figure 2, left) underwent major surgery including laparoscopic cholecystectomy, uterine extirpation, and orthopedic surgery under the cover of 1 dose DDAVP (0.3 µg/kg intravenous preoperatively and on day 1). No bleedings were noted in the perioperative and postoperative period. In a case of symptomatic mild vWD type 1 (Figure 2, right) featured by bruises and moderate menorrhagia since adolescence, we compared the effect of intravenous (IV) DDAVP, intranasal DDAVP, and 1 dose of 3000 units Humate-P (40 U/kg; Figure 2, right). DDAVP showed a restricted response of vWF:Ag and vWF:RCo to values around 1.5 U/mL and normal response of FVIII:C and vWF:CB to values between 2.0 and 3.0 U/mL, whereas the responses of DDAVP intranasal were rather poor as compared to DDAVP IV and Humate-P (Figure 2, right). 2 In 2003, Sadler extended the 2002 concept of Michiels et al 2 in distinguishing pseudo-vWD versus mild, moderate, and severe vWD by the combined use of vWF multimeric analysis and a DDAVP challenge test. Sadler calculated that most diagnoses of mild vWD type 1 are false positive vWD labeled as pseudo-vWD by Michiels et al 17 In the general population, 25% have 1 or 2 mild bleeding (clinically insignificant) and 2.5% low plasma vWF, indicating that 0.25 × 0.025 = 0.6% individuals in the general population have a chance of low vWF and bleeding just by chance. 17 Patients with mild vWD type 1 with levels for vWF:Ag, vWF:RCo, and vWF:CB between 0.30 and 0.60 U/mL and normal ratios for vWF:RCo/Ag and vWF:CB/Ag usually present with no or mild bleeding symptoms, no family history of bleeding, and normal Ivy BTs, and normal PFA-CTs on repeated occasions.
Diagnostic Differentiation of Dominant vWD Type 1 versus 2M versus Vincenza
In 2002, the Rotterdam vWD study group analyzed the clinical and laboratory features and DDAVP responses of dominant vWD type 1 in 10 families (of which 2M in 3), and in vWD type 2A, 2B, and 2N in 10, 4, and 2 families, respectively. 2 The FVIII and vWF parameters in 6 probands with pronounced autosomal dominant vWD and vWF levels between 0.07 and 0.20 U/mL are presented in Table 2. 2 Correct typing of such pronounced cases of vWD as type 1 versus 2M versus Vicenza by the vWF:RCo/Ag ratio is problematic because of the low sensitivity of the vWF:RCo assay at vWF:Ag levels below 0.20 (Table 2). The vWF:CB/Ag ratio was normal in all 6 probands with pronounced vWD type 1 (Table 2). RIPA is normal in vWD type 1 (probands 1, 2, 3, and 6) and decreased in vWD 2M (probands 4 and 5; Table 2). The probands 1 and 2 in Table 2 were diagnosed as pronounced vWD type 1 with a bleeding tendency since early childhood, normal RIPA, normal to slightly prolonged Ivy BT, and normal vWF multimeric pattern. In 3 family members of proband 3 (mother P1, brother P2, and daughter P3; Figure 3, left), the response to DDAVP was high for FVIII:C but decreased for all vWF parameters (Figure 3, left), and the vWF multimeric pattern in medium-resolution gels is normal consistent with vWD type 1. Such high ratios of FVIII:C/vWF:Ag above 3 before and after DDAVP in pronounced vWD type in the family members of proband 3 (P1 and P2; Figure 3, left) are indicative of an secretion defect (SD) of vWF from endothelial cells as the main cause of pronounced vWD type 1. 2
Dominant vWD Type 1 Secretion Defect (High FVIII/vWF:Ag Ratio) Caused by S2179F Mutation in D4 Domain in 3 Families With vWD SD (secretion defect). 18,19,a
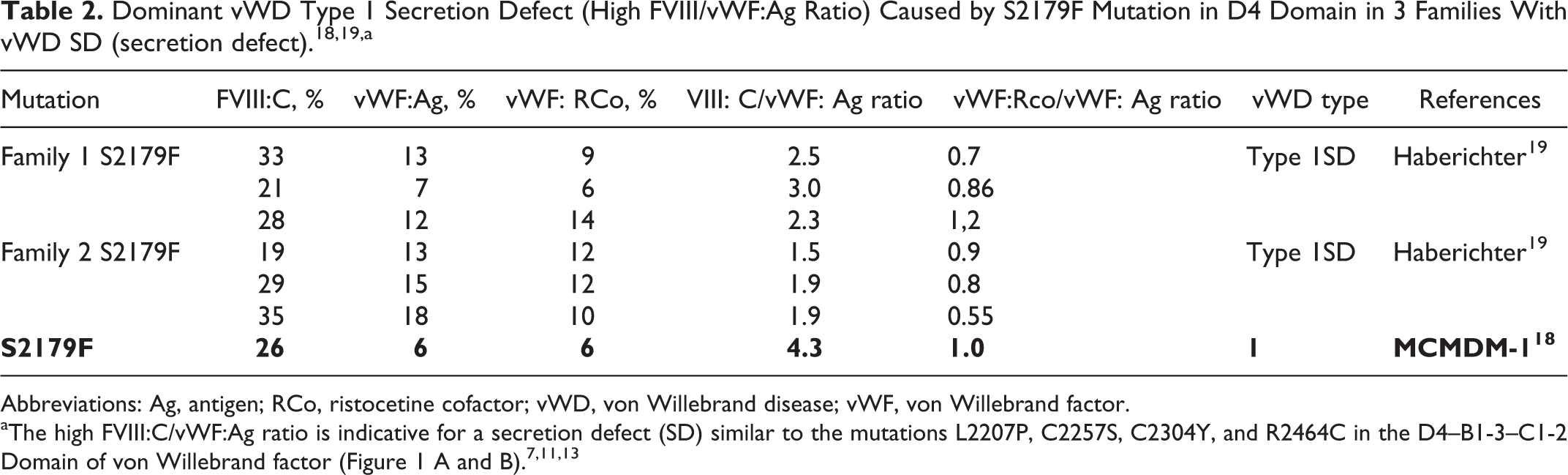
Abbreviations: Ag, antigen; RCo, ristocetine cofactor; vWD, von Willebrand disease; vWF, von Willebrand factor.
aThe high FVIII:C/vWF:Ag ratio is indicative for a secretion defect (SD) similar to the mutations L2207P, C2257S, C2304Y, and R2464C in the D4–B1-3–C1-2 Domain of von Willebrand factor (Figure 1 A and B). 7,11,13
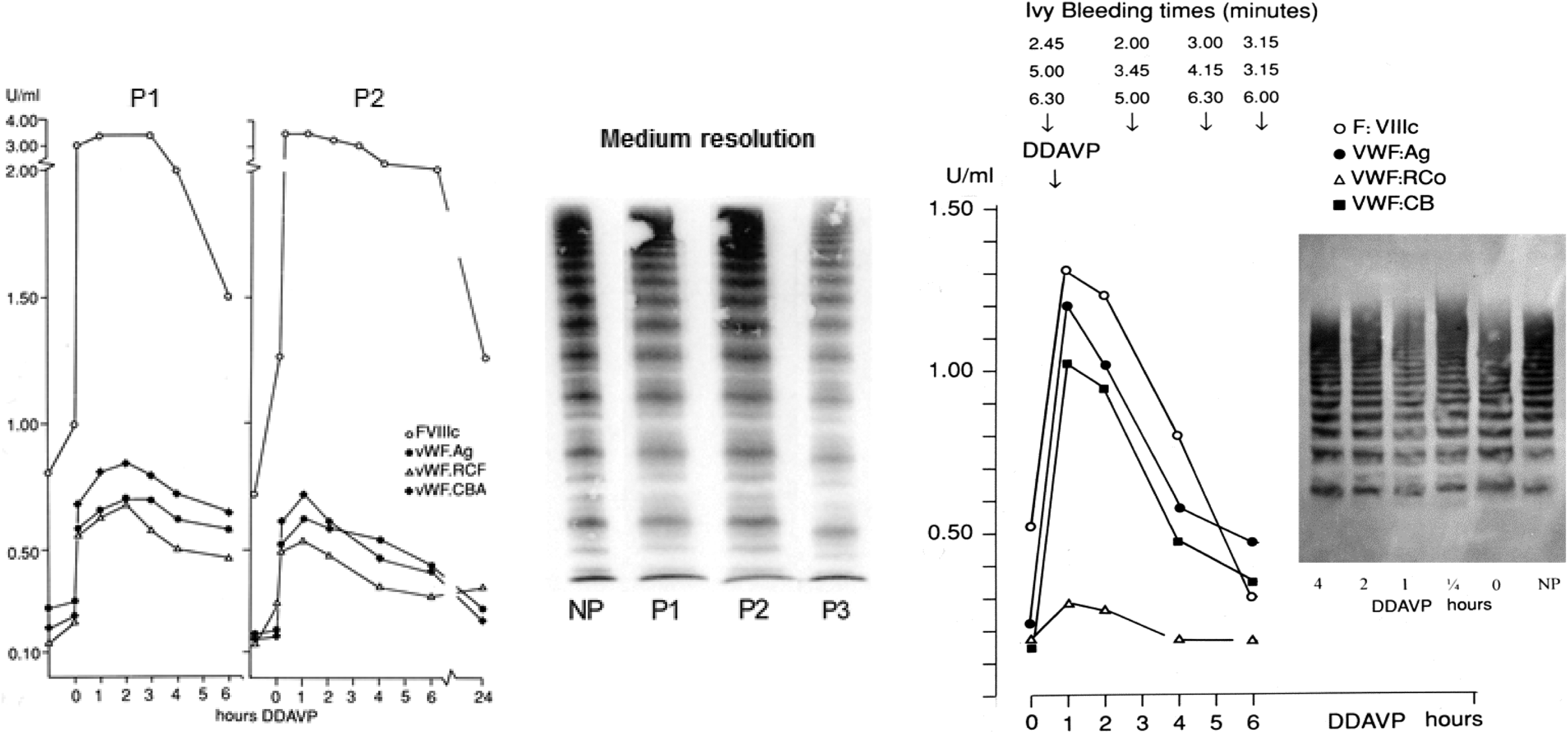
Left: DDAVP responses in pronounced type 1 von Willebrand disease (vWD) showing a normal response of FVIIIC and restricted responses to DDAVP of all von Willebrand factor (vWF) parameters in 2 members of 1 family (proband and her brother, proband 3 in Table 2). The high FVIII/vWF:Ag ratio before and after DDAVP with normal vWF multimers in medium-resolution gels according to Budde 14,15 is consistent with the diagnosis of vWD type 1 secretion defect (SD 2 ). Right: Poor response of vWF:RCo to DDAVP and fairly good responses to DDAVP of FVIII:C, vWF:Ag, and vWF: CB in a case of pronounced vWD 2M with normal vWF multimers before and after DDAVP (cases 4 and 5 in Table 2) showing normal vWF multimeric pattern in low-resolution gel according to Michiels et al. 2 Interestingly the half-life times of FVIII:C, vWF:Ag, and vWF:CB are shortened in pronounced vWD 2M indicative of an additional rapid clearance defect (CD) of the FVIII-vWF complex.
The probands 4 and 5 in Table 2 had overt vWD with moderate bleeding tendency particularly after trauma and surgery with vWF levels below 0.20 U/dL for all vWF parameters, normal vWF multimers in low-resolution gel before and after DDAVP (Figure 3, right), a decreased RIPA and a slightly prolonged Ivy BT (Table 2). The response to DDAVP of vWF:Ag and vWF:CB was rather good, but the response of vWF:RCo to DDAVP was poor (Figure 3, right), indicative of vWD 2M. The half-life times of FVIII:C, vWF:Ag, and vWF:CB post-DDAVP were significantly shortened, indicative of a rapid clearance of the FVIII-vWF complex. The laboratory diagnosis findings in probands 4 and 5 of these 2 families with vWD 2M 2 –6 are typically featured by decreased RIPA; normal vWF multimers before and after DDAVP; decreased response of vWF:RCo to DDAVP and good responses of FVIII:C, vWF:Ag, and vWF:CB to DDAVP followed by rapid clearance of the FVIII-vWF complex.
As shown in Table 2, proband 6 mother and her son had a well-documented autosomal dominant hemophilia-like bleeding tendency associated with occasional hemarthrosis, recurrent hematomas after trauma and muscle bleeding, and recurrent mucocutaneous bleeding since early childhood. Laboratory investigations were consistent with severe vWD type 1 with normal ratios for vWF:RCo/Ag and vWF:CB/Ag, normal RIPA, and vWF multimers on repeated testing. Multimeric analysis of vWF from plasma showed normal vWF multimeric pattern in low- and medium-resolution gels before and after DDAVP. The response to DDAVP 1 hour post-DVT showed completely normal responses of FVIII:C, vWF:Ag, vWF:RCo, and vWF:CB with peak levels 15 minutes post-DDAVP followed by very short half-life time of FVIII and all vWF parameters consistent with the rapid clearance of the FVIII-vWF complex. Such cases with pronounced autosomal dominant vWD type 1 due to rapid clearance (C) of both FVIII and vWF parameters have been described in the vWD literature as vWD type 1 Vicenza (Figure 1B).
Von Willebrand Disease Type 1 With Normal or Smeary vWF Multimeric Pattern Due to Mutations in the D4, B1-3, and C1-2 Domains of vWF
The Canadian and European vWD-1 studies discovered a new category of vWD type 1 due to mutations in the D4, B1-3, and C1-2 domains of the
Prospective Evaluation of vWF Responses to DDAVP in vWD Type 1 and Type 2
Between 1998 and 2008, the Rotterdam vWD study group prospectively evaluated the responses of platelet function analysis closure times (PFA-CTs) vWF:Ag, vWF:CB, and FVIII before and 1 hour after DDAVP (0.3 μg/kg) in patients with vWD type 1 (n = 70). 16 Pretreatment values of FVIII:C and vWF parameters in 70 patients labeled as vWD type 1 ranged from severe, moderate, and mild vWF deficiency to normal values. The PFA-CTs were normal or in the upper region of normal (>300 seconds) in the majority and prolonged (>300 seconds) in only a few cases of vWD type 1. The patients with vWD type 1 treated with DDAVP demonstrate a good dose–response with correction of the PFA-CTs in all patients with vWD type 1. Normalization of the PFA-CTs (< 150 sec) was reached at functional vWF:RCo and vWF:CB levels of 0.75 U/mL and above. Based on the response of vWF:RCo to DDAVP, patients with vWD type 1 were categorized into 2 groups. First, those with restricted responses of vWF:RCo , that is, up to a maximum of 0.50 and 1.2 U/mL (Figure 2, right). 2 Second those with maximal values of vWF:RCo to above 1.5 to 4.5 U/mL indicating complete normal responses to DDAVP in patients (individuals) who in fact do not have vWF deficiency (pseudo-vWD; Figure 2, left). 2,16
Between 1998 and 2008, the Rotterdam vWD study group evaluated the responses of PFA-CT, vWF parameters, and FVIII:C before and after DDAVP in 24 patients with vWD type 2 (n = 14: 8 type 2A, 2 mild type 2, and 4 type 2M). 16 The PFA-CTs were prolonged (<300 seconds) in all patients with vWD type 2 except in 2. None of the patients with severe vWD type 2A showed a transient correction of the PFA-CTs 1 hour after DDAVP. In contrast, patients with vWD type 2M or mild-type 2A (N = 6) showed a transient correction of PFA-CTs to near normal or normal values (<150 seconds) 1 hour post DDAVP. Normal responses of PFA-CT to DDAVP is dependent on the transient correction of functional plasma vWF:CB and the vWF:CB/Ag ratio together with correction of plasma vWF multimer distribution with the reappearance of large multimers.
Diagnostic Differentiation of Dominant vWD 2E Versus 2M Versus 2A
Patients with vWD type 2E caused due to vWF mutations in the D3 domain have laboratory features of dominant vWD type 1 with a type 2E vWF multimeric pattern in low- and medium-resolution gels (Figure 1A and B).
7,13
Schneppenheim described 22 different mutations in the D3 domain of the
2010 Update on Von Willebrand Disease (vWD) Type 2E Due to Missense Mutations in the D3 Multimerization Domain of the Von Willebrand Factor (vWF; Exons 22, 23, 24, 25, 6, and 27) and Related Laboratory Phenotype Type 2 or Type 1 (bold) According to vWF:RCo/Ag or vWF: CB/Ag Ratios in 19 Patients With a vWD type 2E Multimeric Pattern. 23,a
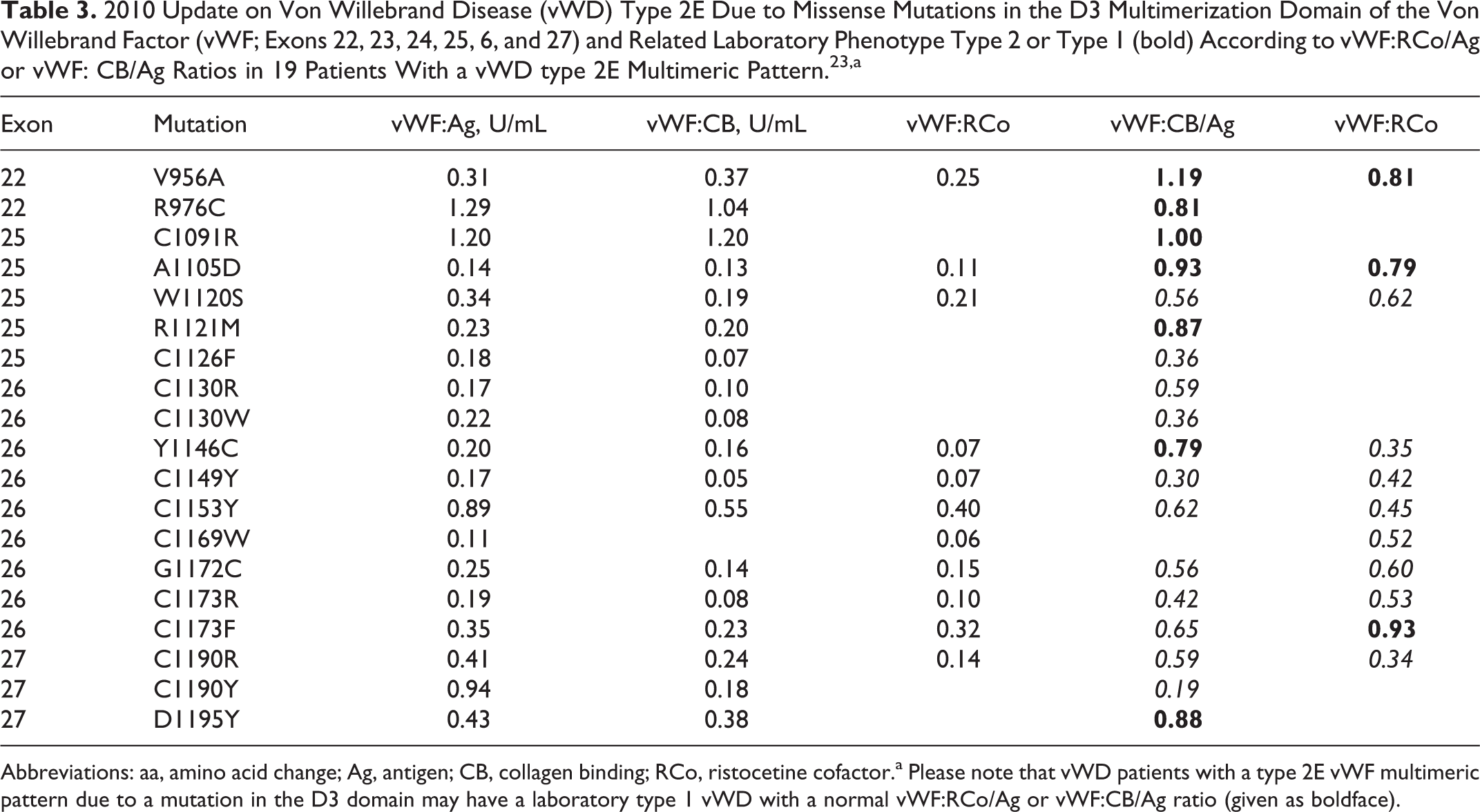
Abbreviations: aa, amino acid change; Ag, antigen; CB, collagen binding; RCo, ristocetine cofactor.a Please note that vWD patients with a type 2E vWF multimeric pattern due to a mutation in the D3 domain may have a laboratory type 1 vWD with a normal vWF:RCo/Ag or vWF:CB/Ag ratio (given as boldface).
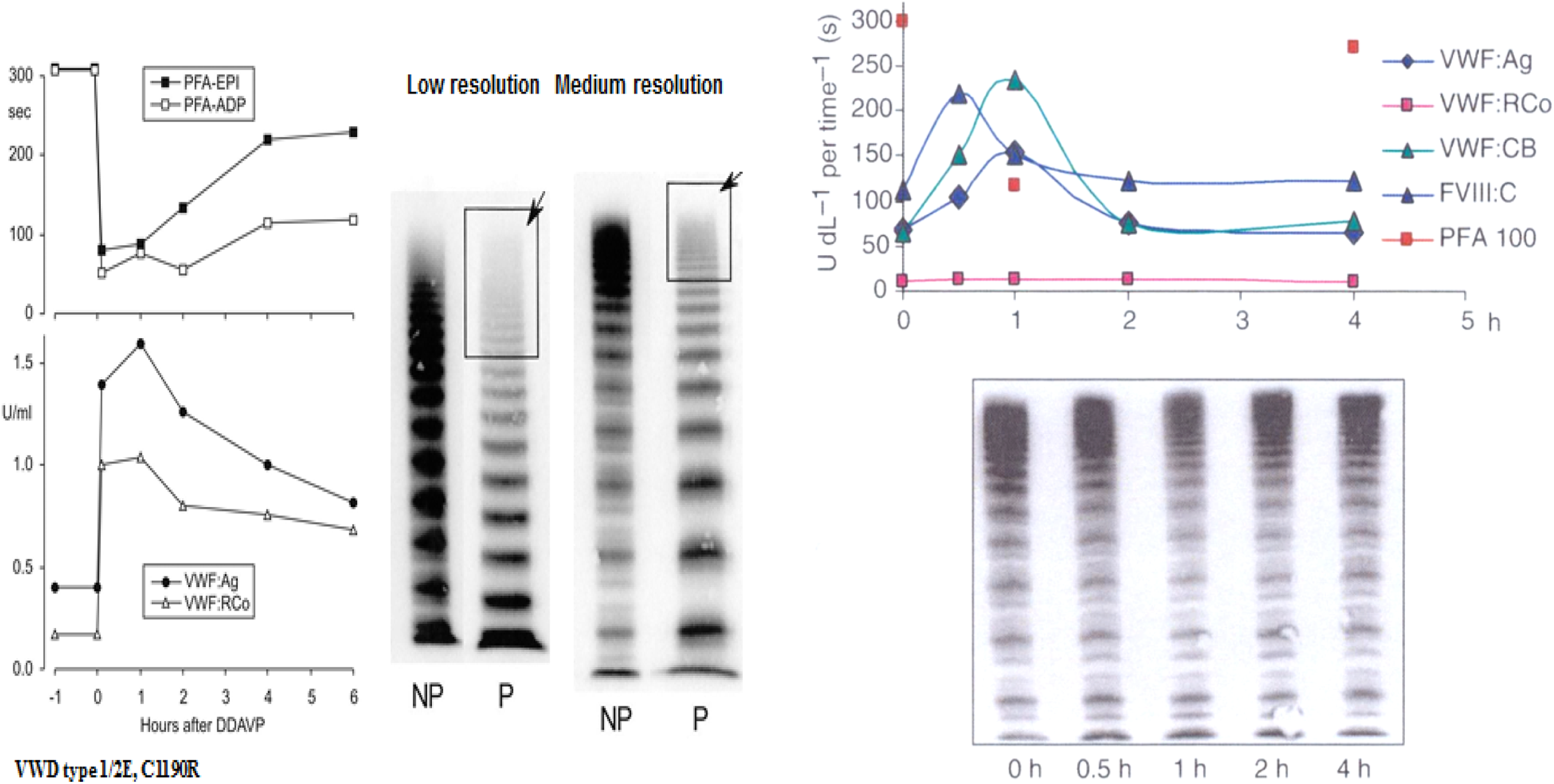
Left: von Willebrand disease (vWD) 2E: Transient correction of PFA-100 closure time and restricted increase of von Willebrand factor (vWF) parameters from around 0.20-0.40 U/mL to around 1.0 U/mL in a case of vWD type 2E (mutation W1120S). The vWF multimeric pattern is characterized by a lack or relative decrease in large multimers and the absence of the outer subband of the normal triplet structure. Please note that both low- and medium-resolution gels according to Budde show a typical vWF 2E multimeric pattern. 17,18 Right: von Willebrand disease 2M: poor response of vWF:RCo to DDAVP, normal vWF multimers before and after DDAVP, and good responses of FVIII:C, vWF:Ag, and vWF:CB followed by shortened half-life time indicating rapid clearance defect of the FVIII-vWF complex in addition to the loss of vWF:RCo function in a typical case of vWD 2M with normal vWF multimers before and after DDAVP 17 in medium-resolution gel, according to Budde. 17,18
In a collaborative basic research, we identified a novel mutation V1499E with a high penetrance in a large Dutch family with autosomal dominant type 2A vWD, which was detected independently in 3 hospitals and academic coagulation laboratories (Table 4). 24 Three affected family members (II-1, III-1, and III-7) had been diagnosed more than 10 years ago (Table 4). The mutation V1499E was independently discovered in 2 vWF research laboratories. Proteolysis of recombinant mutant V1499E vWF by ADAMTS13 was increased consistent with consistent with vWD type 2A. 24 In vWD 2A, there is a lack of large multimers in low-resolution gels according to the methods. The loss of large vWF multimers with markedly pronounced triplet structure of the outer subbands due to increased proteolysis was only seen in medium-resolution gels but not in low-resolution gels (Figure 5). The loss of large multimers together with increased triplet subbands representing proteolytic vWF fragments originating from increased cleavage of vWF at the Y1605–M1606 bond is due to mutations in the A2 domain of vWF (Figure 1A). 15,16,24 –28 Original observations in this family with moderate dominant vWD type 2A group 2 caused by the V1499E mutation 2,6,24 and in 3 families with severe vWD type 2A group 1 (Table 4) 25 are completely in line with the observed heterogeneity of moderate type 2A versus severe type 2A vWD with regard to bleeding symptoms, laboratory phenotypes, and typical responses to DDAVP. Patients with moderate vWD 2A group 2 including the V1499E mutant are identified by normal or subnormal values for FVIII:C and vWF:Ag, vWF:RCo, that is, around 0.30 U/mL; normal RIPA at ristocetin concentrations of 1.2 or 1.75 mg/mL (Table 4); and show a complete but transient correction of large vWF multimers, BT, FVIII:C, and vWF parameters a few hours after DDAVP (Figure 5). 25 Patients with severe vWD 2A group 1 have low values for vWF:Ag, very low or undetectable level for vWF:RCo and vWF:CB, decreased or zero RIPA at high concentration of ristocetin 1.75 or 2.0 mg/mL (Table 4) and show a minor or poor response to DDAVP of functional vWF:RCo and vWF:CB with no correction of vWF multimers and BT directly after DDAVP. 15,25
Laboratory Features of Dominant vWD Type 2A in a Large Dutch Family With the Presence or Absence of the V1499E Mutation in 11 and 5 Family Members, Respectively.a
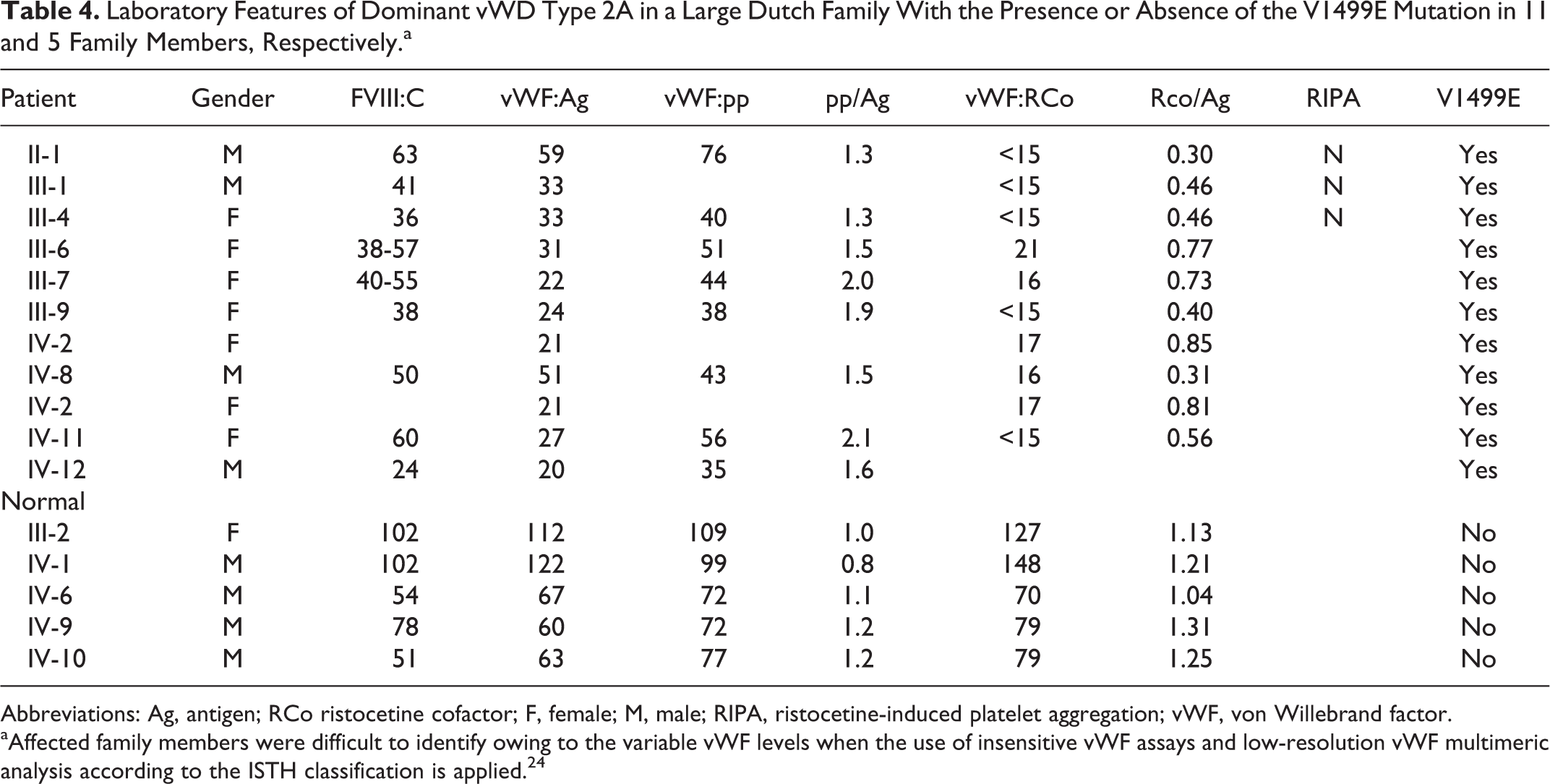
Abbreviations: Ag, antigen; RCo ristocetine cofactor; F, female; M, male; RIPA, ristocetine-induced platelet aggregation; vWF, von Willebrand factor.
aAffected family members were difficult to identify owing to the variable vWF levels when the use of insensitive vWF assays and low-resolution vWF multimeric analysis according to the ISTH classification is applied. 24
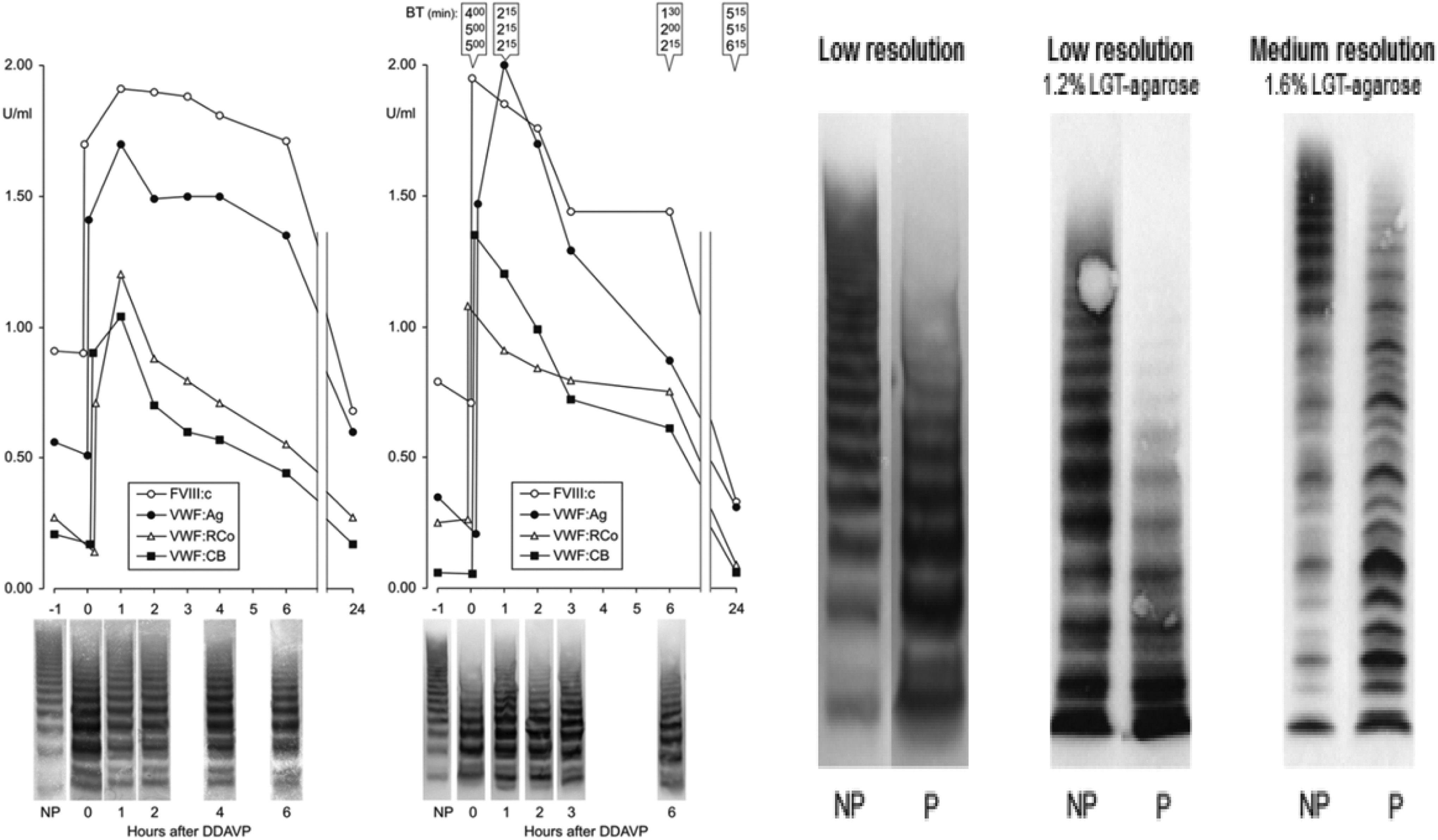
Left: Normal responses to DDAVP of FVIII:C and von Willebrand factor antigen (vWF:Ag) and restricted but transiently rather good responses of functional vWF:RCo and vWF:CB to about 1 U/mL with transient correction of Ivy bleeding times and reappearance of large vWF multimers in moderate vWD type 2A (mutation V1499E) followed by short half-life times of vWF:RCo and vWF:CB due to increased proteolysis of vWF multimers. von Willebrand disease (vWD) type 2A mutation V1499E is featured by the loss of large vWF multimers and increase in intermediate and small vWF multimers in low-resolution gels. 2,25 Right: Please note that the vWF multimers in low-resolution gels, according to the methods of Michiels et al (left) and Budde showing loss of large and increase of small vWF multimers, whereas the vWF multimeric pattern in medium-resolution gel according to Budde reveals the typical triplet structure diagnostic of vWD type 2A. 17,18
Von Willebrand Disease 2A Groups 2 and 1 Due to Mutations in the A2 Domain of vWF
The pertinent findings in patients with vWD type 2A include prolonged BT, consistently low vWF:RCo/Ag ratio and vWF:CB/Ag ratio, absence of large vWF multimers, pronounced triplet structure of individual bands, and increased vWF degradation products due to increased proteolysis (Figure 1; Table 5). von Willebrand disease type 2A results from missense mutations in the A2 domain, exon 28, of the
Laboratory Features of Severe Dominant vWD 2A Group 1 in 3 Unrelated Cases and Moderate vWD of Moderate vWD 2A Group 2 in 3 Related Cases of a large Family With the Mutation V1499E. 24,25

Abbreviations: Ag, antigen; BT, bleeding time; CB, collagen binding; F, female; RCo, ristocetine cofactor; M, male; RIPA, ristocetine-induced platelet aggregation; vWD, von Willebrand disease; vWF, von Willebrand factor.
The absence of high vWF multimers and increased triplet structure is the consequence of increased proteolysis of large vWF multimers (Figures 5 and 6). Structural changes within the A2 domain can produce 2 different characteristic phenotypes of type 2A vWD. 25 Expression studies demonstrated that the single missense mutations V1607D, S1506L, L1540P, and G1505R resulted in poor or no secretion of high molecular weight due to impaired transport of vWF multimers between the endoplasmic reticulum and the Golgi complex (the so-called vWD 2A group 1 defect) with very likely intracellular proteolysis of large vWF multimers. 26 –28 Expression studies demonstrated that at least 5 missense mutations in the A2 domain R1597W, G1505E, E1638K, I1628T, and L1503Q result in normal secretion of high-molecular-weight multimers similar to the wild-type multimers, indicating that subsequent loss-of-large vWF multimers is caused by hypersensitivity to ADMAMTS13 induced increased proteolysis in plasma (the so-called vWD 2A group 2 defect). 25 –28 Interestingly, platelet lysates demonstrated decrease in large vWF multimers for G1505L and S1506L mutants of vWD 2A group 1, but a normal pattern for the G1505E and R1597W mutants of vWD 2A group 2. This simply means that vWF of severe vWD 2A group 2 is already proteolysed in endothelial cells before secretion, whereas vWF in mild to moderate vWD 2A group 2 is secreted as large multimers that after secretion from endothelial are proteolysed due to hypersensitivity to ADAMTS13. 25
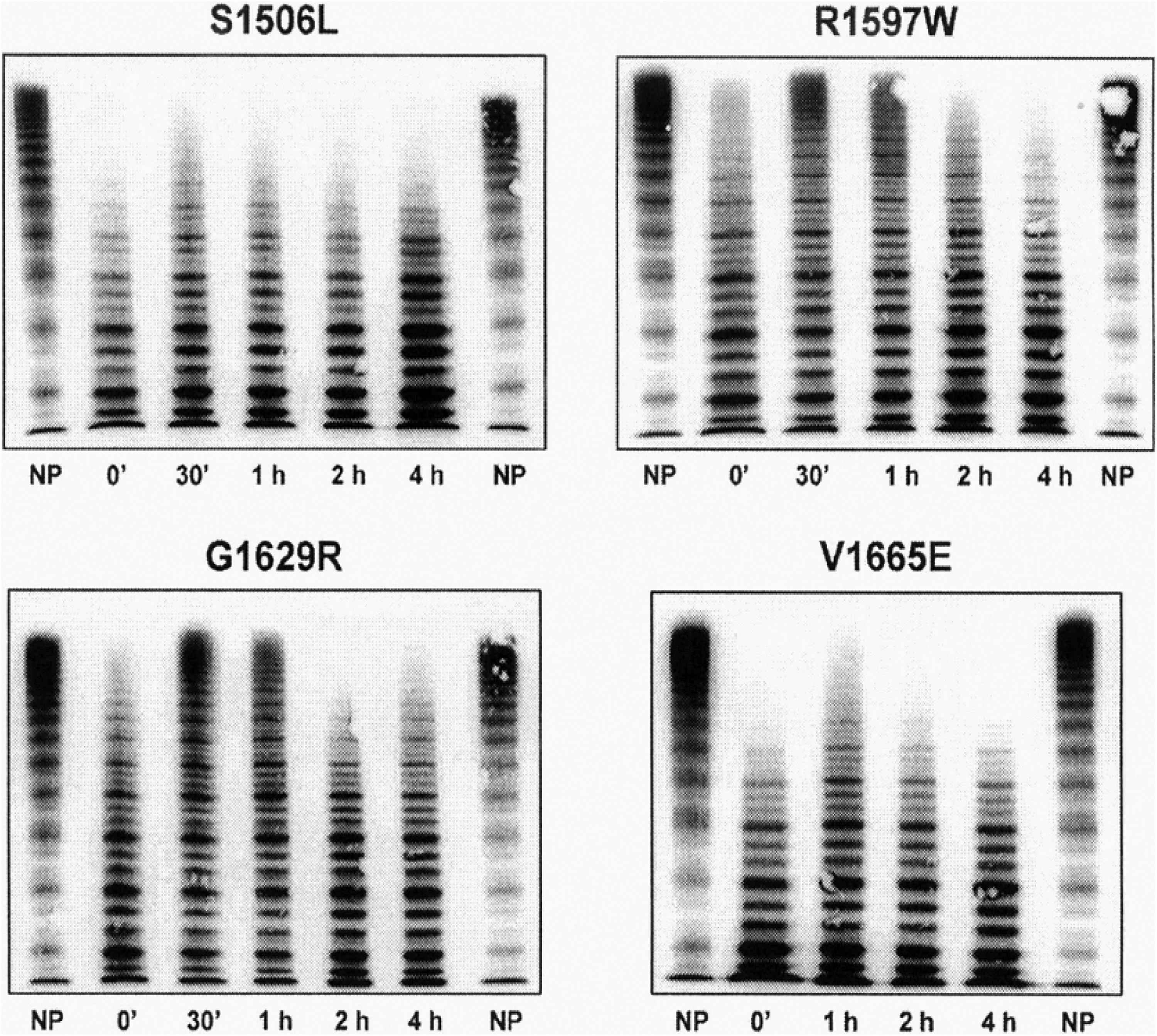
Responses to DDAVP of von Willebrand factor (vWF) multimeric pattern induced the transient reappearance of large vWF multimers in the von Willebrand disease (vWD) 2A type 2 caused by the mutations R1597W and G1629 in the A2 domain, indicating normal intracellular synthesis and secretion of vWF. Responses of vWF multimers to DDAVP did not induce reappearance of large vWF multimers in vWD 2A group 1, indicating impaired assembling transport and proteolysis of intracellular vWF multimers caused by the mutations S1506L and V1665E in the A2 domain of the
Hassenpflug et al investigated the impact of mutations in the A2 domain of vWF commonly found in patients with vWD type 2A on ADAMTS13-dependent proteolysis of vWF. 29 They used recombinant human ADAMTS13 (rhuADAMTS13) to digest recombinant full-length recombinant vWF (rhuvWF) and a vWF fragment spanning the vWF A1 through A3 domains, harboring 12 different vWD type 2A mutations (G1505E, G1505R, S1506L, M1528V, R1569del, R1597W, V1607D, G1609R, I1628T, G1629E, G1631D, and E1638K). 29 With the exception of G1505E and I1628T, all mutations in the vWF A2 domain showed increased specific proteolysis of vWF independent of the expression level. RhuvWF harboring the mutations G1505E, M1528V, G1609R, I1628T, G1629E, G1631D, and E1638K were similar in expression level with normal multimer distribution consistent with group 2 vWD 2A. Due to the lack of proteolytic activity and shear stress in the culture medium both rhuvWFwild-type (WT) and rhuvWF mutants group 2 are fully multimerized in these experimental in vitro studies. 29 The rhuvWF mutants were hypersensitive to ADAMTS13-dependent proteolysis in vitro. The vWD 2M mutation C1272S resulted in resistance of the recombinant vWF fragment to ADAMTS13-dependent proteolysis. The rhuvWF mutants G1505R, S1506L, R1568del, and V1607D resulted in decreased in vitro expression of high- and intermediate-molecular-weight multimers of vWF, 16 consistent with a group 1 mechanism. 25 –29 Proteolytic hypersusceptibility to ADAMTS13-mediated proteolysis of mutant vWF group 2 in vitro closely correlated with the in vivo phenotype in patients with vWD 2A. Increased vWF susceptibility for ADAMTS13 is a constitutive property of classical vWD type 2A, thus explaining the pronounced proteolytic fragments and loss of HMWM seen in multimer analysis in patients with vWD. 25 –28
Federici et al nicely showed that patients with severe vWD type 2A group 1 due to the mutations S1506L and V1665E showed poor responses of functional vWF parameters to DDAVP and no reappearance of the large multimers (Figure 6), with persistence of a strongly prolonged BT, whereas patients with mild to moderate vWD 2A group 2 due to the mutations R1597W and G1629R responded better to DDAVP with transient increase in large multimers (Figure 6) associated with transient correction of BT and vWF:RCo to low normal values for 1 hour (Figure 6). 15 Severe vWD type 2A group 1 shows a typical proteolytic pattern with pronounced triplet before and after DDAVP and in platelet, which strongly suggest that proteolysis of large multimers occurs already intracellular. 15 von Willebrand disease type 2A group 2 shows transient correction of vWF multimers after DDAVP and normal vWF multimers in platelet, indicating that mutant vWF after secretion by endothelial cells in group 2 vWD type 2A is rapidly proteolysed in plasma due to increased sensitivity to ADAMTS13. 15,25
von Willebrand Disease 2M Due to Loss of Function in the A1 Domain of vWF
Autosomal dominant vWD 2M has been misclassified in the literature as vWD 2A, 1B, severe type 1, and 2 Unclassified (2U).
14
Dominant vWD type 2M and 2U are variable expressions of 1 distinct disease entity caused by loss-of-function mutations in the A1 domain of the
The A1 domain (aa 1260-1479) is structurally delineated by a disulfide bridge between Cys1272 and Cys1458. X-ray diffraction studies of the A1 crystal structure revealed a globular shape comprising a central core consisting of 6 hydrophobic α-strands surrounded by 6 amphipathic α-helices. 30,31 The analysis of naturally occurring loss-of-function mutations (vWD 2M), together with mutagenesis and glycoprotein Ib (GPIb) α peptide docking studies, has identified a central front groove on the A1 domain next to strand α3, as part of the binding site for GPIbα. von Willebrand disease type 2M mutations is characterized by loss of function for vWF, while maintaining a normal multimerization pattern, primarily clustering around the vWF interaction site with its platelet receptor GPIbα. Two main clusters vWD 2M with loss-of-function mutations in the A1 domain are located in amino acid (aa) region 1272 to 1302 and in aa1359 to 1437. Three vWD 2M loss-of-function mutations in aa 1315, aa1324, and aa1462 to 1467 can be identified as isolated from 2B vWD gain-of-function mutations. Several mutations in exon 28 of the A1 domain in patients with vWD type 2M have been described, including L1382P, D1277-E78delinsnsl, R1342C, G1415D, I1416N. 13,32 The mutations S1285P L1307 in the EU study very likely belong to the 2M vWD category. 18,33 von Willebrand disease cases of compound heterozygous for R924Q-R1315C, P2145S-R1315C, P1266L-R1315C, and L1481fs-Y1584C in the European vWD type 1 study 33 show predominant features of vWD type 2M. The ISTH registry of vWD has included the R1374C, R1374H, R1374S, R1374L, R1379C, K1405del, and P1462A mutations as unclassified (U) vWD group. L1382 was labeled as 2U or 2A, and F1369I and R1315C as 2M or 2U. 31 The mutations L1282R, S1285F, L1296P, D1302G, G1324S, G1324A, R1392-Q1402del, E1352K, K1362T, P1475S, and P2781S were labeled as vWD 2M. 31
von Willebrand Disease 2B Due to Gain-of-Function Mutation in the A1 Domain of vWF
von Willebrand disease type 2B cannot be distinguished from 2A by multimer analysis alone since their multimeric patterns are very similar (Figure 1A). 8 –10 The combined use of FVIII:C, vWF:Ag, vWF:RCo and vWF:CB, RIPA, and vWF multimeric analysis in low- and medium-resolution gels is of critical importance to differentiate pronounced vWD 1SD from 2E and 2M and to distinguish vWD 2A from vWD 2B (Table 6). The vWF:Ag detects all multimeric forms of vWF equally with no differential sensitivities to species with different molecular weights including large, intermediate, and small multimers. 34 The vWF:RCo assay detects all large and some of the intermediate vWF multimers in all variants of type 2 vWD and in vWF concentrates. 34 The vWF:CB assay better detects the hemostatically potent large vWF multimers than the vWF:RCo assay. 16,34 Adcock et al retrospectively studied 497 cases in whom results for vWF multimeric analysis in low-resolution gels vWF:Ag, vWF:RCo, and vWF:CB were available. 35 The distribution of vWF:RCo/Ag ratios for types 2A and 2B showed that those classified as type 2A the mean vWF:RCo/Ag ratio was 0.48 + 0.040 and for those samples classified as type 2B, the mean vWF:RCo/Ag ratio was 0.35 + 0.023. 35 von Willebrand disease type 2A and type 2B with loss-of-large vWF multimers show that for those classified as type 2A, the mean vWF:CB/Ag ratio was 0.21 + 0.019 and for those classified as type 2B, the ratio vWF:CB/Ag was 0.36 + 0.025. 35 The vWF:CB/Ag ratios were more pronouncedly lower in type 2A as compared to type 2B vWD. The vWF:RCo/Ag ratio was more pronouncedly lower in type 2B as compared to type 2A vWD. The sensitivity and specificity of the vWF:RCo and vWF:CB assays for the diagnosis of vWD types 2A and 2B are 100% in addition to the loss-of-large vWF multimers in a low- and medium-resolution gel (Figure 5). 35
Laboratory Features and Response to DDAVP of Von Willebrand Factor (vWF:Ag, RCo, CB) Parameters in 6 Probands (P) and Additional 3 Affected Family Members, Who Presented With Pronounced Autosomal Dominant Von Willebrand Disease (vWD) Type 1 Secretion Defect (SD), 2M, and vWD type 1 clearance defect (type 1 CD = Vicenza). With Normal vWF Multimers in Low- and Medium-Resolution Gels. 2,a
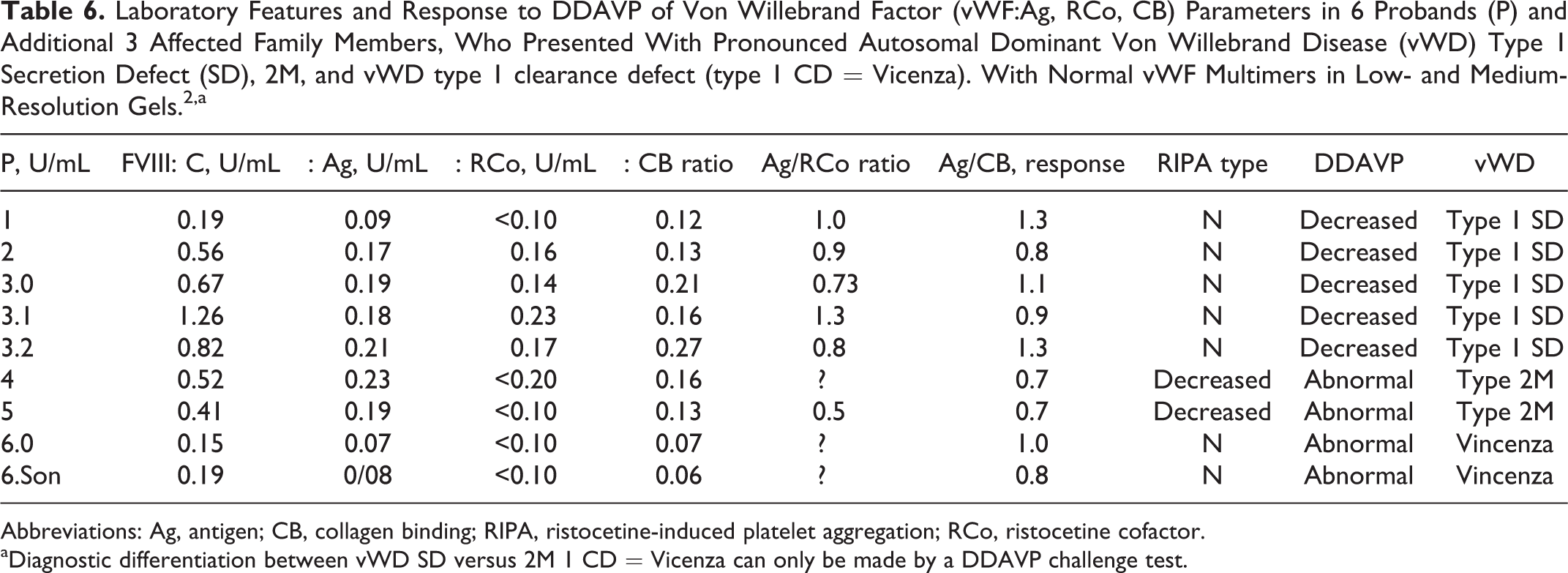
Abbreviations: Ag, antigen; CB, collagen binding; RIPA, ristocetine-induced platelet aggregation; RCo, ristocetine cofactor.
aDiagnostic differentiation between vWD SD versus 2M 1 CD = Vicenza can only be made by a DDAVP challenge test.
von Willebrand disease type 2B is caused by a gain-of-function mutation of the GPIb receptor in the A1 domain of vWF. 8 –11 The crystal structure of a gain-of-function A1 domain mutant R1306Q in complex with the amino-terminal domain of GPIbα (also containing a gain-of-function mutation) confirmed that the frontal part of A1 constitutes the contact area for GPIbα. 30,33,36 Two distinct areas of tight interaction were revealed, the first and most extensive contact site being located near the top of A1, the second involving residues near the bottom face of A1. 36 A main cluster of vWD 2B gain-of-function mutations (increased binding of vWF-A1 and platelet-GPIbα) is located between aa1304 and aa1341 with 2 exceptions aa1315 and aa1324. Two minor clusters of vWD 2B mutations are located at aa1268-1272 and aa1460-1462. 36
The key criterion for the diagnosis of vWD 2B is the loss-of-large vWF multimers (Figure 1A: Table 1) due to increased proteolysis caused by increased interaction of platelets mutated vWF with a gain of function in the A1 domain as reflected by increased RIPA. 2,6,25,36 von Willebrand disease 2B is caused by hyperreactive mutant vWF with increased affinity for the platelet receptor glycoprotein Ib-α in vivo followed by increased proteolysis of large vWF multimers. 34,35 In that process of increased vWF-GpIb-platelet interaction of mutant vWF in vWD 2B clump as soon as the mutant vWF enters the circulation. Clumps of mutant vWF platelets are cleared from the circulation and thereby upon DDAVP or stress complicated by moderate to severe thrombocythopenia. 36 In a cohort of 67 vWD 2B patients from 38 unrelated families, Federici et al evaluated the clinical and molecular predictors of thrombocytopenia and the risk of bleeding. Thrombocytopenia was found in 30% at baseline and in 57% after stress conditions in only those with vWD 2B who did meet the ISTH criteria. 36 Platelet counts were always normal in 16 (24%) patients from 5 families carrying the P1266L or R1308L mutation, who usually have a type 1 variant of mild vWD 2B with normal vWF:RCo/Ag ratios of 0.9 and 0.8, respectively (vWD type 1B). 36 In fact, à patients with classical vWD type 2B usually present with moderate to severe clinical phenotype. Patients with vWD 2B having the mutations (P1266L, Malmo, or New York vWD 1B phenotype) do have a mild bleeding illness with normal ratios of vWF:RCo/vWF:Ag consistent with a laboratory vWD type 1B phenotype with increased RIPA.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
