Abstract
Background:
Transfusion of blood products occurs frequently in ruptured abdominal aortic aneurysm surgery (rAAA). The aim of this study is to establish the impact of packed red blood cell (PRBC), fresh frozen plasma (FFP), and platelet (PLT) transfusion on the 30-day mortality and morbidity (thrombotic versus non thrombotic complications) of rAAAs.
Methods:
A retrospective study of 90 consecutive rAAAs from November 2007 to June 2015 was conducted. Multivariable regression models were produced to determine blood products associated with 30-day morbidity and mortality post-rAAA.
Results:
The overall mortality was 14.6%. At multivariable analyses, transfusion with FFP (>3 units) was independently associated with an increased risk of mortality (odds ratio [OR]: 11.27, 95% confidence interval [CI]: 1.13-96.72,
Conclusion:
Transfusion of FFP and PLTs may be associated with an increased risk of postoperative morbidity and mortality. The use of these blood components should be considered in the context of the patient’s clinical and laboratory data as opposed to a fixed ratio to PRBCs. This may result in the reduction in thrombotic complications emerging in rAAA cohort.
Keywords
Introduction
Previous reports in the literature have suggested that mortality following the repair of ruptured abdominal aortic aneurysm (rAAA) has been predominantly due to hemorrhage secondary to coagulopathy. However, the current literature suggests that fatal hemorrhage secondary to coagulopathy is now rare, and there has been a significant shift toward postprocedure mortality and morbidity as a consequence of thrombotic complications. 1,2 This has been attributed to the new transfusion and resuscitation techniques, where crystalloids and colloids have been replaced by blood and blood component transfusion. 3
The new transfusion (blood and blood component) protocols have evolved as a result of research surrounding patients with military and civilian trauma having catastrophic hemorrhage, where a transfusion ratio of 2:1:1 and/or 1:1:1 of packed red blood cell (PRBC) to fresh frozen plasma (FFP) to platelets (PLTs) conferred a mortality benefit. 3 These protocols have since been used in the resuscitation of all patients presenting with hemorrhagic shock including those with rAAAs. Evidence suggests that the transfusion of PRBCs in rAAAs resuscitation has significantly reduced mortality, however, 4 the impact of the transfusion of FFP and PLT with the aforementioned ratio has yet to be determined. The aim of this study is to determine the effect of transfusion of blood and blood components such as FFP and PLTs on the 30-day morbidity and mortality of patients presenting with rAAAs.
Method
A retrospective consecutive study of all patients presenting with ruptured infrarenal abdominal aortic aneurysm (AAA) at Mid Essex Hospitals NHS Trust from November 2007 to June 2015 was carried out. The hospital, surgical, and anesthetic database for all ruptured cases was searched, and a total of 90 (n = 90) patients were identified. However, only 82 (n = 82) patients had a complete record. None of the patients were on any local screening program, and all patients had an open repair of the infrarenal ruptured abdominal aortic aneurysm. All individuals had a similar method of repair. A straight knitted Dacron graft according to the aorta size (size 16-20 mm) was anastomosed proximally and distally with Polyprolene Monofilament suture size 3 and 4, respectively (Surgipro, Covidien). Furthermore, none of the patients had any known coagulopathy and/or hematological disorder. Eighty individuals (n = 80) were on aspirin 75 mg preoperatively, and none were on any other antiplatelet and/or anticoagulant medication. The transfusion policy was based on clinical expertise of the anesthetic department, and (not on any protocol) this was applicable to all individuals.
The patient demographics on age, gender, comorbidities, American society of Anaesthesiology score (ASA), blood loss, and blood component transfusions of units of PRBC, FFP, and pools of platelet (PLT) were retrieved. None of the individuals received any other additional clotting factors or were subjected to autotransfusion. All patients received 5000 IU of heparin intravenously after the application of the aortic clamp. Postoperatively, all patients received aspirin 75 mg along with enoxaparin sodium 40 mg, subcutaneously once daily. Individual preoperative computed tomography angiogram of the entire cohort was assessed by 2 separate investigators (interventional vascular radiologist and consultant vascular surgeon), and the aneurysm size was calculated and presented in millimeters. The maximum diameter was taken as the true size of the AAA. The agreement level in size measurement was assessed using Cohen’s κ coefficient (κ = .82). The study end point was set at 30 days for all outcomes of mortality, morbidity (thrombotic and nonthrombotic complications). Morbidity was defined according Clavien-Dindo classification ≥3 (considered a major complication). 5 Mortality was defined as death from any cause. Due to lack of any new or alternative intervention and availability of the data for clinical purpose, ethical approval was granted with audit number CA13-226.
Statistical Analysis
For the purposes of the statistical analyses, scale variables were categorized according to their median values. Differences across the outcome groups were examined using Kruskal-Wallis and chi-square analyses. Logistic regression analyses were undertaken to determine factors associated with each outcome (30-day mortality, 30-day morbidity. and 30-day thrombotic complications). Each variable was tested individually for association with the outcome. Those variables that demonstrated a significance of
Results
A total of 82 patients had complete data for analyses. The median age at the time of rAAA was 75 years (range: 51-92). The majority of the population was male (n = 66, 80.5%). The median size of rAAA was 75.52 mm (range: 40-100 mm). The ASA in the order of prevalence was ASA = 4 (n = 36, 36.6%), ASA = 3 (n = 27, 32.9%), ASA = 2 (n = 17, 20.7%), and ASA = 5 (n = 8, 9.8%). Hypertension was found in 60.9% (n = 50), chronic obstructive pulmonary disease in 28.0% (n = 23 of 82), and active smokers in 23.2% (n = 19 of 82) of the cohort. The median intraoperative blood loss was 2100 mL (range: 500-5000). The median length of intensive care unit stay was 72 hours (range: 13-574), and the overall median length of hospital stay was 10 days (range: 5-29; Table 1).
Demographic Details of the Cohort.
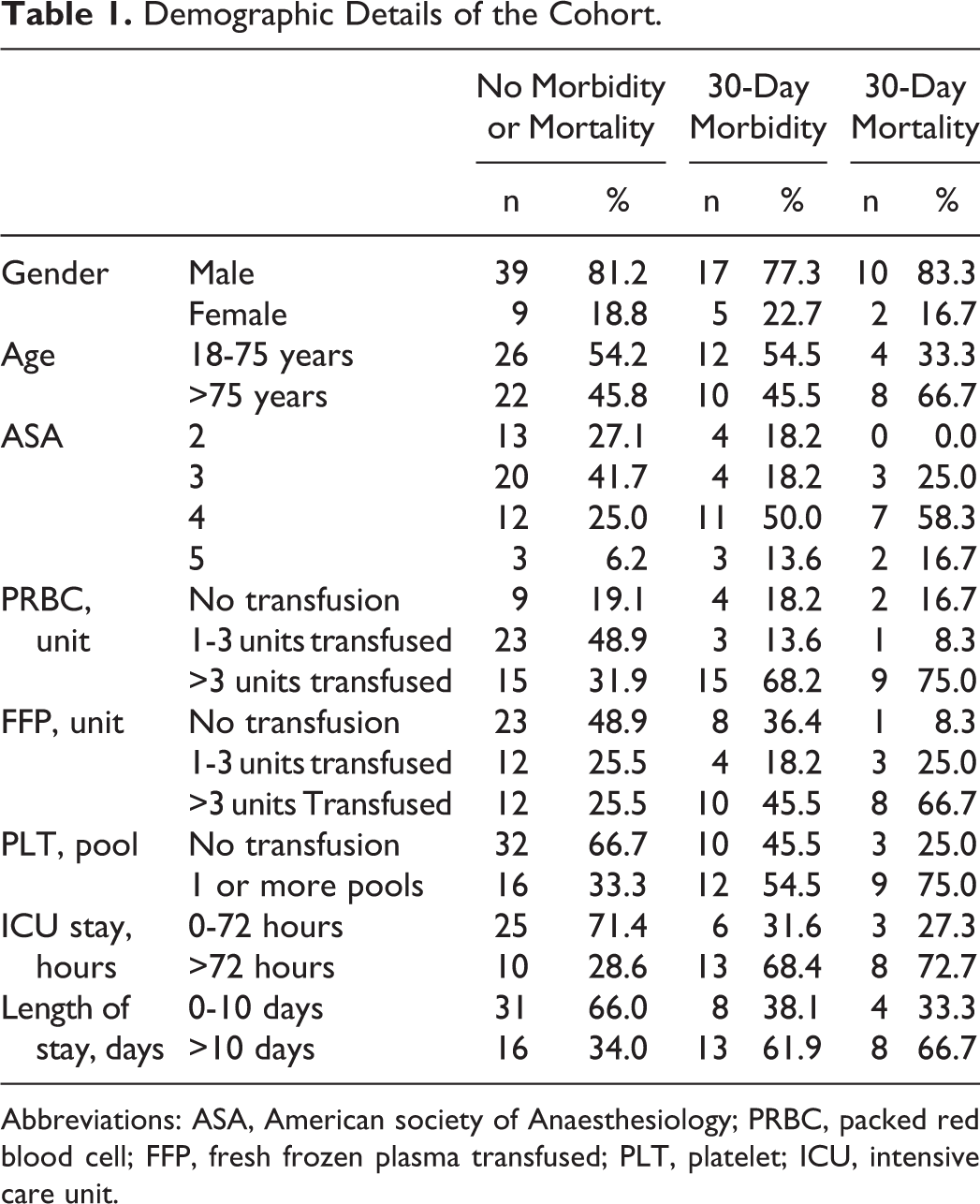
Abbreviations: ASA, American society of Anaesthesiology; PRBC, packed red blood cell; FFP, fresh frozen plasma transfused; PLT, platelet; ICU, intensive care unit.
Mortality
Overall, 14.6% (n = 12) died within the first 30 days of surgery. Of these, the vast majority (n = 10 of 12) were males. Univariable analyses demonstrated increasing ASA score (
Regression Analysis (Univariate and Multivariate) on Factors Associated With 30-Day Mortality.
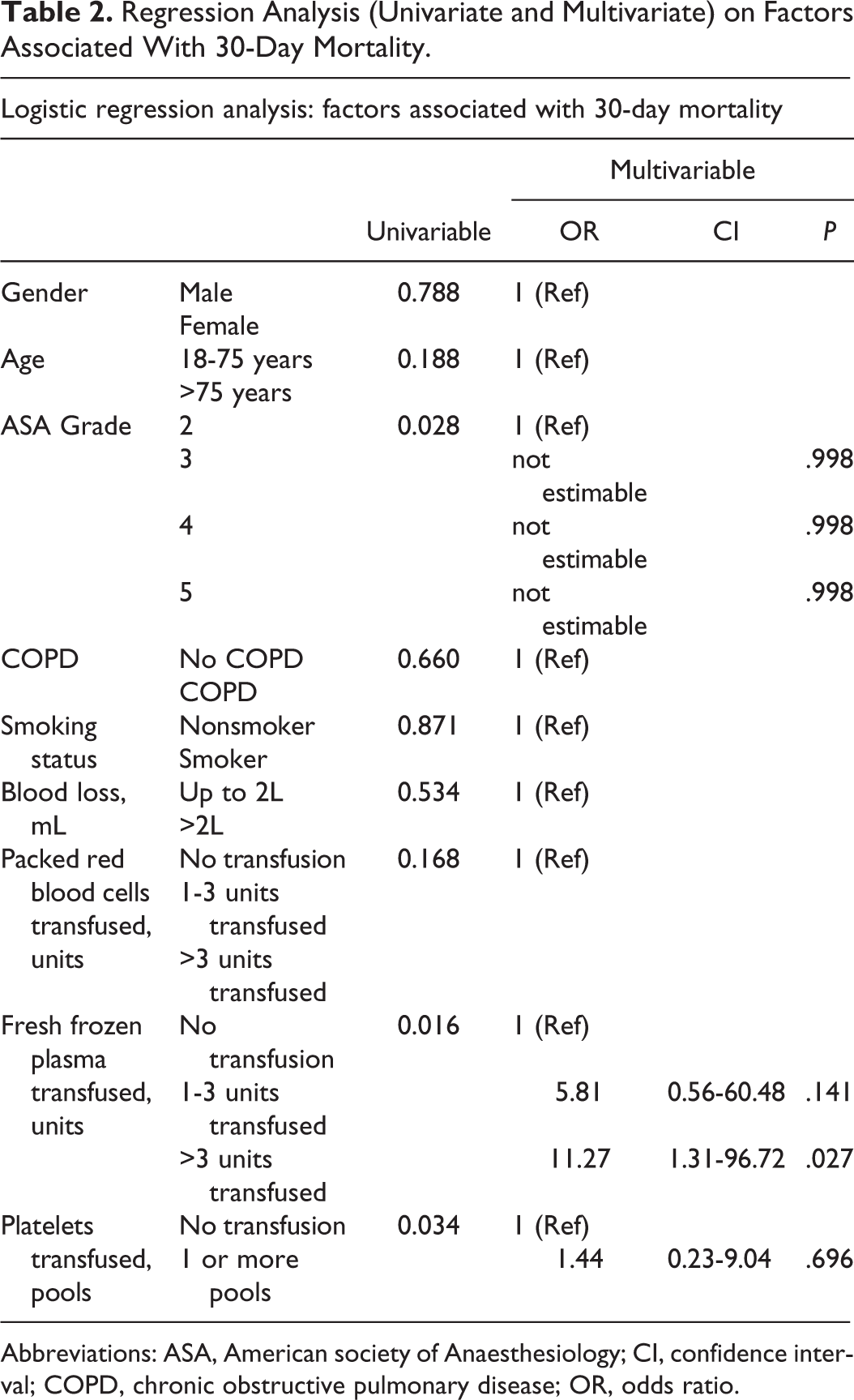
Abbreviations: ASA, American society of Anaesthesiology; CI, confidence interval; COPD, chronic obstructive pulmonary disease; OR, odds ratio.
Morbidity
A total of 22 patients (26.8% of the entire population) experienced morbidity within 30 days post-rAAA surgery. Logistic regression analyses were undertaken to ascertain determinants of morbidity. Univariable analyses demonstrated transfusions of PRBC >3 units (
Regression Analysis (Univariate and Multivariate) of Factors on 30-Day Morbidity.
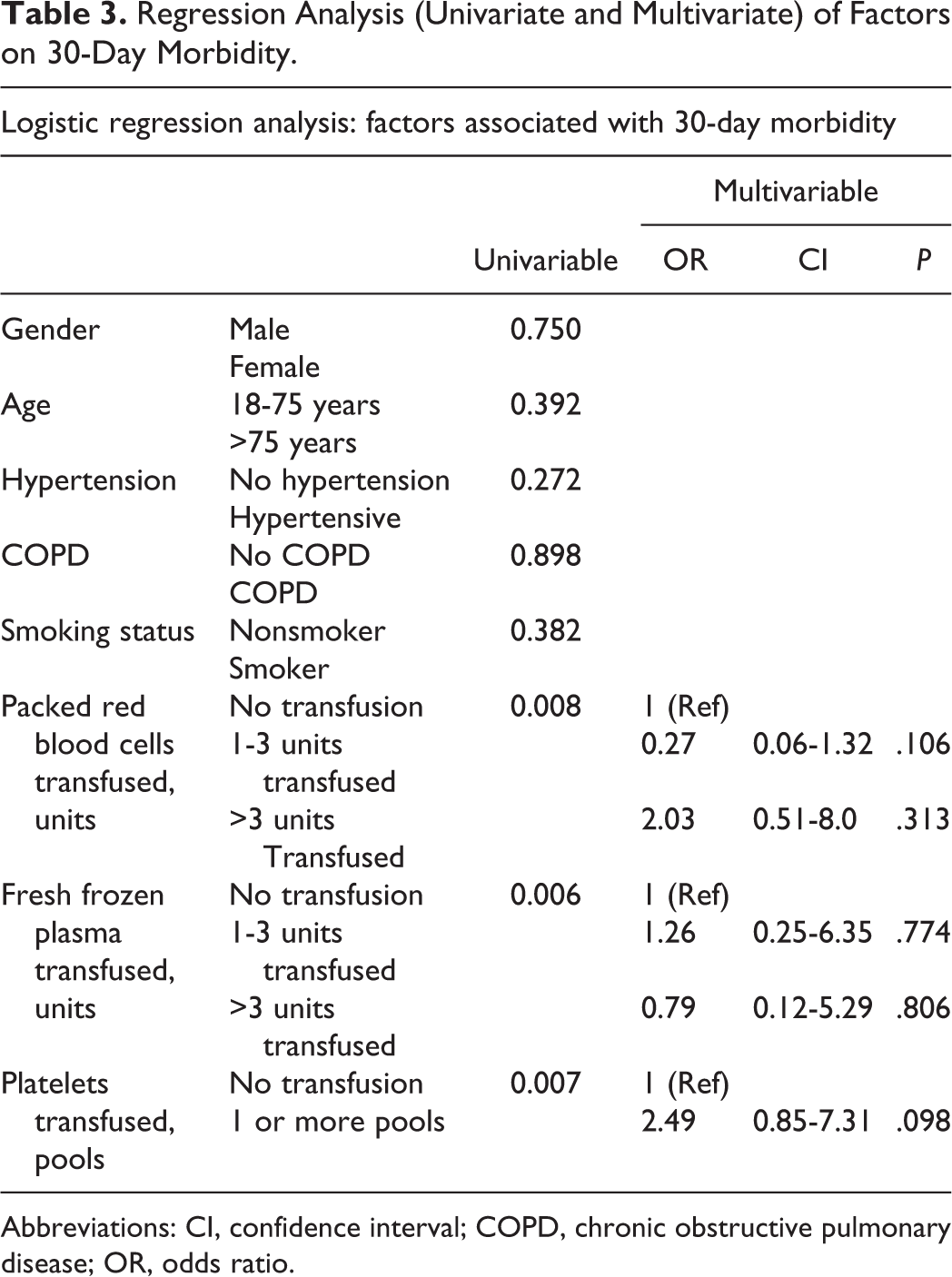
Abbreviations: CI, confidence interval; COPD, chronic obstructive pulmonary disease; OR, odds ratio.
Regression Analysis (Univariate and Multivariate) of Factors Associated With Thrombotic Complications.
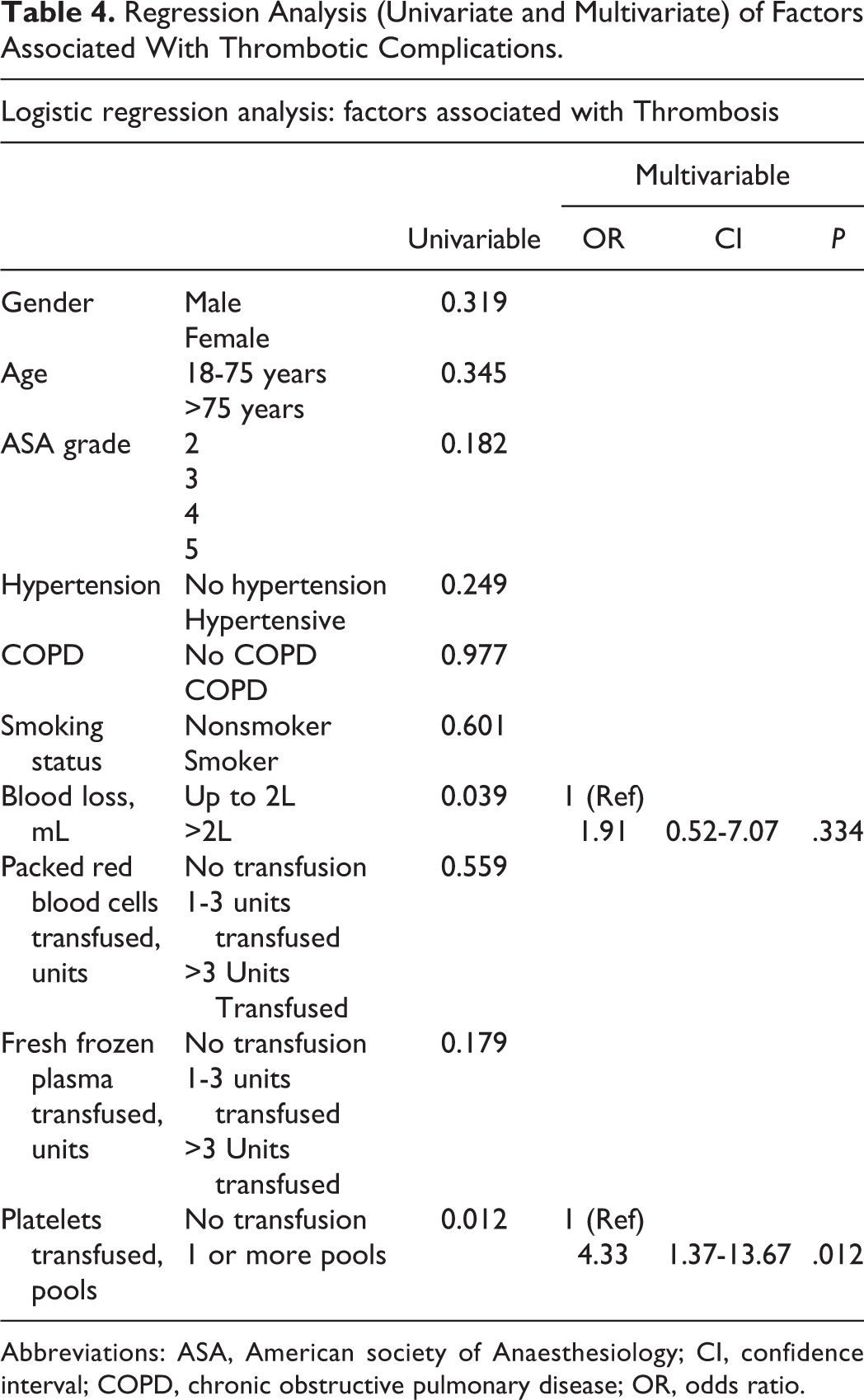
Abbreviations: ASA, American society of Anaesthesiology; CI, confidence interval; COPD, chronic obstructive pulmonary disease; OR, odds ratio.
Information on the Deceased Patients.a
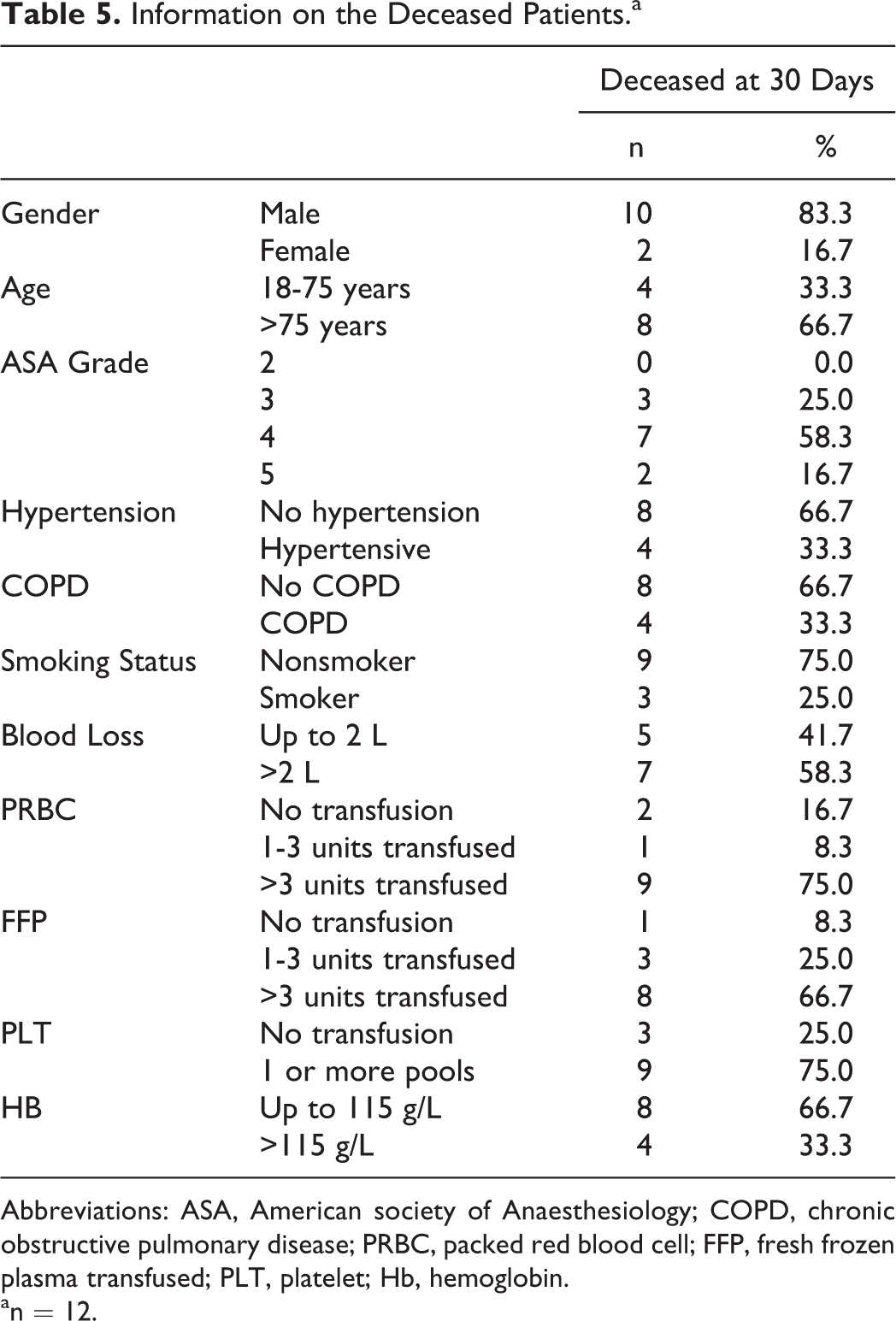
Abbreviations: ASA, American society of Anaesthesiology; COPD, chronic obstructive pulmonary disease; PRBC, packed red blood cell; FFP, fresh frozen plasma transfused; PLT, platelet; Hb, hemoglobin.
an = 12.
Laboratory Results of Deceased Patients Prior to Transfusion.
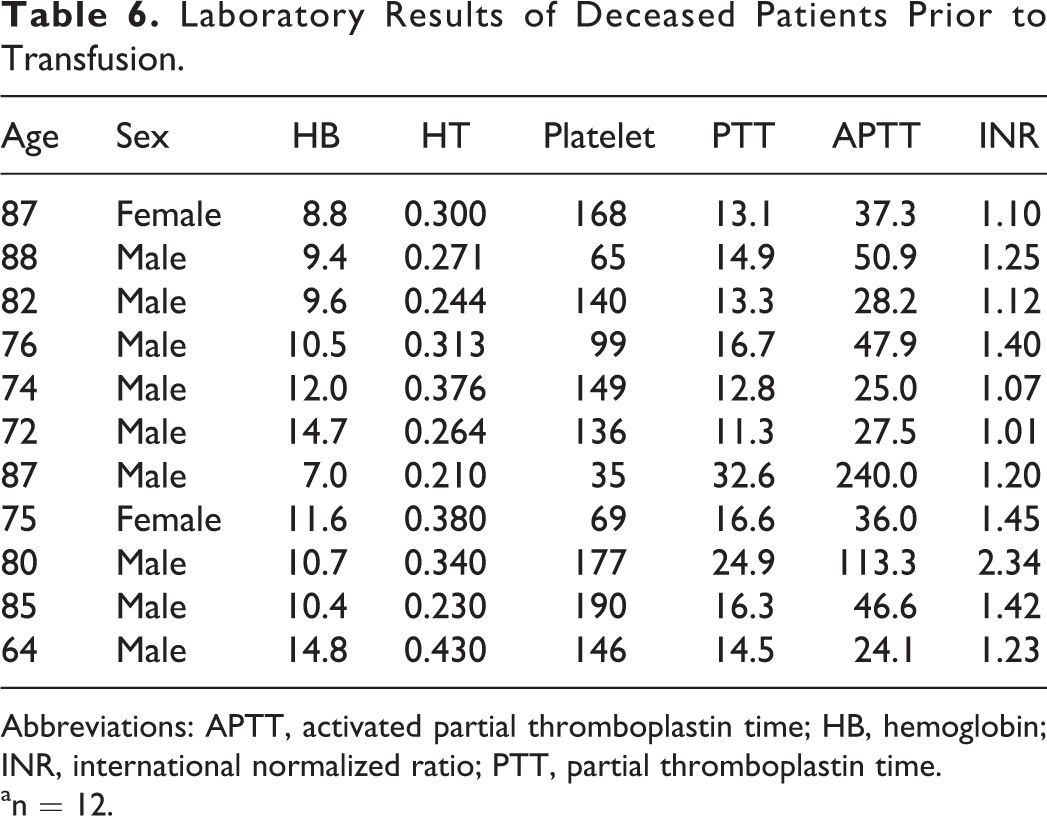
Abbreviations: APTT, activated partial thromboplastin time; HB, hemoglobin; INR, international normalized ratio; PTT, partial thromboplastin time.
an = 12.
Discussion
The outcome of this study suggests FFP transfusion coincides with increased risk of 30-day comorbidity, namely, thromboembolic events. The traditional crystalloid/colloid infusion has now been replaced with PRBC, FFP, and PLT which is based on massive transfusion protocols. 6,7 The initial strategy was aimed at the optimization of cardiac output and oxygen delivery system, and later, at the correction of coagulopathy, believed to develop several hours after the onset of hemorrhagic shock. 8,9 However, recent research suggests that traumatic coagulopathy in hemorrhagic shock is from the activation of anticoagulant protein C pathway due to tissue hypoperfusion and not from the consumption of coagulation factors. Thus, the resuscitation protocols should now aim at limiting hypoperfusion and its duration, which can be assessed by the degree of acidosis. 10,11 This means the new transfusion strategy aims at correcting the trauma triad of hypothermia, acidosis, and coagulopathy. 12
The current transfusion strategy has reduced mortality from catastrophic hemorrhage in patients with rAAA. However with increased survival, there has been an emergence of a new pattern of mortality and morbidity, which is related to thrombotic events. There is a degree of evidence to support the use of PRBCs in this cohort of patients. However, the difference between a patient with traumatic injury and patient with rAAA needs to be considered before the administration of other blood components such as FFP and PLT. 13 In contrast to the population with trauma, the average age in vascular patient is much higher (75 vs 45 years), and they exhibit far more comorbidities and they do not commonly present with hyoptheramia. 14 Aneurysm formation is a time-dependent process, and its morphology alters the coagulation cascade in comparison to the sudden impact of trauma on overall physiology and its immediate effect on the coagulation cascade.
Furthermore, during aneurysm degeneration, the assault to the endothelium acts as a nidus for the adhesion of PLTs, migration of PLTs, and generation of fibrin. The release of von Willebrandt Factor (vWF) and the presence of various other hematological factors promote the activation of tissue factor (TF) that in turn generates thrombin formation through factors X and VII. In addition, the size of mural thrombus exhibits a direct (positive) correlation with the aneurysm size and its anatomical tortuosity that are much higher in rAAA. 15 –17 This indicates rAAAs present with a procoagulant rather than coagulopathic state and therefore do not require the current suggested ratio of FFP and PLT as a rule.
The initial resuscitation strategy most commonly adopted in patients with rAAA across vascular units is “permissive hypotension.” 18 Such hypotension may well result in hypoperfusion and early coagulopathy, although unlike patients with trauma, evidence in the rAAA cohort demonstrates no significant relationship between hypotension and/or hypoperfusion, the degree of coagulopathy, and fibrinolytic parameters. In addition, an earlier suggestion about elevation of fibrinolytic factors in rAAAs could be related to the application of supraceliac cross clamp that in turn reduces the hepatic blood flow and results in elevation of fibrinolytic factors. 19 –21
In the study by Adam et al,21 even nonruptured AAAs exhibited significant coagulation status difference to that of rAAAs. The markers of thrombin generation thrombin–antithrombin complex and prothrombin fragment 1 + 2 concentration were statistically higher in rAAAs in comparison to the nonruptured cases (135.5 μg/L vs 61 μg/L,
Our data suggest that FFP transfusion of more than 3 units is an independent predictor of 30-day mortality in rAAAs. Other authors have reported similar results. In a study comparing the number and types of transfusions of survivor and nonsurvivor groups in rAAA, the authors demonstrated the unit of FFP transfused in the survivor group to be significantly lower than the nonsurvivor group. The postoperative complications leading to mortality in the study by Fransson and colleagues was related to micro- and macro-cardiovascular thrombotic complications.
22
In the same direction, the study by Kauver et al could not establish a reduction in mortality with increased FFP transfusion in patients with rAAA (
Another important issue surrounding the repair of rAAA is the use of unfractionated heparin. It appears that other than tissue plasminogen activator (t-PA), no other fibrinolytic component is affected by heparin. Considering the status of rAAA and the potential loss of significant volume, surgeons are reluctant to use heparin in such settings. The judicial use of heparin after the application of the aortic clamp may reverse and/or decrease the procoagulant state and the associated mortality induced by higher FFP transfusion. In our cohort, all individuals received Heparin, and this may justify the lower mortality incidences compared to the other reported series. Graham et al review also recommends the use of heparin in the repair of rAAA for the reversal of the ongoing procoagulant state and postprocedural thrombotic events. 25,26
Platelet transfusion of more than 1 pool was an independent marker of thrombotic complications in our cohort of patients. In a recent analysis of preoperative bloods (PLT count, prothrombin time, activated partial thromboplastin time) performed on individuals with rAAAs, no coagulopathic state was identified. In addition, no thrombocytopenia and/or platelet count of less than 100 (10/L) was noted in the majority of the individuals. 27 This outcome clearly indicates that patient with rAAA do not necessarily require active platelet transfusion and if so it has to be based on ongoing laboratory result rather than one for all transfusion protocol. In addition, active transfusion of platelet in a patient with adequate platelet count for a major surgery could explain the ongoing trend and shift toward the occurring thrombotic complications in our cohort.
The current study has several strengths and weaknesses. This is the first study in the literature that has evaluated the role of PRBC, FFP, and PLT (massive transfusion protocol and its ratio) in the resuscitation of rAAAs. Our data appear to be in agreement with earlier studies indicating that patients with rAAAs unlike patients with trauma are procoagulant, and liberal use of FFP and PLT can contribute to mortality, morbidity, and thrombotic complications. In addition, this study highlights that the mortality incidence of rAAA has improved, and these patients are no longer succumbing to hemorrhagic shock but instead are dying as a result of thrombotic complications later in the recovery phase. This study inherits the weakness of being retrospective in nature, and a higher number of individuals in a randomized controlled trial would have been optimal. However, given the nature of the surgery, its associated high morbidity, and mortality, such methodology might not be feasible and current practice may have to rely on observational studies.
Conclusion
The findings of this study are that certain blood components such as FFP and PLTs may be associated with increased postoperative morbidity post-rAAA repair. The traditional transfusion protocol and its suggested ratios of blood products to PRBC need to be questioned. Despite reduction in mortality associated with transfusion of PRBC, the use of other blood components such as FFP and PLT should be considered in the context of the patient’s requirement based on clinical and laboratory data. The liberal use of FFP and PLT in patients with rAAA might have a different outcome compared to that of patients with trauma. Thus, further research assessing such factors is required to determine what the ideal transfusion protocol would be.
Footnotes
Acknowledgments
The authors would like to thank the Health Education East of England (HEEoE).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
