Abstract
Aim:
The aim of this open, observational registry was to evaluate the effects of antithrombotic treatment on the development of postthrombotic syndrome (PTS): the effects of “standard management” (SM; according to International Union of Angiology guidelines) were compared to SM in association with sulodexide or aspirin.
Methods:
Postthrombotic syndrome occurrence was observed in 3 nonparallel groups after deep venous thrombosis (DVT); the registry started after the end of the anticoagulation period. The target was to observe the occurrence of PTS in 5 years. Three possible options were suggested to the patients, and the patients and their caregivers defined the type of management. A group of 167 patients was involved in the SM with reevaluation every 6 months; the sulodexide group included 124 patients and the aspirin group included 48 patients.
Results:
The 3 groups were clinically similar and comparable for age and sex distribution. Of the 167 patients in the SM group, 154 patients completed 60 months of follow-up. The percentage of patients with PTS in the SM group ranged from 14.9% (1 year after the end of anticoagulation) to 19.5% (60 months). In the nonparallel group using sulodexide (124 comparable patients at inclusion; 115 at 60 months), the percentage of PTS was variable from 8.8% (1 year after anticoagulants) to 12.17% at 60 months. These percentages are significantly lower than those observed with SM. In the nonparallel aspirin group (48 patients at inclusion and 34 at 54 months), there was a PTS incidence of 23.5% at 54 months (vs 12.17% in the sulodexide group and 18.23% in the SM group). The incidence of PTS was significantly higher in comparison with the other 2 groups. The incidence of PTS was lower in the sulodexide group in comparison with the 2 other groups.
Conclusions:
Sulodexide administration after DVT appears to be effective in preventing PTS in association with recommended management and a number of recurrent DVTs. Modalities of treatment, dosages, and timing of administration should be explored in more comprehensive and complete studies.
Background
Even after effective conventional anticoagulation management (low-molecular-weight heparins (LMWHs) for 5 days followed by warfarin or another oral anticoagulant), between 30% and 50% of patients with proximal deep venous thrombosis (DVT) may develop a postthrombotic syndrome (PTS). Postthrombotic syndrome leads in time to a variable range of clinical signs/symptoms with different degrees of severity, eventually producing venous ulcerations 1,2 in some 30% of patients. 3
According to the recent International Union of Angiology (IUA) Consensus on Thromboembolism, 3 PTS produces limb swelling, pain, heaviness, itching, microcirculatory alterations, and eventually permanent skin changes with ulcerations. 2 –4 Venous ulcers may occur as early as 3 months 2 but usually affect the patients after a few years for several years recurring and requiring complex and tiring management. Postthrombotic syndrome is a significant cause of chronic incapacity, affecting working potential and producing medical, social, and personal costs. 3,5–7
Postthrombotic syndrome is considered the final consequence of chronic venous hypertension (CVH) produced by a combination of reflux in veins with damaged valves and/or by outflow obstruction. 8 Chronic venous hypertension is associated with some degree of inflammation affecting the venous wall and by microcirculation alterations producing excessive capillary leakage—clinically visible as edema—with impairment of skin nutrition leading to skin changes and eventually to ulceration. 9
Postthrombotic syndrome development is associated with proximal (iliac or femoral DVT), 3,5 chronic obstruction, 10,11 increase in weight, 5,12 and recurrence of DVT episodes 12 that alter and obstruct different parts of the “anatomical” circulation or part of the new channels associated with collateral circulation. Substandard management (anticoagulants and compression) allows more frequent recurrence and chronically increased venous pressure. 13 Elevation in inflammatory biomarkers (interleukin-6, intercellular adhesion molecule 1, and C-reactive protein) 14,15 is associated with increased rates of PTS following DVT. 3,14,15
Prevention of Primary and Secondary DVT
Prevention of DVT and recurrent DVT (R-DVT) should reduce the prevalence of PTS. There is a strong connection between PTS and R-DVT. Patients with PTS have a higher frequency of R-DVT, and patients with episodes of R-DVT tend to have a higher incidence and severity of PTS.
Postthrombotic syndrome has been considered as a late complication, but more recent observations indicate that PTS may occur early (in months in some patients); the evaluation of symptoms at 1 month after the onset of DVT is highly predictive of the presence of PTS. 3,5 Prevention of recurrence in patients with DVT appears to control the severity and frequency of PTS. Guidelines aiming to reduce PTS and leg ulcers by 50% in the next 10 years have been published. 16
In PTS, graduated elastic compression reduces venous hypertension and edema and controls the damage to microcirculation. 17,18 In patients with proximal DVT, elastic compression for 2 years reduces the incidence of PTS from 39% to 19%. 19 –22 Treatment of DVT with LMWH combined with early ambulation and elastic compression further prevents PTS. 23,24 Sulodexide is a highly purified mixture of glycosaminoglycans including LMWHs (80%) and dermatan sulfate (20%; Alfa-Wassermann, Bologna, Italy); it is briefly described as an antithrombotic compound and it has been used in the follow-up of patients after DVT to prevent a R-DVT. 25 Sulodexide is effective in promoting the release of lipoprotein lipase activity. Thus, it is conventionally rated on the basis of its lipasemic activity—as lipoprotein-lipase releasing units—or lipasemic units (ULS); 5 ULS correspond roughly to 1 mg of an heparinoids mixture. Aspirin has also been used to prevent R-DVT after a first episode of DVT treated with anticoagulation. 26 The aim of this observational registry was to evaluate the effects of different types of management on the development of PTS. In particular, the effects of sulodexide and aspirin, when added to standard management (SM), were observed in 3 nonparallel groups of patients after DVT (the open registry started after the end of the anticoagulant treatment).
Methods
Patients with PTS after a documented (ultrasound) proximal (iliac or femoral) thrombosis were included in the follow-up. No previous DVT had been documented. Correct treatment for the clinical situation 3 had been used after the detection of the lower limb thrombosis (according to IUA Consensus on Thromboembolism), 3 namely, LMWH for at least 5 days or until international normalized ratio was around 3, followed by 6 months of oral anticoagulants. Antithrombotic stockings had been used since the discovery of DVT. Only 1 limb had been affected by DVT and the other was normal. Signs/symptoms present at the affected limb at inclusion were:
limb swelling;
distal edema;
difference in size between the 2 limbs; and
secondary varicose veins from collateral circulation.
No other arterial or venous alteration was present.
To define the presence of PTS during follow-up, 6 major, common signs were considered significant:
limb swelling, increase in size;
pain (either at rest, after prolonged standing, or on walking);
heaviness;
itching;
microcirculatory alterations; and
permanent skin changes and discoloration.
At least 5 of 6 signs/symptoms had to be present to define the occurrence of PTS; the symptoms were scored and the possible maximum score was determined. Postthrombotic syndrome was arbitrarily defined in this study by a score >40 indicating a clinically significant PTS. A lower score corresponding to a lower clinical level of PTS was considered as “initial PTS” and not considered as a fully established PTS that was the final focus of this registry.
No ulcerations were present at inclusion in the follow-up after the anticoagulation period. These signs/symptoms were scored on an analog scale line (0-10). No other disease was present; no other treatment was used during the follow-up. The needs for significant chronic treatments (lasting more than 30 days) or a newly developing clinical condition were criteria for exclusion. No thrombophilic condition was present at inclusion or had been diagnosed after 6 months of anticoagulation. Patients did not regularly use any other drug of medical treatment during the study, excluding the occasional use of pain killers, symptomatic flu medications (not more than 3 days), or antibiotics if there was a temporary need.
The target of the observational study was to observe the occurrence of PTS in 5 years in these patients. Three possible options were suggested to the patients: the first was SM only; the second was the use of oral sulodexide in association with SM; and the third was the use of aspirin, if tolerated. Patients and their caregivers decided the type of management. The groups were nonparallel with the sulodexide group starting 6 months after the SM group and the aspirin group starting 12 months after. The aim was to reach at least 4 years of follow-up. Patients were fully informed, gave their approval, and were not randomized.
Reevaluation every 6 months included color duplex (upon need if indicated by unusual signs/symptoms),
“Standard management” is defined (according to IUA Consensus) 3 as a combination of compression, control of all thrombotic risk factors (including reduced mobility, prolonged flights, and dehydration), weight, and regular exercise. At the moment, no specific drug is available to prevent PTS.
Comparable Nonparallel Groups
Sulodexide Group
The sulodexide group at the dosage of 2 capsules (cps) daily (time 8-20)—each including 250 ULS—included 124 patients (mean age was 47.2; 5.3 years with a BMI < 25; range 19-25).
Rationale
Sulodexide has been used in a prolonged follow-up to evaluate the occurrence of R-DVT. 25 This study had indicated that oral sulodexide reduces the incidence of R-DVT in patients with PTS (the incidence of R-DVT at 24 months was 17.9% in controls vs 7.4% in the sulodexide group, 2.42 times lower than in controls). The follow-up (still in progress) also indicated that the incidence of PTS in sulodexide-treated patients (10.3% at 24 months) was reduced in comparison with patients using only SM (17.2%).
Aspirin Group
The aspirin group (100 mg/d, time 8
Rationale
The efficacy of aspirin (100 mg daily for 2 years) in the prevention of R-DVT and PTS is still undefined. 26 The incidence of R-DVT was 6.6% with aspirin (vs an 11.2% incidence in a comparable patients using placebo). Prolonged treatment with aspirin may be a choice in patients who could be candidates for anticoagulation after DVT. It is possible that by reducing the incidence of new thrombotic episodes, the evolution of PTS could be reduced or delayed. According to the IUA Consensus, confirmatory studies are needed. The 42% reduction in R-DVT observed in this study is approximately half of the incidence observed and expected with rivaroxaban and dabigatran. In comparison with placebo, these oral anticoagulants reduce the risk of R-DVT by more than 80%. However, aspirin cannot be used in every patient. This nonparallel study group was evaluated every 12 months with a target of at least 4 years of follow-up.
Results
In the SM group, 167 patients (86 females) were involved in follow-up with mail contacts and free consultations and reevaluation every 6 months. Their mean age was 46.4; 4.9 years with a BMI < 25 (19.4-23.6). Of these 167 patients, 154 (78 females) completed 60 months of follow-up: 3 (1.78%) of these patients were lost (10 had R-DVT at the same limb, requiring new anticoagulant treatment) and the other patients were lost to follow-up for logistical reasons (Table 1). Patients were defined as lost when they failed to show up for controls or could not tolerate treatment. In those who failed to show up, phone contacts indicated that they were alive and could not come for working, logistic, or minor (ie, flu) medical problem.
Summary of Results: Patients, Drop Outs, R-DVT Cases and Incidence of Postthrombotic Syndromes.a
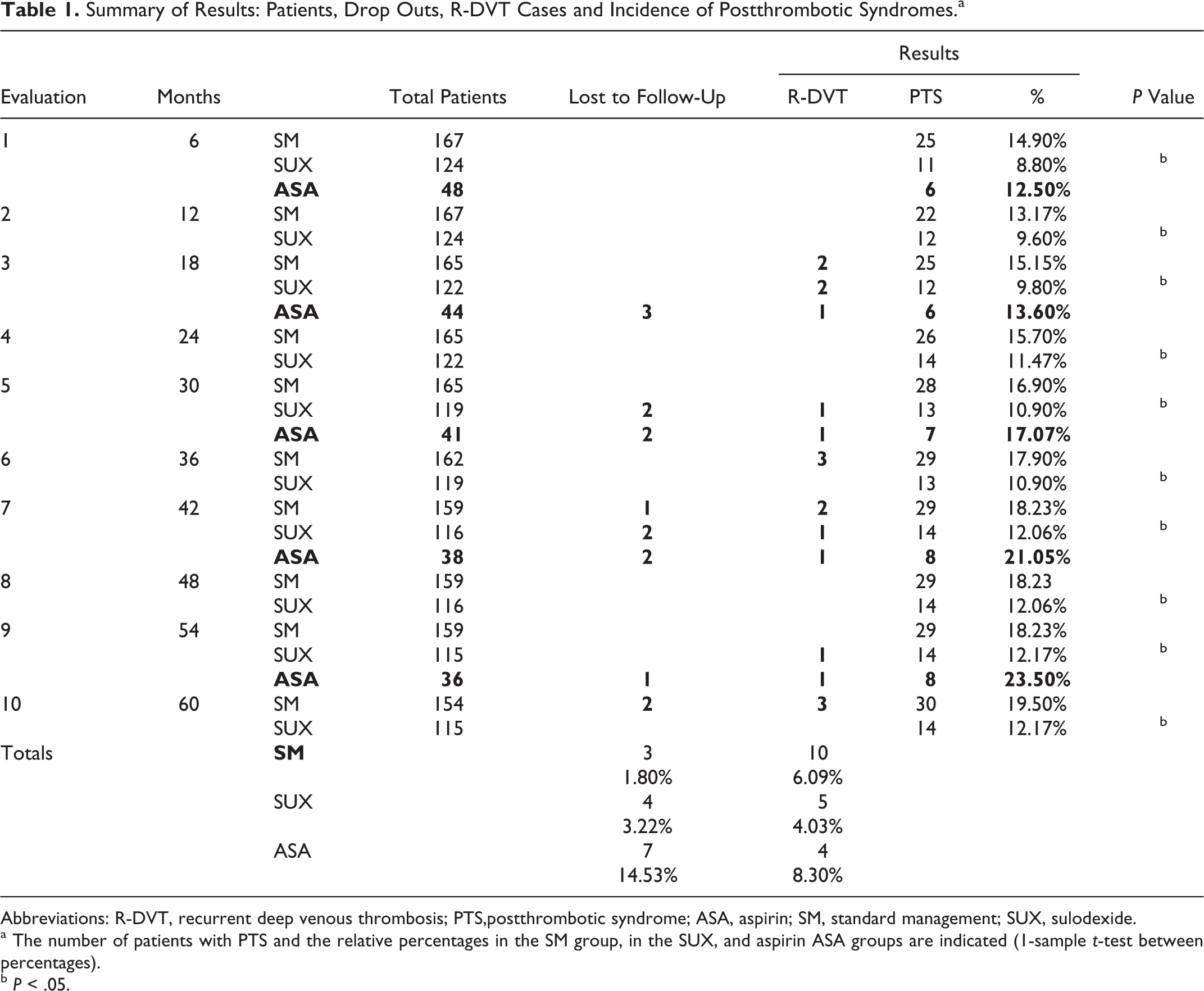
Abbreviations: R-DVT, recurrent deep venous thrombosis; PTS,postthrombotic syndrome; ASA, aspirin; SM, standard management; SUX, sulodexide.
a The number of patients with PTS and the relative percentages in the SM group, in the SUX, and aspirin ASA groups are indicated (1-sample t-test between percentages).
b P < .05.
In the SM group, the percentage of patients with PTS ranged from 14.9% (at 1 year after the end of the anticoagulation period) to 19.5% at 60 months. This observed percentage is an important finding, as we had relatively young, otherwise healthy patients in this registry who were able to cope with instructions and postthrombotic management and to exercise. Older patients with concomitant clinical problems who were less compliant may express a higher incidence of PTS.
We also observed a limited number of patients who had PTS at one of the periodical controls that was attenuated or disappeared at the following controls (3 patients). This probably depends upon management and attention for PTS.
In the comparative, nonparallel group using sulodexide (124 comparable patients at inclusion with 74 females; 115 at 60 months with 71 females), the percentage of PTS was variable from 8.8% at 1 year after the end of anticoagulation to a final 12.17% at 60 months. These percentages are significantly lower than what was observed with SM (P < .05).
In the nonparallel aspirin group (48 patients with 20 females at inclusion and 34 patients at 54 months including 16 females), there were 4 R-DVT (8.3%) with a PTS incidence of 23.5% at 54 months—vs 12.17% (P < 0.05%) in the sulodexide group and 18.23% (P < .05) in the SM group. The incidence of PTS was significantly higher (P < 0.05%) in comparison with the other 2 groups.
As shown in Table 1, the incidence of PTS was significantly lower (P < .05) in the sulodexide group in comparison with the 2 other management groups at 60 months. Also, (Figure 1) the occurrence of R-DVT was higher in the aspirin group (4 in 48 patients equivalent to 8.3%) and lost patients were 14.53% of those included (mostly due, in 6 of 7 patients, to tolerability problems).
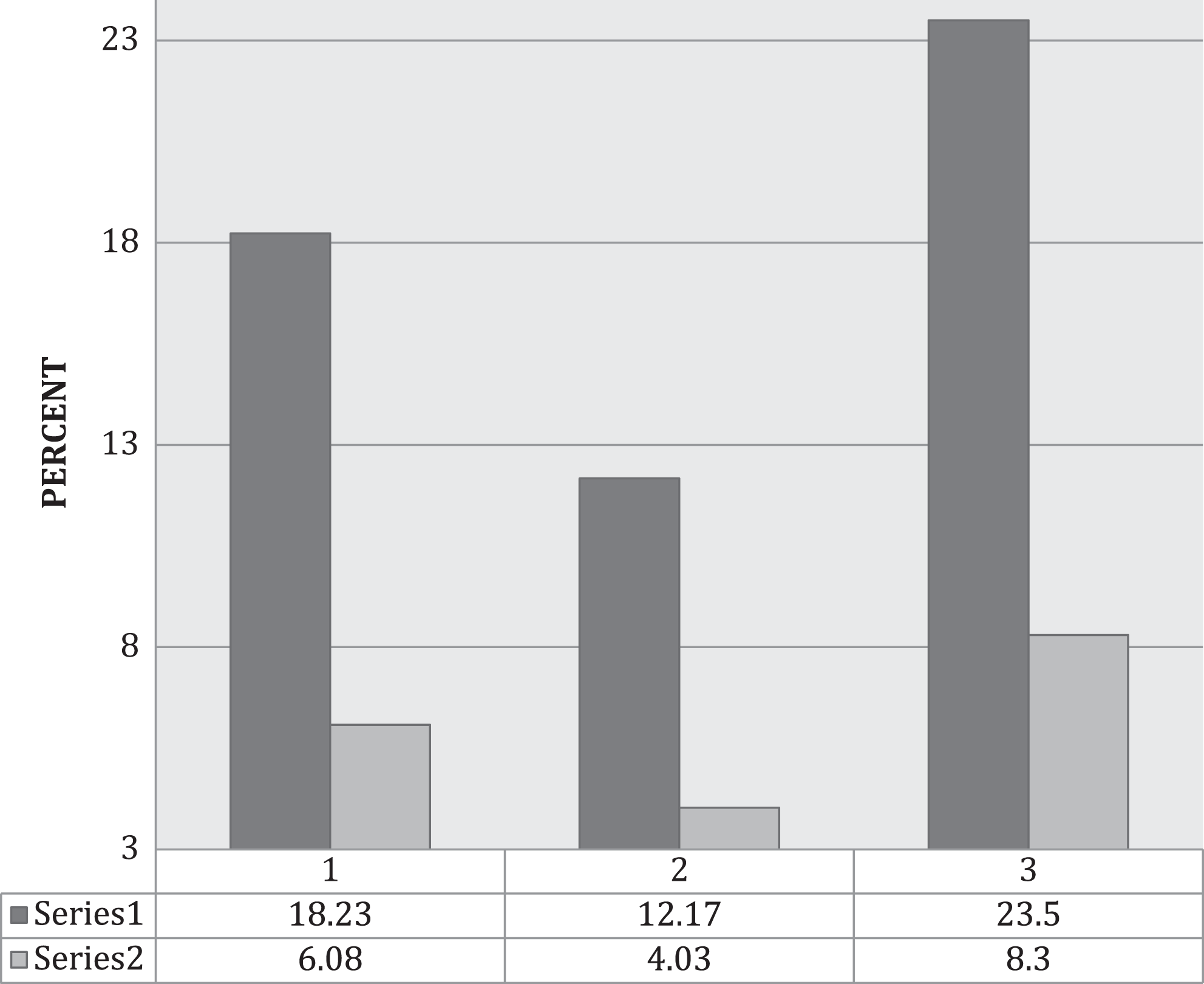
Percentage of patients with postthrombotic limbs (black) or recurrent DVT (gray) at 54 Months: Group 1: standard management (SM); group 2: SM + sulodexide; group 3: SM + ASA. DVT indicates deep venous thrombosis; ASA, aspirin.
Compliance with SM in these patients was optimal with >95% of patients following the instructions. The compliance was also optimal with sulodexide (>93% of the tablets correctly used) and less in the aspirin group with 78% of the tablets correctly used (this group had a significantly higher number of patients with minor tolerability problems, which forced them to skip some administrations). Sulodexide-treated patients experienced no bleeding or other events.
Discussion
Postthrombotic syndrome in the postanticoagulant treatment period and R-DVT have a complex relationship, never fully explored. 3 Their incidence could be variable in different age-groups and complicated by comorbidities that are frequent in older patients using several treatments. 3,5 –14
Invasive treatments used at the moment DVT are diagnosed (ie, thrombolysis) and may increase short- and long-time venous patency, reducing the following incidence of R-DVT and eventually PTS in comparison with anticoagulation only. 27 –29
It is important to observe that these patients had no venous compression that could have predisposed to recurrent thrombosis. 30
Long-term treatment with LMWH versus standard therapy 31 –36 also produces better recanalization. In long-term LMWH groups, there is also a decrease in the incidence of PTS in patients with complete recanalization. 37–40 The development of ulcers 38,39 can be reduced by about 87% with long-term LMWH treatment after DVT. However, alteration in platelets, bleedings, and costs may complicate this type of treatment.
According to the IUA Consensus, 3 in patients with DVT, every effort should be made to reduce recurrences using adequate management and attention (after the prescribed period of anticoagulation). In some patients with DVT associated with nontumoral venous compression, prevention of PTS may require angioplasty or stenting of a proximal stenosis in association with early thrombus removal, as the venous alteration may soon produce a second episode of DVT. 3
The efficacy of medical treatment with antiplatelet agents is relatively limited in venous diseases. Aspirin (100 mg/d) may lower the incidence of R-DVT to 6% to 7% (it is some 10%-12% in comparable patients not using aspirin) in the 3 years following DVT. This 42% reduction in R-DVT is around 50% of the incidence observed with the newer anticoagulants rivaroxaban and dabigatran. However, aspirin cannot be used in all patients and tolerability problems, including gastric bleeding, may occur.
Sulodexide is considered a safe product used for years in prothrombotic and thrombotic conditions for both prevention and treatment. The low molecular weight of both sulodexide fractions allows significant and consistent oral absorption compared to unfractionated heparin. The effects of sulodexide differ from other glycosaminoglycans and are mainly characterized by a longer half-life and reduced effects on global coagulation. Bleeding parameters are not significantly altered. The presence of both glycosaminoglycan fractions enhances the antiprotease activities of antithrombin III and heparin cofactor II. Studies from Loyola University (Chicago) indicate its important antithrombotic effects and their pathways. 41 Other studies have shown the effective action of sulodexide in prothrombotic conditions and its safety. 41 –44
This study, using nonparallel groups, indicates that the occurrence of PTS is significantly reduced in patients using sulodexide. Results are significantly better than those obtained with the SM group and in the group using aspirin (which includes only those who can safely use aspirin). This follow-up also evaluated the rate of recurrence of DVT.
Considering the younger age of these patients, the incidence and consequences of PTS were the main focus of the investigation. In a follow-up of older patients still in progress, the focus will be mainly on recurrence (more frequent in older patients) and on the optimal prevention of R-DVT that may produce more postthrombotic problems.
Conclusions
The interaction between PTS and R-DVT is complex as recurrences cause more PTSs, and a postthrombotic limb is definitely more prone to R-DVT. Sulodexide administration seems to have a definite advantage in this clinical arena where no other significant treatment options are at the moment available or present. Dosages and timing of sulodexide administration should be fully explored in more comprehensive and complete studies.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
