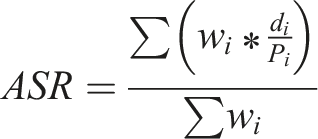Abstract
Objectives
This study aims to provide the most up-to-date temporal trends in incidence, mortality, and disability-adjusted life years (DALYs) of total gastric cancer in China from 1990 to 2019, and to predict the gastric cancer trends up to 2040.
Methods
Data for the incidence, mortality, and DALYs of stomach cancer in China from 1990 to 2019 were extracted from Global Burden of Disease Study 2019 (GBD 2019). We conducted joinpoint regression analysis to explore possible segmented changes in gastric cancer trends. We predicted gastric cancer trends up to 2040 using a Bayesian age-period-cohort model.
Results
The absolute incidence, mortality, and DALYs of gastric cancer increased from 1990 to 2019 in China. However, the age-standardized rates (ASRs) of incidence, mortality, and DALYs for gastric cancer decreased between 1990 and 2019, and the reductions were more pronounced for mortality and DALYs for gastric cancer.
Conclusion
Our study generally reveals favorable declining trends of gastric cancer incidence and predicts that this will continue to 2040. However, the high contemporary incidence combined with China’s aging population will likely slow or even reverse the declining trend in gastric cancer mortality.
Introduction
Gastric cancer is characterized by the growth of cancerous cells within the lining of the stomach. This cancer was the most predominant cancer worldwide less than a century ago. Although gastric cancer has been steadily declining in incidence in the past several decades, it remains 1 of the most common and deadly diseases in the world. 1 According to the most recent estimates from the WHO, there were approximately 1.1 million new cases and around 770,000 deaths due to gastric cancer in 2022 2 ; thus, gastric cancer ranks fifth in incidence and fourth in mortality globally. There is substantial geographic variation in gastric cancer incidence rates with the highest rates in Eastern Asia (Japan, Mongolia, and China) and Eastern Europe. Of note, China alone accounts for 43.9% of the global incident cases, 3 and gastric cancer ranks as the second most diagnosed cancer and the second most common cancer death in China. 4
Previous studies have revealed different risk factors for high gastric cancer incidence rates in China. Helicobacter pylori (H pylori) infection has been recognized as the most predominant risk factor for gastric cancer, 5 and a recent global meta-analysis study suggests that China has the highest prevalence of H pylori infection in Eastern Asia. 6 Epstein-Barr virus (EBV) is another infectious factor that increases the risk of gastric cancer. 7 Many other lifestyle risk factors, including smoking, 8 a highly salted diet, 9 and consumption of foods rich in N-nitroso compounds, have been reported as common risk factors in China. Rapid economic development and continuous urbanization in China have led to dramatic lifestyle changes with increasing smoking rates and dietary habits and better access to health care. These lifestyle changes inevitably impact the trajectory of gastric cancer in China. 10
Many epidemiological studies have reported changes in the incidence and mortality of gastric cancer in China,11-14 yet most previous studies are consecutive cross-sectional studies without standardized methodology. Thus, this study aims to provide the most up-to-date temporal trends in incidence, mortality and DALYs of total gastric cancer in China from 1990 to 2019 and predict the incidence and mortality of gastric cancer up to 2040. These predictions will provide helpful insights for understanding the changing disease spectrum of gastric cancer and optimizing health resource allocation.
Methods
Data sources for the incidence, mortality and disability-adjusted life years (DALYs) of stomach cancer in China from 1990 to 2019 were extracted via the Global Health Data Exchange (GHDx) online data source query tool (https://ghdx.healthdata.org/gbd-2019.) of the GBD 2019. We obtained data on the annual number of cases and age-standardized rates (ASRs) for the incidence, mortality, and DALYs along with their 95% uncertainty interval (uncertainty interval given by GBD databases refers to confidence interval) of gastric cancer, which was defined as C16 in The International Classification of Diseases (ICD) code 10th Revision (ICD-10). All data were extracted for both sexes together, male, female, all age groups and specific age groups, including zero to 14 years, 15 to 49 years, 50 to 69 years, and 70 plus years. This study extracted publicly accessible data from the Global Burden of Disease Study 2019, which contains deidentified data not directly linked to individuals. Thus, the institutional review board waives the requirement for ethical approval.
GBD studies have different estimation processes for nonfatal and fatal outcomes. Detailed methodological descriptions of GBD 2019 can be found elsewhere.15,16 In our study, the incidence of gastric cancer was estimated with DisMod-MR 2.1, an updated Bayesian regression analytical tool used in GBD to estimate nonfatal health outcomes. Estimates of fatal outcomes were performed using the Cause of Death Ensemble model (CODEm), a highly systematized tool that estimates mortality for gastric cancer by location, age, sex, and year. Both DisMod-MR 2.1 and CODEm could produce the estimates with a multiple source of data. The input data for gastric cancer includes data from the National Central Cancer Registry of China with 574 cancer registries in China, covering a population of 438 million (31.5% of the Chinese population). 17
Statistical Analysis
We reported the absolute number and the age-standardized rates (ASR) for incidence, mortality and DALYs of gastric cancer. The ASR was obtained by adjusting for differences in age across different times. For example, the ASR for mortality of gastric cancer:
We estimated the magnitude of the ASR change between 1990 and 2019, and we calculated the percentage of change in ASR for incidence, mortality and DALYs in China. The estimates were reported for overall gastric cancer and sex-specific and age group-specific gastric cancer.
We also conducted joinpoint regression analysis to explore the possible segmented changes in gastric cancer trends. Instead of assuming a universal direction of change, joinpoint regression analysis may specify several joinpoints in a linear regression model fitting a series of joined straight lines to incidence rates, which allows for the assessment of the magnitude and direction of different trends over time. The estimated annual percent change (APC) was then computed for each of the identified trends by fitting a regression line to the natural logarithm of the rates using calendar year as a regressor variable. 18 The tests of significance for each trend used a Monte Carlo permutation method. 19 Following the guidelines of the Joinpoint Regression Program based on the number of data points in the datasets, the number of joinpoints was limited to a maximum of 3. 20
We predicted the age-standardized incidence rates and mortality rates of gastric cancer for males and females up to 2040 using a Bayesian age-period-cohort model. The classic APC model is often modeled as a logit model:
Results
Change of Incidence, Mortality, and DALYs for Gastric Cancer Between 1990 and 2019 in China.

ASR: Age-standardized rates per 100,000; DALYs: disability-adjusted life years; § percentage change in ASR between 1990 and 2019.
Figure 1 presents the full trend of absolute numbers and ASRs of incidence, mortality, and DALYs for gastric cancer in China between 1990 and 2019. The absolute numbers of incidences, mortality, and DALYs for gastric cancer showed increasing trends between 1990 and 2019, and the increase was more pronounced between 2000 and 2005. Of note, the absolute numbers of incident gastric cancer cases and gastric cancer deaths were similar in 1990, but the number of incident gastric cancer cases was substantially greater than that of gastric cancer deaths in 2019. The ASRs of incidence, mortality, and DALYs for gastric cancer presented overall declining trends, and the magnitude of decline was more pronounced for the ASR of gastric cancer mortality. The change trends for incident number and age-standardized rates of gastric cancer in China between 1990 and 2019. (A) Incidence; (B) Mortality; (C) disability-adjusted life years (DALYs); Bar represents incident cases and line represents age-standardized rates.
Figure 2 presents the sex-specific estimates of each year for ASR of incidence, mortality, and DALYs for gastric cancer in China between 1990 and 2019. There is substantial disparity in the ASRs for incidence, mortality, and DALYs between males and females with males exhibiting higher ASRs for incidence, mortality, and DALYs. We also observed trends of disparity expansion. The ratio of ASRs for incidence between males and females was 2:1 in 1990 and increased to 3:1 in 2019. Similar findings were also observed for ASRs of mortality and DALYs between males and females. Sex-specific trends for ASR of incidence, mortality, and DALYs for gastric cancer in China between 1990 and 2019. (A) Incidence; (B) Mortality; (C) disability-adjusted life years (DALYs).
Joinpoint Analysis for Incidence, Mortality and DALYs Rates of Gastric Cancer in China, 1990-2019.

APC = estimated annual percent of change; AAPC = average annual percent of change.
The validation of the Bayesian APC model is provided in Supplemental Figure 1. Despite some variations, the predictions and observed values are generally well aligned. Figure 3 presents the predicted ASR of incidence and mortality for males and females. The ASR of incidence and mortality showed similar values before 2000, and since then, the ASR for incidence substantially surpassed the ASR for mortality, which remained steady in both males and females. It is anticipated that consistent decreasing trends for both incidence and mortality occurred in males and females between 1990 and 2019, and the sharpest decreasing trends were observed between 2005 and 2019. However, from 2019 to 2040, the declining trends for incidence will continue but will be much greater than the trends before 2019 in both males and females. Even mild increasing trends are predicted for mortality from 2019 to 2040, and the effect is more pronounced in males. In 2040, the ASR for incidence will remain substantially higher than the ASR for mortality. Males will still have higher ASRs for incidence and mortality than females. Predicted age-standardized rates of incidence and mortality for gastric cancer in China between 1990 and 2040.
Discussion
To our limited knowledge, this information is the most comprehensive analysis and prediction of the incidence, mortality and DALYs of gastric cancer in China over a period of several decades. Despite population growth, our study reveals general favorable decreasing trends in ASR incidence, mortality and DALYs for males and females between 1990 and 2019. Males generally exhibit greater ASRs of incidence, mortality and DALYs for gastric cancer than females. However, females exhibit greater reductions in ASR incidence, mortality and DALYs than males, which results in an increase in sex-based disparity. The high incidence in contemporary China combined with an aging population and a paucity of breakthrough treatment advances may lead to further increases in mortality of gastric cancer in China.
Despite the increased incidence and mortality, the ASRs of gastric cancer incidence and mortality decreased by 18.6% and 42.4%, respectively, between 1990 and 2019. Our results align with some prior studies that reported continuous declining trends for ASRs for the incidence and mortality of gastric cancer in China.22,23 The decrease in stomach cancer incidence in our study is closely associated with dramatic improvements in the socioeconomic environment and improved lifestyle, including better refrigeration, reduced consumption of salts, and consumption of more fruit and vegetables over the past decades. In addition, the prevalence of H pylori infection, a definite gastric carcinogen, has decreased substantially in China. 6 This reduction in H pylori infection also contributes to the decrease in gastric cancer incidence. However, China has a higher H pylori prevalence (56%) than the UK and USA (35.5% for the UK and 35.6% for the USA). 6 Without national H pylori screening and eradication programs, the incidence rate for gastric cancer will remain higher than that in other Western countries.
A greater reduction in the mortality rate of gastric cancer is noted compared with the incidence rate in China. Endoscopic screening can potentially prevent deaths from gastric cancers by early diagnosis and early treatment and has been widely adopted in screening programs. 24 Despite the lack of a nationwide endoscopic screening program, China launched endoscopic screening exclusively in high-risk areas since 2006. 25 Given that more gastric cancer cases were identified at an early stage by screening tests, initiation of early treatment could improve clinical outcomes and ultimately significantly reduce mortality. Early gastric cancer detection improved the 5-year survival rate from 63.7% to 89%.26,27 A decreasing trend of gastric cancer mortality could be associated with a gradual increase in gastric cancer screening tests in China. In addition, the declining trend of gastric cancer mortality might be associated with improved clinical management. Over the past decades, more attention has been given to standardized treatment and multidisciplinary management of gastric cancer. Multimodality strategies have been demonstrated to improve the survival outcomes of gastric cancer. 28 For example, adjuvant radiochemotherapy following surgery increased the overall survival rate by 32% and relapse-free survival rate by 51%. 29
Males generally have higher ASRs for the incidence and mortality of gastric cancer than females in China, and this sex difference has also been reported in other studies.30,31 Both environmental and genetic risk factors contribute to the patterns of sex differences in gastric cancer. H pylori infection and smoking and alcohol use are well-established risk factors for gastric cancer, and all of these factors exhibit a predominately higher prevalence in males than females.6,32 Biologically, a meta-analysis supported the hypothesis that longer exposure to estrogen effects of either ovarian or exogenous origin may decrease the risk of gastric cancer. 33 Although the ASRs for indigence and mortality experienced declining trends in both males and females, the reduction was more pronounced in females. The differential decline pattern by sex is mainly explained by different reduction rates of H pylori infection prevalence with females reporting a larger reduction in H pylori infection prevalence than males. 34
Our study also predicts the incidence rates and mortality rate of gastric cancer up to 2040 in China, demonstrating continuous declining trends for incidence rates but mild increasing trends for mortality rates in both males and females. However, even with a substantial reduction, the incidence of gastric cancer in 2040 in China will remain higher than that in other Western countries. 35 High baseline prevalence of H pylori infection and dietary habits included consumption of preserved, salty or fried foods, and hot soup/porridge. 36 Although clear epidemiological associations are noted between diet and gastric cancer, the role of dietary interventions remains unproven. However, a recent real-world study indicated that population-based eradication of H pylori can significantly reduce gastric cancer incidence. 37 China currently has no national H pylori screening and eradication program. Given the substantial burden of gastric cancer in China, mass screening and eradication of H pylori should be considered at the national level. The moderate upward trend in gastric cancer mortality in China by 2040 may be due in part to the aging of the Chinese population. 38 The high incidence of gastric cancer in contemporary China combined with an aging population and a paucity of breakthrough treatment advances may lead to further increases in the absolute number of deaths from gastric cancer in China. However, national gastric screening tests that identify gastric cancer at an early stage may offset the increase in mortality of gastric cancer in China.
Several limitations should be noted before interpreting our study findings. The validity and accuracy of the GBD data depend heavily on the availability and quality of raw survey and surveillance data, as well as the data processing methodology. Notably, the input data may not fully cover the entire population, which could affect the comprehensiveness of the results. Second, our analysis was limited to age and sex subgroups, and we were not able to explore the geographic pattern of gastric cancer in China. Further studies examining the detailed distribution of gastric cancer in China are warranted in the future. Finally, the prediction is based on a statistical model that assumes that the trends of gastric cancer are dependent on age, period and cohort effect, but this model does not account for further treatment or prevention advances, such as novel treatment for gastric cancer or massive screening for early-stage gastric cancer. Thus, a scenario simulation model may be more useful.
Conclusion
Our study generally reveals favorable declining trends of gastric cancer incidence from 1990 to 2019 and predicts that those declining trends will continue to 2040. The decrease in stomach cancer incidence in our study may be closely associated with dramatic improvements in the socioeconomic environment and improved lifestyle. Sex differences in gastric cancer in China may provide insight into the development of further interventions, including more alcohol and smoking cessation interventions for men and targeted H pylori screening for men. Notably, although the incidence of gastric cancer is trending further downward, the high contemporary incidence combined with China’s aging population will likely slow or even reverse the declining trend in gastric cancer mortality.
Supplemental Material
Supplemental Material - The Trends of Gastric Cancer in China From 1990 to 2019 and Predictions to 2040: A Bayesian Age-Period-Cohort Prediction Study
Supplemental Material for The Trends of Gastric Cancer in China From 1990 to 2019 and Predictions to 2040: A Bayesian Age-Period-Cohort Prediction Study by Hongyu Yang, Suya Zhou, Wei Wang, Yanrong Zhao, Yinwei Qiu, Xuewen Jiang, Tianxiang Lin, and Qing Yang in Cancer Control
Footnotes
Acknowledgments
We highly appreciate the works by the Global Burden of Disease Study 2019 collaborators.
Author Contributions
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by Zhejiang Province Health and Health Technology Plan (2023PY993).
Ethical Statement
Data Availability Statement
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.