Abstract
Background
Persistent infection with high-risk human papillomavirus (HPV) is closely related to cervical cancer. The epidemiologic characteristics of cervical HPV have regional differences. Therefore, it is necessary to develop the most favorable policies according to the actual situation of each region to prevent and reduce the prevalence of cervical cancer. This retrospective cross-sectional study investigated the prevalence, gene subtypes, and temporal trends of HPV in women undergoing physical examination in Wenzhou, to provide a decision-making basis for further prevention and control of HPV.
Methods
A total of 31 131 cervical exfoliated cell specimens obtained from physical examinations in Wenzhou, a coastal city of China, from 2015 to 2020 were collected. The age distribution was analyzed using the chi-squared test, and the time change trend was analyzed using the Mann–Kendall trend test. On this basis, the distribution characteristics of the HPV subtypes were analyzed.
Results
The total prevalence rate was 9.55%, and the prevalence rate in different age groups ranged from 7.77% to 14.16%. The prevalence rate in different years was 8.84%-11.83%. The prevalence rate was bimodal; it was highest in the group 25 years old, followed by the group >61 years old. The top five high-risk gene subtypes were HPV52, HPV58, HPV53, HPV16, and HPV39, whereas the low-risk subtypes were HPV61, HPV81, HPV44, HPV43, and HPV55. Of all the positive samples, 76.03% were infected with a high-risk subtype.
Conclusion
Most female HPV patients in Wenzhou are infected with high-risk gene subtypes. Therefore, physical examination and screening for HPV should be further strengthened, and the corresponding vaccination policy should focus on high-risk gene subtypes.
Plain language summary
Background: Persistent infection with high-risk human papillomavirus (HPV) is closely related to the occurrence of cervical cancer. The epidemic characteristics of cervical HPV have regional differences, Therefore, it is necessary to formulate the most favorable policies according to the actual situation of each region, so as to prevent and reduce the prevalence of cervical cancer. This retrospective cross-sectional study investigated the prevalence, gene subtypes and temporal trends of HPV in women undergoing physical examination in Wenzhou. To provide decision-making basis for further prevention and control of HPV. Methods: A total of 31,131 cervical exfoliated cell specimens obtained from physical examinations in Wenzhou, a coastal city of China from 2015 to 2020, were collected. The age distribution was analyzed by the chi-squared test, and the time change trend was analyzed by the Mann–Kendall trend test. On this basis, the distribution characteristics of HPV subtypes were analyzed. Results: The total prevalence rate was 9.55%, and the prevalence rate in different age groups ranged from 7.77% to 14.16%. The prevalence rate in different years was 8.84%-11.83%. The prevalence rate was bimodal; it was highest in the group less than or equal to 25 years old, followed by the group greater than 61 years old. The top five high-risk gene subtypes were HPV52, HPV58, HPV53, HPV16 and HPV39, while for low-risk were HPV61, HPV81, HPV44, HPV43 and HPV55, respectively. Of all the positive samples, 76.03% were infected with a high-risk subtype.
Background
Cervical cancer is the most common type of cancer in women worldwide and is one of the leading causes of cancer-related death in women. In 2020, there were 604 200 new cases of cervical cancer and 310 000 cases of cervical cancer-related death globally, 1 seriously threatening the lives and health of women. Of this, 85% of the cancer burden occurs in developing countries.2–6 The incidence and mortality rate of cervical cancer in China are at the international medium level. 7 Cervical cancer is the only malignant tumor with a clear and preventable cause, which is caused by persistent and close infection with the human papilloma virus (HPV). 8 It is mainly transmitted through sexual activity.9–11 Early screening can effectively prevent the occurrence and development of precancerous lesions and cancer. In 2020, WHO released the Global Strategy to Accelerate the Elimination of Cervical Cancer, with 194 countries committing to eliminate cervical cancer for the first time. 12 In recent years, the incidence of cervical cancer has been on the rise in China, especially among young people.13,14 China has the highest number of new cases and deaths from cervical cancer. 15 How to deal with it is a major challenge in the prevention and treatment of cervical cancer. This study investigated the prevalence, genetic subtypes, and time trend of HPV among women who underwent physical examination in Wenzhou City from 2015 to 2020. We analyzed the data using a retrospective cross-sectional epidemiological method to provide a scientific basis for developing prevention strategies.
HPV, a mucosal and skin epithelial virus, is the primary cause of cervical epithelial hyperplasia and cervical cancer. 16 Previous studies have shown spatial and temporal heterogeneity in the prevalence, age distribution, and subtype distribution of HPV.17–19 From the perspective of regional prevention and control of cervical cancer, vaccination effectiveness is closely related to the prevalence and distribution of HPV infection. 20 However, HPV infection usually does not cause physical discomfort, and the incubation period from precancerous lesions to cervical cancer can be up to 10 years. In general, comprehensive prevention and control measures such as early screening, early diagnosis, early vaccination, and early treatment can effectively reduce the incidence of cervical cancer.21,22 Physical examination helps to reflect local cervical cancer rates, and screening can detect precancerous lesions earlier in healthy women. 19
The epidemic characteristics of cervical HPV have regional differences. Therefore, it is necessary to develop the most favorable policies according to the actual situation of each region to prevent and reduce the prevalence of cervical cancer. Wenzhou is an economically developed coastal region in eastern China with a population of approximately 9 million. However, data on the prevalence and genetic subtypes of HPV among women examined in Wenzhou and many other areas are still lacking. HPV DNA detection is one of the main methods to screen and diagnose cervical lesions from the angle of etiology, which has the characteristics of high speed and high sensitivity.23,24 In this study, multiple polymerase chain reaction (PCR) with universal primers and flow cytometry were used to detect HPV DNA in cervical cells of 31 131 women examined at Wenzhou Hospital during 2015-2020. The results revealed the distribution characteristics and genetic subtypes of HPV epidemic and provide epidemiological basis for cervical cancer vaccination. At the same time, it is of great clinical significance to judge the occurrence and development of diseases as an evaluation index for doctors’ diagnosis and treatment.
Materials and Methods
General Information
The data were collected from 31 131 samples of exfoliated cervical cells obtained during physical examinations at a hospital in Wenzhou, Zhejiang Province, China, between January 2015 and December 2020. Duplicate samples from the same woman were excluded. All participants were women who voluntarily visited the hospital for medical examination. Participants ranged in age from 19 to 84 years, with a median age of 44 years and a mean age (±SD) of 44 (±11) years. They were divided into the following nine groups according to their age: ≤25, 26-30, 31-35, 36-40, 41-45, 46-50, 51-55, 56-60, and ≥61 years old.
Patient and Public Participation
This retrospective study was approved by the Ethics Committee of a hospital in Wenzhou, Zhejiang Province (approval number 2021-62). The data were obtained from an anonymized dataset typically used for administrative purposes and did not involve patient interventions. The dataset contains only diagnostic information for outpatients, patient identification number (each patient has a unique number for identification), date of visit, age, and gender. The requirement for informed consent was waived by the Ethics Committee because the data were anonymous. Patients or the public were not involved in the design, implementation, reporting, or dissemination of our studies.
Instrument, Reagents and HPV Genotyping
In this study, HPV DNA in cervical cells was detected by PCR using universal primers and flow cytometry. The Touch thermal cycler with a 96-well module was obtained from Hangzhou Biotechnology Co., Ltd. A Luminex 200 flow cytometry platform was obtained from Luminex. The HPV-DNA typing kit was obtained from Shanghai Tou Jing Life Technology Co., Ltd. The kit can detect 27 HPV subtypes, including 17 high-risk subtypes (HPV16, HPV18, HPV26, HPV31, HPV33, HPV35, HPV39, HPV45, HPV51, HPV52, HPV53, HPV56, HPV58, HPV59, HPV66, HPV68, and HPV82) and 10 low-risk subtypes (HPV6, HPV11, HPV40, HPV42, HPV43, HPV44, HPV55, HPV61, HPV81, and HPV83), as classified by the International Agency for Research on Cancer. HPV genotyping was performed using the HPV typing test kit (PCR + flow fluorescence hybridization). This method was approved by the State Food and Drug Administration (China Food and Drug Administration Certificate (2014):3 400 847). All tests were performed in accordance with the technical operating procedures of the hospital laboratory.
Specimen Collection and Treatment
Specimens were collected as follows. First, the vagina was opened and the cervix was exposed using a vaginal dilator. Second, the cervix and its secretions were wiped with a cotton swab. Third, the cervical brush was rotated four to five times in a clockwise direction. Finally, the cervical brush head was placed into an eluent tube containing cell preservation solution, and the tube was closed and marked, keeping the tube upright. Samples were stored at 4°C and tested within 3 days using a kit following the manufacturer’s instructions.
Statistical Methods
All HPV data from 2015 to 2020 were entered into an Excel spreadsheet and then analyzed using SPSS, and the overall and type-specific prevalences of HPV were calculated. All genotypes from single and multiple infections were computed individually. These data were also stratified by age (≤25 years, 26-30 years, 31-35 years, 36-40 years, 41-45 years, 46-50 years, 51-55 years, 56-60 years, and ≥61 years). Count data are expressed as frequency or percentage. The chi-square test was used to compare the positive rate of each group, and the Bonferroni method was used to adjust the P-value for paired comparisons between the two groups. The time trend of the positive rate over the years was analyzed using the Mann–Kendall trend test. Statistical tests were two-tailed. Statistical analysis was performed using R. If P ≤ .05, the differences were considered statistically significant.
Results
HPV Infection Status
Prevalence of HPV in Different Age Groups.

Prevalence of HPV in Different Years.
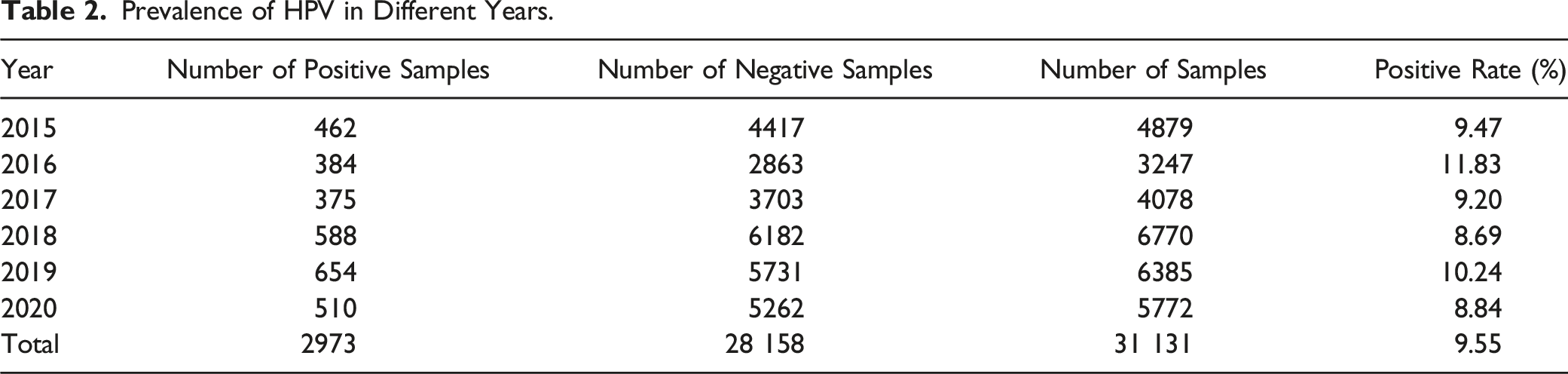
Distribution of HPV Subtypes
Distribution of HPV Subtypes.

HPV is a mucosal and skin epithelial virus that is a major factor in cervical epithelial hyperplasia and cervical cancer. The main factors of cervical epithelial hyperplasia and cervical cancer include more than 100 subtypes, among which more than 30 subtypes can infect human reproductive tract mucosa, and the pathogenic ability of different subtypes is quite different. Based on whether the hyperplastic lesions caused by them are carcinogenic, they are divided into two categories: high-risk type and low-risk type, 25 among which the high-risk type is related to cervical cancer.
Multiple HPV Infections
Multiple Infections of HPV.

Discussion
Cervical cancer is one of the major causes of cancer death in women worldwide 26 and one of the major public health problems worldwide. Seriously threatening the lives and health of women. In this study, 31 131 cervical exfoliated cell samples were collected from female physical examinations in Wenzhou, China, from 2015 to 2020. Mann-Kendall trend test was used to analyze the time change trend of the prevalence rate and the distribution characteristics of HPV genotypes. In contrast to previous studies, physical examination is usually carried out without any symptoms, to reflect the incidence of cervical cancer more objectively in the region and help to develop cervical cancer screening and prevention strategies in line with local conditions. Simultaneously, screening can detect cervical precancerous lesions earlier in healthy women and get active treatment in early detection, to achieve the purpose of early detection, early diagnosis, and early treatment. The results of this study can provide a basis for further improvement of HPV diagnosis and vaccine application in the region. In addition, it is of great clinical significance to judge the occurrence and development of diseases as an evaluation index of doctors’ diagnosis and treatment.
The study found that the total infection rate of HPV was 9.55%, and mainly high-risk subtypes were detected. Among high-risk HPV subtypes, HPV52 was the most common (14.44%), followed by HPV58 (8.75%), HPV53 (8.34%), HPV16 (6.86%), and HPV39 (5.07%). In HPV-positive cases, monotypic infection was significantly more common than polytypic infection. In contrast, polygenic infection rates were significantly higher in those aged ≤25 years and those aged ≥61 years. The HPV infection rate was bimodal in the different age groups. The first infection peak occurred in the age group ≤25, the infection rate of 14.16 %; The second infection peak occurred in the ≥61 age group, with an infection rate of 13.23%. The infection rate of these two groups was significantly higher than the total infection rate of 9.55%. It was highest among young people and second highest among older people. This might be due to different sexual activity, cervical local immune susceptibility, or immune self-clearance status. The higher positive rate in women under 25 years of age is related to the lack of self-protection awareness and also to imperfect acquired immunity, frequent sexual life, and more induced abortion. 27 For young women, health literacy education, especially sex education, should be strengthened. The prevalence of HPV infection in middle-aged and elderly women is on the rise, which may be due to changes in menopausal hormones and sex, the decline of immune function in the elderly, and the weakening of the ability to inhibit or eliminate HPV infection. 28 Another reason may be the latent and reactivated high-risk infection, which leads to the second peak of prevalence in middle-aged and elderly women. 29 For postmenopausal middle-aged and elderly women, it is also necessary to strengthen screening for early cervical cancer.30–32
HPV-Positive Rate in Women Tested in Other Regions of China.

The presence of HPV infection and the HPV subtype(s) are important factors for assessing a woman’s risk of cervical cancer. Studies have shown that there are differences in HPV subtype between different regions and different ethnic groups. In western developed countries such as Britain and the United States, the most common high-risk subtype is HPV16, followed by HPV18, HPV45, HPV33, and HPV31. 37 In Greece the most commonly detected gene subtype was HPV16 (5.3%), followed by HPV53 (4.9%). 38 The geographical environment of China is quite different from that of the West, and the distribution of HPV subtypes is different from that of the West. However, China has a vast territory, and the economic development level and medical service capacity of different regions are different, so there are certain differences in female HPV infection rates. Previous studies on women in Mainland China showed that HPV infection of subtypes HPV16, HPV52, HPV58, HPV53, and HPV18 was the main mode of infection in China, with infection rates as high as 19.0%.39–41 Therefore, further longitudinal studies on cervical cancer prevalence and incidence, as well as age stratification and classification strategies in initial HPV screening, are necessary. Based on regional HPV epidemiology, vaccines that are more suitable for inhibiting high-risk HPV subtypes can be developed to make cervical cancer vaccine coverage more accurate and effective.
To compare HPV infection rates before and after the COVID-19 pandemic, data from 2019 and 2020 were further analyzed. As can be seen from Table 2, the HPV infection rate decreased from 10.24% to 8.84% in 2019, Prevalence in the first 4 years ranged from 8.69% to 11.83%. Thus, the decrease could be due to normal fluctuations, or it could be that control measures during the COVID-19 pandemic may have reduced HPV transmission. During the COVID-19 pandemic, strict outbreak control measures and social distancing measures, which limited all types of contact among people, not only stopped the spread of COVID-19, but also reduced the spread of HPV. While these measures negatively affected the mental health of the general public and routine cancer screening and treatment, they also controlled the spread of HPV, other seasonal respiratory viral infections,and sexually transmitted infections.42,43 During the COVID-19 pandemic, not only seasonal respiratory virus infection rates dropped dramatically, but also the incidence of several sexually transmitted diseases, including syphilis, chlamydia, and gonorrhea.44,45
Common HPV High-Risk Subtypes of Physical Examination Women.

Conclusions
In the present study, we analyzed the epidemiologic characteristics of cervical HPV in Wenzhou, with a focus on the distribution characteristics of HPV subtypes. It was found that the high-risk subtypes were HPV52, HPV58, HPV53, HPV16, and HPV39, and 76.03% of the infected persons were infected with high-risk subtypes. Our study highlights that countermeasures are needed to strengthen the prevention and control of HPV. The results of this study provide a basis for further improving HPV diagnosis and vaccine application locally and provide guidance for the subsequent prevention and control of cervical cancer. We also hope to provide a useful reference for the prevention and control of HPV in other areas.
Footnotes
Author’s Note
All authors agree to publish the final manuscript.
Author Contributions
HX conceptualized and designed this study. HH and MZ developed methodologies for data collection and analysis. YG and YZ participated in data collection and analysis. YG and HX participated in writing and editing. All authors were subsequently involved in critically revising the manuscript. All authors have approved the final version of the manuscript to be published and agreed to be accountable for all aspects of the work.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by Soft Science Project of Ministry of Science and Technology (2011GXQ4D050), Natural Science Foundation of Zhejiang Province (LY12H12002).
Ethical Statement
Data Availability Statement
All data generated or analyzed during this study are included in this published article.
