Abstract
Background:
There is increasing interest in the role of pronation as part of the deformity correction in hallux valgus (HV) especially with the advent of weightbearing computed tomography (WBCT) and percutaneous surgical techniques. This study aimed to assess the coronal rotation of the first metatarsal before and after percutaneous distal transverse osteotomy (Metaphyseal Extra-Articular Transverse and Akin Osteotomy [META]) using WBCT and to correlate these findings with clinical outcome scores.
Methods:
A retrospective analysis of prospectively collected data from a single center of patients who underwent WBCT both before and after percutaneous distal transverse osteotomy for hallux valgus correction. The primary outcome was change in pronation on radiographic parameters; Hallux valgus angle, intermetatarsal angle, metatarsal pronation angle, alpha angle, sesamoid rotation angle, arthritis, and sesamoid position were assessed using coronal WBCT images. Secondary outcomes included pre- and postoperative clinical outcomes, including the Manchester-Oxford Foot Questionnaire (MOXFQ), EuroQol–5 dimensions–5 levels (EQ-5D-5L), visual analog scale (VAS) and complication rates.
Results:
Fifty-one feet from 34 patients (32 female, 2 male, mean age 60.3 ± 10.2 years) underwent META. Radiographic data were available for 94.4% of feet with a mean follow-up of 12.1 ± 3.2 months. There was a significant improvement across all radiographic parameters including pronation correction (P < .05). There was also a significant improvement in clinical foot function for all MOXFQ domains, EQ-5D-5L, and VAS pain outcomes (P < .05). The complication rate was 1.9%. There was no significant correlation of postoperative outcomes with radiographic pronation parameters. Regression analysis did not identify any radiographic or clinical variables that predicted change in the MOXFQ Index domain score.
Conclusion:
Percutaneous distal transverse osteotomy for hallux valgus deformity can significantly correct coronal plane pronation and improve patient-reported outcomes, although correction of pronation was not significantly correlated with clinical improvement.
This is a visual representation of the abstract.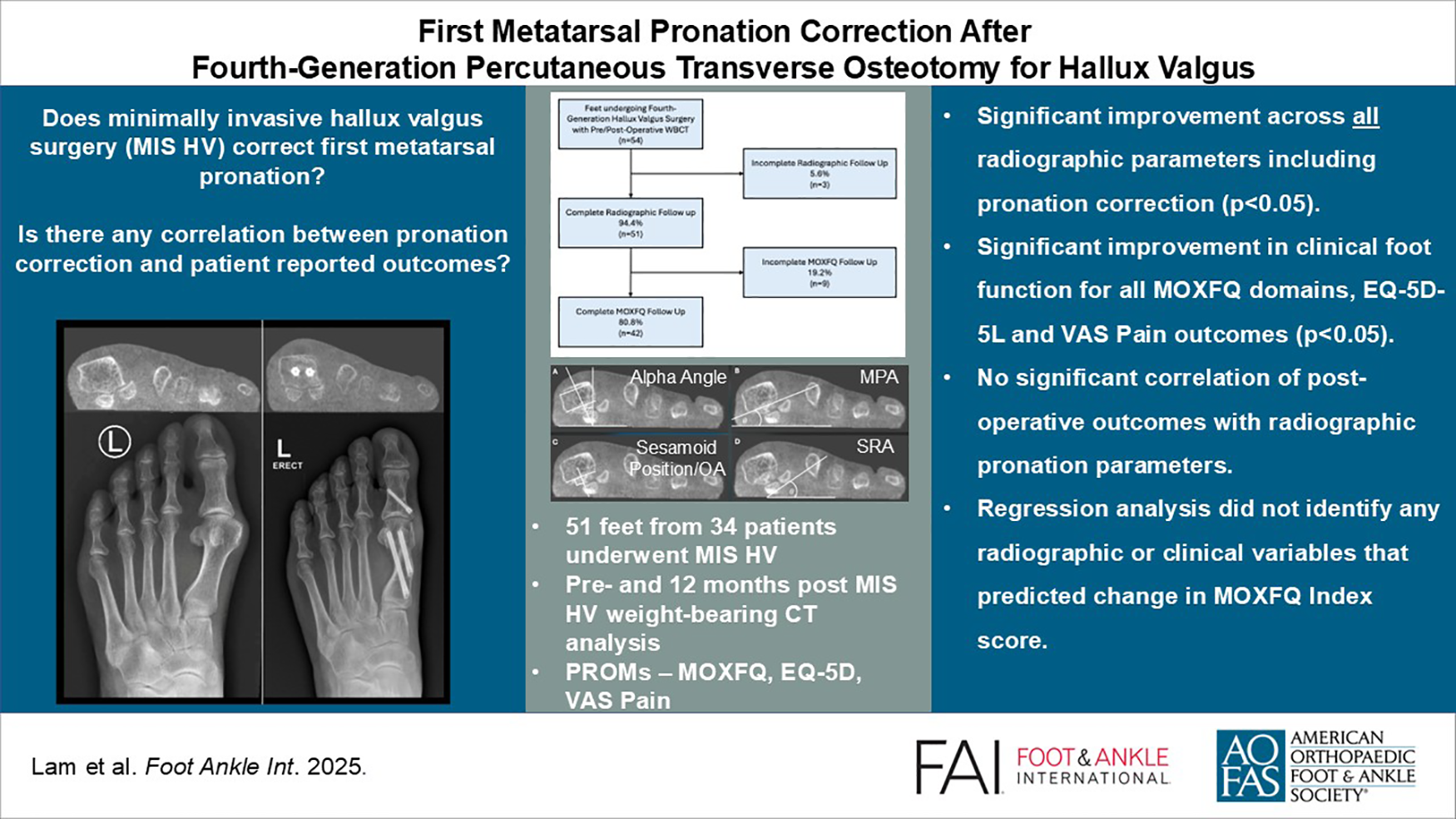
Keywords
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
