Abstract
The impact of acquired brain injury on family members is far reaching. Research has identified experiences of trauma, ambiguous loss and burden of care. Limited research has addressed the ripple effect of brain injury across the wider family. The study aimed to gain a detailed insight into the lived experiences of grandchildren of those who have experienced stroke or brain tumor. Ten participants (eight female and two males aged between 18 and 29) took part in semi-structured interviews about their experiences of grandparental stroke or brain tumor. Data were analyzed using interpretive phenomenological analysis (IPA). Four themes were identified. The data revealed a vivid experience of ambiguous loss, and grief experienced by participants. This was further exacerbated by being protected by family members which led to a sense of isolation from information about their grandparents’ condition. Participants described the secondary impacts on family unit that caused ripples throughout the family network. Finally, participants reported multiple barriers to accessing support that prevented them gaining the emotional and practical support they required. The study highlights the impact of brain tumor and stroke on the wider family unit and the need for systemic approaches to supporting families after brain injury.
Introduction
Brain tumors and strokes are both categorized as acquired brain injuries (ABIs), a type of brain injury that occurs after birth due to traumatic or non-traumatic events (Headway UK, 2020). Across the UK, approximately 16,000 people are diagnosed with a brain tumor each year (The Brain Tumour Charity, 2021) with 88,000 adults and children living with a brain tumor. Additionally, one in six people will have a stroke in their lifetime (Chung, 2014) with an estimated 1.3 million stroke survivors living in the UK (Sentinel Stroke National Audit Programme [SSNAP], 2021).
Post-ABI individuals can experience physiological symptoms, including headaches, motor impairment, impaired balance, impaired vision, and seizures (Marshall et al., 2007). Behavioral and emotional symptoms include anxiety, depression, aggression, and personality changes (Ferro et al., 2016; Gregg et al., 2014). Common cognitive side effects include memory impairment, communication deficits, and executive dysfunction (Coomans et al., 2019; Cumming et al., 2013). Executive dysfunction can cause difficulties with planning, initiating and inhibiting behavior, and decision-making, as well as causing a lack of insight into the individual's condition and abilities (Mukherjee et al., 2006; Wefel et al., 2016). These consequences can lead to lifelong social difficulties for individuals with brain injuries. They can detrimentally impact surrounding family members and their relationship with their relatives. The number and complexity of symptoms and individual experiences differ between cases and can vary throughout their illness trajectory (Arber et al., 2010). An ABI diagnosis and associated symptoms can be life-changing for an individual and significantly impact their family members (Ownsworth et al., 2011).
Family members frequently undertake caregiving responsibilities for those with ABI (Applebaum et al., 2016). Carers UK (2021) define a caregiver as someone who provides unpaid care and support to an individual because of an illness. However, the literature on caregivers primarily focuses on those involved in providing personal care and assistance, overlooking the wider burden caregiving responsibilities have on family members (Odumuyiwa et al., 2019). ABI symptoms can impact an individual's ability to work or complete practical tasks, resulting in increased financial and household responsibilities, and pressure on family members (Sherwood et al., 2006). The burden of care also impacts on the emotional wellbeing of family members (Baker et al., 2017; Tramonti et al., 2019), and their relationship with the injured individual, and others within their family network (Townshend & Norman, 2018). Taking a systemic perspective, while primary caregivers may experience the largest care burden, changes in family dynamics, and responsibilities likely impact the wider family network (Gan et al., 2006). This is particularly relevant when we consider the often close, and special relationship that grandchildren can have with their grandparents (Mills, 2001).
The diagnosis and symptoms of ABI can significantly impact relationships between the individual, and their family members (Ownsworth et al., 2015). Complex care demands and ABI-related changes to the individual's personality have been identified as primary reasons for the deterioration of relationships (Headway UK, 2018). Family members commonly describe their relative's personality changes as a loss of their pre-injury identity, which impacts their ability to maintain a relationship (Townshend & Norman, 2018). This in turn leads to feelings of grief, and loss in family members, impacting the broader family dynamic (Gilmour & Norman, 2025). Behavioral and personality changes such as aggression, irritation, and impulsivity are especially challenging for family members to manage and adjust to (Schubart et al., 2008). The impact of challenging behaviors is exacerbated for family members when the individual lacks insight into their condition, abilities, and limitations (Clark-Wilson & Holloway, 2015). These symptoms are often “invisible,” and the impact can be unrecognized by others, including healthcare professionals (Norman et al., 2020). As a result, family members can experience a lack of understanding and support for these challenges (Holloway et al., 2019), making the impact of brain injury more difficult for injured individuals and their families (Odumuyiwa et al., 2019).
Several studies have found that family members have unmet needs including a lack of information regarding the implications of their relative's illness and prognosis (Arber et al., 2012; Papadakos et al., 2019). Further, Madsen and Poulsen (2011) identified family members who received inadequate practical information to help them manage new caregiving responsibilities, and complex symptoms. The impact of changes in responsibilities, roles, and relationships, combined with unmet needs, can lead to family members experiencing psychological and emotional distress (Applebaum et al., 2016).
Health and social care services rely heavily on informal caregiver contributions (Norman et al., 2024). Therefore, improving our understanding of their experiences and needs is vital (Foley et al., 2022). There is limited research exploring family members’ experiences of having a relative with either a brain tumor or stroke. There is even less focus on the wider family unit and the impact on family members who may not provide the most daily care and support to their loved ones. Research into family members’ experiences has predominantly explored the impacts of direct caregiving responsibilities on the primary caregiver or first-degree relatives. There has been less research focused on the wider family, especially grandchildren and the impact on their relationship with grandparents. From a systemic perspective, such health conditions are likely to have a ripple effect through the wider family, impacting roles, relationships, and support processes. Extended family members often provide crucial emotional and practical support for primary caregivers. The “ripple effect” may therefore result in altered communication patterns, role redistribution and experienced threats to familial relationships (Kitzmüller et al., 2012; Moore & Wagner, 2009). Little research has been conducted looking at intergenerational trauma or psychological distress in these contexts however, these are certainly possible, if not likely when considering comparable difficulties (Boquet et al., 2011). Data from 2023 to 2024 suggests that the average age of onset for stroke fell 6068.2 years in men and 73 in females, meaning more people of grandparenting age are experiencing strokes (NICE, 2025). A similar picture presents regarding brain tumor with those most at risk of developing brain tumors being aged 75–84 years (63.75 per 100,000 (Cancer Research UK, 2021).
Therefore, this study sought to contribute to our understanding of the experiences of wider family members when a relative has an ABI. Specifically, we aimed to gain a detailed insight into the lived experiences of the grandchildren of those who have experienced stroke or brain tumor from a first-person perspective. An interpretative phenomenological approach was adopted to explore grandchildren's accounts of their experiences, and the aspects they highlight as significant to them. The study also sought to understand the support needs of grandchildren, and their experiences with health and social care services. We designed the study to investigate the research question: What are the lived experiences of individuals whose grandparent has a brain tumor or stroke?
Methods
Design
We employed interpretative phenomenological analysis (IPA) in this study. IPA is concerned with a rich, detailed exploration of the lived experiences of individuals from their perspective (Smith & Osborn, 2008). IPA focuses on how individuals make sense of the phenomena they have experienced (Smith & Osborn, 2008). This methodological approach was consistent with the research aims.
IPA is most suited to a data collection method that allows participants to explore their feelings, emotions, and experiences of a phenomenon in their own words (Smith, 2015). Data were collected using online semi-structured interviews; the researcher used a guide to facilitate the interview (Appendix A). The interview guide was informed by previous research into family members’ lived experiences conducted by one of the research team (Gamgee et al., 2023; Townshend & Norman, 2018).
Ethical approval was granted for this study from the University of [University name, School name]. The British Psychological Society Code of Human Research Ethics (BPS, 2021) was adhered to throughout the research. After the interviews, participants were provided with contact details for the second author who is a trained therapist for support with any distress related to talking about their experiences of the research phenomenon.
Participants
The study sample comprised 10 participants (eight females and two males, aged between 18 and 29) each of whom had a grandparent who had experienced a brain injury due to a stroke or a brain tumor. A purposive sampling strategy was utilized to identify and recruit participants with experience of the research phenomenon (Silverman, 2021). We advertised the study on social media through UK organizations that support those with strokes and brain tumors and those that support families, including the Stroke Association, local Headway groups (a UK charity that support people with brain injuries) and Anchor Point (a UK charity that supports family members after brain injury). The study was also advertised through the University research participation pool. To be included in this study, participants had to: (a) have experience with the research phenomenon; (b) be aged 18 years or older; and (c) live in the UK.
Two participants reported the occupations of a hairdresser and compliance inspector, while the rest were university students. For three participants, their relative was deceased at the time of the interview. The sociodemographic information collected from participants can be seen in Table 1; pseudonyms have been used to maintain participants’ confidentiality.
Sociodemographic Characteristics of Participants.
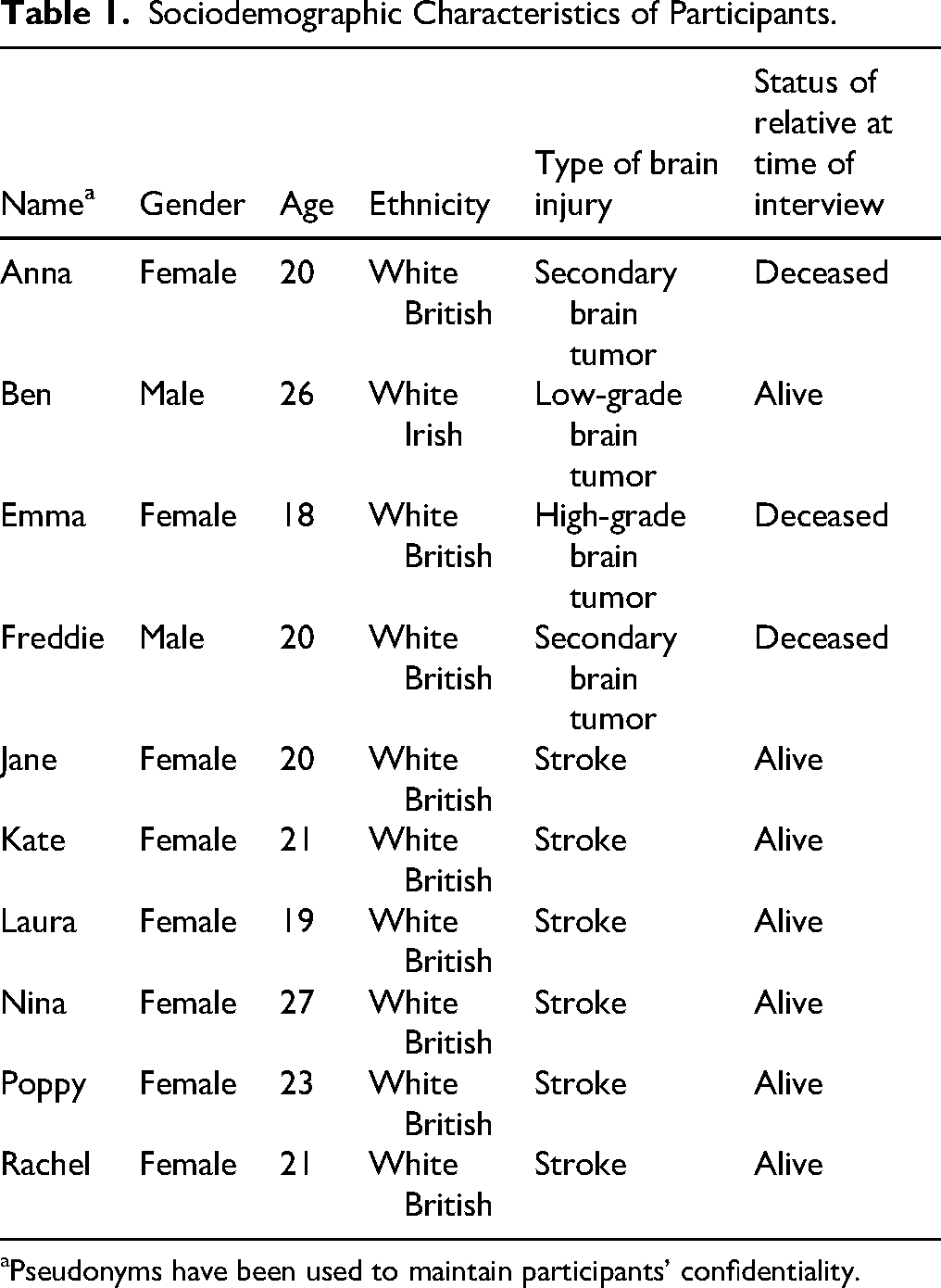
Pseudonyms have been used to maintain participants’ confidentiality.
Data Collection
Participants who expressed an interest in the study after responding to research advertisement were contacted via email and provided with an information sheet, and an electronic consent form and asked to provide demographic information via an online form. The interviews took place online via Zoom, and lasted between 30 and 80 min, with an average time of 45 min. Interviews were audio recorded using Zoom's secure encryption recording service. The first author was responsible for interviewing all participants with experience of brain tumors and the second author interviewed those with experience of stroke. Data was transcribed verbatim, and any identifiable information was anonymized.
Analysis
Data analysis followed Smith and Osborn's (2008) process of IPA: First, the researchers familiarized themselves with a single transcript through rereading and noting down detailed, exploratory notes in the right-hand margin. An inductive approach was adopted to highlight what was emerging from the data, and to comment on the semantic meaning. Second, potential emerging themes were identified and noted in the left-hand margin of the transcript. Themes were collated to review connections and identify themes that represent a central organizing concept of subthemes. This process was repeated with every transcript. Third, the researchers reviewed the analyzed transcripts to integrate emergent themes and identify overarching themes and subthemes. The transcripts were revisited to enable the themes to be refined to ensure a rich, and accurate interpretative analysis of the data. The researchers adopted a multi-perspectival approach. Findings were compared to themes from two research studies that explored the lived experiences of family members whose relatives had a traumatic brain injury (Gamgee et al., 2023; Townshend & Norman, 2018). A multi-perspectival approach synthesizes findings within and between samples to provide insight into congruence or contrast whilst retaining the inductive nature of IPA (Larkin et al., 2019).
Yardley (2008) highlights the importance of demonstrating trustworthiness and validity in qualitative research methods and findings. Smith (2004) identifies two broad categories to demonstrate validity in IPA: (a) internal coherence of study and (b) appropriate representation of enquiry. Internal coherence is concerned with the consistency of the methodological approach, and the research aims. The methodological approach used in this study is consistent with the research aims (to explore and understand the lived experience of grandchildren in families where grandparents had experienced a stroke or brain tumor) and the theoretical underpinnings of IPA. Representation of enquiry refers to the transparency and openness of the research process. Methods of data collection and analysis were clearly outlined under the principles of transparency. Throughout the research process, all those engaged in collecting and analyzing the data kept a reflexive journal to acknowledge and reflect on the positioning and role of the researchers in the study (Yardley, 2008). To improve the trustworthiness of the data analysis, findings, and analyzed subsets of data were discussed with the third, and fourth authors for validity checking (Braun & Clarke, 2013).
Results
Four themes were identified using IPA: “ambiguous loss and grief,” “protected by family members,” “secondary impacts on family unit,” and “barriers to accessing support” (see Figure 1). The themes are presented below and supported through verbatim extracts from participants’ interviews; participants are represented using pseudonyms to maintain their anonymity. For clarity, interviewed family members are referred to as “participants,” their relative with a brain tumor or stroke is referred to as “relative,” and individuals of their family unit are referred to as “family members.”
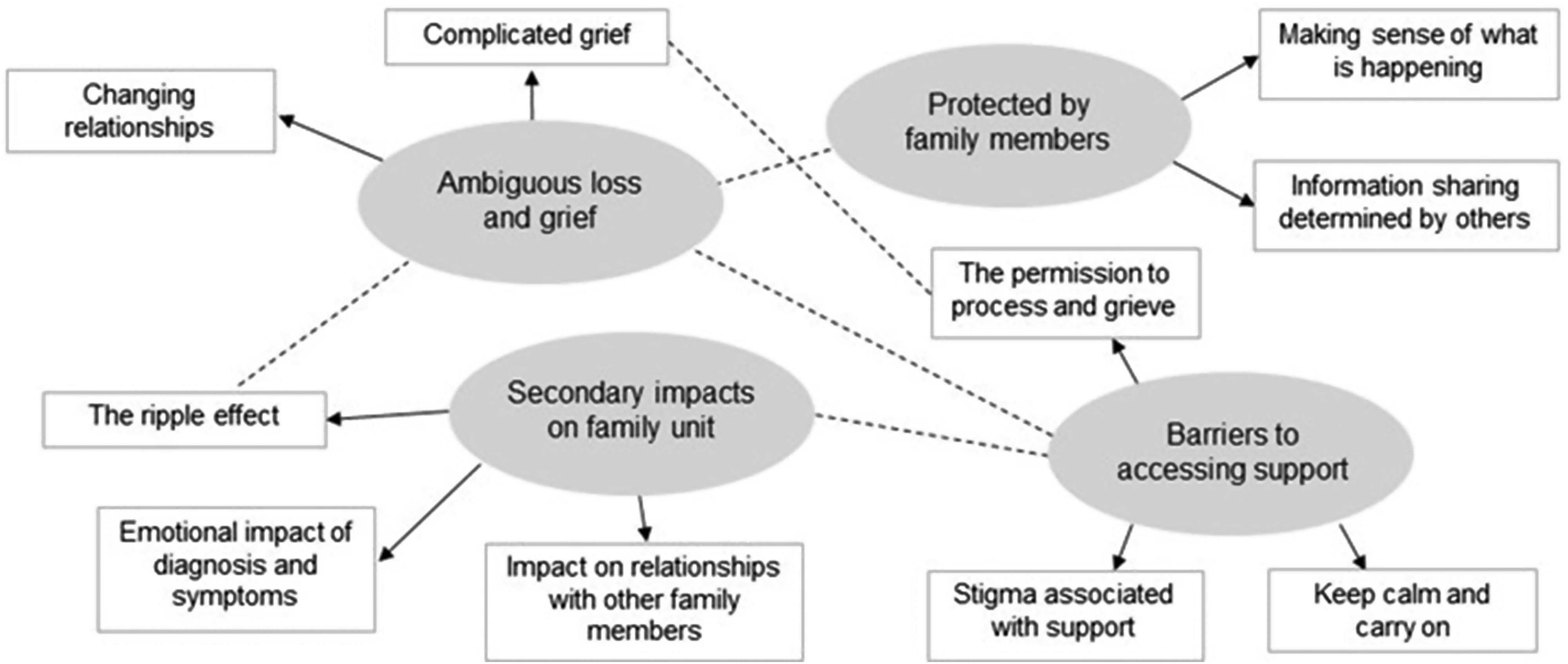
Thematic map of the data.
IPA is also about the use of language. What is noteworthy through all the themes is how the participants talk about their experiences in terms of absence, i.e., what is not communicated, shared and therefore remains unacknowledged and unsupported.
Theme 1: Ambiguous Loss and Grief
This theme captures the multitude of losses participants experienced and the emotional impact and grief participants experienced because of these changes and losses (Boss, 2007).
Participants’ relatives experienced a range of cognitive impairments, such as changes in behavior and personality. These changes resulted in participants feeling a sense of ambiguous loss, a complex grief experienced due to non-death losses. Poppy expressed a sense of grief over the psychological loss of her grandmother describing her as able to “remember everyone, and remember all situations,” but not “there … present in the moment … in her own world.” Participants frequently referred to their relative as “a different person” to express that they no longer recognized the person physically in front of them. Anna described that when visiting her grandmother, she felt “the person that I knew, wasn’t there.”
The loss of who their relative used to be was often difficult for participants to process, and adjust to. Freddie described the challenge of his grandmother being visibly unchanged whilst displaying behavioral changes of aggression and irritation: you know that that's not them. But it's them saying it, with their voice, and their face … it's quite jarring. (Freddie)
Changing Relationships
Several participants highlighted that their sense of loss of their relative impacted their shared relationship. Some participants described adjusting to their relatives’ changed identity, and adapted how they spent time together. Anna and Freddie experienced their grandmothers living with a brain tumor. They expressed how their grandmothers had been the ones to support, and take care of them during their childhood, and that relational role changed. when I was there you know I’d, I'd be the one to make the food… I’d be the one to you know make sure she'd have tablets and, being sort of the extra help…. (Anna) we did have to take more of a caring role when we were visiting … there's like a reversal of roles. (Freddie)
Complicated Grief
All participants described experiencing grief and loss. For some participants of those with brain tumors, or those who had experienced multiple strokes, these were multiple experiences of loss due to their relative's physical, and psychological symptoms progressing over time. For others, the ambiguity of their loss led them to struggle to process their grief, leading to complicated grief (Shear, 2015; Worden, 2018). I really think, I feel … my work was affected, like schoolwork it was definitely affected by the whole thing because my grades went down massively. It's just hard to focus when you're in that position. (Kate) when it happens [grandad dies], it's sort of like, great, cause I don’t have to live through it anymore. (Ben) you deal with it over time, and you start to feel a bit better, but it's never fully gone. (Freddie)
Theme 2: Protected by Family Members
This theme encompasses the impact of being “protected” by other family members while participants tried to make sense of what was happening to their relative. While this protection was meaning well in some instances it had a negative emotional impact on participants, especially in relation to the grief they were experiencing that was not often discussed with wider family members. I didn't talk to my family about stuff that I was going through, because I just felt like it affected them. So, I sort of keep it to myself sort of thing. (Laura) I really wanted to go see him but my parents were very much like, it's probably for the best that you don’t. (Laura)
Information Sharing Determined by Others
All participants were under 18 years of age at the time of their experience. Therefore, most participants relied on their parents to share information with them. Participants reported that healthcare professionals shared information with their parents, and their parents determined what was appropriate to communicate to them. Participants commonly interpreted this as their family members “protecting” them from information because of their age, and to prevent anxiety. For others this was felt to be due to existing difficult relationships within the family. medical professions were very open, like with my parents. Um, but it was very sort of swept under the rug, because of being so young. (Anna) yeah information was just always on the surface level… My family members, we don't really talk about the emotional stuff. (Nina) I think there's definitely people that need to be informed [by medical professionals] of things … rather than relying on just one person in the family. (Emma)
Making Sense of What Is Happening
All participants directly observed some of the symptoms of brain injury experienced by their relative. For many of the participants, an understanding of these symptoms and their relative's diagnosis came from other family members. When this communication was detailed, and comprehensive participants spoke of this positively and expressed it helped them to “understand” and “make sense” of what was happening. I remember them saying like ‘hey look, this is what's going on, this explains some of these things you’ve been noticing’ and we were just kind of a bit shocked, but it made sense you know, it gave a reason for a lot of what we’d been seeing. (Freddie) yeah, especially the communication, I think that was definitely important because I feel like if they didn't really tell me what was going on, I would have felt really alienated. (Kate)
Theme 3: Secondary Impact on Family Unit
This theme captures how a brain injury impacts the individual concerned whilst also, directly, and indirectly, impacting family members. This theme highlights that participants’ relationship with their unwell relative influences the challenges they experience.
Emotional Impact of Diagnosis and Symptoms
All participants shared that experiencing a relative with a brain injury directly impacted on their emotional and psychological wellbeing. Participants expressed they felt shocked and sad on hearing their relative's diagnosis whilst also experiencing fear and uncertainty for the future. Emotionally, it's … tough sometimes, like, seeing her not be able to do something, like on her own, or like not being able to understand some things. (Nina) She had a fall. She sort of fell out of bed, um she would fall down the stairs … like every week there would be a new fall, a new, sort of, like, like concern for her health. (Anna)
Impact on Relationships with Other Family Members
Most participants were not directly involved in caregiving responsibilities, but their parents were, resulting in them being less present in the family home. Participants reported their parents were not always able to balance meeting their needs at home and caregiving responsibilities. it was hard on all of us, I barely saw my Mum most evenings because of her being over there [caring for relative]. (Anna) Definitely it changed my relationship with my mum because the stress on her made it very difficult for her to like … to connect with me. (Kate)
The Ripple Effect
All participants highlighted their relative's brain injury affected many family members in many ways. Participants described how the impacts repeatedly and continually reverberated through their family system. The direct and indirect impacts participants experienced were influenced by each family members’ relational position to their unwell relative. Overall, the participants felt that as grandchildren the indirect impact of this “ripple effect” was often overlooked. This captures how a change in one part of a family system can impact so many people's lives, including wider family members through circular causality. This was particularly relevant to the experience of ambiguous loss across the whole of the family network. I know that it made me sort of have to mature at a very young age… Like every single time something happens to me now… I like to process it and … deal with it a lot a lot better. But I had to learn that far too young. (Kate) I had depression quite a lot when I was growing up for lots of different reasons, but I think a lot of it was … what had happened to sort of Granddad. (Rachel) I was just sort of made aware at a very young age about all of these sort of big adult problems. (Laura)
Barriers to Accessing Support
This theme captures participants’ support needs, and the barriers they experienced to accessing support for themselves. The barriers experienced to accessing and receiving support interconnected with participants’ ability to process their grief and exacerbated the secondary impact on wider family members. Well, so I was already going through some mental health problems at the time. So it was just sort of like another building block on that. Just added into whatever I was going through at the time. I was just keeping myself busy was the only thing I could think of to do. Nobody offered support, which probably would have helped long term. So, I was just like, well, I'll keep plodding along. And wait for it all to be over. (Laura)
The Permission to Process and Grieve
Participants were all children at the time of the onset of their relative's brain injury. Participants often looked to adult family members for cues on how to react and respond to the experience. Many participants observed their family members being irritated and frustrated instead of openly communicating and explaining their feelings of grief. Consequently, this did not “normalize” the grieving process or give participants permission to explore and process the emotional impact of the experience. This, in many instances was associated with a chaotic grief response (Haberecht & Prior, 1997) or one more closely represented by the dual process model of grieving where individual move between restoration-oriented and loss-oriented coping (Stroebe & Schut, 1999). I was just trying to stay positive and everything, but like, deep down like, I was scared and I was upset…. (Jane) for a long time I just felt like I switched my emotions off (Emma) It created kind of like a weird situation because everyone was thinking about it in their heads, but they weren't really saying it out loud, so it was a bit of a weird situation at home. (Poppy) I think more one-on-one support … to have like, someone that I could talk to that wasn't my family, that had sort of no involvement, had no idea what was going on, that I could just talk to about how I felt. (Anna)
Keep Calm and Carry on
Participants described the challenges of finding the time, and space to pause, and process their experience whilst it was occurring. Their relative's brain injury often led to a sudden onset of treatments and input from numerous health and social care services. This left little space for reflection and processing. it was difficult to know when we would need the support … because when it is happening you know, it's normal, it becomes the normal…. (Anna) like there are times, where you have to pull all your emotions to one side. (Jane) yeah, there was a lot of like grief involved. A lot of sort of untreated like grief generally I mean and it was just sort of a keep calm and carry on sort of attitude. (Rachel)
Stigma Associated with Support
All participants experienced emotional and psychological distress because of their relative's brain injury. When reflecting on their experience, many participants felt they would have benefitted from information about available services and how to access them. Yet when directly asked what may have helped with their experience, many participants admitted that they or their families would have been unlikely to seek support. This contradiction highlights a difference between participants perceived and actual support needs, representing a potential personal stigma toward needing support. Participants’ perspectives on accessing support for themselves were influenced by other family members’ views on support and openness to discussing feelings. Unfortunately, many participants described their family members expressed stigma regarding mental health. I think there's a strong stigma in my family when it comes to anything “support”, that has a strong stigma attached to it because that to them, is mental health support, and “we don't have mental health.” (Rachel) There was no sort of grieving support or anything and I think I really think that everyone should have had some sort of grieving support, uhm, just purely on the basis that, like like I said, we come from a family where we just don't handle emotions well, very stiff upper lip you know? (Ben)
Discussion
This study aimed to explore the lived experiences of extended family members with a brain injury caused by tumor or stroke, gaining an insight into grandchildren's perspectives on the significant challenges they experience. Family members’ accounts highlighted the broad impacts they experienced at different points during, and after their relative's injury, contributing to our understanding of the wider family impact.
Participants experienced multiple and significant losses because of their relative's brain injury. The ambiguity of the loss of family members experienced due to the changes in their identity post-injury is consistent with wider ABI literature (Townshend & Norman, 2018). Holloway et al. (2019) highlighted how ambiguous loss complicates family members’ grief as they process the psychological loss of their relative as they once were, whilst they are still physically present. Participants expressed that their relative's symptoms had varying impacts on their relationship. Participants identified their relative's cognitive symptoms, and changes in personality as the primary cause of their strained relationship (Ownsworth et al., 2015).
Participants whose relatives were diagnosed with a malignant brain tumor experienced an accumulation of losses as their relative's symptoms progressed. They faced an extremely challenging time as they simultaneously experienced the neurocognitive changes of an ABI, and the deterioration of their relative from a life-limiting condition. Participants described a continuous sense of loss as they experienced anticipatory grief (Rando, 2000) for the bereavement of their relative. Family members experiencing high levels of pre-bereavement losses are at a higher risk of experiencing prolonged and complicated grief post-bereavement (Treml et al., 2021). Bereavement-related feelings of relief on the death of a loved one are rarely identified in caregiving literature (Allen et al., 2021).
Most participants were under 18 at the time of their experience; therefore, they did not directly communicate with healthcare professionals and relied on their parents for information. Many participants highlighted receiving inadequate information about their relative's diagnosis, symptoms, and prognosis. Several authors have highlighted the unmet informational needs of primary caregivers (Arber et al., 2012; Papadakos et al., 2019); the results from this study expand on those findings by identifying the unmet information needs of the wider family unit. This finding potentially highlights that the unmet information needs of primary caregivers have a knock-on effect on their ability to disseminate information adequately to the extended family.
Participants perceived that, at times, their family members were “protecting” them from the reality of their relatives’ condition by limiting the information shared. However, observing symptoms, and not having access to adequate explanations led to participants feeling worried, confused, and distressed. Participants felt a lack of control over their situation due to this limited information sharing. Weber et al. (2019) highlighted the positive impact effective, and open communication has on a child's ability to process and adjust to a relative's illness. Receiving inadequate information about a relative's illness and not being prepared for a deterioration in their condition have been identified as risk factors for experiencing complicated grief (Mason et al., 2020).
The burden and emotional impact of caregiving responsibilities are widely recognized in the ABI literature (Baker et al., 2017; Tramonti et al., 2019). Many participants’ parents undertook informal caregiving responsibilities for their relatives and experienced challenges balancing conflicting demands. This study shed light on the toll of parents being primary caregivers, inevitably affecting their role as parents with a detrimental impact on their children, and the wider family as a whole. Participants highlighted how their relative's diagnosis and symptoms had a continual ripple effect that reverberated through their family system. This finding is consistent with wider ABI literature, which emphasizes the broad impacts one event can have on many lives (Townshend & Norman, 2018).
Previous research highlights the challenges family members experience as they adjust to a new role while processing the loss associated with their relative's illness (Piil et al., 2015). Participants recognized their family members were experiencing an emotional response to grief, but this grief was often unacknowledged. Dyregrov (2008) highlighted the importance of recognizing and validating children's feelings, as it can support their grieving process. Participants highlighted the accumulation of traumatic losses combined with a rapidly deteriorating situation made it challenging for family members to have the space to process their experience. Previous research has identified family members are at risk of experiencing post-traumatic stress symptoms due to the accumulation of losses they experience during their relative's illness (Kim et al., 2017; Kristensen et al., 2012).
Consistent with previous literature findings, participants received inadequate information about available support services, and how to access them (Arber et al., 2012; Cornwell et al., 2012). However, there was ambiguity about whether support, and signposting were not offered or whether other family members did not communicate information about support to the grandchildren. Systemic and societal stigma toward mental health are also well-recognized barriers to accessing psychological support (Cage et al., 2020; Salaheddin & Mason, 2016). This may be particularly important in the case of ambiguous loss, where grief processes may not be acknowledged due to the absence of the loss of the physical person.
An interesting aspect of the findings in the absence expressed by the participants in many different domains. As noted at the end of the results section, participants referred to their parents being absent, as well as their grandparents, due to changes in who they were as a person. They also noted an absence of communication and support which ultimately led to them struggling to make sense of their own thoughts and emotions. For some this absence left scars into adulthood that were still in need of healing at the time of interview. It is interesting seeing something described almost exclusively in terms of what was not present in their lives at the time and may help to explain why participants in this study expressed great interest in being interviewed as for many it was the first time their experiences had truly been acknowledged.
The findings from this study demonstrate an interconnectedness between unmet information needs, and family members’ ability to process loss and grief. Family members are at a higher risk of experiencing complicated grief due to the multitude of losses that accumulate during their relative's illness. This risk was exacerbated by participants’ unmet information needs, and inadequate communication within the family. Participants highlighted open communication within the family unit would have helped them make sense of their relative's illness. Further, communication would have helped prepare family members for the symptoms and deterioration their relatives experienced. The findings from this study identify a need for healthcare professionals to ensure immediate family members’ information needs are met, and that they receive support to disseminate information. Immediate family members would potentially benefit from support and guidance on how and what to communicate to the wider family unit, particularly when determining age-appropriate information for a child.
Strengths and Limitations
The sample size is appropriate for an IPA study; however, further research would be beneficial to explore whether the findings are reflected in the wider population.
This study aimed to gain insight into family members’ experiences with health and social care services. Due to participants’ relation to their relatives and age at the time of their experience, they offered limited accounts of experiences with healthcare services. However, the sample demographics provided a unique perspective of wider family members’ experiences, which is rarely prevalent in ABI literature. This study presents robust, detailed, and rich findings on family members’ experiences. Further study is needed, however, to understand the lived experiences of grandchildren from more diverse backgrounds given that the population of this study were solely White British and therefore provide no understanding of the impact of cultural diversity. Cultural differences across families may lead to fundamentally different narratives and ways in which families function as a unit following stroke or brain tumor.
It is also important to highlight that due to the retrospective nature of this study, participant accounts are all data collection based on re-remembering of previous lived experiences. This may lead to inaccuracies in the narrative provided by participants.
Study Implications
Further large-scale studies are needed to better understand the ripple effects of brain injury across the whole family as well as the impact on family dynamics. Caregiving responsibilities following ABI are complex for all family members and it is important that clinicians consider the needs of those within the family who are not directly responsible for caregiving or who are less immediately involved with the person with ABI in the future.
Previous research has found that compassion-focused therapy and acceptance and commitment therapy have been effective psychological interventions following grief (Harris, 2021; Speedlin et al., 2016). Therefore, future research could explore whether these psychological interventions are effective in supporting family members and reducing their risk of experiencing complicated grief. Systemic models of practice are also likely to be helpful. Specifically, narrative therapy in externalizing brain injury as a separate entity rather than defining the grandparent by the impacts that they have experienced (White & Epston, 1990). Considering the entire family system is likely to reduce feelings of guilt and resentment, construct new understandings, and strengthen family resilience (Launer, 2018).
Conclusion
This study extends ABI research by exploring the lived experiences of grandchildren, a group largely overlooked in existing literature. Consistent with family systems and ambiguous loss frameworks, the findings show that stroke and brain tumor have enduring ripple effects across the wider family, shaping relationships, communication, and emotional wellbeing. Participants described profound experiences of ambiguous loss and grief linked to changes in their grandparents’ identity, alongside secondary impacts such as disrupted family roles and reduced parental availability. Efforts to protect children through restricted communication often increased confusion, isolation, and distress, limiting participants’ ability to make sense of their experiences. Barriers to accessing support, including inadequate signposting and stigma surrounding mental health, further compounded these difficulties, with grief frequently deferred into adulthood. Overall, the findings highlight the need for systemic approaches to ABI care that recognizes and supports the wider family network. Improving age-appropriate communication and access to psychological support may help mitigate the long-term impact of ambiguous loss and unprocessed grief across generations.
Footnotes
Acknowledgments
We would like to express our gratitude to all the participants who gave up their valuable time to contribute to this research.
Ethical Approval
Ethics was sought and received through the University of Plymouth, School of Psychology ethics committee.
Informed Consent
All participants were provided with an information sheet and gave their informed consent to take part.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability
Due to the sensitive nature of the data, this is available in an anonymized form on request from the corresponding author.
