Abstract
Objective
Anterior craniofacial changes in unilateral lambdoid craniosynostosis include forehead bossing, increased orbital heights, and asymmetry of the midface and mandible, creating a facial twist. The purpose of this study is to comprehensively analyze the post-operative anterior craniofacial changes in patients with unilateral lambdoid craniosynostosis following occipital switch cranioplasty.
Design
Retrospective review of three-dimensional images collected pre-operatively and post-operatively around 2 years.
Setting
Tertiary care pediatric institution.
Participants
Eighteen patients with unilateral lambdoid craniosynostosis.
Interventions
Cranial vault remodeling with occipital switch cranioplasty.
Main Outcome Measures
Frontal, occipital, height, midface, ear, and orbital asymmetry. Nasal and chin deviation.
Results
Frontal and occipital asymmetry significantly improved post-operatively (P = .03; P < .01). Cranial height asymmetry and midface projection asymmetry did not significantly improve (P = .24; P = .59). The nasal deviation was, on average, 3.58 ± 1.69° prior to surgery and significantly improved with a residual deviation of 2.18 ± 1.35° (P = .01). The chin deviation significantly improved post-operatively from an average of 2.21 ± 1.52° to a residual deviation of 1.07 ± 1.12° (P = .04). Ear asymmetry, orbital width, and orbital height asymmetry did not significantly change with surgery.
Conclusions
Two years after occipital switch cranioplasty, patients with unilateral lambdoid craniosynostosis had significant improvements in frontal asymmetry, nasal deviation, and chin deviation. However, nasal and chin deviation remained residually asymmetric. Midface projection contralateral deficiency did not significantly change post-operatively over the study period. The release of the affected suture with occipital switch cranioplasty allowed for remodeling and growth to improve anterior craniofacial symmetry.
Keywords
Introduction
Unilateral lambdoid craniosynostosis (ULC) leads to early suture fusion, restricting growth and causing cranial asymmetry.1–4 The affected occiput is flattened, with parietal and mastoid bulging and contralateral occipital bossing.1–4 The posterior cranial base is canted downward on the ipsilateral side with asymmetrical expansion of the contralateral middle and posterior fossa.3–7 The ear position is altered, but variation exists in reported directionality.2,4,6,8,9 These changes in the cranial base are believed to be the driving force leading to anterior craniofacial changes.4,6,7,10 These anterior deformations have recently been demonstrated in patients with ULC.1,6,10–15 There is a bilateral expansion of the anterior cranial fossa with frontal bossing.1,6,14 Orbital depths are decreased with increasing heights bilaterally.14,15 The contralateral maxilla is expanded with posterior deviation of the mandibular articular fossa.6,10–15 The midface and mandibular alterations create a facial “twist” in which the chin and nasal root are deviated to the contralateral side.1,6,10–15
Surgical intervention in ULC is indicated to prevent elevated intracranial pressure, improve neurocognitive outcomes, address Chiari malformation, and improve cranial shape.16–20 Persistent asymmetry in the cranial vault and facial skeleton has been shown in untreated patients. 1 Current interventions for ULC include traditional cranial vault remodeling with full cranial release or suturectomy that involves release of the lambdoid suture with adjunct molding helmet, distraction, or springs.1,3,4,6,7,21–41
However, these techniques focus on the posterior cranium and do not involve direct intervention to the cranial base or anterior craniofacial region. Clinical observations have shown that the contralateral hemifacial deficiencies only partially resolved following occipital switch cranioplasty.1,7 Nguyen et al reported that facial twist remained following surgical intervention but had partially improved by 2 years post-operatively. 3 These changes are believed to occur following growth after the release of the constricting suture. However, an extensive quantitative evaluation of these changes has yet to be performed. The purpose of this study is to comprehensively analyze anterior craniofacial changes that occur following occipital switch cranioplasty in ULC.
Methods
A retrospective review was conducted on patients with ULC who underwent posterior cranial vault remodeling with switch cranioplasty from both centers, following institutional review board approval by the University of Texas Southwestern Medical Center and share agreement with Wake Forest University. The diagnoses of all patients were confirmed using pre-operative computed tomography (CT) scans. All patients who underwent posterior cranial vault remodeling with occipital switch cranioplasty and had three-dimensional (3D) images obtained pre-operatively and around 2 years post-operatively were included. No included patients had previous operative intervention, genetically identified syndromic craniosynostosis, or other congenital or acquired craniofacial pathology. Three-dimensional (3D) images were analyzed using the 3dMD imaging system (3dMD, Atlanta, GA).
Surgical Technique
All patients underwent occipital switch cranioplasty using the same technique. A bi-coronal flap was raised posteriorly to the torcula before transitioning into a subperiosteal plane carried to the inferior aspect of the occipital constriction. The occipital flaps were marked below the torcula, and the occipital flaps were removed as a single piece. The occipital flap was then rotated 180° so that the anterior articulation became its posterior articulation. The flaps were secured with a combination of suture placement and resorbable plates.
Data Analysis
Radial measurement ratios were utilized to evaluate asymmetry in the frontal, occipital, and cranial heights of the calvarium and midface registered in the Frankfort horizontal (Figure 1). For each ratio measurement, a plane was chosen. For the frontal and the occipital asymmetry ratios, an axial plane 2 cm above the supraorbital rim was defined, as measured on the 3dMD system using the caliper tool (Figure 1A). For the cranial height asymmetry ratio, a coronal plane aligned with the highest point of the superior helical rim was defined to determine differences in cranial height between the ipsilateral and contralateral sides (Figure 1B). For the midface projection asymmetry ratio, an axial plane at the level of the nasal alar base was used to determine differences in midface projection between the ipsilateral and contralateral sides (Figure 1C). The asymmetry was measured as the ratio of the Euclidian distance from the midpoint to the head surface at 30° from the midline bilaterally on the same plane. The contralateral distance was divided by the ipsilateral distance to calculate asymmetry, such that bossing was indicated by ratios greater than 1.0.
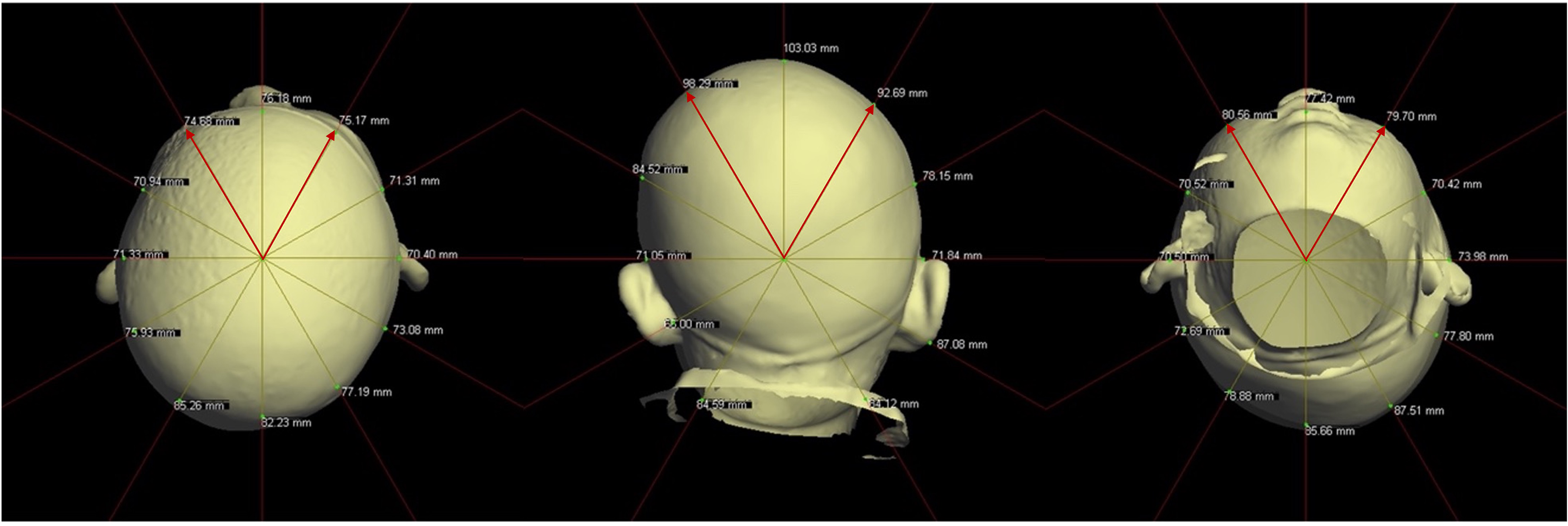
Anterior and posterior calvarium asymmetry (left), height asymmetry (middle), and midface projection asymmetry (right). The asymmetry is measured as the ratio between the ipsilateral and contralateral sides measured at 30° from the midline.
Ear position asymmetry was measured as the difference between the ipsilateral and contralateral sides in the angle created from the horizontal line extending from the lateral canthus to the position of the tragus (Figure 2A). The nasal and chin deviation, that is, the degree of “facial twist,” was measured as the angle from the midline to the nasal tip (Figure 2B) and chin point (Figure 2C). Orbital height and width were measured, and asymmetry was calculated as contralateral divided by ipsilateral distance. Two authors (LMH, KP) each completed all measurements, and averages of each measurement were used for analysis. Interrater reliability by Lin's concordance correlation coefficient showed 0.98, indicating strength of agreement. Statistical analysis was performed to calculate totals, percentages, and averages with standard deviation. Two-sample T-tests compared pre-operative and post-operative asymmetry with a P-value of .05.

Ear position asymmetry (left) was measured as the difference between the ipsilateral and contralateral sides of the angle between a horizontal line extending from the lateral canthus and the position of the tragus. Nasal asymmetry (middle) and chin asymmetry (right) were measured as the angle between the midline and nasal tip or chin point.
Results
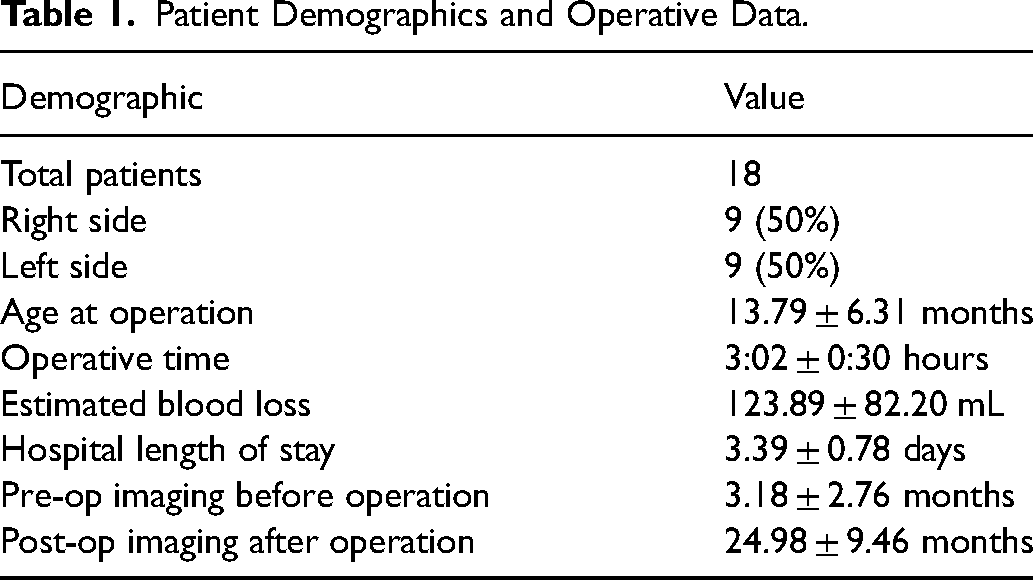
A total of 18 patients with ULC who underwent occipital switch cranioplasty were analyzed (Table 1). Eleven patients were treated at the University of Texas Southwestern Medical Center, and 7 were treated at Wake Forest University. The laterality of the affected suture was equal between the sides. The average age of surgical intervention was on average 13.8 ± 6.3 months of age and operative time was around 3 hours. Estimated blood loss on average was 123.9 ± 82.2 mL, and patients remained in the hospital for around 3 days post-operatively. Pre-operative images were, on average, 3 months prior to surgery and post-operative imaging was, on average, at over 2 years.
Patient Demographics and Operative Data.

The contralateral forehead was, on average, 98% of the projection on the ipsilateral side. Post-operatively, this asymmetry significantly improved (P = .03) (Table 2). On average, the contralateral posterior occiput was increased by 10% compared to the projection of the ipsilateral side, and asymmetry significantly improved post-operatively (P < .01). The height asymmetry showed an increased contralateral height of 6%, which did not significantly improve post-operatively (P = .24). The contralateral midface projection was 97% of the ipsilateral side, and it did not significantly improve by 2 years post-operatively (P = .59).
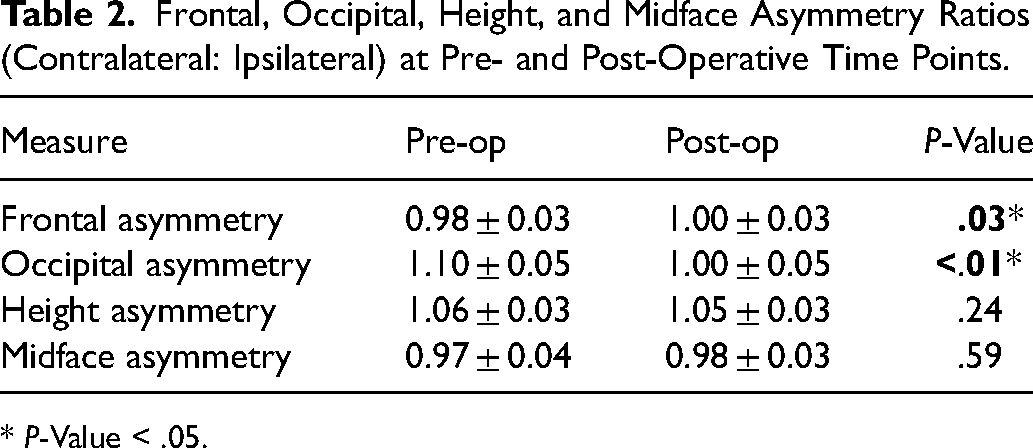
Frontal, Occipital, Height, and Midface Asymmetry Ratios (Contralateral: Ipsilateral) at Pre- and Post-Operative Time Points.
* P-Value < .05.
The pre-operative frontal asymmetry ratio was 0.98, significantly improving to 1.00 post-operatively (P = .03). The occipital asymmetry ratio was 1.10 pre-operatively, indicating 10% contralateral bossing, and significantly improved to 1.00 post-operatively (P < .01). The cranial height asymmetry ratio was 1.06 pre-operatively and did not improve post-operatively at 1.05 (P = .24). The midface projection asymmetry ratio was 0.97 pre-operatively and 0.98 post-operatively, showing no improvement (P = .59) (Table 2). All patients demonstrated improvements in all asymmetry ratios.
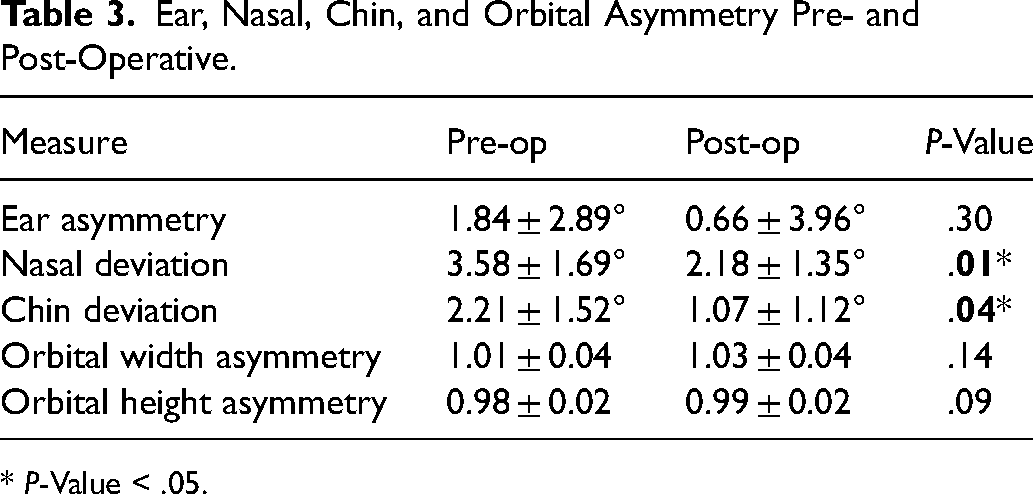
The ear position was similar between the sides and did not significantly change following surgery (P = .30). Nasal deviation was, on average, 3.58° towards the contralateral side. At two years post-operatively, the nasal deviation significantly improved (P = .01), but a residual average deviation of 2.18° remained. Similarly, chin deviation was 2.21° to the contralateral side and significantly improved to 1.07° after surgery (P = .04). Orbital width and height had minimal asymmetry with no significant change post-operatively. (Table 3)
Ear, Nasal, Chin, and Orbital Asymmetry Pre- and Post-Operative.
* P-Value < .05.
Discussion
The premature fusion of the lambdoid suture results in deformational alterations in both the calvarium and cranial base. The calvaria changes are well-defined and include occipital flattening, parietal bossing, and contralateral occipital bossing.1–4 In the cranial base, the posterior fossa deviates toward the affected suture, enlarging the contralateral posterior and middle cranial fossa, while the anterior cranial fossa has bilateral symmetrical enlargement.3–7 The occipitomastoid prominence creates further alterations by forming a posterior twist of the cranial base.3–7
These cranial base alterations are believed to be intrinsically related to changes in facial features.4,6,7,10 There is variability in the severity of the affected facial features, which appears to be dependent on the degree of cranial base deviation.4,6,10 The contralateral middle fossa's expansion displaces the mandible's glenoid fossa posteriorly, the altered biomechanical forces are believed to cause abnormal mandibular growth which can lead to a compensatory increase in body length.1,6,10–12 The abnormal development of the mandible is thought to secondarily create alterations to the maxilla. The zygoma is also said to be a driver transmitting distorting force from the middle fossa to the midface.12,13 The dysmorphology of the mandible and maxilla leads to changes in the chin and nasal deviation, creating a facial twist.3,4,14,15
The expansion of the bilateral anterior cranial fossa is theorized to be compensatory due to the posterior fossa restriction.3,7,13,42 A vertical expansion of the anterior fossa also leads to increased orbital peaking and occasionally turricephaly.14,15,42 In addition, bossing of the frontal bone can be seen on either side, with the contralateral side being a feature of the classically described “trapezoidal” head shape.2,13,14,43–45
These anterior craniofacial features were again seen in our patient cohort prior to surgery, both clinically and on imaging analysis. While the forehead asymmetry was significantly different, the absolute difference was minimal, and no persistent pattern was seen in the laterality of increased frontal bossing. However, the ipsilateral forehead had increased bossing in 84% of the patients. Consistent with previous studies, the contralateral midface projection showed retrusion compared to the ipsilateral side, which created the appearance of a hemifacial deficiency. Both nasal and chin deviation were demonstrated toward the contralateral side, creating the appearance of a facial twist. The orbits were shown to be similar in both height and width.
Multiple operative interventions are currently available for ULC, including cranial vault remodeling and strip craniectomy, with or without springs or distraction osteogenesis devices.1,3,7,20–27,29–40,43,46–51 It is interesting to consider that no matter which surgical intervention is chosen, be it strip craniectomy or an open calvarial vault reconstruction such as that evaluated here, the constricting lambdoid suture is usually incompletely altered. Possibly due to hesitation to completely remove or alter the lambdoid suture to the level of the mastoid bulge. In the current study, we utilized an open occipital switch cranioplasty technique. Two years after surgery, the frontal symmetry ratio significantly improved. The nasal and chin deviation significantly decreased, but a slight residual asymmetry remained at the time of follow-up. However, both values fell within normal limits of deviation of fewer than 5° in nasal deviation and 2° to 4° in chin deviation.52–54 The contralateral midface projection deficiency did not significantly resolve following surgery. The orbital dimensions also remained consistent without significant change. Although posterior switch cranioplasty does not directly impact the anterior cranial vault or cranial base, the release of the suture allowed for remodeling and growth to improve anterior craniofacial symmetry.
The posterior switch cranioplasty was previously evaluated by Smartt et al, who in a review of six patients, found that hemifacial deficiency was not completely resolved at long-term follow-up. 1 These findings are supported by Elliott et al, who found that there were no significant alterations to the cranial base following cranioplasty and persistent hemifacial deficiency. 7 Although improvements were seen in first 2 years following occipital switch cranioplasty, a similar residual hemifacial deficiency remained in our patient cohort. Cranial vault remodeling techniques do not directly address the asymmetry of the cranial base; thus, they do not change the believed driving force for anterior craniofacial changes. 7 Possibly because the entire fused lambdoid suture and extension are not removed. Zubovic et al showed that cranial base and posterior cranial vault asymmetry in ULC persists despite cranial vault remodeling or strip craniectomy with molding helmet. 24
Our study shows improvement, but incomplete correction of the asymmetries found in ULC when employing the occipital switch procedure. However, it also seems to be true that other techniques do not result in the complete restoration of symmetry. This certainly could be that the entire lambdoid suture is incompletely released inferiorly. Neurosurgeons may be wary about the risks inherent in extending craniotomy or craniectomy to the full extent of the lambdoid suture. This also may result from the definition of ULC. Formal anatomic nomenclature states that the lambdoid suture extends between the parietal and occipital bones and terminates at the junction of the occipital bone and mastoid portion of the temporal bone. The lambdoid suture is continuous with the occipitomastoid suture and the occipitoparietal suture. One of the prominent clinical hallmarks of ULC is a significant mastoid bulge. It is worth positing the question that perhaps the entity that is referred to as ULC is not simply lambdoid suture synostosis but perhaps is associated and linked with sutural synostosis or other abnormalities of the occipitomastoid and occipitoparietal sutures. Indeed, no conventional surgical technique to treat ULC addresses these sutures directly, and this may result in incomplete correction or persistence of the mastoid bulge that is often seen with this diagnosis.
In contrast, Nguyen et al reported that although the cranial base twist does not normalize, the facial twist relatively improved but did not reach normal by 2 years following posterior switch cranioplasty. 3 The facial twist immediately post-operatively showed no improvement compared to controls, indicating growth and remodeling in the anterior craniofacial features occurs over time. However, the partial normalization was partly due to increased twist in control cases. 3 In the current study, we also found significant improvements in nasal and chin deviation, leading to improvements in facial twist but with some residual deviation remaining.
The use of springs and distraction osteogenesis has been demonstrated as a viable operative option for ULC.26,33–41 The persistent and progressive tensile strength applied through springs or distraction osteogenesis allows for alterations in skull base angulation.26,40,41 Improvements in cranial base asymmetry was shown by Mittermiller et al, following spring-mediated distraction. 26 Post-operatively there was decreased discrepancy between petrous ridge and the cranial base angles. Aligning with these findings, Mellgren et al found significant change in middle and posterior cranial twist following spring-assisted surgery in six patients with ULC. 40 Further studies are needed to evaluate the comprehensive facial changes seen following spring and distraction osteogenesis in ULC.
ULC patients commonly present later due to similarities with deformational plagiocephaly. Over time, patients who do not receive operative intervention for ULC develop more pronounced and severe facial twist. 1 Goodrich et al previously suggested that most facial twist was corrected in patients who underwent cranial vault remolding before 1 year of age. 48 In our study, patients were, on average, over 1 year of age, possibly limiting the correction seen in the anterior craniofacial features. Additional benefits may be seen at an earlier age of operative intervention; however, it must be balanced against the potential for decreased post-operative growth. Fearon et al reported diminished growth in both head circumference and cranial breath following surgery in a patient with ULC. 50
The sample size of 18 patients is a limitation of our study. However, due to the rarity of the pathology, the cohort is relatively sizable, and valuable insight can still be garnered from our findings. Additionally, the statistical power remains limited due to the cohort size. The age range of the patients in the cohort requires the reliance on angular measurements for cohesive data collection. Another limitation is that the follow-up was around 2 years post-operatively. Continued growth will occur over time, and future studies should be conducted at skeletal maturity.
Conclusions
The anterior craniofacial malformations in ULC were shown to resolve partially by 2 years following occipital switch cranioplasty. The frontal asymmetry, nasal, and chin deviation significantly improved following surgery. The contralateral midface projection deficiency remained. As did residual nasal and chin deviation. However, these values fell within accepted normal limits. Although no direct intervention occurred to the anterior cranial vault or cranial base, the release of the affected suture allowed for remodeling and growth to improve anterior craniofacial symmetry.
Footnotes
Acknowledgments
This work was presented at the Texas Society of Plastic Surgeons 2024 Annual Meeting.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
