Abstract
Implementing early mobilization protocols can improve patient outcomes and accelerate postoperative recovery. This pre-test and posttest randomized controlled experimental study aims to evaluate the effects of early mobilization training on mobility, pain, comfort, and sleep quality in patients undergoing laparoscopic abdominal surgery. The study was conducted at a state hospital in Northern Cyprus between June and October 2022, and participant recruitment and follow-up were reported using the CONSORT 2010 flow diagram. The sample of the study comprised 78 abdominal surgery patients who were equally assigned to the intervention (n = 39) and control groups (n = 39). Perioperative information form and patient mobility scale were used for data collection. The mean ages of the intervention and control groups were 44.82 ± 12.37 and 44.41 ± 10.80 years, respectively. The total duration of mobilization in the intervention group (58.33 ± 11.20 min) was significantly higher than that of the control group (24.92 ± 5.64 min). Postoperative pain scores of the intervention group were significantly lower than those of the control group. Comfort and sleep quality scores of the intervention group were significantly higher than those of the control group. Finally, the length of hospital stay in the intervention group was significantly lower than that of the control group. The findings of this study imply that early mobilization training had a positive impact on reducing postoperative pain and increasing the duration of mobilization, comfort while turning in bed, and lying and the quality of sleep on the first postoperative day. This study provides practical insights for enhancing comfort, mobility, pain management, and sleep quality, while addressing a key gap in the literature and contributing to evidence-based clinical practice.
Introduction
Enhanced recovery after surgery (ERAS) refers to a patient-centered, multimodal perioperative care programs that include evidence-based interventions to optimize postoperative outcomes, leading to improved clinical outcomes such as reduced length of hospital stay and lower complication rates (Boerrigter et al., 2022; Kannan et al.,2025). Early mobilization is one of the fundamental elements of postoperative ERAS protocols (Wael et al., 2025). The ERAS protocol recommends a care plan that encourages patients to be out of bed for 2 hr on the day of surgery; these recommendations are not always effectively implemented in practice, and patients often lack structured education about mobilization strategies (Tazreean et al., 2021). Prolonged bed rest can have adverse effects, including increased insulin resistance and muscle loss, decreased muscle strength, pulmonary function, tissue oxygenation, and an increased risk of thromboembolism (Gustafsson et al., 2019). Conversely, early mobilization improves patient outcomes by preventing these complications and improving recovery outcomes (Fang et al., 2021; Koyuncu & Iyigun, 2022). However, current evidence is limited regarding the effectiveness of early mobilization training for pain control, comfort, and sleep quality in laparoscopic abdominal surgery patients. This study aims to address this gap by evaluating the effects of a structured early mobilization training program on mobility, pain, comfort, and sleep quality in patients undergoing abdominal surgery.
Effective pain management is crucial for accelerating postoperative recovery. Adequate analgesia enhances the quality of recovery and is associated with increased mobilization and a reduction in postoperative complications, emphasizing the importance of effective pain management in accelerating recovery (Rivas et al., 2022). A previous study reported that knowledge about early mobilization reduced the severity of pain after laparotomy (Widayati et al., 2022). Conversely, poor management of postoperative pain reduces patient comfort, which is an outcome of nursing care and an indicator of the quality of care (Rivas et al., 2022; Widayati et al., 2022).
Postoperative patient comfort is influenced by pain and factors associated with pain. The severity of postoperative pain, the presence of drains, and the restriction of movement may negatively impact sleep quality after abdominal surgery (Ni et al., 2022). Inadequate or disturbed sleep in the postoperative period is associated with increased postoperative pain, emotional stress, and delayed recovery, emphasizing the importance of addressing sleep quality in surgical patients (Ayenew et al., 2025; Guo et al., 2025; Ni et al., 2022). Sleep is essential for biological functions and plays a critical role in the postoperative recovery process. Improving sleep quality may also reduce the need for analgesics (Ni et al., 2022).
While early mobilization is an important component of ERAS programs, there are limited studies investigating the effects of early mobilization training on pain control, patient comfort, and sleep quality together. A study has shown that early mobilization reduces pain levels and improves the quality of recovery in laparoscopic cholecystectomy patients (Okcul & Oral, 2023). In a systematic review, it was stated that after abdominal surgery, pain scores in early mobilization groups were significantly lower and sleep times were longer than in control groups (Willner, 2023). Considering the importance of this topic and the need for further research, this study was conducted to analyze the effects of early mobilization training on postoperative pain, mobility, sleep quality, and patient comfort in abdominal surgery patients. The findings of this study may provide data to develop postoperative care guidelines that include early mobilization, which can be effective in improving mobility and patient comfort after abdominal surgery. The hypotheses of the study are as follows:
Method
Study Design and Setting
This study employed a randomized pretest-posttest control group experimental design. It is presented in accordance with the CONSORT 2010 statement, see Supplemental File 1. It was conducted in the surgical ward of a state hospital in Northern Cyprus between June and October 2022.
Sampling
The sample size of the study, the significance level of the hypothesis, and the effect size were determined using the statistical power analysis method via the G*Power (Version 3.1.9.2; Heinrich Heine University Düsseldorf, Düsseldorf, Germany) software. Based on the assumptions of a 95% confidence level (α = .05), 80% statistical power (1–β = .80), and a medium effect size of 0.50, the minimum required sample size was calculated as 66 participants, with 33 individuals in each group. To account for possible data loss or participant withdrawal, the sample size was increased by approximately 15%, resulting in a total of 78 patients (Figure 1). A convenience sampling method was used to recruit voluntary patients aged 18 years and over. Patients who declined participation or who underwent emergency laparoscopic abdominal surgery were excluded from the study. The inclusion criteria were as follows: patients aged 18 years and older who underwent laparoscopic abdominal surgery and were able to read, write, and understand Turkish and comply with the study procedures.
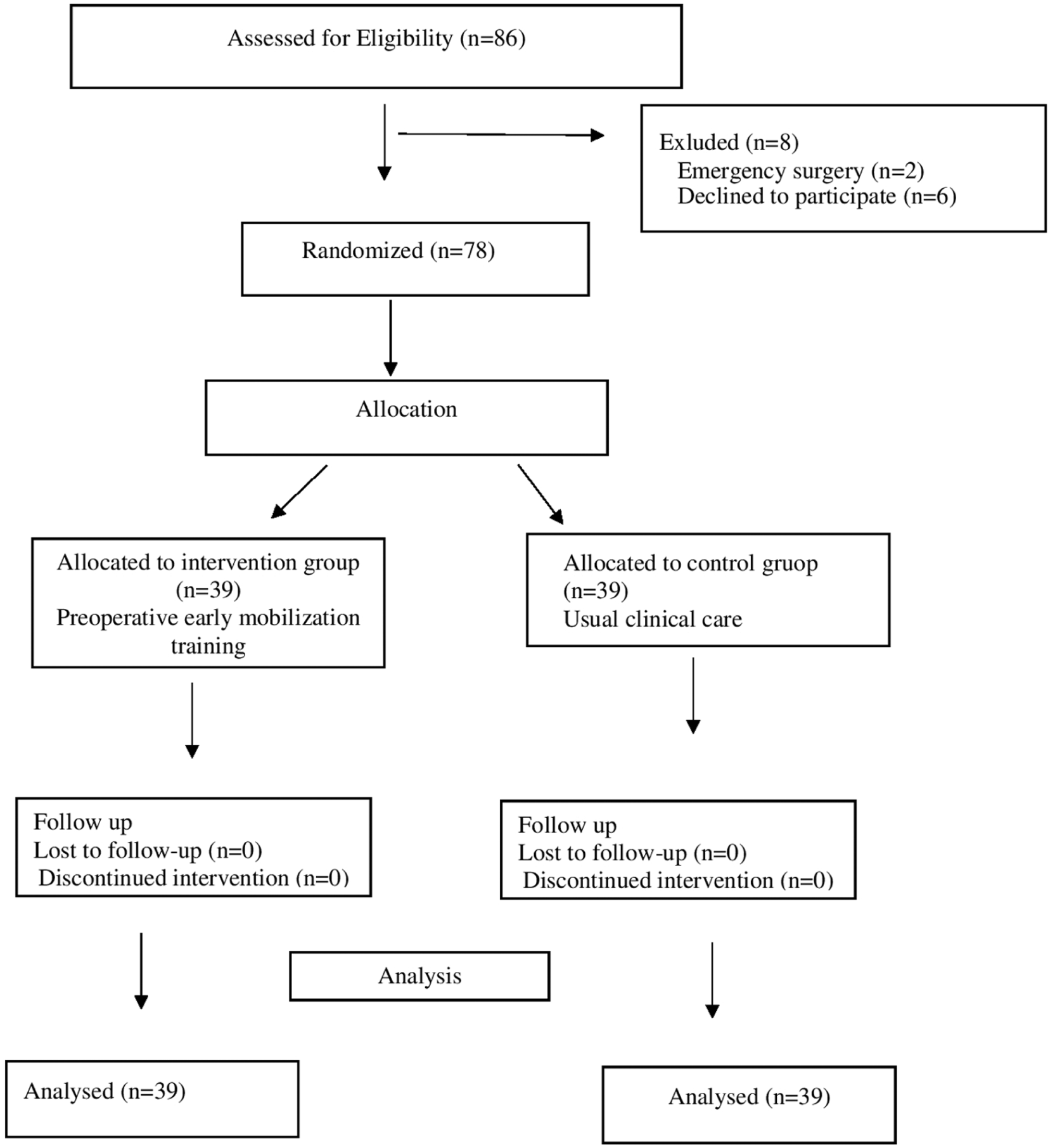
CONSORT 2010 flow diagram of the study participants.
Randomization
Participants were randomized into control and intervention groups using Random Allocation Software (Random Alloc, Ver. 1.0.0, M. Saghaei, Dept of Anesthesia, Isfahan University, Iran). The control group (n = 39) received routine clinical care while the intervention group (n = 39) received preoperative training on early mobilization.
Blinding
In this study, the researchers were aware of the intervention and control group assignments during the data collection process. Similarly, participants in both groups were informed about the purpose of the study. Therefore, neither participant nor researcher blinding was implemented as the intervention involved preoperative early mobilization training that required direct, face-to-face interaction between the researcher and the participants. However, the statistical analyses were conducted by an independent statistician who was blinded to group allocation. Thus, statistical blinding was ensured during the data analysis phase.
Data Collection Tools
Data collection was done using an information form and the Patient Mobility Scale (PMS).
Information Form
This form included questions on demographic characteristics (age, body mass index, gender, marital status, education level, smoking habits) and clinical characteristics (type of surgery, chronic diseases, presence of drain) (Daryani et al., 2023; Koyuncu & Iyigun, 2022). The form assessed preoperative and postoperative mobilization, and evaluated comfort, pain, and sleep quality using separate Visual Analog Scales (VAS) for each outcome
The PMS
The PMS assesses the levels of pain and difficulty experienced by patients during four activities after surgery: turning from one side to another, sitting on the bedside, standing up on the bedside, and walking in the patients’ room. The scale uses a 15 cm VAS, with scores ranging from 0 to 15 for each activity. Higher scores indicate higher levels of pain and difficulty. The scores for pain and difficulty in each activity are summed to obtain a total PMS score, which ranges from 0 to 120. The Cronbach’s alpha values for the original scale were .98 for postoperative day 1 and .98 for postoperative day 2 (Heye et al., 2002). The Turkish version of the PMS had a Cronbach’s alpha value of .90 (Ayoğlu, 2011).
Interventions
The study consisted of two stages: the preoperative stage and the first postoperative day.
Preoperative Period
Before surgery, eligible participants, who met the inclusion criteria, were informed about the study’s aim, and written and verbal consent was obtained. All groups completed the perioperative information form and the PMS. Participants were then allocated to the control or intervention groups.
The intervention group received “Early Mobilization Training” using training materials prepared by the researchers. The training covered techniques and considerations for turning in bed, sitting and standing up from the bedside, and walking in the patient’s room. Information was also provided about the recommended duration of being out of bed on the day of surgery and the postoperative days. Expert opinion was received from 10 nursing faculty members to maintain the content validity of the training material. Item-content and scale-content validity index were above 0.80. A live mannequin performed each stage of the mobilization, which was photographed and explained in the material. The training material was printed as an A5-size color brochure. On the other hand, participants in the control group received routine postoperative care provided by the clinic. This typically included pain management, monitoring of vital signs, wound care, and assistance with activities of daily living as needed. Early mobilization in the control group was initiated passively by the clinical nurse, the patient’s relatives, or floor-care staff, provided there were no contraindications. No structured training or guidance on mobilization was offered. In contrast, the intervention group received the same routine care in addition to structured early mobilization training, which was provided by the researcher prior to surgery.
A standardized anesthesia protocol was followed for all patients undergoing laparoscopic cholecystectomy. Premedication included midazolam (0.03 mg/kg) to induce sedation. For anesthesia induction, fentanyl (1.5 mg/kg), propofol (2 mg/kg), and rocuronium (0.6 mg/kg) were administered. The anesthesia was sustained using a 50% nitrous oxide and oxygen mix, 1% to 2% sevoflurane, and remifentanil (0.5 mg/kg/min). Rocuronium (0.15 mg/kg) was also given for muscle relaxation. The administration of anesthetics was stopped upon completion of the surgery, and a single dose of neostigmine (0.05–0.07 mg/kg) or atropine (0.02–0.03 mg/kg) was given to reverse the muscle relaxant effects. Postoperatively, the patient was awakened and transferred to the recovery room. Ondansetron (0.1 mg/kg) and metoclopramide (0.1 mg/kg) were given to manage postoperative nausea and vomiting. A routine postoperative pain management protocol was used, with meperidine (1 mg/kg) administered three times daily (every 8 hr) on the first day after surgery. Intravenous (IV) fluid administration was applied at a rate of 6 to 8 ml/kg/hr throughout the surgery. An average of 1.5 to 2 liters of IV Isolayt fluid was given until the patient tolerated oral intake on the first postoperative day.
Postoperative Period
The first mobilization after surgery was performed by the researchers at the sixth postoperative hour for all participants. The second and third mobilizations were planned at 4-hr intervals and were applied uniformly to all patients according to the study protocol. Patients were also informed that they could be mobilized outside the planned hours whenever they felt well. The duration of mobilization was recorded on the information form. Patients were asked to complete the PMS and the VAS on pain, sleep quality, and comfort on the first postoperative day after mobilization. After the completion of posttest measurements, the early mobilization training material was also provided to participants in the control group as part of ethical research conduct.
Statistical Analysis
IBM SPSS Statistics for Windows (Version 26.0; IBM Corp., Armonk, NY, USA) was used for statistical analysis. Frequency analysis was used to analyze demographic and clinical characteristics. Data on the duration of postoperative mobilization, PMS scores, and the VAS scores on pain, comfort, and sleep quality were presented using descriptive statistics. The Shapiro-Wilk test and skewness and kurtosis values were used to compare the normal distribution of the data. An independent samples t-test was used for intergroup comparisons of continuous variables, while the chi-square test was used to compare categorical variables.
Ethical Consideration
The necessary approvals were obtained from the Scientific Research and Publication Ethics Committee of the university and ethic committee of the hospital. Written informed consent was obtained from all participants.
Results
In Table 1, the sociodemographic and clinical characteristics of the intervention and control groups are presented. The intervention group consisted of 51.28% females with a mean age of 44.82 ± 12.37 years. The control group consisted of 53.85% females with a mean age of 44.41 ± 10.80 years. There were no statistically significant differences in sociodemographic characteristics between the two groups (p > .05).
Sociodemographic and Clinical Characteristics.
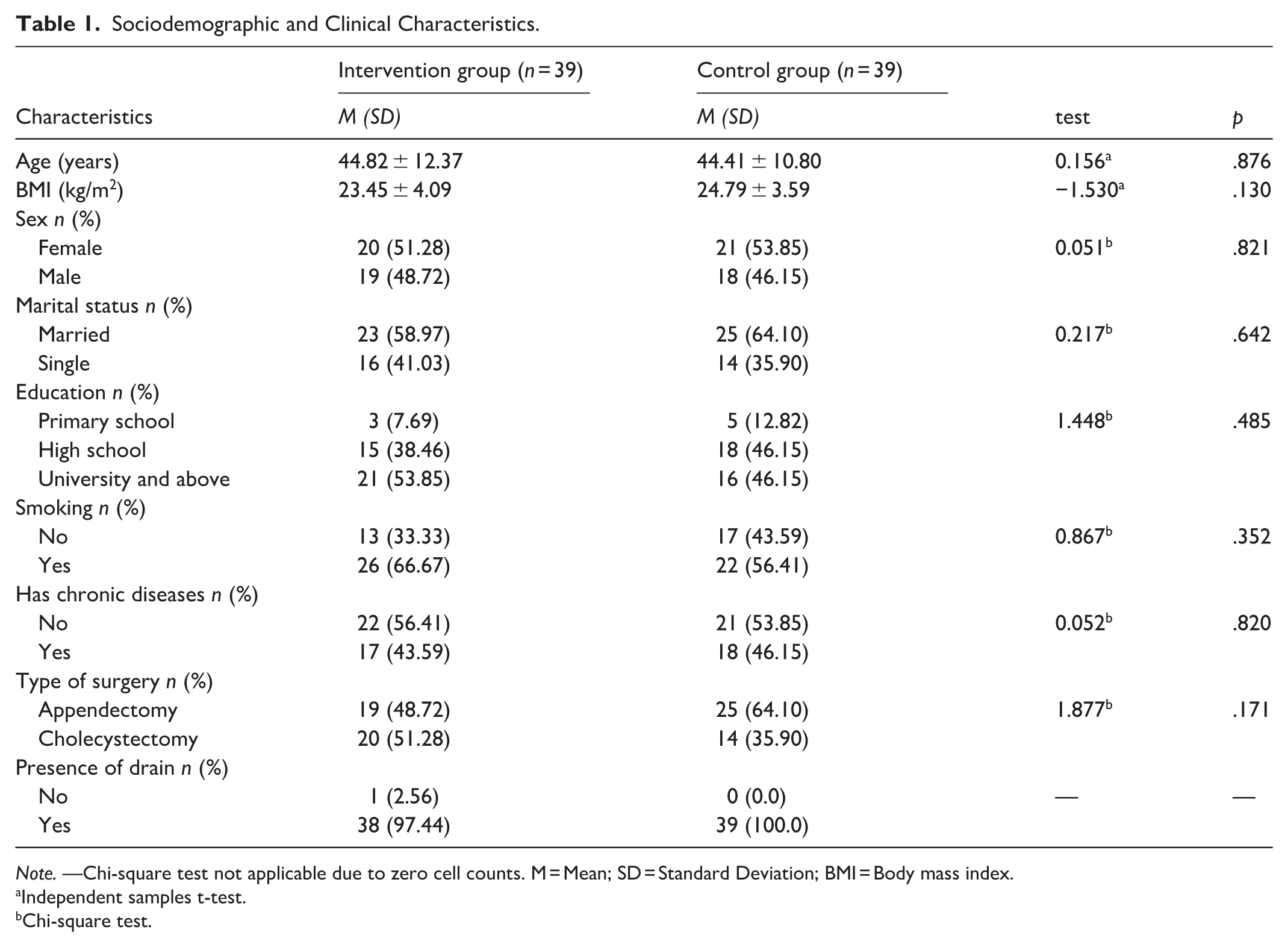
Note. —Chi-square test not applicable due to zero cell counts. M = Mean; SD = Standard Deviation; BMI = Body mass index.
Independent samples t-test.
Chi-square test.
Table 2 compares the duration of mobilization between the intervention and control groups. The intervention group had significantly longer duration for the first (12.44 ± 3.42 min), second (13.85 ± 3.13 min), and third mobilization (17.31 ± 4.27 min) compared to the control group (8.77 ± 2.15, 8.85 ± 2.42 and 6.67 ± 4.64 min, respectively) (p < .05). The total duration of other mobilizations from the third mobilization until discharge was also significantly higher in the intervention group (15.00 ± 6.88) than the control group (0.77 ± 2.93) (p < .05). The total duration of mobilization was also significantly higher in the intervention group (58.33 ± 11.20 min) compared to the control group (24.92 ± 5.64 min) (p < .05). In addition, the length of hospital stay was significantly shorter in the intervention group (1.38 ± 0.49 days) compared to the control group (2.15 ± 0.67 days) (p < .05).
Comparison of the Duration of Mobilization.
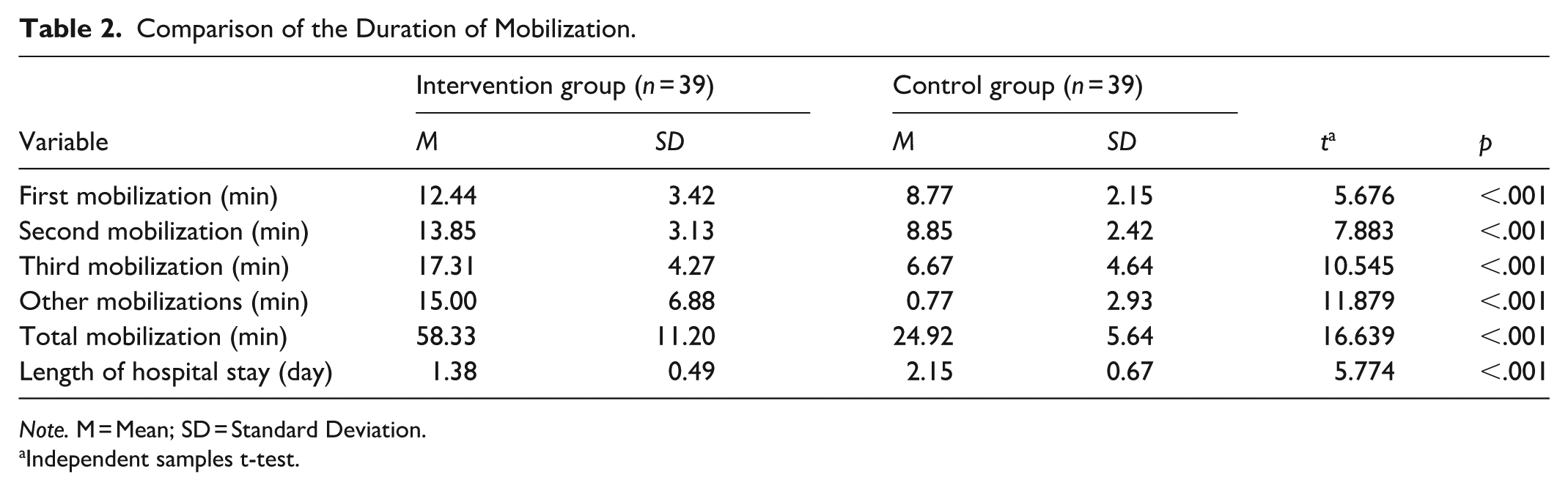
Note. M = Mean; SD = Standard Deviation.
Independent samples t-test.
Table 3 presents the comparison of the VAS scores for postoperative pain, comfort, and sleep quality. The mean postoperative pain scores of the intervention and control groups were 6.28 ± 1.23 and 9.23 ± 1.18, respectively. There was a statistically significant difference between the postoperative pain scores of the intervention and control groups (p < .05). On the other hand, the comfort scores of the intervention group while turning in the bed (7.46 ± 1.23), lying (7.28 ± 1.21), and sitting (7.36 ± 1.29) were significantly higher than the control group (p < .05). Moreover, the sleep quality score of the intervention group on the first postoperative day (6.31 ± 1.73) was statistically significantly higher than the control group (2.90 ± 1.86) (p < .05). Although not shown in the table, the presence of drain (87.18% and 71.79%), pain (56.41% and 87.18%), and noise (46.15% and 56.41%) affected the comfort of patients in the intervention and control groups, respectively.
Comparison of the VAS Scores on Pain, Comfort, and Sleep Quality.
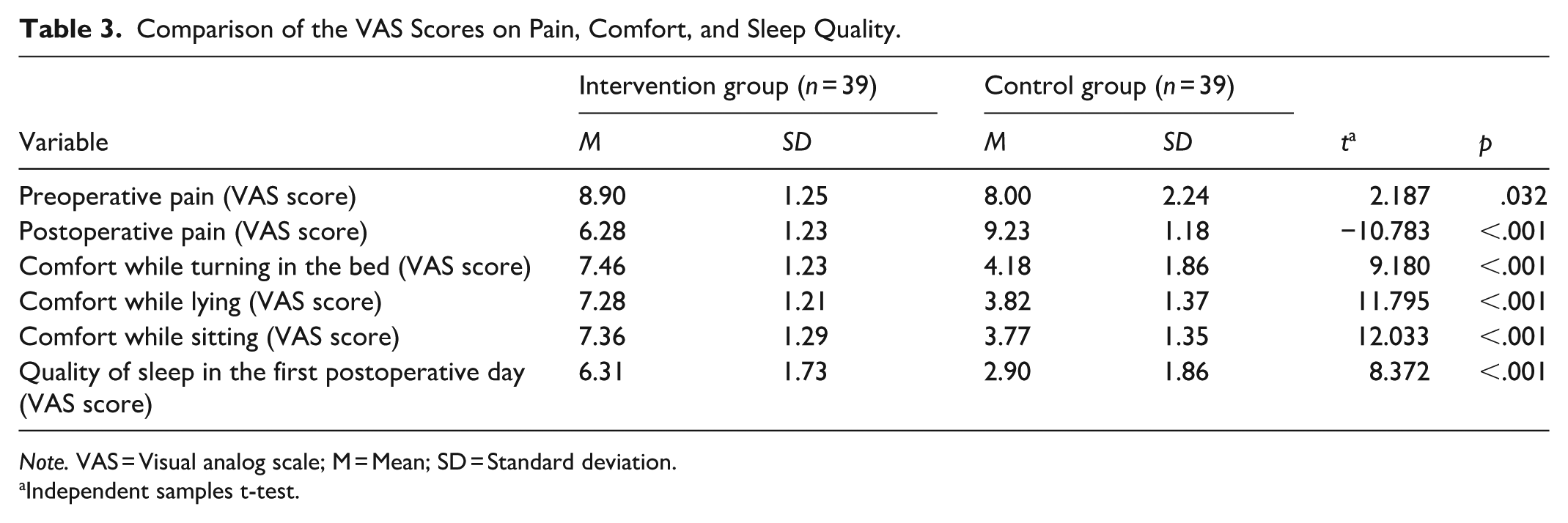
Note. VAS = Visual analog scale; M = Mean; SD = Standard deviation.
Independent samples t-test.
Table 4 displays the findings on the comparison of the preoperative and postoperative PMS scores. No statistically significant difference was found between the preoperative PMS results of the patients in the intervention and control groups (p > .05). Accordingly, there was a significant difference between the scores obtained by the intervention and control groups from the turning in bed from one side to another (pain and difficulty), sitting on the bedside (pain and difficulty), standing up on the bedside (pain and difficulty) and walking in the patient’s room (pain and difficulty) (p < .05). On the other hand, the mean PMS score in the intervention group (39.42 ± 16.88) was significantly lower than the control group (98.08 ± 16.63) (p < .05).
Comparison of the Patient Mobility Scale Scores.
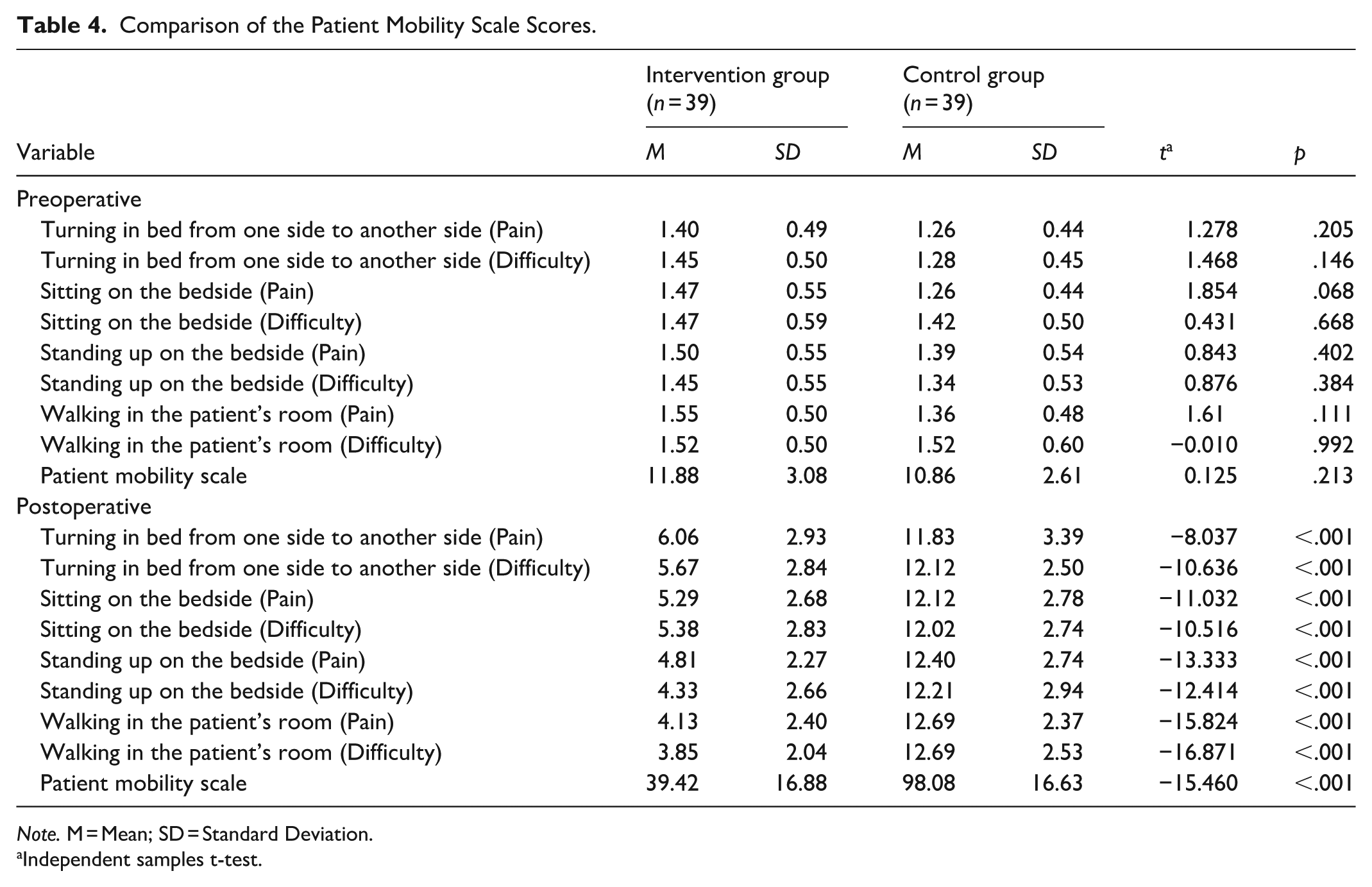
Note. M = Mean; SD = Standard Deviation.
Independent samples t-test.
Discussion
The findings of this study demonstrated that early mobilization training had positive effects on mobility, pain, comfort, and sleep quality in patients undergoing abdominal surgery. The study followed the early mobilization protocol recommended by the ERAS guidelines, which suggests mobilizing patients for 2 hr on the day of surgery and 6 hr daily thereafter (Gustafsson et al., 2019). In this study, all patients underwent their first mobilization at the sixth hour postoperatively in accordance with the clinical protocol. The total duration of mobilization and the duration of mobilization on the first, second, and third postoperative days were significantly higher in the intervention group compared to the control group. This suggests that the early mobilization training effectively increased the amount of time patients spent mobilizing after surgery. Recent studies comparing ERAS protocols with conventional perioperative care have consistently demonstrated earlier postoperative mobilization in patients managed under ERAS pathways. For instance, postoperative mobilization was initiated significantly earlier in the ERAS group compared to the conventional care group (12 vs. 18 hr; p < .012) (Rida et al., 2024). Similarly, time to ambulation was significantly shorter among patients receiving ERAS-based care than those managed with conventional protocols (p = .008) (Yilmaz et al., 2020). In another study, patients who underwent pancreatic surgery were given an early mobilization protocol according to the ERAS protocol. The study found that patients in the intervention group were mobilized earlier after surgery, and that the overall average daily walking distance was statistically significantly greater between the first and seventh days after surgery and during hospitalization (Li et al., 2024). In addition to these, Nishijima et al. (2020) reported that early mobilization education positively contributed to the postoperative mobilization period in patients who underwent abdominal surgery. In conclusion, these studies demonstrate that early mobilization education extends mobilization duration, leading to a faster recovery. Nurses should encourage and support patients in the importance of early mobilization in the postoperative period.
In the study by Koyuncu and Iyigun (2022), patients in the intervention group who underwent abdominal surgery began mobilization earlier after admission to the intensive care unit compared to those in the control group, and the time to first mobilization after surgery was shorter in the intervention group. This indicates that the early mobilization protocol implemented in the intervention group facilitated earlier mobilization initiation (Koyuncu & Iyigun, 2022). In the study by Widjaya et al. (2024) examining the effectiveness of the ERAS Nursing Program; the average time for patients who underwent laparoscopic cholecystectomy in the intervention group to start early mobilization after surgery was 3.45 hr, while it was 9.12 hr in the control group. In the study that included the best practices for early postoperative mobilization in patients undergoing abdominal surgery, it was stated that early mobilization practices had a positive effect on recovery parameters such as the time to first in-bed exercise, the time to first out-of-bed exercise, and the distance of first ambulation (Hu et al., 2019). Consistent with the existing literature, the current study found that the total duration of mobilization in the intervention group was higher, indicating the effectiveness of the preoperative training. These findings collectively suggest that implementing routine early mobilization protocols, supported by preoperative training, can contribute to improved patient outcomes and potentially increase employee satisfaction by promoting proactive patient care.
Length of hospital stay is another outcome of early mobilization practices, which constitute an important step of perioperative care. A study by Qin et al. (2024) reported that patients who followed the ERAS protocol after laparoscopic cholecystectomy had shorter hospital stays. Nishijima et al. (2020) reported lower postoperative complications and earlier hospital discharge in early mobilized patients (Nishijima et al., 2020). A meta-analysis by Sauro et al. (2024) indicated that implementation of the ERAS guidelines reduced hospital length of stay by an average of 1.88 days. Similarly, a systematic review and meta-analysis by McKechnie et al. (2024) evaluated the effectiveness of ERAS protocols in patients undergoing intra-abdominal surgery. In the upper gastrointestinal subgroup, across five randomized controlled trials, the ERAS group had a mean postoperative hospital stay that was 3.35 days shorter, while in the lower gastrointestinal subgroup, the reduction was 2.80 days across two trials. In the present study, the length of hospital stay in the intervention group was found to be 0.77 days shorter than in the control group (1.38 ± 0.49 vs. 2.15 ± 0.67 days, respectively). This outcome supports the potential benefits of early mobilization interventions. Encouraging early mobilization through nurse-led initiatives may significantly enhance patient recovery. Moreover, by reducing hospital stay, early mobilization can contribute to healthcare cost savings and help alleviate the workload of healthcare professionals.
Maintaining patient comfort in the postoperative period is an indicator of the quality of healthcare. The comfort levels of the intervention group while turning in bed, lying, and sitting were higher than those of the control group. Therefore, we can suggest that early mobilization training was effective in increasing patient comfort by providing pain control. A good comfort level during the recovery period will have positive effects on patient recovery (Aydıngulu & Arslan, 2021). Because of this reason, nurses and other health professionals have important responsibilities in taking and implementing measures to increase patient comfort during the preoperative period. We also found that the presence of the drain had a negative effect on 87.18% of the patients in the intervention and 71.9% of the patients in the control groups. Recent evidence indicates that surgical drains can cause substantial discomfort and negatively impact postoperative quality of life, limiting the ability to perform daily activities and increasing pain levels in many patients (Gadiraju et al., 2025). In addition, evidence-based drain management within perioperative care frameworks suggests that tailored and early removal practices may improve postoperative outcomes and recovery when integrated with comprehensive recovery protocols (Salib et al., 2025). Other studies found that the presence of a drain after surgical intervention may delay or prevent mobilization by increasing their dependency and pain levels (Akpolat et al., 2021; Lim & Panahkhahi, 2017). Nurses should mobilize patients after minimizing the factors that prevent early mobilization and providing a safe environment. While preoperative mobilization training is given to patients, they should be informed that they can be mobilized with drains/catheters, etc., and that these equipment will not prevent mobilization from being used safely. Furthermore, ERAS protocols recommend that routine use of prophylactic drains should be avoided (Tan et al., 2023). Drains/catheters, etc., should be removed as soon as the indication is over; these practices should be made routine practices of the clinics, and nurses play a very important role in the follow-up of the process.
Sleep is a physiological requirement for survival. Factors such as hospital stay, surgical operations, environmental factors, anxiety, and pain may reduce the quality of sleep (Ji & Liu, 2025; Para & Uslu, 2022). Recent studies show that sleep disorders are quite common in the perioperative period and become particularly pronounced in the early postoperative period. It is reported that sleep disorders occurring during this period delay the healing process, increase pain perception, and negatively affect functional recovery (Ji & Liu, 2025). A study reported that 30.7% of patients experienced sleep problems before surgery and 59.6% experienced sleep problems on the night of surgery, which can have negative effects on patient comfort and recovery, leading to prolonged hospital stays (Özşaker et al., 2019). Furthermore, it is emphasized that impaired sleep quality in the postoperative period is associated with fatigue, decreased physical, emotional, and mental function, and may negatively affect early mobilization (Ayenew et al., 2025; Guo et al., 2025). Therefore, maintaining adequate sleep before and after surgery will contribute to postoperative recovery. Consistent with the literature, the sleep quality score of the participants in the intervention group was higher than that of the control group (Koyuncu & Iyigun, 2022; Ni et al., 2018). Therefore, clinical nurses should include early mobilization practices in nursing care protocols to improve sleep quality, facilitate recovery, and help patients cope with surgical stress.
Prevention or reduction of postoperative pain is among the responsibilities of healthcare professionals. Poorly managed acute postoperative pain may lead to the development of chronic post-surgical pain, which occurs in 20%–30% of patients after various common operations with an important negative impact on patients’ quality of life (Rosenberger & Pogatzki-Zahn, 2022). The pain scores in the intervention and control groups of this study were 6.28 and 9.23, respectively. Existing studies have reported that early mobilization programs had positive effects on pain management (Daryani et al., 2023; Idawati et al., 2023). The findings of this study may be explained with reference to the fact that the positive effects of mobilization on relieving pain were emphasized during the early mobilization training. Nurses and other healthcare professionals have a moral obligation to manage postoperative pain. This underscores the necessity for nurses to be well versed in pain assessment and management strategies to enhance patient outcomes and promote a better recovery process.
Early mobilization after surgery has been shown to facilitate patient recovery and minimize the risks of complications (Castro et al., 2015). Consistent with this, the PMS scores of the participants in the intervention group were significantly lower, indicating a higher level of mobility compared to the control group. This aligns with a previous study that found participants who received preoperative training had a higher level of mobility (Ayoğlu, 2011). Jones et al. (2020) demonstrated a 40% increase in mobility after implementing a nurse-led mobility program to mitigate immobility-related risks, emphasizing that the program was effective in promoting safe and early mobilization (Jones et al., 2020). Additionally, Boerrigter et al. (2022) reported that 87.4% of patients undergoing gastrointestinal and oncological surgery achieved the highest possible mobility scores during the first three postoperative days with the aid of mobilization training (Boerrigter et al., 2022). Based on these findings, it is advisable to develop early mobilization protocols in surgical clinics and incorporate them into routine practices. Early mobilization has positive effects on patient outcomes, including patient satisfaction, early discharge, and a reduction in postoperative complications.
This study, with its randomized controlled experimental design, provides high-level evidence and comprehensively evaluates the effects of early mobilization training on multidimensional outcomes such as mobility, pain, comfort, sleep quality, and length of hospital stay in patients undergoing abdominal surgery. The intervention’s positive contributions to both physical and psychosocial patient outcomes are consistent with the holistic care approach. Demonstrating that an education-based and applicable intervention is effective provides practical suggestions for healthcare professionals, while also providing valuable information regarding the efficient use of hospital resources. Reporting the study in accordance with the CONSORT 2010 principles is another strength that increases its scientific validity and reliability.
This study has several limitations. First, the study was conducted in a single center using a convenience sampling method and included only patients who underwent laparoscopic abdominal surgery. Therefore, the results may not be generalizable to other surgical populations, settings, or open surgical procedures. Second, neither participant nor researcher blinding was implemented, as both the researchers and participants were aware of group allocation during the intervention and data collection processes. Statistical analyses were performed by an independent statistician who was blinded to group allocation. However, the lack of blinding during the intervention and data collection processes may have introduced performance or detection bias. In addition, a standardized anesthesia and analgesic protocol was applied to all participants, which may have influenced postoperative pain and mobility outcomes and should be considered a potential confounding factor. Another limitation is the short follow-up period, which was restricted to the first postoperative day. As a result, the longer-term effects of early mobilization training on patient outcomes could not be evaluated. Finally, the inclusion of patients with chronic conditions that may affect mobilization could have influenced the outcomes, despite randomization.
Conclusion
In line with the study hypotheses (H1–H5), the results of this study demonstrate that early mobilization training for laparoscopic abdominal surgery patients is beneficial in terms of longer duration of mobilization, improved mobility, lower pain scores, increased patient comfort, and enhanced sleep quality. These findings highlight the significance of implementing early mobilization protocols as a routine practice in surgical wards while considering the unique characteristics of individual patients. To gain further insights into the factors influencing the early mobilization of surgical patients and to develop individualized early mobilization programs, it would be valuable to conduct qualitative studies involving clinic nurses and patients. These studies could explore the barriers and facilitators of early mobilization, patient preferences, and experiences, as well as the perspectives of healthcare professionals. Such research can contribute to the development of tailored interventions and strategies to optimize early mobilization practices and promote positive patient outcomes. Also, further research involving diverse patient populations and surgical procedures would help to better understand the generalizability of the findings.
Supplemental Material
sj-doc-1-cnr-10.1177_10547738261433799 – Supplemental material for Effects of Early Mobilization Training on Mobility, Pain, Comfort, and Sleep Quality in Laparoscopic Abdominal Surgery Patients: A Randomized Controlled Trial
Supplemental material, sj-doc-1-cnr-10.1177_10547738261433799 for Effects of Early Mobilization Training on Mobility, Pain, Comfort, and Sleep Quality in Laparoscopic Abdominal Surgery Patients: A Randomized Controlled Trial by Fatma Nur Daldaban and Sevinc Tastan in Clinical Nursing Research
Footnotes
Acknowledgements
The authors would like to express their sincere gratitude to all participants who contributed to this study. The English translation of the manuscript from Turkish was supported by ChatGPT, an AI language model developed by OpenAI.
Ethical Considerations
To carry out the research, ethics committee permits were obtained from the Eastern Mediterranean University (ETK00-2022-0104) and the Dr. Burhan Nalbantoglu State Hospital (YTK.1.01-Ek 21/22). Necessary permissions were obtained by e-mail from the authors of the scales used in the research.
Consent to Particpate
Written permission was obtained from the patients participating in the research with the “Voluntary Informed Consent Form.”
Author Contributions
The study was designed and analyzed collaboratively by F.D. and S.T. Data collection was carried out by F.D.. The manuscript was written by F.D. under the academic supervision of S.T., and both authors contributed to the final version. All authors contributed to the final data analysis and critically revised the manuscript for important intellectual content
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data are available from the corresponding author upon reasonable request.*
Clinical Trial Registration
The full research protocol is available at ClinicalTrials.gov (NCT05657561).
Effects of Early Mobilization Training on Mobility, Pain, Comfort, and Sleep Quality in Laparoscopic Abdominal Surgery Patients: A Randomized Controlled Trial
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
